Abstract
Objective:
The purpose of this study was to develop a new method to change a bracket position without debonding the metal bracket that was bonded with a polymethyl methacrylate (PMMA) orthodontic adhesive resin by using an ultrasonic device.
Materials and Methods:
An originally designed scaler tip was developed for a piezoelectric ultrasonic scaler. The adhesive turned to melting state by thermal heat that was generated by ultrasonic frictional heat. When the adhesive was in melting state, the bracket was rotated approximately 20° and held in this position until the adhesive hardened again by air cooling. Shear bond strengths were measured on each sample in the control and the repositioning groups. To evaluate the thermal effects of the increased temperature on the enamel surface and pulpal cavity, extracted human lower premolars were monitored during the repositioning time.
Results:
The time required for the repositioning procedures was approximately 7 s. The temperature of the enamel surface increased by 53°C and the pulpal wall increased by 0.5°C during the repositioning procedures. The bonding strength showed no significant difference between the control and repositioning groups.
Conclusion:
This method for bracket repositioning without debonding using an ultrasonic device proved to be a new method for bracket repositioning.
Introduction
Bonding brackets at the best position on the malaligned teeth is usually a challenging process for orthodontists in clinical practice.1, 2 Thus, a few brackets might appear to be malpositioned and may require repositioning to reach the ideal positions during treatment, although the others have already been aligned well. In this situation, a lot of chair time is needed to debracket and rebond the bracket, and also the patient may feel discomfort such as toothache or may fear enamel fracture due to the debonding process.3-6 If the adhesive could be softened and the bracket repositioned to an optimal position without debonding, it would be useful for both patients and orthodontists. Significant decreases of bond strengths have been previously observed in rebonded brackets.7 Therefore, this study aimed to develop a new method for repositioning brackets without the debonding process, using the specific characteristics of the polymethyl methacrylate (PMMA) (4-methacryloxyethyl trimellitate anhydride in methyl methacrylate tri-n-butyl borane [4-META/MMA-TBB]), which is an orthodontic resin. This adhesive is thought to be slightly softened by heat at the glass transition temperature (Tg).8, 9 In this study, utilizing these characteristics, metal brackets bonded to extracted bovine anterior teeth by this orthodontic adhesive were assessed to determine the repositioning time and shear bond strengths before and after the procedure. Furthermore, the thermal effects of the repositioning procedure at the enamel surface and the pulpal cavity of extracted human lower premolars were analyzed to determine the safety of this procedure in vitro study.
Materials and Methods
Materials
This study was exempted from ethical approval as it is in vitro study. The Helsinki Declaration was followed during the performance of this study. Extracted intact bovine mandibular incisors were used, and the roots were cut off before soft tissues and coronal pulps were removed. Popular types of stainless steel brackets for maxillary lateral incisors (0.022-inch slot, Mini Uni-Twin, 3MUnitek, CA, USA) were bonded with 4-META/MMA-TBB resin adhesive (Super-Bond, Sun-Medical, Moriyama, Japan), which consisted of polymer and monomer components. The ultrasonic device was a piezoelectric ultrasonic scaler (Varios 970, 28–32 kHz, NSK-Nakanishi, Kanuma, Japan) with the maximum output of 11 W. The tip that was originally made for this experiment was carved to a height of 2.0 mm, width of 0.4 mm, and length of 4.0 mm from a regular scaler tip by using a carborundum point (Figure 1) and the surface was polished smoothly by a silicone point. This custom-made tip was designed to suit well for the repositioning procedure and oscillate smoothly within the bracket slots.
Custom-made Oscillating Tip Made from a Regular Scaler Tip

Preparation
Each bovine crown was embedded in a 1-inch diameter cylinder with an auto polymerizing epoxy resin in preparation for the shear tests and bracket repositioning. The labial surface of the enamel was positioned as parallel as possible to the basal area of the cylinder. After curing the embedded resin, the teeth were ground and smoothed under running water to expose the crown enamel and standardize the enamel surfaces. The teeth were ground and polished with a polishing machine (Refine-polisher; Refine Tec, Kanagawa, Japan) by using #180-, #320-, #600-, and #1200-grit silicon-carbon papers in succession. Before the bonding procedure, the bonding surfaces of all specimens were polished with dental paste (Adonest Coarse, Neo, Tokyo, Japan) for 15 s, rinsed, and dried with oil-free compressed air. The acid etching and bonding processes were performed according to the manufacturers’ recommendations. For bonding, the bracket was positioned at the center of the labial surface. Excess resin was carefully removed from the edges of the bracket bases.
Specimens were divided into two groups: control brackets (n = 10) tested without repositioning and brackets tested after repositioning (n = 20). The resin adhesive was cured thoroughly and the entire assembly was then stored at 100% humidity and 37°C temperature for 24 h.
Repositioning Procedure
For the repositioning procedure, the scaler tip must be placed in such a position that the ultrasonic oscillation could generate frictional heat effectively on the basal side of the square-shaped bracket slots (Figure 2). A few seconds after beginning the oscillation, the adhesive turned to melting state and the bracket now could be rotated with light force and slow movement. Then, the bracket was rotated by 20° as per the guideline marked on the epoxy resin (Figure 3). After rotating the bracket, the oscillation was stopped and the bracket was pressed against the tooth surface to secure a thin layer of adhesive during the melting state. The bracket was then held in that place for several seconds until the adhesive hardened again with air cooling using a three-way syringe. Finally, the ultrasonic tip was carefully released from the bracket slot, thus completing the repositioning procedure. To ensure proper repositioning, a pair of tweezers was used to hold the bracket during the procedure.
Repositioning Procedure for a Metal Bracket on Extracted Bovine Tooth Before Softening
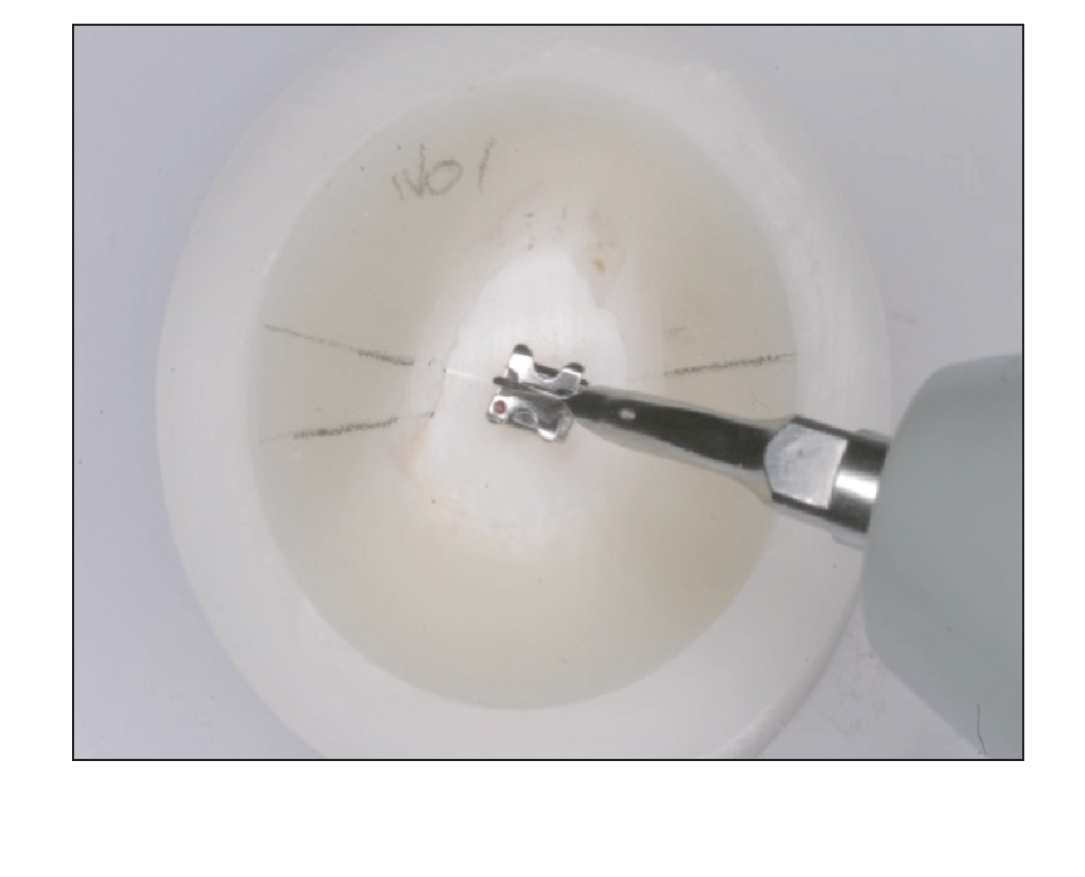
Metal Bracket After 20° Rotation With Heat by Ultrasonic Scaler

Evaluation of Bond Strength
The shear bond strength was measured with a universal testing machine (AG–10kNIS, Shimadzu, Kyoto, Japan) for both groups. The crosshead speed was 1 mm/min.
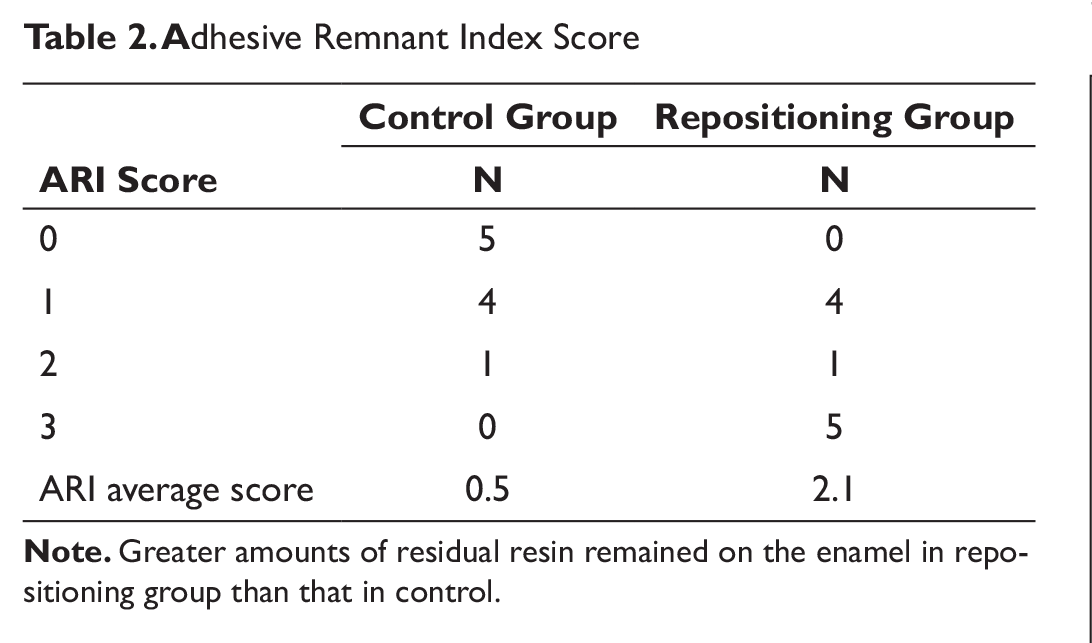
After the shear tests, the bracket bases and tooth surfaces were observed with a stereoscopic microscope. An adhesive remnant index system was used to evaluate the amount of adhesive left on the enamel surface after the shear tests. 10 The adhesive remnant index was assessed by a distinct impression of the bracket mesh, and the criteria were as follows: 0 = no adhesive left on the tooth, 1 = less than half of the adhesive left on the tooth, 2 = more than half of the adhesive left on the tooth, and 3 = all adhesive left on the tooth.
Thermal Effects
The thermal effects of the repositioning procedure on the enamel surface and pulpal wall were measured directly. For this purpose, extracted human lower premolars (n = 20) were used. These teeth were divided into 2 groups. Each specimen was drilled with a high-speed dental bur from the lingual surface to the enamel surfaces in one group and to the pulp chamber in the other group. To remove the pulp chamber contents, the specimens were washed and dried. In one group, the temperature of the enamel surface area was monitored, and in the other, the pulpal wall temperature was monitored during the repositioning procedure. Each group was further divided into two groups, namely, “with air cooling” and “without air cooling” groups. The same metal brackets were bonded on premolars by using the same procedure and the same adhesive. After the adhesives were thoroughly cured, each tooth was stored at 100% humidity and 37°C for 24 h. Finally, 0.2-mm diameter K-type thermocouple sensors (Ishifuku Metal Industry, Tokyo, Japan) were positioned at the border between the enamel surface and adhesive, which was directly under the bracket (Figure 4) and at the pulpal dentin wall (Figure 5). Temperature changes were digitally monitored using a four-channel data-logger recorder (TM–947SDJ, Sato Syoji, Kawasaki, Japan). The room temperature was 23 ± 1°C.
K-type Thermocouple Sensor Positioned on the Enamel Surface of Extracted Human Lower Tooth for Monitoring the Temperature of the Adhesive
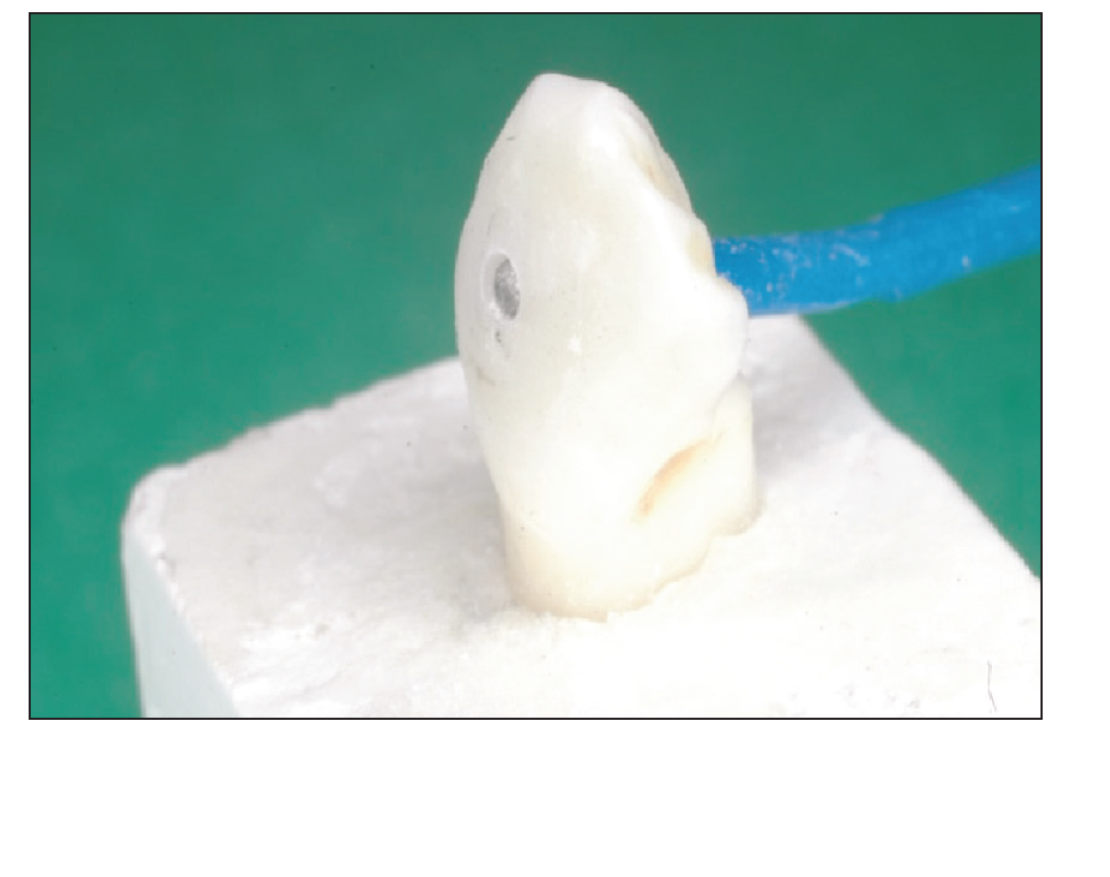
Repositioning Procedure on the Extracted Human Tooth
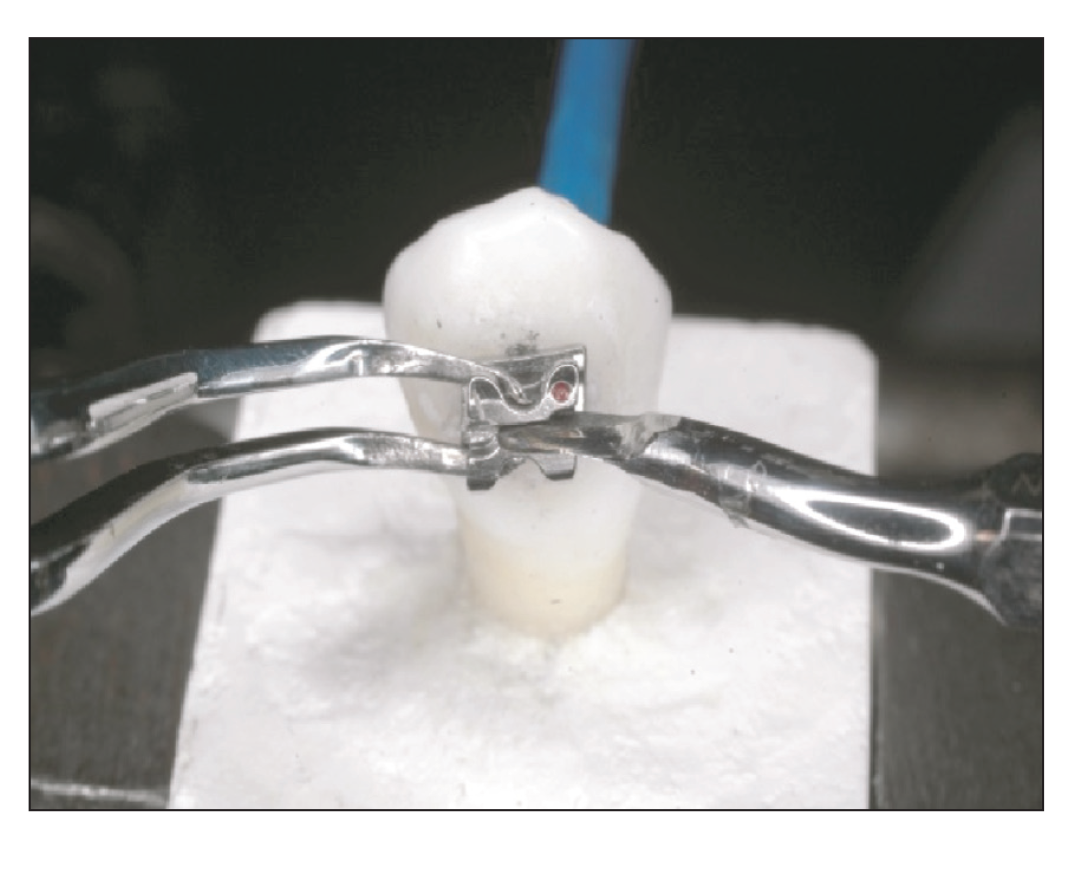
Statistical Analysis
The means and standard deviations were calculated, and Student’s t-test (Microsoft Excel 2013, P < .05 was considered significant) was conducted to determine the shear bond strengths for each group. Mean ± standard deviation is used for the numbers.
Results
Shear Bond Strengths
Shear Bond Strengths (MPa)

Adhesive Remnant Index Score
Time Required for the Bracket Repositioning Procedure
The Time for the Procedures (s)

Thermal Effects
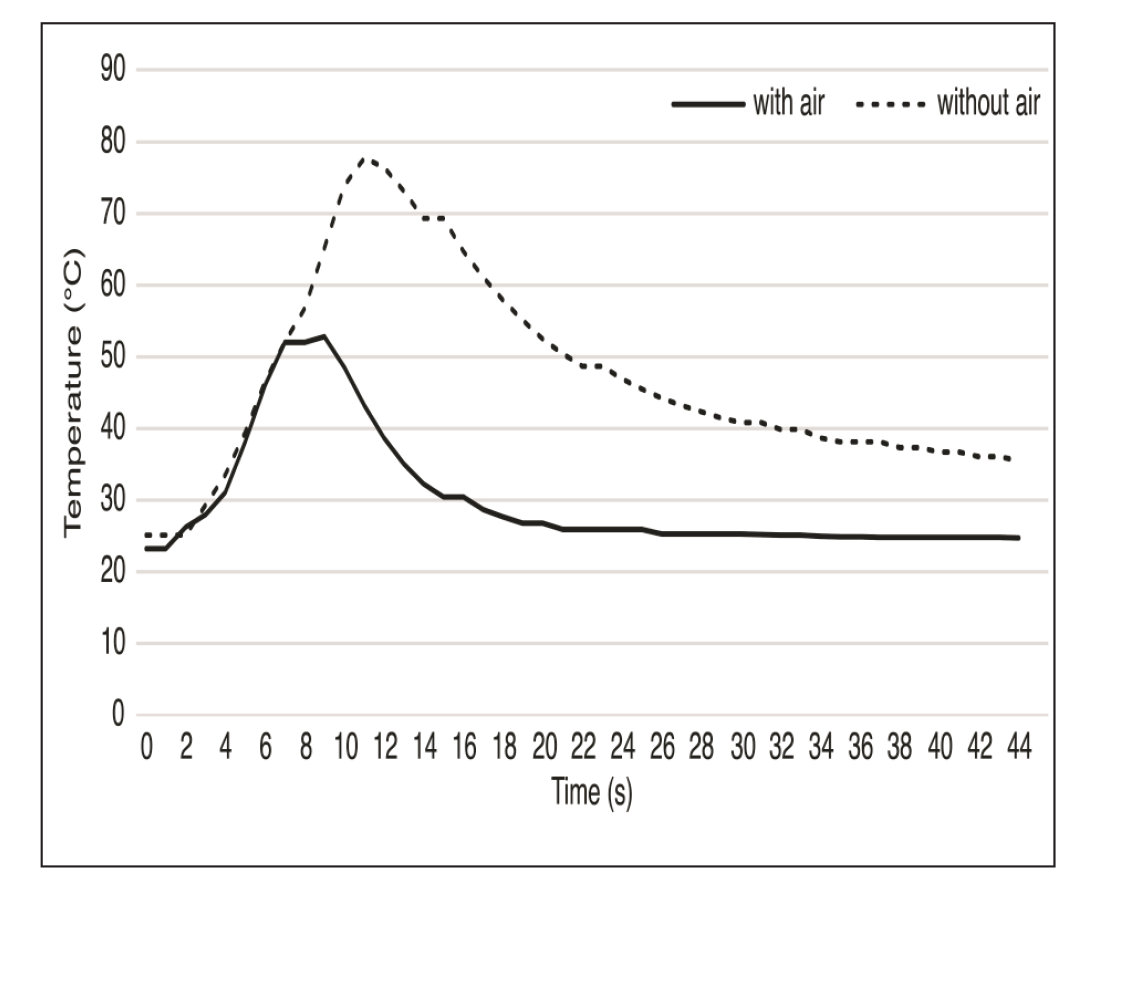
The increases in the temperature of the adhesive heated by the ultrasonic scaler at the enamel surface during repositioning procedure are shown in Figure 6. The temperature increased to 46.1 ± 4.5°C at 7 s, 52.8 ± 5.0°C at 9 s, and 48.5 ± 8.4°C at 11 s, in samples with air cooling after bracket rotation. In contrast, the temperature increased to 77.7 ± 3.5°C at 12 s in samples without air cooling after bracket rotation. The temperature on the pulpal wall is shown in Figure 7. These results revealed that the temperature of the pulpal wall increased by 2.5 ± 1.7°C at 7 s and by 2.5 ± 1.7°C at 11 s in samples with air cooling. Whereas, the maximum increase of the temperature of the pulpal wall was 8.6 ± 1.5°C at 20 s in samples without air cooling.
Temperature of Adhesive at the Enamel Surface With Air Cooling and Without Air Cooling
Increased Temperature of the Pulpal Wall
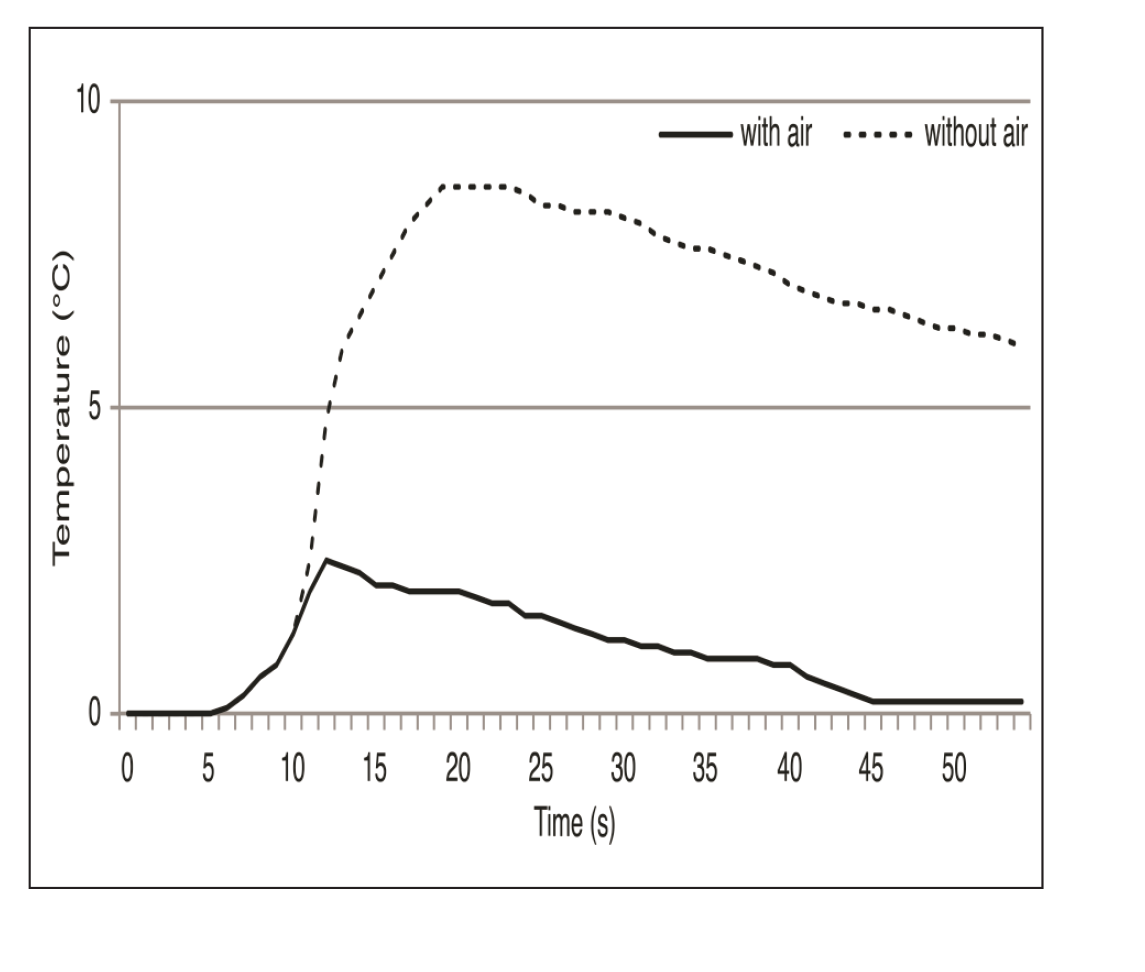
Discussion
Super-Bond is a PMMA resin adhesive that was developed for both the orthodontic and prosthodontic treatment.11-13 It is a no-filler resin adhesive available in both liquid and powder forms. The advantages of Super-Bond are its softness, which facilitates the reshaping of the resin by steal burs after curing, its metal-bonding ability, and its high bonding strength. 14 In contrast, the limitations of Super-Bond are its complicated handling and long curing time. However, the repositioning procedure in the present study was performed considering its specific reaction to heat. This reaction cannot be obtained while using the currently available light-cure resins such as Transbond XT or Transbond Supereme (3MUnitek, CA, USA), because the key characteristics of light-cure resins are their hardness and high melting temperatures. 15 It is reported that PMMA resin may change its composition through a glass-like metamorphosis when it is heated above the glass transition temperature (Tg: 70–114°C). 9 With Super-Bond, the bracket can be rotated slightly when it is heated above the Tg. This characteristic facilitates the repositioning procedure. However, more research is required to ensure the composition of PMMA resin following rehardening in order to ensure the repositioning procedure can be repeated many times.
To achieve the new strategy, the scaler tip must fit into the bracket slot to generate heat. The direction of piezoelectric oscillation seems to be parallel to the long axis of the device’s hand piece. Therefore, a proprietary tip was designed for this study, and it could be used efficiently to generate a sufficient amount of heat in conjunction with 0.022-inch slot brackets via an ultrasonic scaler used with a high-power setting. 16 An ultrasonic scaler relatively generates a huge sound during oscillating, so it was clear for the operator to notice the noisy sound became lower a little when the adhesive turns to melting state. This was an important indication to succeed the repositioning procedure.
Debonding brackets using electrothermal devices have already been reported in the literature17-19 and rebonding brackets repeatedly following debracketing have also been reported. 20 However, no previous study has reported the bracket repositioning procedure performed likely as in the present study. To complete this procedure, a process was required that made the adhesive sufficiently soft to rotate a bracket slightly before rehardening. Moreover, the bond strength needed to be adequately high to bond the brackets to the teeth during orthodontic treatment. Gwinnet reported that the shear bond strengths for metal brackets needed to be 12.1 ± 4.6 MPa. 21 Therefore, the shear bond strengths in both control and repositioning groups, in the present study, should be as high as the values reported by Gwinnet. In the present study, these strengths were found to be adequate for the orthodontic treatment.
Compared with the control group, the repositioning group had more resin adhesive remnants on the tooth surface than on the bracket base. This might have been caused by the push to the enamel surface immediately after the rotation of the bracket. In the absence of this push, the shear bond strength of the repositioning group might be lower than that of the control group.
The oscillating time for softening the adhesive was approximately 5 s. The time required to complete the repositioning procedure was approximately 7 s. However, these times are subject to deviation, largely because sometimes the tip came out of the slot because of the oscillation. Therefore, a pair of tweezers may be required to stabilize the tip in the bracket slot.
The oscillation was stopped immediately after the repositioning procedure was completed. The average temperature of the adhesive on the enamel surface was approximately 46°C at 7 s, which increased to 52.8°C at 9 s. The temperature was prevented from increasing any further than 52.8°C and returned to 36°C after 10 s with air cooling just after the rotation. However, without air cooling, the temperature continued to increase to 77.7°C at 12 s. In this case, the temperature returned to 36°C approximately 120 s later. To prevent a large and long-time increase of the temperature of enamel and retain the normal condition, air cooling may be essential.
In contrast, the average increase in the temperature of the pulpal wall was approximately 0.5°C at 7 s with air cooling. This temperature further increased to 2.5°C at 11 s without air-cooling, because of the residual heat in the bonding adhesive. 22 Zach and Cohen reported that 15% of the teeth heated at increments of 5.5°C failed to recover. 23 The 2.5°C increase measured in the present study may be below the threshold required to induce pulpal damage, and thus can be considered to be within biologically acceptable limits.24, 25
The present study demonstrated the following findings:
The custom-made tip effectively oscillates in the bracket slots during the repositioning procedure.
The shear bond strengths after bracket repositioning remained unchanged.
The oscillation time for the metal brackets was approximately 5.0 s and the repositioning time was 7.3 s.
The maximum time for the repositioning procedure was approximately 11 s for the metal brackets.
The use of an ultrasonic scaler with air cooling proved to be safe for both the enamel surface and the pulp of the human teeth.
Repositioning brackets using Super-Bond is a potentially useful approach to enable repositioning without debracketing, thus avoiding patient discomfort and saving chair time and wires for orthodontists.
Footnotes
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
