Abstract
Background:
Orthoses are a well-known intervention for the treatment of thumb osteoarthritis; however, there is a multitude of orthotic designs and not enough evidence to support the efficacy of specific models.
Objective:
To examine the influence of different orthoses on pain, hand strength, and hand function of patients with thumb osteoarthritis.
Study design:
Literature review.
Methods:
A scoping literature review of 14 publications reporting orthotic interventions for patients with thumb osteoarthritis was conducted. Functional outcomes and measures were extracted and analyzed.
Results:
In total, 12 studies reported improvements in pain and hand strength after the use of thumb orthoses. Comparisons between different orthotic designs were inconclusive.
Conclusion:
The use of orthoses can decrease pain and improve hand function of patients with thumb osteoarthritis; however, the effectiveness of different orthoses still needs support through adequate evidence.
Clinical relevance
Multiple orthoses for thumb osteoarthritis are available. Although current studies support their use to improve pain and hand function, there is no evidence to support the efficacy of specific orthotic designs. Improved functional outcomes can be achieved through the use of short orthoses, providing thumb stabilization without immobilizing adjacent joints.
Background
Thumb carpometacarpal osteoarthritis (CMC OA) is one of the most common diseases affecting the hand, 1 with up to 36% of the general population presenting radiographic signs of joint degeneration. 2 Due to the unique role of the thumb in grasp movements, CMC OA can lead to severe limitations in daily living activities due to pain, limited joint mobility, reduced grip strength, and restricted hand function.3–5
Although the articular damage caused by OA is a combination of mechanical abnormalities and systemic predisposition, 6 the lack of joint stability provided by hand muscles and ligaments is highlighted as one of the main contributing factors to CMC OA pathology.7 –9 Thumb displacement during opposition and pinching movements can lead to increased contact stress between articular surfaces, further compromising the joint integrity and hand function.7,10,11
Rehabilitation strategies for CMC OA management focus on symptom alleviation, through a combination of exercises, patient education, and the use of orthotic devices. 12
Considered a primary option of treatment for thumb OA, orthosis interventions aim to provide mechanical support to the CMC, reducing pain and facilitating hand function, without limiting the movement of adjacent, unaffected joints. 13
Systematic reviews conducted in the past 10 years unanimously reported evidence to support the use of orthoses to reduce hand pain.1,3,4,11,14 –16 However, despite the advent of increasing number of quality clinical trials, the impacts of different orthotics for the thumb CMC on hand pain, strength, and hand function are still controversial. Different approaches regarding joint positioning, orthosis length, fabrication material, and dosage for use have given rise to a multitude of orthosis designs, making the comparison of intervention studies a problem. 3
Studies that aimed to evaluate the association between the use of orthoses for CMC OA and hand function presented a high-risk bias, which did not support comparisons through a systematic review and meta-analysis.1,3,4,15 The fact that many studies on orthotics for the CMC joint are not randomized clinical trials restricts the number of publications considered for systematic reviews, 4 precluding a broad investigation into the current challenges of orthotic research. Scoping reviews can be used to address the many types of evidence available in a particular area, with a broader coverage than traditional review studies. 17
Given the existence of a variety of strategies for the use of orthotics in CMC OA treatment, this scoping study aimed to investigate the influence of different thumb orthosis designs on pain, hand strength, and hand function of patients with CMC OA.
As secondary objectives, we examined the differences described in thumb OA literature regarding orthotics wearing instructions, materials used for fabrication, and patient adherence to orthotic use.
Methods
The five-stage framework for scoping reviews outlined by Arksey and O’Malley 17 (identifying research questions; identifying relevant studies; selecting the study; charting the data; and collating, summarizing, and reporting results) was used in this study. Two independent authors (P.A. and T.B.P.) conducted separate literature searches to identify studies that evaluated the influence of orthotics as a treatment for OA of the thumb CMC. For research questions, this study investigated the following:
What orthotic devices are described for patients with thumb osteoarthritis?
What is the impact of the different existing orthoses in CMC OA patients’ pain, hand strength, and hand function?
Are there outcome changes when using different orthotic designs or materials?
What are the existing trends for orthotic dosage?
Is the dosage related to functional outcome?
MEDLINE, CINAHL, EMBASE, SCOPUS, PEDro, and OTSeeker databases were searched for articles published from their inception until September 2015, with the following keywords: Osteoarthritis, Arthrosis, Thumb, Carpometacarpal Joint, CMC, and Trapeziometacarpal Joint combined with Orthosis, Orthoses, Orthotics, Splints, or Braces.
Manual searches for studies listed in reference sections of relevant articles and additional publications were also conducted, as well as gray literature search to identify all possible studies not found by this search strategy.
The selection of studies was based on (a) the use of orthotics as a treatment modality for patients older than 18 years, diagnosed with thumb CMC OA; (b) which results reported at least one functional outcome, measured by a standardized assessment; and (c) who included a description of the orthotic design selected for the study. Only articles published in English were included. Since the use of orthoses for OA is described by many authors as a primarily conservative treatment,1,7,11,14,18 studies on interventions with patients who underwent surgical procedures were excluded from the review. Publications that only described orthotic design and rationale guidelines for both orthosis fabrication and CMC OA treatment that did not aim to evaluate the influence of orthoses on functional outcomes were also excluded.
After the initial search, retrieved publications were independently screened for the identification of relevant studies, based on title and abstract. Eligible articles that satisfied the inclusion criteria were cross-referenced and underwent a full-text review.
Key information was collected and organized in a structured form, according to the following headings: first author, title, year of publication, study design, sample size, orthoses details, and wearing instructions. Study objectives and outcomes were also collected. Any discrepancies regarding selected articles were resolved on consensus basis after data extraction.
For this study, the description of orthotic models was based on the Splint Classification System,19,20 describing orthosis location, involved anatomic parts, kinematic function, the purpose, and number of joints included in the design. Additionally, we included information regarding orthosis type (custom-made or prefabricated), material (thermoplastics, neoprene, elastic fabric, rigid, or soft), and the anatomical base of orthotics, as suggested by O’Brien and McGaha. 21
Results
Study characteristics
All information regarding selected studies is described in Table 1.
Description of studies and orthotics.
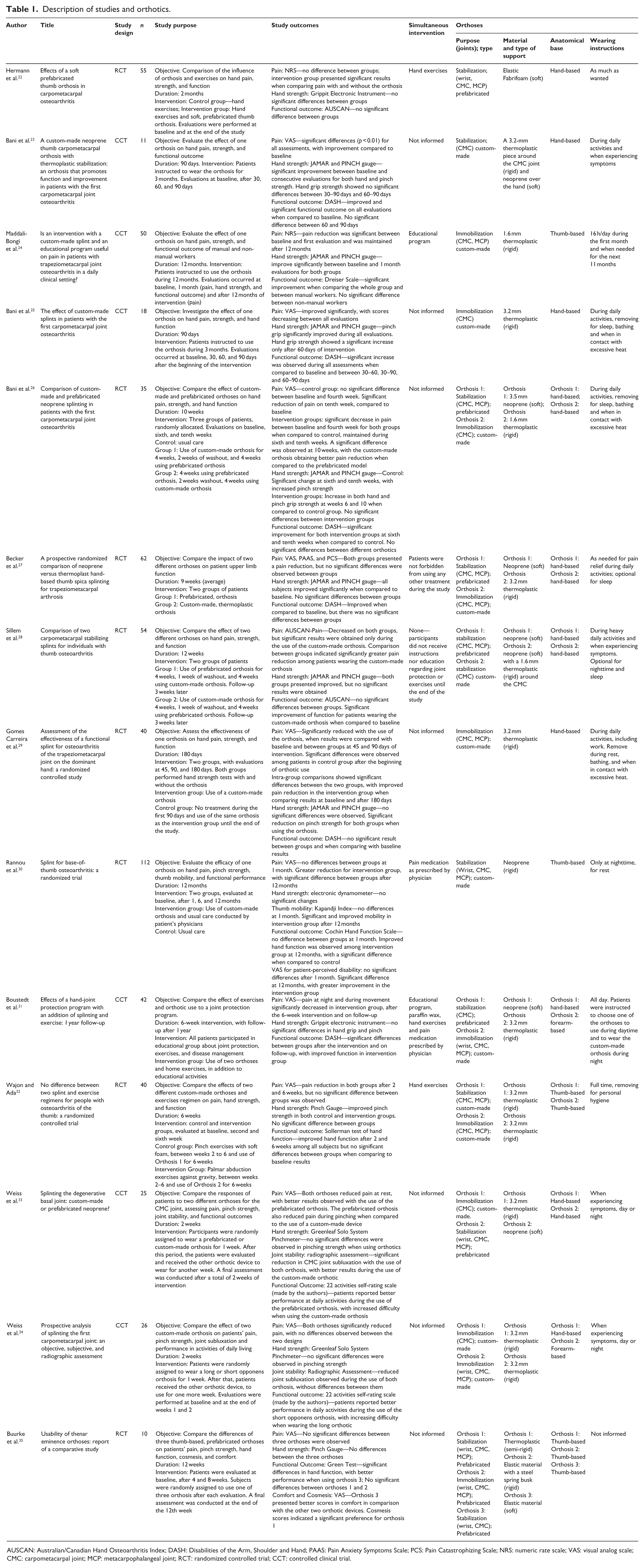
AUSCAN: Australian/Canadian Hand Osteoarthritis Index; DASH: Disabilities of the Arm, Shoulder and Hand; PAAS: Pain Anxiety Symptoms Scale; PCS: Pain Catastrophizing Scale; NRS: numeric rate scale; VAS: visual analog scale; CMC: carpometacarpal joint; MCP: metacarpophalangeal joint; RCT: randomized controlled trial; CCT: controlled clinical trial.
Based on inclusion criteria, 14 articles have been chosen for this review (Figure 1). Publications described eight randomized controlled trial (RCT)22,25,27 –31,35 and six controlled clinical trial (CCT) studies.23,24,26,32–34 Seven studies investigated only custom-made orthosis,23,24,26,29,30,32,34 with five comparing custom-made with prefabricated models,25,27,28,31,33 and two studies used exclusively off-the-shelf orthotics.22,35
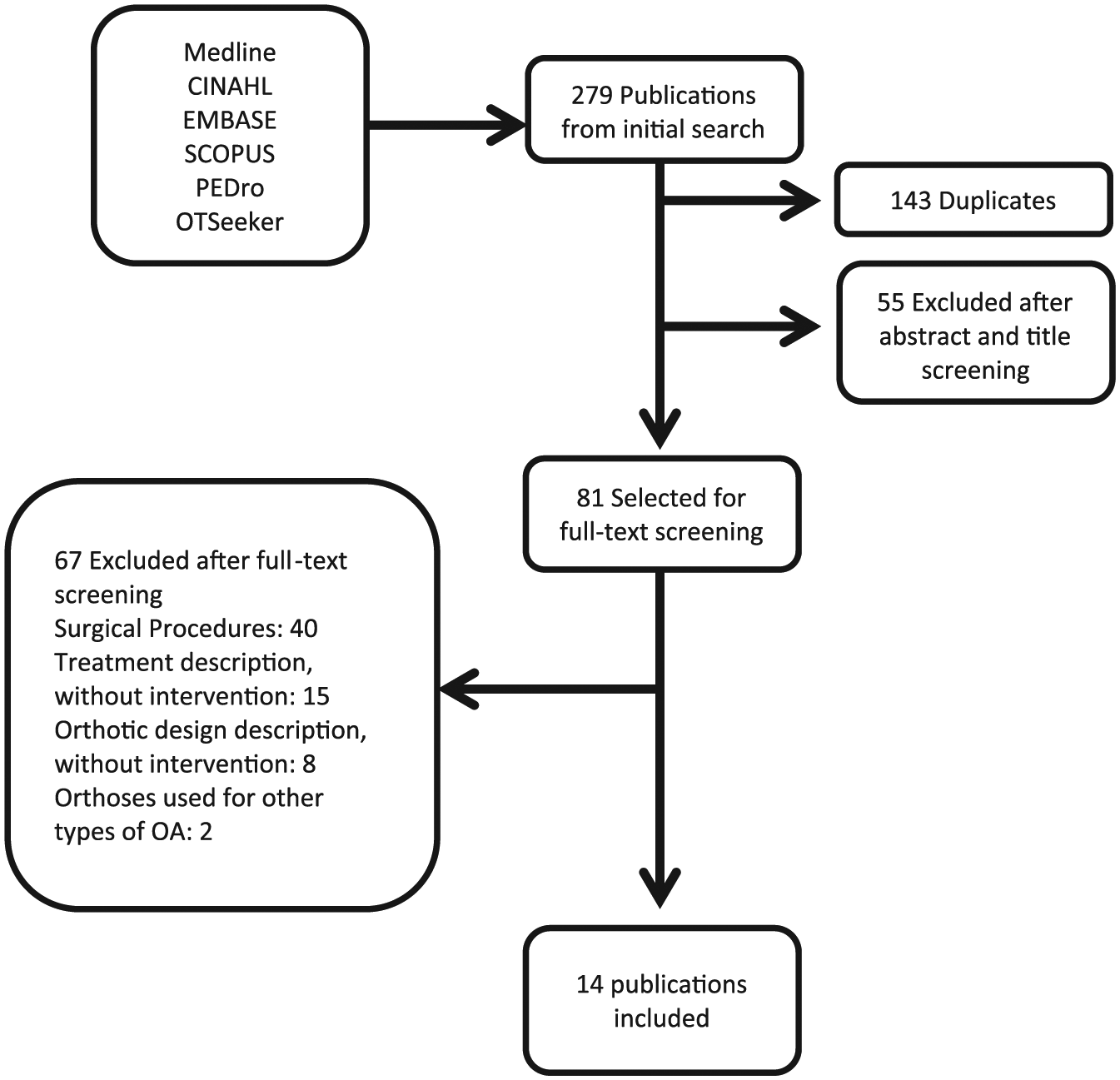
Flow diagram of study selection.
Information regarding the purpose of orthotic intervention and biomechanical rationale supporting selected models was described by five studies,24 –26,28,32 all investigating the use of hand- and thumb-based orthoses. While the main objectives of all orthotic interventions consisted in improving the CMC joint stability without hindering the movement of adjacent joints, additional rationale included positioning the thumb in a functional position for pinch,25,26 improved hand grip and pinch through a more flexible orthosis, 28 and prevention of metacarpophalangeal hyperextension to avoid CMC subluxation.24,32
Five RCTs22,25,29 –31 had control groups that used alternative treatments (joint protection techniques, exercises) or no treatment at all, while the other three RCTs27,28,35 and four CCTs24,32–34 investigated the influence of two or more different orthotic devices among independent groups. Two studies23,26 examined the impact of orthoses in the same group during different time periods.
The 14 studies included a total of 580 subjects, with a mean of 41 (standard deviation (SD): ±26.1) participants per study, ranging from 1035 to 11230 subjects. Women represented the majority of participants, with an average of 80.2% of samples composed of females. Mean age of subjects was 56.9 years. One study 33 did not report participant’s age.
To determine the eligibility of patients, 10 studies23 –26,29,30,32 –35 required radiographic evidence as inclusion criteria for CMC OA diagnosis. Symptom duration was described by 11 publications,22,25,28–35 with a mean time of 2.8 years, ranging from 0.98 25 to 15.2 years 22 of disease duration. Two studies described symptom duration using time intervals, with the majority of patients reporting clinical conditions between 6 months 33 and 1–5 years. 34
All selected studies evaluated the impact of orthoses in hand function and pain at the CMC joint. Nine studies22 –29,31 evaluated both hand grasp and pinch strength, while five publications30,32 –35 examined only pinch strength.
Adherence to orthotic use was measured by five studies23 –26,28 through patients’ report. Mean time of orthoses use ranged from 7.7 to 13 h/day. Total duration of interventions reported by selected studies ranged from 2 weeks33,34 to 12 months.24,30
Orthotic devices
Hand-based orthoses were the most common design for the majority of studies,22,23,25,26 –29,31,33,34 while long, forearm-based orthoses were described by just two publications.31,34 Four studies24,30,32,35 analyzed only thumb-based models (Figure 2).
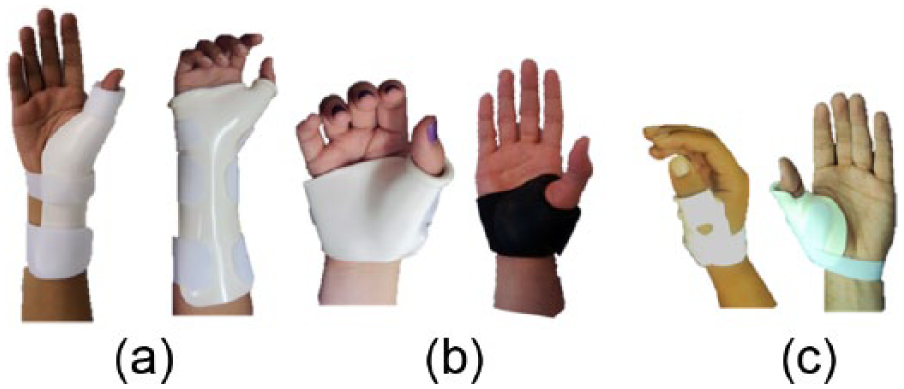
Example of orthoses described for the treatment of CMC osteoarthritis: (a) forearm-based orthoses, (b) hand-based models, and (c) thumb-based orthoses.
Selected studies included a total of 23 orthotic designs, all classified as articular according to the Splint Classification System. 20 In total, 12 orthoses aimed to stabilize the involved joints while allowing some degree of motion, and 11 designs were fabricated with rigid materials whose objective was to restrict thumb movement.
The inclusion of both the carpometacarpal and metacarpophalangeal joints was the most common strategy for orthotic intervention, with eight models described in seven studies.24,25,27 –30,32 Thermoplastics were the most often used material for orthotic fabrication, followed by neoprene and elastic fabrics. Three orthoses described23,28,35 used a hybrid approach, combining both rigid and soft materials.
Custom-made models comprised 60% of described orthoses, with nine prefabricated devices included in the selected studies.
Wearing instructions
No standard instruction regarding orthotic use was observed among the selected publications. Three studies instructed patients to wear the orthoses during daily activities,25,26,29 and in seven studies,22 –24,27,28,33,34 patients were oriented to use the orthoses whenever they experienced symptoms, as long as necessary. Only one study 24 established strict schedules for orthotic use (16 h/day for the first month).
The study conducted by Rannou et al. 30 instructed patients to use the orthosis only at nighttime, while Boustedt et al. 31 and Wajon and Ada 32 suggested a full-time orthotics regime for 6 weeks. One study 35 did not report orthotics wearing instructions.
Outcome assessment tools
Visual analog scale (VAS) was used for pain assessment in all but three studies: the numeric rate scale (NRS) was used by two studies,22,24 while one publication 28 measured pain using the Australian/Canadian Hand Osteoarthritis Index (AUSCAN). One study 27 included the Pain Anxiety Symptoms Scale (PAAS) and the Pain Catastrophizing Scale (PCS) in addition to the VAS for pain evaluation.
Hand grip and pinch strength were evaluated with the JAMAR and/or pinch gauge dynamometers in nine of the selected studies.23 –29,32,35 Two studies22,31 used the Grippit Electronic Instrument, two33,34 selected the Greenleaf Solo System Pinchmeter, and one 30 used a non-described electronic dynamometer.
Hand function and functional status were assessed mostly through standardized questionnaires. The Disabilities of the Arm, Shoulder, and Hand (DASH) was the most used evaluation to measure hand function, selected by six studies.23,25 –27,29,31 Other six functional evaluations were used (AUSCAN, Dreiser Functional Index for Hand Osteoarthritis (FIHOA), Cochin Hand Function Scale, Sollerman Test of Hand Function, and Green Hand Assessment), and two studies33,34 evaluated the impact of orthoses on activity performance through a questionnaire made by the authors.
Except for the Green Hand Assessment, all standardized questionnaires used in the studies measured function in relation to the degree of difficulty reported by patients during the performance of activities of daily living.
Impact of orthotics on pain, hand strength, and hand function
The use of orthoses significantly decreased pain at the CMC joint for patients in 12 of 14 studies reported in selected publications. Only one study 22 did not show significant differences in pain during the use of orthotics. Buurke et al. 35 did not include any data regarding a baseline evaluation, and therefore, the results of this study could not be considered for this step of the review.
Although the use of orthoses reduced hand pain, comparisons between different orthotic designs were not conclusive. Three studies25,28,33 showed improved pain reduction during the use of specific models: Sillem et al. 28 and Bani et al. 25 found better results during the use of two hand-based, custom-made designs involving only the CMC joint when compared to a prefabricated, neoprene orthosis. However, Weiss et al. 33 observed significantly less thumb pain among subjects who wore this same prefabricated orthosis when compared to a rigid thermoplastic design for CMC immobilization. Four studies27,32,34,35 did not show significant changes in pain between different orthoses.
The use of orthoses showed inconclusive results for both hand grip and pinch strength, with seven studies23 –25,27,28,32 reporting patients’ improvement and six studies22,30,31,33 –35 showing no significant difference of orthosis use on hand strength.
Gomes Carreira et al. 29 observed a decrease in hand grip and pinch strengths when patients were evaluated using the orthotic device. All seven studies that compared different orthotic designs reported no significant changes in hand and/or pinch strength when using different orthoses.
Overall analysis indicated significant improvements in hand function of patients with the use of thumb orthoses: 12 of 14 studies reported that patients presented better functional outcomes during the use of orthotic devices (Table 2).
Average function scores before and after orthotic intervention. a
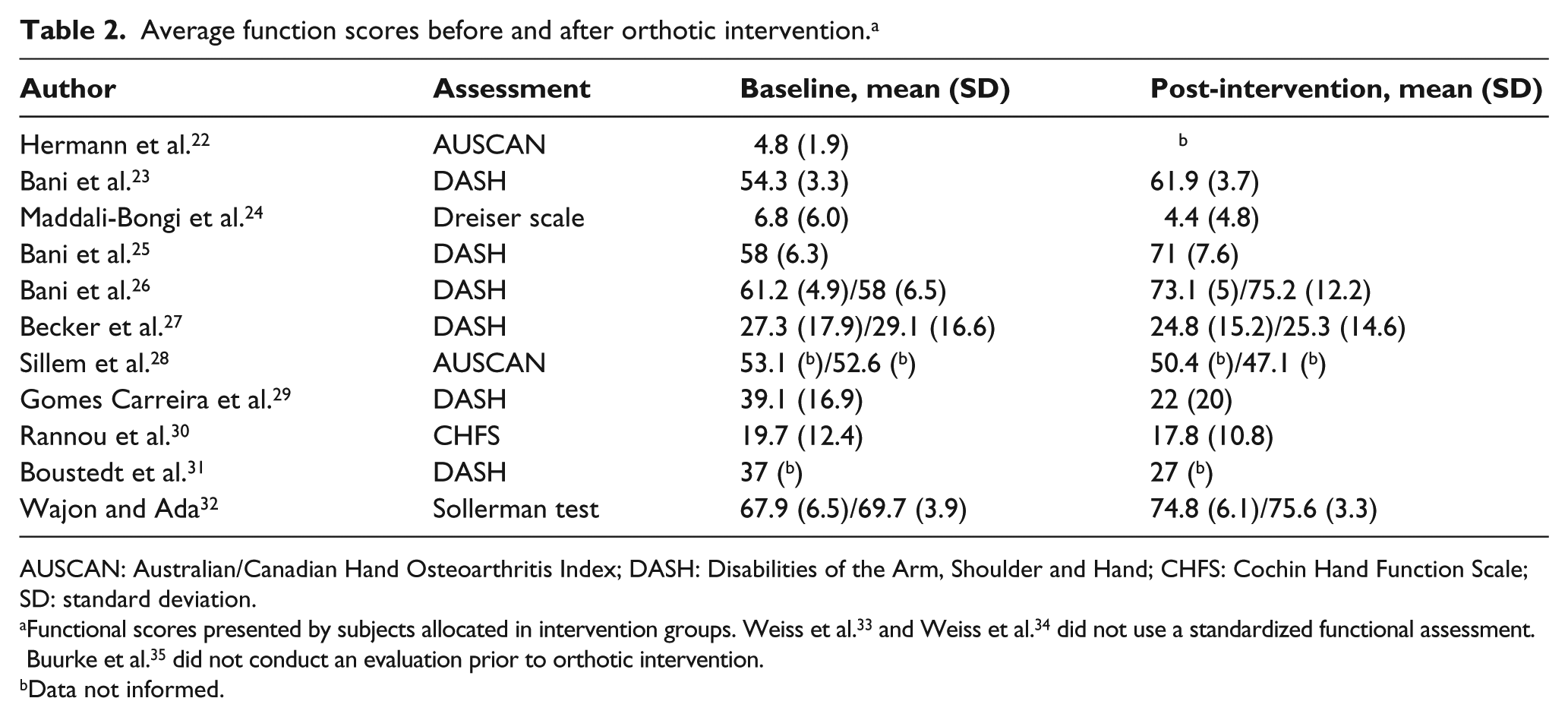
AUSCAN: Australian/Canadian Hand Osteoarthritis Index; DASH: Disabilities of the Arm, Shoulder and Hand; CHFS: Cochin Hand Function Scale; SD: standard deviation.
Functional scores presented by subjects allocated in intervention groups. Weiss et al. 33 and Weiss et al. 34 did not use a standardized functional assessment. Buurke et al. 35 did not conduct an evaluation prior to orthotic intervention.
Data not informed.
Although orthoses improved hand function when compared to situations where no orthotic device was used, only three studies observed significant differences between different orthotic designs. Weiss et al. 33 found better results among patients who wore a prefabricated, hand-based, neoprene orthosis in comparison with a custom-made, thermoplastic device. Another study from the same authors 34 compared two custom-made, thermoplastic orthoses and observed improved functional performance when subjects wore a short, hand-based orthosis in comparison to a long, forearm-based one. Buurke et al. 35 reported improved functional outcomes between patients who wore a soft, elastic, hand-based, stabilization orthosis when compared to a rigid device.
Differences in wearing instructions seemed to have not influenced the functional outcome in the selected publications. Six studies in which patients were instructed to wear the orthoses if they experienced symptoms related to the OA23,24,27,28,33,34 reported improvement in hand function and activity performance while one 22 found no significant functional change. Studies that established a full-time schedule for orthotic use also observed improvement in daily activities performance, whether the recommendations instructed use day and night31,32 or only during sleep time. 30
The five studies that measured patients’ orthotic adherence found a mean time of use of 8.8 h/day, and all these studies observed significant functional improvements among patients in short (4 weeks) 23 and long term use (after 1 year). 24 However, the impact of orthotic adherence and time of use on hand function, pain, and grip strength was not analyzed by any of the studies.
Other outcomes
Joint stability, perceived disability, thumb mobility, and orthotic cosmesis were also investigated in four studies.30,33 –35
Weiss et al.33,34 evaluated the impact of orthoses on thumb subluxation through radiographic assessment and observed improved joint positioning during the use of orthoses, with a better alignment provided by custom-made, rigid designs.
Rannou et al. 30 measured patient-perceived disability using the VAS, observing significant improvement among patients who wore orthosis for 12 months. The authors also evaluated thumb mobility through the Kapandji Index and observed significantly increased joint mobility after 1 year of orthosis use.
Buurke et al. 35 noted a significant cosmetic preference for a semi-rigid, thermoplastic, prefabricated orthoses in comparison to two other off-the-shelf orthoses.
Long-term results
Although most of the studies had a mean time of intervention below 6 months, four studies24,29 –31 reported that patients maintained outcome improvements at long-term follow-up: Boustedt et al. 31 observed pain reduction and increased hand function at 6 weeks and after 1 year of intervention, while Rannou et al. 30 found significant improvement in pain, joint mobility, and function only after 12 months of orthotic use. Two other studies24,29 observed that pain reduction was maintained within 6 months 29 and after 1 year 24 of orthosis use, but did not find improvements in other outcomes measured.
Simultaneous treatment
Seven publications included information regarding the use of other treatment modalities during the studies’ duration. Concurrent interventions during orthosis use included hand exercises,22,32 educational programs, 24 use of prescribed pain medication 30 and a combination of multiple treatments.27,31 Sillem et al. 28 did not provide patients with exercises or education programs until the final assessment, but did not inform whether patients were allowed to use other treatment during the orthotic intervention period.
Discussion
This scoping review investigated the influence of different orthoses on pain, hand strength, and functional outcomes of patients with CMC OA. Although the literature provides evidence to support the use of thumb orthoses to decrease pain and improve hand function, there is no sufficient investigation on the impact of different orthotic designs and wearing strategies on patients’ pain, hand strength, and function.
The variety of orthoses and thus the impossibility to compare studies’ results were also highlighted by previous reviews: the wide range of orthosis designs could be related to the challenge to obtain the optimal balance between joint stabilization and movement during orthotic fabrication,13,16 but might also suggest the absence of biomechanical rationale behind orthotic interventions for the thumb. In a systematic review conducted in 2011, only one of nine RTCs included a detailed description of the orthosis’ purpose. 15 Despite the increasing number of studies including this information, the majority of the publications still do not clearly state the reasoning used for orthotic fabrication and intervention.
Pain is the most important symptom for patients with hand OA, 36 significantly contributing to occupational restrictions among this population. 7 The reduction in pain obtained through orthosis use is underlined by all review studies published in the last 10 years1,3,4,11,14 –16 and by the guidelines provided by the European League Against Rheumatism (EULAR). 5 However, there are no conclusive results regarding different orthoses: meta-analyses studies3,4,15 reported that orthoses reduce pain when compared to baseline assessments, but no significant differences were observed among groups who wore two distinct orthoses.
Results observed in this scoping review also suggest a positive effect of orthoses on hand function of CMC OA patients: 12 of 14 studies observed improvements in activity performance after orthotic interventions but only three found significant differences between unique orthoses. The results are similar to the findings of previous systematic reviews3,4,15 which observed moderate evidence to support the use of orthoses to improve hand function, but were unable to determine whether or not a specific model provides better functional outcomes.
Contrasting to the positive results for pain and hand function, data regarding the influence of orthoses on hand grip and pinch were inconclusive. Although half of the selected studies observed improved hand strength after orthotic use, the other seven studies did not find significant changes, with one study reporting decreased grip and pinch strength when patients wore orthoses. 29
Despite the fact that few studies showed significant changes in different orthotic designs on patients’ functional outcomes, the literature suggests that improved performance in activities of daily living and pain reduction can be achieved through the use of short, hand-based orthoses providing adequate stabilization to the CMC without immobilizing adjacent joints.25,28 –30,34 Although not conclusive, it appears that orthoses made with more flexible materials can also facilitate their use during daily living activities, with no increase in pain.23,28,33
These results agree with a minimalistic approach advocated by some authors,13,37,38 in which the orthotic design aims to support the CMC joint, allowing complete movement of the wrist and the metacarpophalangeal joints, having a minimum influence on patients’ activities and occupations.
Implications for clinicians
There is enough evidence to support the use of orthoses during the rehabilitation of patients with CMC OA, particularly to reduce joint pain and improve hand function. Although there is no conclusive data to support the selection of a specific orthotic design, wearing instructions, and dosage, evidence suggests that the use of short, hand-based orthoses, for at least 2 weeks, improves function and reduces joint pain.
Due to the unique pattern of occupations and activities of daily living performed by patients, clinicians are encouraged to adapt the prescription of orthotic devices according to the demands and challenges presented during the performance of self-care, working, and leisure activities: A short orthosis, fabricated with rigid materials could benefit patients whose primary occupations involve the use of physical strength (i.e. crafting and manufacturing tasks), providing sufficient stabilization of the CMC joint during grasping. However, the same orthosis could compromise a fast-paced task, which does not involve the use of significant hand strength, such as typing on a computer keyboard. 24
A thorough evaluation of patients’ occupations, expectations, and aims with the treatment should complement the physical examination performed by clinicians during the selection and prescription of orthotic devices for CMC OA. The use of this approach is related to better functional outcomes and improved adherence of the patient. 39
Suggestions for future studies
Currently, no standard procedure regarding orthoses for the patient with CMC OA exists, and although the literature suggests positive effects of orthoses on pain and hand function, no conclusive results can indicate if a particular design is better than others.
Despite an increasing concern of researchers with methodological procedures in studies investigating the influence of orthoses on patients’ functional outcomes, few publications provided an adequate assessment of patients’ satisfaction, comfort, and adherence to the treatment. Besides, data regarding the rationale for the selection of a specific orthotic design, its relation with patients’ or therapeutic goals, costs, and the barriers for orthotic intervention were not described by any of the 14 studies in this scoping review.
Therefore, future studies should aim not only to provide standardized measures of the orthotic intervention outcomes but also to investigate the impact of this therapeutic procedure on the patient’s objectives, adherence, and performance through a more client-centered perspective.
Study limitations
The small number of publications included contrasts with the importance of orthotic interventions during the treatment patients with CMC OA. While the use of orthoses is one of the most common modalities in thumb OA rehabilitation, there are not sufficient investigations to provide conclusive evidence of the efficacy of specific designs.
Notwithstanding the increasing attention of researchers to the influence of socioeconomic barriers and facilitators to rehabilitation interventions, the economic evaluation and comparisons between the costs of orthotic devices could not be assessed in this review.
Although the authors tried to perform a broad literature review, only publications in English were selected for this scoping study. This decision could have excluded relevant studies published in other languages and should be addressed in future research.
Conclusion
The results of this scoping study suggest that the use of orthoses can decrease pain and improve functional performance of patients with osteoarthritis of the CMC joint, with improved functional outcomes obtained through the use of short, hand-based models, providing sufficient joint stability and reducing pain without hindering the mobility of the upper extremity. Despite an increasing number of high-quality studies, the impact of different orthoses on patients’ comfort, treatment adherence, occupations, and activity performance on both short and long terms still need support through adequate evidence.
Footnotes
Author contribution
All authors contributed equally in the preparation of this manuscript.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: Conselho Nacional de Desenvolvimento Científico e Tecnológico (10.13039/501100003593 207168/2014-8).
