Abstract
Wilms’ tumor is associated with a high treatment success rate, but there is still a risk of recurrence. Cisplatin, which is one of the chemotherapeutic agents used for its treatment, is associated with a very high rate of resistance. Par-4 (prostate apoptosis response 4) is a tumor suppressor, which is capable of sensitizing tumor cells to chemotherapy. Therefore, the aim of this study was to determine whether combined treatment with Par-4 and cisplatin is effective for inhibiting growth of Wilms’ tumor. Wilms’ tumor and control cell samples were collected and analyzed by immunofluorescence assay and immunohistochemistry. Total proteins extracted from cultured cells were analyzed using western blotting and flow cytometry. In addition, a mouse xenograft model was established. We discovered significantly low expression of Par-4 in the tumor tissue, which was positively correlated with high expression of GRP78 (glucose-regulated protein 78). In addition, we found that ectopic Par-4 co-localized with cell surface GRP78 and induced high expression of the endoplasmic reticulum proteins ATF4 and BAX, which activated the endoplasmic reticulum apoptosis pathway. Moreover, treatment with ectopic Par-4 and cisplatin suppressed xenograft growth in nude mice. In conclusion, our results showed that Par-4 overexpression and cisplatin had a synergistic effect on SK-NEP-1 cells, as a result of which cell growth was inhibited and cellular apoptosis was induced. Thus, in vitro and in vivo upregulation of Par-4 expression is indispensable for the trafficking of GRP78 to the cell membrane and subsequent apoptosis of cancer cells.
Introduction
Wilms’ tumor is the most common abdominal malignancy in children, affecting 1 out of every 10,000 children worldwide. 1 This tumor often presents in patients aged 1 to 5 years. 2 It is treated using multimodal methods, including surgery, radiotherapy, and chemotherapy, and the success rate is high. Moreover, the prognosis of this disease has dramatically improved in the last few decades. 3 The two main international Wilms’ tumor study groups, that is, the International Society of Paediatric Oncology and the Children’s Oncology Group, reported that the 5-year survival rate exceeded 90% in developed countries. 4 However, tumor recurrence is still a problem, and the mortality rate is unacceptably high in some cases. Therefore, researchers have been investigating new and more effective therapeutic methods.
Prostate apoptosis response 4 (Par-4) protein, a pro-apoptotic protein that was primarily identified in prostate cancer cells, selectively regulates apoptosis in a wide variety of cancer cells. 5 All the Par-4 studies conducted so far have focused on its intracellular role. One of these studies was our previous study, which reported the mechanism underlying the regulatory effect of Par-4: Par-4 and THAP1 work in synergy to induce CCAR1 gene expression and cellular apoptosis in T-cell acute lymphoblastic leukemia. 6 Furthermore, Par-4 has been found to act as a tumor suppressor in numerous human cancers, namely, renal cell carcinoma and colon, lung, and pancreatic cancer. 7
Recent studies have shown that ectopic Par-4 is part of a novel extrinsic apoptosis pathway that involves its SAC (selective for apoptosis in cancer cells) domain and cell surface receptor glucose-regulated protein 78 (GRP78). 8 GRP78 belongs to the family of heat shock proteins and plays the role of a molecular chaperone in the endoplasmic reticulum (ER). 9 The expression of GRP78 at the cell surface was found to be regulated by intracellular Par-4. 10 Moreover, extracellular Par-4 could integrate with cell surface GRP78 and induce ER stress (ERS), which in turn upregulates GRP78 expression. 11 Based on all these findings, it is possible that the co-localization of Par-4 and GRP78 in the ER plays a role in the regulation of survival and apoptosis of wild type (WT) cells, but this has not been investigated by any study so far. 12
Currently, actinomycin-D and vincristine are the standard chemotherapeutic agents that are efficacious for the treatment of Wilms’ tumor, including preoperative and postoperative chemotherapy. 13 In cases where the first line of chemotherapy fails, cisplatin (used for the treatment of various solid tumors) can be used as a feasible alternative to actinomycin-D. However, resistance to the chemotherapy drugs is a major limitation. Both in vitro and in vivo studies have revealed that par-4 sensitizes colon tumors to 5-fluorouracil, but it is not clear whether Par-4 is involved in cisplatin resistance in Wilms’ tumor. 14
The aim of our study was to examine the in vitro and in vivo anti-tumor activity of combination therapy with ectopic par-4 and cisplatin in Wilms’ tumor and the possible underlying molecular mechanisms. We have shown that combined treatment with ectopic Par-4 and cisplatin resulted in an increase in the expression of apoptosis-related proteins by inducing the ER apoptosis pathway in vivo and in vitro. These findings may prove useful for future therapeutic strategies for Wilms’ tumor.
Materials and methods
Samples and cell lines
The nephroblastoma and normal kidney tissues were provided by the Urology Surgery Department of Nanjing Children’s Hospital. The human WT cell line SK-NEP-1 was purchased from the American Type Culture Collection (Manassas, VA, USA) and cultured in McCoy’s 5A (Gibco, USA) supplemented with 15% fetal bovine serum (HyClone, USA) and 1% penicillin–streptomycin at 37°C in a 5% CO2 incubator.
Transfection
The cell medium in which the SK-NEP-1 cells were cultured in was replaced with antibiotic-free medium before transfection at 36 h. Then, the cells were transfected using Lipofectamine®2000 according to the manufacturer’s instructions. The pEGFP-C1 plasmid was used in the negative control group. The apoptosis rate in the transfected cells was determined by flow cytometry, and protein expression was analyzed using western blot analysis.
Immunofluorescence assay
Cells were fixed in 4% paraformaldehyde and permeabilized in 0.5% phosphate-buffered saline (PBS)/Triton X-100 (PBST). The cells were then blocked with 5% goat serum to decrease non-specific binding for 30 min at room temperature and were incubated with mouse anti-Par-4 antibody (1:100; Abcam, USA), rabbit anti-calnexin antibody (1:150; Abcam), mouse anti-GRP78 antibody (1:100; Abcam), and rabbit anti-calnexin antibody (1:150; Abcam) at 4°C for overnight in a wet box. They were then incubated with the secondary antibodies rhodamine (TRITC) goat anti-mouse IgG (1:100; Jackson, USA) and FITC AffiniPure goat anti-rabbit IgG (1:100; Jackson) for 1 h at room temperature in the dark. After staining with 4′,6-diamidino-2-phenylindole for 40 s, the cells were observed and photographed using a confocal laser scanning microscope.
Immunohistochemistry
Tissue slides were fixed in 10% neutral formalin and embedded in paraffin. The sections were cut into a thickness of 5 µm with a microtome deparaffinized in xylene and were rehydrated in a gradient series of ethanol. Then, 3.3% of H2O2 was added to inhibit endogenous peroxide activity for 10 min at room temperature, and the sections were exposed to boiled 0.01 mol/L citrate buffer (pH 6.0) in a microwave for antigen retrieval. The slides were then blocked with 5% goat serum to decrease non-specific binding for 20 min at room temperature and incubated with mouse anti-Par-4 antibody, mouse anti-GRP78 antibody, and mouse anti-BAX antibody (1:100; Abcam) at 4°C for overnight. The slides were washed with PBS and were incubated in biotin-labeled goat anti-mouse immunoglobulin G (IgG) at 37°C for 20 min. They were then incubated with the streptavidin–biotin complex (SABC) for 20 min. The slides were visualized using hematoxylin–eosin (H&E) staining. The average density was calculated using Image-Pro Plus 6.0.
Western blot analysis
For western blot analysis, total proteins from the pEGFP-C1-Par-4 plasmid, pEGFP-C1 plasmid, and blank control (BC) groups were extracted in lysis buffer (KeyGen Biotech, China). According to the protocol, the proteins were separated on 10% sodium dodecyl sulfate–polyacrylamide gel electrophoresis (SDS-PAGE) and then transferred onto a polyvinylidene fluoride (PVDF) membrane. The PVDF membrane was blocked with 5% bovine serum albumin for 2 h and incubated with glyceraldehyde 3-phosphate dehydrogenase (GAPDH) or the Par-4, GRP78, ATF4, or BAX antibody (1:1000; Santa Cruz Biotechnology, Dallas, Texas, USA) at 4°C for overnight. After washing three times with Tris-buffered saline containing Tween, they were incubated with the corresponding horseradish peroxidase–conjugated secondary antibodies. The bands of proteins on the membranes were visualized with 3,3′-diaminobenzidine (DAB), observed using ChemiDOC™XRS, and analyzed by Image Lab.
Flow cytometry analysis
Cells (2 × 106) were incubated in six-well plates and were treated with the pEGFP-C1-Par-4 plasmid (Clontech Co., USA), pEGFP-C1 plasmid (Clontech Co.), cisplatin (Selleck, Shanghai, China), pEGFP-C1 plasmid + cisplatin, or pEGFP-C1-Par-4 plasmid + cisplatin. After culturing for 48 h, the cells from different groups were washed with PBS and fixed with 70% ethanol at 4°C for overnight. After Annexin V/fluorescein isothiocyanate (FITC) staining was performed, a flow cytometer was used to examine cellular apoptosis.
Mouse xenograft experiments
Cells were resuspended in McCoy’s 5A medium (Gibco) and Matrigel gel (BD Co., USA) for adjusting the density of the SK-NEP-1 cells to 1.5 × 107/mL. The xenograft tumor model was established by injecting SK-NEP-1 cells into the right axilla of female BALB/c nude mice aged 4–6 weeks and weighing 17–20 g (provided by SLAC Laboratory (License: SCXK 2012-0002), China) that were raised at the Nanjing Medical University SPF Animal Experiment Center. After 24 days, the transplanted tumors grew to 8–10 mm in diameter. Then, the mice were randomly divided into five groups: the Par-4 + cisplatin group (treated with adenovirus-mediated Par-4 (1.0 × 1010 pfu (plaque-forming unit)) and cisplatin), Par-4 group (treated with adenovirus-mediated Par-4 (1.0 × 1010 pfu)), cisplatin (treated with cisplatin), negative control Par-4 group, and BC groups. Cisplatin was administered in the abdominal cavity, and Par-4 was injected into tumor tissues. The subcutaneous tumors were measured every 3 days with vernier calipers. The mice were euthanized on the 22nd day, and the tumors were individually assessed for their volume and weight. Expression of the Par-4, GRP78, and BAX proteins in the transplanted tumor tissues was determined by H&E staining and immunohistochemical analysis.
Statistical analysis
By using the SPSS16.0 software for statistical analysis, data were expressed as the mean ± standard deviation (SD) values. Differences between groups were analyzed by analysis of variance (ANOVA). The Student’s t test was used to analyze p values, which were considered to indicate statistically significant differences if they were less than 0.05.
Results
Par-4 expression in nephroblastoma cells
Immunohistochemistry was used to determine the expression of the Par-4, GRP78, and BAX proteins in both the nephroblastoma and control groups. As shown in Figure 1(a) and Table 1, the expression level of Par-4 and BAX was significantly higher in the peritumoral tissues (0.493 ± 0.006 and 0.431 ± 0.009, respectively) than in the tumor tissues (0.320 ± 0.007 and 0.326 ± 0.010, respectively; p < 0.05). The expression level was determined according to the mean density measured by Image-Pro Plus 6.0. Moreover, the expression of GRP78 was significantly lower in nephroblastoma tissue (0.372 ± 0.013) than in normal renal tissue (0.549 ± 0.014; p < 0.05). We also discovered that the mean density of Par-4 was negatively correlated to the mean density of GRP78 in Wilms’ tumor tissues (r = −0.740, p < 0.01; Figure 1(b)). In contrast, the mean density of BAX and Par-4 showed a positive correlation (r = 0.791, p < 0.01).
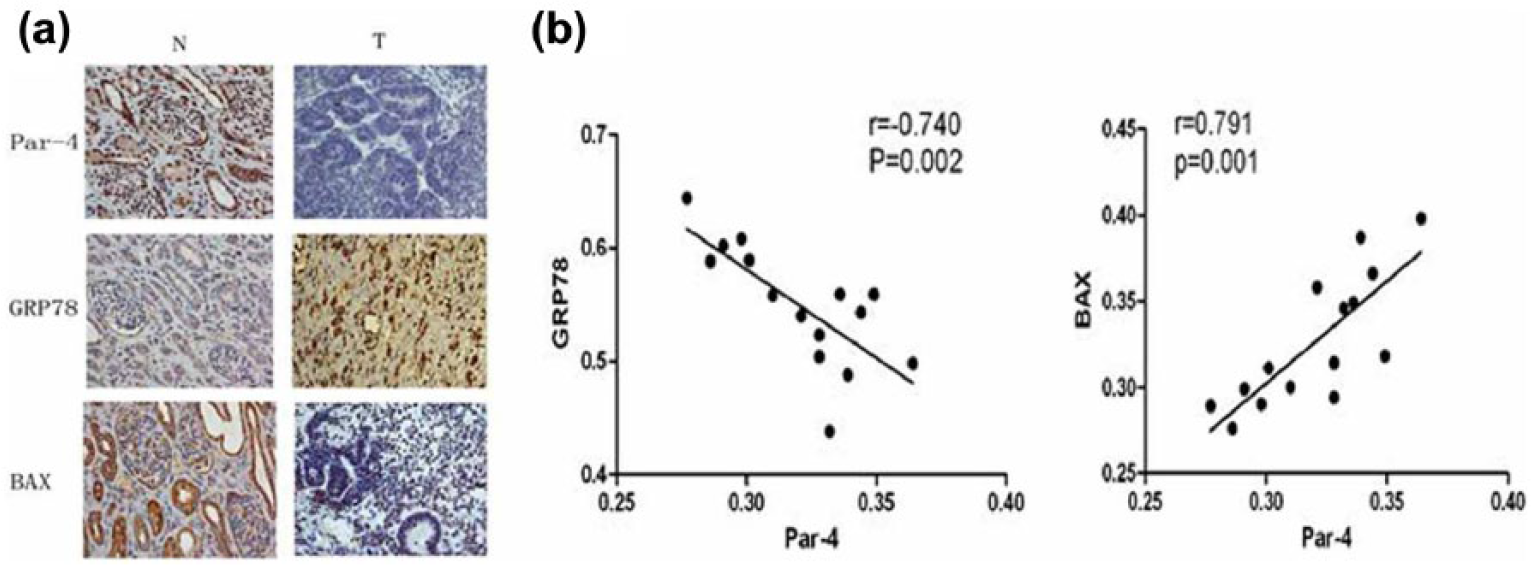
Par-4, GRP78, and BAX expression in nephroblastoma tissues. (a) Expression of Par-4, GRP78, and BAX in nephroblastoma and normal renal tissues (400×). Par-4, GRP78, and BAX expression was analyzed immunohistochemically in nephroblastoma (T) and normal renal tissues (N). The brown-yellow granules represented the stained proteins. (b) Correlation of Par-4 expression with GRP78 and BAX expression in nephroblastoma tissues. The mean density of Par-4, GRP78, and BAX was measured by Image-Pro Plus 6.0. Par-4 expression was found to be negatively correlated with GRP78 expression, while it was positively correlated with BAX expression.
The mean density of Par-4, GRP78, and BAX in nephroblastoma and normal renal tissues.

Par-4: prostate apoptosis response 4; GRP78: glucose-regulated protein 78.
p < 0.05.
Co-localization of Par-4 with GRP78 in the ER of SK-NEP-1 cells
In a large number of human solid tumors, the expression of endogenous Par-4 is apparently downregulated, and this has also been verified in nephroblastomas. Therefore, pEGFP-C1-Par-4 plasmids were transfected into the nephroblastoma cell line SK-NEP-1 to promote Par-4 expression; pEGFP-C1 plasmids were transfected into the control group of cells. The transfection efficiency in the control group and pEGFP-C1-Par-4 group was determined to be 70% using fluorescence microscopy (Figure 2(a)). The results revealed that Par-4 co-localized with calnexin, an ER marker. GRP78 was also found to co-localize with calnexin. These findings indicate that Par-4 binds to GRP78 in the ER (Figure 2(b)).

Transfection of SK-NEP-1 cells with the pEGFP-C1-Par-4 plasmid and co-localization of Par-4 with GRP78 in the endoplasmic reticulum. (a) Transfection efficiency observed by fluorescence microscopy. The pEGFP-C1-Par-4 (Par-4 overexpression) or pEGFP-C1 (control plasmid) plasmid was transfected into SK-NEP-1 cells. The efficiency of transfection was evaluated at 48 h to be almost 70% by fluorescence microscopy. The images on the right are representative of the same field, as observed under an optical microscope. (b) Immunofluorescence assay showing the localization of Par-4 and GRP78 in the SK-NEP-1 cell line under a confocal microscope. At 48 h after transfection of the pEGFP-C1-Par-4 plasmid, the SK-NEP-1 cells were fixed and double-stained with antibodies against Par-4 (green fluorescence) and calnexin (red fluorescence) or GRP78 (green fluorescence) and calnexin (red fluorescence). DAPI (blue fluorescence) in the images represented the stained nuclei, and the merged images (yellow fluorescence) corroborated the co-localization of Par-4 and GRP78.
Upregulation of ATF4 and BAX expression in SK-NEP-1 cells transfected with the pEGFP-C1-Par-4 plasmid via activation of the ER apoptosis pathway
As reported by recent studies, ectopic Par-4 co-localizes with GRP78 at the plasma membrane and induces ERS response, which results in the translocation of GRP78 from the ER to the cell surface and further enhances ERS. As shown in Figure 3(a), western blot analysis confirmed significant upregulation of GRP78 by extracellular Par-4. Moreover, we noted that activation of the ER apoptosis pathway via the interaction of Par-4 with GRP78 resulted in a significant increase in the expression of ATF4 and BAX on the ER (Figure 3(a) and (b)).
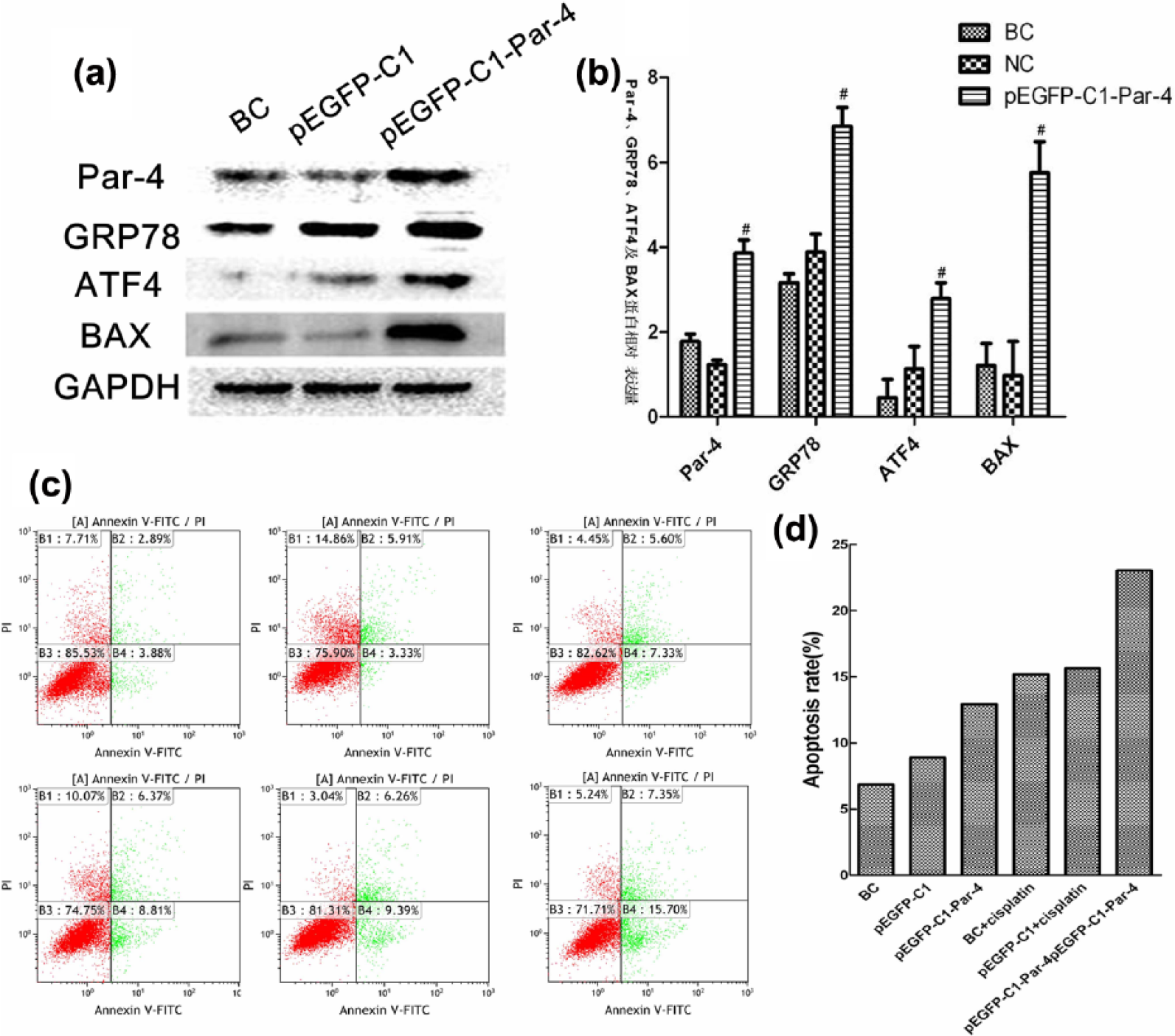
Upregulation of the expression of ATF4 and BAX and increase in the apoptosis rate in SK-NEP-1 cells transfected with the pEGFP-C1-Par-4 plasmid and treated with cisplatin. (a and b) Activation of the ER apoptosis pathway significantly increased the expression of ATF4 and BAX in the ER. Western blot analyses revealed that the SK-NEP-1 cells were successfully transfected with the pEGFP-C1-Par-4 plasmid. Moreover, we also found significantly higher expression of GRP78, ATF4, and BAX in the pEGFP-C1-Par-4 group than in the pEGFP-C1 group and blank control (BC) group, even though there was no significant difference in the expression of GRP78, ATF4, and BAX between the pEGFP-C1 group and BC group. (c and d) Transfection with the pEGFP-C1-Par-4 plasmid increased chemosensitivity to cisplatin, as depicted by flow cytometry analysis. The apoptosis rate of SK-NEP-1 cells was measured by flow cytometry analysis using Annexin V–FITC/PI staining. The apoptosis rate in the pEGFP-C1-Par-4 + cisplatin group (23.05%) was significantly higher than that in the BC group (6.77%) and BC + cisplatin group (15.18%).
Increase in the apoptosis rate of SK-NEP-1 cells by transfection of the pEGFP-C1-Par-4 plasmid and cisplatin treatment
We evaluated the apoptosis rate of SK-NEP-1 cells, which were transfected with the pEGFP-C1-Par-4 plasmid, treated with cisplatin, or subjected to a combination of both treatments. These groups (BC, pEGFP-C1, pEGFP-C1-Par-4, BC + cisplatin, pEGFP-C1 + cisplatin, pEGFP-C1-Par-4 + cisplatin) were treated for 48 h and were then subjected to flow cytometry to detect labeled Annexin V–FITC/propidium iodide (PI). We found that the apoptosis rate of SK-NEP-1 cells treated with the pEGFP-C1-Par-4 plasmid and cisplatin was significantly higher than that of cells in the other groups (Figure 3(c) and (d)). This finding indicated that combining Par-4 overexpression with cisplatin was highly efficient in inducing cellular apoptosis in the SK-NEP-1 cells.
Inhibition of Wilms’ tumor growth via Par-4-induced sensitization to cisplatin
Since our in vitro experiments showed that Par-4 sensitizes WT SK-NEP-1 cells to cisplatin, we tried to investigate the in vitro effects of Par-4 in a mouse xenograft model. The pretreament and posttreament volume of the transplanted tumors in the Par-4 + cisplatin group, Par-4 group, cisplatin group, negative control Par-4 group, and BC groups are shown in Table 2. In the Par-4 + cisplatin, Par-4, and cisplatin groups, tumor growth was remarkably restrained compared to the negative control Par-4 and BC groups. The tumor volume in the Par-4 + cisplatin group was the lowest, and it could be validated based on the growth curve of the volume of the transplanted tumors (Figure 4). We also observed that the weight of tumor tissues in the Par-4 + cisplatin, Par-4, and cisplatin groups was lower than that in the negative control Par-4 and BC groups (Table 3). As shown in Table 3, the tumor inhibition rate in the Par-4 + cisplatin group was the most prominent.
The volumes of the transplanted tumors before and after treatment.

BC: blank control.
p < 0.05.

Volume of the transplanted tumors in each group. The growth curve of the transplanted tumors in response to treatment with PBS, adenovirus-mediated Par-4, and cisplatin is shown here. The results showed that the volume of the transplanted tumors in the Par-4 + cisplatin group was obviously suppressed compared with the negative control Par-4 group or BC group. The transplanted tumors treated with adenovirus-mediated Par-4 or cisplatin alone also showed restrained growth.
Tumor weight and growth inhibition of nude mice xenografts on the 22nd day.

BC: blank control.
p < 0.05;**p < 0.01.
H&E staining of the transplanted tumor tissues (Figure 5(A)) showed that tumor necrosis regions were seldom observed in the negative control Par-4 and BC groups under the microscope. However, enlarged and hyperchromatic nuclei and an increase in the nucleus-to-cytoplasm ratio were observed. Moreover, necrotic areas and apoptosis caused by adenovirus-mediated Par-4 or cisplatin were observed in the Par-4 and cisplatin groups.
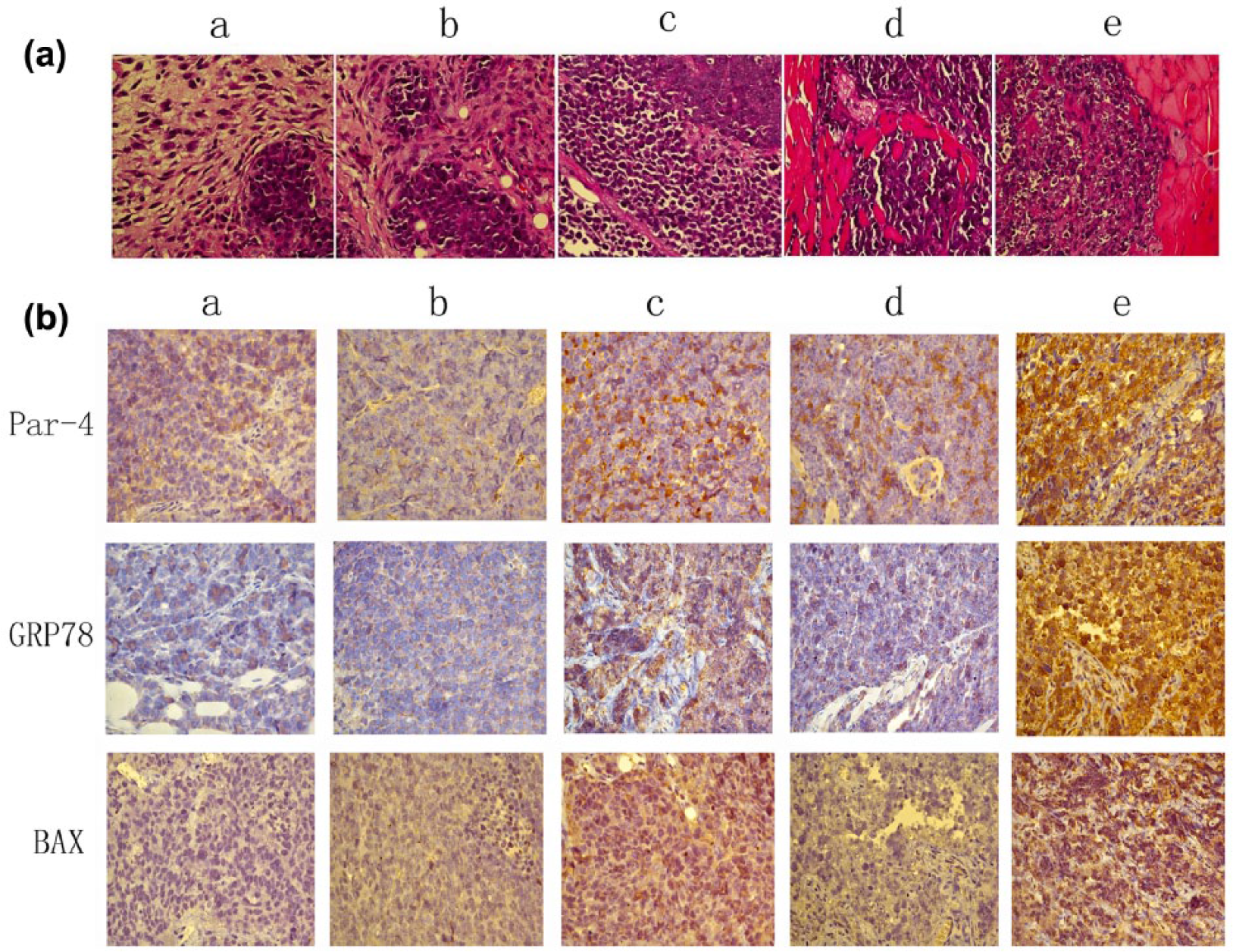
Hematoxylin–eosin (H&E) staining and immunohistochemical analysis of the transplanted tumor tissues. (A) H&E staining of nude mice xenografts in each group. The nude mice xenografts were divided five groups (a: BC, b: negative control Par-4, c: Par-4, d: cisplatin, and e: Par-4 + cisplatin), and the tumor tissues were stained with H&E and observed under 400× magnification. (B) Immunchistochemical method to detect the expression of Par-4, GRP78, and BAX in transplanted tumors. In five groups (a: BC, b: negative control Par-4, c: Par-4, d: cisplatin, and e: Par-4 + cisplatin), the transplanted tumor tissue was immunohistochemically stained to analyze the expression of Par-4, GRP78, and BAX (magnification: 400×). The brown-yellow granules represented stained proteins.
The mean density was calculated using Image-Pro Plus 6.0. The results showed that the mean densities of Par-4, GRP78, and BAX were significantly higher in the Par-4 + cisplatin, Par-4, and cisplatin groups than in the negative control Par-4 or BC group (Figure 5(B), Table 4). However, there was no statistically significant difference in the mean density of GRP78 between the cisplatin and BC groups (Table 4), which further confirmed that ectopic Par-4 stimulated overexpression of GRP78.
The mean density of Par-4, GRP78, and BAX in transplanted tumor of each group.

Par-4: prostate apoptosis response 4; GRP78: glucose-regulated protein 78; BC: blank control.
p < 0.05;**p < 0.01.
Discussion
In this study, we have shown that Par-4 overexpression and cisplatin treatment promotes apoptosis in the Wilms’ tumor cell line SK-NEP-1 and boosts sensitivity to apoptosis induced by cisplatin. Moreover, this combined treatment was also found to reduce in vivo growth of xenograft tumors.
Our study also confirmed that Par-4 and GRP78 co-localized in the ER. The SK-NEP-1 cells, which were transfected with the Par-4 plasmid, could elicit ERS, which has also been observed in other types of tumor cells.15–17 ERS is closely associated with the combination and decomposition of GRP78 in the ER. Severe and continuous ERS can trigger cellular functional dysfunction and even apoptosis. The ER stress–related apoptosis pathway leads to the apoptosis of tumor cells by upregulation of the pro-apoptosis gene BAX.18–20 This may explain why BAX expression was upregulated in the cells transfected with the Par-4 plasmid. The upregulation of these proteins was confirmed by western blot analysis.
To induce overexpression of Par-4, the pEGFP-C1-Par-4 plasmid was successfully transfected into SK-NEP-1 cells. The cells transfected with the Par-4 overexpression plasmids grew adhering to the wall more slowly, and more cells were found floating in the culture medium than in the pEGFP-C1 control group. Flow cytometry analysis verified that Par-4 overexpression and cisplatin worked in synergy to inhibit SK-NEP-1 cell growth and induced cellular apoptosis. Similar findings were obtained in a nude mouse model of Wilms’ tumor.21,22 The in vivo results confirmed that overexpression of Par-4 could inhibit the growth of nude mice xenografts.16,23,24 Moreover, the anti-neoplastic effects were remarkably obvious in the group treated with a combination of Par-4 and cisplatin.
In summary, our findings indicate that combined treatment with ectopic Par-4 and cisplatin suppressed the growth of human Wilms’ tumor cells in vitro and in vivo and that the effect might be associated with the activation of the ER apoptosis pathway and the interaction between extracellular Par-4 and GRP78. Thus, this combined therapeutic strategy may have potential for the treatment of Wilms’ tumor.
Footnotes
Acknowledgements
J.W. and Y.L. contributed equally to this work.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by the National Natural Science Foundation of China (Grant number: 81170487).
