Abstract
The present study aimed to evaluate the effects of curcumin on the percentage of Tregs as well as miR-21 gene expression and IL-6 levels in peripheral blood mononuclear cells (PBMCs) in patients experiencing myocardial infarction (MI) compared to the controls. Isolation of PBMCs was performed from the peripheral blood of the subjects of the studied groups (50 patients with MI as a case group, and 50 controls). The effects of the low doses of curcumin (0.1 and 1 µM, for 48 h) on the studied parameters were evaluated and compared to the positive and negative controls in vitro. Flow cytometry analysis was used to determine the percentages of regulatory T cells. For gene expression measurement and cytokines assay, Real-time PCR and ELISA were carried out. The proportion of regulatory T cells was markedly lower in PBMCs from patients with MI (P = .03) compared to the controls. microRNA (miR)-21 expression (P = .01) was decreased while the serum level of IL-6 was increased (P = .008) in PBMCs from patients with MI compared to the controls. In vitro, curcumin treatment improved the percentage of Tregs (P =.02) while decreasing miR-21 expression (0.03) and the IL-6 level (P = .02) in PBMCs isolated from patients with MI when compared to untreated cells. The present study provided new insights into the mechanism of the anti-inflammatory effect of curcumin by affecting miR-21/Tregs in MI. Therefore, curcumin may be effective in the improvement of cardiac injury after MI through immunomodulatory mechanisms.
Highlights
miR-21/regulatory T cell axis control inflammatory response in patients with MI.
The proportion of Tregs is decreased in patients with MI while the gene expression of miR-21 is increased.
A low dose of curcumin can increase the percentage of Tregs and decrease the expression of miR-21 and IL-6 in patients with MI.
Introduction
Myocardial infarction (MI) and subsequent reperfusion injury are the most common and clinically significant forms of acute cardiac injury and result in the ischemic death of cardiomyocytes. 1 Infiltration of inflammatory cells including neutrophils, dendritic cells (DCs), and T cells into the injured myocardium suggests the role of inflammation in the pathogenesis of MI.2–4 Regulatory T cells (Tregs) are one of the sub-populations of CD4+ T cells that play a significant role in maintaining self-tolerance and suppressing autoimmunity.5–9 Tregs-induced M2-like differentiation within the healing myocardium is associated with decreased expression of inflammatory responses and activation of myofibroblast and increased expression of monocyte/macrophage-derived proteins. 5
MicroRNAs (miRs) are the small nucleic sequences that regulate gene expression and are important mediators in a wide range of cellular processes associated with the pathogenesis of various diseases.10–12 miRs can affect cellular processes in the infarcted heart, including neovascularization, cardiomyocyte, cell death, proliferation, and progenitor-cell-mediated repair.13,14 It was found that the circulating levels of miRs are associated with occurring cardiovascular diseases, and can be considered as a biological marker for heart failure, cardiac hypertrophy, and coronary disease.10,11 Therefore suppression or over-expression of miRs after MI may be useful to limit tissue injury and improve neovascularization to prevent long-term negative remodeling and heart failure. 13
miR-21 is known as an up-regulated miR in different cancers.15,16 It has been indicated that upregulation of mir-21 is associated with fibrosis enhancement via involvement in the anti-apoptosis process after MI in the infarcted zone. It has been also found that levels of miR-21 are up-regulated by ischemic stress in cardiac cells and the cardiomyocyte-derived from MI rats.17–20 In addition, there are several reports suggesting that miR-21 is involved in the development of several inflammatory diseases21,22 and T-cell differentiation.23,24 miR-21 is specifically up-regulated in Tregs in comparison to the conventional T cells, indicating that miR-21 may have an important role in Tregs biology. Increasing expression of miR-21 may regulate FOXP3 expression as the specific marker and transcription factor of Tregs.25,26
Curcumin is a natural component that is derived from the rhizomes of Curcuma longa with a wide range of cellular and pharmacological activities, including antioxidant, pro-apoptotic, anti-proliferative, chemotherapeutic, and anti-microbial properties.27–36 Mounting evidence shows that curcumin served as an excellent immunomodulatory agent in a wide range of conditions with uncontrolled inflammation.37,38 One of the most important aspects of the immune-modulatory effects of curcumin is affecting the function, development, or differentiation of Tregs which leads to the control of unfavorable inflammatory responses.39–41 It was found that curcumin balanced Treg/Th17 axis in several inflammatory diseases including, systemic lupus erythematosus (SLE), inflammatory bowel diseases, and diabetes type 2 associated with colitis.39,40,42,43 Regarding the effects on miR-21, curcumin treatment was found to reduce miR-21 promoter activity and expression in a dose-dependent manner by inhibiting AP-1 binding to the promoter and inducing the expression of the tumor suppressor Pdcd4 (programmed cell death protein 4). 44 To our knowledge, how curcumin affects inflammatory responses after MI has not been studied yet. We designed the present study to evaluate the impacts of curcumin on the proportions of Tregs and miR-21 as well as IL-6 as the pro-inflammatory cytokine in peripheral blood mononuclear cells (PBMCs) from patients with MI and the control group.
Material and Methods
Patients and Controls
This study was performed at the outpatient clinic of The First People's Hospital of Lanzhou City. Before this study, the approval of the Medical Ethical Committee of Shanxi Cardiovascular Hospital was obtained. And 50 MI patients (25 males and 25 females, mean age 57.6 ± 15.8 years) participated. MI was confirmed by definite 2 mm ST-segment elevations in at least two consecutive leads and a significant rise of creative kinase-MB and troponin I levels according to the previous study. 26 Control subjects were selected based on a recent angiography showing normal coronary arteries (25 males and 25 females, mean age 54.3 ± 14.9).
Patients with the following conditions were excluded from the study: (a) thromboembolism, disseminated intravascular coagulation, advanced liver disease, renal failure, malignant disease; (b) inflammatory disease or inflammatory conditions probably associated with an acute-phase response; (c) chronic-immune-mediated disorders; (d) valvular heart disease, atrial fibrillation or pacemaker user; (e) use of anti-inflammatory drugs and/or immunosuppressive agents; (f) Individuals with alcohol or drug abuse history.
Isolation of PBMCs and Cell Culture
Cell culture and isolation of PBMCs were done according to the structure that has been described in previous studies.45–47 PHA was used as the positive control in cell culture. Curcumin (Sigma-Aldrich, Cat# C7727, purity ≥94%) was dissolved in DMSO (vehicle) and diluted in RPMI-1640 culture media to final concentrations of 0.1 µM and 1 µM. The DMSO concentration was kept below 0.1% in all cultures. Vehicle control cells received an equal volume of DMSO without curcumin.
Real-Time PCR
The mRNA expression levels of specific genes were quantified by qRT-PCR explained in the previous study. 47 The sequence of Forward and reverse primers for miR-21 were 5′-CCGGCCTAGCTTATCAGACTG-3′, and 5′-AGTGCAGGGTCCGAGGTA-3′, respectively.
ELISA
IL-6 cytokine levels were measured using a commercial Human IL-6 ELISA Kit (R&D Systems, Cat# D6050) in accordance with the manufacturer's protocol. 47
Flow Cytometry
For Treg analysis, the following monoclonal antibodies were used: anti-CD4-FITC (BioLegend, Cat# 317406), anti-CD25-PE (BioLegend, Cat# 302606), and anti-Foxp3-APC (eBioscience, Cat# 17-5773-82). Isotype controls matched to each fluorochrome were used accordingly. 45
Statistics Analysis
For statistical analysis, SPSS 16.0 software was used. ANOVA and the parametric T-test were used to compare mean results. Significant P-values were considered as those less than .05. The confidence interval is considered as 0.80%.
Results
Effect of Curcumin Treatments on Apoptosis of PBMCs
We initially determined the toxicity of curcumin treatments on PBMCs primary culture by MTT assay. Isolated PBMCs were treated with curcumin at different concentrations (0, 0.1, 1, 10, and 100 µM) and at different times (12 h, 24 h, 48 h, 72 h). Curcumin reduced cell viability in a dose-dependent manner. A significant decrease of viable cells was found after treatment of 10 and 100 µM of curcumin (P = .001 and P = .002, respectively, compared to 0 µM), while other doses did not significantly reduce the number of viable cells. Based on these results, 10 and 100 µM of curcumin were toxic to PBMCs, and those concentrations were not used in further experiments. The optimum time for cell culture was 48 h.
The Percentage of Tregs Decreased While the Gene Expression of miR-21 Increased in Patients with MI
Our results showed that the frequency of Tregs decreased in PBMCs from patients with MI compared to the controls (3.71 ± 0.32 vs 1.92 ± 0.37, P = .03, Figure 1A), representing a disturbance in the regulatory immune mechanism in MI. miR-21 gene expression was found to increase in PBMCs from MI patients relative to the controls (314.24 ± 58.70 vs 138.14 ± 25.50; P = .01, Figure 1B). A schematic figure of flow cytometry of Tregs is shown in Figure 2.

The frequency of Tregs decreased in PBMCs from patients with MI compared to the controls from patients with MI, curcumin enhanced the frequency of Tregs compared to the untreated cells (A). miR-21 gene expression was found to be increased in PBMCs from MI patients relative to the controls. Curcumin treatment decreased the miR-21 expression in cell culture in MI patients compared to the untreated cells (B). Serum levels of IL-6 as the pro-inflammatory cytokine were increased in the patients with MI compared to the controls in PBMCs from patients with MI. Curcumin treatment decreased the IL-6 levels in cell culture supernatants compared to the untreated cells in MI patients (C).
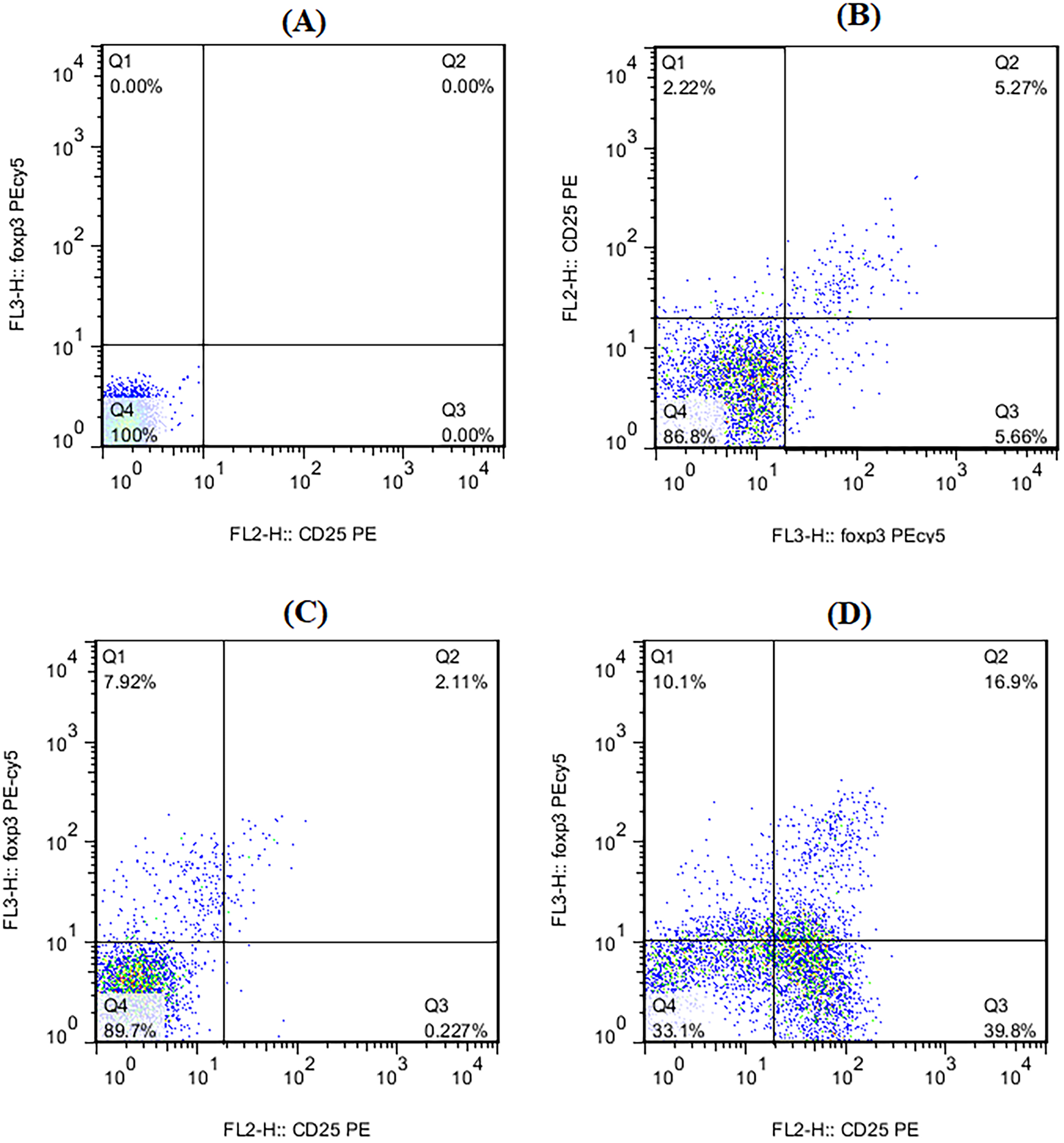
Representative flow cytometric analysis of CD4+ CD25high Fox + Tregs and among isotype control (A), curcumin treated (B), untreated (C), and PHA (10 µM) treated (D), respectively. For Tregs assessment CD4+ CD127− cells were gated and CD25high Foxp3+ cells percentage was analyzed.
The serum Levels of IL-6 Cytokine Increased in MI Patients
It was found that the serum levels of IL-6 as the pro-inflammatory cytokine were enhanced in the patients with MI compared to the controls (285.1 ± 55.02 vs 56.3 ± 14.2; P = .008, Figure 2A).
Curcumin Increased the Frequency of Tregs While Regulating the Expression of miR-21 in Patients with MI
In PBMCs from patients with MI, curcumin enhanced the frequency of Tregs compared to the untreated cells (4.9 ± 0.6732 vs 3.08 ± 0.56, P = .02, Figures 1A and 2) while in the control group, curcumin treatment did not significantly alter the portion of Tregs (P > .05, Figure 1A). Curcumin treatment decreased the miR-21 expression in cell culture in MI patients compared to the untreated cells (139.09 ± 58.7 vs 314.24 ± 18.01, P = .02, Figure 1B).
Curcumin Decreased the Levels of IL-6 in Cell Culture Supernatants in Patients with MI
Curcumin treatment decreased the IL-6 levels in cell culture supernatants compared to the untreated cells (94.05 ± 29.01 vs 305.01 ± 59.03, P = .02, Figure 1C) while in the control group, curcumin treatment did not markedly change the levels of IL-6 in the supernatants of PBMCs culture (P > .05, Figure 1C).
Discussion
MI occurs when blood flow to a part of the heart is inhibited or interrupted, resulting in injury to the cardiac muscle. 48 This research was aimed at evaluating the effects of curcumin on Tregs as the regulator of immune responses and miR-21 and IL-6 in PBMCs from patients experiencing MI and the controls. Curcumin was found to enhance the percentage of Tregs, while it decreased the miR-21 gene expression. Curcumin decreased IL-6 levels as the prominent pro-inflammatory cytokines in PBMCs from patients with MI. In this study, we found that miR-21 was up-regulated after MI which was associated with reducing the frequency of Tregs. The serum levels of IL-6 as the prominent pro-inflammatory cytokine increased in patients with MI compared to the controls.
It was recently proposed that Tregs contribute to cardiac immune tolerance, and the breakdown of immune tolerance to self-antigens in the heart may cause cardiac inflammation. 49 Tregs in the heart have higher proliferative rates than Tregs in blood and lymphoid tissue, suggesting that local renewal is particularly important for Tregs expansion in the heart, even in the absence of cardiac injury. 50
The development of an inflammatory network, which involves inflammatory cell aggregation and the production of inflammatory cytokines such as IL-6, can affect the progression of cardiovascular diseases including MI, atherosclerosis, myocarditis, heart failure, and hypertension. 51 Tregs can suppress the pro-inflammatory cells and the production of IL-6, both of which are associated with cardiovascular complications. 51 Tregs dysfunction may lead to uncontrolled inflammatory responses of Th1 and Th17 cells and, consequently, MI and heart failure. 52 A decreased percentage of circulating Tregs has been associated with a higher risk of heart failure hospitalization, inversely correlated to IL-6 levels. 48 Transfusion of Tregs improved infarct size and left ventricular dilation in a mouse model of MI. 49 Activated M2-like macrophages released anti-inflammatory cytokines such as IL-10, IL-13, and TGF-β that are essential in wound healing, tissue remodeling, and angiogenesis.50,53 Interestingly, Tregs improved M2-like monocyte differentiation post-MI by producing IL-10, TGFβ, and IL-13 in vivo and in vitro. 51 These cytokines promoted collagen deposition by myofibroblasts and accelerated the formation of scar tissue. 54 As a result, cardiac healing after MI was improved. 52 Tregs could also enhance wound healing in COVID-19 patients with MI by influencing macrophage differentiation. 55
miR-21 plays a role in the induction and resolution of inflammatory response and may serve as a biomarker of inflammation a condition in which Tregs play a key role.54–56 miR-21 is known to be specifically expressed in Tregs 57 and controls Tregs fate and function.56,58 It was found that miR-21 can regulate and promote Tregs function. miR-21 has the potential to positively regulate Tregs activity by directly targeting a proposed negative regulator of TGF-β signaling, SMAD7. 59 In contrast, other studies have suggested that miR-21 restrains Treg activity through intrinsic Treg-specific mechanisms and limiting FOXP3 activity 16 or indirectly by promoting the activity of Th17 cells, whose pro-inflammatory nature counters Tregs function. 14 The decrease in TGF-β and FoxP3 expression in PBMCs from patients with atherosclerosis was consistent with an increase in miR-21 expression resulting in increasing expression. Additionally, miR-21 was found to promote cardiac fibrosis via repressing Smad7 in mice models of MI in vivo. 19 These results confirm that the miR-21/Treg axis is active in cardiovascular diseases.
The involvement of miR-21 was shown in cardiovascular diseases such as atherosclerosis. miR-21 is up-regulated in the human peripheral blood of atherosclerosis patients. 59 In addition, miR-21 expression was shown to be increased in PBMCs from patients with a history of MI relative to control patients with chest pain yet no vascular disease. Interestingly, in other intermediate patient groups with progressing from stable to unstable angina and increasing incidence of vascular disease, there is also an increase in PBMCs miR-21 expression, suggesting the induction of miR-21 in the progression of cardiac diseases. 59 miR-21 expression was found to be gradually enhanced in PBMCs from SA to UA to AMI patients, which suggests that miR-21 expression levels are increased as the pathology of AS becomes more severe.
The present study indicated that miR-21 gene expression was increased in PBMCs from patients with MI which was associated with the reduction of the number of Tregs in PBMCs of those patients. This is in parallel with another study that showed over-expression of miR-21 decreased the frequency of circulating Tregs and the expression level of FOXP-3 in PBMCs of patients with coronary heart disease. 60 Therefore, according to the results of our study and the mentioned study, we suggest that miR-21 may act to reduce the percentage of circulating Tregs, in PBMCs from patients with cardiac complications including coronary heart diseases such as MI and consequently may have a pro-inflammatory role in the development of cardiac injuries.
Curcumin, a natural substance that depends on the dose, target cells, and the physiological and pathological context, curcumin may have anti-inflammatory and, antioxidant, anti-parasitic, antispasmodic, and anti-cancer properties. 61 It was shown that curcumin down-regulated the expression of several pro-oncogenic miR-20a, miR-17-5p, miR-21, and miR-27a in human tumor cell lines. 62 Curcumin was found to regulate miR-21 expression and suppress invasion and metastasis of cells in colorectal cancer and breast cancer.44,63–65 It was suggested that curcumin attenuated cardiac fibrosis following MI by regulating collagen deposition, ECM degradation, and CFs’ proliferation and migration. The protective effects of Curcumin were attributed to SIRT1 activation. 66
Curcumin was found to influence various features of the immune system in various diseases with immunological etiology. 40 For the first time, the current study evaluated the effects of low doses of curcumin on Tregs and the expression of miR-21, as well as IL-6 as the most prominent pro-inflammatory cytokine in patients with MI. The idea for designing this research came from the works on the effects of curcumin on the Treg in diseases with inflammatory etiology. As mentioned, Tregs imbalance may have a role in the pathogenesis of MI and autoimmunity. It was shown that curcumin acts as a modulator of the immune responses through the balancing of the Treg/Th17 axis in auto-immune diseases including SLE, MS, osteoarthritis, diabetes, and ulcerative colitis (UC).
Administration of low doses of curcumin (0.1 and 1 µM) could increase percentages of Treg and TGF-β1 productions in CD4+ T cells from patients with SLE. 67 A clinical trial indicated that curcumin relieved pain and modulated Th17/Treg axis in patients with osteoarthritis. Additionally, administration of curcumin (80 mg daily for 3 months) increased Treg/Th17 cells ratio. 68 Another clinical trial demonstrated that after treatment with nano curcumin in osteoarthritis, the frequency of Tregs and expression of miR-146a and FoxP3 gene expression was significantly increased in patients. 69 miR-146a is one of the miRs prevalently expressed in Tregs and is necessary for the suppressive function of Tregs. 70 FOXP3 is the specific transcription factor of Tregs that is related to the function and development of Tregs. 45 Treatment with nano curcumin enhanced levels of IL-10 and TGF-β and lowered IL-6 secretion in osteoarthritis patients. 69 In diabetic mice with UC, curcumin (100 mg/kg/day) significantly improved the symptoms of diabetes complicated by UC, with a lower insulin level, heavier weight, and less inflammatory cell infiltration. Curcumin-treated mice showed attenuated Th17 responses and enhanced Treg function. Curcumin effectively alleviated colitis in mice with type 2 diabetes mellitus by restoring the homeostasis of Th17/Treg and improving the composition of the intestinal microbiota. 71
Conclusion
Our findings showed that the proportion of Tregs as the important regulatory cells that control inflammatory response was decreased while the gene expression of miR-21 was increased in patients with MI. The serum levels of IL-6 as the prominent inflammatory cytokine were increased in those patients. The present study provides new insights into the mechanism of the anti-inflammatory role of curcumin in MI. The findings of this study suggested that miR-21/Tregs may have a role in the pathogenesis of MI. A low dose of curcumin increased the percentage of Tregs in PBMCs culture and decreased the expression of miR-21 and IL-6 in patients with MI ex vivo. Of note, miR-21 was shown to have a role in both vascular disease and Tregs function. In the development and progress of MI, there is a decrease in the frequency of Tregs in circulation which may be driven by miR-21 and leads to enhanced unfavorable inflammation. Identifying the cellular and molecular mechanisms controlling the miR-21/Treg axis will improve our understanding of MI pathogenesis. It is suggested that future clinical studies evaluate the effects of curcumin in the prevention or improvement of MI and identify the probable signaling pathways in the Tregs-miR-21 axis. Therefore, testing curcumin as a supplement therapy or auxiliary therapeutic agent along with classic treatments may improve the therapeutic approach in the treatment or prevention of MI.
Footnotes
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This study was supported by the Nanchong City School Science and Technology Strategic Cooperation Project (22SXQT0015).
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data Availability Statement
The data that support the findings of this study are available from the corresponding author upon reasonable request.
