Abstract
Objectives
To determine the proportion of patients with spontaneous intracranial hypotension (SIH) who had a cerebrospinal fluid (CSF) pressure >6 cm H2O and to investigate the clinical and imaging variables associated with CSF pressure (
Methods
We retrospectively reviewed 106 patients with SIH.
Results
Sixty-one percent of patients had a
Conclusions
Normal CSF pressure is common in patients with SIH; the absence of a low opening pressure should not exclude this condition. Body habitus, symptom duration, and brain imaging are correlated with
Keywords
Introduction
Spontaneous intracranial hypotension (SIH) is an increasingly recognized disorder characterized by a loss of cerebrospinal fluid (CSF) through defects in the spinal thecal sac (1). Classically, patients with SIH exhibit low CSF pressure (
Despite the frequent observation of low
The purpose of this investigation was to evaluate the range of
Methods
Patients
Diagnostic criteria for spontaneous intracranial hypotension, modified from Schievink et al. (7).

Demographic information and clinical history, including age, sex, duration of symptoms, and history of previous EBP, were recorded from the medical records of the patients. The investigation was approved by the authors’ local institutional review board and was compliant with HIPAA regulations.
CSF pressure measurements
CSF opening pressures were obtained from procedure reports from the initial computed tomography (CT) myelogram, which is obtained as part of the standard workup in all cases of suspected SIH at our institution. Pressure was measured by lumbar puncture performed at the L3–4 or L4–5 level using fluoroscopic or CT-fluoroscopic (CTF) guidance and either a 22- or 24-gage needle with the patient in the lateral decubitus position. Pressures were measured with the patient’s legs extended, after instructions not to talk or the Valsalva maneuver. The procedures were performed by one of two board-certified radiologists with 32 and 12 years of experience in performing image-guided lumbar punctures and who held a certificate of added qualification in neuroradiology.
Image analysis
Available pre-procedural brain imaging studies were reviewed to determine whether imaging signs of SIH were present. The review was carried out in the picture archiving and communication system by a board-certified radiologist who was a second-year fellow in neuroradiology. Brain MRI was considered to be positive for SIH if pachymeningeal enhancement or brain sagging was present according to the previously reported criteria (7). Brain sagging was judged on sagittal T1- or T2-weighted images and pachymeningeal enhancement was judged on axial or coronal post-contrast T1-weighted images. Borderline cases were adjudicated by a board-certified radiologist who held a certificate of added qualification in neuroradiology and had 12 years of experience interpreting brain MRI scans and extensive experience of treating patients with SIH. If the patient had only a non-contrast brain MRI scan, then the imaging was only considered positive if brain sagging was present.
Abdominal circumference was determined from imaging obtained as part of the CTF-guided lumbar puncture using the technique reported previously by Ciudin et al. (9) This technique uses bi-dimensional diameters from CT imaging to estimate the perimeter of an ellipse and has been shown to accurately predict standing waist circumference (9). Body mass index (BMI) was not used as these data were incomplete for a large number of patients. However, it has previously been shown that abdominal circumference and BMI are very highly correlated, with one analysis of four multicenter trials showing correlation coefficients between these two measures of 0.84–0.89 (10).
Statistical analysis
Univariate analysis
The dependence of
Multivariate analysis
The joint effect of the six univariate predictors on 
The modeled outcome was the observed CSF pressure for patient
Results
Patient demographics
We identified 106 patients (69 women and 37 men) ranging in age from 18 to 83 years (mean ± SD 47.6 ± 13.2 years) who met the inclusion criteria for SIH. The mean ± SD abdominal circumference was 89.9 ± 13.8 cm (range 60.6–127.8 cm). The abdominal circumference could not be calculated in one patient because the images were technically inadequate.
A total of 44 (42%) patients had undergone EBP prior to opening pressure measurement at our institution; in all instances these patients either had no benefit from the prior EBP or had a relapse of their symptoms. Data about symptom duration were available in 95 (90%) patients. The mean ± SD symptom duration was 20.2 ± 38.5 months (range 0.3–240 months); however, the distribution was heavily skewed toward a symptom duration of <1 year, with 46% of the patients reporting symptoms of <6 months duration and 69% reporting symptoms of <12 months duration.
Brain imaging findings
Pre-treatment brain MRI data were available in 99 (93%) patients. Of those patients with available brain MRI data, 93 included both pre- and post-contrast images (94%), whereas six (6%) patients had only non-contrast images. Of the patients with available post-contrast brain images, 77 (82%) showed evidence of smooth, diffuse dural enhancement. Of all the patients with brain images, 60 (60%) showed evidence of brain sagging. A total of nine (9%) patients showed neither dural enhancement nor brain sagging on MRI and thus were considered to show no evidence of SIH on brain imaging.
Distribution of CSF pressure
Figure 1 shows histograms of the Histograms of 
CSF pressure correlations
Figure 2 shows the univariate analyses of categorical variables (i.e. positive brain MRI, prior EBP, and sex) and Figure 3 shows the continuous variables (i.e. duration of symptoms, abdominal circumference, and age). Table 2 gives the estimated effects from the multivariate model of Univariate analysis of categorical variables. Box-and-whisker plots comparing dependence of Univariate analysis of continuous variables. Scatterplots of dependence of Estimated effects from multivariate modeling of 

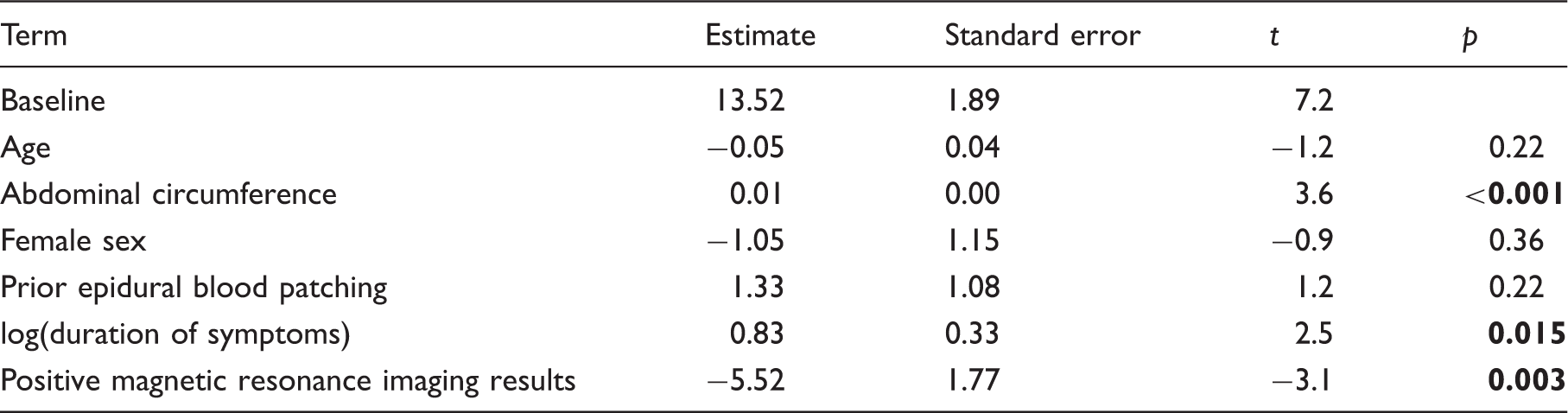
Abdominal circumference was positively correlated with
The correlation between
Female sex was marginally correlated with lower opening pressure on univariate analysis (
Even for those terms that were found to be strongly correlated with
Discussion
SIH has historically been understood to be a direct manifestation of low CSF pressure caused by leaks of spinal CSF. Despite this understanding, previous investigators have reported that, in some patients, the CSF pressure may be normal rather than low, observations that led Mokri (11) to propose the alternative terminology of CSF hypovolemia rather than intracranial hypotension for the syndrome. Still, the finding of
In contrast with conventional assumptions about CSF pressure in patients with SIH, only 34% of patients with SIH in our series actually had a low CSF pressure ( A 37-year-old woman presented with a positional headache and a cerebrospinal fluid (CSF) opening pressure of 20.4 cm H2O. (a) Axial image from computed tomography myelogram obtained immediately after opening pressure measurement showing active leakage of CSF into the epidural space (arrowheads). (b) Sagittal image from the same computed tomography myelogram showing a calcified disk protrusion in the upper thoracic spine (arrow). Subsequent digital subtraction myelogram (not shown) confirmed that the CSF leak originated at this level. (c) Intraoperative photograph showing the dural tear (arrow) caused by the disk (photo courtesy of Wouter Schievink).
Our results differed from those of several previous smaller series. In a series of 40 patients with SIH diagnosed on the basis of orthostatic headache and diffuse dural enhancement on MRI, Mokri et al. (3) reported that normal pressure was only seen in seven (18%) patients. In a series of 30 patients with SIH, Chung et al. (12) found only four patients with opening pressures of >6 cm H2O and, of these four, only one had a pressure >10 cm H2O. In that series, patients were considered to have SIH if they demonstrated at least two criteria including orthostatic headache, low CSF pressure, or diffuse dural enhancement on MRI.
In a more recent series in which the opening pressure was measured in 76 patients referred for clinically suspected SIH, Luetmer et al. (13) found that 43% of patients had a pressure between 10 and 18 cm H2O and 8% had a pressure >18 cm H2O, results similar to our findings. These varied observations regarding the frequency of normal
To help explain the spectrum of pressures observed in our patients, we examined several factors that could potentially influence
The effect of obesity on CSF pressure in normal patients remains controversial, with some studies showing a positive correlation between increasing CSF pressure and BMI and others showing no association (15–18). Of the variables investigated in our model, however, abdominal circumference was most strongly correlated with
It is possible that some patients with clinical symptoms of SIH, but normal
Duration of symptoms was also associated with
Our investigation found significant correlations between the absence of brain imaging findings (i.e. either dural enhancement or brain sagging) and
Despite these physiological relationships, it is well known that brain imaging changes are not present in all patients with SIH (27). This may be of clinical significance because some evidence suggests that patients with clinical symptoms of SIH who lack MRI changes may be more refractory to treatment (28). It is equally notable that
Specifically, it is likely that brain imaging findings in SIH are reflection of decreased CSF volume rather than a direct manifestation of low CSF pressure (11). Although, under normal circumstances, CSF volume and pressure are related by a monoexponetial curve (29,30), this relationship seems to be altered some cases of CSF leak – for example, some patients with myelographic CSF leaks (and therefore decreased CSF volume) have a normal CSF pressure. Compensatory mechanisms such as dilation of the intraspinal and intracranial venous structures, a process known to occur in SIH (25,31), could alter the compliance of the craniospinal compartment, thus altering the relationship between CSF pressure and volume. Changes in the relative rates of CSF production and reabsorption could also potentially affect this relationship. Greater understanding of these effects could potentially help in the management of patients with SIH refractory to treatment, as well as with the development of novel alternatives to epidural patching or surgery for those with the disease. Although it is beyond the scope of this investigation, further exploration of the relationships between individual brain imaging signs, myelographic findings, CSF pressure, and symptom duration in patients with SIH is also warranted.
Several factors may influence the reliability of a single CSF pressure measurement, potentially adding to the variation we have observed in our study cohort. It has been hypothesized that some cases of SIH may be due to intermittent leaks (32), which could, in theory, result in variability in the measured CSF pressure depending on whether the leak was active. However, a previous study by Luetmer et al. (13) showed that active CSF leakage on myelography was not associated with a lower CSF pressure than in patients in whom no leak was seen. This suggests that whether a leak was continuous or intermittent did not have a large effect on the CSF pressure. Another potential confounder may be the variability in CSF pressure in an individual patient throughout the day, a phenomenon suggested previously (33).
We conclude that
It is important to note that our multivariate model fitted our data moderately poorly (
This investigation has several limitations. First, our practice at a tertiary care referral center introduces the potential for referral bias, possibly selecting for some atypical variations in
Conclusions
Normal CSF pressure is common in patients with SIH; the absence of a low opening pressure should not be used to exclude the condition.
Clinical implications
CSF pressure >6 cm H2O is common in patients with spontaneous intracranial hypotension. Absence of a low opening pressure should not be used to exclude the condition. CSF pressure should be interpreted in the context of brain imaging findings and myelographic evaluation for CSF leakage in patients with symptoms suggestive of spontaneous intracranial hypotension.
Footnotes
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
