Abstract
Background
Diabetes mellitus (DM) is a persistent metabolic condition resulting from insufficient insulin or insulin resistance, which gives rise to diverse complications endangering human well-being. Ramulus Mori (Sangzhi) alkaloids (SZ-A) have various pharmacological effects, potentially benefiting clinical comprehensive kidney and cardiovascular protection. Nevertheless, the potential protective effect of SZ-A on myocardial injury in individuals with type 2 diabetes mellitus (T2DM) remains unexplored.
Materials and Methods
Sprague-Dawley (SD) rats were divided into four groups, including control, model, metformin, and SZ-A. The establishment of the type 2 diabetes model was initiated by injecting streptozotocin (STZ) along with a diet of high glucose and fat. Following a 12-week period of treatment, measurements were taken for heart mass index (HMI), fasting blood glucose (FBG), and 2-h postprandial blood glucose (2hPG). Additionally, serum glycated hemoglobin (HbA1c), indicators of myocardial injury, and oxidative stress were assessed. The expressions of mammalian target of rapamycin (mTOR), p-mTOR, beclin-1, and LC3 in myocardial tissue were detected by Western blot.
Results
The administration of SZ-A effectively reduced the levels of HMI, FBG, 2hPG, HbA1c, malondialdehyde (MDA), lactate dehydrogenase (LDH), and creatine kinase isoenzymes (CK-MB) in rats with type 2 diabetes while enhancing the activity of superoxide dismutase (SOD). Additionally, SZ-A could improve myocardial tissue arrangement structure and fibrosis degree. Additional analysis revealed that SZ-A suppressed the activation of p-mTOR while enhancing the levels of Beclin-1 and LC3, suggesting that the potential therapeutic impact of SZ-A on myocardial damage could be attributed to its ability to regulate autophagy, thereby mitigating oxidative stress.
Conclusion
In summary, the results indicate that SZ-A might possess inhibitory properties against myocardial damage in rats with type 2 diabetes, presenting a potential therapeutic approach in the clinic.
Introduction
Insulin deficiency or resistance causes diabetes mellitus (DM), which is a long-term metabolic disorder resulting in multiple complications that significantly endanger human health (He et al., 2021). In 2019, there were approximately 463 million adults (aged 20−79) worldwide diagnosed with DM, with China accounting for approximately 116.4 million of them. Meanwhile, this number of DM patients is projected to increase to 147.2 million by 2045. Myocardial injury is a prevalent and significant complication (Yan et al., 2017). Nevertheless, the precise mechanism of myocardial injury in DM remains uncertain, although it is believed to encompass oxidative stress, myocardial fibrosis, apoptosis, and autophagy (K. Li et al., 2019; Wold et al., 2005). Hence, it is imperative to investigate efficient strategies for preventing and treating myocardial injury in DM.
Autophagy is an essential biological process regulated by autophagy-related proteins that help to maintain intracellular homeostasis (Li et al., 2022). Autophagy in diabetic myocardial injury is commonly linked to factors like nutritional deficiency, hypoxia, oxidative stress, or elevated glucose concentrations (Chen et al., 2020). In addition, autophagy also has a notable impact on conditions like cardiomyopathy, heart failure, and hypertension (Mei et al., 2015). Furthermore, regulating autophagy activity is a protective mechanism in myocardial injury of DM. Researches have indicated that metformin exerts a safeguarding and anti-inflammatory impact on myocardial injury in DM by stimulating AMPK/mTOR autophagy and suppressing NLRP3 inflammasome activity (Zou et al., 2022).
The mammalian target of rapamycin (mTOR) is a crucial factor in regulating autophagy, and its activity is inhibited as autophagy increases (Qian et al., 2020). Experiments using rat models of diabetic cardiomyopathy and H9C2 cell injury caused by glucose toxicity have demonstrated that oxidative stress harm in the myocardium and H9C2 cells increases the expression of p-mTOR, resulting in the suppression of autophagy activity (Yu et al., 2018). In vivo and in vitro studies have shown that drugs such as liraglutide and NaHS can reduce p-mTOR expression, decrease oxidative stress, increase autophagy activity, and ultimately protect the heart (Yang et al., 2017).
In the prevention and treatment of myocardial injury in DM, Traditional Chinese Medicine (TCM) has crucial functions. Ramulus Mori (Sangzhi) alkaloids (SZ-A) tablets were approved by the State Administration of Medicine for treating type 2 diabetes mellitus (T2DM). According to research conducted by Liu et al. (2021), it has been found that SZ-A has a positive impact on glucose metabolism and increases insulin levels in KKAy mice. Moreover, SZ-A selectively inhibits intestinal alpha glycosidase enzymes, promotes the secretion of GLP-1, protects islet beta cells, and improves insulin resistance by regulating intestinal microecology. SZ-A possesses diverse pharmacological properties that could potentially contribute to the overall protection of the kidneys and cardiovascular system in the clinical settings (Qu et al., 2021). Nevertheless, the potential protective effect of SZ-A on myocardial injury in individuals with T2DM remains unexplored. Our hypothesis suggests that SZ-A could potentially safeguard against myocardial injury in T2DM by diminishing oxidative stress and regulating autophagy function.
Materials and Methods
Drugs and Reagents
Ramulus Mori (Sangzhi) alkaloids (SZ-A) were purchased from Shanghai Yansheng Industrial Co., Ltd. located in China. Metformin hydrochloride tablets were acquired from Sino-American Shanghai Squibb Pharmaceutical Co., Ltd. in China. Nanjing Jiancheng Bioengineering Institute in China provided assay kits to measure Glycosylated Hemoglobin (GHb), Creatine Kinase Isoenzyme (CK-MB), Lactate Dehydrogenase (LDH), Superoxide Dismutase (SOD), and Malondialdehyde (MDA). Proteintech in the USA provided primary antibodies for β-actin, mTOR, Beclin-1, and LC-3, whereas the primary antibody for P-mTOR was purchased from Arigobio in China. The secondary antibodies of anti-mouse and anti-rabbit were purchased from SeraCare in the USA.
Animals
We obtained 40 male Sprague-Dawley (SD) rats weighing 180 ± 5 g from Beijing Hua Fukang Biotechnology Co., Ltd. (SCXK (Beijing) 2020-0004), all of which were of SPF-grade. All animal experiments (2022-SY-031) were authorized by the Laboratory Animal Ethics Committee at North China University of Science and Technology.
Model of T2DM Induction and Treatment
A total of 40 male SD rats were divided into two groups, namely the control group (n = 10) and the experimental group (n = 30), using random assignment. The rats in the control group were provided with a regular diet containing 10% fat, whereas the rats in the model group were given a diet high in sugar and fat (20 kcal% protein, 35 kcal% carbohydrate, and 45 kcal% fat). After 4 weeks, streptozotocin (STZ) (30 mg/kg) was intraperitoneally injected according to body weight. The normal group rats received an intraperitoneal injection of a normal saline solution. After a period of 3 days, the levels of fasting blood glucose (FBG) and PG2h were assessed, using FBG>11.1 mmol/L or PG2h>16.7 mmol/L as the criteria according to the model proposed by King in 2012 (King, 2012).
After eliminating rats with sub-standard blood glucose, a total of 24 rats with FBG levels exceeding 11.1 mmol/L were randomly assigned to the three groups: the model group (n = 6), the metformin group (n = 6), and the SZ-A group (n = 6). According to a previous study (Yang et al., 2015), rats in the control and model groups were administered with distilled water orally, while rats in the drug treatment groups were given metformin (200 mg/kg/day) and SZ-A (40 mg/kg/day), respectively.
Blood Glucose and Biochemical Analysis
Tail-tip blood sampling was used to measure FBG and PG2h. The levels of glycated hemoglobin (HbA1c), LDH, CK-MB, SOD, and MDA (both in the serum and myocardium) were measured by using the provided assay kits’ instructions.
Heart Mass Index Determination
The rats were anesthetized using intraperitoneal injection of sodium pentobarbital at a dose of 30 mg/kg. The rat hearts were quickly removed, washed with pre-cooled saline, and weighed. The heart mass index (HMI) was calculated as HMI (mg/g−1) = heart weight/body weight.
Histopathological Examinations
Histopathological examinations were performed on the hearts by fixing them with 4% paraformaldehyde, followed by paraffin immersion and cutting into 5-µm sections after gradient ethanol dehydration. The sections were then dewaxed and dehydrated for hematoxylin & eosin (H&E) and Masson staining. The pathological structure of the myocardium and the degree of myocardial fibrosis were observed using a microscope.
Western Blotting
To perform Western blotting, 50 mg myocardial tissue was combined with 500 µL RIPA lysate in a 1.5-mL EP tube. After that, the resulting mixture was centrifuged, and the liquid portion was collected. The protein concentration of the collected supernatant was determined using the BCA protein detection kit. Following electrophoresis and electrotransfer, the samples were moved to the PVDF membrane and left to incubate overnight at 4°C with different primary antibodies (β-actin (1:2000), mTOR (1:5000), p-mTOR (1:1000), Beclin-1 (1:2000), and LC3 (1:1000)) overnight at 4°C. The TBST solution was used to wash the membranes three times, followed by incubation with secondary antibodies at a concentration of 1:10000 for 2 h at a temperature of 25°C. Protein bands were identified using a highly sensitive ECL chemiluminescence agent and a gel imaging sensor.
Statistical Analyses
Statistical analyses were performed using SPSS 22.0. Multiple groups were subjected to a one-way ANOVA analysis. To compare variances, the LSD test was employed when the variances were homogeneous, while the Tamhane’s test was utilized when the variances were not homogeneous. The experimental findings were presented as average ± standard deviation, and p < 0.05 was considered statistically significant.
Results
SZ-A Improves FBG, 2hPG, HbA1c, and HMI in Type 2 Diabetic Rats
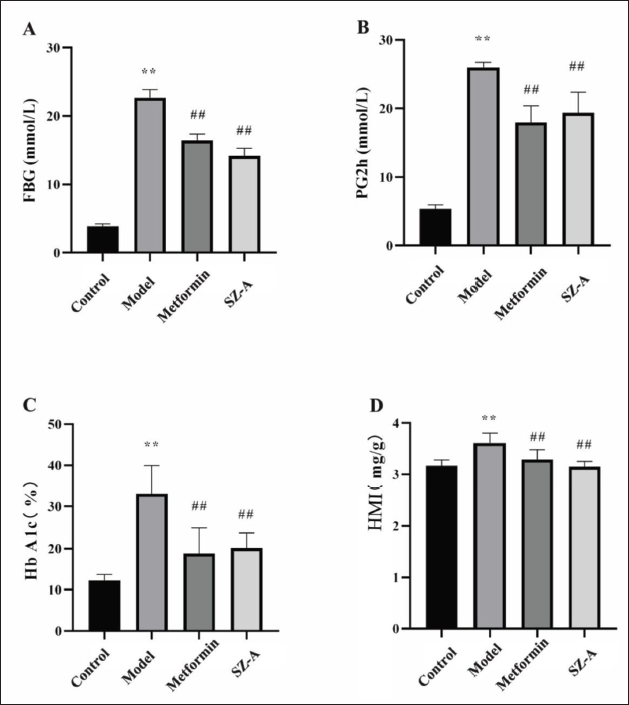
Following a 12-week period of drug intervention, the model group exhibited significantly elevated levels of FBG, 2-h postprandial blood glucose (2hPG), HbA1c, and HMI compared to the control group (p < 0.01). However, treatment with metformin and SZ-A resulted in significant reductions in FBG, 2hPG, HbA1c, and HMI (p < 0.01, Figure 1).
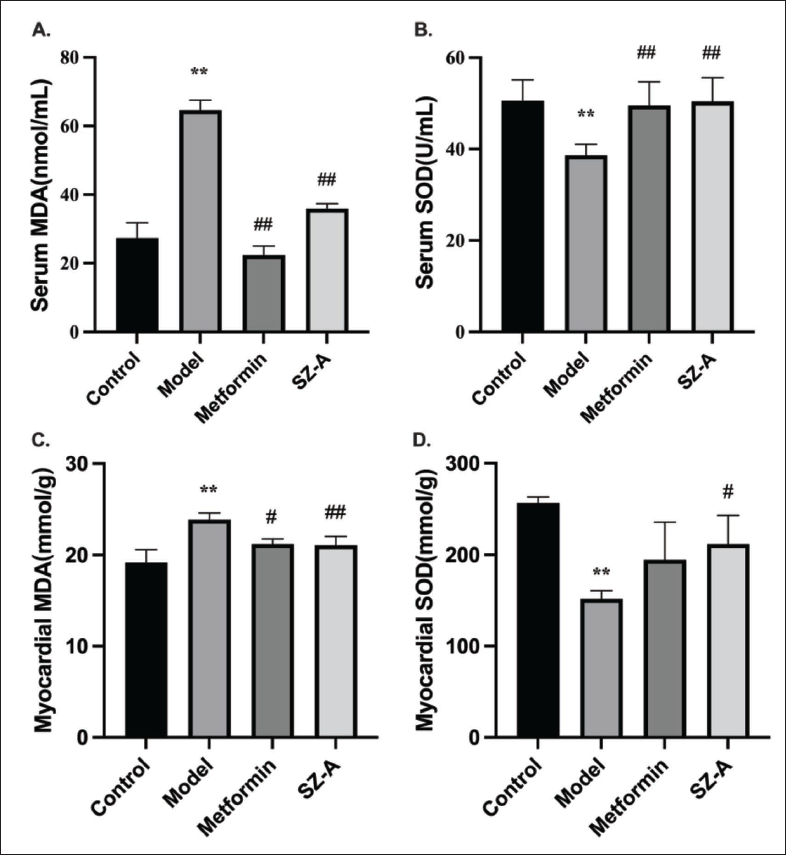
SZ-A Enhances SOD Activity and Reduces MDA Levels in Type-2 Diabetic Rats
In comparison with the control group, the model group exhibited reduced levels of SOD and elevated levels of MDA in both the serum and myocardium (p < 0.01). However, the metformin and SZ-A groups showed increased SOD levels and decreased MDA levels (p < 0.01, Figure 2).
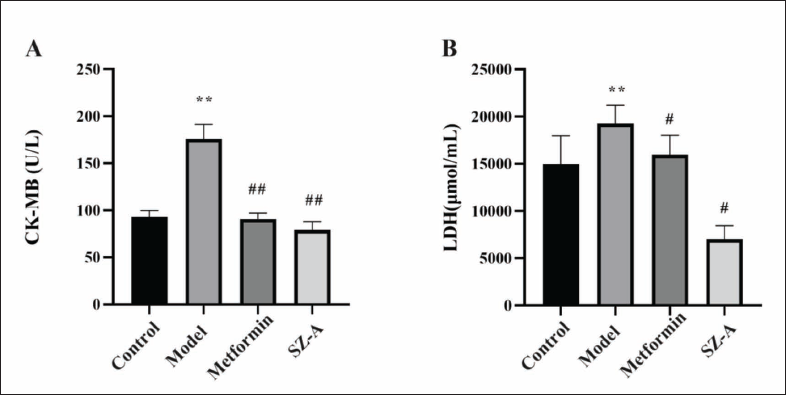
SZ-A Decreases CK-MB and LDH in Type-2 Diabetic Rats
The levels of CK-MB and LDH in the model group were significantly higher than those in the control group (p < 0.01). Nevertheless, the administration of the metformin and SZ-A groups resulted in a significant decrease in CK-MB and LDH levels (p < 0.01, p < 0.05, Figure 3).
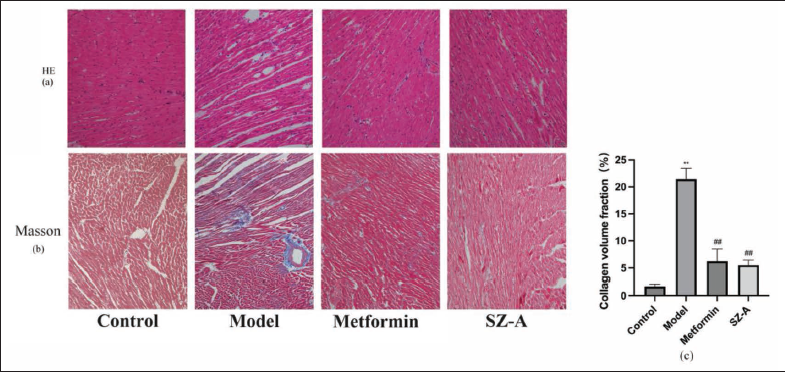
SZ-A Improves Myocardial Tissue Structure and Fibrosis in Type-2 Diabetic Rats
The impact of SZ-A on the structure of myocardial tissue and fibrosis was examined through the utilization of HE and Masson staining techniques. The HE staining results indicated that the cardiomyocytes in the control group exhibited an orderly arrangement with a distinct structure and consistent staining, whereas the Masson staining revealed minimal fibrosis. However, in the model group, cardiomyocytes were disordered, and the intercellular space was enlarged. Masson staining showed severe myocardial fiber injury and fibrosis staining. Collagen volume fraction was significantly higher in the model group. In comparison with the model group, the administration of the metformin and SZ-A groups resulted in enhanced organization of cardiomyocytes and decreased fibrosis (Figure 4).
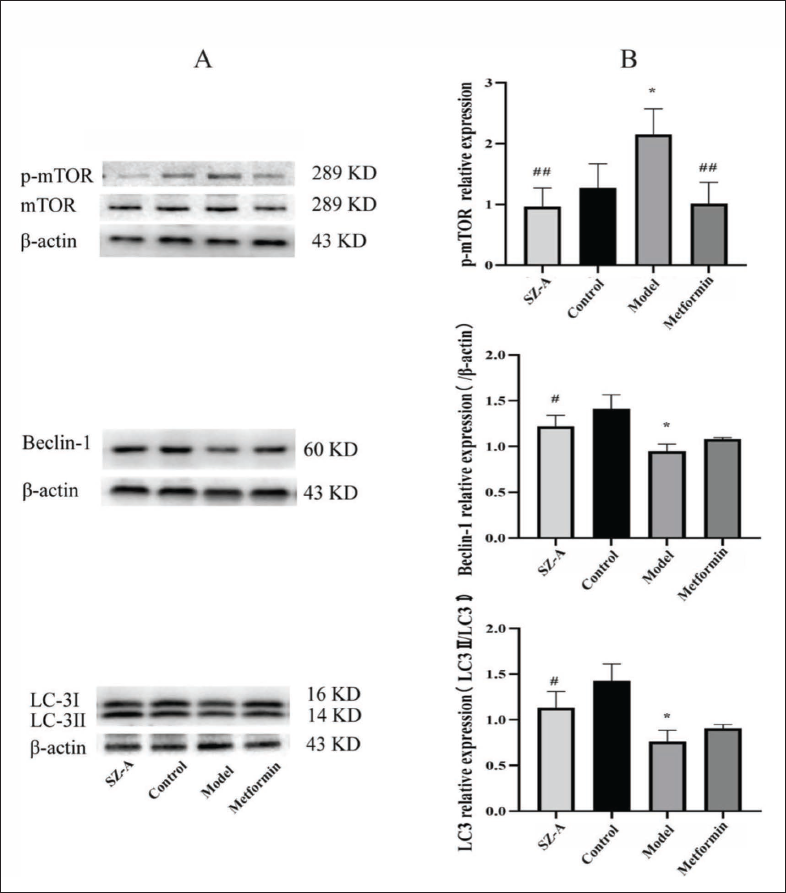
SZ-A Regulates Protein Expression Levels of p-mTOR, Beclin-1, and LC3 in Myocardial Tissue of Type-2 Diabetic Rats
Western blot analysis was conducted to examine the potential mechanism of SZ-A in improving diabetic myocardial injury. Following a 12-week administration period, it was noted that the model group exhibited an increase in the expression of p-mTOR compared to the control group. Conversely, the levels of Beclin-1 and LC3 expression were found to be decreased in the model group (p<0.05). Nevertheless, in the groups treated with metformin and SZ-A, the levels of p-mTOR were notably decreased, whereas the levels of Beclin-1 and LC3 were significantly increased in the SZ-A group (p < 0.05, p < 0.01) (Figure 5).
Discussion
Myocardial injury is a common occurrence among individuals with diabetes, potentially resulting in the development of heart failure. This injury is characterized by cardiomyocyte hypertrophy, apoptosis, and fibrosis (Luo et al., 2020). In patients with T2DM, cardiovascular disease is a major contributor to illness and death, presenting a higher likelihood of cardiovascular events when compared to the overall population (Bugger & Abel, 2014; Rawshani et al., 2018). Despite this, there are no effective treatments for myocardial injury resulting from DM, making it essential to develop corresponding therapeutic drugs. SZ-A, a novel Chinese medicine, has been approved for treating T2DM by the State Administration of Medicine. Research has demonstrated that the inhibition of p38 MAPK, ERK, and JNK signaling pathways effectively reduces inflammation (Cao et al., 2021). Additionally, mulberry leaves contain alkaloids, flavonoids, and polysaccharides, which have the ability to regulate blood glucose levels (Ge et al., 2018).
To examine the impact of SZ-A on myocardial injury in DM, we created a T2DM rat model by administering STZ through intraperitoneal injections and providing a diet high in glucose and fat. Significant elevations were observed in FBG, 2hPG, HbA1c, LDH, CK-MB, and HMI within the model group. HE staining showed irregular myocardial tissue arrangement, and Masson staining revealed myocardial fibrosis, indicating myocardial damage. The administration of SZ-A and metformin resulted in decreased blood glucose and myocardial injury indexes, improved arrangement of myocardial tissue, and reduced fibrosis. These findings indicate that these medications have the potential to prevent myocardial injury in individuals with T2DM.
Excessive production of reactive oxygen species (ROS) due to hyperglycemia plays a crucial role in causing myocardial injury in individuals with DM (Kurian et al., 2016). Oxidative stress is a significant pathogenesis of diabetic myocardial injury (Pérez-Matute et al., 2009). Increased ROS production can aggravate myocardial injury in diabetic patients. SOD, the primary antioxidant enzyme for cell detoxification, poses the effect of relieving peroxide damage and maintaining the balance between free radical production and antioxidant defense ability (Djordjevic et al., 2004; Wu et al., 2017). Conversely, MDA, referred to as the lipid final product and generated through lipid peroxidation, builds up and disrupts the structure of the cell membrane, resulting in metabolic disturbances and cytotoxicity (Esterbauer, 1993). During our experiment, there was a reduction in SOD levels and an increase in MDA levels in the serum of rats belonging to the model group, which suggests the presence of oxidative stress. However, after SZ-A treatment, SOD increased and MDA decreased, indicating that SZ-A could improve the oxidative stress state.
Autophagy is a natural process where various cellular components, including proteins, ribosomes, lipids, and even organelles, are engulfed by double-membrane structures and targeted for degradation by lysosomes. Maintaining cellular equilibrium is essential as it minimizes the harm caused by detrimental metabolites, breaks down liberated fatty acids, and decomposes advanced glycosylation products. In the improvement of diabetic myocardial injury, autophagy is also crucial as it decreases oxidative stress and insulin resistance while enhancing hypoxia and metabolic disorders (Kobayashi & Liang, 2015; Kubli & Gustafsson, 2014; Mellor et al., 2013). The decreased autophagy function in the heart may result in the excessive buildup of irregular proteins and organelles, leading to apoptosis and impairment of cardiac function (Xie et al., 2011). Thus, autophagy is crucial for preserving the balance of cardiomyocytes and enhancing the function of the heart in individuals with diabetes. Numerous research studies have demonstrated that the modification of autophagy function plays a vital role in diabetic myocardial injury. Autophagy recovery can improve diabetic myocardial injury, as demonstrated in various studies. For example, vaspin has the ability to reduce STZ-induced damage to the heart muscle and enhance autophagy, while suppressing the activation of NLRP3 inflammasome (X. Li et al., 2019). Moreover, barbering has demonstrated the ability to enhance the restoration of mitochondrial autophagy in H9C2 cells through the activation of the AMPK signaling pathway, thereby mitigating the injury caused by high glucose in cardiomyocytes (Hang et al., 2018). Beclin-1 is a vital autophagic protein for autophagosome formation that regulates autophagy activity (Zhu & He, 2015). The activation of Vps34 by Beclin-1 is crucial for regulating autophagy. The ability of Beclin-1 activating Vps34 is regulated by transcriptional regulation, miRNA, post-translational modification, and interaction with Beclin-1 binding proteins. The regulation of proapoptotic BH3 domain containing proteins is also influenced by the interaction between Beclin-1 and Bcl-2/XL, consequently impacting apoptosis. Consequently, the modulation of Beclin-1 has a substantial impact on both autophagy and apoptosis, ultimately leading to a profound effect on the survival and demise of cardiomyocytes. The elevated Beclin-1 protein expression results in heightened autophagy levels, concurrently decreasing the incidence of apoptosis (Abedin et al., 2007; Maejima et al., 2016). Abnormal autophagy function can be induced when the expression of autophagy is reduced, leading to apoptosis. In addition to mTOR, there are various other signals that regulate autophagy. When the expression level of mTOR is up-regulated, the expressions of its associated proteins Beclin-1 and LC3 are decreased and vice versa (Rosa et al., 2016). Research has indicated that oxidative stress, resulting from hypoxia, can reduce ATP levels. This reduction activates acetylate-activated protein kinase and deactivates mTOR, triggering the Beclin-1 pathway and resulting in autophagy. Consequently, this process leads to cardiac hypertrophy and impaired cardiac function (Wang et al., 2018). The mTOR protein expression level was reduced in this experiment, while the expression levels of Beclin-1 and LC-3 were notably increased following the administration of metformin and SZ-A derived from mulberry twig, aligning with findings from previous research. This suggests that the drug could regulate autophagy activity and participate in protecting myocardial injury in T2DM. There are still some limitations in our research. Firstly, there are a few groups of rats in this experiment. There is only one group of SZ-A with a fixed concentration, and no groups with other concentrations are set. Therefore, we cannot discuss the dose-effect relationship of SZ-A for diabetic myocardial protection. Secondly, we did not conduct research on the relevant pathways regulating autophagy through in vitro experiments. In the future, we will improve the experiment and continue to conduct in-depth research.
Conclusion
In conclusion, SZ-A has demonstrated the ability to improve glucose metabolism and reduce myocardial injury in rats with T2DM, which is possibly attributed to the expression of mTOR protein being decreased, the expression levels of Beclin-1 and LC-3 being significantly up-regulated, and the activation of autophagy to alleviate myocardial cell damage. These findings offer an empirical foundation for the prevention and drug development of diabetic myocardial injury in clinical settings.
Abbreviations
DM: Diabetes mellitus; SZ-A: Ramulus mori (Sangzhi) alkaloids; T2DM: Type 2 diabetes mellitus; SD: Sprague-Dawley; STZ: Streptozotocin; HMI: Heart mass index; FBG: Fasting blood glucose; 2hPG: 2-h postprandial blood glucose; HbA1c: Glycated hemoglobin; mTOR: Mammalian target of rapamycin; MDA: Malondialdehyde; LDH: Lactate dehydrogenase; CK-MB: Creatine kinase isoenzymes; SOD: Superoxide dismutase; ROS: Reactive oxygen species; CVF: Collagen volume fraction.
Authors’ Contributions
The manuscript was drafted by Ying Liu, Leilei Ma, and Wenxuan Xu, who made equal contributions to it. Xiaojin La, Biwei Zhang, Jianmei Cui, and Chunyu Tian were responsible for critically revising the important intellectual content. The study was conceived by Ji-an Li and Hong Chang, who also revised the manuscript and provided final approval for its submission for publication. The manuscript was revised by all authors who also read and approved the final version.
Footnotes
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical Approval
All animal experiments (2022-SY-031) were authorized by the Laboratory Animal Ethics Committee at North China University of Science and Technology.
Funding
This work was supported by grants from the Key International Cooperation Projects of the Ministry of Science and Technology Fund Project (KY201904005) and the Tangshan Science and Technology Bureau Innovation Team Fund Project (19130205C).
