Abstract
Background:
Load-bearing exercises are performed by transfemoral amputees fitted with an osseointegrated implant to facilitate bone remodelling.
Objective:
This study presents the loading compliance comparing loads prescribed and applied on the three axes of the implant during static load-bearing exercises with a specific emphasis on axial and vectorial comparisons.
Study design:
Cohort study.
Methods:
A total of 11 fully rehabilitated unilateral transfemoral amputees fitted with an osseointegrated implant performed five trials in four loading conditions using a static standing frame. The load prescribed was monitored using a vertical single-axis strain gauge connected to an electronic display. The tri-axial forces applied on the implant were measured directly with an instrumented pylon including a six-channel transducer. The analysis included ‘axial’ and ‘vectorial’ comparisons corresponding to the difference between the force applied on the long axis of the implant and the load prescribed as well as the resultant of the three components of the load applied and the load prescribed, respectively.
Results:
The results demonstrated that axial and vectorial differences were significant in all conditions (p < 0.05), except for the vectorial difference for the 40 kg condition (p = 0.182).
Conclusion:
The significant lack of axial compliance led to systematic underloading of the long axis of the implant.
Clinical relevance
This study contributes to a better understanding of the load applied on an osseointegrated implant during the static load-bearing exercises that could contribute to improve the design of apparatus to monitor loading exercises as well as clinical guidelines for the loading progression during rehabilitation.
Keywords
Background
Individuals with transfemoral amputation (TFA) fitted with conventional socket-suspended prostheses often experience socket-related discomfort leading to a significant decrease in quality of life. 1 Most of these concerns can be overcome by a two-stage surgical technique enabling bone-anchored prostheses using either screw-type implants or press-fit fixations.2–12 Clinical evidence demonstrated undoubtedly that the screw-type osseointegrated prosthesis for the rehabilitation of amputees (OPRA, Integrum AB, Sweden) implant and procedure are beneficial,13,14 with long-term implant stability 15 and acceptable rate of infections.13,16 Logically, this success should, somehow, be attributed to the OPRA rehabilitation program and more par-ticularly to the progressive mechanical loading prescribed to promote bone remodelling around the implant.17,18
Thoroughly described by Hagberg and Brånemark, 19 this rehabilitation program relies on a combination of dynamic and static load-bearing exercises (LBEs).2,3,19 The static LBEs are guided by the principle that a timely application of a suitable stress stimulates bone remodelling and gradually prepares the bone–implant unit to tolerate the mechanical loading likely to occur during activities of daily living.20–23 Studies confirmed that this stress is primarily applied on the residuum’s long axis.20,22–28 Early overloading might place the bone–implant interface at risk while underloading might slow down osseointegration and delay unrestricted use of the prosthesis.
Practically, these static LBEs involve axial weight-bearing with a short training prosthesis, which is performed at home twice a day for about 30 min. The loading starts at 20 kg and progresses gradually depending on patients’ residual skeleton’s bone quality, body weight and pain level until full and comfortable weight bearing is possible. The mechanical loading applied during static LBEs is monitored with a bathroom scale providing immediate visual feedback but only on the magnitude of the vertical component of the applied force.19,29 Consequently, this component is considered a surrogate of the actual load applied on the implant. However, the lack of control, accuracy, knowledge and recollection of the actual instantaneous forces and moments applied on the three axes of the implant could be considered as a shortcoming. Indeed, evidence of the link between positive outcomes of the procedure, more particularly the implant stability, 15 and the rehabilitation program is lacking.
Alternatively, Frossard et al. 30 have presented a proof-of-concept study establishing the benefits of a kinetic portable system relying on a commercial transducer to measure the actual load applied on the residuum. This basic work led to the recording of the tri-axial forces and moments applied on the implant for a cohort of TFAs (N = 11). In contrast with the actual way static LBEs are performed by patients during their rehabilitation program, one of the originalities of this work was to use a specifically designed loading frame. This static standing device (70 × 40 cm) had two handles to enable participants to maintain balance. The frame contained a single-axis strain gauge embedded into a plate with adjustable height. This strain gauge was connected to an electronic display indicating the force applied on the vertical axis in real time. Timely and fatigue-free testing was achieved by limiting individual recording to five repetitions in four loading conditions ranging from lowest to highest (i.e. 10 kg, 20 kg, 40 kg and a maximum load). Further study confirmed that magnitude of the loading showed a high between-participants’ variance and high reliability between the loading conditions. 31
However, additional work is needed to better understand the static LBEs, starting with the investigation of the trustworthiness of monitoring the load prescribed (LP) using only the vertical force applied on the implant. This requires looking at the loading compliance comparing LP and load applied. This study relies on the simple assumption that a small difference equating to a strong compliance could validate the monitoring of the vertical force. One of the primary aims of static LBE is to stimulate the bone–implant interface along the long axis. Consequently, a compliance analysis should include an ‘axial comparison’ corresponding to the difference between the force applied on the long axis of the fixation and LP. However, bone remodelling might also be influenced by a combination of loading on all three axes. Therefore, a compliance analysis should consider a ‘vectorial comparison’ looking at the difference between the resultant of the three components of the load applied on the fixation and LP. In this case, the overall loading is considered rather than the magnitude and direction of each component.
The purpose of this study was to present the loading compliance during experimental measurements relying on a purposely designed frame and loading program. The objectives were to characterise and report this loading compliance through axial and vectorial comparisons in four loading conditions.
Methods
Participants
A total of 11 unilateral TFAs fitted with an OPRA implant (Integrum AB) participated in this study (eight males, three females, age: 46.8 ± 10.5 years, height: 1.75 ± 0.10 m, mass without prosthesis: 81.54 ± 16.28 kg, time since implantation: 4.2 ± 2.2 years ranging from 1.2 to 7.8 years). All participants were treated, recruited and tested at the Sahlgrenska University Hospital, Gothenburg, Sweden. Patients were considered eligible if they were fitted with an OPRA implant, fully rehabilitated to accommodate timely recording and loading safety and lived close to the testing facility. 31 Human research ethical approval was received from the research institution’s human ethics committee. Written consent was obtained from all the participants.
Apparatus, recording and data reduction
Participants loaded the implant through an instrumented short pylon while standing in a loading frame featuring two handles to maintain balance (Figure 1) and steadiness during loading (Figure 2).30,32
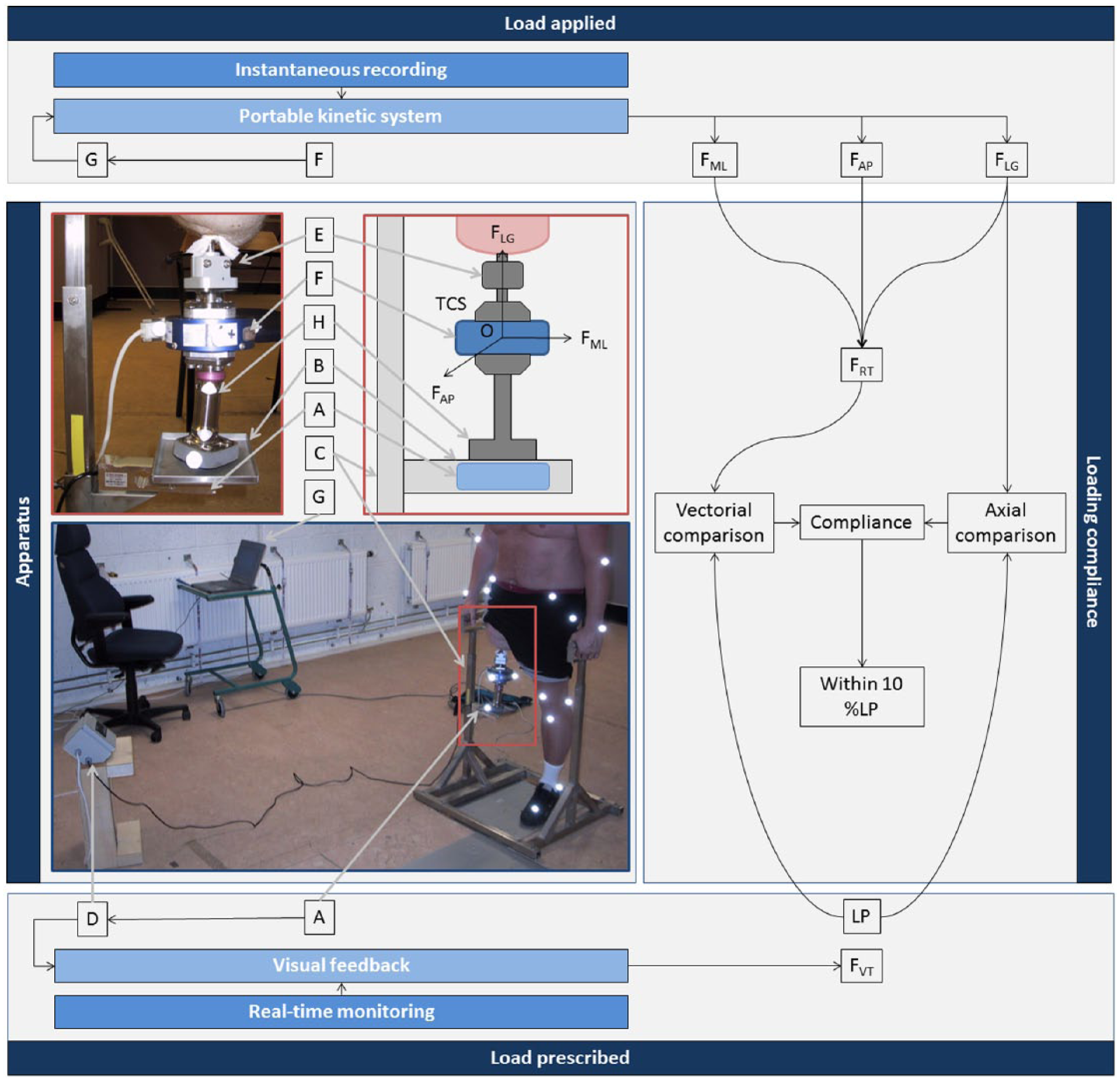
Overview of the apparatus used to provide visual feedback to monitor the load prescribed (LP). The apparatus consists of a single-axis strain gauge (A) that was embedded in the plate (B) of the support frame (C) and connected to an electronic display (D), showing the vertical force (FVT) applied on the osseointegrated implant (E). The resultant (FRT) and the components on the medio-lateral (FML), antero-posterior (FAP) and long (FLG) axes of the forces in the transducer coordinate system (TCS) are measured by a transducer (F) that was fitted between the abutment of the implant (E) and built-in the pylon (F) and connected to a laptop (G), enabling the registration of the axial and vectorial comparisons. The reflective markers were used to collect kinematic data to be presented elsewhere.
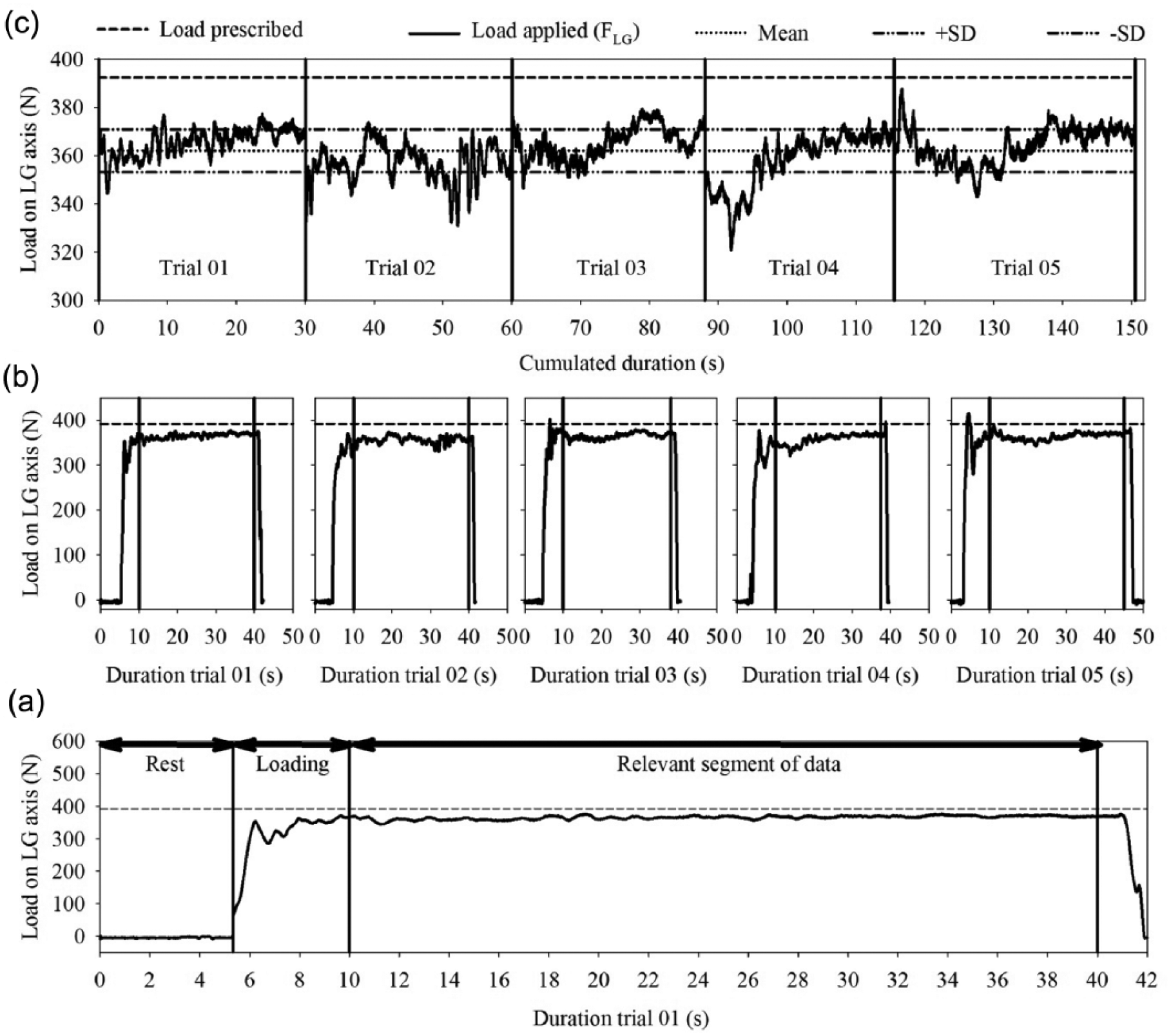
Example of data reduction for the load applied on the long axis (FLG) of the osseointegrated fixation of the participant TFA09 as recorded with portable kinetic system during an LP corresponding to a force of 400 N on the vertical axis (FVT), involving (a) an overview of selection of relevant segment of data for trial 01, (b) the selection of relevant data for all trials and (c) the collation and averaging of the load applied for all the trials.
LP corresponded to a set force to be applied on the vertical axis (FVT). The vertical component of the load applied was monitored through the single-axis strain gauge embedded into the loading frame. The vertical component of the load applied was not recorded but provided in without-real-time through a visual instantaneous feedback with an electronic display placed approximately 0.5 m off the floor and 1.5 m in front of the participants.
All other components of the load applied were measured using a portable kinetic system including a six-channel commercial transducer (model 45E15A; JR3, Inc., Woodland, CA, USA) built-in a short pylon (Figure 1).21,30,33–35 The force on the medio-lateral (FML), antero-posterior (FAP) and long (FLG) axes of the implant was measured directly by the transducer at 200 Hz with an error less than ±1 N.21,30,33–35
The recording of the load applied started when participants were in front of the frame. They were asked to apply LP as constantly as possible while monitoring the liquid crystal display (LCD). The recording ended after a steady loading occurred for approximately 30 s. Participants performed five trials in each of the four consecutive LPs: 10 kg (98.10 N), 20 kg (196.20 N), 40 kg (392.40 N) and a maximum load. Participants were instructed to rest as much as needed between trials to avoid fatigue.
The raw tri-axial forces were processed in a customised MATLAB software program (MathWorks, Inc., Natick, MA, USA).30,32 Data for four participants with left-sided amputation were translated into right-sided amputation, so that FAP, FML and FLG were consistently positive anteriorly, laterally and in compression, respectively.
Then, the longest possible period when FLG followed steadily LP was selected (Figure 2). The resultant of the force (FRT) was calculated. For both FLG and FRT, the selected segments of five consecutive trials were compiled into a large data set and averaged (Figure 2). Finally, the formulas (mean FLG − LP) and (mean FRT − LP) were used for the individual raw axial and vectorial comparisons, respectively (Figure 1). Relative axial (((mean FLG − LP)/LP)×100) and vectorial (((mean FRT − LP)/LP)×100) comparisons, corresponding to the raw axial and vectorial differences expressed in the percentage of LP (%LP), were also calculated for each participant in order to account for the magnitude of LP. The group results were represented by the median and interquartile range (IQR).
Statistical analyses
For each loading condition, Wilcoxon one-sample signed rank tests were used to investigate whether significant differences (p < 0.05) could be demonstrated between the force applied on the long axis and LP (i.e. axial comparison) and between the resultant of the force and LP (i.e. vectorial comparison).
Friedman tests were conducted to assess whether the axial and vectorial comparisons were significantly different (p < 0.05) between the four loading conditions. When appropriate, post hoc Wilcoxon paired sample tests with Bonferroni corrections were used to assess pairwise differences between the loading conditions. Statistical analyses were performed with IBM SPSS statistics v21 (IBM, Armonk, NY, USA).
Characterisation
Clinical understanding was facilitated by counting participants presenting a negative or positive difference indicating that the load applied was lesser or greater than LP, and thus that the implant was underloaded or overloaded, respectively. Furthermore, given the difficulties of applying targeted loads consistently over a given period of time, the number of participants with loading applied within 10% of LP was also counted. By definition, using a percentage allowed a wider range of load applied as LP increases. However, preliminary analyses demonstrated that the 10% threshold was the least biased towards the lighter or heavier loads prescribed for axial comparison. 30
Results
Individual and median, first and third quartiles of the magnitude of FML, FAP, FLG and FRT in each loading condition are presented in Table 1. The median LP was only calculated for the maximum condition ranging from 490.50 to 981.00 N. The median of each component and the resultant followed linearly the progression of LP. Indeed, the difference between the medians in 10 kg and maximum conditions was 101.31, −25.48, 629.02 and 585.84 N for FML, FAP, FLG and FRT, respectively.
Individual and median, first (P25) and third (P75) quartiles of the load prescribed (LP) of the magnitude of the component on the medio-lateral (FML), antero-posterior (FAP) and long (FLG) axes as well as the resultant (FRT) of the force applied on the implant in each loading condition (10 kg, 20 kg, 40 kg and a maximum load).
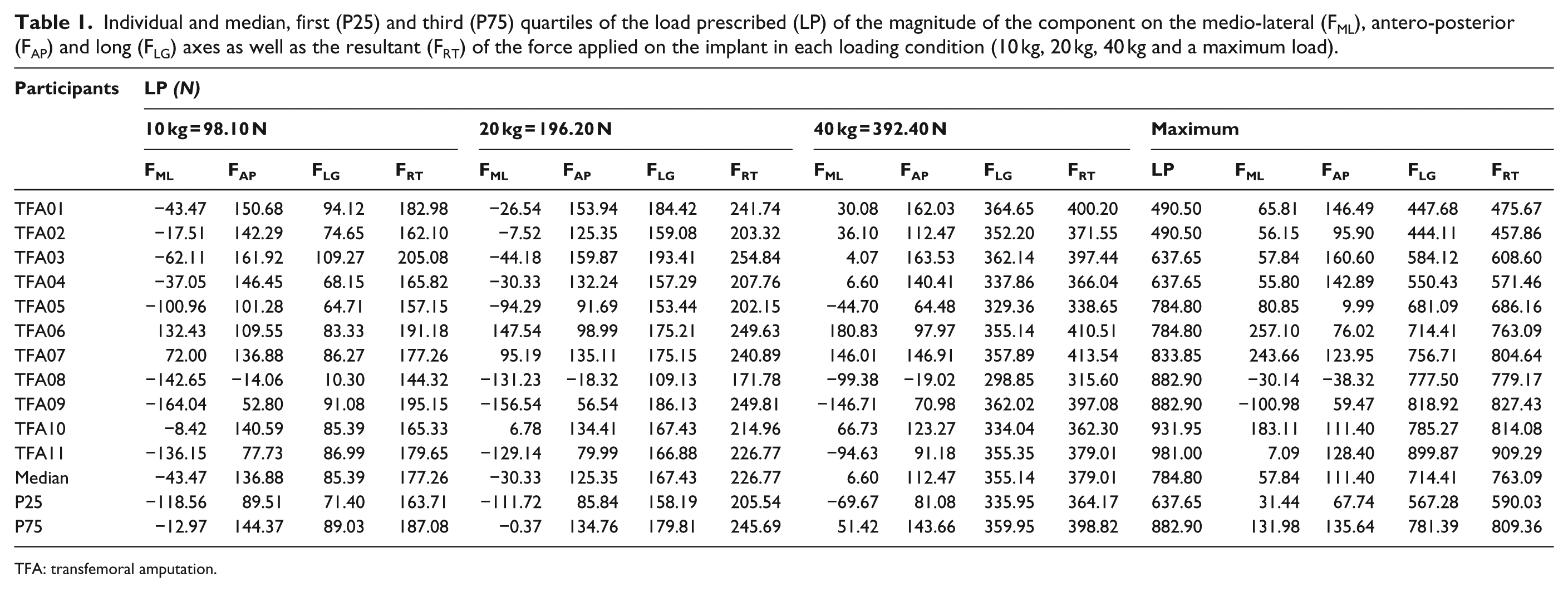
TFA: transfemoral amputation.
The median and range of raw and relative axial and vectorial differences in each condition are presented in Figure 3.
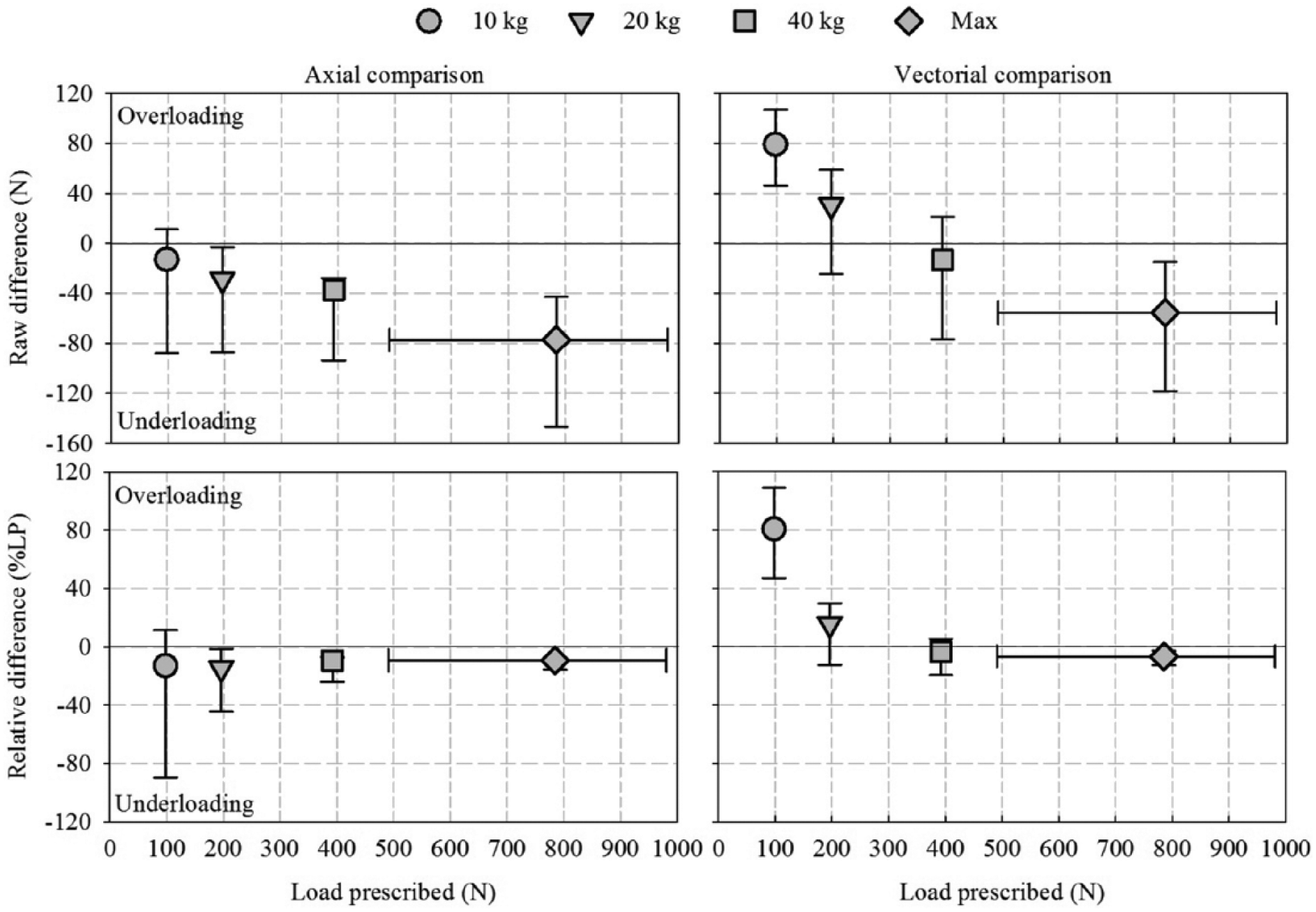
Median and range of axial and vectorial comparisons using the component on the long axis (FLG) and the resultant (FRT) of the force applied on the implant expressed in Newton and percentage of the load prescribed (%LP) in each loading conditions (10 kg, 20 kg, 40 kg and a maximum load).
Axial comparison
The median and IQR of raw axial differences were −12.71 N (17.63 N), −28.77 N (21.63 N), −37.26 N (24.00 N) and −77.14 N (36.71 N), while relative axial differences were −13 %LP (18 %LP), −15 %LP (11 %LP), −9 %LP (6 %LP) and −9 %LP (4 %LP) for the 10 kg, 20 kg, 40 kg and maximum conditions.
The results of the Wilcoxon one-sample signed rank tests demonstrated that the raw axial differences were significantly different from zero in all conditions (p < 0.05). The Friedman analyses showed significant axial differences between the four conditions for raw axial comparisons (p < 0.001) but non-significant differences for relative axial comparisons (p = 0.484). Post hoc pairwise raw axial comparison with Wilcoxon paired tests using Bonferroni corrections showed that differences between all conditions were significant (all p < 0.05).
The raw axial difference was negative for all participants in every condition, except for TFA03 while loading 10 kg (11.17 N). The load applied on the long axis was within 10% of LP for 2 (18%), 3 (27%), 6 (55%) and 7 (64%) participants in 10 kg, 20 kg, 40 kg and maximum conditions, respectively.
Vectorial comparison
The median and IQR of raw vectorial differences were 79.16 N (23.37 N), 30.57 N (40.15 N), −13.39 N (34.65 N) and −55.47 N (56.05 N), while relative vectorial differences were 81 %LP (24 %LP), 16 %LP (20 %LP), −3 %LP (9 %LP) and −7 %LP (7 %LP) for the 10 kg, 20 kg, 40 kg and maximum conditions.
The Wilcoxon one-sample signed rank tests demonstrated that raw vectorial differences were significantly different from zero in all conditions (p < 0.05), except for the 40 kg condition (p = 0.182). The Friedman tests showed significant differences in vectorial comparison between the four conditions (all p < 0.001) for both raw and relative vectorial comparisons. Post hoc pairwise Wilcoxon paired tests using Bonferroni corrections showed that raw and relative vectorial comparisons were significantly different between all conditions (all p < 0.05), except between the 40 kg and maximum condition for relative vectorial comparison (p = 0.300).
The raw vectorial differences were positive for all, 10 (91%) and 5 (45%) of the participants in 10, 20 and 40 kg conditions, respectively. The resultant of the applied load was within 10% of LP for none, 4 (36%), 9 (82%) and 7 (64%) participants in 10 kg, 20 kg, 40 kg and maximum conditions, respectively.
Discussion
Contributions
This study demonstrated a significant lack of axial compliance. The load applied on the long axis was significantly smaller than LP in every condition. This led to a systematic underloading of the implant on the long axis during the proposed experimental LBE.
Furthermore, the analysis of the raw axial comparison indicated that the difference between the load applied on the long axis of the implant and LP was the smallest for the 10 kg followed by the 20 kg, 40 kg and maximum loading conditions. Since all pairwise differences were proven to be statistically significant, these results showed that the loading frame was better indicated to monitor lighter loadings. Nonetheless, the outcome changed notably when the magnitude of LP was taken into consideration. Indeed, the relative axial comparison showed no statistically significant pairwise differences indicating that the loading frame used performed equally in all conditions.
This study also showed that the analysis of the vectorial compliance was more complex. Results indicated a clear vectorial overloading and underloading of the implant in the 10 kg and maximum conditions, respectively. However, the raw vectorial compliance was more pronounced in the 20 and 40 kg conditions. Indeed, Figure 3 indicated that the group might be the most compliant around an LP of approximately 30 kg.
The number of participants applying a load within 10% of LP tolerance increased systematically for axial but less consistently for vectorial loadings as LP increased. Interestingly, 64% of the participants were within 10% of LP for both axial and vectorial loadings in the maximum condition.
By definition, the loading compliance was influenced by the orientation of the transducer’s coordinate system in relation to the vertical axis. In other words, the participants with the least compliance could be those with the short prosthesis the least orthogonal to the loading plate. Consequently, a full understanding of the lack of compliance will require further comprehensive kinematic analyses (e.g. orientation of prosthesis). Such analysis was beyond the scope of this study. However, a preliminary study presented in abstract form describing participants’ body posture during these LBEs might provide some insights. 36 Typically, participants placed both hands on the handles at hip level and ahead of the trunk while, more importantly, their sound feet on the floor were on the side and behind the loading plate. Furthermore, participants seemed to increase the loading on the plate by shifting their body weight mainly from a medial to a lateral position. This phenomenon has been previously reported, but it has yet to be substantiated by strong evidence.19,30,36,37 Nonetheless, this possible explanation was supported by the rather stable FAP applied anteriorly with a magnitude around 102 N across all loading conditions and the progression of FML crossing from medial to lateral when LP was between 30 and 40 kg.
Finally, this study highlighted that monitoring LP through the vertical force corresponded marginally to the actual load applied on the implant during the proposed experimental LBE. Obviously, monitoring LP with a device such as a single-axis vertical strain gauge or bathroom scale is a practical, affordable, low-tech and easy-to-use method accommodating a wide range of circumstances. Unfortunately, this study confirmed that the trade-off inherent to the lack of control of the actual force applied was substantial.
Altogether, the results indicated that the specific experimental loading frame and set-up used in this study were only partially reliable to load the implant according to the proposed loading program. Nonetheless, this study could raise awareness about potential limitations of using a scale to monitor loading and, eventually, provide guidance on how to perform LBEs (e.g. control of body shift).
Limitations
The generalisability of these results is limited due to cohort sample size, lack of kinematic data, no recording of actual FVT and other dynamic data. Furthermore, there were noticeable differences between the loads assessed in this study and the ones applied during the actual rehabilitation program in terms of recording conditions, loading apparatus and loading progression. Therefore, further clinical interpretations should be considered cautiously.
Future studies
Additional clinical understanding of the loading compliance could be gained through subsequent longitudinal studies focusing on simultaneously recording of FVT and all axes of the load applied during the actual course of static and dynamic LBEs.19,36 Additional cross-sectional studies could focus on recording load applied during LBE and complementary information such as registration of pain, kinematic confounders and bone remodelling.8,9,24,27,38
Conclusion
This study was the first attempt to establish to what extent the load applied on the implant of 11 individuals with TFA was comparable to the LP during experimental LBEs aiming at promoting bone remodelling. The results confirmed the lack of axial and vectorial compliances. Consequently, monitoring the vertical force might be a surrogate partially reflective of the actual load applied, particularly on the long axis of the implant.
Nevertheless, this study contributes to a broader reflection about the fundamental objectives of static LBEs within the rehabilitation program. In particular, this study highlights the need for an adequacy between the loading constraints given to patients and the design of the apparatus used to implement these instructions. A broad consideration of multi-axial forces and moments loading would involve establishing the loading progression on each axis as well as the design of the apparatus enabling this loading. Incidentally, substantial modifications of the proposed loading frame and, more likely, the scale method must be made if mainly the long axis of the implant should be loaded. Furthermore, this work highlights the need to further explore other means to monitor the LP, such as loading pain.
In conclusion, the work presented here is a stepping stone in the development of an evidence-based LBE program relying on guidelines for tri-axial loading and a suitable loading apparatus.
Footnotes
Author contribution
All authors contributed equally in the preparation of this manuscript.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This study was partially funded by the Australian Research Council Discovery Project (DP0345667), Australian Research Council Linkage Grant (LP0455481), Queensland University of Technology Strategic Link with the Industry and Institute of Health and Biomedical Innovation Advanced Diagnosis in Medical Device Grant.
