Abstract

LGBTQ+ is an acronym describing sexual orientations and gender identities, such as lesbian, gay, bisexual, transgender, and queer/questioning, as well as any other expressions of sexual orientation and gender (e.g. asexual, pansexual, intersex, two-spirit, gender non-conforming, gender fluid). 1 Individuals who are identified as LGBTQ+ face many health-related disparities. LGBTQ+ identifying individuals report higher rates of obesity,2,3 smoking, 4 and risks for cardiovascular disease 5 compared with straight identifying people. Additionally, LGBTQ+ identifying people are often enrolled in health insurance plans at a lower rate than straight identifying individuals. 6 In 2011, the National Transgender Discrimination Survey (NTDS) was conducted by the National Center for Transgender Equality and National Gay and Lesbian Task Force. 6 Key health-related findings are outlined in Table 1. Results of the survey indicated that more than a quarter of transgender or gender non-conforming individuals have been subjected to harassment in a medical facility, including doctors’ offices, emergency rooms, and other healthcare settings. 6 The report also indicated that 41% of transgender or gender non-conforming individuals had attempted suicide at least once. 6 This proportion indicates a major health-related disparity for transgender and gender non-conforming people, especially when only 5% of a generalized sample of Americans and 2.7% of a global sample have reported attempting suicide. 7
Key health-related findings of the 2011 National Transgender Discrimination Survey, conducted by the National Center for Transgender Equality and the National Gay and Lesbian Task Force. 6

In December 2010, the US Department of Health and Human Services released Healthy People 2020, a set of 10-year goals and objectives to promote health and prevent disease for Americans. 8 One goal aimed to improve the health, safety, and well-being of lesbian, gay, bisexual, and transgender (LGBT) individuals. 8 Similarly, the United Nations (UN) adopted the 2030 Agenda for Sustainable Development in September 2015, pledging to work toward a world that provides economic, health, and legal equity for all, including LGBTQ+ identifying people. 9 Many international agencies and non-profit organizations aim to improve health equity for LGBTQ+ identifying people across the globe, including the World Health Organization, 10 Human Rights Campaign Global, 11 and OutRight Action International. 12 Despite these efforts, LGBTQ+ identifying people continue to face many forms of discrimination such as racism, sexism, and classism. The intersectionality of these multiple forms of discrimination cumulate and overlap, contributing to the overall experiences of individuals and groups 13 (Figure 1). For LGBTQ+ identifying people who require orthotic and prosthetic (O&P) care, it is possible that the intersection of sexual orientation, gender identity, and physical abilities creates a unique experience of discrimination.
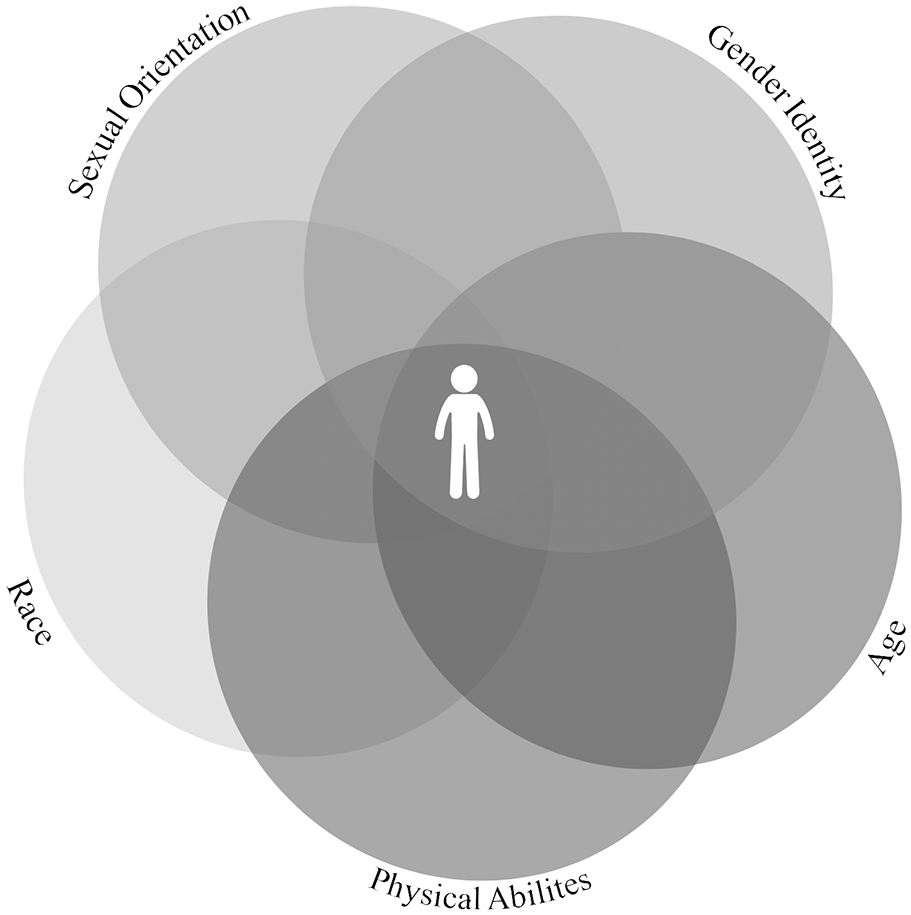
A variety of characteristics and modes of discrimination contribute to the experience of every individual—though there are far more traits that contribute to discrimination a person may face than are included in this figure. This editorial seeks to describe the intersectional experience of sexual orientation, gender identity, and physical abilities for LGBTQ+ identifying individuals who require orthotic and prosthetic care.
Knowledge and understanding of LGBTQ+ health concepts are the first step to providing culturally competent care for LGBTQ+ identifying people. 14 Evaluation of the attitudes of providers and suggestions for integrating LGBTQ+ health-related content and cultural considerations has been explored in various healthcare fields, including medical schools,15,16 nursing, 17 physical therapy, 18 and occupational therapy. 19 However, these concepts have yet to be evaluated and implemented in O&P education, clinical care, and research. It is essential that the field of O&P stays at the forefront of creating safe, affirming, and comfortable healthcare environments for LGBTQ+ identifying people. As such, this editorial aims to introduce the health-related experiences of LGBTQ+ identifying patients and suggest ways O&P students, educators, practitioners, and researchers can advocate for LGBTQ+ identifying individuals.
Incorporating LGBTQ+ healthcare concepts into O&P education
Integrating LGBTQ+ population-specific concepts into the curriculum for healthcare students positively impacts the awareness, understanding, and skills required to care for LGBTQ+ identifying patients. 17
A 2018 study 17 described a framework for introducing LGBTQ+ healthcare concepts to students in a baccalaureate nursing program. At the conclusion of the program, all participating nursing students (n = 13) perceived an improvement in their communication style with LGBTQ+ identifying individuals, increased knowledge of the health-related needs of this population, and ideas about changes they could make to better serve LGBTQ+ identifying people. 17 Similarly, a review of academic medical programs indicated that students who enrolled in 13 medical schools across the United States were positively impacted by the components of their curriculum discussing LGBTQ+ healthcare concepts, suggesting these components increased their knowledge of this population’s needs and better prepared them to care for LGBTQ+ identifying people in their careers as physicians. 15
Integrating information regarding the healthcare needs, health-related disparities, and strategies for communicating with LGBTQ+ identifying individuals into O&P educational curricula would likely be an effective means of improving care for this population. Integrated learning objectives should include
Introduction of the many sexual orientations and gender identities experienced by LGBTQ+ identifying individuals.
Discussion of the unique health-related disparities that LGBTQ+ identifying individuals face, including increased rates of obesity, smoking, and suicide.
Sensitivity to the process LGBTQ+ identifying individuals experience while coming out and knowledge that sexual orientation and gender identity are fluid and may change over time.
Improvement of communication skills, both while interacting with LGBTQ+ identifying individuals and while affirming the identities of LGBTQ+ identifying patients to family, colleagues, and other members of the healthcare team.
Experiential learning with LGBTQ+ identifying individuals should also be included in O&P curricula, as interactive sessions have shown to be beneficial in other healthcare programs. 17 These experiences can take many forms, including
Interaction with patient models who are identified as LGBTQ+ to allow students to practice communication and evaluation and learn from mistakes in a controlled scenario.
Peer-to-peer teaching regarding topics related to the needs and care of LGBTQ+ identifying patients.
Discussion-based seminars or panels with LGBTQ+ identifying individuals allowing students to ask questions and increase knowledge from firsthand accounts of individual experiences.
Validating and treating LGBTQ+ identifying patients in O&P practice
Creating a safe, comfortable environment to receive medical treatment is of particular importance to LGBTQ+ identifying individuals. 20 A 2010 report indicated that 56% of lesbian, gay, and bisexual identifying adults and 70% of transgender identifying adults had experienced some type of discrimination in a healthcare setting. 21 Similarly, 29% of lesbian, gay, and bisexual identifying adults and 73% of transgender identifying adults perceived that they would be treated negatively by healthcare providers if they were open about their sexual orientation or gender identity. 21 These factors present a barrier for LGBTQ+ identifying individuals seeking care, with some outright avoiding visiting medical facilities unless absolutely necessary for fear of the harassment they may face. 6
It is essential that O&P care providers and clinical staff are aware of methods to encourage inclusivity, promote well-being, and prevent discrimination of LGBTQ+ identifying patients. Some strategies for creating a more inclusive O&P care-delivery environment20,22 are to
Provide continuing education to all members of the clinic to increase knowledge and provide suggestions for improving O&P care for LGBTQ+ identifying patients.
Expand intake forms to include more gender terms and identity options, preferred name, and personal pronouns. An example patient intake form is shown in Table 2.
Wear a lapel pin or sticker when visiting patients stating your own personal pronouns (e.g. she/her, he/him, they/them, zie/zim); not only does this allow patients to address you correctly but also invites LGBTQ+ identifying patients to be comfortable discussing gender identity and personal pronouns with you.
Designate a single-stall restroom in the clinic as “Gender Neutral” to prevent the discomfort associated with using a restroom that does not align with one’s gender identity.
Place a “Safe Space” emblem or rainbow flag in a window or at the front desk indicating to LGBTQ+ identifying patients they are safe to discuss elements of sexual orientation and gender identity in the practice without judgment.
Draft or amend a non-discrimination policy barring discrimination on the basis of sexual orientation or gender identity in the practice and provide the policy to all patients at check-in.
Affirm the identities of LGBTQ+ identifying patients within the care team; for example, use the patient’s personal pronouns and preferred name when communicating with other members of the treatment team.
Avoid asking questions or pushing for information regarding an individual’s sexual orientation or gender identity not essential for the treatment of the patient. While it might be important for an O&P clinician to know an LGBTQ+ identifying individual’s personal pronouns and whether they smoke, it is likely not necessary for an O&P clinician to collect a patient’s sexual history or inquire as to whether the patient has any sexually transmitted infections.
Example patient information intake form with LGBTQ+ affirming options.

Supporting LGBTQ+ identifying people in O&P research
Researchers in orthotics and prosthetics, rehabilitation medicine, and other areas of healthcare also have a responsibility to affirm and support LGBTQ+ identifying research participants. A set of standards for conducting research with LGBTQ+ identifying people 23 describes techniques researchers can use to ensure LGBTQ+ identifying individuals feel comfortable and advocated for in O&P and related research. Suggested methods are to
Include a variety of gender and personal pronouns options on consent documents, research forms, and surveys, and include a fillable “Other” option to capture information from those who do not ascribe to the provided options.
Utilize person-first terminology in grants, protocols, and research documents to avoid pathologizing sexual orientation and gender identity (e.g. “participants who are identified as LGBTQ+” rather than “LGBTQ+ participants”).
Be aware of and maintain continuity in the differences between sexual orientation (e.g. lesbian, gay, bisexual) and gender identity (e.g. man, woman, non-binary) when speaking to and interacting with research participants.
Maintain privacy from other research participants, family members, and so on to allow research participants to be as open about their sexual orientation and gender identity as they feel comfortable in the context of the study.
Avoid bias when preparing findings for dissemination and ensure findings are free from assumptions and generalizations regarding sexual orientation and gender identity.
Remain aware of implicit cultural biases or stereotypes and work consciously to avoid these interfering with O&P research.
The 7th edition of the Publication Manual of the American Psychological Association added guidelines on bias-free writing seeking to encourage inclusivity and respect in scientific writing for all people. Chapter 5: Bias-Free Language Guidelines 24 outlines specific techniques for writing about people with varying sexual orientations and gender identities; some techniques are summarized here:
Understand the difference between “gender” (i.e. the traits, characteristics, and roles an individual ascribes to based on the psychological and cultural interpretations associated with being a “man,” “woman,” or something else) and “sex” (i.e. the biological sex assigned to an individual at birth, typically “male,” “female,” or another variety of biological sex)—and use terms with precision, as gender and sex terms are not interchangeable.
Unless describing differences due to biological sex, use gender terms to categorize subjects based on their personal gender identities. For example, when reporting subject inclusion in an abstract or manuscript, write “10 men, 14 women, and 2 non-binary participants were included in the study.”
Reduce bias using the singular “they”—rather than “he,” “she,” or “(s)he”—when writing about a hypothetical subject or when the gender of the subject or subjects is not relevant.
Avoid terms and phrases that imply only two genders or two sexes and opt instead for phrases describing a spectrum of sexual orientations and gender identities (i.e. “people of other genders” instead of “people of the opposite gender”).
Gaining awareness and insight into the experiences of LGBTQ+ identifying individuals will allow all in the field of orthotics and prosthetics—students, clinicians, researchers, and beyond—to advocate for and affirm the unique identities of LGBTQ+ identifying people. At the time of publication, no information has been reported regarding the experiences of LGBTQ+ identifying people in O&P educational, clinical, or research settings; much work remains to ensure that LGBTQ+ identifying people in all O&P domains are receiving fair treatment and are not subjected to harassment and discrimination. The outlined suggestions and techniques are only a starting point and, as such, a supplemental list of additional resources is also included (supplemental material). The author strongly encourages readers to delve deeper into works referenced in this editorial; seek ways to create welcoming and inclusive educational, clinical, and research environments; and encourage others to expand their knowledge to improve the experiences of LGBTQ+ identifying people in O&P.
Supplemental Material
10.117_0309364620954954_Supplemental_Material – Supplemental material for Affirming LGBTQ+ identities in orthotics and prosthetics education, practice, and research
Supplemental material, 10.117_0309364620954954_Supplemental_Material for Affirming LGBTQ+ identities in orthotics and prosthetics education, practice, and research by Nicole R Walker in Prosthetics and Orthotics International
Footnotes
Acknowledgements
The author would like to acknowledge John M. Looft, PhD; Sally DiBello, MPO, CPO, LO; and Maya Gougeon, MS, CPO, for their efforts and time spent supporting the writing of this editorial.
Author Contributions
NW - Conceptualization, Writing – original draft.
Declaration of Conflicting Interests
The author(s) disclosed no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed that they received no financial support for the research, authorship, and/or publication of this article.
Supplemental material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
