Abstract
Environmental degradation and climate change pose an increasingly serious threat to global health, necessitating urgent action to implement environmentally sustainable healthcare practices. Interventional radiology (IR) is a resource-intensive specialty that has not historically emphasized environmental sustainability. This review aims to examine the environmental impact of IR and highlight opportunities for transitioning to more sustainable practices within the IR suite. The environmental impact of IR is assessed in 3 critical domains: (1) energy consumption, (2) waste production, and (3) water pollution. For each domain, actionable strategies are proposed to mitigate environmental harm. Key actions include powering down equipment when not in use, utilizing energysaving modes, minimizing the reliance on single-use items where possible, collaborating with industry to reduce excessive packaging, and implementing recycling programs for waste and iodinated contrast media, along with incorporating environmental sustainability as a quality metric in the departments quality improvement program. Barriers to adopting environmentally sustainable changes include a lack of awareness, financial considerations, and the absence of government, institutional, and industry regulations. Leadership from professional societies and collaboration with industry partners will be essential for driving systemic change. However, individual departments can take action to foster a culture of environmental responsibility and implement sustainable practices.
Introduction
Environmental degradation has been recognized as one of our most urgent global challenges, with widespread consequences including accelerated biodiversity loss, increased air and water pollution, pressure from rising heat, and extreme weather events. 1 The health of our planet is fundamentally linked to human health. Negative health effects associated with environmental decline include worsening cardiovascular and respiratory diseases, increased heat related morbidity and mortality, food and housing insecurity, alterations in the duration and prevalence of infectious diseases, along with a greater potential for the emergence of new diseases and worsening health inequalities, as many climate related health pressures disproportionately affect marginalized groups.2,3
As the effects of environmental degradation and climate change become increasingly evident, healthcare sectors are recognizing their roles and responsibilities in addressing this crisis. The environmental impact of the medical industry is estimated to account for 7% to 10% of carbon emissions. 4 Within the healthcare sector, radiology is a leading contributor, primarily due to the high energy requirements of medical imaging equipment and the reliance on single-use devices, many of which use excessive plastic packaging. 5 Research into microplastic pollution and its effects on human health is ongoing, but early findings suggest that microplastics could pose significant environmental and public health risks. 6 Efforts to reduce plastic production and improve waste management systems are essential to mitigating these potential harms.
Recently, there has been a growing body of literature on environmental sustainability in radiology, including the development of sustainability frameworks and expert consensus statements on best practices.2,7,8 The Canadian Association of Radiologists has issued a statement indicating that immediate and strategic action is necessary to enhance environmental sustainability and mitigate the detrimental effects of climate change and waste disposal. 7 This statement underscores the importance of minimizing the negative impacts of radiology service delivery on the environment and optimizing the environmental sustainability of radiology departments to address increasing health needs. 7
Within radiology departments, Interventional Radiology (IR) is a substantial and unique contributor to detrimental environmental impact and represents a critical area where sustainability can be prioritized. Given considerable energy consumption and waste production associated with IR procedures, interventional radiology as a specialty has the potential to adopt innovative practices that not only enhance patient care but also reduce the specialty’s ecological footprint. By embracing sustainable strategies, from energy-efficient technologies to waste reduction initiatives, interventional radiologists can contribute significantly to the healthcare sector’s efforts to combat climate change, fostering a healthier planet for future generations. This review aims to discuss the current state of the environmental impact of IR practice and highlight opportunities for improvement and ways to move toward more sustainable practices within the IR suite.
How IR Contributes to Climate Change
IR is a dynamic and innovative specialty characterized by its proclivity for solutions to complex problems, minimally invasive procedures, and improving patients’ quality of life. It is a specialty grounded in collaboration, technological advancement, and creative problem-solving. Historically, environmental sustainability has not been a priority in IR. The specialty contributes significantly to environmental burdens through high energy consumption, the need for continuously evolving technologies, waste generation, and water pollution. As the demand for IR services continues to grow, so does its environmental footprint, underscoring the urgency of addressing these issues.
To mitigate the environmental impact of IR, it is essential to adopt sustainable practices. We will discuss the current environmental impact and key opportunities in 3 critical domains: (1) energy consumption, (2) waste production, and (3) water pollution (Figure 1).
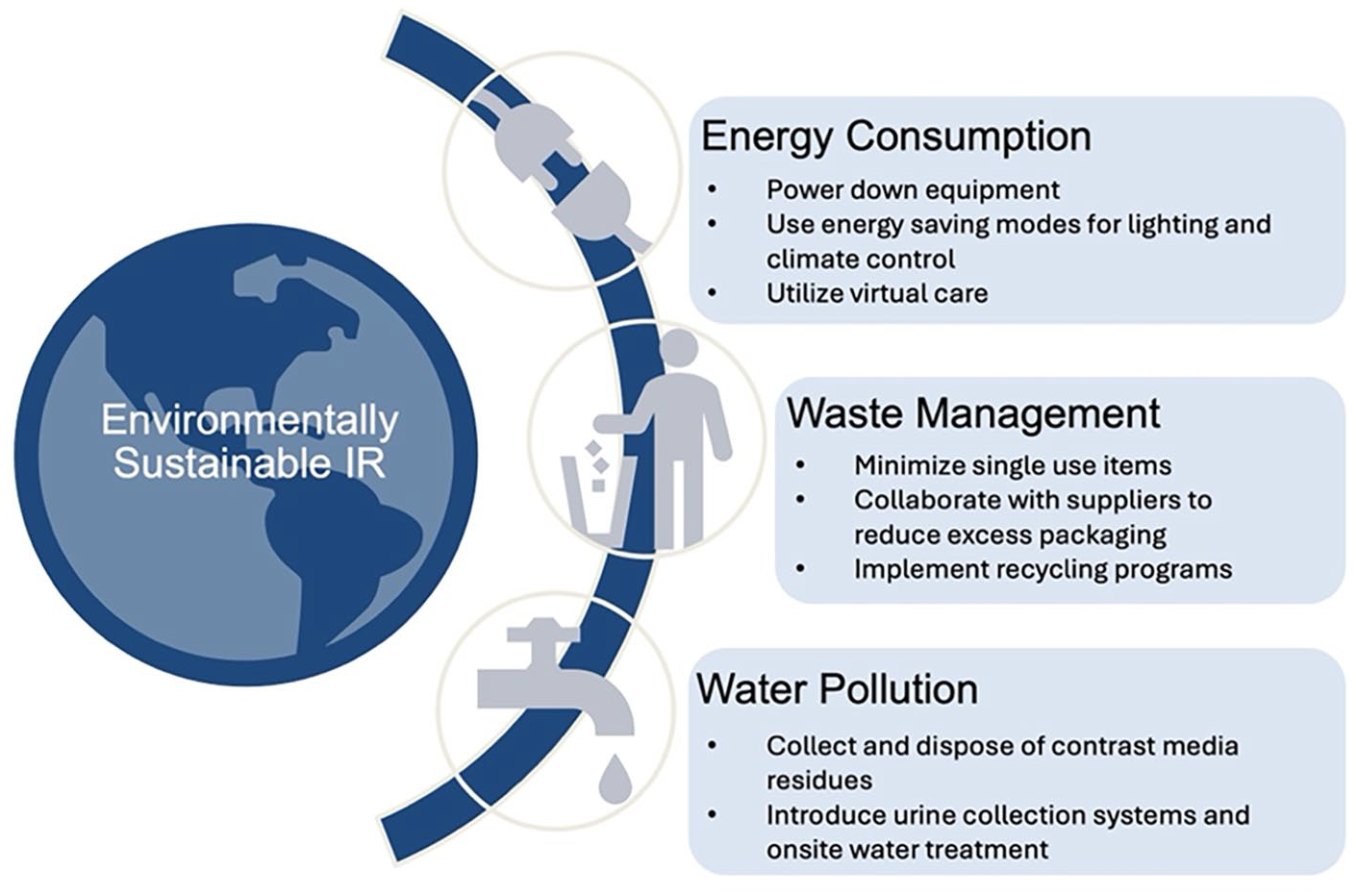
Interventional Radiology (IR) contributes to environmental burdens through high energy consumption, waste generation, and water pollution. An environmentally sustainable practice in IR can be achieved by making changes in these 3 areas.
Energy Use
Energy consumption in IR primarily arises from 2 areas: the energy expenditures associated with the operation of IR suites and those linked to patient travel for IR services. A life cycle assessment by Chua et al estimated that a tertiary care IR service produced 23 500 kg of CO2 emissions in 1 week, equivalent to the amount of CO2 absorbed by 389 tree seedlings over 10 years. 9 Climate control systems, including Heating, Ventilation, and Air Conditioning (HVAC), contributed to 49% of these emissions, with 57% of HVAC energy consumption occurring outside scheduled work hours when the IR suite was unoccupied. 9 This aligns with findings in surgical literature, where operating room climate control systems are similarly recognized as a significant source of energy expenditure and greenhouse gas (GHG) emissions.10,11 HVAC systems could be optimized to mitigate energy-related IR emissions. For example, installing occupancy sensors and adjusting climate control settings to operate within a broader temperature range during non-working hours can help reduce energy usage without compromising operational efficiency.
Medical imaging equipment such as advanced monoplanar and biplanar angiography and fluoroscopy systems accounts for another area of energy consumption in IR. While MRI and CT power consumption are typically a focus in the literature, the energy requirements of interventional imaging systems are also substantial. The mean idle-state power draw of a biplane angiography system (ARTIS icono biplane, Siemens Healthineer) is 7.4 kW compared to 3.0 kW from a conventional single-source CT scanner and 12.9 kW from an MRI scanner (on average across models). 12 Manufacturers have begun incorporating energy efficiency into their designs; newer platforms have reduced the idle-state power draw to 1.95 kW (monoplanar) and 3.44 kW (biplanar; Philips Azurion). 13
Encouragingly, energy-saving measures can significantly reduce these emissions. Vosshenrich et al found that powering down interventional imaging systems during periods of inactivity decreased power consumption by 22% to 93% without affecting the systems’ lifespan, warranties, or performance. 12 Vendors now recommend consistent shutdowns during overnight hours and idle periods exceeding 1 hour. For example, a Philips Azurion system consumes 0.26 kW in shut-down mode, an 87% reduction in energy usage compared to the ready state. 13 Implementing such practices can yield substantial energy savings—up to 39 000 kWh annually—equivalent to a reduction of 5 metric tons of CO2 emissions and $10 000 USD in electricity cost savings. 12
In addition to the energy expenditures related to IR suite operations, patient travel for IR procedures also has an environmental impact. Patients undergoing comprehensive oncology, vascular, and vascular malformation procedures in IR receive ongoing clinical follow-up care. Various international societies, including the Canadian Association of Interventional Radiology, have promoted this shift in practice.14-16 GHG emissions related to patient travel are significant. A meta-analysis provides a wide range of GHG emissions per visit of 0.69 to 190 kg CO2/visit. 17 Given the geographical spread and the concentration of advanced IR care primarily in large urban centres, patient travel to these centres likely contributes significantly to the overall GHG emissions of an IR department.
Tele-medicine is a potentially useful solution to reduce patient travel follow-up GHG emissions in IR. Shifting to virtual care through telemedicine has been reported to save an average of 11.3 kg of GHG emissions per patient visit. 18 The use of tele-medicine increased dramatically during the COVID-19 pandemic out of necessity. The utility of such tele-medicine visits varied between sub-specialties, with psychiatry, medicine, and oncology shifting the most to virtual care, and surgical specialties shifting the least. The interventional oncology sub-population of patients is a likely good candidate for virtual follow-up care. Most of the follow-up care is led by the patient’s symptoms and follow-up imaging, with the physical exam contributing a minor role. With the venue of provincial-based generalized access to imaging, coordination of follow-up imaging close to the patient’s city of residence can significantly reduce emissions. In contrast, peripheral vascular and vascular malformation patients do benefit from in-person physical examination. Coordination of clinical follow-up with same-day imaging could reduce unnecessary travel GHGs emissions.
A study by Paquette and Lin investigating the impact of tele-medicine services in follow up of vascular surgery patients found that for 146 telemedicine encounters, there was an estimated 1632 kg of CO2 emissions and 194 gallons of gas saved due to reduced travel. 19 The impact of implementing a centralized system for imaging follow up versus traditional outpatient imaging follow up was investigated by Peres et al. 20 In this study, surveillance imaging was performed at a site local to the patient and was reviewed centrally by a dedicated surveillance team. Over 5 years, it was estimated that 3718 traditional outpatient appointments were avoided, resulting in a travel reduction of 248 173 km, savings of US$76,969 in fuel costs, and a decrease of 146 tons in CO2 emissions. 20 By coordinating imaging follow-up closer to the patient’s home and utilizing virtual follow-up appointments where appropriate, the energy expended on transportation can be minimized. This approach not only lowers the carbon footprint but also enhances patient convenience and should be routinely implemented for IR procedural follow up where appropriate.
Further, an opportunity exists to address and minimize unnecessary imaging. This applies to Diagnostic Radiology as a whole; however, IR specifically can implement changes in terms of appropriate imaging follow up for our patients in an environmentally conscious way. This can help reduce the environmental burden in terms of energy to acquire imaging and energy associated with patient transportation. The environmental cost of different imaging follow-up strategies for IR patients is not explored in the literature. There is an opportunity for further research to characterize the energy expenditure associated with the imaging modality for follow up of various interventional procedures. Examples could include the energy difference for vascular peripheral revascularization follow-up with doppler versus CTA versus MRA, or in interventional oncology, the energy requirements for CT versus MRI for follow-up of lung/liver/renal ablations. Choosing a follow-up imaging modality with less environmental impact may become a consideration in the future.
Energy consumption also includes all the energy used by manufacturers to produce the materials we need and to deliver them to us. Manufacturers increasingly involved in reducing GHG emissions by improving energy efficiency, using of renewable energy sources and greener transport. Most of them are investigated in International Organization for Standardization (ISO) Certification. The ISO standards are designed to set out requirements that demonstrate core competencies in a wide range of related to the manufacture of products, services and products, services and systems. Companies that choose a “green way” must be supported by IR.
Waste
IR significantly contributes to hospital waste due to a high volume of short cases and frequent use of single-use items, many of which include excessive packaging. Single-use disposable medical supplies are the second largest contributor to GHG emissions in IR suites, accounting for 41% of total emissions. 9 In an audit of 17 neurointerventional procedures in the IR suite, Shum et al report an average waste generation of 8 kg per case. 21 The procedure with the highest waste burden was coiling, which produced 13.1 kg of waste. 21 Even less complex cases, such as central access and ports, generate excess waste. Brassil and Torreggiani found that 12% of PICC set components and 14% of port set components were routinely discarded. In some cases, auxiliary equipment was used in line with local practices and preferences. 22 There is an opportunity for IR to collaborate with industry suppliers to develop tailored procedural packs to minimize discarding unused equipment. Improving customized kits, containing only the materials needed for each type of procedure should be a priority to reduce waste. Additionally, interventional radiologists and technologists should clearly communicate before opening equipment to limit unnecessary waste.
Efforts should further be made to decrease reliance on single-use items and select alternatives where possible. For example, single use surgical gowns generate up to 7 times more solid waste and 2 times more GHG emissions compared to reusable gowns. 23 Switching from single-use to reusable gowns has been shown to result in substantial waste reduction. For example, one hospital reported a reduction of 63 000 kg of waste after implementing reusable gowns. 24 Switching to reusable gowns may also be associated with a small cost reduction.24,25 However, more studies are needed to compare the total cost related to reusable versus single-use gowns to take into consideration all the costs (acquisition, sterilization, disposal). A World Health Organization led review did not demonstrate any increased risk of infection between reusable and disposable gowns and drapes. 26 Despite the environmental and potential cost benefits, most IR practices in Canada utilize single-use surgical gowns.
Although there has been no reported difference in surgical site infections or wound contamination between reusable and disposable equipment in the surgical literature, 27 the reprocessing and reuse of IR equipment is controversial, the primary concern being device malfunction.28,29 For example, Oliveira et al demonstrated that the structural integrity of multiple types of catheters is lost with reprocessing. 30 Another study examining the effects of chemical cleaning and mechanical vibration during the sterilization process for guidewires, found guidewire coating and surface deterioration, rendering them unsuitable for multiple use. 31 The life cycle of IR devices and procedural equipment is not currently prioritized in the design and manufacturing processes. Manufacturers are not interested in reusing disposable instruments and often do not provide information on how they can be appropriately recycled and sterilized. Incentives or regulations are needed to promote innovation and design efforts focusing on sustainability.
One area where individual IR departments can reduce waste is through efficient inventory management. IR suites are equipped with a diverse range of inventory, some of which are rarely used but are kept available for emergencies or unexpected complications. 21 Consequently, it is common for devices to remain unused and be discarded after their expiry. 32 To mitigate waste associated with expired inventory, IR departments can adopt a “first in, first out” strategy, ensuring that older stock is utilized before newer supplies, thereby reducing the likelihood of expiration. 33 Implementing electronic database tracking software in interventional radiology departments would assist in identifying products nearing the end of their life, prevent unnecessary use of longer-lasting alternatives, and facilitate optimal stocking decisions and strategies to avoid waste while maintaining minimum product availability.
In addition to the single-use devices, a significant amount of waste arises from excessive packaging. Clements et al assessed 72 different IR products from 26 manufacturers, discovering that excessive packaging accounted for, on average, 54.8% of the total product weight, with some instances reaching as high as 89.8%. IR products and device manufacturers should be encouraged to package their products in ways that reduce the overall waste burden while maintaining device sterility. Higher packing density has been shown to lead to up to a 33% reduction in the packaging of medical supplies, resulting in less waste and lower transportation energy and costs. 34
It is encouraging that approximately 76% of IR device packaging waste is potentially recyclable. 35 However, in practice, it is often not correctly identified and is discarded with general waste. Waste misclassification results in suboptimal recycling and an increased cost of up to 20 times to treat and dispose of waste correctly. 36 Before implementing recycling initiatives for packaging materials, a waste audit should be conducted to measure and classify waste, identify local practices, and tailor solutions to local needs. For example, Brassil and Torreggiani found that the physical proximity of recycling bins to the procedural area affected proper waste segregation. 22 By strategically placing recycling bins closer to the point of waste generation and positioning clinical waste bins further away, they observed a behavioural change among staff, leading to a 60% reduction in improperly segregated waste. 22 Educational initiatives can effectively raise awareness and enhance competence in waste segregation, fostering a culture of environmental responsibility and encouraging staff to actively engage in sustainability efforts.
Plastics are a major source of worldwide pollution, and the healthcare system takes part in plastic waste production. It is estimated that by 2050, 12 000 000 kilotons of plastics will have been disposed of in landfills or the environment. 37 A recent publication highlights that Canadian policy makers recognize the urgency for concerted actions to reduce plastics, and the healthcare sector must also consider a more sustainable plastics system. 38 The focus should be on reducing consumption. Moreover, sorting plastics is a complex process, and improving user knowledge appears essential to avoid poor waste segregation.
Waste management in IR has the potential to reduce overall impact. Comprehensive studies are required to examine overall energy use and waste production and the possible effects of interventions within interventional radiology departments. Two potential, easily applicable interventions that require further study are returning to reusable/washable gowns and drapes and implementing medical supply database software that optimizes in-house stock to avoid end-of-life shelf waste.
Water Pollution
IR contributes to water pollution mainly through the use of iodinated contrast media (ICM). While essential for many diagnostic and interventional procedures, ICM poses environmental risks.39-41 After administration, 95% of ICM is excreted unmetabolized through feces and urine, contaminating the water supply. 40 Studies have found elevated concentrations of ICM (up to 100 μg/L) in rivers, streams, and sewage, as well as in ground, surface, and drinking water. 40 Any body of water affected by communal wastewater effluents servicing urban areas with diagnostic centres will likely show the presence of ICM. 41 Standard water purification methods are ineffective at removing ICM due to its high water solubility and metabolic stability. 39 This results in the formation of toxic iodinated disinfection by-products with potential cytotoxic and genotoxic risks.42-44 With global ICM consumption reaching approximately 3.5 million kg per year 40 the widespread use of ICM agents in diagnostic and interventional radiology, combined with ineffective purification techniques, leads to environmental harm.
In a review of ICM water contamination, Dekker et al discuss mitigating measures focused on the application and excretion of contrast media. 41 They propose reducing the use of contrast media by optimizing dosing protocols and collecting residues of contrast media at the point of application. 41 For instance, IR departments should implement systems to collect unused contrast media, treating it as hazardous waste to prevent it from entering the sewage system. Major contrast manufacturers commonly facilitate such a program.
Mitigation strategies to address the excretion of ICM include implementing special urine collection systems and waste-water processing techniques in hospitals. 41 The use of on-site medical waste treatment systems has proven effective in removing pharmaceuticals and contrast media from hospital wastewater before it enters the public sewage system. 45 A simple and cost-effective solution to prevent ICM water pollution is employing urine bags to collect urine from patients after procedures utilizing ICM, thereby stopping it from entering wastewater. In a pilot study where urine bags were provided to 2200 patients, wastewater measurements indicated a 45% reduction in the concentration of ICM. 41
Addressing Challenges and Key Actions Toward Sustainable IR Practices
Energy, waste, and water mitigation strategies emphasize the importance of a comprehensive approach involving healthcare professionals, manufacturers, and governing bodies to mitigate the environmental impact from IR practices. However, despite the growing evidence of the environmental harms of current practice, there is still little action for change. A study in the Netherlands by de Reeder et al found that there is a high awareness of the need for sustainability within IR but that there is still limited action. 46 They identified barriers as: (1) sustainability not being a priority, (2) a dependency on employees, and (3) factors that an individual IR department or hospital can’t change. Overall, there was a willingness to become more sustainable, but feeling that systemic barriers were limiting change. 46
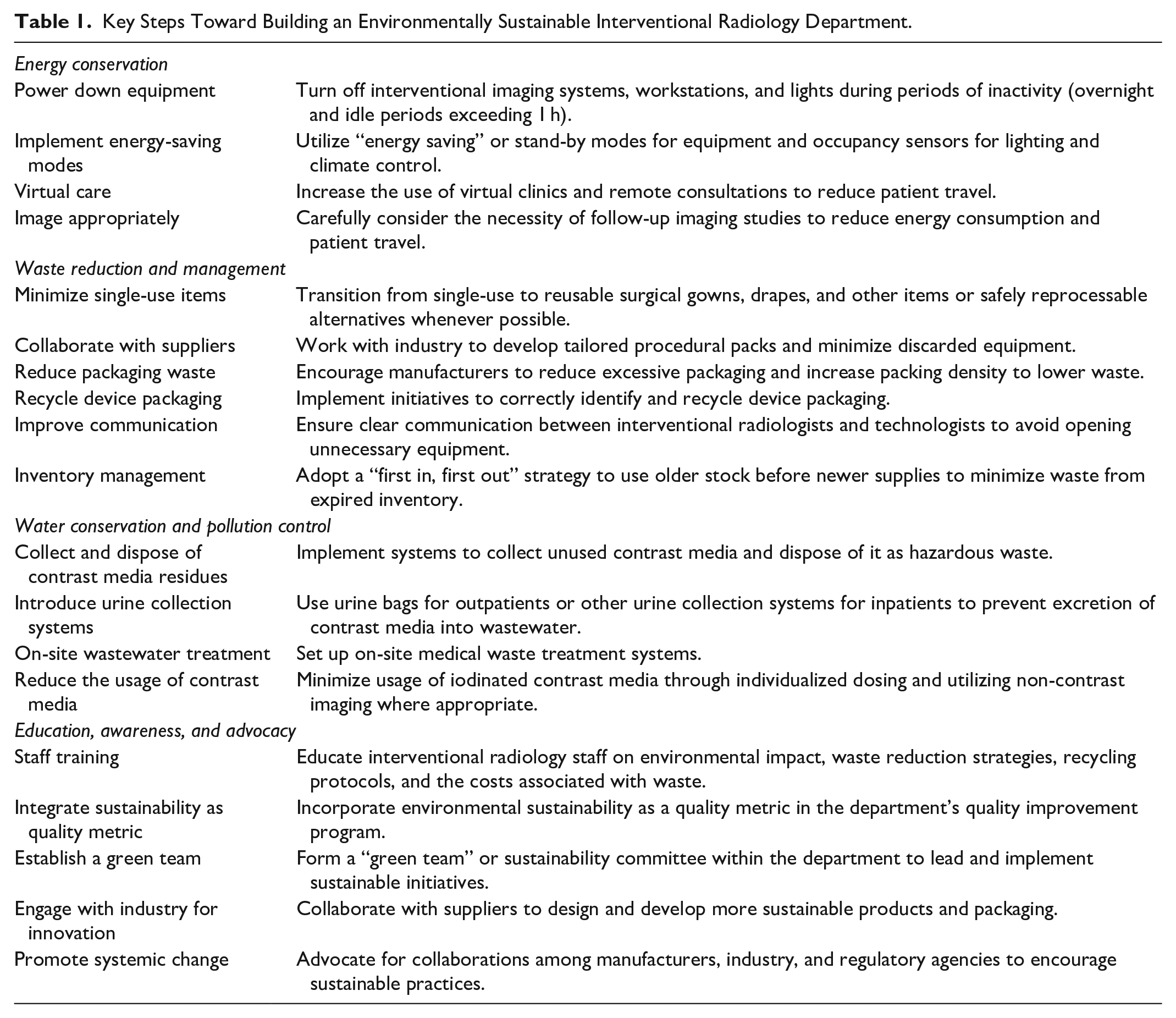
To empower IR departments to implement sustainable changes, we have compiled a list of key steps toward building an environmentally sustainable IR department (Table 1). This list can serve as a starting point, enabling departments to explore their current practices in the areas listed and implement changes as appropriate. By implementing some of these suggestions, IR departments can take actionable steps toward more environmentally sustainable practices.
Key Steps Toward Building an Environmentally Sustainable Interventional Radiology Department.
Future Steps and Recommendations
Future steps to implement sustainable IR practices in Canada will require a coordinated approach that includes collaboration among manufacturers, industry representatives, associations such as the Canadian Association of Radiologists and the Canadian Association for Interventional Radiology, as well as regulatory agencies like Health Canada. A critical step is to integrate waste reduction criteria into the request for proposals for medical supplies and equipment. This will encourage suppliers to prioritize sustainability in their offerings. Furthermore, incorporating comprehensive recycling systems into the IR suite area will facilitate effective waste management and reduce the environmental impact of IR practices.
As discussed regarding energy conservation, shutting down angiographic suites when they are not in use for significant periods and automating HVAC systems should be integrated into standard operational policies. Energy consumption and monitoring should be included as criteria during the acquisition of angiographic suites to enable departments to make informed choices that support sustainability goals. Additionally, collaboration with the provincial government is necessary to ensure proper physician compensation that encourages virtual follow-up care.
Future clinical research is necessary and should focus on comparing the overall environmental impact of IR-centred therapies with their surgical and medical alternatives. This includes evaluating interventions such as endovascular revascularization versus surgical bypass, thermal ablation compared to surgical excision, and Y-90 therapy relative to chemotherapy or external beam therapy, among others. Further research is needed to investigate the environmental implications of virtual follow-up care compared to traditional in-person clinic follow-ups.
Conclusion
As leaders in healthcare collaboration, innovation, and a willingness to disrupt the status quo, interventional radiologists must question our existing practices and explore sustainable alternatives. When you begin quantifying the waste produced and the unsustainable practices in the IR suite, it becomes difficult to align our current actions (or inaction), particularly since many of the required changes are not technically complex. Rather, they demand a collective shift in mindset and behaviour. IR can significantly reduce its ecological footprint by implementing strategies such as optimizing energy use, reducing single-use waste, and improving recycling practices. Collaborating with manufacturers to create sustainable products and packaging, alongside ongoing education and awareness among staff, will be vital in cultivating a culture of environmental responsibility. While systemic change is critical, the impact of individual and departmental efforts should not be underestimated. Each small step, every mindful change in practice, contributes to meaningful progress toward a more sustainable future for IR. Through these initiatives, IR can promote health for both patients and the planet, ensuring a healthier future for generations to come.
Footnotes
Abbreviations
GHG Greenhouse gas
HVAC heating ventilation and air conditioning
ICM iodinated contrast media
IR Interventional Radiology
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
