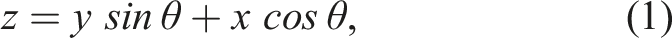Abstract
Background
Femoral neck shortening following internal fixation of unstable femoral neck fractures can compromise functional recovery, particularly in young, active patients. This study aimed to evaluate the efficacy of a length-stable dynamic hip screw (LSD) construct in minimizing postoperative shortening compared to the femoral neck system (FNS).
Methods
A retrospective review was conducted on 65 patients with high-grade unstable femoral neck fractures treated between February 2016 and February 2023 at a single institution. Patients underwent either FNS (n = 31) or LSD (n = 34) fixation. Femoral neck shortening was quantified using vector-based analysis derived from contralateral femoral comparison at final follow-up. Functional outcomes were assessed using the Hip Disability and Osteoarthritis Outcome Score (HOOS).
Results
The LSD group demonstrated significantly less femoral neck shortening compared to the FNS group (5.0 ± 4.6 mm vs 10.4 ± 6.7 mm, p = 0.001). Final HOOS scores were significantly higher in the LSD group in the symptom (88.1 vs 75.8, p = 0.049) and stiffness subdomains. Union was achieved in 31 of 34 patients (91.2%) in the LSD group and 26 of 31 (83.9%) in the FNS group (p = 0.605). Other complications were more frequent in the FNS group but did not reach statistical significance.
Conclusion
Length-stable fixation using the LSD construct significantly reduced postoperative femoral neck shortening in high-grade unstable fractures, without compromising union rates or functional recovery. Our results support the role of length-stable constructs as a reliable option for maintaining anatomic integrity in unstable femoral neck fractures.
Keywords
Introduction
Unstable femoral neck fractures, particularly Garden type III/IV and Pauwels type III, present significant challenges due to displacement, which compromises structural integrity and vascularity—factors that elevate the risk of nonunion, femoral neck shortening, and avascular necrosis.1,2 Unlike stable fractures, these patterns lack inherent mechanical stability and are more susceptible to external forces, making maintenance of postoperative reduction difficult.3,4 Common complications such as femoral neck shortening and varus collapse can result in leg length discrepancy, impaired abductor function, and persistent pain, ultimately reducing mobility and quality of life.5–7 Selecting a fixation method that achieves both compression and resistance to shortening is essential for fracture healing and functional recovery.
Standard treatments include the use of cannulated screws (CSs), dynamic hip screws (DHS; DePuy Synthes, Oberdorf, Switzerland), and hybrid constructs. 8 While CSs offer a minimally invasive option, they lack angular and rotational stability, rendering them less suitable for unstable fracture configurations.9,10 In contrast, the DHS functions as a fixed-angle device and provides superior varus and rotational stability compared to CSs. However, when used as a solitary implant in unstable femoral neck fractures, DHS may still allow excessive sliding under shear forces, which can result in excessive femoral neck shortening and varus collapse.10–12
To overcome these limitations, augmentation techniques such as the addition of anti-rotation screws13,14 and the development of length-stable dynamic hip screw (LSD) constructs—combining DHS with fully threaded CSs—have been introduced. These configurations have demonstrated greater axial stiffness and failure load than conventional DHS in biomechanical studies.15–17 Another recent innovation, the femoral neck system (FNS; DePuy Synthes, Oberdorf, Switzerland), integrates compression and anti-rotation in a single implant,10,18,19 allowing controlled sliding of up to 20 mm. Although it offers comparable resistance to varus and rotational forces as DHS,10,20,21 its overall construct stiffness is lower than DHS augmented with additional screws. 17 Moreover, concerns remain regarding excessive femoral neck shortening in unstable fractures due to its allowance of unresisted collapse at the fracture site.22–26
This biomechanical trade-off between dynamic compression that promotes healing but risks shortening and rigid fixation that preserves neck length but may hinder union poses a clinical dilemma in treating unstable femoral neck fractures. Given these limitations, we hypothesized that the LSD construct—designed to maintain anatomical femoral neck length by resisting excessive postoperative sliding—would offer biomechanical and clinical advantages by enhancing union and preserving alignment. To investigate this, we compared radiologic and functional outcomes of patients with Garden type III and IV femoral neck fractures treated with either FNS or LSD constructs, with emphasis on femoral neck shortening, fracture union, and alignment preservation.
Materials and methods
Study design, population, and basic parameters
A retrospective review was conducted on patients who underwent surgical treatment for primary femoral neck fractures (AO/OTA classification, 31-B) at a single university hospital between February 2016 and February 2023. The inclusion criteria were (1) age 18–65 years and (2) newly diagnosed Garden type III/IV femoral neck fractures. The exclusion criteria were as follows: (1) pathological fractures; (2) multiple fractures in the contralateral or ipsilateral lower limb, acetabulum, and pelvis; (3) prior hip arthroplasty in the contralateral limb; (4) lower extremity deformities; and (5) a follow-up period of less than 1 year.
During the study period, patients with unstable femoral neck fractures were assessed for suitability for internal fixation based on a comprehensive evaluation that included age, bone quality, pre-injury functional status, comorbidities, and timing of presentation. Preoperative 3-dimensional CT was routinely reviewed, and internal fixation was selected when satisfactory reduction and stability were considered achievable, including cases in which anterior–medial cortical contact could be restored even in the presence of comminution. When restoration of anterior or medial cortical support was deemed unlikely due to severe comminution, arthroplasty was performed instead, and these patients were excluded from the study cohort.
When osteosynthesis was deemed appropriate, fixation was carried out using either the LSD or the FNS construct. Prior to the introduction of the FNS at our institution, the LSD construct was the standard method for treating unstable fractures. After the FNS became available in late 2019, all subsequent cases were treated with the FNS.
Baseline demographic data, including sex, age, body mass index (BMI), side of injury, time from injury to surgery, and reduction method, were extracted from electronic medical records. Fracture-related characteristics such as Garden classification, Pauwels type and angle, and the presence of posterior comminution, as well as operation-related parameters including reduction type, reduction quality, and tip–apex distance (TAD), were assessed via radiographs and computed tomography images stored in the institutional picture archiving and communication system. The study protocol was approved by the Institutional Review Board of Korea University (IRB No: 2024GR0257).
Surgical technique and postoperative care
All surgical procedures were performed by two board-certified orthopedic trauma surgeons, each with more than 10 years of independent operative experience. All patients were positioned supine on a radiolucent fracture table under general or spinal anesthesia. Closed reduction was attempted initially using gentle traction and internal rotation under fluoroscopic guidance. Anatomical reduction was verified using fluoroscopic imaging obtained at 10-degree intervals with a mobile C-arm, in addition to standard anteroposterior and lateral views. If anatomical reduction could not be achieved with closed methods, open reduction was performed using the Smith–Peterson anterior approach. The femoral head fragment was mostly manipulated using a joystick technique, and the fracture site was compressed using a pointed reduction clamp. Provisional fixation was then strategically achieved using more than two 3.2-mm Steinmann pins inserted percutaneously through a separate lateral incision under fluoroscopic guidance, carefully avoiding the location and planned approach of the definitive fixation implants. Definitive fixation with the assigned implant (FNS or LSD) was performed once anatomical reduction was confirmed.
In the FNS group, a minimally invasive lateral approach was utilized to insert a central barrel along the axis of the femoral neck. A one- or two-hole FNS plate was used. The barrel was positioned centrally within the femoral head, and an anti-rotation screw of equal length was inserted through the targeting guide (zig) to enhance rotational stability. The construct was secured to the lateral cortex using a locking plate to provide angular and rotational stability. Interfragmentary compression was achieved by inserting the multifunction rod and rotating the black screw of the FNS insertion handle counterclockwise. Final implant positioning was confirmed with fluoroscopy prior to wound closure.
In the LSD group, a standard lateral approach was used. A DHS lag screw was first inserted centrally along the femoral neck axis to achieve axial compression across the fracture site. Subsequently, a compression screw was inserted into the hip screw to augment interfragmentary compression. This was followed by insertion of two 6.5-mm CSs—either both fully threaded or a combination of one partially threaded and one fully threaded—arranged in an inverted triangle configuration (superior-anterior and inferior-posterior). In cases where a minimal residual gap persisted following reduction, the partially threaded screw was placed first to diminish the gap and achieve interfragmentary compression. After definitive fixation was completed, the fully threaded screw was inserted to capture and preserve the achieved reduction in a length-stable manner (Figure 1). Illustration and radiographs of surgical treatments. (a) LSD consisting of a DHS with two fully threaded cannulated screws. (b) FNS with one-hole plates. (LSD: length-stable dynamic hip screw, DHS: dynamic hip screw, FNS: femoral neck system).
Postoperatively, all patients followed a standardized rehabilitation protocol: toe-touch weight-bearing for the first 4 weeks, followed by gradual progression to full weight-bearing, depending on radiographic healing and symptom resolution.
Variables
Reduction quality was evaluated intraoperatively using fluoroscopic imaging, with the C-arm rotated in approximately 10° increments to obtain multiple orthogonal views. The final grading was determined from the view demonstrating the greatest residual deformity. Reductions with <2 mm of displacement in any plane and <5° of angulation were classified as “anatomic,” those with 2–5 mm of displacement and/or 5–10° of angulation as “fair,” and those with ≥5 mm of displacement and/or ≥10° of angulation were classified as “poor”. 27 TAD was measured on immediate postoperative radiographs using standard magnification-corrected techniques.
Patients were assessed postoperatively at 2 weeks, 6 weeks, 3 months, 6 months, 12 months, and 24 months. Bone union was defined as continuity of cortical margins on anteroposterior and lateral radiographs. Nonunion was defined as the absence of cortical bridging or persistent fracture lines on radiographs at 6 months postoperatively. At the final follow-up, functional outcomes were assessed using the Hip Disability and Osteoarthritis Outcome Score (HOOS), which consists of five subdomains. Postoperative complications, including avascular necrosis, nonunion, malreduction, implant failure, wound infection, and unscheduled secondary surgery were documented.
To quantify femoral neck shortening, the latest follow-up radiograph was analyzed by overlaying images of the injured and uninjured sides, allowing for measurement of the distance between the shortened, operated femoral neck and the uninjured side.5,16 These measurements were standardized by matching the actual scale with known screw diameters. This approach provided values for shortening the horizontal (x) and vertical (y) axes. The resulting femoral neck shortening vector along the femoral neck angle (z) was calculated using the following equation:
To enhance reliability in measuring the NSA and femoral neck shortening, the assessments were independently performed by two orthopedic surgeons. To enhance both intra- and inter-observer reliability, each observer conducted the measurements twice at 2-week intervals. The final values were determined by calculating the averages of the measurements.
Statistical methods
Statistical analyses were performed using the IBM SPSS Statistics for Windows (version 27.0; IBM Corp., Armonk, NY, USA). Continuous data are presented as means and standard deviations and were compared using either the independent t-test or the Wilcoxon rank-sum test, depending on the normality of each dataset. Normality was assessed using the Shapiro-Wilk test. Categorical data were compared using the chi-square or Fisher’s exact tests, based on the expected cell frequencies. The level of significance was set at p < 0.05. Missing data for the key variables were handled using list-wise deletion.
In the subgroup analyses, statistical methods were selected according to the type of variables being compared. Categorical variables were evaluated using chi-square or Fisher’s exact tests, and results are presented as odds ratios with corresponding p-values. Continuous variables compared across two-level categorical groups were analyzed using independent t-tests and reported as mean differences with p-values. Continuous variables compared across three-level categorical groups—such as Pauwels type—were analyzed using one-way ANOVA, with F statistics and p-values provided. Associations between continuous variables were examined using Pearson correlation analysis, and correlation coefficients (r) with corresponding p-values are reported.
Results
Population characteristics
A total of 65 patients were enrolled in the study, with 31 in the FNS group and 34 in the LSD group (Figure 2). Baseline characteristics—including sex distribution (FNS: 51.6% male; LSD: 58.8% male), mean age (53.0 vs 47.1 years, p = 0.063), BMI (23.7 vs 22.7, p = 0.423), injured side (p = 0.849), and fracture classification—were comparable between groups (Table 1). All patients sustained Garden type III or IV fractures, and more than two-thirds had Pauwels type III patterns (FNS: 61.3%; LSD: 73.5%; p = 0.390). Pauwels angle (53.6° vs 56.9°, p = 0.315), incidence of posterior comminution (58.6% vs 52.9%, p = 0.843), and operative parameters such as reduction method, reduction quality, and TAD showed no significant differences (Table 1). Flowchart of the study population. Patient demographics. BMI: body mass index, Post. Comm.: posterior comminution, OR: open reduction, CR: closed reduction; TAD: tip-apex distance; FNS: femoral neck system; LSD: length-stable dynamic hip screw.

Treatment outcomes
Treatment outcomes.

HOOS: Hip Disability and Osteoarthritis Outcome Score.
Statistically significant differences are indicated by asterisks (*p < 0.05, **p < 0.01).
In the subgroup analyses, BMI was significantly associated with nonunion in both the overall cohort (p = 0.017) and the FNS group (p = 0.047), while older age was associated with nonunion only in the LSD group (p = 0.049). Among operative variables, the need for open reduction was strongly associated with failure to achieve union in the overall cohort (OR 0.130; p = 0.007) and the FNS group (OR 0.078; p = 0.042). Similarly, poor reduction quality was significantly related to nonunion in both the overall cohort (p = 0.015) and the FNS subgroup (p = 0.037). In contrast, fracture pattern–related variables, including Garden type, Pauwels type, Pauwels angle, and posterior comminution, showed no significant association with union rate in any subgroup (Supplemental Table 1).
Femoral neck shortening
Femoral neck shortening.

Statistically significant differences are indicated by asterisks (*p < 0.05, **p < 0.01).

Radiographic comparison of femoral neck shortening in Pauwels type III fractures treated with different constructs.
Across the univariate analyses of radiographic offsets, several patient- and procedure-related variables demonstrated significant associations in specific axes or subgroups (Supplemental Table 2–4). Higher BMI was consistently related to greater displacement, showing significant vertical offset in the overall cohort (p = 0.038) and horizontal offset in the LSD group (p = 0.038). Garden type IV fractures were associated with increased displacement, particularly vertical offset in the overall cohort (p = 0.030) and both femoral neck axis and horizontal offsets in the FNS group (p = 0.044 and p = 0.039). The requirement for open reduction was also consistently associated with larger offsets, including femoral neck axis displacement in the overall and FNS groups (p = 0.029 and p = 0.022) and vertical offset in the LSD group (p = 0.014). Other variables—including age, sex (except in the LSD subgroup), Pauwels type, Pauwels angle, posterior comminution and TAD—showed no significant or consistent associations with any radiographic offset parameters.
Discussion
This study highlights the importance of minimizing femoral neck shortening in unstable fractures and demonstrates that the LSD construct offers superior mechanical stability and functional recovery compared to the FNS. Although both fixation techniques achieved comparable union rates, the LSD group exhibited significantly less femoral neck shortening and improved functional scores, particularly in the symptom and stiffness domains. These findings are particularly meaningful for younger, high-demand patients, in whom the preservation of femoral neck alignment is critical for restoring baseline function and ensuring long-term mobility (Figure 4). A 44-year-old female presented with a Garden IV, Pauwels type 3 femoral neck fracture with posterior neck comminution (red arrow). (a) Open reduction was performed via the Smith-Petersen approach. (b) Initial reduction was achieved using pointed reduction forceps, and the fracture was provisionally stabilized with two K-wires. Intraoperative C-arm imaging revealed a posterior gap, which was compressed using a partially threaded screw (yellow arrows). (c) A DHS was inserted, and interfragmentary compression was obtained with the compression screw. A fully threaded screw was added to complete the LSD construct. (d) Serial radiographs demonstrated bony union without loss of reduction. (e) At the 2-year follow-up, no signs of femoral head avascular necrosis or leg-length discrepancy were observed. (f) The patient achieved full recovery of hip function.
Our findings are supported by multiple biomechanical studies emphasizing the LSD construct’s superior resistance to axial collapse. In cadaveric testing, Stoffel et al. 10 demonstrated that FNS (748.9 ± 211.4 N/mm) did not exhibit a significant stiffness advantage over conventional DHS (688.8 ± 132.6 N/mm), raising questions about its performance under high-load conditions. In contrast, Kemker et al., 15 using synthetic femur models, reported that LSD constructs achieved higher axial stiffness (1854 N/mm) compared to solitary DHS (1482 N/mm) and multiple cannulated screws (1450 N/mm). Moreover, finite element analysis by Jiang et al. 17 demonstrated that a DHS construct combined with two partially threaded screws (DHS + BS), a configuration mechanically analogous to LSD exhibited lower fracture displacement (0.24 mm vs 0.68 mm) and reduced peak implant stress (120 MPa vs 310 MPa) relative to FNS, indicating superior load transfer and fatigue resistance.
Clinical findings in the literature align closely with our observations. Boraiah et al. 16 reported a 94% union rate and minimal femoral neck shortening (1.98 mm) in patients treated with an LSD construct, which included 29 Garden type III/IV fractures among 54 cases. Their Garden IV subgroup exhibited an 89.7% union rate, comparable to our cohort. The observed discrepancy in shortening magnitude between studies may be attributed to methodological differences: while we compared final follow-up radiographs to the contralateral side, Boraiah et al. assessed changes between immediate postoperative and 6-months radiographs. Nonetheless, both studies reinforce the notion that LSD constructs effectively minimize femoral neck shortening in unstable fractures without compromising healing potential.
Conversely, previous studies assessing FNS have yielded variable outcomes, particularly in the context of unstable fracture patterns. Gupta et al. 24 reported that FNS resulted in less femoral neck shortening than CSs (3.77 ± 1.87 mm vs 6.53 ± 1.59 mm); however, their cohort was predominantly composed of Garden type II fractures. In contrast, Zheng et al. 18 found that in a cohort with more severe Garden III/IV fractures, FNS was associated with greater shortening (4.5 mm) compared to CSs (2.8 mm). Similarly, Ge et al. 28 observed marginally less shortening with FNS than with blade-type DHS, but only 27.9% of their sample comprised Garden IV fractures. Our study, which included a higher proportion of unstable cases (64.7% Garden IV fractures with vertical orientation and posterior comminution), demonstrated significantly greater shortening in the FNS group. Furthermore, these results correspond with our subgroup analyses, which indicated that Garden type IV fractures exhibited increased postoperative offset when managed with FNS, while the LSD construct effectively mitigated such displacement. Collectively, this suggests that the severity and morphology of the fracture may critically influence the mechanical efficacy of FNS fixation.
Recent clinical data further support the limitations of FNS when used in isolation, particularly in unstable fracture configurations. A retrospective study involving 129 young adults with femoral neck fractures reported that patients treated with FNS combined with a supplementary CS experienced significantly improved outcomes compared to those treated with FNS alone. The combined group demonstrated the shortest time to fracture union, the smallest change in the neck-shaft angle (0.76 ± 0.54°), reduced femoral neck shortening, and the highest Harris Hip Scores at final follow-up. 29 These findings complement our results and underscore that, particularly in highly unstable fracture patterns, transforming FNS into a length-stable construct through the use of additional screw fixation may improve axial stability and mitigate collapse, paralleling the benefits seen with dedicated constructs like LSD.
This study has several limitations. First, its retrospective design and relatively modest sample size may restrict the generalizability of the findings. Although the strict inclusion criteria reduced the number of eligible patients, they strengthened internal validity and enabled a focused evaluation of fixation outcomes in young patients with unstable femoral neck fractures—a population in which high-quality evidence remains limited due to the rarity of these injuries. Future multi-center studies with larger cohorts are needed to validate and extend our results. Second, the use of contralateral femoral comparison to assess postoperative shortening may overestimate early implant-induced compression rather than capturing true fracture collapse. However, this method enables evaluation of cumulative femoral neck shortening—including changes during reduction, intraoperative compression, and subsequent healing—thus providing a comprehensive assessment of morphological alteration. Nevertheless, because plane radiographs cannot fully capture the complex three-dimensional nature of femoral neck deformation, future studies integrating cross-modality comparisons—such as CT-based or three-dimensional assessments—are warranted to further strengthen the methodological rigor of shortening evaluation. Moreover, as this study did not include augmented FNS configurations, future investigations are warranted to evaluate whether similar length-stable strategies using modified FNS constructs can achieve comparable biomechanical and clinical outcomes.
Conclusion
Length-stable fixation using the LSD construct significantly reduced postoperative femoral neck shortening in high-grade unstable fractures, without compromising union rates or functional recovery. Our results support the role of length-stable constructs as a preferred option for maintaining anatomic integrity in unstable femoral neck fractures.
Supplemental material
Supplement Material - Length-stable fixation reduces femoral neck shortening in unstable femoral neck fractures: A retrospective comparative study of length-stable dynamic hip screw versus femoral neck system fixation
Supplemental Material for Length-stable fixation reduces femoral neck shortening in unstable femoral neck fractures: A retrospective comparative study of length-stable dynamic hip screw versus femoral neck system fixation by Seonghyun Kang, Wonseok Choi, Jeong Seok Choi, Eic Ju Lim, SungJin Ahn, Jong-Keon Oh, William T. Kent, Whee Sung Son, and Jae-Woo Cho in Journal of Orthopaedic Surgery.
Footnotes
Ethical considerations
This study was conducted following the Declaration of Helsinki and approved by the Institutional Review Board of Korea University (IRB No. 2024GR0257, approval date: Jul. 11, 2024).
Consent to participate
Written informed consent was obtained from the patient featured in Figures 3 and ![]() for publication of the clinical images and radiographs.
for publication of the clinical images and radiographs.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This research was supported by the Korea Health Industry Development Institute (KHIDI) under the Global Physician-Scientist Training Program, funded by the Ministry of Health and Welfare, Republic of Korea (RS-2025-02264012), and by the AO Foundation (AOTrauma_S_APAC_2025-01918).
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.