Abstract
A 6-week-old, female, mixed-breed dog with a clinical history of sudden onset of neurologic signs was presented for necropsy. The dog was diagnosed with suppurative and histiocytic meningoencephalitis based on necropsy findings and histopathology. Mycoplasma sp. was isolated in pure culture from the brain and meninges and was identified as Mycoplasma edwardii using DNA sequencing.
Keywords
A 6-week-old, female, mixed-breed dog was presented to the Tifton Veterinary Diagnostic and Investigational Laboratory (University of Georgia, Tifton, Georgia) for necropsy. The dog had a clinical history of sudden onset of neurologic signs characterized mainly by seizures. Euthanasia was elected, and the dog was submitted for postmortem examination. A complete necropsy was performed. At necropsy, the dog was in good nutritional condition. Patchy areas of congestion were present bilaterally in the pulmonary parenchyma. On the right side of the head, approximately 1.5 cm above the right eye, there was a focal, 2-cm-diameter, subcutaneous, red (congested) area that did not communicate with the skin surface. On cut section, the dermis was slightly thickened, and the subcutis had a brown to dark red discoloration. On the same location, the skull was slightly depressed along the suture line between the right frontal and right parietal bones, but evidence of fracture was not observed. At this location, on the periosteum adjacent to the dura mater, there was a 0.4 cm × 0.3 cm bony proliferation (osteophyte). A mild to moderate amount of thick yellow to green exudate (interpreted as pus) was observed on the surface of the leptomeninges of the entire brain, especially at the base (Fig. 1A) and within the ventricular system. The right side of the cerebrum, involving part of the frontal and parietal lobes, had locally extensive brown discoloration and softening (interpreted as malacia), and a similar exudate was observed within the cerebral parenchyma communicating with the ventricular system. The leptomeninges of the cerebellum were congested. No other significant gross findings were observed.
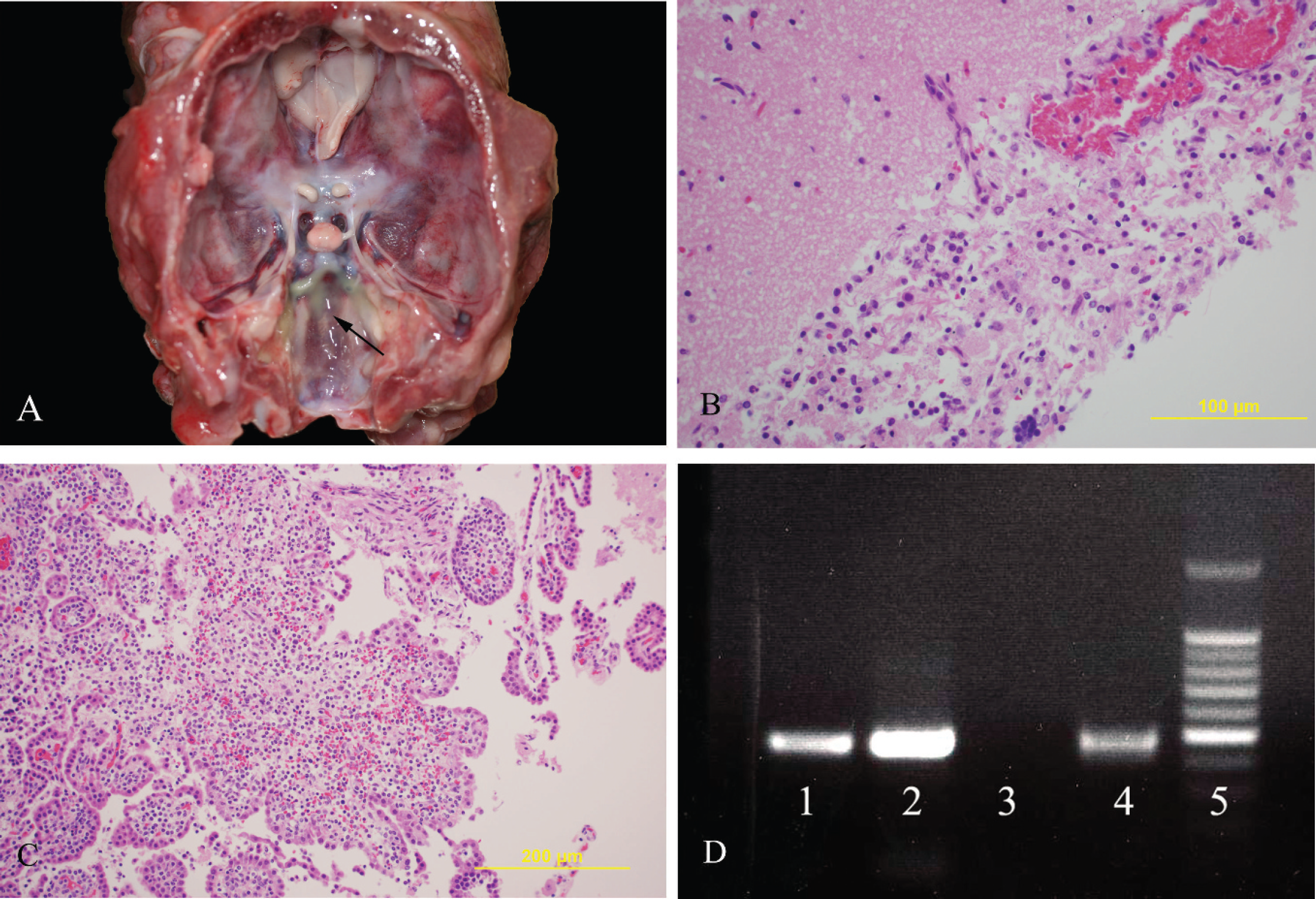
Meningoencephalitis caused by Mycoplasma edwardii in a dog.
Tissues for histopathology and bacterial culture were collected at necropsy. For histopathology, tissues were fixed in 10% neutral buffered formalin, embedded in paraffin, sectioned at 5-μm thickness, stained with hematoxylin and eosin, and examined by light microscopy. Routine aerobic and anaerobic cultures were performed on fresh samples of lung, spleen, kidney, liver, brain, and swabs from meninges and brain according to the standard operating procedures in bacteriology.
The main histopathological lesions were suppurative and histiocytic leptomeningitis (Fig. 1B), ventriculitis, and plexus choroiditis (Fig. 1C) characterized by multifocal areas within leptomeninges and choroid plexus infiltrated by few to large numbers of macrophages, neutrophils, and lymphocytes. In markedly affected areas, the inflammation extended to the gray matter of the brain parenchyma and was characterized by perivascular cuffing of moderate numbers of macrophages, lymphocytes, and rare neutrophils within the neuropil. Mild multifocal lymphohistiocytic bronchointerstitial pneumonia with intra-alveolar squamous cells and basophilic globular material was present in both lungs and was interpreted as aspiration pneumonia that was likely secondary to the seizures. The subcutaneous lesion of the head was consistent with subacute necrotizing suppurative dermatitis and panniculitis characterized by small, multifocal to coalescing fistulous tracts filled with fibrin and cellular debris. This was surrounded by moderate amounts of fibrovascular reactive tissue containing large numbers of neutrophils and lesser numbers of histiocytes surrounded by fibrosis at the periphery.
Routine aerobic culture of the brain tissue yielded heavy growth of fine alpha hemolytic colonies after 48 hr of incubation. The colonies did not stain by Gram staining. Polymerase chain reaction using genus-specific Mycoplasma primers yielded positive result with the colonies and brain tissue (Fig. 1D). A portion of 16S ribosomal DNA of the isolate was amplified and sequenced. The sequence was used to search GenBank using BLASTn nucleotide search (http://www.ncbi.nlm.nih.gov/blast/Blast.cgi). The sequence obtained from the isolate had 99% identity with Mycoplasma edwardii.
The gross and histological lesions were consistent with suppurative and histiocytic meningoencephalitis, ventriculitis, and plexus choroiditis, and M. edwardii was isolated from the brain. Mycoplasmas in dogs are described mainly as respiratory pathogens and are thought to be part of the normal bacterial flora of the upper respiratory tract. 3 The most important pathogenic Mycoplasma spp. in dogs are usually associated with anemia (Mycoplasma haemocanis), 3 respiratory disease (Mycoplasma cynos), 3,4,6,9,15 and urogenital tract infections (Mycoplasma canis). 3,14 Mycoplasma cynos has been implicated in cases of canine infectious respiratory disease or kennel cough, but rarely as a primary infectious agent. 15 More often, it is a secondary infectious agent associated with other bacterial and viral respiratory pathogens. 3,6,9,11
Mycoplasma edwardii is considered a mycoplasma species of dogs since it has been mainly isolated from canine tissues. It was initially described as strain PG-24 (prototype species) and was later reclassified as M. edwardii. 1,13 The original isolation site of M. edwardii in dogs was the oral cavity. Since then, M. edwardii has been isolated from the lungs, trachea, oropharynx, tonsil, cervix, prostate, prepuce, vagina, nasal cavity, and lymph node of dogs. 3,5,13 In one study, 4 M. edwardii was isolated from lungs and tonsils of 19% and 42% of the healthy dogs, respectively, and from only 10% of the dogs with canine infectious respiratory disease. Although considered a Mycoplasma species of dogs, M. edwardii has also been isolated from the oral and nasal cavities and rectum of wild healthy raccoons in Japan. 8 Mycoplasma edwardii has been associated with pneumonia in early reports 3,13 and was recently isolated from a dog with acute polyarthritis and septicemia, which developed following a surgical procedure. 12
In human beings, Mycoplasma spp. have been associated with development of brain abscesses and meningitis in neonates. 2,5,7,10 These conditions, however, are distinctly rare. Mycoplasma hominis has been implicated in the majority of the cases. 7,10 Predisposing factors in human beings include medical procedures involving the central nervous system, such as cerebrospinal fluid drainage and intracranial surgeries. 5,10 Meningitis in neonates has been associated with infection through the colonized birth canal or fetal infection in utero. Although colonization with Mycoplasma spp. is common in neonates, invasive disease is rare. 7 It is thought that infection of the nervous tissue by Mycoplasma spp. could happen following nervous tissue damage, resulting in areas of malacia and secondary Mycoplasma colonization via the bloodstream or direct inoculation of the nervous tissue secondary to trauma or surgical procedures. 2,10 Interestingly, the dog in the present study had a subcutaneous inflammatory lesion that extended to the skull at the level of the suture line between the right parietal and frontal bones. A skin wound communicating with the subcutaneous lesion was not seen at this site. Although a penetrating wound was not observed on the epidermis, it is possible that a penetrating traumatic lesion to the frontal right region of the head had occurred and that the epidermal lesion had healed by the time the necropsy was performed. Although only speculative, there is the possibility that a penetrating wound reaching the skull was the initial site of inoculation of M. edwardii in this dog.
In the last decade, reports of Mycoplasma sp. infection in dogs have increased, and the role of this pathogen as a primary or secondary infectious agent in dogs has been studied. 3,4,9,11 To the authors' knowledge, the current study is the first case reported in the veterinary literature in which M. edwardii caused meningitis in a dog. This finding should urge veterinary clinicians and pathologists to consider Mycoplasma spp. as potential pathogens that cause primary or secondary infections in dogs and should encourage them to request appropriate diagnostic tests to rule out Mycoplasma infection.
Acknowledgements
The authors would like to thank the staff from the Histopathology and Bacteriology sections of the Tifton Veterinary Diagnostic and Investigational Laboratory for assistance in tissue processing.
