Abstract
Neurologic disease associated with migration of plant material is reported infrequently in dogs. Here we describe meningoencephalomyelitis associated with foreign plant material in a 2-y-old castrated male West Highland White Terrier dog with acute neck pain. Magnetic resonance imaging revealed spinal meningeal contrast enhancement. Although clinical signs improved after treatment with steroids, the dog was readmitted for further evaluation 3-mo later and was euthanized after generalized epileptic seizures. Autopsy findings consisted of coalescing, pus-filled, neuroparenchymal cavitations surrounded by hemorrhage in the left caudal colliculus and rostral left cerebellar hemisphere. Histologically, lesions consisted of necrosis and suppuration, which surrounded a 1 × 2-mm foreign body morphologically consistent with plant material and clusters of gram-positive bacterial cocci. Affected areas were surrounded by reactive astrocytes, fibrous connective tissue, and mixed inflammatory infiltrates. Areas of hemorrhage and infiltration by neutrophils and foamy macrophages with fibrinoid change of small capillaries were observed in the adjacent neuroparenchyma. The inflammation extended to the perivascular spaces in the leptomeninges (mesencephalon, cerebellum, and brainstem, and spinal cord) and spinal central canal. Anaerobic bacterial culture of frozen samples of cerebellum yielded heavy growth of Bacteroides pyogenes.
Lesions associated with foreign bodies in the brain or spinal cord are documented uncommonly in dogs and are typically associated with migration of plant material (especially grass awns)3,5,8,11,12,16 or traumatic implantation of porcupine quills,4,20,21 wooden sticks, 18 or metallic foreign bodies. 17 Porcupine quills, wooden sticks, and metallic objects typically reach the CNS via direct traumatic implantation of neighboring tissues, such as the oral cavity and oropharynx.17,18 Alternatively, the morphology of porcupine quills and plant material (particularly grass awns) allows for their migration across tissues after penetration at the primary site.8,9
Different plant parts have been associated with lesions in dogs, including grass awns, florets, stems, grains, seeds, and parts of leaves or twigs.6,7 The plant species varies according to the geographic area.6,8 Although the inflammatory response in the affected tissues can be sterile (centered only on the foreign body), plant material can carry bacterial or rarely fungal microorganisms that lead to septic inflammatory reactions that can complicate the clinical outcome. 6 Intralesional plant material can be detected during surgery, 3 autopsy, or histology.5,12,16 When recovered during surgery or autopsy, plant parts can be more easily subjected to morphologic identification and speciation. 5
After tissue implantation, plant material follows the path of least resistance and migrates in a unidirectional movement through tissues, until its lodgment, sequestration, and triggering of an inflammatory response within an organ or body cavity.1,8 Clinical signs vary greatly according to the primary site of implantation and the path of migration of the material but typically include swelling of the skin and deeper soft tissues of the ear canal, head, face, neck, thorax, flank, and interdigital areas, as well as in the conjunctival, oral, and nasal mucosal membranes.1,6,10 In addition, plant material has been associated with a wide range of inflammatory lesions in internal organs, 8 including brain3,5,11,16,22 and spinal cord.2,12,13,23
Occasional reports of neurologic disease associated with plant material migration in dogs have focused mostly on the epidemiology and clinical management of patients,2,3,8,12,13,15,23 with only a few reports of the neuropathology findings.5,11,16,22 Here we describe the clinical signs and neuropathology of a case of meningoencephalomyelitis associated with plant material in a 2-y-old castrated male West Highland White Terrier dog from Arizona that was examined because of acute neck pain. Magnetic resonance imaging revealed spinal meningeal contrast enhancement, and CSF analysis revealed a neutrophilic pleocytosis. The patient was initially diagnosed with steroid-responsive meningitis-arteritis (SRMA). The neck pain improved after treatment with steroids but recurred after 3 mo. The dog was readmitted for further evaluation, at which point SRMA was considered less likely given the patient’s breed. The dog developed generalized epileptic seizures with 2 episodes of status epilepticus and was euthanized because of the progressive nature of the clinical signs.
Autopsy findings were restricted to the brain and consisted of coalescing pus-filled cavitations surrounded by dark red rims of hemorrhage that expanded the left caudal colliculus and rostral portions of the left cerebellar hemisphere (Fig. 1). There was a right midline shift as a result of the extensive necrosis and associated inflammation. Routine tissue samples were collected (including brain and spinal cord), fixed in 10% neutral-buffered formalin, processed routinely for histology, and stained with H&E. Unfixed brain samples (frontal telencephalic lobe, cerebellum, caudal brainstem) were stored frozen.
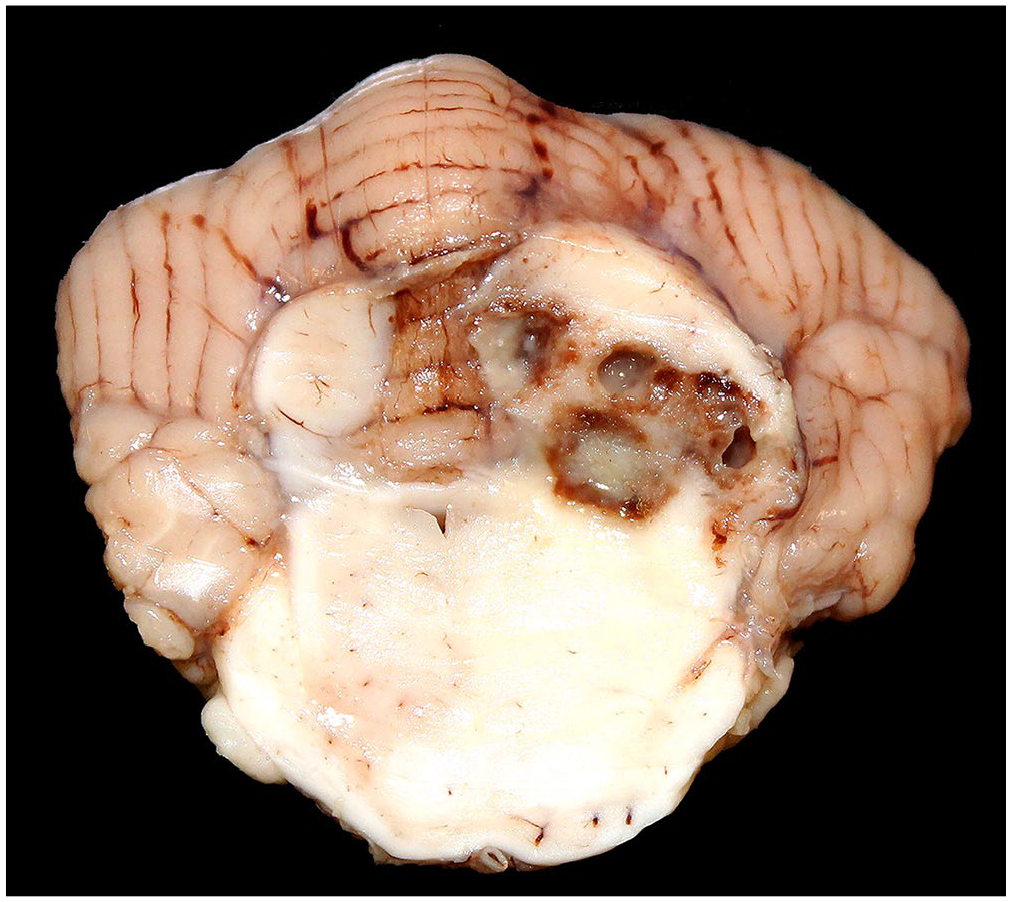
Meningoencephalitis associated with foreign plant material in a dog. Coalescing pus-filled cavitations rimmed by hemorrhage expand the left caudal colliculus and shift the midline to the right.
Histologically, the left caudal colliculus and rostral cerebellar hemisphere were expanded and effaced by coalescing areas of necrosis and suppuration that occasionally surrounded a 1 × 2-mm foreign material morphologically consistent with plant material (Fig. 2). The plant material had an outer multicellular wall containing pointed barbs and was surrounded by clusters of gram-positive bacterial cocci and sheets of neutrophils and foamy macrophages (Figs. 3, 4). Affected areas were surrounded by thick bands of fibrous connective tissue admixed with clusters of neutrophils, foamy and hemosiderin-laden macrophages, lymphocytes, and plasma cells (Fig. 5). Areas of hemorrhage and infiltration by neutrophils and foamy macrophages with fibrinoid change of small capillaries were observed in the adjacent neuroparenchyma (Fig. 6). A moderate number of neutrophils, lymphocytes, and plasma cells also extended to the perivascular spaces of the mesencephalic, cerebellar, brainstem, and cervical, thoracic, and lumbar spinal leptomeninges (Fig. 7). The spinal central canal was partially expanded by neutrophils (Fig. 8). No other lesions were observed. Anaerobic bacterial culture of frozen samples of cerebellum yielded heavy growth of Bacteroides pyogenes. No growth was detected on aerobic bacterial culture.
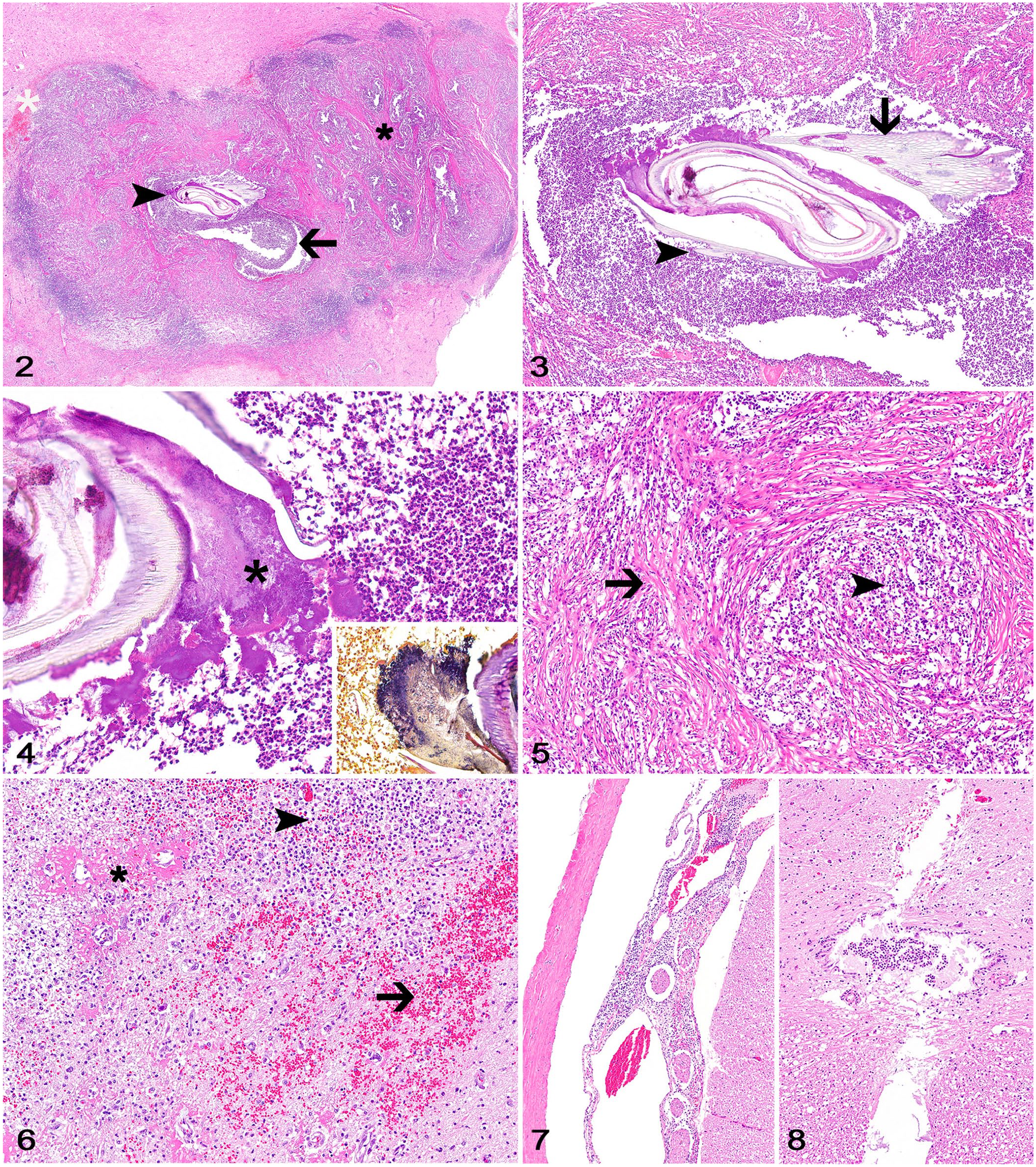
Meningoencephalomyelitis associated with foreign plant material in a dog.
Plant material has been associated infrequently with neurologic disease in dogs.2,3,5,11–13,16,22,23 Plant material typically gain access to the brain after implantation and migration through adjacent tissues, such as the skin, ear canal, conjunctiva, nasal cavity and paranasal sinuses, and oral cavity.2,3,5,16 However, as evidenced by our case, the primary site of cutaneous or mucosal penetration is usually not elucidated at the time of diagnosis.5,16 As expected, clinical signs vary according to the neurolocalization and extent of the lesions in the brain or spinal cord and to whether the lesion is sterile or septic.2,3,5,12,16,23 Neuroimaging can be helpful to determine the inflammatory nature and the neurolocalization of the lesion,3,13,16 and occasionally allows for the identification of the foreign body.13,23 Although surgery and antibiotic therapy can be attempted for localized lesions, particularly those in the spinal cord,3,13,23 the extent of the inflammation in the brain typically leads to progressive clinical signs and death or euthanasia of affected patients.5,16
Reported gross neuropathologic changes in dogs include ventricular dilation with suppurative or mucoid exudate,5,22 telencephalic (frontal or occipital lobe) abscesses,3,5 meningeal hemorrhages, 5 and epidural or intraparenchymal abscesses in the spinal cord.12,13,23 However, as highlighted by our case, these lesions are not specific for plant material migration and, in the absence of clinical suspicion of a foreign body, diagnostic confirmation can only be achieved by the histologic observation of intralesional plant fragments. In our case, no suspicion of a foreign body was raised clinically or during autopsy, and the plant material was identified only on histology, which did not allow for its speciation. Histologically, lesions consist of extensive-to-widespread suppurative, pyogranulomatous, or granulomatous meningoencephalitis with necrosis, lateral ventriculitis, and hemorrhage.5,11,12,16,22 Lymphocytic meningitis in the spinal cord associated with the primary brain lesions was reported on one occasion, similar to the observation in our case. 5
As is the case for extraneural lesions associated with plant material, 6 bacterial organisms can be observed occasionally within lesions in the CNS. 5 Reported cases in which bacterial culture was performed confirmed that CNS lesions were often associated with mixed bacterial infections caused by Staphylococcus spp., Streptococcus spp., Escherichia coli, and Pasteurella multocida, and less often Pseudomonas aeruginosa, Corynebacterium sp., and Micrococcus sp.3,5,13,23 In our case, the gram-positive bacteria observed histologically and the gram-negative B. pyogenes identified by anaerobic bacterial culture confirmed a mixed bacterial infection as a contributing factor for the development of the lesions. It is possible that the gram-positive cocci were Staphylococcus sp. or Streptococcus sp. but that supposition could not be confirmed by bacterial culture. 5 B. pyogenes is a component of the normal oral flora of dogs and cats, 14 and although its pathogenicity is poorly understood, organisms have been isolated from dog and cat bite wounds in humans, 14 meningoencephalitis in dogs, 19 and thoracic and abdominal wall lesions caused by plant material in dogs. 6
Footnotes
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
