Abstract
Aim:
The aim of the study is to investigate protective effect of resveratrol (Res) on acute kidney injury (AKI) in sepsis.
Methods:
Rats in sham group received sham operation; in sham + Res received sham operation and Res (3 mg/kg); in cecal ligation and puncture (CLP) established as sepsis; in CLP + Res (3 mg/kg) with sepsis and Res (3 mg/kg); and in CLP + Res (10 mg/kg) with sepsis and Res (10 mg/kg). Survival rate, serum indexes, inflammatory factors, NF-κB-P65, and SIRT1 were detected. Lipopolysaccharide (LPS) mesangial cell was with Res and SIRT1 silencing.
Results:
(1) Res intervention improved survival rate of CLP rat. (2) Compared to sham, serum creatinine, blood urine nitrogen, serum cystatin C, neutrophil gelatinase-associated lipocalin, kidney injury molecule-1, tumor necrosis factor-α, interleukin-1β, IL-6, and renal injury index increased in CLP group, while decreased in CLP + Res (3 mg/kg) and CLP + Res (10 mg/kg), significantly, as dose-dependent (p < 0.05). (3) With Res, NF-κB-P65 and de-acetylated SIRT1 decreased, while SIRT1 and de-acetylated Nuclear factor kB-p65 9 NF-κB-P65) increased, significantly (p < 0.05). (4) SIRT1 and de-acetylated NF-κB-P65 decreased in LPS cells, while SIRT1 increased after Res intervention, significantly (p < 0.05). After silencing SIRT1, de-acetylated NF-κB-P65 increased, significantly (p < 0.05).
Conclusions:
Res increases the survival rate of septic rats by inhibiting inflammatory factors to ease AKI and promotes NF-κB-P65 de-acetylation by upregulating SIRT1.
Introduction
Sepsis was the excessively systemic inflammatory response induced by the invasion of microorganisms or other pathogens in human body, which could result in sepsis and septic shock. 1 –3 Acute kidney injury (AKI) was one of the common complications induced by sepsis. 4 –6 Therefore, it is imperative to investigate the pathophysiological mechanisms in the early stage and to search for the newly effective therapy on AKI induced by sepsis.
Resveratrol (Res) is a kind of non-flavonoid phenol. Previous study found that Res could improve the renal microcirculation, which could protect the epithelial cells of renal tubules from injury. 7 However, there were few researches on the effects of Res on AKI induced by sepsis, and whether Res could improve the symptoms of AKI in septic patients was still confused.
In our study, we established septic rat models with AKI by cecal ligation and puncture (CLP) and observed the pathological changes in renal tissues and the renal functions in the septic rats with or without Res intervention, in order to investigate the functionary mechanisms of the protective effects of Res on AKI in septic rats.
Materials and methods
Agents
Res was obtained from Aladdin Holdings Group (Shanghai, China). enzyme linked immunosorbent assay (ELISA) kits for tumor necrosis factor-α (TNF-α), neutrophil gelatinase-associated lipocalin (NGAL), kidney injury molecule-1 (KIM-1), interleukin-1β (IL-1β), IL-6, and IL-10 were obtained from Becton, Dickinson and Company (Shanghai, China). Hematoxylin and eosin (H&E) staining kit and BCA protein quantitation kit were obtained from Beyotime Biotechnology (Haimen, China). Rabbit anti-SIRT1, rabbit anti-NF-κ-P65, rabbit anti-β-actin polyclonal antibodies, and goat anti-rabbit secondary antibody labeled by horseradish peroxidase were obtained from Santa Cruz Biotechnology, Inc (Shanghai, China). SYBRPremix Ex Taq™ II kit was obtained from TaKaRa Biotechnology Co., Ltd (Dalian, China). Lipofectamine 3000 and Opti-MEM were obtained from Thermo Fisher Scientific Inc (Shanghai, China). Phosphate buffer salt (PBS) was obtained from Boster Bioengineering Co., Ltd (Wuhan, China). Tween-20 was obtained from Sigma-Aldrich (Shanghai, China). Electrochemiluminescence (ECL) kit was obtained from Merck Millipore Corporation (Darmstadt, Germany).
Animal treatments
Fifty male Sprague-Dawley rats (150–200 g) were obtained from the experimental animal center of Southern Medical University and housed in a temperature- and light-controlled room (21–25°C and 12 h light–dark cycle) with free drinking and eating in accordance with the U.K. Animals (Scientific Procedures) Act, 1986. 7 According to the previous references with the Res dose, 8,9 the rats were randomly divided into five groups, 10 of each, including (1) sham group with the rats being received sham operation, (2) sham + Res group with the rats being received sham operation and intraperitoneally injected with Res (3 mg/kg), (3) CLP group with the rats being established as septic models by CLP, (4) CLP + Res (3 mg/kg) group with the rats being established as septic models by CLP and intraperitoneally injected with Res (3 mg/kg), and (5) CLP + Res (10 mg/kg) group with the rats being established as septic models by CLP and intraperitoneally injected with Res (10 mg/kg). The rats in sham + Res, CLP + Res (3 mg/kg), and CLP + Res (10 mg/kg) groups were intraperitoneally injected with Res according to the setting concentrations after 2 h of surgery. After 12 h of surgery, the blood was collected from the inner canthal orbital vein. All the rats were killed after 72 h except for those already died.
Ethical approval was approved by the local research ethics committee in Southern Medical University.
ELISA detecting TNF-α, NGAL, KIM-1, IL-1β, IL-6, and IL-10
The blood samples were collected in anticoagulative tube with Ethylenediaminetetraacetic acid (EDTA) and centrifuged at 3000×g for 10 min. The supernatant, serum, was separated and stored at −80°C for the detection of cytokines by ELISA within 3 days. According to the specifications of the ELISA kits, the serum levels of TNF-α, NGAL, KIM-1, IL-1β, IL-6, and IL-10 were detected with six replicates and three repeats in each. The absorbance values at 450 nm were measured and recorded. The standard curves of those cytokines were drawn and the concentrations were calculated.
Automatic biochemistry analyzer detecting serum creatinine, blood urine nitrogen, and serum cystatin C
The concentrations of serum creatinine (Scr), blood urine nitrogen (BUN), and serum cystatin C (ScysC) in the blood of the rats were detected by AU400 automatic biochemistry analyzer (Olympus, Japan) according to the standard steps of the specification. The results were analysed and recorded.
Ultrasonic Doppler detecting renal blood flow and glomerular filtration rate
Acuson Sequoia 512 was used for contrast-enhanced ultrasonography by low mechanical index gray-scale imaging (CPS) with frequency of 7.0 MHz, mechanical index of M10-18 and focus on the region of renal injury. Renal blood flow and glomerular filtration rate (GFR) were detected.
Pathologic injury score on renal tissue
Renal tissues of the rats were stained by H&E and observed under microscopy (200×) to score the pathologic injury of renal tissue. The pathological changes of kidney tissue were examined by light microscopy and the slices were reviewed blindly and scored with a semiquantitative scale to evaluate changes. Definition of renal tubular injury: tubular epithelia proliferating, brush border losing, vacuolar degenerating, tubular forming and exuviation. The standard score of renal tubular injury was followed: 0, normal renal tissue; 1, renal tubular damaged area <25%; 2, renal tubular damaged area of 25–50%; 3, renal tubular damaged area of 50–75%; 4, renal tubular damaged area 75–100%. 10,11
Transfecting mesangial cell HRMC
Mesangial cell human renal mesangial cells (HRMC) was obtained from American type culture collection. small interfering RNA (siRNA) targeting SIRT1 was synthesized by GenePharma (Shanghai, China). The sequences were as follows: Sense 5′-GAUGAAGUUGACCUCCUCATT-3′; anti-sense 5′-UGAGGAGGUCAACUUCAUCTT-3′. Mesangial cell HRMC was cultured in six-well plate. When the confluent reached 70–90%, the cells were transfected with siRNA using Lipofectamine 3000 according to the specifications. Those without transfection were taken as negative control. After 48 h, the total RNA or the proteins were extracted. Real-time polymerase chain reaction and WB were used for detecting SIRT1 expression before and after transfection.
WB detecting SIRT1 and NF-κB-P65 expressions
The cells were collected and lysed using precooling lysis buffer for 15 min. After centrifugation at 12,000×g for 30 min, the supernatant was collected using BCA protein quantitation; 50 μg protein was analyzed by 10% separating gel and 5% stocking gel and transferred to Polyvinylidene Fluoride (PVDF) membrane (Merck Millipore Corporation). The membranes were incubated with rabbit anti-SIRT1 (1:1000), rabbit anti-NF-κB-P65 (1:1000) and rabbit anti-β-actin (1:1000) polyclonal antibodies at 4°C overnight. After washing with PBS containing 0.05% Tween-20, the membrane was incubated with goat anti-rabbit secondary antibody at 25°C for 60 min. The proteins were exposed by ECL.
Statistical analysis
All the data were analyzed by SPSS 17.0 software. Measurement data were analyzed by one-way analysis of variance homogeneity of variance, while Welch test was used with heterogeneity of variance. Least significant difference was used for pairwise comparisons with homogeneity of variance, while Dunnett’s T3 was used with homogeneity of variance. Kaplan–Meier was used for survival curve of sepsis combined with AKI. A value of p < 0.05 was considered statistically significant.
Results
Renal histological changes in rats
The histological changes are shown in Figure 1. Compared to sham group (Figure 1(a), a′), the renal structure in CLP group (Figure 1(a), b′) was unclear with obvious edema; more inflammatory infiltrate; glomerular enlarging; hemorrhagic spots in interstitium; narrow renal tubules; and epithelium swelling, degenerating, and falling. In CLP + Res group (Figure 1(a),-c′ and d′), the inflammation of the renal glomeruli, interstitium, and tubules released, and the inflammatory infiltrate of the renal tissue was less than that in CLP group. In CLP + Res (10 mg/kg) group (Figure 1(a), d′), the pathological changes of the renal tissue were less than that in CLP + Res (3 mg/kg) group (Figure 1(a), c′).
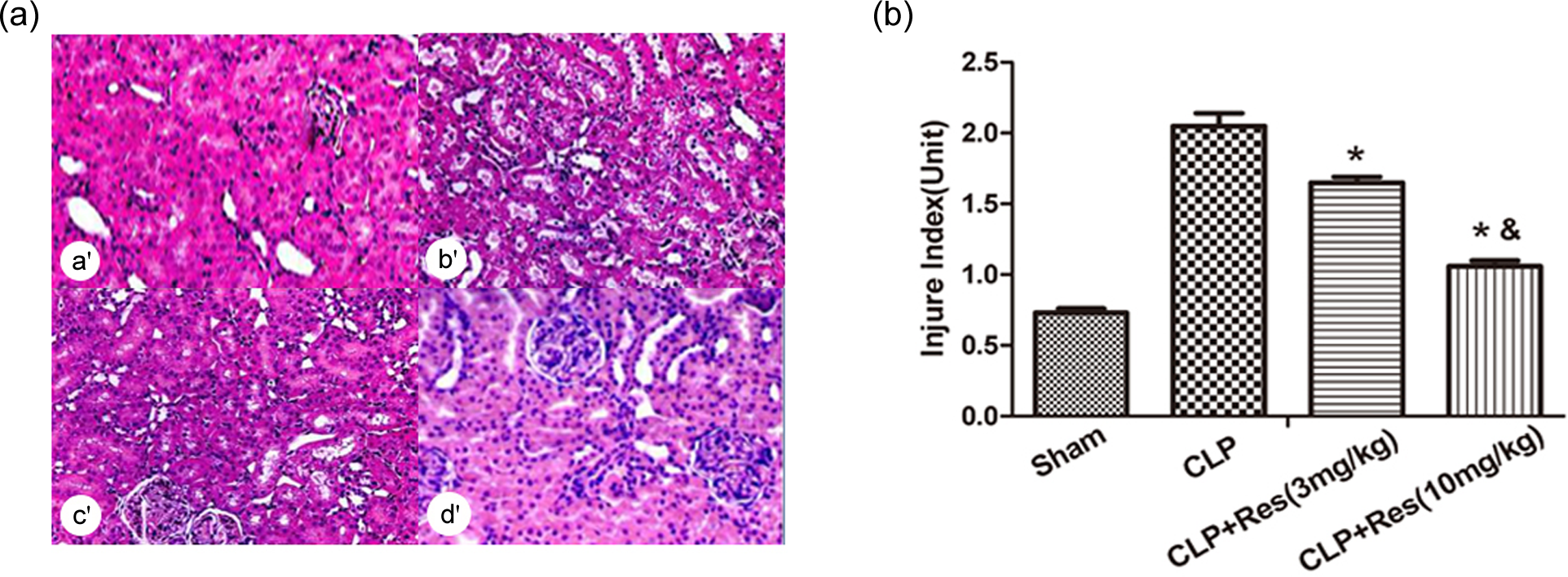
(a) Sham group (a′); CLP group (b′); CLP + Res (3 mg/kg) group (c′); CLP + Res (10 mg/kg) group (d′). (b) Comparing the score on the index of renal injury (*comparison between CLP + Res group and CLP group, p < 0.05; &comparison between CLP + Res (10 mg/kg) group and CLP + Res (3 mg/kg) group, p < 0.05). CLP: cecal ligation and puncture; Res: resveratrol.
Each tubular profile was assigned to one of the five categories: 0, 1, 2, 3 and 4, as described previously.
Comparing the score on the index of renal injury in sham, CLP, CLP + Res (3 mg/kg), and CLP + Res (10 mg/kg) groups (Figure 1(b)), the score in CLP group was higher than that in sham group, while that in CLP + Res groups was lower than that in CLP group, significantly (p <0.05). The score in CLP + Res (10 mg/kg) group was lower than that in CLP + Res (3 mg/kg) group, significantly (p < 0.05), indicating that as the concentration of Res increasing, the score on the index of renal injury decreased, significantly (p < 0.05).
Res intervention improving renal function in rats with AIK
According to Figure 2(a), there was no significant difference on Scr, BUN, ScysC, NGAL, or KIM-1 (p > 0.05), which indicated that Res had no obvious effect on the renal function of the rats in sham + Res group. On the contrary, Res could improve the renal function of the rats in CLP group compared to CLP + Res groups, as well as the renal functions being improved as the concentration of Res increasing, significantly (p < 0.05).

(a) Index changes of renal functions in different groups ((a′) Scr; (b′) BUN; (c′) ScysC; (d′) NGAL; (e′) KIM-1; (f′) renal blood flow; *comparison between CLP + Res groups and CLP group, p <0.05; &comparison between CLP + Res (10 mg/kg) and CLP + Res (3 mg/kg), p < 0.05). (b) Serum levels of TNF-α (a′), IL-1β (b′), IL-6 (c′), and IL-10 (d′) in different groups (pg/mL; *comparison between CLP + Res groups and CLP group, p < 0.05; &comparison between CLP + Res (10 mg/kg) group and CLP + Res (3 mg/kg) group, p < 0.05). Scr: serum creatinine; ScysC: serum cystatin C; NGAL: neutrophil gelatinase-associated lipocalin; KIM-1: kidney injury molecule-1; CLP: cecal ligation and puncture; Res: resveratrol.
From the results of the detection on renal blood flow and GFR, we found that the renal blood flow and GFR after Res intervention were improved compared to CLP group, as well as the renal functions being improved as the concentration of Res increasing, significantly (p < 0.05). The renal functions were improved in the rats in the sham group, significantly (p < 0.05) (Figures 4 and Figure 2(f))
Inflammatory factors changing after Res intervention
As shown in Figure 2(b), compared to sham group, Res had no influence on the serum levels of TNF-α, IL-1β, IL-6, and IL-10 in the rats in sham + Res group (p >0.05). Compared to CLP group, Res decreased the serum levels of TNF-α, IL-1β, IL-6, and IL-10 in the rats in CLP + Res groups, and as the concentration of Res increases, the serum levels of the TNF-α, IL-1β, IL-6, and IL-10 decreased gradually, significantly (p<0.05).
Survival rate comparisons
In order to investigate the effects of Res on the survival rate in septic rats with AKI, we compared the survival rate between CLP group and CLP + Res (10 mg/kg). As shown in Figure 3, there were eight rats died in 20 h in CLP group, with the survival rate of 20% in 20 h and that of 0% in 37 h. After Res intervention, there was no rat died in 24 h, and the survival rate between 50 h and 72 h was 60%. By Kaplan–Meier, the average survival rate of CLP + Res (10 mg/kg) group was higher than that of CLP group, significantly (p = 0.008).

Survival rate comparisons between CLP and CLP + Res (10 mg/kg) groups. CLP: cecal ligation and puncture; Res: resveratrol.
NF-κB-P65 and SIRT1 expressions changing in different groups
As shown in Figure 4(a), NF-κB-P65 expression in CLP group was higher than that in sham group, while in CLP + Res groups was lower than that in CLP group, significantly (p < 0.05). On the contrary, SIRT1 expression in CLP group was lower than that in sham group, while in CLP + Res groups was higher than that in CLP group, significantly (p < 0.05).

(a) Comparison of NF-κB-P65 and SIRT1 expressions in renal tissues among sham, CLP, and CLP + Res groups. (b) Comparison of acetylated NF-κB-P65 and SIRT1 expressions in mesangial cell HRMC among control, LPS, LPS + Res, and LPS + SIRT1 RNAi groups. CLP: cecal ligation and puncture; Res: resveratrol; LPS: lipopolysaccharide.
As shown in Figure 4(b), Res was used to intervene the mesangial cell HRMC after stimulated by lipopolysaccharide (LPS) in vitro. The results showed that compared to the control group, SIRT1 expression decreased in LPS group, significantly (p < 0.05). Compared to LPS group, the SIRT1 expression in LPS + Res group increased, while that in SIRT1 RNAi group decreased, significantly (p < 0.05). Compared to LPS group, the de-acetylated NF-κB-P65 in the control was higher, while that in LPS + Res group was lower, significantly (p < 0.05). After transfection with SIRT1 siRNA, the de-acetylated NF-κB-P65 increased significantly (p < 0.05), which indicated that Res could promote the de-acetylation of NF-κB-P65 by upregulating SIRT1.
Discussions
Res protecting kidney in septic rats
Res and polydatin (PD) were the natural components extracted from the plants, which were the non-flavonoid phenol. As the antioxidant, Res was involved in functions such as dilating blood vessels; preventing and treating arteriosclerosis, cardiovascular, and cerebrovascular disease; and so on, 9 –12 as well as highly anti-tumor activity and cancer prevention. 13 –17 However, there were few research on Res in sepsis, which were without conclusion and needed further investigations.
AKI was one of the common complications in sepsis. Scr, BUN, and ScysC were the classical standard to evaluate AKI. The early AKI marker, including KIM-1 and NGAL, would increase in 24–48 h before Scr increasing. 18 –20 All of these indexes were helpful for the early diagnosis on AKI, as well as important for the prognosis. Therefore, we selected the five indexes mentioned earlier combining with renal blood flow and GFR to evaluate the protective effect of Res on kidney in sepsis. The results showed that after Res intervention, serum concentrations of Scr, BUN, ScysC, KIM-1, and NGAL decreased, while renal blood flow and GFR increased, obviously. These phenomena indicated that Res could promote the renal function in septic rats, and as the concentration of Res increasing, the protective effect was more obvious. Therefore, we confirmed that Res could protect the renal function in septic rats and the higher concentration of Res is with better protective effect on septic rats with AKI.
From the results of the histopathological sections of renal tissues in rats, it was observed that after Res intervention, the inflammatory changes in renal glomeruli, interstitium, and tubules were improved, as well as the inflammatory cell infiltration. As the Res concentration increased, the inflammatory changes were improved more obviously. With the Res intervention, the survival time and rate were both higher than that in the control, which also indicated that Res could control or reverse the AKI in septic rats effectively.
Res protecting kidney in septic rat by regulating inflammatory factors
Inflammation is the basic mechanism to defend from pathogen invasion, which is the complicated biological process, including some of the cytokines synthesizing and releasing. Therefore, we detected the cytokines in serum of the rats and found that after Res intervention, serum levels of TNF-α, IL-1β, IL-6, and IL-10 were decreased as the Res concentration increasing, obviously. These results indicated that the protective mechanisms of Res on kidney in septic rats with AKI might be related to the inhibition of inflammation. Res could release the inflammation, as well as decrease the release of inflammatory factors to protect kidney in septic rats with AKI.
In previous studies, NF-κB played an important role in inflammatory reactions. 21,22 NF-κB, which was with high activity in some of the region with inflammatory disease, could induce the gene expressions of inflammatory cytokines (TNF-α, IL-1, and IL-6), chemokines, adhesion molecules (intercellular adhesion molecule-1 [ICAM-1] and vascular cell adhesion coagulation-1 [VCAM-1]) and inflammatory enzymes (inducible nitric oxide synthase [iNOS] and cyclooxygenase-2 [COX-2]), as well as enlarging inflammatory cascade. 23,24 NF-κB-P65 was the transcription factor of many inflammatory factors, which played a critical role in inflammation. 25 Sirtuin was a kind of deacetylase, including seven family members already confirmed: SIRT1–SIRT7. Sirtuin family could regulate many acetylation and adenosine diphosphate (ADP)-ribosyl modification. However, whether Res could promote de-acetylation of NF-κB-P65 by upregulating SIRT1 to inhibit the release of inflammatory factors is still unclear and draws attentions.
In our study, we detected the SIRT1 and NF-κB-P65 expressions in renal tissues of different groups and found that NF-κB-P65 was inhibited after Res intervening the AKI rats, while SIRT1 expression was increased. Following the detection, we used the mesangial cell HRMC induced by LPS as the model. After Res intervention, NF-κB-P65 expression decreased, while de-acetylated NF-κB-P65 increased after transfecting with SIRT1 siRNA, significantly. These results indicated that Res could promote de-acetylation of NF-κB-P65 by upregulating SIRT1.
When the body was invaded by pathogens including bacteria and virus, the infection would induce a series of inflammatory reactions, which would lead to the feedback and activate the autoimmune response to release inflammatory factors. The transcription of the cytokines depends on the activation of NF-κB, including IL-l, IL-6, IL-8, TNF-α, digestive enzyme in extracellular matrix, ROS, cyclooxygenase-2, growth factors, iNOS, and so on. The release and increase of the cytokines would activate NF-κB again, which enlarge the originally inflammatory information and aggravate the microcirculation injury until DIC or death. 26 –28 This condition was common in sepsis syndrome and adult respiratory distress syndrome.
According to previous reports, Sirtl could react with NF-κB-P65 by de-acetylation, which would result in the loss of the genes activating NF-κB and decreasing the NF-κB binding to proinflammatory gene. 29 These reactions would lead to the decrease of releasing IL-1, TNF-α, and so on. 30
Conclusively, Res could protect the renal functions in the septic rats with AKI, as well as increasing the survival rate of the septic rats by inhibiting the release of inflammatory factors and promoting NF-κB-P65 de-acetylation by upregulating SIRT1 expression to ease AKI induced by sepsis. However, there were some limitations in our study, such as the small sample of the septic rats, difficulty to record the long-term survival, and only using one kind of mesangial cell, HRMC cell. Further investigations on the protective effects of Res on the kidney in sepsis are still needed.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This study was supported by the National Natural Science Foundation of China (grant no. 81272027).
