Abstract
Ischemia-reperfusion (I/R) is a common clinical process, and the lung is one of the most sensitive organs of I/R injury, which often leads to acute lung injury (ALI). Tanshinone IIA (Tan IIA) has anti-inflammatory, antioxidant, and anti-apoptotic activities. However, the effects of Tan IIA on lung I/R injury remain uncertain. Twenty-five C57BL/6 mice were randomly divided into five groups: control (Ctrl), I/R, I/R + Tan IIA, I/R + LY294002 and I/R + Tan IIA + LY294002 group. Tan IIA (30 μg/kg) was injected intraperitoneally 1 h before injury in the I/R + Tan IIA and I/R + Tan IIA + LY294002 groups. These data showed that Tan IIA significantly improved I/R-induced histological changes and scores of lung injury, decreased lung W/D ratio, MPO and MDA contents, reduced infiltration of inflammatory cells, and decreased the expression of IL-1β, IL-6 and TNF-α. Meanwhile, Tan IIA significantly increased the expression of Gpx4 and SLC7A11, and decreased the expression of Ptgs2 and MDA. Moreover, Tan IIA significantly reversed the low expression of Bcl2, and the high expression of Bax, Bim, Bad and cleave-caspase 3. Furthermore, Tan IIA caused a significant increase in the phosphorylation levels of PI3K, Akt and mTOR in the lungs. However, these beneficial effects of Tan IIA on I/R-induced lung inflammation, ferroptosis and apoptosis were offset by LY294002. Our data suggest that Tan IIA significantly ameliorates I/R-induced ALI, which is mediated through activation of PI3K/Akt/mTOR pathway.
Keywords
Introduction
Acute lung injury (ALI) is a series of clinical syndromes caused by injury of alveolar epithelial and capillary endothelial cells. 1 The main manifestations are diffuse alveolar parenchyma injury and intractable hypoxemia. Severe cases can develop into acute respiratory distress syndrome (ARDS). 2 ALI induced by ischemia-reperfusion (I/R) usually occurs when the ischemic lung tissue recovers respiration and/or blood supply. Clinically, I/R occurs frequently in many cases, including lung transplantation, septic shock, pulmonary embolism and cardiopulmonary bypass disturbance. 3 Although I/R can maintain cell survival and restore tissue function, it can also cause organ damage by triggering a series of physiological and biochemical reactions. I/R can lead to pulmonary edema, nonspecific alveolar injury and increased vascular permeability, as well as neutrophil recruitment. 4 The process of ALI induced by I/R is complex, including the production of reactive oxygen species (ROS), immune response and activation of alveolar macrophages. 5 However, the specific molecular mechanism has not been fully elucidated. Moreover, there is a lack of effective strategies to treat ALI. Therefore, it is necessary to develop new effective drugs to improve the pathological features of patients with ALI.
Phosphatidylinositol 3-kinase (PI3K)/protein kinase B (AKT)/mammalian rapamycin target (MTOR) complex is a signal pathway that plays an important role in basic cellular activities such as cell metabolism, cell growth, cell proliferation, apoptosis and angiogenesis. 6 PI3K is activated when specific receptors are activated by extracellular ligands. Activated PI3K catalyzes the phosphorylation of PIP2 at position 3 of the inositol ring to PIP3. PIP3 can recruit two protein kinases, AKT and PDK1, to the plasma membrane through their Peckstrin homologous interaction domain. 7 Once AKT is gathered on the cell membrane, it is phosphorylated by mTORC2 (mTOR complex 2) on Ser473, changing the conformation of AKT and allowing it to be phosphorylated by PDK1 on Thr308. 8 Activated AKT phosphorylates the target proteins on the cell membrane, then loses the connection to the cell membrane, and phosphorylates other target proteins in the cytoplasm and nucleus. It has been found that PI3K/Akt/mTOR signal is an important functional regulator of TLR4/NF- κ B activity in the inflammatory pathway, and it also plays a key role in inhibiting apoptosis, immunomodulation, regulating anti-inflammatory cytokines and promoting extracellular matrix degradation. 9 In addition, the activation of PI3K/Akt/mTOR signal is involved in the inhibition of oxidative stress. PI3K/Akt signaling pathway is a highly conserved signaling pathway, which plays a crucial role in mediating some physiological and pathological processes including inflammation, oxidation and cell survival. 10 The results showed that the phosphorylation levels of PI3K, Akt and mTOR in the lungs decreased significantly after I/R, suggesting that the PI3K/AKT pathway was inactivated in the lung tissue after I/R. 11 The above results suggest that PI3K/Akt/mTOR signal pathway may play a role in I/R-induced injury.
Tanshinone IIA (Tan IIA) is a kind of Chinese herbal medicine containing many kinds of active ingredients. In vitro and in vivo studies have shown that Tan IIA has a wide range of anti-inflammatory, anti-oxidant, anti-apoptosis and anti-tumor activities.12–14 A large number of studies have found that Tan IIA is often used to treat cardiovascular diseases, 15 nervous system diseases, 16 injury diseases 17 and other diseases. It has been found that Tan IIA has a protective effect on cell death and apoptosis induced by ethanol. 18 Tan IIA can reduce the apoptosis of H9C2 cardiomyocytes, inhibit the activation of caspase-3 and the release of cytochrome c, and resist cardiomyocyte injury induced by hypoxia/reoxygenation. 19 Tan IIA can also inhibit neonatal rat cardiomyocyte apoptosis induced by angiotensin II by activating Akt phosphorylation. 20 In addition, studies have shown that Tan IIA can reduce cigarette smoke-induced lung inflammation and oxidative stress in mice through MAPK/HIF-1 a-mediated pathway. 21 A recent study found that Tan IIA prevented I/R -induced inflammation, and promoted alveolar epithelial repair via regulating the polarization of macrophages. 22 However, it remains to be elucidated whether Tan IIA can attenuate I/R-induced ALI, and whether its effect is related to PI3K/Akt/mTOR signaling pathway.
Therefore, the purpose of this study was to explore the protective effects of Tan IIA on I/R-induced lung inflammation, ferroptosis and apoptosis. On this basis, we further investigated whether the protective effect of Tan IIA on ALI induced by I/R is related to PI3K/Akt/mTOR signaling pathway.
Materials and methods
Animals and experimental protocol
Twenty-five healthy male C57BL/6 mice (aged 6–8 weeks) were provided by Benxi Changsheng Biotechnology Co., Ltd (Shenyang, China). Tan IIA (No. CCPE900047, CAS: 568-72-9) was purchased from Sinopharm Group Co., Ltd (Shenyang, China). LY 294002 (DMSO solution) was obtained from Abcam, UK. The mice were kept in a standard animal room with a 12-h light/dark cycle at temperature (20–24°C) and humidity (55 ± 5%). All mice were free to eat and drink. After 1 week of environmental adaptation, 25 mice were randomly divided into five groups (5/group): control group (Ctrl), (I/R) injury group, I/R + Tan IIA, I/R + LY294002, I/R + Tan IIA + LY294002 group. Tan IIA (30 μg/kg) was injected intraperitoneally 1 h before injury in the I/R + Tan IIA and I/R + Tan IIA + LY294002 groups. LY294002 (specific PI3K/Akt signaling pathway inhibitor) was diluted to 0.5 mg/mL in DMSO to prepare a stock solution. And 10 μL of the stock LY294002 was then injected 30 min prior to modeling. The mice in the Ctrl group were injected intraperitoneally with the same amount of normal saline as negative control. All animal protocols were approved by the Institutional Animal Care and Use Committee of Liaoning Provincial people’s Hospital (No. SYYXY2022082001), and all care and handling of animals was in accordance with the criteria outlined by National Institutes of Health guidelines.
Lung water content 23
48 h after I/R, the mice were anesthetized with 2% pentobarbital sodium (1.5 mL/kg, Sinopharm Group Co., Ltd, China). After the mice were killed, blood and lung samples were collected. The upper lobe of the right lung was dried with filter paper and weighed on the analytical balance to calculate the wet weight. After drying at 60°C for 72 h, the dry weight of the right lung was recorded. The formula for calculating the wet/dry ratio is as follows: W/D = wet weight/dry weight. Lung water content test is used to indicate the degree of lung edema.
Histological analysis
In order to evaluate the lung injury induced by I/R and the therapeutic effect of TanIIA, the left lungs were fixed with 10% formalin solution and embedded in paraffin. Paraffin sections were cut into 3–4 μm thickness using a fully automatic rotary slicer (Leica RM2265, Germany) Hematoxylin-eosin staining (H&E) was used to evaluate histopathological abnormalities. The degree of lung injury was scored according to lung hemorrhage, inflammatory cell infiltration and alveolar wall thickness. 24
Determination of oxidative stress
According to the manufacturer’s instructions, a number of biomarkers of lipid peroxidation, including myeloperoxidase (MPO), malondialdehyde (MDA) and superoxide dismutase (SOD) were detected using commercial ELISA kits (SEA601Mu, CEA597Ge, SES134Mu, Cloud-Clone Corp, China). The optimal density at 450 nm was used to measure the concentration of MPO, MDA and SOD in a microplate reader. The curve equation and r value were calculated to determine the concentrations of samples. 25
TdT-mediated dUTP-biotin nick-end labeling (TUNEL)
TUNEL staining was performed according to the TUNEL kit instruction (ab206386, Abcam, UK). The nuclei of apoptotic cells were stained brown. Five fields were randomly selected under a high-power microscope (× 400) to calculate the apoptotic index. The TUNEL positive cells were calculated via Image J software (Bethesda, MD, USA). The apoptosis level was evaluated by the percentage of positive cells in the total cell count.
Western blot analysis
The appropriate primary antibody.
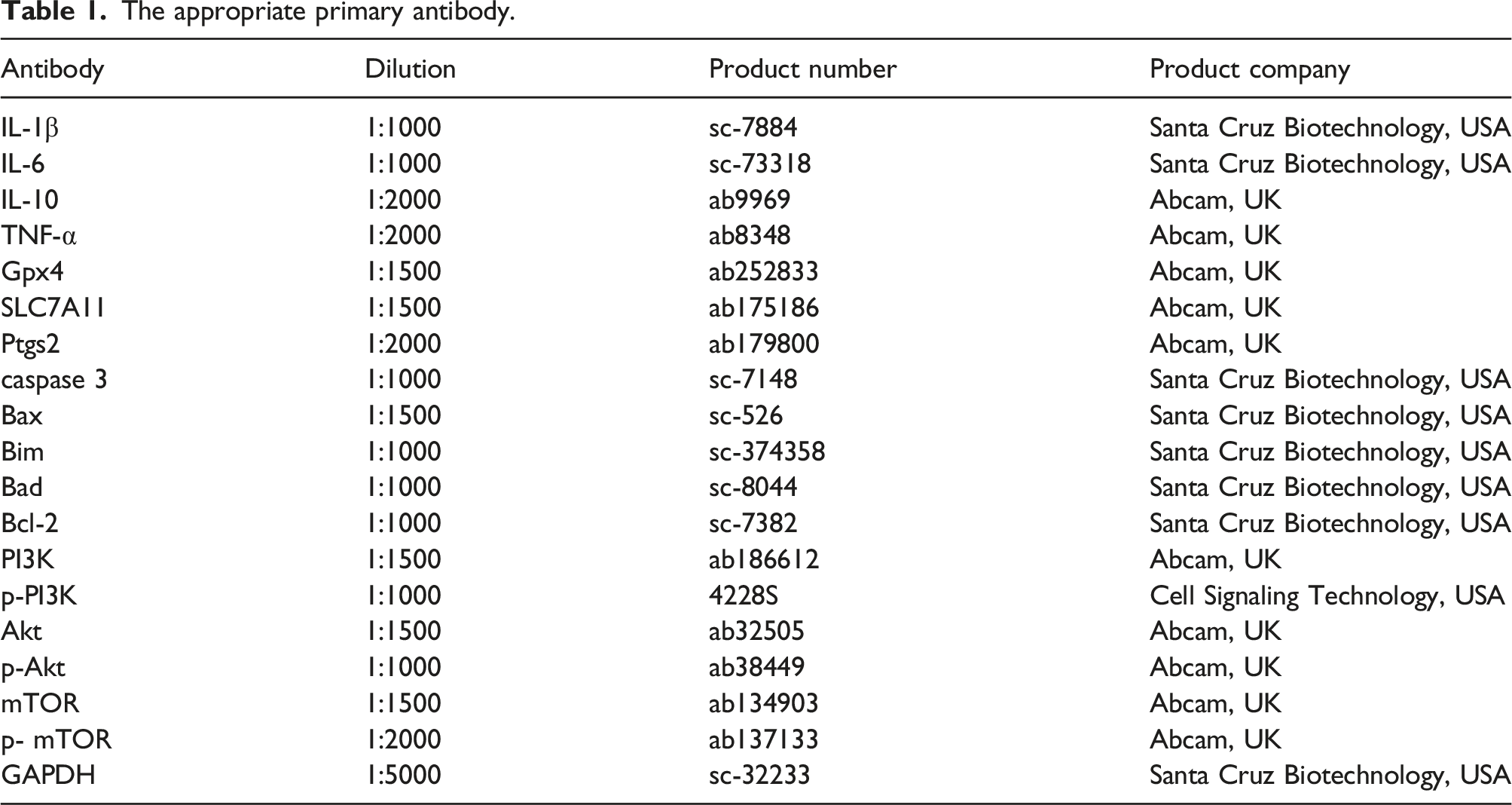
Statistical analysis
Statistical analysis was done using SPSS 26.0 software (IBM Corp., Armonk, NY, USA). All data were shown as means ± standard error (SE). Statistical comparisons between groups were analyzed by one-way analysis of variance (ANOVA). Multiple comparisons were tested by Duncan’ test.
Results
Tan IIA treatment attenuated I/R-induced acute lung injury
In order to evaluate the effects of Tan IIA on ALI, we used I/R to induce ALI in mice. As shown in Figure 1(a), the mice the I/R group showed typical histological changes of ALI, including hemorrhage, inflammatory cell infiltration and alveolar interstitial edema. Compared with the Ctrl group, lung injury score, W/D ratio, MPO and MDA contents were significantly increased, while SOD content was significantly decreased in the I/R group (Figure 1(b)–(d), Tan IIA treatment attenuated I/R-induced acute lung injury. (a) Representative histopathological images (HE staining, bar: 50 μm). (b) Lung injury score. (c) Lung weight/body weight ratio. (d) W/D ratio. (e–g) The content of MPO, MDA and SOD. Results are expressed as the mean ± SEM (
Tan IIA treatment ameliorated I/R-induced lung inflammation
A large number of studies have shown that Tan IIA has anti-inflammatory effects, and lung I/R injury is closely related to inflammatory response. The anti-inflammatory effect of Tan IIA on lung I/R injury was evaluated by detecting the expression of inflammatory factors. Our data showed that I/R caused significant increase in the expression of IL-1β, IL-6 and TNF-a, and a decrease in the expression of IL-10 in the lungs compared with the Ctrl group. After Tan IIA treatment, the expression of TNF-a, IL-6 and IL-1β was significantly decreased, while the expression of IL-10 was increased (Figure 2, Tan IIA treatment ameliorated I/R-induced lung inflammation. (a) Representative western blot images. (b–e) The expression of IL-1β, IL-6, IL-10 and TNF-α. Results are expressed as the mean ± SEM (
Tan IIA treatment inhibited I/R-induced ferroptosis
It is reported that Tan IIA has the potential to alleviate oxidative stress, whereas oxidative injury is involved in lung I/R injury. Therefore, we next detect markers of ferroptosis and lipid peroxidation in the lungs. As shown in Figure 3, compared with the Ctrl group, the expression levels of Gpx4 and SLC7A11 were significantly decreased, while Ptgs2 expression was significantly increased in the I/R group, suggesting that I/R can lead to ferroptosis in the lungs. After Tan IIA treatment, the expression levels of Gpx4 and SLC7A11 were significantly increased, and Ptgs2 expression was significantly decreased compared with the I/R group (Figure 3, Tan IIA treatment inhibited I/R-induced ferroptosis. (a) Representative western blot images. (b–d) The expression of Gpx4, SLC7A11and Ptgs2. Results are expressed as the mean ± SEM (
Tan IIA treatment decreased I/R-induced apoptosis
To elucidate the effects of Tan IIA on apoptosis induced by I/R, lung samples were stained with TUNEL and detected by western blotting. Our results demonstrated that the number of TUNEL-positive cells in the I/R group was significantly higher than that in Ctrl group, suggesting that I/R leads to lung apoptosis, while Tan IIA treatment could significantly reduce the number of TUNEL-positive cells, as compared with I/R group (Figure 4(a) and (b), Tan IIA treatment decreased I/R-induced apoptosis. (a, b) Representative images and semi-quantitative analysis of lung tissue apoptosis (TUNEL staining, scale bar = 50 μm). (c) Representative western blot images. (d–h) The expression of Bcl-2, Bax, Bim, Bad, cleave-caspase3 and GAPDH. Results are expressed as the mean ± SEM (
Effects of Tan IIA on PI3K/Akt/mTOR signaling pathway
PI3K/Akt/mTOR signaling pathway is a crucial functional regulator, which promotes cell division and proliferation, regulates inflammation, apoptosis, and autophagy. Some studies have shown that PI3K/Akt plays an important role in I/R injury, and Tan IIA is involved in the process of injury. Our data showed that I/R caused a significant decrease in the phosphorylation levels of PI3K, Akt and mTOR in the lungs, whereas Tan IIA treatment significantly reversed these changes (Figure 5, Effects of Tan IIA on PI3K/Akt/mTOR signaling pathway. (a) Representative western blot images. (b–d) The expression of p-PI3K, p-Akt and p-mTOR. Results are expressed as the mean ± SEM (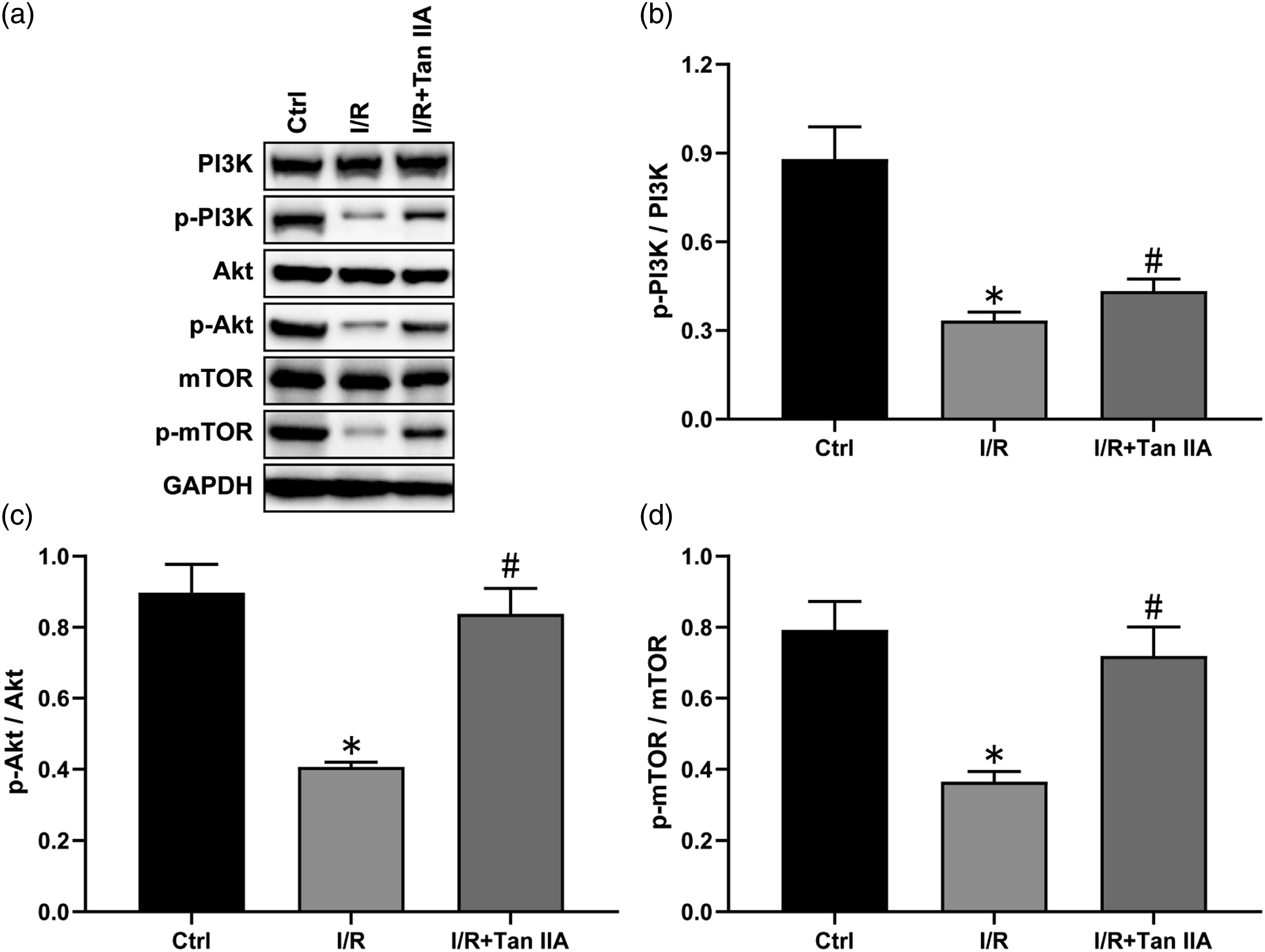
LY294002 offset the protective effects of Tan IIA on I/R-induced ALI
To further explore the potential mechanism of Tan IIA on I/R-induced ALI, LY294002, a PI3K/Akt inhibitor was used. Our data showed that LY294002 pretreatment caused a significant decrease in the phosphorylation levels of PI3K, Akt and mTOR in the lungs(Figure 6(a)–(d), LY294002 offset the protective effects of Tan IIA on I/R-induced ALI. (a–d) Representative western blot images and quantitative analysis of p-PI3K, p-Akt and p-mTOR. (e, f) lung weight/body weight ratio and W/D ratio. (g–k) Representative western blot images and quantitative analysis of IL-1β, IL-6, TNF-α, IL-10 and GAPDH. (l–q) Representative western blot images and quantitative analysis of Bax, Bim, Bad, caspase3, Bcl-2 and GAPDH. (r–u) Representative western blot images and quantitative analysis of Ptgs2, Gpx4, SLC7A11, and GAPDH. Results are expressed as the mean ± SEM (
Discussion
In the present study, our data showed that Tan IIA significantly improved I/R-induced histological changes and scores of lung injury, decreased lung W/D ratio, MPO and MDA contents, reduced infiltration of inflammatory cells, and decreased the expression of IL-1β, IL-6 and TNF-α. Meanwhile, Tan IIA significantly inhibited I/R-induced decreased levels of Gpx4and SLC7A11, and the increased expression of Ptgs2 and MDA. Moreover, Tan IIA significantly reversed the low expression of Bcl2, and the high expression of Bax, Bim, Bad and cleave-caspase3. Furthermore, Tan IIA caused a significant increase in the phosphorylation levels of PI3K, Akt and mTOR in the lungs. However, these beneficial effects of Tan IIA on lung I/R injury were reversed by LY294002. Our data suggest that Tan IIA significantly ameliorates I/R-induced ALI, which is mediated through activation of PI3K/Akt/mTOR pathway.
A large amount of evidence in vivo and in vitro shows that oxidative stress, endothelial dysfunction, mitochondrial dysfunction, increased pro-inflammatory cytokines and immune response are involved in the process of I/R, resulting in ferroptosis, apoptosis and autophagy. 27 Moreover, Tan IIA was reported to improve cigarette smoke-induced abnormal pulmonary function, pulmonary function, decreased the expression levels of TNF-α and IL-1β. 21 Meanwhile, high doses of Tan IIA has also been proven to alleviate lipopolysaccharide-induced ALI through reducing the expression levels of IL-1β and IL-6. 28 Similar to these findings, our results showed that I/R caused typical histological changes of ALI, increased the expression of pro-inflammatory cytokines IL-1β, IL-6 and TNF-a and decreased IL-10 expression, suggesting that Tan IIA can ameliorate I/R-induced inflammation.
A recent study has demonstrated that the enrichment of gene clusters related to cell death and inflammation is the most significant signal during lung I/R injury. 29 Several types of cell death are closely related to the regulation of inflammation. When ferroptosis occurs, it mediates inflammation and interferes with the immune system to deal with dead cells. Cells with ferroptosis release ATP, nucleotides and proinflammatory cytokines to promote the sustainable development of inflammation. 30 In addition to its anti-inflammatory effect, Tan IIA improved seawater-induced lung cell apoptosis, and reverse changes in Bcl-2 and caspase-3. 31 Moreover, Yadav et al. 32 found that Tan IIA alleviated oxidative stress induced by hypoxia by regulating the expression of MAPK and Nrf2 transcription factors. In turn, it can maintain a high level of antioxidant enzymes and genes (HO), and improve cell survival. Liu et al. 33 reported that Tan IIA also significantly improved the increase of MDA5 and IRE-an and the decrease of SOD-1 induced by blast exposure, and in return increased Bcl-2 expression and decreased Bax and Caspase-3 expression. Similar to these results, our data demonstrated that Tan IIA significantly reversed the low expression of Bcl2, and the high expression of Bax, Bim, Bad and cleave-caspase3. Interestingly, Guan et al. 34 found that Tan IIA increased lipid peroxidation and upregulated the expression of Ptgs2 and Chac1 in gastric cancer cells, which are two markers of ferroptosis, whereas Ferrostatin-1, a lipid peroxidation inhibitor suppressed lipid peroxidation induced by Tan IIA, and reversed the expression of Ptgs2 and Chac1. By contrast, our results showed that Tan IIA significantly inhibited the I/R-induced decreased levels of Gpx4, SLC7A11 and GSH, and the increased expression of Ptgs2 and MDA, showing that Tan IIA can ameliorate I/R-induced lung apoptosis and ferroptosis.
PI3K/Akt/mTOR pathway has been considered to play a vital role in the regulation of cell division and proliferation, apoptosis, autophagy, and inflammation. More and more studies have suggested that the activation of PI3K/Akt pathway plays a major role in inflammation, apoptosis and ferroptosis, and these changes are achieved by regulating the phosphorylation of downstream protein mTOR.35–37 Some studies have shown that PI3K/Akt plays an important role in I/R injury, 38 and Tan IIA improves in the process of injury through activing the PI3K/Akt signaling pathway. 39 Our data showed that I/R caused a significant decrease in the phosphorylation levels of PI3K, Akt and mTOR in the lungs, whereas Tan IIA significantly reversed the changes of these proteins. Similarly, Li et al. 40 found that renal I/R led to a significant decrease in the phosphorylation levels of Akt in the lungs, suggesting that PI3K/Akt pathway is inactivated in ALI after renal I/R. Moreover, Wen et al. 41 showed that limb I/R had also been reported to cause a significant decrease in the phosphorylation levels of PI3K, Akt and mTOR in the lungs. Subsequently, we selected LY294002, a PI3K/Akt inhibitor, to further investigate the mechanism of Tan IIA on lung I/R injury. Our data showed that LY294002 pretreatment significantly exacerbated I/R-induced lung inflammation, ferroptosis and apoptosis. Meanwhile, LY294002 significantly reversed the effects of Tan IIA on I/R-induced lung injury. It is reported that Tan IIA inhibits PI3K/Akt pathway, increases the expression of caspase-3/caspase-9, and then promotes the apoptosis of fibroblast like synoviocytes in rheumatoid arthritis. 42 More over, a study found that Tetrahydropalmatine had a significant protective effect on I/R-induced ALI, which might be achieved by saving PI3K/Akt/mTOR activity to inhibit autophagy. 41 Meanwhile, Tan IIA increased Akt phosphorylation in oxygen/glucose deprivation-induced neuronal injury, which was abolished by LY294002. 43 Furthermore, Tan IIA was also reported to increase cell viability, cause cell apoptosis, and these changes were reversed by LY294002. 44
In conclusion, our results show that I/R leads to lung inflammation, ferroptosis and apoptosis, whereas Tan IIA protects against I/R-induced ALI through PI3K/Akt/mTOR-mediated anti-inflammation, anti-ferroptosis and anti-apoptosis.
Footnotes
Author contributions
Rui Zhang and Jihui You designed experiments and wrote the manuscript. Rui Zhang, Yunen Liu and Baiping Ge completed animal experiment, pathological experiment, molecular biology experiment.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by the Key Projects of Liaoning Provincial Department of Education (No. LJKZ1153).
Ethical approval
The animal use protocol was approved by the Institutional Animal Care and Use Committee of Liaoning Provincial people’s Hospital (Shenyang, China), and the permit number is SYYXY2021092001.
