Abstract
Climate change is the most important challenge of this century. Global surface temperature is continuously rising to new record highs, adversely affecting the health of the planet and humans. The purpose of this article is to review the impact of climate related environmental exposures on human health, healthcare delivery, and medical imaging and explore the potential to leverage medical imaging as a non-invasive tool to advance our understanding of climate related health effects. Radiology departments and healthcare systems must focus on building resilience to the effects of climate change while ensuring that the delivery of care is environmentally sustainable. Further research is needed to refine our understanding of the effects of climate change on human health and to forecast the expected changes in the demand for healthcare and radiology services.
Introduction
Human health is intrinsically connected to the health of the planet.1,2 The triple planetary health crisis includes inter-related phenomena of climate change, biodiversity loss, and pollution. 3 Climate change refers to long-term shifts in temperatures and weather patterns, driven by human activities, primarily due to the burning of fossil fuels like coal, oil, and gas. Burning fossil fuels generates greenhouse gas (GHG) emissions that act like a blanket around the Earth, trapping the sun’s heat and raising global temperatures. The main GHGs that cause climate change include carbon dioxide and methane. Annual average surface temperature set a record high in 2023 of 1.4°C above the pre-industrial baseline. 4 Human health is impacted by changes in temperature, precipitation, weather, air quality, water quality, and food. 5 Biodiversity loss refers to a decrease in biodiversity within a species, an ecosystem, a given geographic area, or Earth as a whole. Biodiversity loss impacts human health by increasing the risk of infectious diseases emerging and spreading as well as disrupting ecosystems necessary to provide clean water, food security, and mental wellbeing from contact with nature. 6 Burning fossil fuels, wildfire smoke, and other human activities release harmful pollutants into the atmosphere. Climate change and air pollution are interconnected because air pollutants are frequently co-emitted with GHGs. 7
The triple planetary health crisis has led to increasing environmental exposures, such as extreme weather events, exposure to extreme temperatures, and worsening air pollution, adversely affecting human health. The consequences of climate change have also amplified health inequities, with the most vulnerable individuals and communities often experiencing the most significant impacts due to increased exposure to environmental hazards and limited capacity to respond. 8 At the same time, these same groups have often contributed the least to global GHG emissions, exacerbating existing health inequities. Therefore, climate justice and health equity need to be central in responding to the climate crisis by building capacity and increasing access to medical imaging globally while minimizing the detrimental environmental effects of the delivery of medical imaging care. 9
The healthcare sector consequently faces significant challenges. Climate-related environmental exposures are linked to adverse outcomes, increased use of healthcare services and economic costs. For example, air pollution contributed to approximately 8 million excess deaths worldwide in 2019, 10 and it has driven rises in emergency department visits, hospital admissions, and medical imaging usage. 11 A recent study estimated that USD 143 billion of the costs of extreme weather events can be annually attributable to climate change. 12 The harmful impacts of climate change on ecosystems, human health, and socioeconomic stability require immediate global action to build resilience as well as mitigation efforts to reduce GHG emissions. A health-centred response is needed in radiology, reinforcing the role of radiologists as physicians and emphasizing the opportunity for medical imaging to promote health and advance our understanding of climate-related health effects. 13
The purpose of this article is to review the impact of climate related environmental exposures on human health, healthcare delivery, and medical imaging and explore the potential to leverage medical imaging as a non-invasive tool to advance our understanding of climate-related health effects.
Health Impacts of Climate-Related Environmental Exposures
There is growing recognition that environmental exposures caused by climate change are independent risk factors for adverse health outcomes. These exposures include extreme weather events (eg, wildfires, droughts, hurricanes), extreme temperatures, air and water quality deterioration, altered food supply, shifting vector distributions, and social disruptions. 4 This section provides a system-based overview of current evidence on the impact of environmental exposures on human health (Figure 1). These climate-related health impacts are relevant to radiology as they impact expected findings, including incidence, severity, and patient populations impacted, along with potentially higher demand for medical imaging. As these climate-related health impacts are expected to increase in the coming years, education, training, and emergency planning are needed.14,15

Summary of human health effects associated with climate-related environmental exposures.
Cardiovascular
Climate change has detrimental effects on cardiovascular health, in particular exposure to extreme temperatures and air pollution. Air pollutants that have been linked to adverse cardiovascular outcomes include fine particulate matter with 2.5-µm or smaller aerodynamic diameter (PM2.5), particulate matter with a diameter of less than 10 µm (PM10), nitrogen dioxide (NO2), and ozone (O3). 16 Induced physiologic changes include increased heart rate, altered vascular resistance and oxidative stress, leading to inflammation, thrombosis, and ischaemia. 17 Multiple studies have demonstrated associations between extreme temperatures and air pollution with cardiovascular mortality and morbidity. A meta-analysis that included 201 studies with patient populations from different climate zones worldwide found that every 1°C increase in temperature was associated with a 2.1% increase in cardiovascular disease-related mortality. 18 In a large cohort study from California, a 10 μg/m3 increase in 1-year PM2.5 mean exposure was associated with 8% higher cardiovascular-related mortality. 19
For ischaemic heart disease, a recent large study reported odds ratios for myocardial infarction mortality associated with heatwaves and cold spells ranging from 1.1 to 1.7 and 1.04 to 1.12, respectively. 20 Similarly, for ischaemic stroke, data from a 25 country-study found that extreme cold and hot days contributed to 9.1 and 2.2 excess deaths, respectively, for every 1000 ischaemic stroke deaths. 21 Exposure to PM2.5 is also associated with myocardial infarction mortality. 20 The incidence of stroke increases by 10% for every 5 μg/m3 increase in PM2.5 levels, as shown in a study of the European ELAPSE cohorts. 22
Respiratory
Extreme temperatures and air pollution lead to respiratory disease morbidity through mechanisms of inflammation and oxidative stress. 23 High temperature exposures are linked to increased frequency and severity of asthma and chronic obstructive pulmonary disease (COPD). During Portugal’s 2006 heatwave, each 1°C increase in temperature was associated with 5% higher COPD morbidity. 24 Short-term exposure to air pollutants is associated with increased risk of respiratory infection, including pneumonia and bronchiolitis. 23 Air pollution is also associated with lung cancer morbidity and mortality, with PM2.5 exposure accounting for approximately 14% of global lung cancer deaths in 2017. 25
Gastrointestinal
Extreme weather events, air pollution, and food insecurity negatively impact gastrointestinal health. Heatwaves are associated with increased risk of inflammatory bowel disease and flares of infectious gastroenteritis, with 4.6% and 4.7% increased risk, respectively, for every additional day of exposure during a heat wave. 26 Exposure to air pollutants are linked to increased risk of metabolic dysfunction and fatty liver disease due to oxidative stress and inflammation affecting liver metabolism. 27 A cohort study involving over 227 000 individuals found that a 200 ng/m3 increase in sulphur-containing PM2.5 levels was associated with increased gastric cancer risk by 92%. 28
Genitourinary
The renal system is vulnerable to the dehydration and inflammation triggered by extreme heat. 29 Rising temperatures are linked to increased risk of kidney stones at mean daily temperatures of 29°C to 30°C. 30 A meta-analysis also reported an 11% rise in kidney failure risk and a 3% increased risk of kidney disease mortality per 1°C rise in temperature. 31 In kidney transplant recipients, short- and long-term exposure to PM2.5 were associated with increased risk of acute rejection, graft failure, and mortality. 32
Reproductive Health
Rising temperatures, air pollution, and climate-related infectious diseases adversely affect maternal and fetal health. A meta-analysis reported a 16% higher risk of preterm birth during heatwaves. 33 Extreme temperatures also increase the risk of placental abruption at term by 12%, particularly in younger, nulliparous, and socioeconomically disadvantaged women. 34 For air pollution, a 47% increase in hypertensive pregnancy was found for each 5 μg/m3 rise in PM2.5, and a 12% higher risk of preterm birth for every 10 μg/m3. 35
Neurologic and Mental Health
Extreme temperatures exacerbate dementia-related hospital admissions and emergency visits for conditions like multiple sclerosis and psychiatric disorders. 36 A scoping review of 51 studies determined that PM2.5 is a major contributor to dementia, cognitive decline, Alzheimer’s-related hospitalization, and white matter loss in the brain. 37 Similar trends were reported in Parkinson’s disease, where a large Ontario study found that long-term exposures to PM2.5, NO2, and O3 were associated with 3% to 4% increase in risk. 38 Short-term exposure to air pollutants was also linked to migraines, tension-type headaches, and increased hospital visits. 37
Musculoskeletal
Extreme temperatures and air pollution contribute to risk of injury and trauma by impairing cognition, reaction time, and decision-making. Hot summers are associated with increased mortality from traffic-related collisions. 39 A study in Edmonton found that a 13 ppb increase in NO2 was associated with a 2.2% rise in emergency department visits for injuries among males during the cold season, whereas in Toronto, the increase was 0.9%. 40 Air pollution is also associated with increased risk of rheumatologic diseases, for example, PM2.5 and NOx exposure as linked to increased risk of rheumatoid arthritis. 41
Endocrine
Extreme temperatures and air pollution have been linked to endocrine and metabolic disorders including diabetes mellitus and thyroid disfunction. 42 Heat waves are associated with increased morbidity and mortality in patients with diabetes. Higher PM2.5 exposure during pregnancy is also linked to higher maternal thyroxine levels and increased total thyroxine (TT4) levels in newborns. 43 PM2.5 exposure is also associated with higher risk of papillary thyroid carcinoma. 44
Infectious Diseases
Climate change has resulted in changes in infectious disease patterns, in particularly vector-borne diseases. 45 The environmental suitability for the transmission of multiple vectors has increased in recent decades. For example, compared to the 1951 to 1960 period, the global annual average transmission risk of dengue by Aedes albopictus increased by 46% in 2014 to 2023, and the transmission risk of Zika by Aedes aegypti increased by 10%. 4 In the same period, the land area suitable for the transmission of Plasmodium falciparum (malaria) increased 17%. 4 Mora et al found that climatic hazards have aggravated the pathogenic pathways of approximately 58% of known infectious diseases worldwide. 46
Health System Impacts of Climate-Related Environmental Exposures
In addition to the direct and indirect impacts on human health, climate-related environmental exposures also impact the delivery of health care and the health system, potentially leading to higher costs, reduced access, and lower quality of care, Figure 2. 16
Climate-related environmental exposures impact human health and the delivery of health care, potentially leading to higher costs, reduced access, and lower quality of care.
Increased Utilization of Healthcare and Radiology Services
Climate-related exposures increase utilization of healthcare services, including higher emergency department (ED) visits and hospital admissions. A study of weather disasters between 2011 and 2016 found 22% higher rates of ED utilization within the first week following an extreme weather event. 47 A nationwide study in the U.S. of approximately 22 million ED visits for any cause, showed a 7.8% excess relative risk of ED visits during days of extreme heat. 48 A study in Brazil showed that for every 10 μg/m3 increase in PM2.5, there was a 3% increase in the risk of hospital admission for respiratory diseases. 49
While all patient populations are impacted, individuals and groups who are already the most vulnerable may be impacted the most. For example, youth with asthma had 4.8% increased risk of requiring admission for every increase of 5 μg/m3 of particulate matter exposure (PM10 to PM2.5). 50 Further research is needed to identify patients at highest risk of climate-related health risks.
Higher ED visits and hospital admissions is expected to lead to higher medical imaging utilization. In a retrospective analysis of 1 666 420 medical imaging studies from 4 emergency departments in Toronto, short-term exposure to higher ambient temperature and PM2.5 were associated with overall imaging utilization increases of 5.1% and 4.0%, respectively. 11 Heat exposure days and air pollution exposure days were associated with increased utilization of radiography (excess relative risk, 2.7% and 2.1%, respectively) and CT (excess relative risk, 2.0% and 2.7%) but not US or MRI. The delivery of medical imaging also generates substantial waste and GHG emissions, thus contributing to the climate crisis. 9 Excess imaging attributed to heat and air pollution across Canada is estimated to generate excess GHG emissions of 36 261 kg CO2e/year and 40 648 kg CO2e/year, respectively, thus contributing to the worsening climate crisis in a negative feedback loop. 51 Further research on the impact of climate-related exposures on the specific utilization and costs of medical imaging services is needed to inform adaptation strategies to build resilience.
Increased Healthcare Costs
One of the consequences of higher health system utilization is higher costs related to environmental exposures. A study in Australia found that ED visits associated with exposure to high ambient temperatures in the 2012 to 2019 period resulted in an estimated USD $1.8 million in heat-attributable healthcare costs. 52 Another study estimated the costs associated with 6 climate-related events in the US between 2000 and 2009, with more than 760 000 healthcare encounters estimated to have cost the system approximately USD $740 million. 53 Healthcare systems are already facing financial pressure related to the aging population and sustained increases in utilization, thus planning is needed to ensure that health systems are able to meet the health needs of the populations they serve with budget and resource planning.
Preparedness Planning
In addition to increased costs, evaluation of and upgrades to healthcare infrastructure may be needed to manage increasing demand for health services and ability to withstand direct effects of environmental exposures. Medical imaging departments may be at increased risk of damaging effects of climate-related disasters, such as flooding, as many are located on ground-floors or basements of healthcare facilities due to requirements for shielding. Damage to infrastructure can further compromise the ability to deliver healthcare, for example during Hurricane Harvey that affected the Texas state in 2017, 60 dialysis clinics and more than 75% of the total pharmacies were closed. 54 These natural disasters may disrupt medical supply chains and may result in shortages of pharmaceuticals and other medical supplies such as intravenous contrast agents. 55
To date, climate response actions in radiology have largely focused on mitigation.56,57 Mitigation refers to human interventions to reduce GHG emissions or decrease the concentration of GHGs in the atmosphere through capture or other means of removal. Mitigation strategies in radiology include powering down equipment when not in use and abbreviating imaging protocols. 58 In parallel, adaptation and resilience actions are needed. Adaptation refers to understanding the adverse effects of climate change and acting to adjust for those effects. This includes making changes to protect healthcare buildings and other infrastructure from environmental exposures. Resilience is closely related and refers to preparing for the impacts of climate change and building capacity to recover quickly from those impacts.
There are several ways healthcare institutions can build resilience to the impacts of climate change. Some centres within Canada have already implemented strategies, such as heat and alert response (HARS) systems, which alert communities of extreme heat events and provide methods to reduce the adverse consequences of such events such as access to cooling centres. 59 Linking healthcare facilities to weather warning systems and air quality alerts can also be used for early warning to prepare for increased health system utilization related to wildfires and other natural disasters. 59
Upgrades and reinforcement of healthcare infrastructure are also needed. Departments and facilities that are prone to extreme heat can improve temperature monitoring and regulate air flow to lower the heat within buildings, thereby reducing the harm associated with heat exposure. 59 Back-up generators can be installed to power critical devices and information technology services during power outages. 59 Moreover, machinery integral to the delivery of care should be housed in protected and reliable areas within hospital centres, especially in regions prone to flooding. For radiology, multiple actions can be taken to increase preparedness. 2 Imaging devices such as CT scanners and MRI machines should be located in watertight rooms as they are susceptible to damage, are costly, difficult to repair or replace, and are essential for patient care.
Medical Imaging as a Tool to Understand Environmental Health Impacts
Medical imaging provides a unique opportunity to identify the adverse health effects of climate change non-invasively and advance our understanding of the underlying pathophysiologic mechanisms of disease. 13 To date, most of the published literature related to imaging of climate-related environmental health effects has focused on cardiovascular, respiratory, and neurologic systems. An overview of the current evidence is provided (Figure 3).
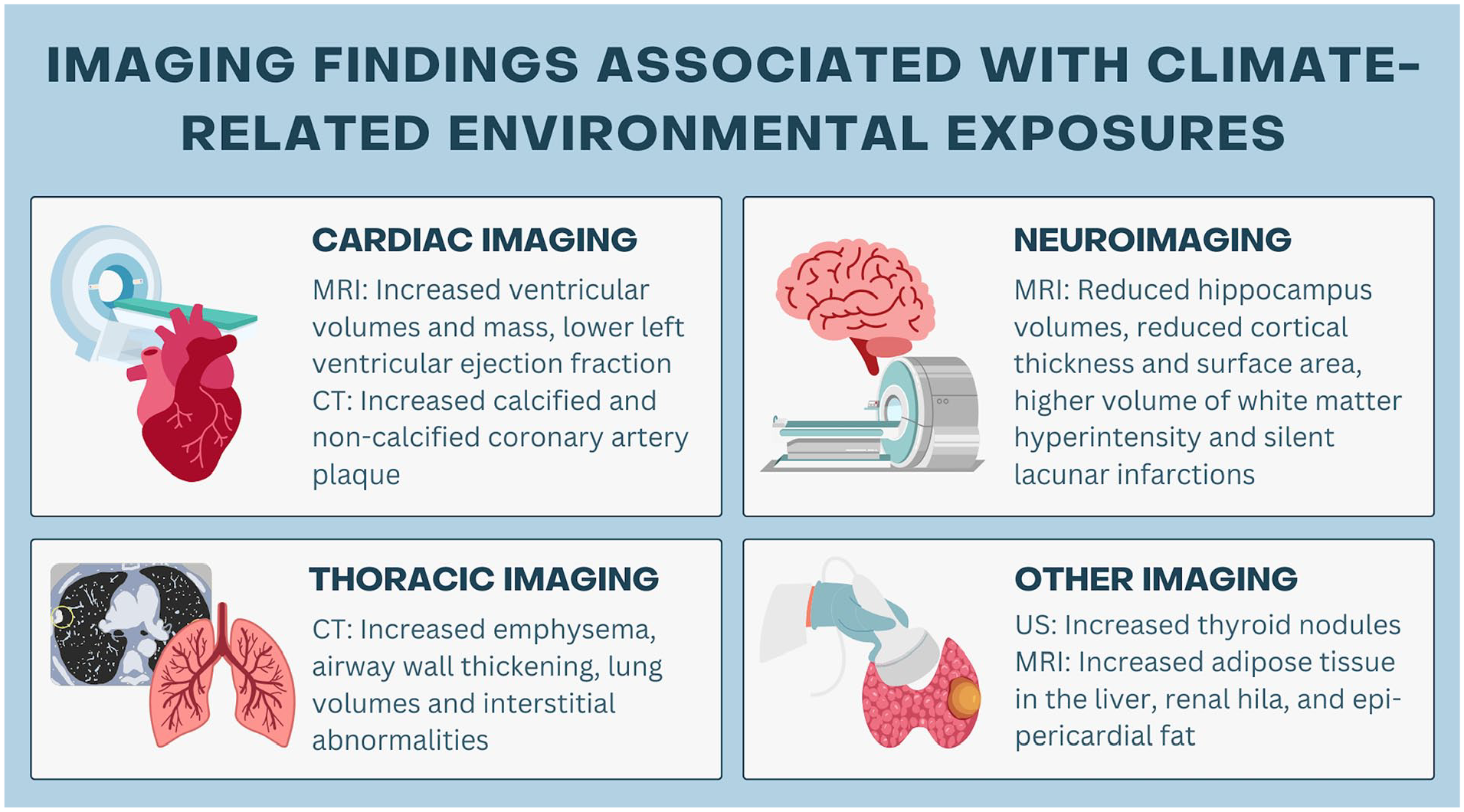
Medical imaging findings associated with climate-related environmental exposures.
Imaging of Cardiovascular Health Effects
A few prior studies have evaluated associations between extreme temperatures and air pollution with structural and functional changes in the heart using cardiac imaging. 60 For example, a study of 3920 individuals with no pre-existing cardiovascular disease demonstrated that long-term exposure to PM2.5 was associated with larger left ventricular end-diastolic and end-systolic volumes assessed by cardiac MRI. 61 Another cardiac MRI study found that nitrogen dioxide exposure was associated with higher indexed left ventricular mass and lower left ventricular ejection fraction in patients with dilated cardiomyopathy, with largest effect in women. 62 Another study found that a 6 μg/m3 increase in NO2 exposure due to traffic related air pollution was associated with 1.9% global reduction in left ventricular wall thickness assessed by MRI, with more pronounced changes in women and older patients. 63
The results of several large studies have shown positive associations between long-term exposure to air pollution and sequela of coronary disease assessed by cardiac CT. 64 The proposed underlying mechanisms include oxidative stress and endothelial damage. Wang et al reported a 27% increase in coronary calcium score per 30 μg/m3 rise in PM2.5 exposure. 65 Kilbo Edlund et al reported a 34% increase in non-calcified coronary plaque per 2.0 μg/m3 rise in PM2.5 exposure. 66
The effects of extreme temperatures have also been investigated using cardiac imaging. For example, a recent study using positron emission tomography-computed tomography (PET-CT) found that a 1.5°C increase in the body core temperature using heat exposure was associated to an approximately 2-fold increase in myocardial blood flow. 67 This suggests that heat-induced myocardial ischaemia may be an underlying mechanism of heat-related cardiac diseases.
Imaging of Respiratory Health Effects
Several studies have demonstrated associations between air pollution and CT-detected changes in lung and airway anatomy. For example, the Korean CODA cohort study identified higher indices of emphysema and airway wall thickening associated with long-term exposure to PM10. 68 Similarly, Rice et al reported increased lung volumes measured by CT in individuals residing closer to major roads. 69
Air pollution is also associated with interstitial lung abnormalities (ILA), considered a precursor of interstitial lung disease and reported in up 5% to 10% of asymptomatic individuals. 70 The MESA Air-Lung Study reported a 2.6-fold increased risk of ILA for each 40 ppb rise in NOx exposure. 71 Rice et al found a 1.2-fold increased risk of ILA and 1.3-fold risk of ILA progression for every 0.14 µg/m3 increase in elemental carbon exposure. 72
In the pulmonary vasculature, air pollution can lead to inflammation and trigger vasoconstriction and remodelling, potentially exacerbating pulmonary vascular diseases. Using CT imaging, Synn et al 73 showed a 0.3 cm3 reduction in small-vessel volumes per each 1.7 ppb increase in ozone levels, suggesting a vasoconstrictor effect of this pollutant. Aaron et al 74 reported a 0.4 cm3 increase in peripheral pulmonary vascular volume per 0.3 μg/m3 exposure to black carbon, which suggest a remodelling effect. Further research is needed to determine whether air pollution is associated with other vascular diseases, such as thromboembolic disease.
Imaging of Neurologic Health Effects
Climate environmental exposures have been linked to adverse neurologic and brain effects as assessed by imaging. These exposures can lead to structural brain changes visible on MRI scans, with proposed mechanisms including oxidative stress and inflammation induced by air pollution, and heat-related neuroinflammation and vascular dysregulation triggered by extreme temperatures. For example, a large systematic review found a strong association between air pollution and reduced brain structure volumes, cortical thickness, and surface area, particularly in the prefrontal cortex and temporal lobe, measured by MRI. 75 Outdoor particulate matter (PM2.5, and to a lesser extent PM10) may reduce hippocampal volume in adults measured in MRI, potentially contributing to memory loss, cognitive decline, and dementia. 76
Long-term exposure to air pollution can induce inflammatory cytokine release that affects endothelial function and promotes oxidative stress in the context of cerebral small vessel disease. Nanoparticle components of fine particulate air pollution can also cross the blood-brain barrier directly damaging vascular and neural structures. A study of 3257 asymptomatic Korean adults found that annual exposure to PM10 was associated with elevated white matter hyperintensity volume and silent lacunar infarctions assessed by MRI. 77
Imaging of Other Health Effects
There is currently limited imaging data of climate-change exposures in other organ systems, highlighting an opportunity for radiologists to lead further research on this topic. In the endocrine system, a large study of 4.9 million Chinese adults demonstrated that different air pollutants were associated with an increased risk of thyroid nodules identified by ultrasound. 78 The adjusted excess risk for a 10 μg/m3 increase were 6% for PM2.5, 4% for PM10, 10% for NO2, and 15% for O3. The proposed mechanisms include oxidative stress, disrupted TSH regulation and immune interactions. Increased exposures to PM10 and particle number concentration are also associated with increases in mean adipose content in multiple organs assessed by MRI, 63 including liver, renal hilus, and epi- and pericardial fat. For pancreatic fat tissue, a reduction was observed in association with air pollution exposure instead, which suggest a redistribution of fat storage mechanisms with different effects induced by air pollution in different organs.
Future Research Directions
Future research should focus on addressing knowledge gaps at the intersection of climate change, human health, healthcare systems, and medical imaging. 15 Key areas include:
Imaging of Climate-related organ sequela: Evaluation of imaging findings associated with climate change related environmental exposures in other organ systems is still needed.
Effects of Climate-change in medical imaging services: There is limited data to date related to the current and future impact of climate change on radiology departments, such as the economic costs, changes in the demand for imaging studies, and changes in the pattern, incidence, and severity of imaging findings.
Global collaboration and health inequities: The effects of climate change can vary across multiple socio-economic and geographic regions. Therefore, global collaboration in research is needed to address data gaps, particularly in low-resource settings, which are disproportionately affected.
Practical Implications for Clinical Practice and Public Health Policy
Practical steps should be implemented to address the health impacts of climate change and improve resilience in radiology:
Infrastructure adaptation and sustainable practices: Reinforce the infrastructure of healthcare facilities and radiology departments to ensure continuity of quality care through climate-resilient designs. Building and re-designing environmentally responsible imaging departments should be prioritized to reduce energy consumption without compromising image quality or diagnostic accuracy.
Preparedness and advocacy: Radiologists must be engaged with the healthcare and community systems to increase preparedness and awareness of climate change related health and health system impacts. Preparedness plans are needed to ensure health systems are connected to nationwide alert systems for monitoring and early recognition of potential surges in service demands due to unexpected climate-related events (eg, hurricanes, heatwaves).
Public health policy integration: Research is needed to inform policy decisions, especially regarding addressing health inequities and to implement tailored interventions for populations mostly affected by climate-change environmental exposures.
Conclusions
Climate-related environmental exposures adversely impact human health and the delivery of healthcare services including medical imaging. Radiology has a central role in diagnosing climate-related diseases in multiple organs. Education is needed to prepare radiologists for changing disease patterns, incidence, and severity. Adaptation strategies are needed to build resilience to the impacts of climate change in physical infrastructure and develop capacity to meet changing demands including higher imaging utilization. Medical imaging can be leveraged to advance our understanding of the underlying mechanisms of climate related environmental diseases non-invasively. Finally, further research is needed to understand climate health effects to guide policies and strategies to reduce the adverse health effects.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
