Abstract
Cytopathologists lack reliable criteria to distinguish neoplastic from reactive spindle cells; however, with computer-based nuclear morphometry, it is now possible to more objectively and precisely quantify differences between selected populations of cells. Forty-four cutaneous soft tissue sarcomas and 5 cases of reactive spindle cell proliferations in the dog were morphometrically analyzed with regard to median and standard deviation (SD) of nuclear area, diameter (max, min, mean), radius (max, min), perimeter, and roundness. Overall, nuclei from reactive spindle cells were larger, with greater variation in nuclear size and shape. Significant differences (P < 0.05) were found for several nuclear parameters, including the median and SD of maximum diameter and radius, as well as the SD of roundness. No significant differences were found in nuclear parameters between soft tissue sarcomas divided by histologic grade, mitotic index, or tumor necrosis score. Analysis of the sources of variation indicated near-perfect intraobserver and substantial interobserver agreement. The largest source of variation was due to selection of different measurement fields, reflecting the inherent biological variation in nuclear size within the tumor cell population. The results indicate that nuclear morphometry on cytologic preparations is a reproducible method that may be able to differentiate cutaneous soft tissue sarcomas from reactive mesenchymal lesions in the dog. Further studies, including a larger number of cases, are warranted to assess repeatability of results.
Introduction
Soft tissue sarcoma (STS) encompasses a heterogeneous group of mesenchymal neoplasms derived from soft connective tissues. Although STS can arise in any location, the neoplasms are most commonly found in the cutaneous and subcutaneous tissues and account for 8–15% of skin neoplasms in the dog. 5 Middle-aged to older, medium- to large-breed dogs are overrepresented.6,14 Despite its various histogenesis, cutaneous STS tends to have a similar histological appearance and biological behavior.5,7,9 As such, a grading scheme has been developed for this group of tumors incorporating the level of tissue differentiation, mitotic index, and amount of tumor necrosis. 9 Histologic grade is considered one of the most important prognostic factors, especially in terms of predicting recurrence and for indicating metastatic risk.5,9,14
Prior to biopsy or surgical excision, many cutaneous masses are first evaluated cytologically to establish a diagnosis and to help direct further diagnostic investigation or therapeutic intervention. 15 Soft tissue sarcomas tend to be poorly exfoliative, but fine-needle aspiration may reveal a population of spindle cells with variable degrees of anisocytosis and anisokaryosis. Unfortunately, this appearance is not pathognomonic, as aspiration of many inflammatory lesions, such as granulation tissue, may result in a similar-appearing population of cells.6,7 The lack of reliable criteria to distinguish neoplastic from reactive or dysplastic spindle cells often forces clinicians to submit tissue sections for histopathology to attain a diagnosis. However, with the advent and widespread use of computer-based methods of quantitative cytological analysis, such as nuclear morphometry, it is now possible to more objectively investigate the differences between selected populations of cells.4,11–13,16–20
The objective of the current study was to determine, on cytologic preparations, whether neoplastic and reactive spindle cell populations can be distinguished using nuclear morphometry and whether cells from soft tissue sarcomas of different histologic grades have different nuclear morphometric patterns. Reproducibility of nuclear morphometry was also investigated by determining the sources of variation, including intraobserver, interobserver, and field selection.
Materials and methods
Cases
The database at Prairie Diagnostic Services Inc. (PDS) in Saskatoon, Canada, was searched to identify dogs diagnosed with cutaneous STS from 2000 to 2010 that had both histologic and cytologic slides available to review. Tumors included in the STS category included peripheral nerve sheath tumors (non–brachial plexus), fibrosarcomas (not including oral fibrosarcomas), myxosarcomas, liposarcomas, perivascular wall tumors such as hemangiopericytomas, pleomorphic sarcomas, mesenchymomas, and undifferentiated sarcomas. 5 A further search was conducted to identify dogs with histologically confirmed cutaneous reactive tumor–like lesions that had corresponding cytologic preparations consistent with a spindle cell proliferation. Cytologic slides stained with modified Wright stain a were reviewed prior to randomization by 1 observer (Meachem) to ensure an appropriate level of cellularity and staining for evaluation. Corresponding histological slides were then collected, randomized, and reviewed by 3 blinded observers (Meachem, Burgess, Davies) to confirm the diagnosis and provide histologic grade in cases of STS. Cases with inadequate histologic tissue sections (e.g., insufficient material to establish a mitotic index) were excluded from the study. Using these criteria, 44 cases of STS were identified, including 1 anaplastic sarcoma, 2 liposarcomas, 2 fibrosarcomas, 10 hemangiopericytomas, and 29 cases identified only as STS. Five cases of reactive lesions were identified, including a single case each of superficial dermal fibrosis, granulomatous panniculitis, and focal pannicular fibrosis, as well as 2 cases consistent with granulation tissue. Cytological slides were then randomized and relabeled prior to nuclear morphometric analysis to blind observers to patient identity and previous diagnosis.
Histological grade
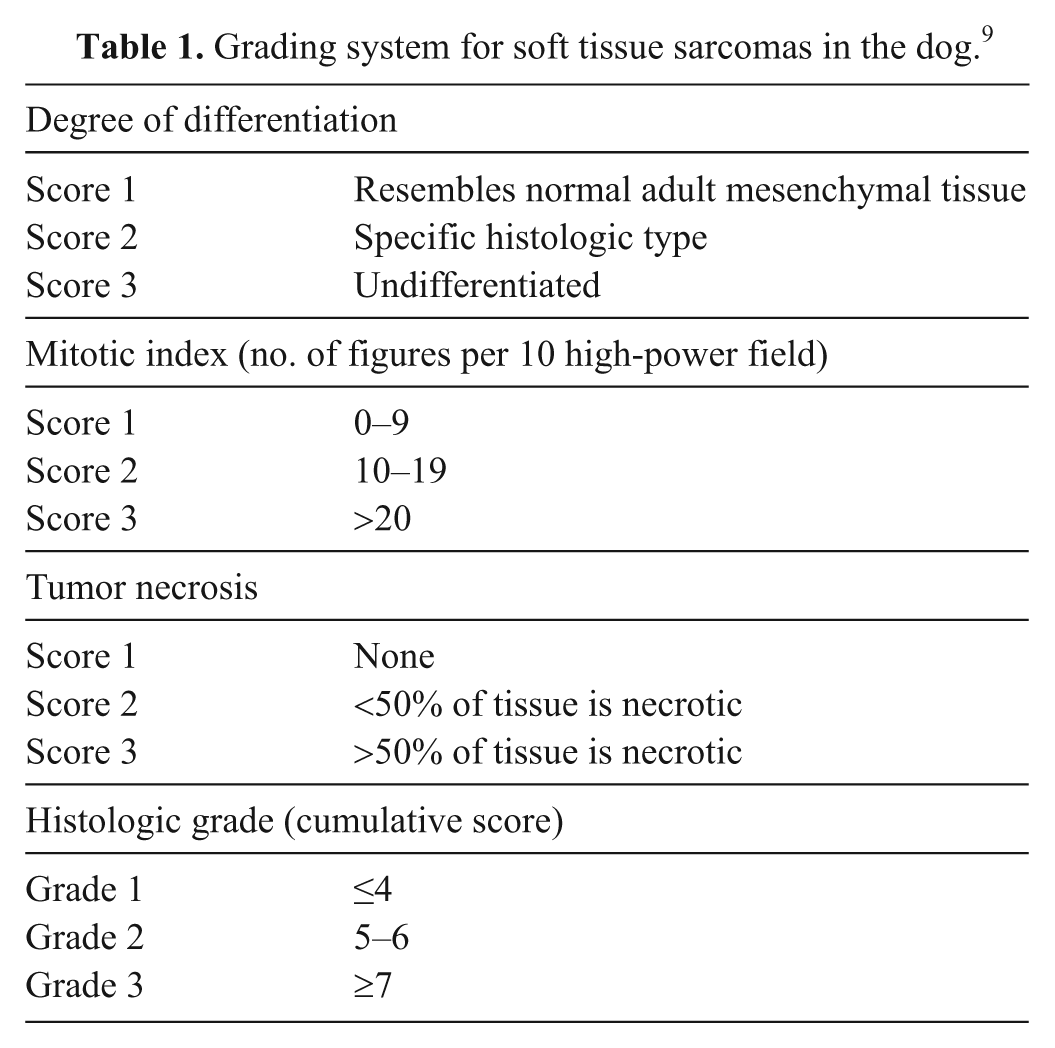
Histological grading was performed as the “gold standard” against which subsequent nuclear morphometric data from cytological slides could be compared. As previously mentioned, randomized histologic slides for each of the 44 STS were reexamined by 3 observers blinded to patient identity, previously reported tumor grade, tumor size and site, and patient history. Observers then independently graded each neoplasm, in the order provided in the slide boxes, using a previously established classification scheme (Table 1) widely accepted for use in veterinary medicine. 9 For the purposes of statistical analysis, the final grade of each tumor was assigned based on agreement between at least 2 observers.
Grading system for soft tissue sarcomas in the dog. 9
Cytological nuclear morphometry
As previously mentioned, a single blinded observer captured images from cytologic slides of all 49 cases via a trinocular microscope b linked to a digital camera system and a computer equipped for image analysis. Imaged fields were selected by chance, and the fields encompassed all cellular areas of the slide or slides available. However, poorly preserved areas, markedly hemodilute areas, or any area in which the cells were constricted or not intact were avoided. A 100 oil immersion lens was used to capture 15–50 images depending on the degree of cellularity, and the images were saved as an image set.
Images for each case were then opened using specialized imaging software c and calibrated. For each tumor, at least 100 consecutive (i.e., the first 100 nuclei that observers came across that fulfilled the criteria) nuclei from intact spindle cells that were not superimposed and had sharp nuclear limits were traced with the help of a computer mouse (Fig. 1). All tracings were conducted by a single observer (Meachem) to minimize interobserver variance. The imaging software then calculated 8 nuclear parameters for each cell: nuclear area, diameter (max, mean, min), perimeter, radius (max, min), and roundness. Roundness was interpreted such that a value of 1 was consistent with a perfect circle, whereas values greater than 1 indicated a more oblong or noncircular shape. The morphometric data collected from all 49 cytological slides was subsequently stratified into groups based on the diagnosis (STS vs. nonneoplastic lesion) and further divided by histological grade in cases of STS.
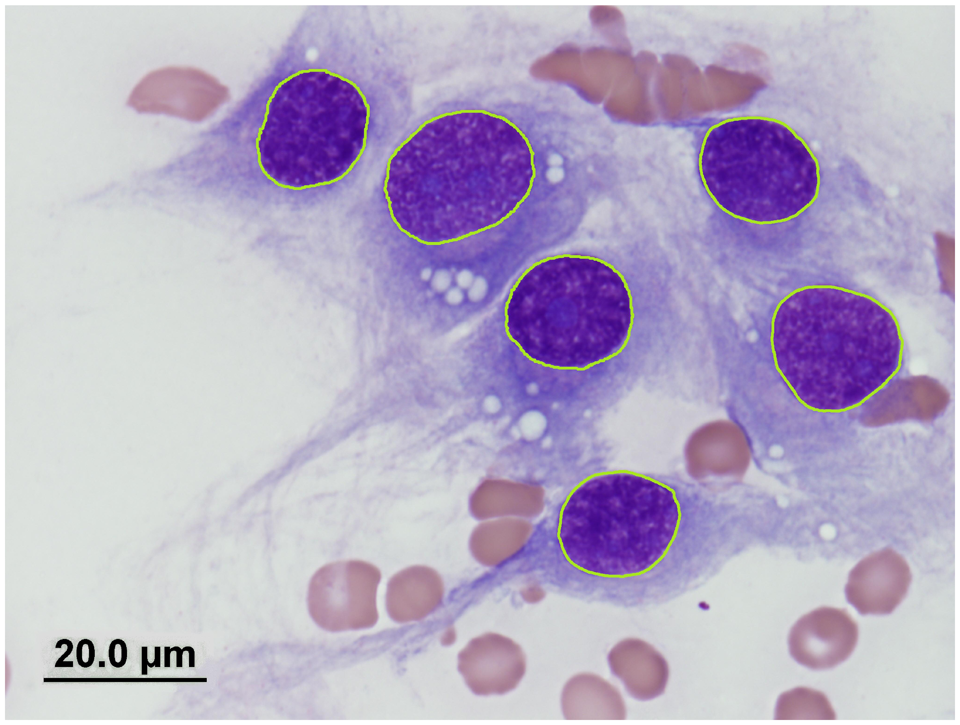
Nuclei from a canine cutaneous soft tissue sarcoma digitally outlined using a computer mouse. Cytological preparation; modified Wright stain. Original magnification 100×. Bar = 20 µm.
Analysis of sources of variation of cytological nuclear morphometry
Three potential sources of variation were identified that may influence the collection of cytological nuclear morphometric data: intraobserver, interobserver, and variation due to selecting different measurement areas, referred to as interfield.1,8 First, intraobserver variation was investigated by having a single observer (Meachem) measure the same 10 cytological cases twice, using the same image set. Second, to evaluate interobserver variation, 3 observers (Meachem, Burgess, Kidney) measured the same 10 cytological cases once, all using the same image set. Finally, interfield variation was estimated by having a single observer (Meachem) measure the same 10 cytological cases twice, using 2 different image sets, each independently collected by 2 different observers (Meachem, Kidney).
Statistical analysis
Cohen kappa (κ) 2 was used to compare agreement between observers for overall histologic grade and each subcategory within the current grading scheme. Complete agreement was considered to have occurred when all 3 observers assigned the same grade to a case. Cytologic nuclear morphometric data from each case were found to be Gaussian, and therefore means and standard deviations (SDs) were calculated. However, comparison of these values between multiple cases revealed non-Gaussian distributions, and thus nonparametric tests were performed for all subsequent statistical analyses, and median values, rather than means, were reported. As such, a Kruskal–Wallace analysis of variance followed by a Dunn multiple comparison post hoc test was used to compare the median value and median standard deviation of the 8 cytological nuclear parameters between nonneoplastic lesions and STS separated into groups by histologic grade, mitotic index score, and tumor necrosis score. A Mann–Whitney test was further used to compare median values and median SDs of the cytological nuclear parameters between nonneoplastic lesions and all STS combined as a single group. Sources of variation were analyzed using Lin’s 10 concordance correlation coefficient (CCC) to assess intraobserver, interobserver, and interfield agreement. Values of CCC ≥0.99, ≥0.95 to < 0.99, ≥0.90 to < 0.95, and <0.90 indicated almost perfect, substantial, moderate, and poor agreement, respectively. 21 Statistical analyses were performed using Prism software, d and statistical significance was set at P < 0.05.
Results
Using the final grade, 30 of the 44 cases of STS were grade 1 (68.2%), 13 were grade 2 (29.5%), and 1 was grade 3 (2.3%). Moderate agreement (κ = 0.50) was found between observers for histologic grade, whereas agreement was slight (κ = 0.12) for degree of tissue differentiation, moderate (κ = 0.54) for mitotic index score, and substantial (κ = 0.62) for tumor necrosis score. Complete agreement occurred in 45.5% of cases (Table 2) and was higher for grade 1 cases (60.0%) compared with grade 2 cases (15.4%). At least 2 observers agreed on histologic grade in every case, and no cases had both a grade of 1 and 3 assigned together.
Complete agreement between 3 blinded observers for histologic grade for 44 cutaneous soft tissue sarcoma cases in the dog.

Analysis of nuclear morphometric data showed that the medians of the 8 nuclear parameters were greater in the nonneoplastic cases compared with STS combined as a single group; however, differences were statistically significant only for maximum diameter, maximum radius, and perimeter (Table 3). The SD of the nuclear parameters displayed similar results, with differences in maximum diameter, maximum and minimum radius, and roundness being statistically significant (Table 3). However, there were no significant differences between the median and SD of any nuclear parameter when comparing STS grouped into histologic grades, mitotic index score, and tumor necrosis score. In addition, no significant differences were found when each histologic grade of STS was compared separately with the group of nonneoplastic cases.
Comparison of cytologic nuclear morphometric parameters in 44 cutaneous soft tissue sarcoma cases and 5 cases of reactive spindle cell proliferations (reactive) in the dog.*
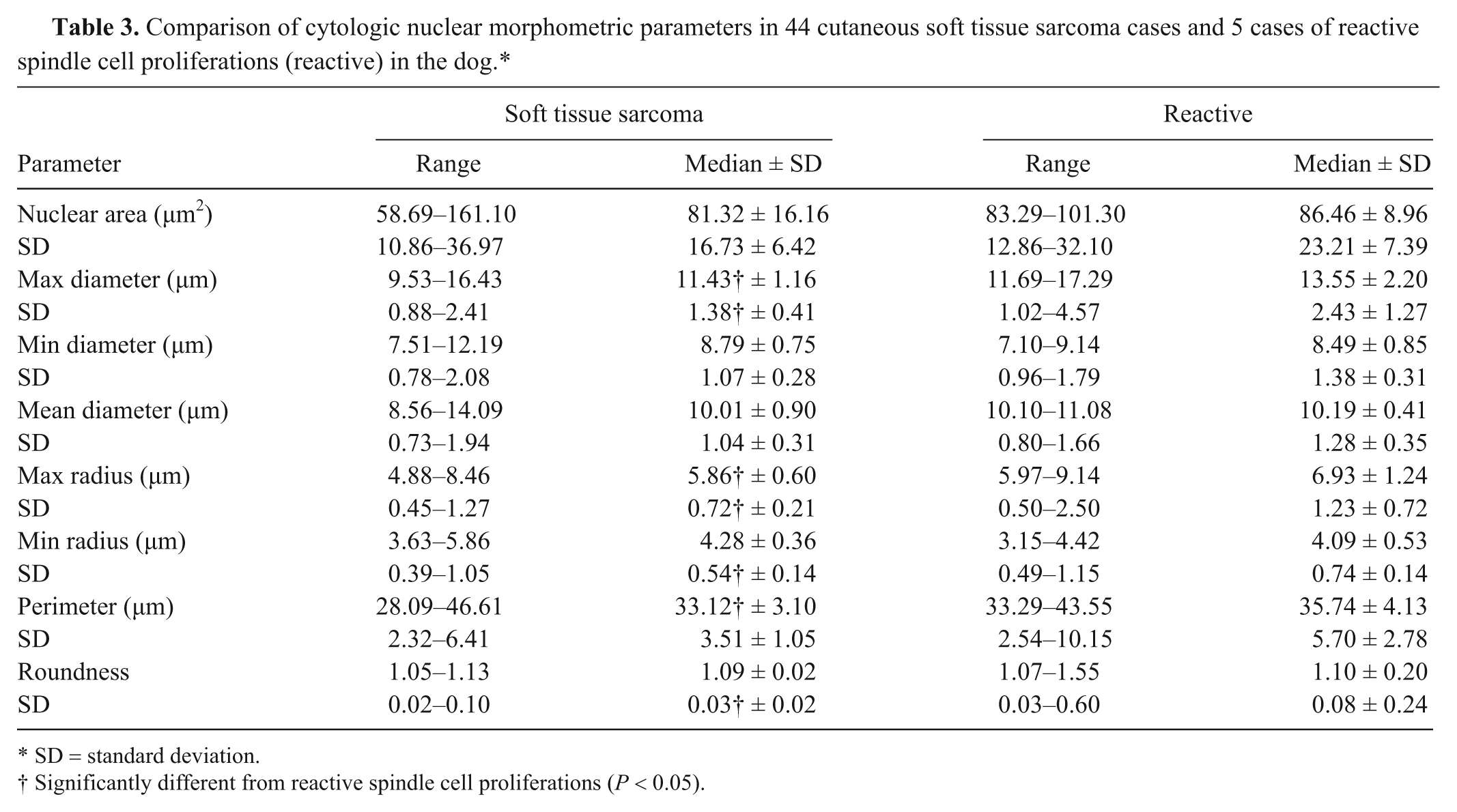
SD = standard deviation.
Significantly different from reactive spindle cell proliferations (P < 0.05).
Correlation between repeated measurements of 1 observer using the same image set (intraobserver agreement, CCC = 0.9963) was found to be higher than when 2 image sets were used (interfield agreement, CCC = 0.9281). Correlation varied between pairs of observers (interobserver agreement; CCC = 0.9934, 0.9716, 0.9879; mean CCC = 0.9843). Correlation was found to be statistically significant in all cases (P < 0.0001).
Discussion
One purpose of the current study was to identify reliable cytologic criteria able to differentiate neoplastic from nonneoplastic spindle cell proliferations. To more objectively quantify such differences, computer-based nuclear morphometry was employed to calculate 8 nuclear parameters for 44 cutaneous STS cases and 5 cases of reactive mesenchymal lesions. In general, nuclei from nonneoplastic spindle cells were larger, with significantly greater maximum diameters, radii, and perimeters. Variation in nuclear size was also found to be greater in nonneoplastic cases, supported by significantly larger SDs in several nuclear parameters (maximum diameter, maximum and minimum radius). As a measure of variance, the SD in nuclear dimensions reflects the degree of anisokaryosis present within the population. The mean roundness value did not differ significantly between STS and nonneoplastic lesions; however, the SD was significantly larger in the latter. This suggests that greater variation in nuclear shape was also present in reactive spindle cell populations.
Although statistically significant, these differences in nuclear parameters are still very small in scale (µm) and thus are likely not visually perceptible. As such, precise quantitative measurement techniques, such as nuclear morphometry, will likely continue to play an important role in future attempts to reliably diagnose STS on cytologic preparations. Further studies that include a greater number of cases, especially of reactive spindle cell proliferations, are needed to ensure that these differences are indeed representative and applicable to spindle cell proliferations in general. Increasing the number of cases may also highlight other significant differences in nuclear parameters that were potentially obscured by small sample size. The low number of nonneoplastic lesions included in the present study stems from difficulties in collecting cases with sufficient histologic and cytologic material available to review. For instance, if cytologic evaluation indicates that a lesion contains spindle cells of questionable malignancy, clinicians may delay biopsy to allow potential inflammatory lesions to resolve; thus, histologic slides would not be available in these cases. Furthermore, many tumors and tumor-like lesions may be surgically excised without prior aspiration for various clinical or client-related reasons.
The present study failed to find any significant differences in cytologic nuclear parameters between histologic grade 1 and grade 2 STS, as well as sarcomas separated by mitotic index or necrosis score. Failure to find such differences may relate directly to the low sample size; however, the results reinforce the need for wide surgical excision of all STS regardless of the degree of malignancy suspected.6,7 Furthermore, a previous report found a significant difference in recurrence risk between grade 1 and grade 2 tumors only with marginal excision, whereas no difference associated with grade was found when tumors were completely removed. 14 The low number of grade 3 tumors in the current study is consistent with previous reports involving mainly primary excisions of STS.5,14 Unfortunately, there were too few grade 3 tumors to draw conclusions with regard to differences in nuclear parameters. Additional studies that evaluate survival time in relation to nuclear morphometry of cytologic and histologic preparations of canine STS may be useful.
Acceptance of a new diagnostic technique in clinical practice requires an understanding of the sources of variation, which may influence the results and conclusions. 8 With the aim of investigating intraobserver and interobserver variation, as well as variation due to field selection (interfield), 3 separate trials were conducted. First, intraobserver agreement was found to be near perfect with repeated measurements by 1 observer, indicating that a single observer is very consistent in tracing nuclei. Second, interobserver agreement between 3 observers was found to be substantial, although slightly larger variation was present when compared with the first trial. This variation may be due to different observer experience levels, innate coordination, and/or differences in computer hardware (e.g., computer mouse) that are employed for nuclear tracings. As such, a standardized measurement protocol, as was used in the current case, is needed to minimize variance due to interobserver differences. Nonetheless, the greatest amount of variation was found in the third trial using different image sets; interfield agreement was moderate. Consequently, field selection has the potential to significantly affect morphometric results, as cells within the tumor, and thus within any 1 field of the cytologic sample, may vary in size and shape. Similar results have been found in a prior study 8 investigating the morphometric variance of human mammary carcinoma. In future investigations, it will be important to account for this biological variation, such as ensuring that cells are measured from all areas of the slide or slides available. Clinicians should also be encouraged to sample multiple areas of the tumor or lesion in question, especially if large, to make certain that aspirates are representative. For example, a standardized protocol may entail aspiration of every 1 cm2 of the tumor, such that both the central and peripheral areas are sampled.
As part of the current study, all cutaneous STS were regraded independently by 3 blinded observers using a well-established histologic grading scheme (Table 1). Complete agreement was found to be relatively low (45.5%), with greater agreement for grade 1 cases (60.0%) compared with grade 2 cases (15.4%). The greatest amount of disagreement was found in the subcategory of tissue differentiation, which has been criticized for being overly subjective. 5 The results suggest that modifications to the current grading scheme, such as excluding the tissue differentiation category, may be warranted to improve reproducibility. In the human literature, agreement between pathologists using a similar grading scheme was found to be higher, with 75% agreement for grade; agreement was still lowest (61%) for differentiation of the 3 subcategories analyzed. 3
In summary, computerized nuclear morphometry may be a useful technique to reliably distinguish neoplastic from inflammatory spindle cell proliferations on cytological aspirates in the dog. Further studies to assess repeatability of measurement results are warranted, and larger numbers of cases are needed. Overall, nuclear morphometry was found to be simple, easy to apply, and reproducible.
Footnotes
a.
Hematek® Modified Wright’s Stain, Siemens Healthcare Diagnostics Inc., Tarrytown, NY.
b.
Olympus® BX 51, Olympus Corp., Melville, NY.
c.
Image-Pro Plus® version 7.0 for Windows®, Media Cybernetics Inc., Bethesda, MD.
d.
GraphPad Prism® version 5.00 for Windows®, GraphPad Software, San Diego, CA.
The author(s) declared that they had no conflicts of interest with respect to their authorship or the publication of this article.
The author(s) declared that they received no financial support for their research and/or authorship of this article.
