Abstract
Background:
CHA2DS2-VASc score has been validated in risk prediction for stroke and thromboembolism in patients with atrial fibrillation (AF). Association of CHA2DS2-VASc score with higher risk of venous thromboembolism and pulmonary embolism (PE) has also been shown. In this study, we investigated the long-term prognostic value of CHA2DS2-VASc score in patients with acute pulmonary embolism (APE).
Methods:
Consecutive patients with APE presenting to our emergency department were retrospectively recruited. Patients with AF and who died secondary to causes other than PE were excluded from the study. The CHA2DS2-VASc score and pulmonary embolism severity index (PESI) were calculated.
Results:
Two hundred seventy seven participants were included in the study. The mortality rate was 18.7%. Twenty-two cases died within 30 days, and 30 cases died during the follow-up period (median: 13 months). The mean CHA2DS2-VASc score was significantly higher in dead patients compared to survivors (3.61 ± 1.35 vs 1.95 ± 1.52, P < .01). In multivariate regression analysis, systolic pulmonary artery pressure (hazard ratio [HR]: 1.03, 95% confidence interval [CI]: 1.01-1.06, P = .02), PESI score (HR: 1.010, 95% CI: 1.004-1.017, P < .01), and CHA2DS2-VASc score (HR: 1.67, 95% CI: 1.19-2.16, P < .01) were found to be independently correlated with mortality. The patients whose CHA2DS2-VASc score was between 1 and 3 had 5.67 times and patients whose CHA2DS2-VASc score was ≥4 had 16.8 times higher risk of mortality compared to patients with CHA2DS2-VASc score = 0.
Conclusion:
Patients with higher CHA2DS2-VASc scores had higher rates of mortality after APE.
Introduction
Acute pulmonary embolism (APE) is a common clinical presentation of venous thromboembolism (VTE) and is associated with high mortality rates, especially in patients presenting with hemodynamic instability. 1 Cardiovascular risk factors such as hypertension (HT), diabetes mellitus (DM), hypertriglyceridemia, low high-density lipoprotein (HDL) cholesterol levels, and obesity have been shown to be associated with an increased risk of VTE. 2 Besides, pulmonary embolism (PE) risk is higher in patients with cardiovascular diseases such as myocardial infarction (MI) and heart failure (HF), 3,4 and patients with VTE have an increased risk of MI and stroke. 5
Several prognostic indicators of mortality such as admission clinical properties and laboratory parameters have been defined in APE. 6 –10 Pulmonary embolism severity index (PESI) is a powerful predictor of worse prognosis, and clinical use of PESI is recommended by the European Society of Cardiology. 7,11,12
CHADS2 and CHA2DS2-VASc scores have been widely used in patients with atrial fibrillation (AF) for the prediction of risk of thromboembolic events and also for the management of anticoagulant therapies. 13,14 Higher CHA2DS2-VASc scores have been shown to be correlated with a higher risk of APE in patients with AF. 15 In addition, potential clinical use of CHA2DS2-VASc score in patients with HF and coronary artery disease (CAD) has been shown. 16,17
Several reports suggest that there is a close association between components of the CHA2DS2-VASc score and risk of VTE. 18 –25 From this point of view, we speculated the hypothesis that higher CHA2DS2-VASc scores might be associated with risk of mortality in patients with APE.
Materials and Methods
Study Population
Medical records of our institution were screened for patients who were treated with the diagnosis of APE between January 2011 and January 2015. Initially, a total number of 343 participants were recruited. The exclusion criteria were acute coronary syndrome within the previous 30 days, renal or hepatic failure, acute infectious disease, severe chronic obstructive pulmonary disease, active cancer, heart rhythm other than sinus on 12-lead electrocardiogram, use of anticoagulant drugs before the admission, anemia (a hemoglobin level <13 g/dL in men and <12 g/dL in women), history of blood transfusion within the last 3 months, hematological disorders, and use of immunosuppressant medication. In addition, we excluded cases with a history of PE. According to these criteria, 45 cases were excluded from further analysis.
For the evaluation of long-term events, hospital records, telephone interviews, and state-wide death registry database were used. Patients who were defined to die secondary to causes other than PE were excluded from the study. This group included 7 cases of acute coronary syndrome, 2 cases of cerebrovascular accident, 4 cases of HF, and 8 cases of noncardiac death. Finally, a total number of 277 patients were included in the study. In all of the analysis, we have compared dead patients with survived patients. The study was approved by the local ethics committee.
Definitions
Acute PE was diagnosed by the presence of typical clinical symptoms and abnormal findings in the laboratory parameters, transthoracic echocardiography, and contrast-enhanced computed tomography (CT). In the study population, all of the cases had CT imaging.
Demographic and clinical variables that are components of the CHA2DS2-VASc score were obtained from the hospital database. The CHA2DS2-VASc score is a risk stratification score that ranges from 0 to 9 and is calculated as follows: congestive HF (1 point), HT (1 point), age 65 to 74.9 years (1 point), age ≥75 years (2 points), DM (1 point), stroke (2 points), vascular disease (1 point), and female gender (1 point). 26 The CHA2DS2-VASc score was calculated for each patient. We separated patients into 3 groups such as CHA2DS2-VASc score = 0, between 1 and 3, and ≥4.
Pulmonary embolism severity index is a validated scoring tool estimating 30-day mortality related to APE. 9 For risk stratification, patients’ PESI scores that included 11 parameters (age, male sex, cancer, chronic HF, chronic pulmonary disease, pulse rate, systolic blood pressure [BP], respiratory rate, temperature, altered mental status, and arterial oxyhemoglobin saturation) were calculated. 7 Hypertension was defined as the use of antihypertensive drugs or initial BP over 140/90 mm Hg, DM was defined as the use of antidiabetic drugs or fasting plasma glucose levels of >126 mg/dL, and hyperlipidemia was defined as total serum cholesterol levels >240 mg/dL. Smoking status was defined as current tobacco use. Hypotension was defined as a systolic BP <90 mm Hg or a pressure drop of more than 40 mm Hg for longer than 15 minutes if not caused by a new-onset arrhythmia, hypovolemia, or sepsis. 7 Congestive HF was defined as moderate to severe systolic dysfunction or patients with recent decompensated HF requiring hospitalization, irrespective of ejection fraction. 26 Vascular disease was defined as history of MI, peripheral arterial disease, or aortic atherosclerosis. 13
Laboratory Analysis
According to the hospital protocol, venous blood samples were taken from antecubital vein and collected in calcium EDTA tubes during the emergency admission. Blood counts were studied by an autoanalyzer (Cell-Dyn 3700, Abbott Laboratories, Illinois, USA) within 30 minutes after blood sampling. The results of other routine biochemical laboratory parameters, such as maximal troponin I, brain natriuretic peptide (BNP),
Echocardiography and CT Imaging
A complete echocardiographic study was performed with Vivid 3 system (General Electric, Norway) during the initial evaluation of the patients. Systolic pulmonary arterial pressure (sPAP) was calculated by adding transtricuspid pressure gradient to mean right atrial pressure estimated from inferior vena cava diameter and motion during respiration as follows: mean right atrial pressure was estimated to be 5 mm Hg if there was a complete collapse of a normal diameter inferior vena cava during inspiration; 10 mm Hg if a normal diameter inferior vena cava collapse was >50%; 15 mm Hg if a dilated inferior vena cava collapsed by >50% with inspiration; and 20 mm Hg if there was no visible evidence of dilated inferior vena cava collapse. 27
Multislice spiral 64-slice CT was performed in the radiology clinic using PE protocol (field of view: 35 cm, section thickness: 3 mm, contrast material volume: 135 mL, and contrast material injection rate: 4 mL/s). Diagnosis of APE was established in case of a complete or partial luminal filling defect in the main pulmonary artery or its branches.
Medications
Enoxaparin was commenced in all patients with a dose of 1 mg/kg twice a day immediately after the diagnosis of APE was ascertained. Thrombolytic treatment (tissue plasminogen activator [tPA]) was given as an intravenous infusion of 100 mg in 2 hours in patients with hemodynamic instability. Oral warfarin therapy was started in all patients on the day of admission, except for the cases treated with tPA who had warfarin treatment 24 hours after the therapy. Patients continued oral anticoagulation therapy for at least 3 months after discharge. The duration of oral warfarin therapy was left to the discretion of the primary physician.
Statistical Analysis
All data were presented as a mean ± standard deviation (SD) or a median [interquartile range] for parametric variables and as percentages for categorical variables. Continuous variables were checked for the normal distribution assumption using Kolmogorov-Smirnov statistics. Differences between survivors and nonsurvivors were evaluated using independent samples t test or Mann-Whitney U test. Categorical variables were tested by Pearson χ2 test and Fisher exact test. Cox regression analyses were used to investigate the univariable and multivariable predictors of mortality during the study period. Forward stepwise multivariable regression models using parameters with P < .10 were created in Cox regression analyses. Kaplan-Meier estimates and curves were generated (Figure 1), and CHA2DS2-VASc subgroups were compared using log-rank tests. P values were 2 sided, and values <.05 were considered statistically significant. All statistical studies were carried out using Statistical Package for Social Sciences software (SPSS 16.0 for Windows; SPSS Inc, Chicago, Illinois).
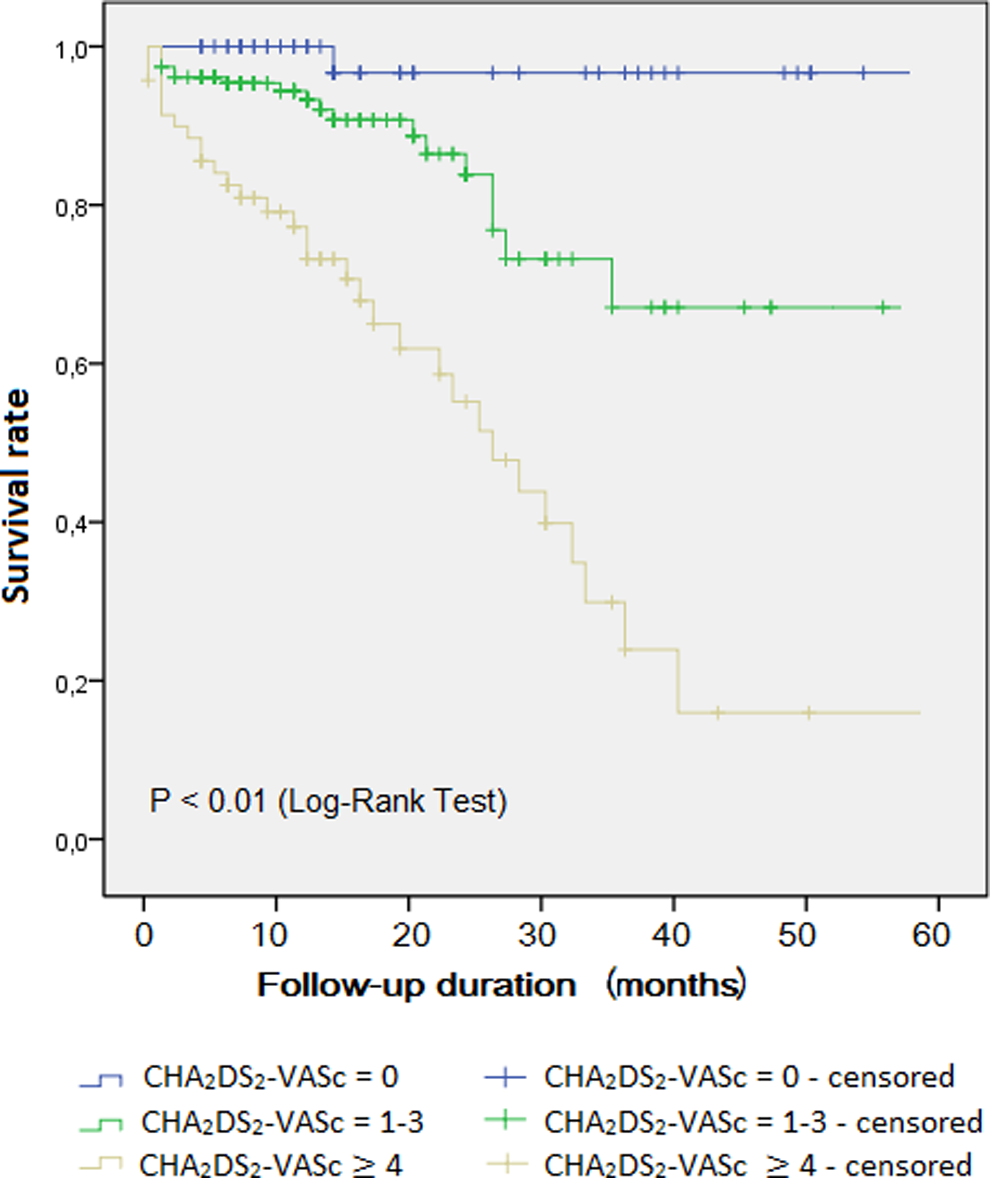
Kaplan-Meier curve showing the significant mortality difference between CHA2DS2-VASc subgroups.
Results
During a follow-period of 13 [15] months, 52 (18.7%) patients died. Twenty-two of the dead participants died within 30 days. Clinical, demographic, and laboratory characteristics of the survived and dead patients are summarized in Tables 1 and 2. Between the 2 groups, significant differences were observed in terms of age, gender, systolic BP, history of HT, congestive HF, CAD, and cerebrovascular disease. The mean PESI scores and systolic pulmonary artery pressure were significantly higher in the dead patients compared to the survived patients (151 ± 60 vs 77 ± 24 mm Hg and 71 ± 18 vs 49 ± 10 mm Hg; P < .01 and P < .01, respectively). Hemoglobin, white blood cell count, fasting glucose, maximal troponin I, and BNP levels were significantly higher, and total cholesterol, HDL cholesterol, low-density lipoprotein cholesterol, and triglyceride levels were significantly lower in dead patients compared to survived patients. However, platelets, urea, creatinine, and maximal
Comparison of Demographic and Clinic Parameters and Clinical Outcome of the Study Population.
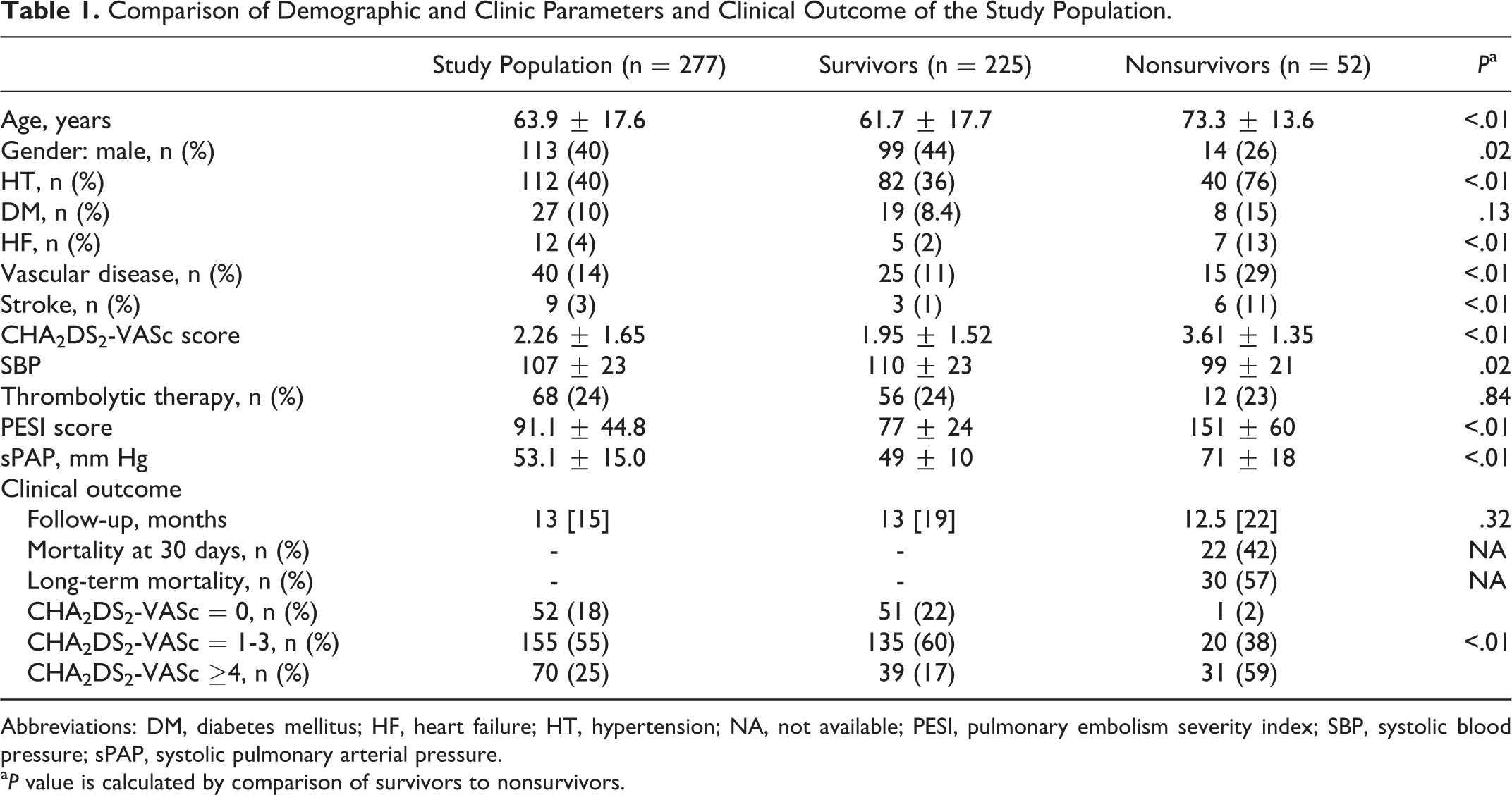

Abbreviations: DM, diabetes mellitus; HF, heart failure; HT, hypertension; NA, not available; PESI, pulmonary embolism severity index; SBP, systolic blood pressure; sPAP, systolic pulmonary arterial pressure.
a P value is calculated by comparison of survivors to nonsurvivors.
Comparison of Laboratory Parameters in the Study Population.
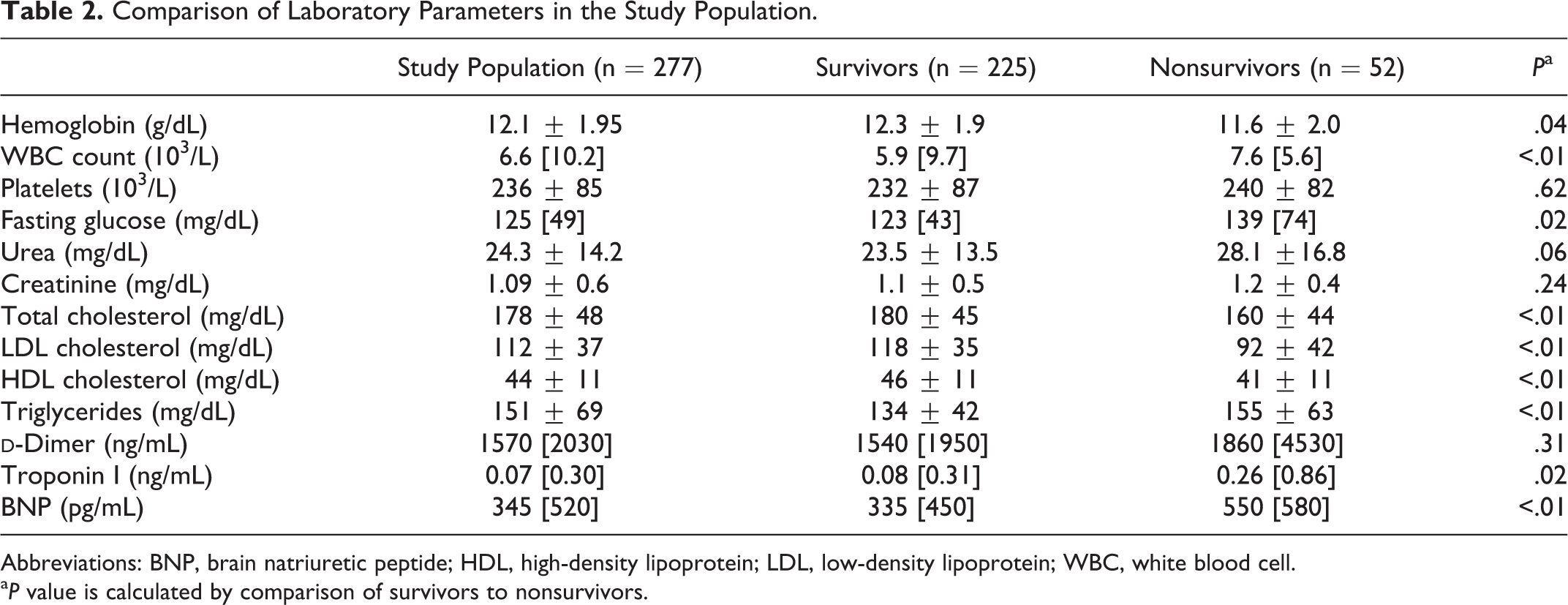
Abbreviations: BNP, brain natriuretic peptide; HDL, high-density lipoprotein; LDL, low-density lipoprotein; WBC, white blood cell.
a P value is calculated by comparison of survivors to nonsurvivors.
The mean CHA2DS2-VASc score was significantly higher in dead patients compared to survivors (3.61 ± 1.35 vs 1.95 ± 1.52, P < .01). The frequency of patients whose CHA2DS2-VASc score = 0 (2% vs 22%) and CHA2DS2-VASc score = 1 to 3 (38% vs 60%) was lower, and the frequency of patients with CHA2DS2-VASc score ≥4 was higher in nonsurvivors (59% vs 17%, P < .01) compared to survivors.
In univariate Cox regression analysis, age, gender, systolic BP, PESI score, sPAP, troponin I, BNP, and CHA2DS2-VASc score were found to be correlated with mortality in the study population (Table 3). In multivariate regression analysis, using model adjusted for the aforementioned parameters, CHA2DS2-VASc score (hazard ratio [HR]: 1.67, 95% confidence interval [CI]: 1.19-2.16, P < .01), PESI scores (HR: 1.010, 95% CI: 1.004-1.017, P < .01), and sPAP (HR: 1.03, 95% CI: 1.01-1.06, P = .02) were found to be independently correlated with mortality. The patients whose CHA2DS2-VASc score = 1 to 3 had 5.67 times higher risk for mortality, and patients whose CHA2DS2-VASc score ≥4 had 16.8 times higher risk for mortality compared to patients with CHA2DS2-VASc score = 0 (P < .01 and P < .01). In Kaplan-Meier curve, patients with CHA2DS2-VASc score = 1 to 3 and patients with CHA2DS2-VASc score ≥4 had significantly higher risk for mortality (log-rank P < .01).
Univariate and Multivariate Cox Regression Analysis of Possible Predictors of Total Mortality in the Study Population.
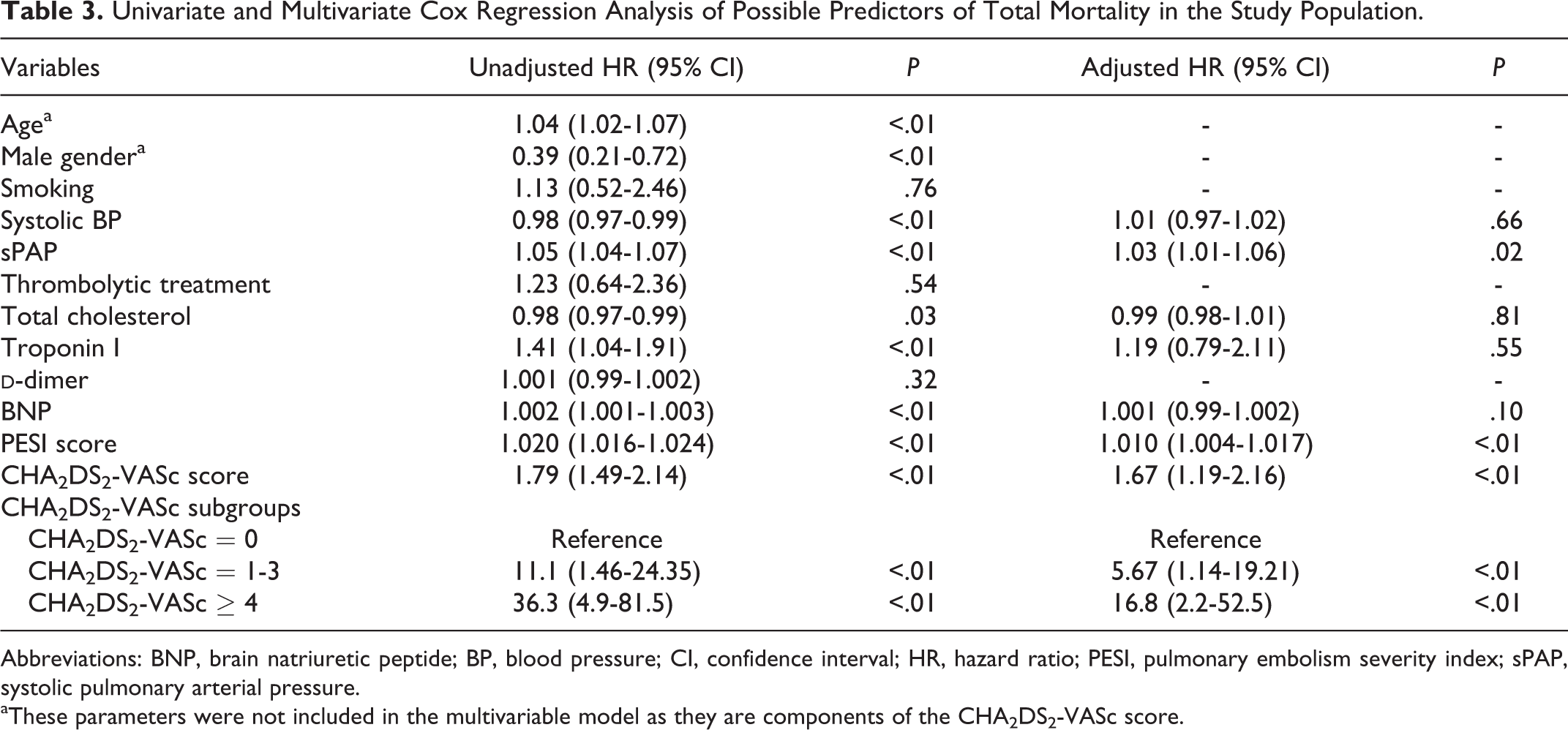
Abbreviations: BNP, brain natriuretic peptide; BP, blood pressure; CI, confidence interval; HR, hazard ratio; PESI, pulmonary embolism severity index; sPAP, systolic pulmonary arterial pressure.
aThese parameters were not included in the multivariable model as they are components of the CHA2DS2-VASc score.
Discussion
In this study, we have shown that mortality rate of APE increased with increasing CHA2DS2-VASc scores. Patients whose CHA2DS2-VASc score ≥4 had 16.8 times higher risk for mortality compared to patients with CHA2DS2-VASc score = 0. The CHA2DS2-VASc scoring system is easy to apply and is familiar to clinicians in daily practice. Thus, we suppose that it may have clinical use in patients with APE besides PESI.
Several studies suggest that VTE of unknown origin and cardiovascular disorders may share common risk factors. 25,28 The atherosclerotic risk factors such as obesity, diabetes, arterial HT, and dyslipidemia have also been demonstrated to be risk factors for VTE. 21,24,29 –32 Activation of platelets and coagulation cascade triggered by atherosclerosis that causes fibrin turnover is the basis of pathogenesis consequently. 33 –36 Diabetes mellitus is associated with increased levels of procoagulant factors. 37 Dyslipidemia is associated with hypercoagulability, endothelial dysfunction, and increased platelet aggregation. 38
Many of the risk factors of VTE and atherosclerosis are also the components of CHA2DS2-VASc score. The higher CHADS2 and CHA2DS2-VASc scores are associated with poor prognosis in cardiovascular diseases. Yaghi et al reported an association between presence of CHADS2 components and stroke-related in-hospital mortality in patients with AF. 39 Poçi et al noticed the correlation between CHADS2 score and poor prognosis in patients with acute coronary syndrome who do not have AF. 40 Paoletti Perini et al mentioned that CHA2DS2-VASc score is an independent predictor of major clinical events at 30-month follow-up in patients with HF. 16 Thus, we speculated the hypothesis that higher CHA2DS2-VASc scores may be associated with worse prognosis in patients with APE.
Saliba and Rennert have shown the association between CHA2DS2-VASc score and incidence of PE in a large number of participants with AF. 15 They have emphasized that patients with AF having higher CHA2DS2-VASc score also had a higher risk for PE. In addition, they have shown that all-cause mortality rate increased with increasing CHA2DS2-VASc score. However, the association of CHA2DS2-VASc score with mortality rate after APE was not reported. In our study, we have excluded cases with AF, and for the first time in the literature, our findings implicate the prognostic value of CHA2DS2-VASc in APE even if the participants are in sinus rhythm.
Pulmonary embolism severity index is accepted as a reliable clinical prognostic score for 30-day mortality. 9 In our study, the mean PESI scores were significantly higher in dead patients compared to survivors. In multivariate regression analysis, sPAP, PESI scores, and CHA2DS2-VASc score were found to be independently correlated with mortality. Some differences have been observed in our study population compared to large-scale studies of PE. In our study, female patients had higher mortality rates compared to males. This is a contradictory finding when PESI score is concerned, as male gender is a negative prognostic parameter in PESI. This study was performed in a tertiary center, which may affect the proportion of patients with high-risk features in the study population. As most of the study participants were referred from other hospitals, our findings may not directly reflect the general population. This result implies that the use of CHA2DS2-VASc score besides PESI score may give additional prognostic information in patients with APE.
Limitations
This is a retrospective, observational, and single-center study with limited number of patients and has inherent limitations of a retrospective design. The duration and effectiveness of the anticoagulant therapy during follow-up period could not be standardized. Nevertheless, all of the patients had international normalized ratio controls monthly after hospital discharge (according to the hospital protocol) for at least 3 months.
Conclusion
CHA2DS2-VASc score that is usually used in patients with AF can also be used for risk prediction in patients with sinus rhythm and APE. CHA2DS2-VASc score may further give prognostic clues besides PESI score, which is a well-validated score for risk stratification in APE. Further prospective studies are warranted to investigate the clinical use of CHA2DS2-VASc score in APE.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
