Abstract
Oral squamous cell carcinoma is one of the most common neoplasm in the world. Despite the improvements in diagnosis and treatment, the outcome is still poor now. Thus, the development of novel therapeuticapproaches is needed. The aim of this study is to assess the synergistic anti-tumor effect of andrographolide with cisplatin (DDP) in oral squamous cell carcinoma CAL-27 cells in vitro and in vivo. We performed Cell Counting Kit-8 proliferation assay, apoptosis assay, and western blotting on CAL-27 cells treated with andrographolide, DDP or the combination in vitro. In vivo, we also treated CAL-27 xenografts with andrographolide or the combination, and performed terminal deoxynucleotidyl transferase–mediated deoxyuridine triphosphate nick-end labeling assay and immunohistochemical analysis of Ki-67. The results showed the combination of andrographolide and DDP synergistically inhibited CAL-27 cell proliferation in vitro and caused tumor regression in vivo in the CAL-27 xenografts. In addition, the synergistic anti-tumor effect of andrographolide with synergistic was due to an enhanced apoptosis. Moreover, the combination therapy upregulated the expression level of p-p53 in vitro and decreased Ki-67 expression in vivo. Our data indicate that the combination treatment of andrographolide and DDP results in synergistic anti-tumor growth activity against oral squamous cell carcinoma CAL-27 in vitro and in vivo. These results demonstrated that combination of andrographolide with DDP was likely to represent a potential therapeutic strategy for oral squamous cell carcinoma.
Keywords
Introduction
Oral squamous cell carcinoma (OSCC) is one of the most common neoplasms worldwide, with increasing incidence in Asian countries in the past decade. 1 According to the GLOBOCAN estimates 2012, there were approximately 300,373 new cases of lip/oral cavity cancer in the world (4.0 per 100,000), and in the south-east Asia region, the estimated age-standardized rate (ASR (world)) for lip/oral cavity cancer is the highest (6.4 per 100,000). 2 Current oral cancer therapy is always surgery and then chemotherapy and/or radiotherapy. Cisplatin (DDP), which induces cytotoxicity through the formation of DDP-DNA adducts, is the front-line clinical chemotherapy for OSCC. 3 Unfortunately, the prognosis of OSCC was still poor; the 5-year overall survival rate is no more than 50%. 4 The reason is considered to be drug resistance and numerous undesirable side effects of DDP. Therefore, studies have focused on developing new therapeutic strategies, including combinatorial drug regimens for OSCC treatment. Yasukawa et al. 5 reported that combination therapy of DDP with AZD2281, a poly(ADP-ribose) polymerase (PARP) inhibitor, showed synergetic anti-carcinoma effects in vitro (HSC-2, Ca9-22, and SAS cell lines) and enhanced suppressive effects against the growth of HSC-2 xenograft in vivo.
Andrographolide (Andro) is a diterpenoid lactone isolated from the traditional herbal medicine Andrographis paniculata, which has been widely used for treatment of sore throat, fever, diarrhea, and inflammatory disorders. 6 Andro possesses various biological activities, including anti-inflammatory, immunomodulatory, antiviral, and antitumoral effects. In recent years, Andro has been reported to retard cell proliferation and induce apoptosis in many kinds of cancer cells, including C6 glioma cells, 7 TD-47 human breast cancer cells, and B16F-10 melanoma cells.8,9 These data suggested the potential novel application of Andro in cancer therapy.
The transcription factor p53 has been shown to play a key role in tumor prevention. Depending on the cell and tissue type, p53 regulates cell cycle arrest, DNA repair, apoptosis, or senescence to maintain genomic stability and prevent tumor formation. 10 p53 protein mutations are present in almost all tumors including OSCC. 11 Zedan et al. 12 reported that OSCC tumor samples showed a positive staining with the immunohistochemical expression of p53 protein, indicating p53 gene mutations would be used for a prognostic marker in OSCC patients.
In this study, we assessed the combinatorial effect of Andro and DDP in oral tongue squamous carcinoma cell line in vitro and xenograft tumor model in vivo. Andro showed synergistic anti-carcinoma effects with DDP in vitro and enhanced the suppressive effects of DDP against the growth of xenografts in vivo. We also examined the p53 expression levels using western blotting to find out the molecular mechanism of Andro and DDP treatment. Our results revealed a potential modulating role of Andro for OSCC therapy in addition to conventional chemotherapy.
Materials and methods
Chemicals
Purified Andro (Cat. no. 365645) and DDP were purchased from the Sigma-Aldrich Chemical Co. (St. Louis, MO, USA). The AKT, phospho-AKT (p-AKT and Ser 473), p53, and phospho-p53 (p-p53 and Ser 15) antibodies were purchased from Cell Signaling Technology (Beverly, MA, USA). All reagents were of analytical grade and were used without further purification.
Cell line and culture
The human tongue squamous cell carcinoma cell line (CAL-27) was obtained from American Type Culture Collection (ATCC, Rockville, MD, USA). The cells were thawed and maintained in Dulbecco’s Modified Eagle’s Medium (DMEM; Thermo Fisher Scientific, Waltham, MA, USA) and 10% fetal bovine serum (Thermo Fisher Scientific), with the addition of penicillin (50 U/mL) and streptomycin (50 µg/mL). The cells were cultured at 37°C with 5% CO2 in a constant temperature cell incubator. CAL-27 cells are epithelial and polygonal with a highly granular cytoplasm, which is not sensitive to DDP treatment. Therefore, we used CAL-27 cell line for investigating DDP combination treatment.
Cell survival assay
Cell survival rate was assessed by the Cell Counting Kit 8 (CCK-8; Dojindo Laboratories, Kumamoto, Japan). The cells were digested and seeded into 96-well plates, each well containing 100 µL of the cells with the density of 1 × 104 cells/mL. Then, cells were treated with Andro (0, 2, 4, 8, 16, and 32 µM), DDP (0, 50, 100, 200, 400, and 800 nM), or increasing concentrations of DDP in combination with 16 µM Andro. After 48 h, 10 µL of CCK-8 solution was added to each well and incubated at 37°C for 3 h. Optical density (OD) was determined at a wave-length of 450 nm by a spectrophotometer (Microplate Reader 550; Bio-Rad, Hercules, CA, USA). We performed combination index (CI) analysis in order to evaluate the synergy between two drugs based on Chou–Talalay method. 13 Wherein, synergy is defined when a CI value less than 0.7, and a decreasing CI values meaning better synergy.
Assessment of cell morphology
Cells were cultured and treated with 16 µM Andro, 200 nM DDP, or both for 48 h. After that, cell morphology was determined by examining the culture cell without preliminary fixation under inverted electron microscope at magnification of 100×. The micrographs were recorded using a Nikon phase-contrast microscope (Tokyo, Japan).
Apoptosis detection assay
Cellular apoptosis was detected according to the protocol of R&D TACS® Annexin V-FITC Kit, containing identified Annexin V-FITC and propidium iodide (PI) in binding buffer. Annexin V binds to the phosphatidylserine (PS) in the early apoptosis, while PI is a marker of late apoptotic and necrotic cells. First, cells were seeded and incubated with 16 µM Andro, 200 nM DDP, or both. After 48 h, the cells were harvested by trypsinization, washed twice with cold phosphate-buffered saline (PBS), and diluted to 1 × 106 cells/mL in 1× binding buffer. Then, 5 µL of Annexin V and PI solution was added to every 100 µL of cell suspension (about 1 × 105 cells). Cells were gently mixed and incubated at room temperature (RT) in the dark for 15 min. Each tube was added with 400 µL of 1× binding buffer. Finally, cells were sorted by flow cytometry on FACScan (Becton Dickinson, Franklin Lake, NJ, USA) within 1 h and then analyzed by FCS Express 4 software.
Western blotting
Cells were harvested and lysed in radioimmunoprecipitation assay (RIPA) buffer (1% Triton X-100, 0.1% sodium dodecyl sulfate (SDS), 1% sodium deoxycholate (DOC), 10 mM Tris-HCl pH 7.4, 150 mM NaCl, 5 mM ethylenediaminetetraacetic acid (EDTA), 10 µg/mL leupeptin, and 1 mM Na3VO4) with protease inhibitors (Sigma-Aldrich, St. Louis, MO, USA). Protein concentration was determined using the bicinchoninic acid (BCA) protein assay kit (Promega, Madison, WI, USA). The protein samples (20 µg) in loading buffer were separated on 10% SDS polyacrylamide gel electrophoresis (PAGE) and transferred to polyvinylidene fluoride (PVDF; Bio-Rad Laboratories, Hercules, CA, USA). The membranes were blocked with 5% (w/v) non-fat milk in Tris buffered saline with Tween 20 (TBST) for 1 h and incubated with antibodies against AKT, p-AKT, p53, and p-p53 (1:1000 dilution; Cell Signaling Technology) overnight at 4°C. After incubation with appropriately diluted horseradish peroxidase (HRP)-conjugated secondary antibodies (1:2000 dilution), the immunoreactive protein bands were visualized using a chemiluminescent substrate (ECL Kit; Amersham Biosciences Corp, Piscataway, NJ, USA). The density of each protein band was normalized to β-actin.
In vivo tumor xenograft study
Female BALB/c-nude mice provided by Vital River Laboratories Co., Ltd (Beijing, China) weighing about 20 g at 6–8 weeks old were used in this study for tumor model establishment. All animals were maintained in a controlled animal facility with a 12-h light–dark cycle; 2 × 106 CAL-27 cells in 200 µL growth medium were injected into the dorsal skin subcutaneously. Once the tumor volume had reached about 150 mm3, 24 mice were randomly divided into four groups and treated as follows: (1) saline (vehicle, oral, and once daily); (2) Andro at 50 mg/kg (oral and once daily); (3) DDP at 5 mg/kg (intraperitoneal and once weekly); and (4) combination of (2) and (3) for 3 weeks. The tumor volume and body weight were measured at 3-day intervals for 3 weeks. 14 The mice were sacrificed at the end of 21 days of treatment period, and the tumors were resected to perform immunohistochemistry. The tumor volume was calculated using the following equation: tumor size = length × width2 × 0.5. Tumors were resected and immediately fixed in 10% formalin/PBS, followed by immersion in 70% alcohol and embedding in paraffin; 4-µm-thick sections were cut and mounted on silane-coated microscope slides.
Terminal deoxynucleotidyl transferase–mediated deoxyuridine triphosphate nick-end labeling assay
Slides were deparaffinized in xylene three times for 5 min and rehydrated with descending concentrations of ethanol. Terminal deoxynucleotidyl transferase–mediated deoxyuridine triphosphate nick-end labeling (TUNEL) assay was used to detect the DNA strain breaks. 15 The tissue sections were stained using the Click-iT™ TUNEL Colorimetric IHC Detection Kit (Thermo Fisher Scientific, USA) as per the manufacturer’s instructions. Apoptotic and necrotic cells were stained with 1× 3,3′-diaminobenzidine (DAB) reaction mixture supplied by the kit. The apoptotic cell nuclei were stained in brown.
Immunohistochemistry
Another tissue sections were used for immunohistochemistry staining of Ki-67. Ki-67 can be detected in phases G1, S, G2, and M of the cell cycle, but not on G0 phase, which makes the Ki-67 protein a reliable marker of proliferating cells. 16 The deparaffinized and dehydrated slides were heat-treated with citrate buffer (pH 6.0) to retrieval antigen and washed with 3% H2O2 in 1× TBS to block endogenous peroxidase activity. After that, the sections were incubated with a Ki-67 antibody (dilution 1:200; Cell Signaling Technology) overnight at 4°C and a biotinylated secondary antibody for another 30 min. Avidin–biotin–peroxidase complex (Dako LSAB2 System; Dako Co., Produktionsvej, Denmark) was added, and the color was developed using DAB. Counterstaining was performed with hematoxylin. The sections were viewed under a BX51 System Microscope (Olympus, Tokyo, Japan). Images were recorded using a digital microscope camera (DP70; Olympus).
Statistical analysis
All data and results presented are representative of, or calculated from, at least three independent experiments. The data were expressed as mean ± SD. The significance of difference was evaluated with one-way analysis of variance (ANOVA), followed by Student’s t-test to statistically identify differences between the control and treated groups. A p value of less than 0.05 was considered to indicate a statistically significant result.
Results
Andro and DDP synergistically reduced CAL-27 cell proliferation
CCK-8 assay was used to assess the anti-proliferation effect of Andro and/or DDP on CAL-27 cells. Cells were treated with different concentrations of Andro, DDP, or the combination of both drugs for 48 h. Figure 1(a) showed that Andro (from 2 to 32 µM) exerted weak toxicity on cell proliferation, while DDP alone inhibited the cell survival rate in a dose-dependent manner (Figure 1(b)). The IC50 of treatment with DDP alone was 218 nM, while Andro at non-toxic dose (16 µM) enhanced the anti-proliferation effect induced by DDP. The cell survival rate was significantly reduced when treated with combination of Andro (16 µM) and various concentrations of DDP (Figure 1(b)). Similarly, based on morphological examination using an inverted electron microscope, decreased cell number was observed upon drug treatments, especially in the Andro/DDP combination treatment group (Figure 1(c)), which is consistent with the result of CCK-8 assay. The result of CI value evaluation also indicated that co-treatment of Andro and DDP had a synergistic anti-proliferation effect on CAL-27 cells (Table 1).

Andro and DDP synergistically reduced CAL-27 cell proliferation. CAL-27 cells were treated with (a) 0–32 µM Andro or (b) 0–800 nM DDP alone or in combination with 16 µM Andro for 48 h. Cell survival rate was analyzed by CCK-8 assay. Values are expressed as mean ± SD (n = 3). (c) Representative microscopy images captured showing the effect of cells treated with (1) vehicle, (2) 16 µM Andro, (3) 200 nM DDP, and (4) 16 µM Andro + 200 nM DDP for 48 h (magnification 100×).
The CI value evaluation of DDP alone treatment or DDP plus Andro using Chou–Talalay method.

CI: combination index.
The concentration of DDP ranged from 0 to 800 nM.
Andro enhanced DDP-induced CAL-27 cell apoptosis
In order to evaluate the enhanced effect of Andro on the DDP-induced apoptosis in CAL-27 cells, flow cytometry was performed to quantify the cell apoptotic rate. The results revealed that Andro/DDP combinatorial treatment significantly increased the portion of apoptotic cells, compared to either treatment alone (Figure 2(a)). Andro-alone treatment showed no significant increase in apoptotic cell fraction. As shown in Figure 2(b), control group did not show any apoptosis, and the percentage of early apoptotic and late apoptotic cells was only 4%. After treated with 16 µM Andro, 200 nM DDP, or the combination, the corresponding quantities were 18%, 39% (p < 0.05), and 47% (p < 0.01), compared to vehicle group. These data indicated that Andro alone had a very limited CAL-27 cell growth inhibition, but it significantly enhanced the apoptotic cell death induced by DDP.

Andro enhanced CAL-27 cell apoptosis induced by DDP. (a) CAL-27 cells were treated with Andro, DDP, or both for 48 h and subsequently stained with Annexin V/PI for cell sorting under flow cytometry. (b) Percentage of cells undergoing early apoptosis (right lower quadrant) and late apoptosis (right upper quadrant) were analyzed by FCS Express 4 software. Values are expressed as mean ± SD (n = 3; *p < 0.05 and **p < 0.01 vs DMSO group).
Andro and DDP combinatorial treatment upregulated p-AKT and p-p53 levels in CAL-27 cells
We next investigated the mechanism of the synergetic effects of Andro and DDP in CAL-27 cells by analyzing the protein levels using western blotting. The transcription factor p53 has been shown to induce apoptosis by causing mitochondrial dysfunction. It is reported that a high incidence of p53 protein mutations exists in OSCCs. 17 The data indicated that the protein level of p-p53 was increased in the DDP group and further enhanced in the combination group, while that of p53 was no different. Andro alone had almost no effect on the expression of p-p53 (Figure 3(a) and (b)), which was consistent with cell proliferation results. We also tested the p-AKT and total AKT levels. The data revealed that p-AKT was elevated, while AKT was not affected by the same treatment (Figure 3(a) and (b)).

Western blotting analysis of p-AKT and p-p53 protein levels in CAL-27 cells. (a) CAL-27 cells were treated with Andro or DDP or both for 48 h and then lysed in RIPA buffer and subjected to western blotting analysis to detect p-AKT, AKT, p-p53, and p53 protein expression. (b) Normalized protein expression levels of p-AKT, AKT, p-p53, or p53 separated with western blotting. Values are expressed as mean ± SD (n = 3).
In vivo effects of Andro and DDP on CAL-27 xenograft tumor growth
To evaluate the clinical application of Andro and/or DDP for OSCC, the effects of Andro and/or DDP on the in vivo tumor growth of CAL-27 xenografts were tested in a subcutaneous xenograft tumor model. The dose selection was made according to the study by Lin et al. 14 The results indicated that tumor volume of control group mice increased during the experimental period. Moreover, the tumor growth of DDP group was significantly inhibited comparing to the control group and that of combination group was further decreased. However, the inhibitory effect of Andro on tumor growth was very weak (Figure 4(a)). After treatment for 21 days, average tumor weights were 1.79 ± 0.20, 1.58 ± 0.18, 0.95 ± 0.12, and 0.62 ± 0.10 g in vehicle, Andro, DDP, and combination group, respectively (Figure 4(b) and (c)). Thus, Andro (50 mg/kg, once daily) and DDP (5 mg/kg, once per week) combinatorial treatment was considered to be effective in the inhibitory growth of CAL-27 xenograft model in vivo. This is consistent with the results from in vitro assay. The body weights of the mice were not significantly different in all treatment groups compared with vehicle (Figure 4(d)), thus confirming that the used treatment protocol was tolerable.
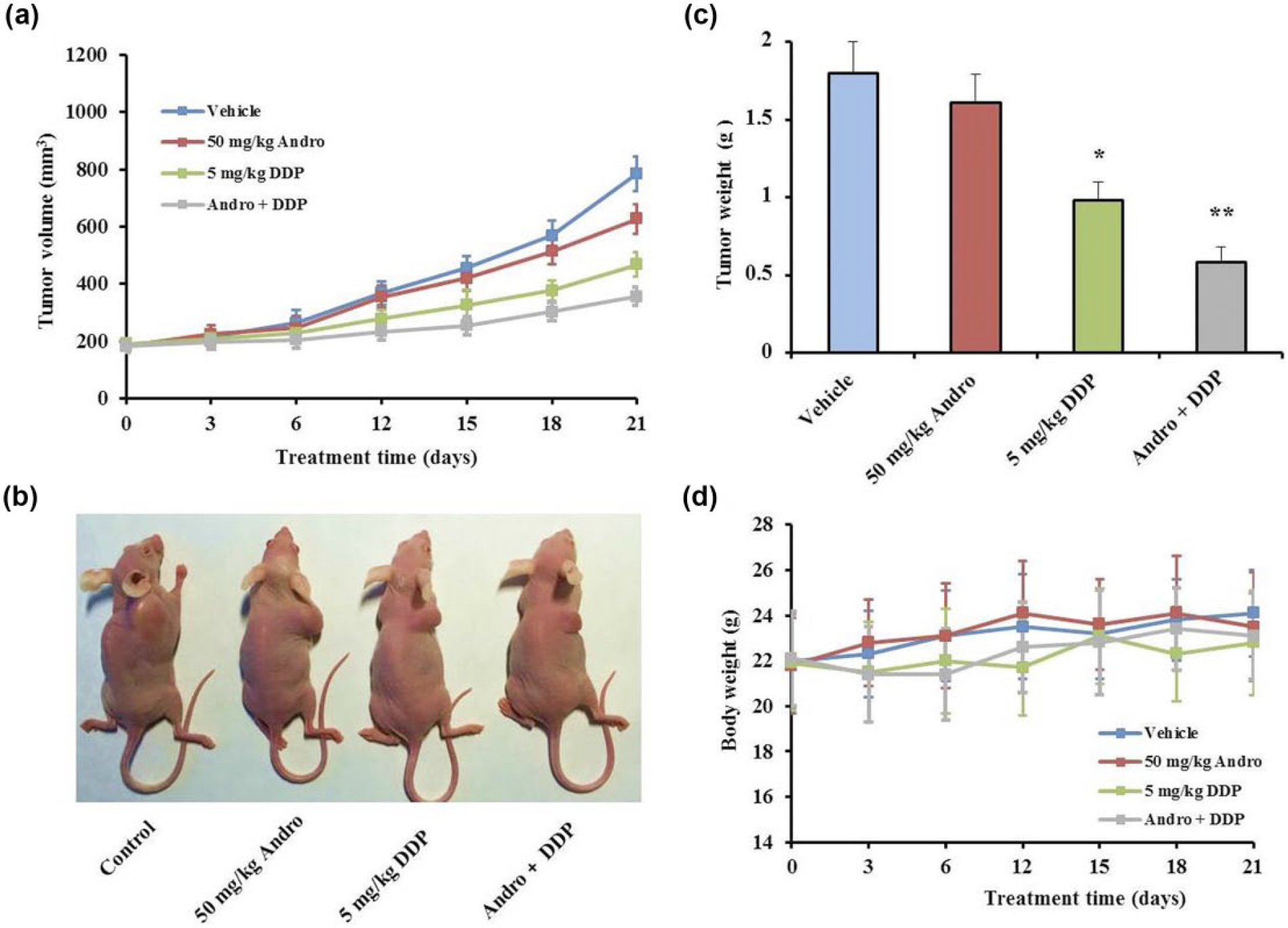
Combinatorial effect of Andro and DDP on CAL-27 xenograft growth in nude mice. Tumor-bearing nude mice were randomly separated into four groups: saline (oral and once daily), Andro at 50 mg/kg (oral and once daily), DDP at 5 mg/kg (intraperitoneal and once weekly), and combination of Andro and DDP for 3 weeks. The body weight and tumor size were monitored at 3-day intervals. (a) The tumor volumes of xenografts during treatment period. (b) In the end of study, the mice were sacrificed and taken pictures. (c) The tumors were isolated from mice and weighted (*p < 0.05 and **p < 0.01 vs vehicle group). (d) The body weight of nude mice in each group. Values are expressed as mean ± SD (n = 6).
The effect of combinatorial treatment of Andro and DDP significantly on TUNEL and Ki-67 expression in CAL-27 xenografts
Tumors were removed from mice after treatments, and the numbers of apoptotic cells were quantified by the TUNEL assay. In the control group, only a few TUNEL-positive apoptotic cells were observed by microscopy, while strong apoptosis was observed in tumor cells in the DDP group. In combination group, Andro enhanced the TUNEL-positive cells induced by DDP comparing to vehicle group (p < 0.01, Figure 5(a) and (b)). The synergetic anti-tumor effect of Andro and DDP in mice tumor was further confirmed by immunohistochemistry staining of Ki-67 antibody. It is reported that expression of Ki-67 antigen was higher (70%) in OSCC patient, 18 which makes Ki-67 a potential biomarker of carcinogenesis in OSCC. Ki-67 was widely observed in mice tumors of the control group (61%), while it was significantly reduced in DDP group to 17% comparing to vehicle group (p < 0.01). Consistent with the highest sensitivity of combination treatment in TUNEL assay, Ki-67 expression was decreased by combinatorial treatment of Andro and DDP to 9%, compared with the vehicle group (p < 0.01, Figure 6(a) and (b)).

TUNEL staining of CAL-27 tumor tissues in control, Andro, DDP, or combination group. TUNEL-positive cells were stained in brown (scale bar = 50 µm). (a) Representative photographs of TUNEL staining.

The effect of Andro and/or DDP on Ki-67 expression in CAL-27 tumors. (a) Representative immunohistochemistry photographs showing Ki-67 expression in CAL-27 xenografts. Ki-67 antigen was stained with brown (scale bar = 50 µm). (b) Percentage of Ki-67-positive cells per field are expressed as mean ± SD (n = 3; **p < 0.01 vs vehicle group). The Ki-67-positive cells were calculated by ImageJ software.
P-AKT and p-p53 levels were also upregulated by the combinatorial treatment in CAL-27 tumor tissues
Tumors were removed from mice after treatments, and p-AKT and p-p53 expression levels were detected by western blotting. Similar to in vitro results, p-AKT and p-p53 expression was upregulated by DDP alone and further enhanced by the combination treatment. However, Andro had no effect on the protein expressions (Figure 7(a) and (b)). The data revealed that the synergistic anti-tumor effect of Andro may be due to p-AKT and p-p53 upregulation, at least in part.
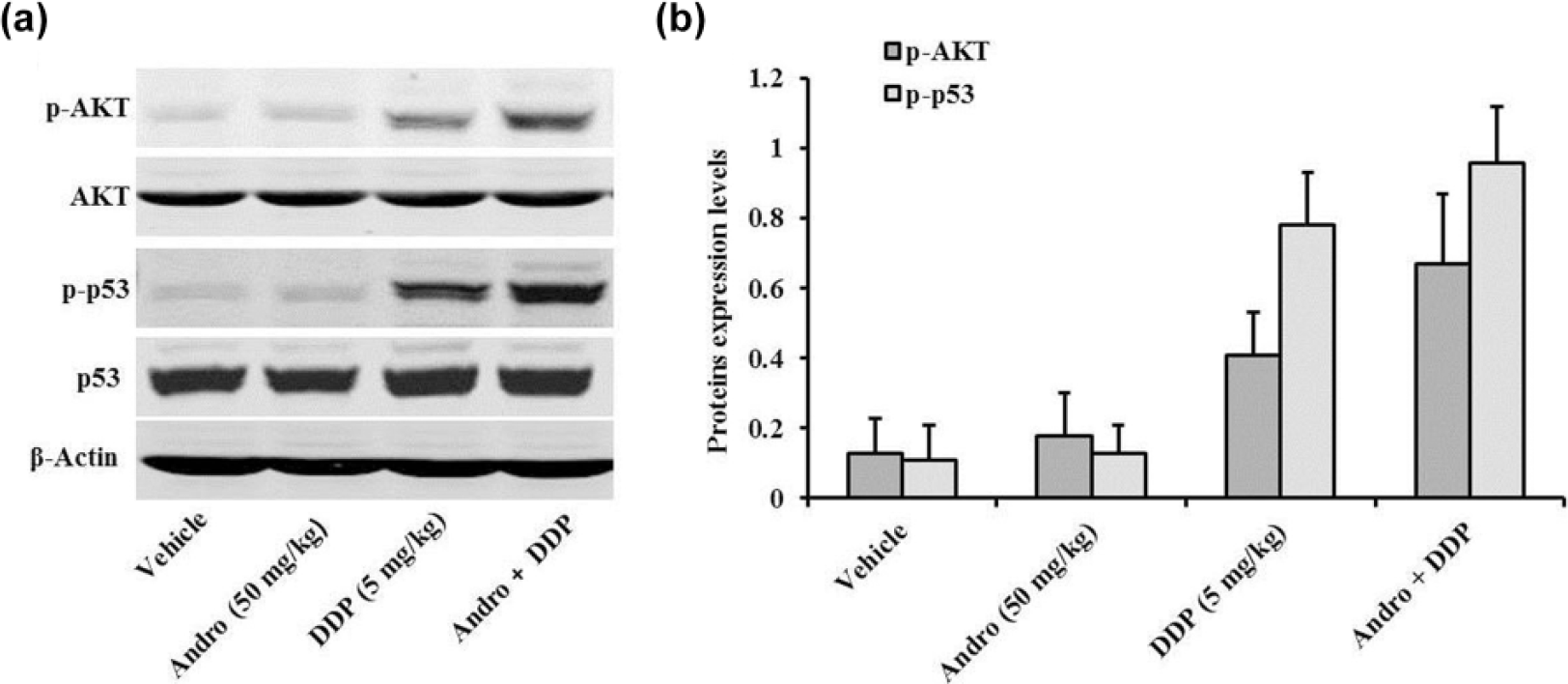
Western blotting analysis of p-AKT and p-p53 protein levels in CAL-27 xenografts. (a) In the end of in vivo study, the tumor-bearing mice were scarified and the tumors were detected by western blotting. (b) Normalized protein expression levels of p-AKT, AKT, p-p53, or p53 separated by western blotting. Values are expressed as mean ± SD (n = 3).
Discussion
Andro is the major component of Andrographis paniculata extract with cytotoxic activity. 19 Andro has been reported to inhibit the in vitro proliferation of various kinds of tumor cell lines. The IC50 values are around 5–15 µM. 20 About OSCC, Wang et al. 21 demonstrated that Andro suppressed squamous cell carcinogenesis induced by 9,10-dimethyl-1,2-benzanthracene (DMBA) in the hamster model, and it also inhibited growth and proliferation of Tb cells (a human tongue squamous cell carcinoma cell line). In our study, Andro was used alone or in combination with DDP to treat CAL-27 cells or nude mouse xenografts model. Inconsistent with previous studies, Andro alone (2–32 µM) showed very weak activity on CCK-8 proliferation assay and apoptosis assay in vitro. In the xenograft tumor model experiments, Andro also showed very weak inhibitory effect on tumor growth and apoptosis. When Andro was used in combination with DDP, it potentiated the anti-carcinoma effects induced by DDP both on in vitro and in vivo assays.
In recent decades, many Chinese scientists have found that Andro could sensitize the anti-carcinoma effect of classical chemotherapeutic agents when used in combination with these drugs. Zhou et al. 22 found that Andro enhanced doxorubicin-induced cytotoxicity via promoting caspase-dependant apoptosis pathway in four different kinds of cancer cell lines. Guo et al. 23 demonstrated that Andro combined with bleomycin (BLM) was more effective than BLM alone on apoptotic cell death, and Andro dramatically alleviated the lesion in pulmonary fibrosis induced by BLM. Yuan et al. 24 revealed that the combination of Andro and paclitaxel (PTX) exerted significant synergistic anticancer effect on A549 cells in vitro and in vivo. DDP is another well-known chemotherapeutic drug for numerous human cancers, since DDP treatments are always associated with substantial side effects and drug resistance. Thereby, combination therapies of DDP with other drugs are common for cancer treatment. Lin et al. 14 proved that Andro in combination with DDP had synergistic effect on the anti-proliferation and apoptosis of human colorectal carcinoma Lovo cells as well as xenograft tumor model. Yunos et al. 25 also found that Andro could enhance the apoptotic cell death of resistant A2780cisR cell line toward DDP. In our study, it is the first time Andro was used in combination with DDP for OSCC treatment. Andro sensitized the cytotoxicity of CAL-27 cell line and xenograft tumor model toward DDP.
As we know, wild-type p53 has a short half-life which cannot be detected while mutations are more stable with a extended half-life that can be detected using immunohistochemical methods. Evidence showed that p53 expression had a positive correlation with the histological grade of invasive oral tongue SCC as well as tongue dysplasia. 26 P53 could be a biomarker for diagnosis of OSCC. 18 In our study, the expression of p53 is very high in the control group cells, which decreased upon drug treatment, especially in the combination treatment group. The increasing expression of p-p53 confirmed that the function of p53 protein was restored by Andro/DDP treatment. Zhou et al. 27 found that Andro sensitized DDP-induced apoptosis in human cancer cell lines via inhibition of autophagy not p53-dependent pathway. This is different from our findings.
Another interesting finding was the elevated p-AKT expression induced by Andro and/or DDP treatment. This finding suggests that AKT may be involved in a new pathway for cancer prevention. It is possible that p-p53 activation results in a feedback p-AKT activation. The molecular mechanism needs further investigation in the future.
Based on these results, Andro/DDP showed synergistic cytotoxic effect toward CAL-27 cell line and in vivo mouse model, suggesting the combination of Andro and DDP in the treatment of OSCC as novel chemotherapeutic strategy.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
