Abstract
Objectives:
Inaccurate design, insertion or loading of mini-implant may lead to disturbed bone turnover and subsequent implant failure. This study assesses the two commonly used types of implants and their bone stress pattern and determines which type of implant may be more patient-compatible.
Method:
The samples were categorized into four groups and analyzed by scanning electron microscopy to assess the surface morphology. Stress distribution was estimated using finite element method for which three-dimensional (3D) models of the maxilla and mini-screws were prepared. The implant was then inserted 5 mm from the alveolar crest onto the buccal cortical plate of maxilla between the second premolar and first molar within the platform of Ansys Workbench software. Two loads were applied: 5 Ncm and 2 N. Evaluation of von Mises stresses in the bone was estimated.
Results:
The study concluded that tapered stainless steel screws exerted greater stress on the bone than titanium screws in both situations. As the diameter increased from 1.3 mm to 1.5 mm, the mini-screw displacement and stress were less. Under 2 N force, the stress was distributed around the head and neck of the mini-implant and the cortical bone.
Conclusion:
The assessment of von Mises stress distributed around an orthodontic mini-implant under a constant load revealed that stainless steel mini-screws generated more stress than titanium mini-screws. It was observed that the majority of the stress and strain is tolerated by the cortical bone, not the cancellous bone. The diameter of mini-screw is more significant irrespective of material composition.
Introduction
Tooth movement by orthodontic force application occurs by changes in dental and paradental tissues, namely dental pulp, periodontal ligament (PDL), alveolar bone and gingiva. These tissues, when exposed to varying degrees of magnitude, frequency and duration of mechanical force, express expansive macroscopic and microscopic changes. 1
Teeth can be moved in the desired direction only when anchorage is sufficiently strong to offset orthodontic forces. Anchorage is the resistance to undesirable tooth movement and is a pivotal component of fixed orthodontic treatment. Orthodontic mini-implants (OMI) have become increasingly popular as they provide absolute anchorage like ankylotic teeth. 2 Dental implants need osseointegration to operate, whereas mini-screws or mini-implants are self-tapping or self-drilling types do not need osseointegration and can be loaded without it. 2 Typically, orthodontic min-implants are manufactured from a titanium–aluminium–vanadium alloy or stainless steel (SS) F138 (18% Cr, 14% Ni and 2.5% Mo). 3
Excellent stability of mini-implants is necessary for a successful orthodontic treatment. To achieve this, it is essential to identify their profile, dimensions and mechanical properties. Implant design is a contributing factor for successful implantation4, 5 by directly affecting the biomechanics of peri-implant bone. Mini-screws offer mechanical retention through contact between bone and implant without damaging bone physiology. They should not be traumatic to the tissue. The shape of the screw, the length, diameter and profile of the screw threads (shape, depth and pitch) affect the primary stability of the mini-implant. 6
Hypothetically, by assessing the magnitude and distribution of stress and strain in the peri-implant bone when a load is applied, it can be assumed whether the mini-implant is safe to use. Since clinical or experimental studies on stress and strain in the bone are difficult, limited investigations have been carried out in this area. 7 The three-dimensional finite element method (3D FEM) is a non-invasive technique for the analysis of stress distribution and is unique because of its ability to model geometrically complex structures such as bone.
Even though self-drilling mini-implants are easy to insert and are compatible to the patient, they are more prone to cause micro-damage in the dense cortical bone as they necessitate the application of greater force. Inaccurate design, insertion or loading of mini-implant may lead to disturbed bone turnover and subsequent implant failure. 8 Hence, this study assesses the two commonly used types of implants and their bone stress pattern and determines which type of implants may be more patient-compatible. The present study aimed to analyze the stress distribution of two types of OMI in the maxillary bone as the dimension changes.
Method
This study was carried out in the Department of Orthodontics and Dentofacial Orthopaedics, KMCT Dental College, with technical assistance from National Institute of Technology and CADD Center. Ethical clearance was obtained from the Institutional Ethics Committee.
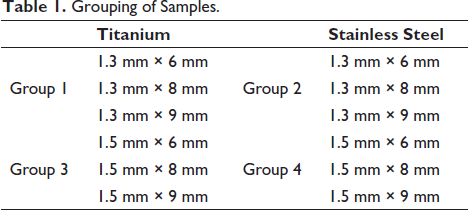
The study was conducted on 12 self-drilling mini-implants categorized into four groups. The dimensions of titanium and SS mini-implants used were: Diameter—1.3 mm and 1.5 mm; length—6 mm, 8 mm and 9 mm. The area of placement of the mini-implant was assigned as the buccal cortical plate of the maxilla between second premolar and first molar, which is the most common interradicular site in the maxilla. Implants retrieved from patients after orthodontic treatment, implants with manufacturing defects, and bone screws were excluded from the study. Mini-implants used in this study are titanium alloy (TiA) and SS implants and are grouped into four categories (Table 1).
Grouping of Samples.
The samples obtained were analyzed non-destructively by scanning electron microscopy (SEM) to assess the surface morphology. Before the microscopic analysis, each mini-implant was stored separately in plastic containers noted by length, diameter and material. Followingly, the mini-implants were mounted on aluminium sample holders with a carbon double-sided sticky tape and were marked for identification. The mini-implants were analyzed by SEM (HITACHI SU6600). Surface images were captured by a computer and evaluated. Magnification ranged from 25 to 500 kx. The variations in morphological characteristics as the dimension varies were assessed for both types of implants.
Stress distribution was estimated using the FEM. Finite element analysis is the simulation of a physical phenomenon using a numerical mathematic technique referred to as the FEM. This process is the core of mechanical engineering.
In this study, 3D models of the maxilla and tapered mini-screws were prepared and model components were integrated. The maxilla model was developed using cone beam computed tomography (CBCT) scan data (Planmeca Romexis 5.3.5.80). For this purpose, a CBCT image of the maxilla was taken at angles of 0–360°. The images were obtained in multiplanar slices (sagittal, coronal and axial) as Digital Imaging and Communications in Medicine (DICOM) file data. From these DICOM images, a 3D volume-rendered image of the maxillary bone was created in stereolithographic format (.stl) in 3D slicer v5.0.3 software. The stereolithographic image was transferred to the Autoconverter-x64 software, where it was converted to step file format. The step file format was compatible with the FEM software, Ansys 2021 R2. Further modelling of tissues was done with the SolidWorks Mimics 2012 software (Figure 1).
Mesh Model of Implant-bone Assembly and Mini-implant.

Due to the complex structure of the maxillary bone and to reduce the operation time, the bones were demarcated as cortical and cancellous bone only in the region where the mini-screws were located. In other parts, the bone was assumed to be homogeneous. 2 From the CBCT data, the cortical bone thickness was obtained as 1 mm. The cancellous bone was reconstructed below the cortical bone and thickness was obtained from scan data as 7.05 mm. For ease of procedure, the mucosa was reconstructed with a thickness of 2 mm. 2
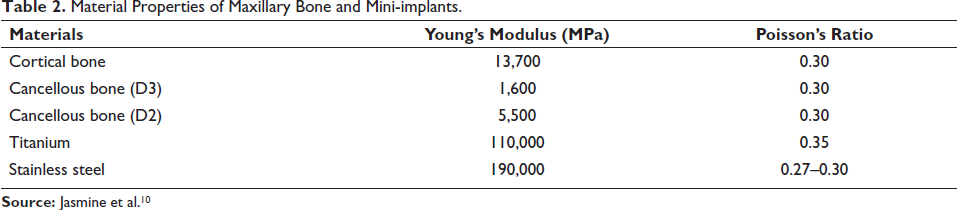
Twelve different dental implants were constructed by SolidWorks. The total length of the mini-implants ranged between 6 and 9 mm, and the diameter chosen was 1.3 and 1.5 mm. The pitch was analyzed by SEM as 784–848 µm, hence arbitrarily taken as 0.8 mm. The thread shape is viewed as a reverse buttress. The present study treats non-living structures (implants) as isotropic, so two independent material constants, Poisson’s ratio and Young’s modulus, are assigned. 9 A linear elastic behaviour was imposed to the bone. Material properties of elements are taken from Jasmine et al. 10 and are given in Table 2.
Material Properties of Maxillary Bone and Mini-implants.
The implant was then placed 5 mm from the alveolar crest onto the buccal cortical plate of the maxilla between the second premolar and first molar within the platform of Ansys Workbench software. Regarding load application, the literature showed insertion torque in the range of 5–10 Ncm. 11 In this study, a moment of 5 Ncm was directly applied to the centre of the head of the implant for each model. A second model was created onto which a vertical concentrated load of 2 N2, 8, 12 was applied to assess the stress distribution around mini-implants.
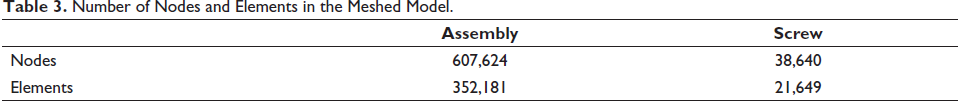
Each model consisted of nodes and elements as given in Table 3. The bottom surface of the bone was considered as fixed during the analysis.
Number of Nodes and Elements in the Meshed Model.
Evolution of von Mises stresses in the bone was estimated. Failure can be predicted by von Mises stress according to the von Mises yield criterion, which states that yielding of a material occurs when the von Mises stress exceeds the yield strength in tension.13, 14 Data thus obtained were subjected to suitable statistical analyses.
Results
A total of 12 samples were studied under two different loading conditions. The assessment was done for titanium and SS mini-implants across varying diameters.
Normality was checked using Kolmogorov–Smirnov and Shapiro–Wilk test, and the statistics show that the values are normally distributed. So unpaired Student t-test was done to compare the means across the categories.
von Mises Stress in Implants when 5 Ncm Insertion Torque is Applied
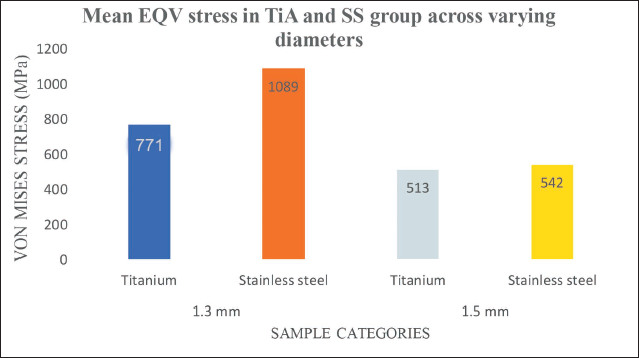
The average von Mises stress in the study among the total 12 samples was 728 MPa, with a standard deviation (SD) of 345.71, and ranges from 348 to 1,598. Unpaired Student t-test demonstrates that even though there is a higher mean stress in SS compared to titanium, the difference is not statistically significant, with a p value of .141 at degree of freedom 10 and t statistics of –0.858 (Figure 2).
von Mises Stress in Implants when 2 N Vertical Load is Applied
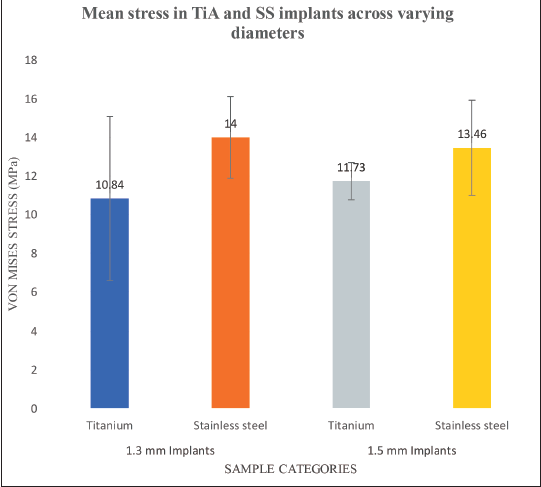
The average von Mises stress in the study among the total 12 samples was 12.50 MPa, with an SD of 2.677, and ranges from 6.43 to 16.33. The t-test statistics show a p value of .116, which is more than significant p value .05 at degree of freedom 10 and t-statistics of 1.719. Hence, it is concluded that there is no significant difference in mean between SS (mean ± SD) and titanium (mean ± SD) groups (Figure 3).
Graphical Representation of Comparison of Equivalent Stress in Titanium Alloy (TiA) and Stainless Steel (SS) Orthodontic Mini-implant (OMIs) across 1.3 and 1.5 mm Diameter Group at 2 N Load.
Discussion
In daily orthodontics, proper anchorage is a pivotal factor for a successful treatment result. Recently, mini-implants, with their absolute anchorage, have become the pathbreakers of orthodontics. The confines of mini-implants are important for primary stability and clinical success. 13 Most of the mini-implants fail due to the presence of stress-induced inflammatory mediators resulting in peri-implantitis and thereby bone loss. 15
The purpose of this study was to assess the two commonly used types of OMIs and their stress pattern in bone employing the FEM and to determine which type of mini-implant may be more patient-compatible. In the abundance of commercially available mini-implants, it is the clinician who chooses the implant that best suits his requirements. While doing this, several factors like the pitch of the implant, angle of insertion, site of implant placement, the quantity and type of bone and loading force should be looked into for the success of the implant treatment. 8
The comparison was made between TiA and SS as there were not many studies found in the literature comparing these two materials. Even though titanium mini-implants are popularly used these days, it is essential to know whether there are any significant differences between any of the properties of these two materials except the biocompatibility of titanium. The assessment was also made among 1.3 mm diameter, titanium and SS OMIs and 1.5 mm diameter, titanium and SS OMIs. The assessment was done under two different loads: 5 Ncm insertion torque and 2 N perpendicular load.
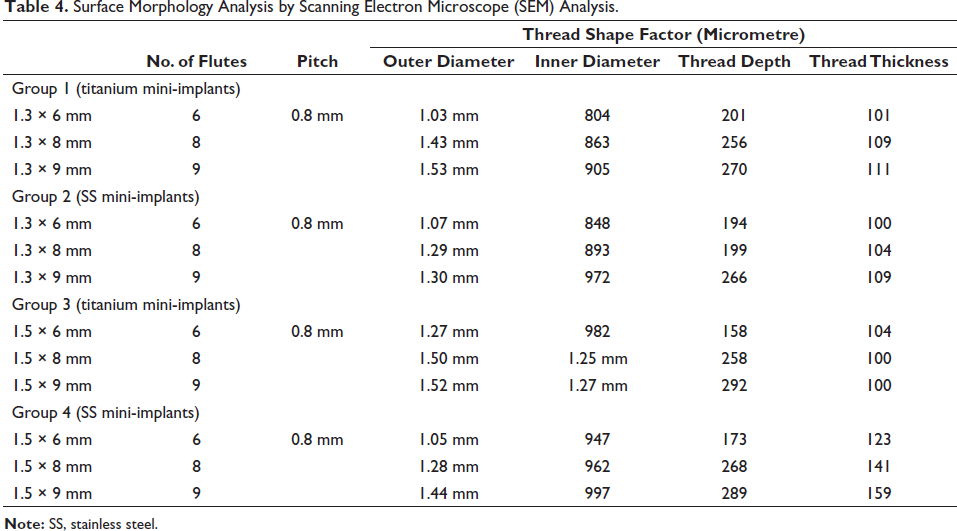
In the present study, the surface morphology varied as the diameter, length and thread shape factor varied between each mini-implant, whereas pitch of the screw, shape of thread, degree of taper and angulation were constant. The contradictory results may be due to the variations in the morphological and dimensional characteristics of thread and the shape of the mini-implant head among different commercial brands that may significantly influence the stress pattern (Figures 4–7). The morphological analysis is given in Table 4.
Scanning Electron Microscope (SEM) Images of Group 1 Titanium Mini-implant (MI). (a) 1.3 × 6 mm, (b) 1.3 × 8 mm and (c) 1.3 × 9 mm.
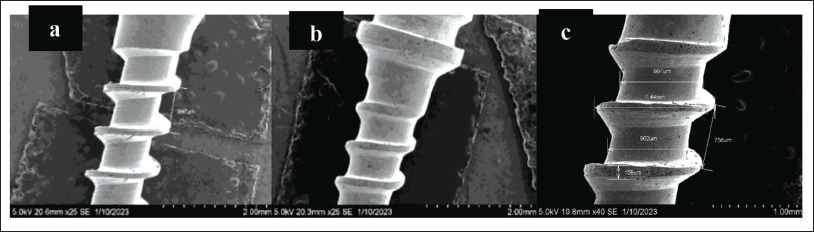
Scanning Electron Microscope (SEM) Images of Group 2 Stainless Steel Mini-implant (MI). (a) 1.3 × 6 mm, (b) 1.3 × 8 mm and (c) 1.3 × 9 mm.

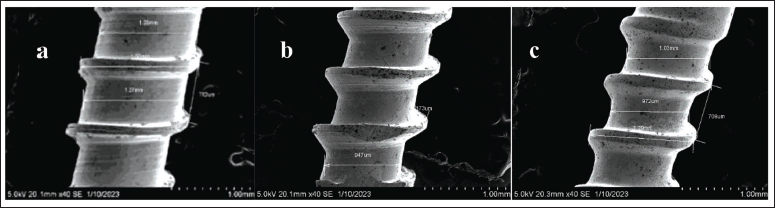
Scanning Electron Microscope (SEM) Image of Group 3 Titanium Mini-implant (MI). (a) 1.5 × 6 mm, (b) 1.5 × 8 mm and (c) 1.5 × 9 mm.

Scanning Electron Microscope (SEM) Image of Group 4 Stainless Steel Mini-implant (MI). (a) 1.5 × 6 mm, (b) 1.5 × 8 mm and (c) 1.5 × 9 mm.
Surface Morphology Analysis by Scanning Electron Microscope (SEM) Analysis.
Stress Distribution with 5 Ncm Insertion Torque
Stress generated during torsional force application was found to be more in tapered SS OMIs in the present study. It was found that even though the difference in mean stress between the titanium and SS group was not significant, SS screws exhibited more stress (Figures 8a and b). The stress was distributed along the long axis of the implant, and maximum stress was found to be at the last thread of OMI (Figure 9).
(a) Stress Distribution and Displacement in Stainless Steel (SS) Mini-implant with 5 Ncm Torque. (b) Stress Distribution and Displacement in Titanium Alloy (TiA) Mini-implant with 5 Ncm Torque.
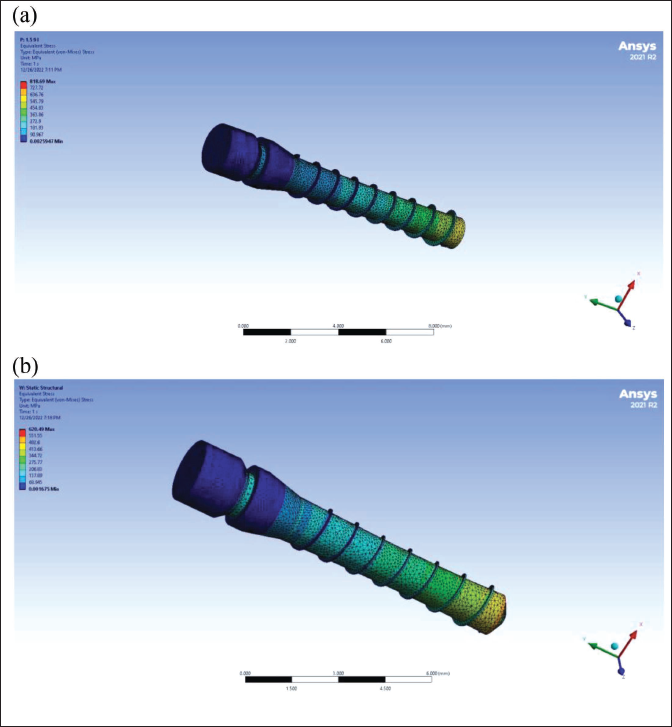
Stress and Deformation in Mini-implant Distributed along the Long Axis of the Implant Body when 5 Ncm Insertion Torque was Applied.
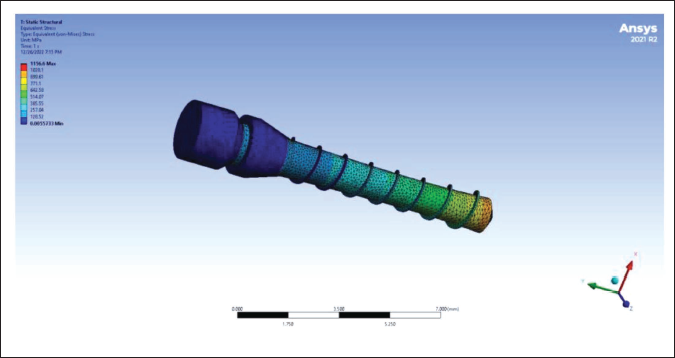
This finding is in correlation with an experimental study conducted by Barroz et al., 16 where they concluded that SS-mini-implants had higher mechanical strength and obtained a higher fracture torque than TiA-mini-implants. According to them, SS-mini-implants had 13.2% more torsional resistance than TiA-mini-implants. The higher von Mises stress value in SS implants in this study can be correlated with the above findings. Since these implants have higher mechanical strength and torsional resistance, it is obvious that the stress generated will be more when compared to TiA implants. Contrary to this study, Sabley et al., 17 from their comparative study, found that SS implants generated less stress during linear and torsional force application than the titanium implant.
Although stress values were found to be high in SS group, the mini-screw displacement was less compared to TiA group. While self-drilling the mini-implant, it was noticed that the displacement and deformation were more at the tip of the implant. It was also found that as the diameter increased from 1.3 mm to 1.5 mm, the mini-screw displacement was less. The study conducted by Al-Tayar et al. 18 and Duabais et al. 19 also concluded the same. According to them, the mini-screw diameter can be regarded as a determinant variable since the displacement is minimized as mini-screw diameter increases (Figures 10a and b). Mini-implants are available in a wide range of dimensions, but the effect of differing lengths and diameters of mini-implants on the stress pattern of bone and implant are inadequately understood, and limited studies have been published concerning this content. 13
(a) Stress Distribution and Displacement in 1.3 Diameter Mini-implant with 5 Ncm Torque. (b) Stress Distribution and Displacement in 1.5 Diameter Mini-implant with 5 Ncm Torque.
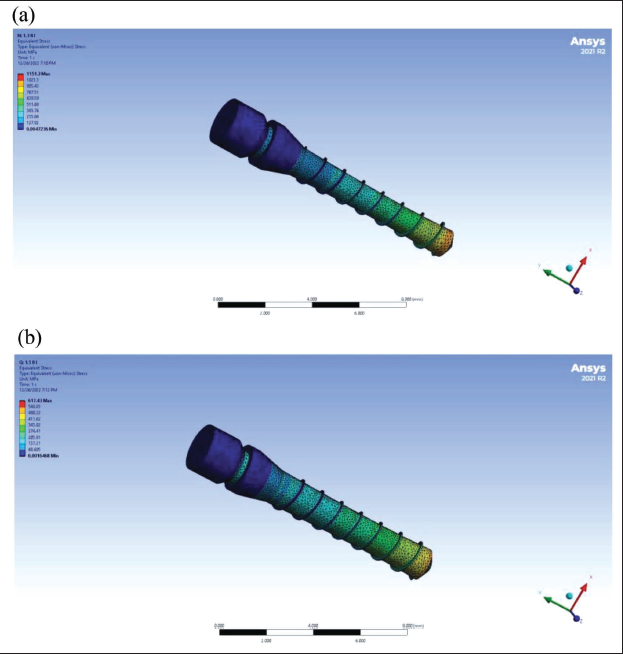
Literature reviews suggest the angle of placement for mini-implants to be 30–90° depending on the site of insertion. In this study, the angulation was considered to be 90°. In a study conducted by Ramesh et al., 13 the replicated mini-implants were inserted at a 90° angulation to the bone surface, and minimum stress was noticed, thus indicating that mini-implants should be placed as perpendicular to the bone as possible for better stability. Similarly, Marimuthu et al. 20 concluded that maximum von Mises stress in the cortical bone and OMI decreased as the insertion angle increased from 30° to 90°. Other works by Lee et al., 21 Woodall et al., 22 and Jasmine et al. 10 have recommended placing the mini-implant at 90° to the bone surface as it aids in the biomechanical stability of the mini-implant. An angle <90° creates longer lever arms, causing increased stress and displacement around the mini-implant. Studies by Deguchi et al. 23 and Miyawaki et al. 24 countered this by suggesting an angle of 30° as an essential criterion for the stability of the implant due to increased cortical bone engagement with the mini-implant.
The majority of the stresses were concentrated in the cortical bone, while stress value decreased considerably in cancellous bone. These data have been confirmed in literature (Arantes et al., 12 Ramesh et al., 13 Choi et al., 25 and Sabri et al. 26 ) in which the quality of cortical bone has been shown to influence the primary stability of the mini-implant.
Stress Distribution with 2N Vertical Load
The second scenario in this study is done by applying a 2 N perpendicular force onto the head of the mini-implant. Lin et al. 27 conducted a study and reported that the stress values in cortical bone are rarely affected by the direction of the orthodontic force application. Hence, different directions of loading force were not taken into consideration in this study.
The patterns of stress distribution of the mini-implant under loading of 200 g (2 N) of force were found to be around the head and neck of the mini-implant and in the cortical bone. The maximum stress concentration was noticed around the point of force application, that is, the head and neck region of the mini-implant (Figure 11). This stress concentration gradationally dropped from the neck towards the apex region of the mini-implant. This was presumably because the greatest resistance is exerted at the mini-implant entry point into the cortical and cancellous bones. These findings correlated well with other similar studies by Jasmine et al., 10 Holm et al., 28 van Staden et al., 29 and Sarmah et al. 30
Maximum Stress Distribution at the Head and Neck Region when 2 N Load is Applied.

From this study, it can be concluded that, as the diameter of the OMI increased, the stress reduced (Figures 12a and b). Hence, a larger diameter of the mini-implant should be used wherever possible within the anatomical confines of the situation. Among 1.3 mm and 1.5 mm diameter TiA mini-screws, the stress on OMI was found to be more in the 1.3 mm diameter group. The same pattern was observed in the SS group also. This finding is per the study conducted by Reddy et al., 31 who concluded that increasing the diameter of a micro-implant reduces the stress concentration in bone, thereby increasing the likelihood of implant stability.
(a) Stress Distribution in 1.3 Diameter Mini-implant (MI) when 2 N Load is Applied. (b) Stress Distribution in 1.5 Diameter MI when 2 N Load is Applied.
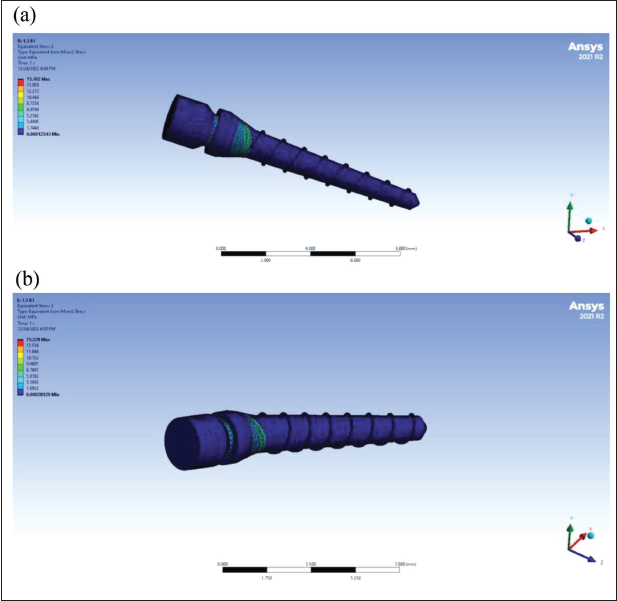
But when stress distribution in TiA and SS mini-screws were assessed, it was found that even though there were no significant differences, SS mini-implants exhibited more stress with a mean value of 13.73 ± SD. In titanium OMIs, the mean von Mises stress was found to be 11.28 ± SD. The mean von Mises value of OMIs of this study was very close to Jasmine et al.’s 10 findings (12.5 MPa) and disagreed with Stahl et al.’s 32 results (26 MPa) and Zhang et al.’s 33 results (0.56 MPa). It was proved from the experimental study conducted by Barros et al. 16 that SS-mini-implants had higher flexural strength than TiA-mini-implants. In contrast, as per Yépez et al., 34 the TiA MSs showed higher stress and deflection than the SS at the same cortical bone thickness and with the same transmucosal profile.
The transmucosal profile maintains the health of surrounding tissues, especially in areas with thin attached gingiva, because inflammation is a contributing factor to MS failure. 10 From the SEM analysis, the transmucosal length was found to be within 2 mm. According to Yépez et al., an MS with a 2 mm transmucosal profile has a longer lever arm, and application of the load generated a greater moment and, consequently, higher bending stress. According to this study, the largest deformation was observed in the MS head, and it decreased as length and diameter increased.
Limitations of the Study
Although the factors estimated in this FEM analysis are based on clinical conditions, it is irrefutable that the biological tissues are unlike the finite element model. The human tissue may vary from patient to patient and between males and females. It is impractical to measure stresses around the mini-implant in vivo. 27 Hence, this study incorporated certain factors, which might not be ideal to the real situation.
Like any other simulated model of a biological system, FEA includes some basic assumptions such as material properties of the structures. For simplicity and due to inadequate scientific quantitative data on bone behaviour material properties, the present study assumed that all materials are linear, homogenous and isotropic.
Precise results of the finite element analysis depend mainly on the accuracy of the models developed, so they must be constructed as close to the real object as possible. Accurate modelling will make the process lengthy and more complex and cumbersome.
Recommendations
In the present study, both SS and TiA OMIs were of the same manufacturer. Therefore, the surface morphology was found to be almost similar. Hence, further experimental studies on this subject should be undertaken by varying parameters as it would clear the ambiguity on mini-implants and answer many unsolved puzzles in this expanding field.
Conclusion
Despite the limitations, the findings of this study can be concluded as:
The assessment of von Mises stress distributed around an OMI under a constant load revealed that SS mini-screws generate more stress than titanium mini-screws. The difference in stress generated in SS implants and titanium implants for both forces was not significant. Under this condition, the two types of MSs are suitable for orthodontic applications. Most of the stress and strain are tolerated by the cortical bone and not the cancellous one. The greatest stresses to the screw were concentrated around either the neck or the tip of the screw when a loading force is applied, whereas during insertion more stress is distributed around the tip of the mini-implant. The diameter of OMI is more significant irrespective of the material composition of the OMI. As the diameter increases, stress decreases. The surface morphological variations are not significant since the OMIs used in the current study are from the same manufacturer. Still, it is obvious that as the morphological parameters vary, the stress pattern also varies. Hence, the null hypothesis of the study can be rejected.
Footnotes
Abbreviations
PDL, Periodontal ligament; FEM/FEA, Finite element method/finite element analysis; SEM, Scanning electron microscope; MSI, Mini-screw implant; OMI/MI, Orthodontic mini-implant/mini-implant; TAD, Temporary anchorage device; CT/CBCT, Computed tomography/cone beam computed tomography; DICOM, Digital Imaging and Communications in Medicine; ANSYS, Analysis System; EQV, Equivalent; TiA, Titanium alloy; SS, Stainless steel.
Acknowledgements
The authors express their sincere gratitude to Dr Naseem Keeranthodika, Professor, Department of Orthodontics and Dentofacial Orthopaedics for his support and guidance throughout the study. The authors extend their sincere thanks to Dr Binu Purushothaman Panar Kandy, Professor and Head of the Department. The authors also thank all the professors, teaching and non-teaching staff and my colleagues for making this study a reality. The authors would also like to express their gratitude towards NIT, Calicut and CADD Center, Calicut for providing technical assistance in completing this study.
Authors’ Contributions
Naseem Keeranthodika conceived the study and participated in its design and coordination, critically revised the manuscript. Indu Nambiar participated in the design of the study, performed the SEM analysis, model creation and FEM analysis, prepared the figures and tables and critically revised the manuscript. Binu Purushothaman Panar Kandy performed the related discussion and critically revised the manuscript. Amrita Ashok performed the related discussion and critically revised the manuscript. Muhammed Fairooz Palakkott Parambil contributed to data analysis and critically revised the manuscript. Aswathi Kandoth contributed to data analysis and critically revised the manuscript. All authors gave final approval and agreed to be accountable for all aspects of the work.
Availability of Data and Materials
The data underlying this article are available in the article and its online material.
Declaration of Competing Interests
The authors declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Ethical Approval
Ethical clearance was obtained from Institutional Ethics Committee (Ethical Committee review no: KMCTDC/IEC/2020/11).
Funding
The authors received no financial support for the research, authorship and/or publication of this article.
Informed Consent
Not applicable.
