Abstract
Keywords
Introduction
As described by Jean Dubousset, individuals maintain an ergonomic position within the “cone of the economy”. 1 Ideal spinal alignment enables an individual to assume a standing posture with minimum energy expenditure, without any compensation. Even in asymptomatic individuals, spinal sagittal malalignment can cause greater muscle recruitment and energy expenditure in order to maintain an erect posture and require the usage of compensatory mechanisms.
Compensatory mechanisms include cervical hyper-lordosis, 2 reduction in thoracic kyphosis, 3 pelvic retroversion, 4 knee flexion (KF),5,6 and ankle extension. 4 The interactions of the aforementioned compensation mechanisms and the correlations between such compensations and health-related quality of life (HRQOL) remain unclear. The alignment of the knee joint is especially important among lower-extremity alignments, and abnormal knee alignment potentially triggers the onset and development of knee osteoarthritis and leads to deformity in lower extremities.7,8 Furthermore, knee osteoarthritis is associated with spinal sagittal malalignment. 9 Therefore, it is important to investigate the relationship between knee alignment and the severity of knee osteoarthritis and spinal deformity in the older population.
Several studies have reported that lower-limb flexion compensate for the sagittal alignment in patients with adult spinal deformity without mentioning the presence of knee osteoarthritis.6,10 However, it remains unclear how knee osteoarthritis and spinal deformity interact with KF. Using a propensity score-matched analysis for the adjustment of baseline data, we aimed to clarify the relationship between KF in the standing position and the severity of spinal deformity and knee osteoarthritis in community-dwelling older volunteers. We hypothesized that KF in the standing position would not be due to the progression of knee osteoarthritis, but due to the compensation mechanism of spinal deformity.
Materials and methods
Ethics approval
This study was approved by the Clinical Ethics Committee of our institution. Written informed consents were obtained from all volunteers prior to participation in the study.
Study design
A total of 279 adult volunteers participated in the 2018 Health Screening Program in Toei (Aichi, Japan; Figure 1). The inclusion criteria were as follows: (1) individuals undergoing spine radiography, musculoskeletal screening, and physical examinations (height, body weight, and body mass index [BMI]) during their basic health check-up; and (2) those who provided informed consent to participate. The exclusion criteria were as follows: (1) age < 60 years; and (2) individuals with a history of hip, knee, or spinal surgery. Study design. KF, Knee flexion; BMI, body mass index.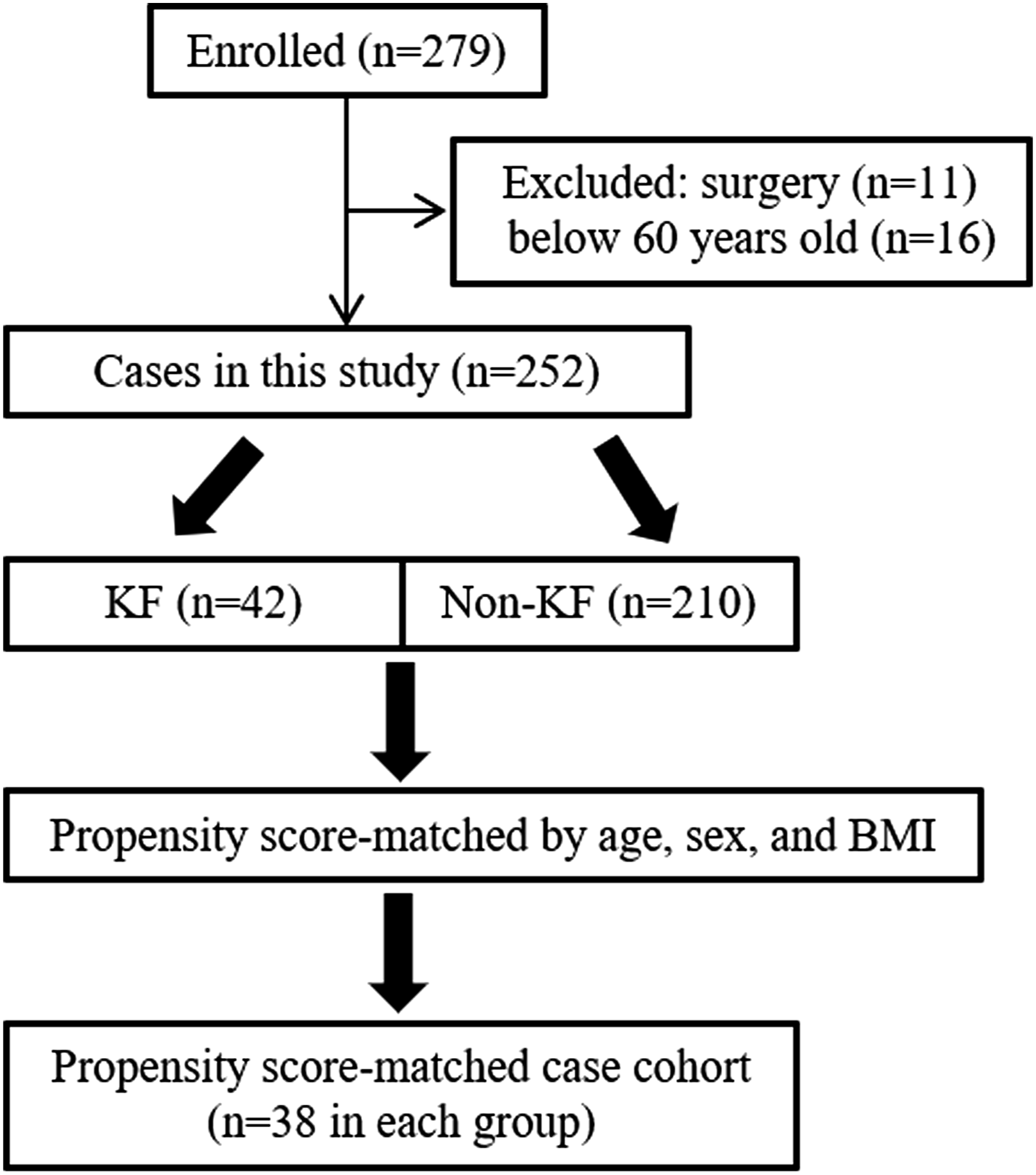
Data collection
The following demographic characteristics of the participants were evaluated: age, sex, height, body weight, BMI, femoral neck bone mineral density (BMD), lumbar BMD, and grasping power. Low back pain and knee pain were measured using a questionnaire; cases were requested to mark the pain intensity on a diagram of the body surface on a scale of 0–10, with 0 representing “no pain” and 10 representing “severe pain,” and data regarding the knee and lower-back areas were selected. The 25-question Geriatric Locomotive Function Scale (GLFS-25) was evaluated to assess the risk of locomotive syndrome, including muscle weakness, joint or spine disorders and osteoporosis, knee pain, and low back pain. 11 Furthermore, the Oswestry Disability Index (ODI) was evaluated to determine the HRQOL associated with low back pain. 12
Radiographic measurements
Lateral and anteroposterior radiographs of each case were taken in a free-standing position with their fingers resting on their clavicles. Furthermore, the radiographs were obtained from a 1.5 m distance between the radiography tube and the film for all participants.
13
After the digitally obtained radiographs were transferred, all parameters were measured using imaging software (Surgimap Spine, Nemaris Inc., New York, NY). The following spinopelvic parameters were assessed in the frontal or lateral radiographs: C2-sagittal vertical axis (C2-SVA), C7-SVA, T1 pelvic angle (TPA), cervical lordosis (CL), thoracic kyphosis (TK, Cobb angle between T5 and T12), lumbar lordosis (LL), pelvic incidence (PI), pelvic tilt (PT), sacral slope (SS), PI minus LL (PI–LL), C7-center sacral vertical line (the distance between the C7 plumb line and center sacral vertical line), Cobb angle of degenerative lumbar scoliosis (measured by Cobb method; the range of the curve apex is from T10 to L5), and L4 tilt. The following lower-extremity parameters were assessed in the frontal or lateral radiographs (Figure 2): knee angle (KA, angle between the femoral and tibial mechanical axes, angle between the midpoint of the two femoral heads and the line between the midpoint of the tibial plateau on each side and the midpoint of the ankle joint on each side), ankle angle (AA, angle between the tibia mechanical axes and the vertical), pelvic shift (PS, offset between the posterior superior sacrum and the anterior distal tibial cortex), femur-tibia angle (FTA, the average of the left and right FTAs; the lateral angle at the intersection of the femoral and tibial bone axes); and the hip-knee-ankle angle (HKA angle, the average of the left and right HKA angles; the lateral angle between the femoral and tibial mechanical axes).10,14 Radiographic measurements of lower extremity parameters. (a) Sagittal lower extremity radiograph; (b) Coronal lower extremity radiograph. KA, knee angle; AA, ankle angle; PS, pelvic shift; FTA, femur–tibia angle; HKA, hip–knee–ankle.
Grouping
Once all the data were collected, the included participants were divided into the following two groups based on the radiographic findings: KF group (KA ≥10°) and non-KF group (KA <10°), based on the study by Obeid et al. 6 Furthermore, we performed subgroup analysis by severity of adult spinal deformity by the SRS-Schwab classification and of knee osteoarthritis by Kellgren Lawrence (KL) grading. The SRS-Schwab classification is classified according to non-pathologic, moderate, and marked deformity. 15 We classified non-pathologic and moderate deformity into the mild spinal deformity group, and marked deformity was classified into the severe spinal deformity group. KL grading is classified from grade 0 (no osteoarthritis) to grade 4 (severe osteoarthritis). 16 We classified KL grade 0 to 2 into the mild osteoarthritis group, and KL grade 3 and 4 into the severe osteoarthritis group.
Statistical analysis
We compared baseline data between KF and non-KF groups as a preliminary analysis. A one-to-one propensity score matching analysis was performed because of significant differences in baseline values between the groups. Age, sex, height, body weight, and BMI were included in the multivariate logistic regression model to calculate the propensity score for the presence of KF. The C-statistic was calculated to evaluate the goodness of fit. We compared the data between matched KF and non-KF groups in subsequent analyses.
The Pearson correlation test was used to evaluate the correlation of factors related to KF. We considered r values of ≥0.70 to represent a very strong correlation, 0.40 to 0.69 representing a strong correlation, 0.30 to 0.39 representing a moderate correlation, 0.20 to 0.29 indicating a weak correlation, and values <0.2 representing a negligible correlation. Categorical variables are expressed as absolute numbers and percentages and were analyzed using Chi-square tests or Fisher’s exact tests, as appropriate. We used the Shapiro–Wilk test to determine whether continuous variables were normally or non-normally distributed. Continuous variables with normal distributions are expressed as means ± standard deviations (SD) and were analyzed using unpaired t-tests. Statistical analyses were conducted with SPSS Version 25.0 (IBM, Armonk, NY, USA). p values of less than 0.05 were considered statistically significant.
Results
The correlation of factors related to knee flexion.

Statistically significant at *p < 0.05; **p < 0.01.
ODI, Oswestry disability index; KL grade, Kellegren-Lawrence grade.
Analysis of the entire cohort
Comparison of data between knee flexion (KF) and non-KF groups.

Values expressed as mean ± SD or number (percentage). *statistically significant difference.
BMD, bone mineral density; YAM, young adult mean; GLFS-25, 25-question Geriatric Locomotive Function Scale; ODI, Oswestry disability index; C7-CSVL, C7 plum line and the center sacral vertical line; DLS, degenerative lumbar scoliosis.
Analysis of the matched cohorts
Comparison of data between knee flexion (KF) and non-KF groups after propensity score-matched analysis.

Values expressed as mean ± SD or number (percentage). *statistically significant difference.
BMD, bone mineral density; YAM, young adult mean; GLFS-25, 25-question Geriatric Locomotive Function Scale; ODI, Oswestry disability index; C7-CSVL, C7 plum line and the center sacral vertical line; DLS, degenerative lumbar scoliosis.
Subgroup analysis for clarifying the hypothesis
Subgroup analysis between knee flexion (KF) and non-KF groups.
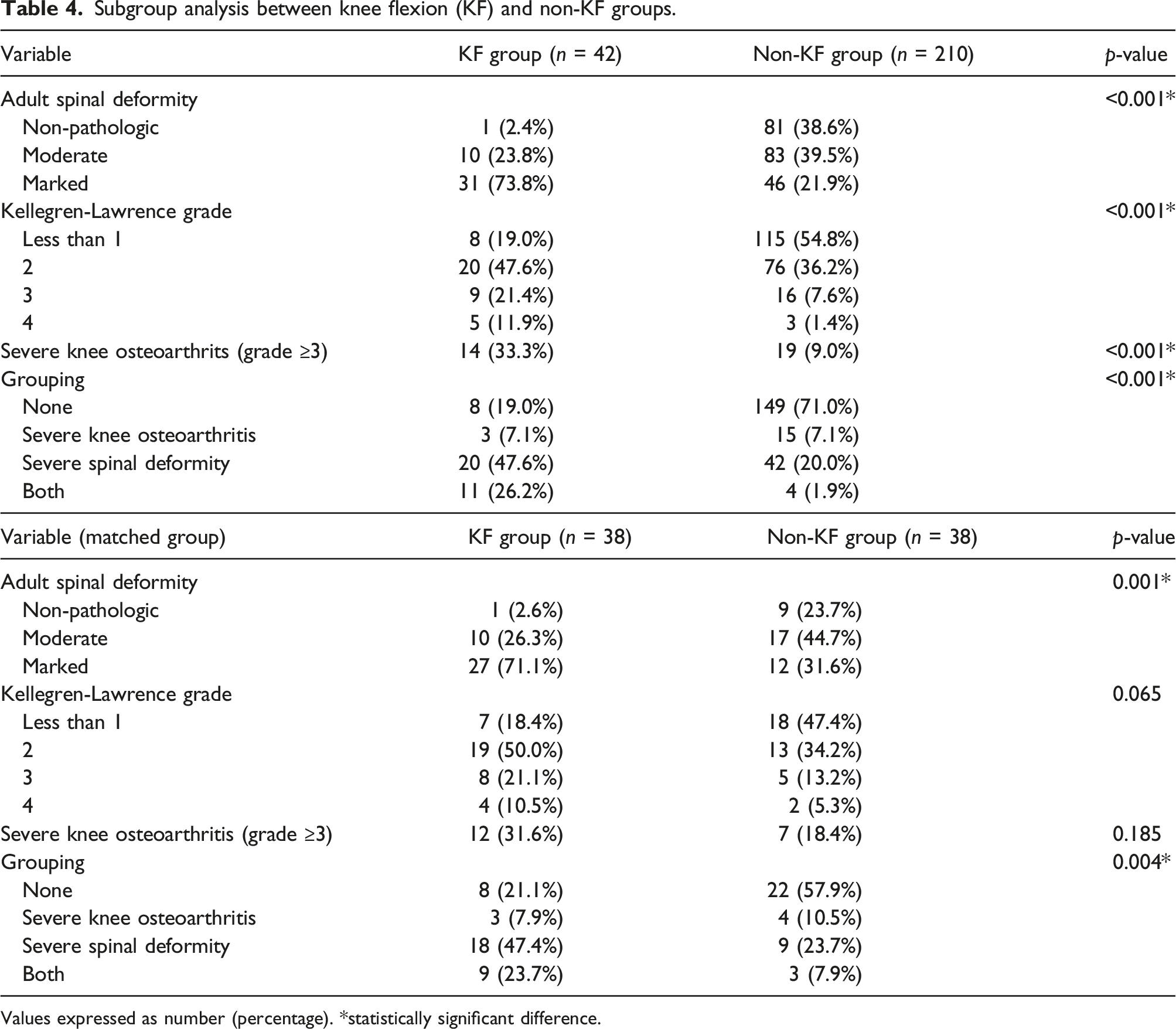
Values expressed as number (percentage). *statistically significant difference.
Among the matched cohort, the severity of adult spinal deformity in the KF group was more as compared with the non-KF group (p = 0.001). However, the severity of knee osteoarthritis and the presence of severe knee osteoarthritis did not differ between the KF and non-KF groups (p = 0.065 and p = 0.185, respectively). In the KF group, 71.1% of the participants had severe spinal deformity, and 31.6% of them had severe knee osteoarthritis. Of the 31.6%, 7.9% were attributable to knee osteoarthritis alone, and 23.7% to both knee osteoarthritis and spinal deformity.
Cases presentation
The radiographic parameters of Figure 3 were 41° for PT, 136 mm for C7-SVA, 40° for PI-LL, 18.4° for KA, 13.6° for AA, 80.9 mm for PS, 176.8° for FTA, 178.2° for HKA, 1 for KL. She is a 76-year-old patient with knee flexion due to severe spinal deformity alone, but no knee osteoarthritis. The radiographic parameters of Figure 4 were 17° for PT, -6 mm for C7-SVA, 0° for PI-LL, 3.9° for KA, 4.4° for AA, 68.7 mm for PS, 182.4° for FTA, 188.7° for HKA, 3 for KL. She is a 73-year-old female without severe spinal deformity and knee flexion, but with severe knee osteoarthritis. Standing Radiographs of a representative case with knee flexion due to severe spinal deformity alone. A 76-year-old female patient without knee osteoarthritis. (a) Sagittal spinopelvic radiograph; (b) sagittal lower extremity radiograph; (c) coronal lower extremity radiograph. Standing radiographs of a representative case without severe spinal deformity and knee flexion. A 73-year-old female patient with severe knee osteoarthritis. (a) Sagittal spinopelvic radiograph; (b) sagittal lower extremity radiograph; (c) coronal lower extremity radiograph.

Discussion
In this study, the prevalence of KF (defined as KA ≥10°) was 16.7% among community-dwelling volunteers aged over 60 years. To our knowledge, there has been no previous report on the prevalence of KF determined from older volunteers at a musculoskeletal screening. However, there was a report on the mean KA value among asymptomatic volunteers (aged 61–70 years, 1.9°; aged over 70 years, 5.2°). 17 In this study, as the mean KA value of cases aged 61 to 60 years was 0.7°, and of individuals aged over 70 years was 4.7°, the prevalence of KF in our results would be similar in other regions or ethnicities. 17 Among the pre-matched cohorts in this study, the KF group had whole-body malalignment, including spinopelvic and lower-extremity malalignments. Compared to the non-KF group, knee pain, low back pain, ODI, and GLFS-25 scores were significantly higher in the KF group; however, there were significant differences in age and BMI between the two groups. It is already known that aging, higher BMI, and female sex are the main risk factors of knee osteoarthritis and decreased HRQOL.9,18 Our results were more trustworthy following propensity score-matched analysis for baseline data modification. Among the matched cohorts, we discovered that KF was associated with sagittal spinopelvic and lower-extremity malalignment, as shown by high SVA, TPA, PT, PI-LL, KA, AA, and PS. There was a significant difference in low back pain, ODI, and GLFS-25 between the KF and non-KF groups. However, there was no relationship between KF and knee pain. As the results of the subgroup analysis, we clarified that compensatory changes due to spinopelvic malalignment (71.1%), not due to knee osteoarthritis alone (7.9%), mainly affect KF in the standing position. We believe that the presence of spinopelvic malalignment as well as the knee osteoarthritis should be assessed to identify the primary cause of KF for symptomatic outpatients with KF in the standing position.
Spinal aging is characterized by hypertrophic facet joint arthritis, degenerative disc disease, and atrophy of extensor muscles, resulting in progressive kyphosis of the lumbar spine. 5 According to Oe et al., 19 sagittal pelvic alignment deteriorates with aging and differs significantly between men and women. A concordant relationship between the cranium, spine, and pelvis is required for spinal sagittal alignment. 20 When there is a significant spinopelvic malalignment, pelvic retroversion is no longer effective, and another compensatory mechanism is induced, which involves the lower extremities. 6 First, the hips achieve their maximum extension at the same time of pelvic retroversion, following which the KF begins, i.e., the last compensatory mechanism is KF. 6 In this study, we investigated the relationship between KF and whole body alignment. We decided the cut-off value of KA based on the article of Obeid et al., 6 as most cases with KA ≥10° had a loss of LL of >30°, which means obvious spinal deformity. After removing the bias of baseline data, KF was associated with sagittal spinopelvic and lower-extremity malalignment, which was consistent with previous reports.6,21,22 Furthermore, this study revealed that the standing position in cases with KF was maintained by shifting the ankle positions anteriorly to the pelvis and ankle dorsiflex as compensation mechanism.
The lower extremities are engaged to compensate for spinopelvic alignment to sustain trunk alignment [4]. Especially, KF is associated with sagittal spinopelvic and lower-extremity malalignment;6,21,22 however, it remains unclear how knee osteoarthritis and spinal deformity interact with KF. The FTA and HKA are used to evaluate knee alignment in the coronal plane, and knee deformity increases articular cartilage stress, resulting in knee osteoarthritis.7,8,23 Yasuda et al. 9 reported that there was sagittal spinopelvic malalignment in cases with knee osteoarthritis. In a previous study with a follow-up period of over 22 years, an increase in PI-LL was associated with changes in FTA. 14 In the present study, KF was associated with FTA after adjustment for age, sex, and BMI. In short, compensatory mechanisms of lower-extremity due to spinopelvic malalignment included not only KF in the sagittal plane but also knee varus in the coronal plane. Knee varus would result in increased mechanical stress on the lateral articular cartilage. 24 These compensatory changes may induce the development and progression of knee osteoarthritis.
In previous studies, various self-assessed HRQOL measures in patients with adult spinal deformity have been performed; whereas we used ODI to quantify disability related to low back pain. 25 Pelvic posterior shift significantly correlates with ODI, and the correlation emphasizes the role of compensatory mechanisms associated with sagittal malalignment. 25 After the adjustment of age, sex, and BMI in this study, there were significant differences in low back pain, GLFS-25, and ODI scores between the groups; however, the knee pain score was not significantly different. We found that KF correlated with decreased HRQOL mainly due to low back pain, not due to knee pain. The result of our study emphasizes that KF is a compensatory parameter that is as important as the pelvic posterior shift.
This study had some limitations. First, all of the data were collected from Japanese participants; thus, it may be difficult to generalize these findings to other populations, limiting its generalizability. However, since Japan has the highest percentage of older persons as compared with other countries, these findings would improve the understanding of age-related changes in other populations. Second, as the participants in our study were community-dwelling volunteers, clinical assessments, including pre- and postoperative assessments of the compensatory mechanisms after corrective spinal surgery for spinal deformity were not performed. Further prospective longitudinal research is required to better understand the cause of KF and the impact on an individual’s HRQOL. Finally, there are many reasons for spine deformity and perhaps the postures observed in this study were temporary compensatory postures. In future studies, we need to add more numbers and analyze relevant factors.
Conclusions
In conclusion, we clarified that compensatory changes due to spinopelvic malalignment, not due to knee osteoarthritis alone, mainly affected KF in the standing position. After the adjustment of age, sex, and BMI, KF was strongly associated with sagittal spinopelvic and lower-extremity malalignment, and decreased HRQOL due to low back pain, however, there was no relationship between KF and knee pain score.
Footnotes
Acknowledgements
We sincerely thank for hospital staff in Toei, and express their sincere gratitude to Ms. Nao Kuwahara, Tomoe Mabuchi, Mrs. Taku Nagao, and Tomokazu Suzuki, secretaries in the Department of Orthopedic Surgery, Hamamatsu University School of Medicine. The authors also would like to thank Editage (![]() ) for English language editing.
) for English language editing.
Declaration of conflicting interests
The author(s) declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: Yu Yamato and Shin Oe work at a donation-endowed laboratory and are funded by Medtronic Sofamor Danek Inc., Japan Medical Dynamic Marketing Inc., and Meitoku Medical Institution Jyuzen Memorial Hospital. For the remaining authors, none were declared. The submitted manuscript does not contain information about medical devices/drugs.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by the funding sources of Yu Yamato and Shin Oe. Medtronic Sofamor Danek Inc., Japan Medical Dynamic Marketing Inc., and Meitoku Medical Institution Jyuzen Memorial Hospital
Ethics approval
The study was approved by Hamamatsu University School of Medicine hospital’s institutional review board (IRB No.16-115).
