Abstract
Environmental sustainability in radiology has a growing role in health care as climate changes intensify. Quality Initiative/Improvement (QI) projects lead to improved patient care and safety as well as efficient use of limited health care resources. When designing a QI project, including an environmental lens increases awareness of sustainability in medicine. This document will focus specifically on sustainability in QI (SusQI) in the field of radiology, though similar principles may be applied in other medical fields. The sustainable QI model updates the value equation denominator from cost to the triple bottom line of environmental, social, and economic measures. Using this SusQI model can lead to a win (patient)-win (health care system)-win (environment). This article will also discuss the importance of the environment for human health and the link between quality initiatives and environmental sustainability in demonstrating the value of Radiology and improving the quality of patient care. It will provide some examples of sustainability applied to many quality initiatives in Radiology: For example, reduction in oral contrast use for many previously used indications, streamlined MRI protocols, as well as using ultrasound over CT or MRI for indications that are equally appropriate.
Evolution of Medicine and Importance of QI
Since the discovery of the X-ray by Dr. Wilhelm Roentgen in 1895, the field of radiology has been at the forefront of medical innovation. Over the past century, diagnostic and interventional radiology have undergone remarkable transformations, contributing significantly to the understanding, diagnosis, and treatment of various diseases. The integration of advanced imaging techniques, such as computed tomography (CT), positron emission tomography (PET), magnetic resonance imaging (MRI), and ultrasound, has revolutionized the ability of clinicians to visualize internal structures and make informed decisions. Similarly, interventional radiology has shifted the model of treatment by offering minimally invasive procedures, reducing patient morbidity and recovery times, shortening hospital stays and concurrently, improving clinical outcomes. These advancements underscore the critical role radiology plays in modern medicine. As healthcare systems have evolved, so too has the need for continuous improvement to address imaging safety, growing demands combined with limited resources, and increasing complexity associated with patient care. Quality Improvement (QI) has emerged as a cornerstone of modern healthcare, providing a structured approach to enhancing patient care, safety, and operational efficiency.
What is QI
Quality Improvement (QI) is a systematic, data-driven approach to enhancing healthcare processes and outcomes. It involves the continuous assessment and refinement of practices to improve safety, effectiveness, efficiency, patient-centredness, timeliness, and equity—collectively known as the six pillars of QI. These pillars guide healthcare providers in identifying areas for improvement, implementing evidence-based interventions, and evaluating their impact over time. QI methodologies include Plan-Do-Study-Act (PDSA) cycles, Lean model, and Six Sigma. 1 These methodologies enable healthcare systems to reduce variability, eliminate waste, and optimize patient care delivery. By emphasizing evidence-based interventions and data-driven decision-making, QI enables healthcare providers to deliver consistent, reliable, and patient-centred services. In radiology, QI initiatives often focus on streamlining workflows, standardizing imaging protocols, and incorporating advanced technologies to enhance diagnostic accuracy and operational efficiency. Change management plays an important role in QI; this includes involving all stakeholders at the outset of QI project planning, which allows for smoother adoption and long-term integration of the changes. By fostering a culture of continuous improvement, QI ensures that healthcare systems can adapt to changing demands while maintaining high standards of care. 2
Environmental Sustainability as a Domain of QI
The growing recognition of healthcare’s environmental impact has brought sustainability to the forefront of medical practice. As a sector that relies heavily on energy-intensive technologies and resource-intensive processes, radiology bears a responsibility to address its ecological footprint. Sustainability in healthcare encompasses the environmental, social, and economic dimensions of delivering care, all of which are interlinked with efficient use of limited resources, and patient outcomes. Incorporating sustainability into QI initiatives aligns with global efforts to mitigate climate change and conserve finite supplies while maintaining high standards of care.
The inclusion of sustainability as a distinct domain within the QI frameworks is both timely and necessary. Traditional QI domains—such as safety, effectiveness, and efficiency—have focused primarily on optimizing clinical and operational aspects of care (Figure 1). However, the environmental consequences of healthcare practices have often been overlooked. By integrating sustainability as a seventh pillar of QI, healthcare systems can adopt a more holistic perspective that evaluates environmental implications of clinical decisions. This approach not only enhances the value of care delivered but also aligns with societal goals of reducing carbon emissions and promoting environmental stewardship.3,4
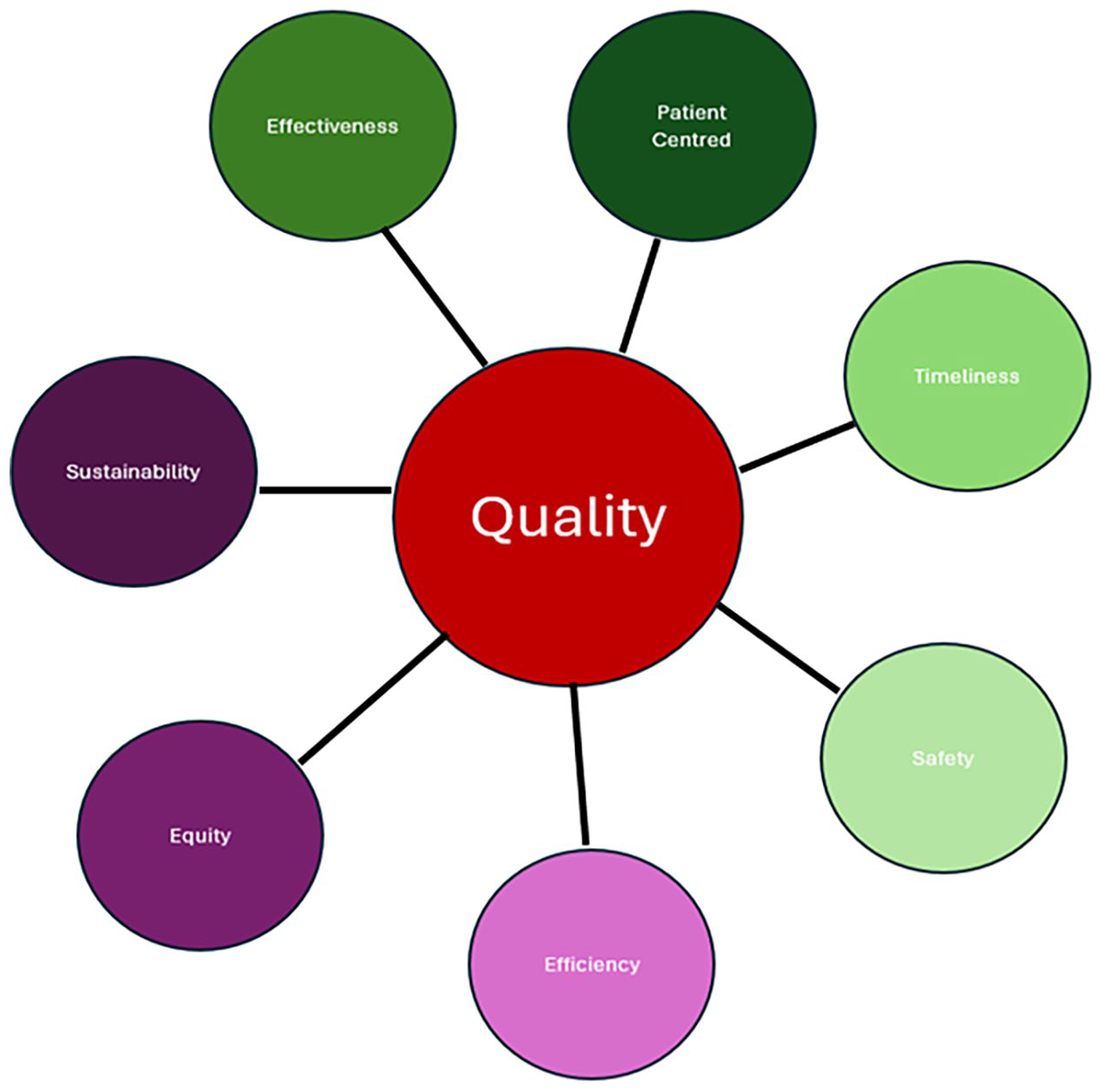
Sustainability as a domain of QI.
Environmental Sustainability is an integral pillar in QI because it bridges the gap between quality care and responsible resource utilization. By addressing issues such as waste reduction, energy efficiency, and sustainable procurement, radiology departments can achieve meaningful progress toward environmental goals without compromising patient outcomes. Moreover, an environmental sustainability focus fosters innovation, encouraging the development of low-carbon technologies and practices that enhance overall system resilience. As healthcare systems worldwide grapple with the dual challenges of environmental degradation and rising demand, incorporating sustainability into QI frameworks offers a pathway to balance these competing priorities effectively.3,4
Health Equity and Access
The health impacts of the climate crisis are not evenly distributed globally or even within regions. Populations more vulnerable to extreme weather events, food insecurity, reduced access to potable water, mental health impacts and violence include those already stressed by adverse social determinants of health, extremes of age, low socioeconomic status, women, minorities, and the underhoused. 5 For example, a precariously housed family who cannot afford home insurance may have limited resources to recover from losing their home to a wildfire or flood. In the June 2021 BC heat dome, 67% of deaths occurred in people over 70 years of age, most of whom lived in materially deprived neighbourhoods, and 13% of deaths were patients with schizophrenia. The inequity is particularly striking in that these populations have typically contributed the least to pollution and global emissions. 6
Global Action for Universal Health is the theme for World Health Day April 7, 2025. This theme underscores the WHO commitment to universal health coverage to provide equitable access to high quality healthcare for all individuals and communities. 7 Our commitment as radiologists to reducing waste and promoting environmental sustainability in medical imaging is a health equity action. 8 Through mitigation to reduce our impact, we reduce air and water pollution. Through adaptation to increase resilience to extreme weather events we ensure that all communities including rural and remote areas retain equitable access to imaging services.
Environmental sustainability in Radiology works in concert with well-established national climate change and health assessment processes. Health Canada has published reports such as 2022 Health of Canadians in our Changing Climate and provides healthADAPT grants to assist the health sector in preparing for climate impacts. 9 Globally, Health Canada is the current co-chair of the WHO Alliance for Transformative Action on Climate and Health (ATACH) working group, with the goal to implement global climate resilient and low-carbon sustainable health systems. 10
Integration of Sustainability Into QI Projects (SusQI)
The integration of sustainability into Quality Improvement (SusQI) represents a transformative approach to healthcare, addressing not only patient outcomes but also environmental and societal impacts. SusQI expands traditional QI frameworks by embedding the principles of sustainability into every stage of the process. By aligning healthcare practices with the “triple bottom line” of environmental, social, and economic dimensions, SusQI ensures that quality improvements are both impactful and environmentally sustainable.
The Centre for Sustainable Healthcare has outlined key tenets of SusQI, which include prevention, patient empowerment, lean clinical pathways, and low-carbon alternatives. 11
Prevention focuses on early detection and lifestyle interventions, reducing the disease burden before significant resources are required. Patient empowerment emphasizes the role of informed decision-making and self-care, fostering a collaborative relationship between patients and providers. Lean clinical pathways streamline workflows to minimize waste, improving efficiency and reducing environmental impact. Lastly, low-carbon alternatives prioritize environmentally friendly practices, such as transitioning to less resource-intensive imaging modalities where appropriate. 11
By adopting these principles, radiology departments can address the environmental challenges of modern healthcare without compromising patient care. For instance, using opportunistic imaging for preventive care can identify risk factors early, reducing the need for future resource-intensive interventions. Similarly, optimizing imaging protocols and implementing multi-use contrast systems can significantly reduce waste and environmental harm. These practices highlight the synergy between sustainability and quality, demonstrating the potential of SusQI to transform radiology into a more sustainable discipline.
To learn more about integration of sustainability into quality improvement (SUSQI) projects, the CASCADES Canada website offers comprehensive resources and provides detailed framework, best practices, and case studies for various health care settings. It also contains playbooks that are particularly useful for people in Canada but can be applicable worldwide. 12
Applications of SusQI in Radiology
The application of SusQI principles in radiology offers numerous opportunities to enhance patient care while minimizing environmental impact. By reevaluating traditional practices through a sustainability lens, radiology departments can identify areas for improvement that align with both clinical and environmental goals. Given that QI requires all partners to be involved early in the process, additional stakeholders may be needed when considering a sustainability lens, since environmental services, industry/suppliers, and IT may have roles not previously considered in standard QI projects.
One such example includes optimization of image acquisition protocols, which involves streamlining imaging workflows to reduce overall resource use. For instance, MRI protocols can be optimized to lower the overall volume of gadolinium used. This can be combined with abbreviated protocols reducing time required for scanning each patient and also lead to overall reduction in energy consumption. Each of these strategies can influence environmental impacts as well as improve patient experience and access to imaging through more efficient scheduling templates. Similarly, transitioning from MRI or CT to ultrasound for appropriate indications can significantly lower overall energy consumption, while maintaining diagnostic accuracy. Clinical trials and research studies have been used to ensure standardization of imaging protocols which will in turn lead to reduction of unnecessary exposure to radiation and contrast agents.13-15
In an era of limited resources and long wait times for patients, this redistribution of appropriate imaging modalities for a particular indication can help alleviate some of the excessive demand on equipment and human health resources.13-15
Contrast agent management is another example of SusQI. Implementing multi-use dispensing systems and standardizing protocols can minimize waste, ensuring that contrast agents are used efficiently and potentially increasing patient throughput. Additionally, efforts to reclaim and recycle contrast agents are emerging as innovative solutions to reduce their environmental footprint.13,16
Energy efficiency measures, such as powering down imaging equipment during non-imaging time and utilizing motion-sensor lighting, can further reduce the carbon footprint of radiology departments (Table 1). Upgrading equipment rather than replacing existing units can also help reduce environmental impacts, while allowing continued improvement in scan quality and patient care. 17 These practices, combined with broader infrastructure improvements, such as designing facilities resilient to extreme weather events, underscore the potential of SusQI to drive meaningful change. 6
Sustainable practices that can be adopted with their potential projects.
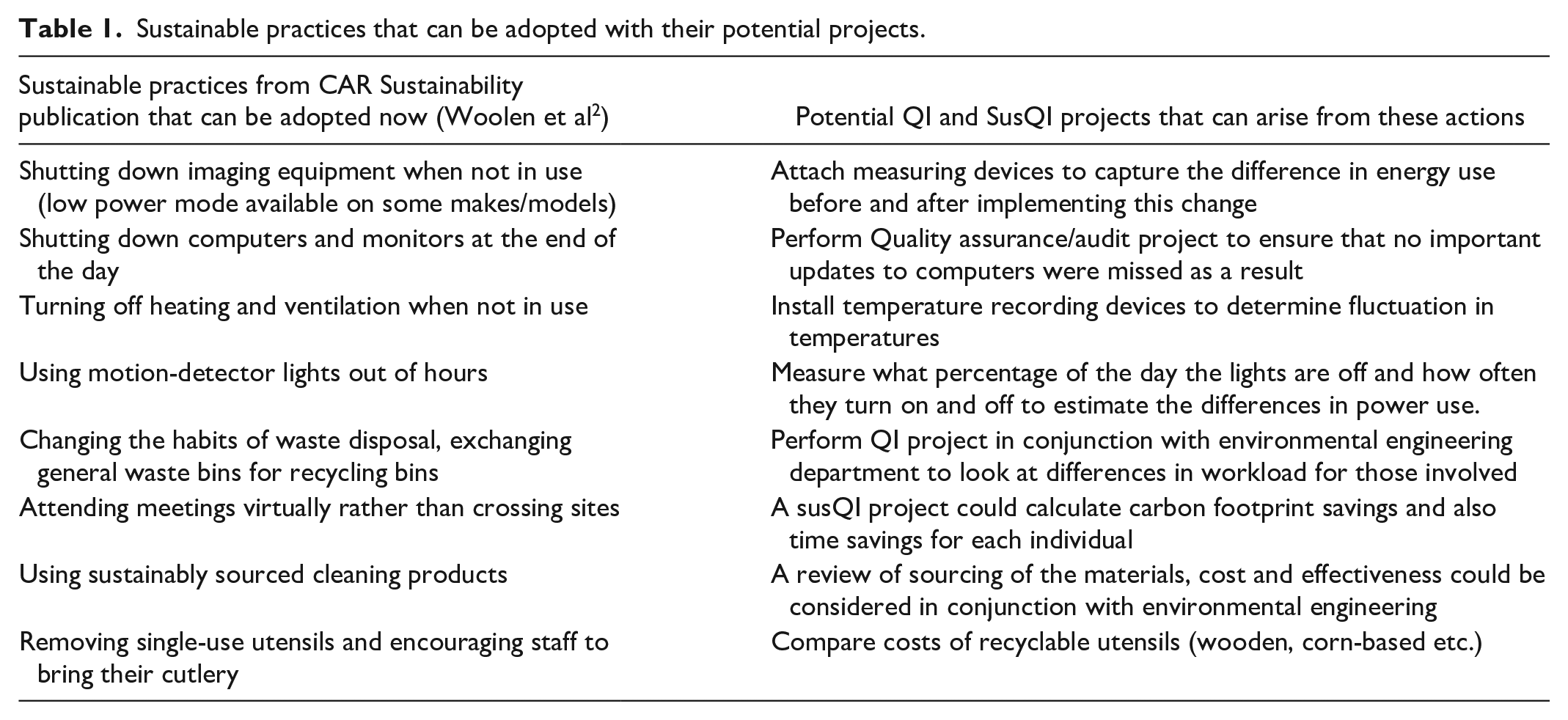
Preventive care, such as opportunistic screening during imaging for other medically indicated reasons, represents another promising application of SusQI, if specific AI algorithms are integrated into medical imaging practices. By leveraging increasing amounts of available imaging data to identify early indicators of medical conditions such as hepatic steatosis, osteoporosis, and atherosclerosis, radiology can contribute to preventive health strategies that reduce future healthcare demands. This proactive approach aligns with the principles of SusQI, demonstrating the value of integrating sustainability into clinical practice. 18
SusQI has the potential to address disparities in healthcare access by promoting efficient and sustainable resource utilization. By optimizing workflows and reducing unnecessary imaging studies, radiology departments can free up limited imaging resources to serve underserved populations. For example, transitioning to portable imaging modalities, such as point-of-care ultrasound, can bring diagnostic services to remote or resource-limited settings, improving access for communities that face barriers to traditional healthcare facilities. 19
Similarly, the use of telemedicine and teleradiology, and remote scanning technology, supported by sustainable practices, ensures equitable access to diagnostic expertise regardless of geographic location. These solutions can also help manage the human health resource shortages occurring across the country and internationally. These approaches demonstrate how integrating sustainability into QI can create a more inclusive and accessible healthcare system and reduce burnout of the healthcare workers as well. 20
The Canadian Association of Radiologists (CAR) statement on planetary health education in radiology emphasizes the importance of incorporating planetary health education into radiology residency programs. This integrated curriculum ensures that radiologists are not only aware of their ability to minimize the environmental impact of their practice but also supports the implementation of SusQi into their workflow. The CAR statement on planetary education emphasizes the role academic radiology departments have in providing leadership in environmentally sustainable radiology, including dedicated time and project funding, to enable incorporation of sustainability and SusQI concepts throughout Diagnostic Radiology CanMEDS competencies. 21
Research and Sustainable Quality Improvement
Research plays a pivotal role in advancing the principles of Sustainable Quality Improvement (SusQI), bridging the gap between theory and practice. By fostering a culture of innovation, radiology departments can lead the way in developing and implementing environmentally sustainable practices that benefit both patients and the planet. Integrating sustainability-focused leadership roles within residency and fellowship programs is essential for engaging learners and shaping future leaders in the field. These roles can encourage trainees to undertake projects that align with SusQI principles, providing valuable insights into the intersection of quality, efficiency, and environmental stewardship.
Radiology residency programs should consider formally identifying a “sustainability champion” to mentor trainees and oversee research initiatives. This role would facilitate trainee-led projects that address sustainability in QI, fostering collaboration between trainees and faculty. Furthermore, academic programs could collaborate with national organizations, such as the Canadian Association of Radiologists (CAR), to develop standardized resources and frameworks for sustainability-focused research. For instance, creating a centralized database of sustainable imaging quality improvement projects would enable knowledge sharing, prevent duplication of efforts, and streamline the implementation of best practices.
Engagement with vendors also plays a crucial role in sustainable research. Given that the supply chain accounts for a significant proportion of healthcare’s greenhouse gas emissions, fostering partnerships with manufacturers of imaging equipment and supplies can encourage development of low-carbon footprint technologies. Trainee involvement in these collaborations, guided by academic and clinical mentors, ensures that future radiologists contribute to the design and adoption of sustainable medical imaging technologies.
By prioritizing sustainability in research and QI, radiology departments can position themselves as leaders in the transition to low-carbon healthcare. This commitment not only addresses environmental challenges but also strengthens the role of radiology in delivering innovative, efficient, and patient-centred care.
Broader Implications and Future Directions
The broader implications of SusQI extend beyond individual radiology departments, highlighting its potential to transform healthcare systems as a whole. The adoption of SusQI in radiology has broader implications for the healthcare system. It encourages a shift towards preventive care, reducing the need for resource-intensive interventions.
Collaboration is also essential to advancing SusQI in radiology. Establishing national databases to share resources, prevent duplication of efforts, and facilitate knowledge exchange can drive progress and innovation. By fostering collaboration among radiologists, trainees, and healthcare institutions, these initiatives can ensure that best practices are widely adopted and continuously improved.
Leadership development is another critical component of SusQI. Introducing sustainability-focused roles in residency and fellowship programs can engage trainees and inspire the next generation of radiologists to prioritize environmental stewardship. Formal sustainability champions within academic radiology programs can mentor trainees, oversee sustainability initiatives, and advocate for system-wide changes that align with SusQI principles.
Metrics and benchmarking are critical for assessing the effectiveness of SusQI initiatives and driving continuous improvement and are still evolving. Developing standardized metrics allows radiology departments to measure the environmental, economic, and clinical impacts of their sustainability efforts (Table 2). For instance, metrics such as energy consumption per imaging study, the volume of recycled contrast agents, or the reduction in unnecessary scans provide tangible data to evaluate progress. Benchmarking involves comparing these metrics against industry standards or peer institutions to identify areas for improvement. Establishing a centralized database for sharing metrics and best practices can facilitate collaboration and knowledge exchange among radiology departments globally. Additionally, incorporating these metrics into regular performance reviews ensures that sustainability remains a priority in QI initiatives. By focusing on measurable outcomes, radiology departments can demonstrate the value of SusQI, gaining support from stakeholders and fostering a culture of accountability.
Hierarchy of Effectiveness That Could Be Implement for Future SusQI Projects.

The integration of sustainability into QI frameworks represents a transformative opportunity for healthcare systems to address the dual challenges of rising demand and environmental impact. By embedding SusQI principles into clinical practice, radiology can lead the way in delivering high-quality, sustainable care that meets the needs of both patients and the planet.
The CAR has established a Sustainability working group which has created and published a checklist for sustainability efforts within Canadian radiology departments. 22 Canadian Academic Radiology Programs, in collaboration with the CAR, as well as with their respective hospital QI Research Ethics Boards, could create a National Database of Sustainable Imaging Quality Improvement Projects, and Shared Resources. This would facilitate knowledge translation across the country as well as collaboration amongst radiologists and trainees as well as preventing duplication of efforts.
One key area of focus is the integration of artificial intelligence (AI) into radiology workflows. AI has the potential to optimize imaging processes, reduce redundancies, and prioritize urgent cases, improving efficiency and patient care. However, the environmental costs of AI, such as its carbon footprint, must be carefully evaluated to ensure that its benefits align with sustainability goals. Artificial intelligence (AI) is increasingly being incorporated into various aspects of radiology, with positive impacts on image reconstruction, efficiency of scheduling patients as well as having potential benefits of improving diagnostic accuracy. The carbon footprint associated with AI can be challenging to calculate, and research is needed to better understand the environmental costs of AI. However, when incorporating existing AI into a radiology health care system, the potential to reduce redundancy, increase patient throughput thereby reducing wait-times (affording improved equity of health care access), as well as improving patient care needs to be considered.
Conclusion
Sustainability as a domain of QI represents a transformative opportunity for radiology. By embedding SusQI principles, radiologists can deliver high-quality patient centred care while addressing environmental challenges. This integration aligns with modern healthcare’s priorities, ensuring radiology remains a sustainable and essential service in the face of global challenges.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
