Abstract
P-glycoprotein (P-gp/ABCB1) and breast cancer resistance protein (BCRP/ABCG2) expression are frequently related to multidrug resistance (MDR) in neoplastic cells. Canine inflammatory and grade III noninflammatory mammary carcinomas (IMC and non-IMC) are aggressive tumors that could benefit from chemotherapy. This study describes the immunohistochemical detection of P-gp and BCRP in 20 IMCs and 18 non-IMCs from dogs that had not received chemotherapy. Our aim was to determine if P-gp and BCRP expression was related to the “inflammatory” phenotype, to establish a basis for future studies analyzing the response to chemotherapy in dogs with highly malignant mammary cancer. Immunolabeling was primarily membranous for P-gp with a more intense labeling in emboli, and immunolabeling was membranous and cytoplasmic for BCRP. P-gp was expressed in 17 of 20 (85%) IMCs compared to 7 of 18 (39%) non-IMCs (P = 0.006). BCRP was expressed within emboli in 15 of 19 (79%) emboli in IMC, 12 of 15 (80%) primary IMCs, and 12 of 18 (67%) non-IMCs, without statistically significant differences (P > .05). All IMCs and 67% of non-IMCs expressed at least 1 of the 2 transporters, and 63% (12/19) of IMCs and 39% (7/18) of non-IMCs expressed both P-gp and BCRP. P-gp and BCRP evaluation might help select patients for chemotherapy. P-gp, expressed in a significantly higher percentage of IMCs vs non-IMCs, might play a specific role in the chemoresistance of IMC.
Keywords
P-glycoprotein (P-gp) and breast cancer resistance protein (BCRP) are well-known adenosine triphosphate-binding cassette (ABC) transporter efflux pumps influencing chemotherapy resistance in cancer. Due to their capacity to export a wide variety of cell substrates, including many of the currently available chemotherapeutic compounds, the pumps prevent the intracellular action of these drugs. 20 De novo or intrinsic multidrug resistance (MDR) occurs in a tumor when ABC transporters such as P-gp and BCRP are expressed and functional in neoplastic cells before induction chemotherapy, while secondary or acquired expression of ABC transporters appears after the first chemotherapy treatment. 10 ABC transporters are also considered markers of the so-called side population of cancer-initiating cells. 7,23,43 Because of this, the regulation of stem cell biology by ABC transporters has emerged as an important new field of investigation. The complex role of P-gp and BCRP in breast cancer has been addressed in human research, 14,34 whereas data on the role of chemoresistance mediated by ABC transporters in veterinary oncology are currently scant. 30,68
Canine mammary neoplasia comprises a group of tumors with heterogeneous pathological phenotypes and clinical behavior. 55 Carcinomas of the bitch are classified into 3 different histological grades of malignancy according to the most recent system. 50 Histological grade III carcinomas are the rarest and have the worst prognosis, with 71% of cancer-related death and/or recurrence/metastasis within a 28-month follow-up period. 50 Based on the limited clinical information available in veterinary medicine, the drugs effective in human breast cancer, such as cyclophosphamide, 5-fluorouracil, and doxorubicin, have been translated into veterinary oncology in an attempt to treat canine mammary carcinoma (CMC). 19,27,60 Treatment guidelines for malignant canine mammary gland tumors have been proposed, 60 but the administration of a chemotherapeutic regimen to dogs with aggressive CMC has yielded conflicting results. 3,21,26,27,34,40,59,62
Human inflammatory breast cancer (IBC) and its counterpart in the dog, canine inflammatory mammary cancer (IMC), are considered the most malignant mammary tumors. 17,41,51,52,56,57,65 IBC and IMC are clinicopathological entities diagnosed on the basis of a rapid progression of signs, dermal erythema, induration, and edema of the mammary region, with the histological feature of massive embolization of neoplastic cells in superficial dermal lymphatic vessels. 52,56,65 This neoplasm bears a unique rapid-growing, angioinvasive and angiogenic phenotype, which is far from being completely understood. 2,17,29
The therapeutic approach in women with IBC usually involves neoadjuvant anthracycline- and taxane-based chemotherapy, associated when feasible with ablative surgery and locoregional radiotherapy. 6,22,61,64,65 Despite recent advances in multimodality treatments, the prognosis for women with IBC is still poor, with a median disease-free survival of less than 2.5 years. 29,66 One study on medical treatment for dogs with IMC suggests a beneficial effect of nonsteroidal anti-inflammatory drugs like piroxicam as a single-agent; 37 in another study, the administration of piroxicam combined with carboplatin, doxorubicin, capecitabine, or cisplatin showed some improvement in prolonging survival time but without statistical significance. 41 New therapeutic strategies to improve survival are needed in both species. Chemotherapeutic molecules like anthracycline are substrates of many ABC transporters, and the onset of chemoresistance to these compounds has been attributed to the expression of P-gp and BCRP in human oncology. 14,45,47 Some studies on canine mammary tumors have investigated P-gp and BCRP expression, 4,16,25,28,32,33,49,53 but the role of these chemoresistance modulators is still incipient. A previous study designed and carried out by some of the present study’s authors (M.L., B.B., G.S., C.B.) evaluated the immunohistochemical expression of P-gp and BCRP in a cohort of canine mammary hyperplasia and benign and malignant mammary tumors. 35 In that study, 22 of 47 (47%) of hyperplastic mammary lesions expressed P-gp, and 27 of 45 (60%) of these lesions were BCRP positive. However, P-gp and BCRP were most commonly expressed in malignant mammary tumors, with 35 of 46 (77%) of the cases being P-gp positive and 36 of 44 (82%) of the cases being BCRP positive, while only 4 of 10 (40%) of adenomas expressed P-gp positivity and 2 of 10 (20%) expressed BCRP. 35 Other studies have reported that these chemoresistance markers are more frequently expressed in aggressive mammary tumors compared to their benign counterparts. 16,32,48,53
Hence, the present study focused on a cohort of aggressive canine mammary tumors that included 20 IMCs and 18 grade III non-IMCs of different histological types from dogs that had not received chemotherapy. The goal of this study was to investigate if expression of these molecules was significantly associated with the “inflammatory” phenotype and to establish a basis for future studies analyzing the response to chemotherapy of canine patients with highly malignant mammary cancer. As canine mammary tumors, especially IMCs and other invasive carcinomas, have been proposed as useful spontaneous models for studying their human counterparts, 1,9,37,46,51,52,54 a better understanding of their biological behavior and chemoresistant phenotype would be helpful in both human and veterinary oncology.
Materials and Methods
Samples and Histopathology
Samples were retrieved from the archive of the Veterinary Pathology Service, Veterinary Teaching Hospital, Complutense University of Madrid, Spain. According to the reports, the dogs had not received chemotherapy at the time of biopsy. Thirty-eight formalin-fixed and paraffin-embedded tissue samples of mammary gland from 38 dogs were selected based on the clinical and histopathological diagnoses of IMC and histologic grade III non-IMC. Carcinomas were graded according to the system proposed by Peña et al. 50 In cases of IMC, the primary mammary carcinoma was included in the study when available (n = 15). All primary IMCs were histological grade III.
IMC diagnosis was based on the typical clinical presentation (with dermal erythema and edema in the ventral abdominal dermis), histologically associated with neoplastic emboli in superficial dermal lymphatic vessels. IMC emboli were detectable in each case (20/20), while the corresponding primary IMC was available in 15 cases. Hematoxylin and eosin–stained slides were histopathologically examined, and when necessary, the original diagnosis was updated according to the current histologic classification proposed by Goldschmidt et al. 18 Only grade III carcinomas were included in the study.
Immunohistochemical Expression of P-gp and BCRP
Paraffin blocks were sectioned (3 μm) and placed in a PT module (Lab Vision, Fremont, CA) containing EDTA buffer solution (pH 8.0) (MAD-004072R/D; Master Diagnostica, Granada, Spain), heated for 20 minutes at 95°C, and cooled to 60°C (dewaxing and antigen retrieval). Slides were rinsed in warm tap water and placed in an automated immunostainer (Lab Vision) for immunohistochemistry. Slides were incubated for 120 minutes at room temperature with the following primary antibodies: mouse monoclonal anti–P-gp/CD243 (C494, GTX23365, dilution 1:1500; GeneTex International, Irvine, California) and mouse monoclonal anti-BCRP (BXP-21, Millipore-MAB4146, dilution 1:200; Merck, Darmstadt, Germany). Immunolabeling was detected with the peroxidase Master Polymer Plus Detection System (MAD-000237QK; Master Diagnostica), and subsequently, the slides were counterstained with Mayer’s hematoxylin and permanently mounted with DPX mountant. External (normal canine liver) and internal (endothelium of blood and lymphatic vessels) positive controls for P-gp and BCRP were used. The cell membrane of hepatocytes (especially at the biliary canaliculi level), biliary epithelial cells, and endothelial cells are normally labeled by both anti-Pgp and anti-BCRP antibodies, and these served as positive controls.
Corresponding negative control slides were processed in parallel by replacing the primary antibody with nonreactive antibody. P-gp and BCRP immunolabeling was considered positive when >20% and >10% of cells were labeled for P-gp and BCRP, respectively, as suggested by previous studies. 13,35,53 A further semiquantitative evaluation of the immunostaining was performed, and the positive carcinomas were assigned to 2 subgroups according to the percentage of positive cells: intermediate positivity (range of 20%–50% of P-gp–positive cells; range of 10%–50% of BCRP-positive cells) or high positivity (>50% of P-gp–positive cells; >50% of BCRP-positive cells). One case of IMC with no available primary tumor was excluded from the evaluation of immunolabeling with anti-BCRP antibody because the internal control did not show the expected immunoreactivity with BCRP, probably due to antigen denaturation by overfixation. The selected samples included 20 IMCs and 18 non-IMCs.
Statistical Analysis
P-gp and BCRP expression were compared by Fisher’s exact method (GraphPad Software, La Jolla, CA). In IMCs, neoplastic cell emboli were evaluated separately from the primary tumor and compared to each other. P-gp expression was evaluated in IMC emboli vs non-IMC and primary IMC vs non-IMC. BCRP expression was evaluated in IMC emboli vs non-IMC and primary IMC vs non-IMC. P < .05 was considered significant.
Results
In the 15 IMCs for which the primary carcinoma was available, histotypes of the primary IMCs included 6 micropapillary invasive carcinomas, 3 comedocarcinomas, 2 lipid-rich carcinomas, 2 solid carcinomas, 1 adenosquamous carcinoma, and 1 anaplastic carcinoma. Five cases of IMC did not have evidence of an associated primary mammary carcinoma; these samples were composed of dermal incisional biopsies (4 were sampled at necropsy, and 1 was submitted for histologic evaluation by a private practitioner) and histologically had massive embolization by neoplastic cells in dermal lymphatic vessels. In 8 cases of IMC, the embolized lymphatic vessels were surrounded by desmoplasia, often accompanied by severe dermal edema. Only 2 cases showed multifocal areas of intratumor colliquative necrosis, while another 2 cases had abundant inflammatory infiltrates of neutrophils, lymphocytes, and plasma cells associated with the neoplasia.
Histotypes of non-IMC included 7 solid carcinomas, 5 micropapillary invasive carcinomas, and 1 each of carcinoma mixed type, tubulopapillary carcinoma, comedocarcinoma, anaplastic carcinoma, adenosquamous carcinoma, and carcinoma and malignant myoepithelioma. Eight cases of non-IMC showed multifocal areas of colliquative necrosis in more than 50% of the tumor. Examples of IMC and non-IMC histotypes are shown in Supplemental Figures S1 to S4.
The diffuse membranous immunolabeling of canine normal liver, the positive control for P-gp and BCRP, is shown in Supplemental Figures S7 and S8, while the negative controls are shown in Supplemental Figures S9 and S10.
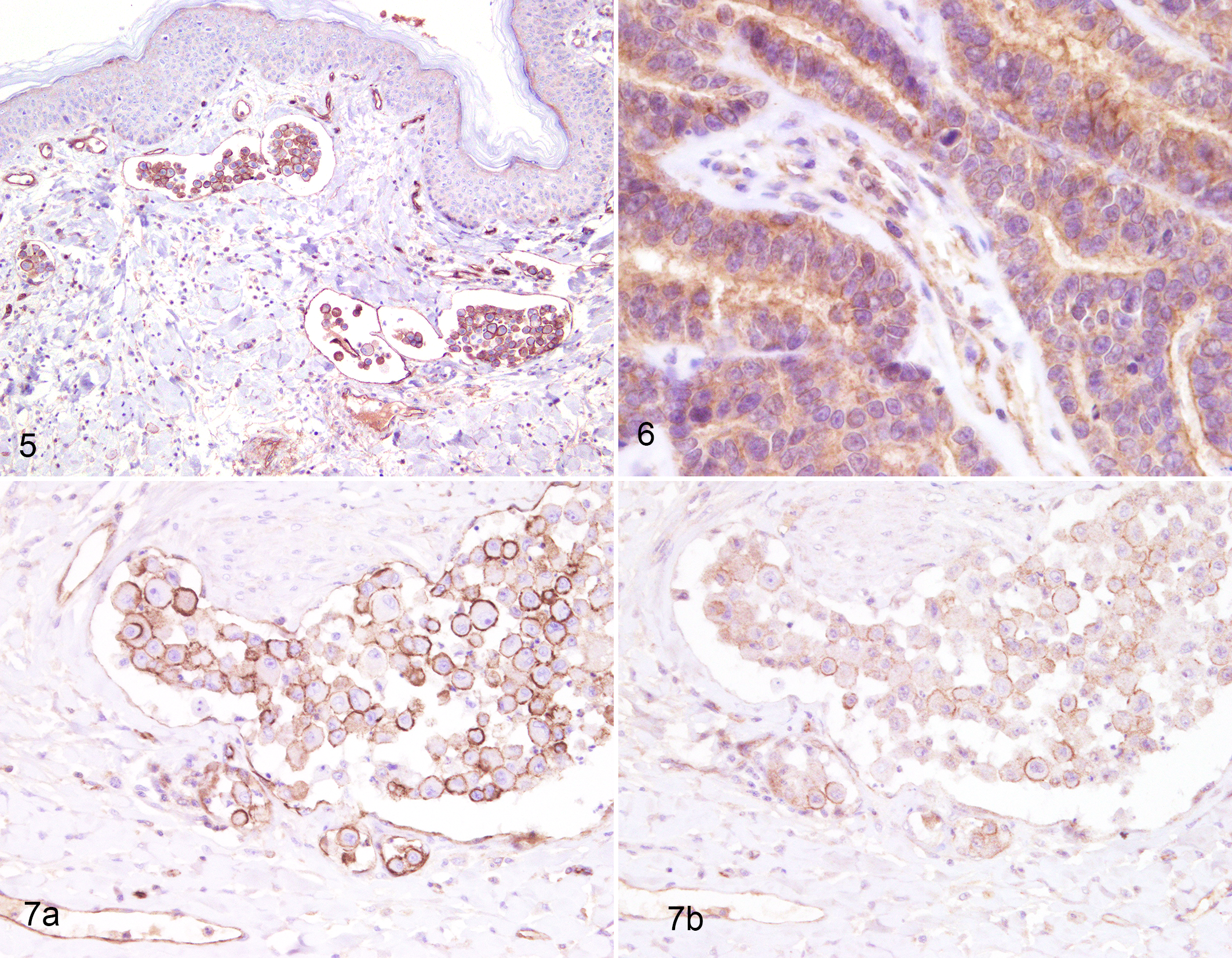
In tumor cells, P-gp immunolabeling was mainly membranous (Fig. 1) and was particularly strong in neoplastic emboli of IMC (Fig. 2). IMC emboli had cells with peculiar morphological features of severe anisokaryosis and anisocytosis. Some tumor cells stood out for their endothelial-like morphology, characterized by a rim of elongated cytoplasm containing extended eccentric nuclei encircling an empty round space and suggestive of vasculogenic mimicry. These cells were intensely immunolabeled for P-gp (Figs. 3, 4). BCRP showed membranous and cytoplasmic immunolabeling (Figs. 5, 6). Considering IMCs and non-IMCs together, P-gp was expressed in 24 of 38 (63%) tumors, and BCRP was expressed in 27 of 37 (73%) tumors. IMCs expressed P-gp in lymphatic emboli in 17 of 20 (85%) cases and in 12 of 15 (80%) primary IMCs. Fewer non-IMCs (7/18, 39%) expressed P-gp. P-gp expression was significantly higher in emboli of IMC vs non-IMC (P = .006) and in primary IMC vs non-IMC (P = .032) (Suppl. Fig. S5).
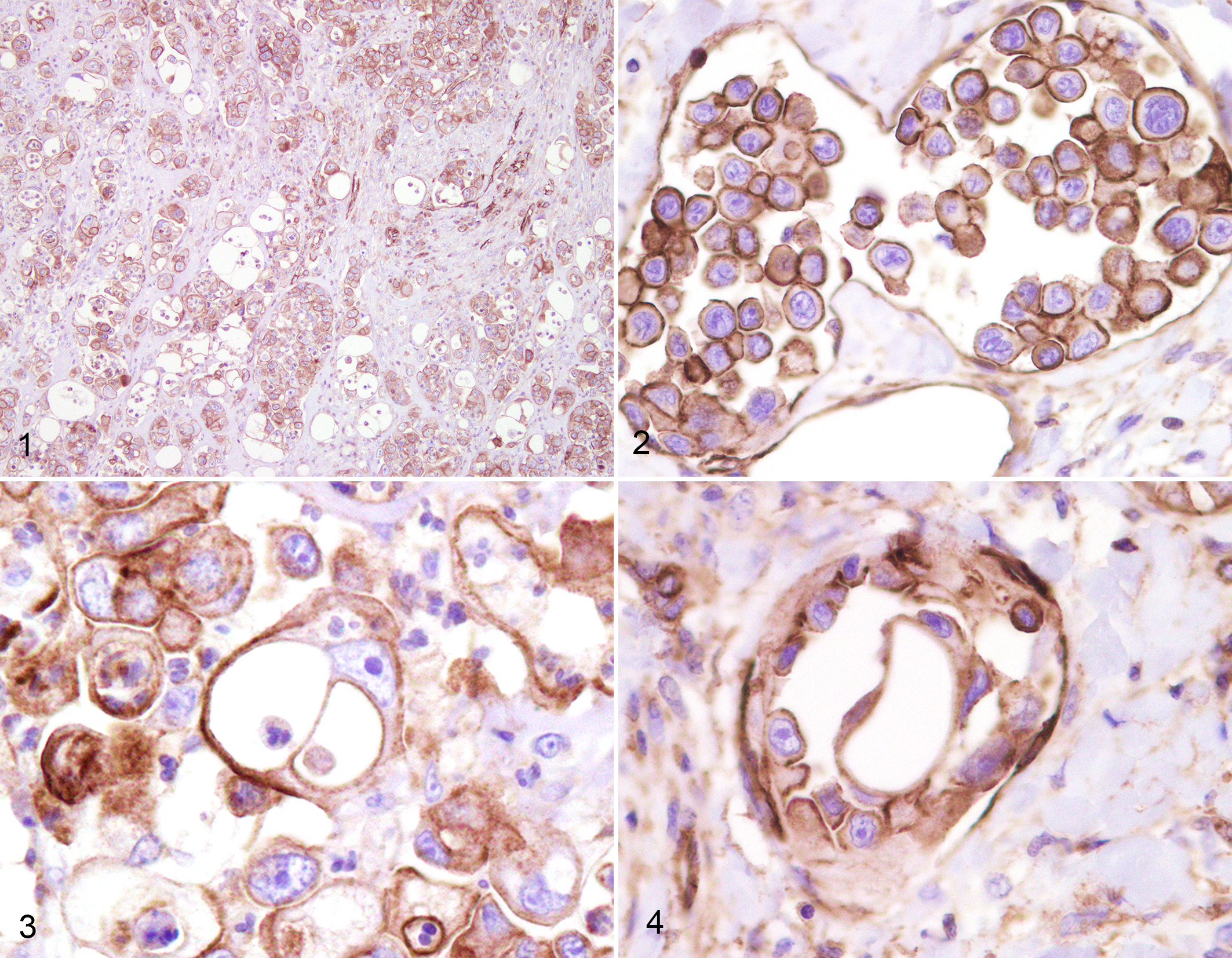
Canine inflammatory mammary cancer (IMC), mammary gland, dog. Immunohistochemistry for P-glycoprotein (P-gp).
Mammary gland, dog. Immunohistochemistry for breast cancer resistance protein (BCRP) and P-glycoprotein (P-gp).
BCRP was expressed in 15 of 19 (79%) IMC emboli, 12 of 15 (80%) primary IMCs, and 12 of 18 (67%) non-IMCs (Suppl. Fig. S6). There was no significant difference in BCRP expression between IMC and non-IMC.
Coexpression of P-gp and BCRP in the same tumor is summarized in Table 1.
Expression of Both P-gp and BCRP in Canine Inflammatory and Grade III Noninflammatory Mammary Carcinomas.
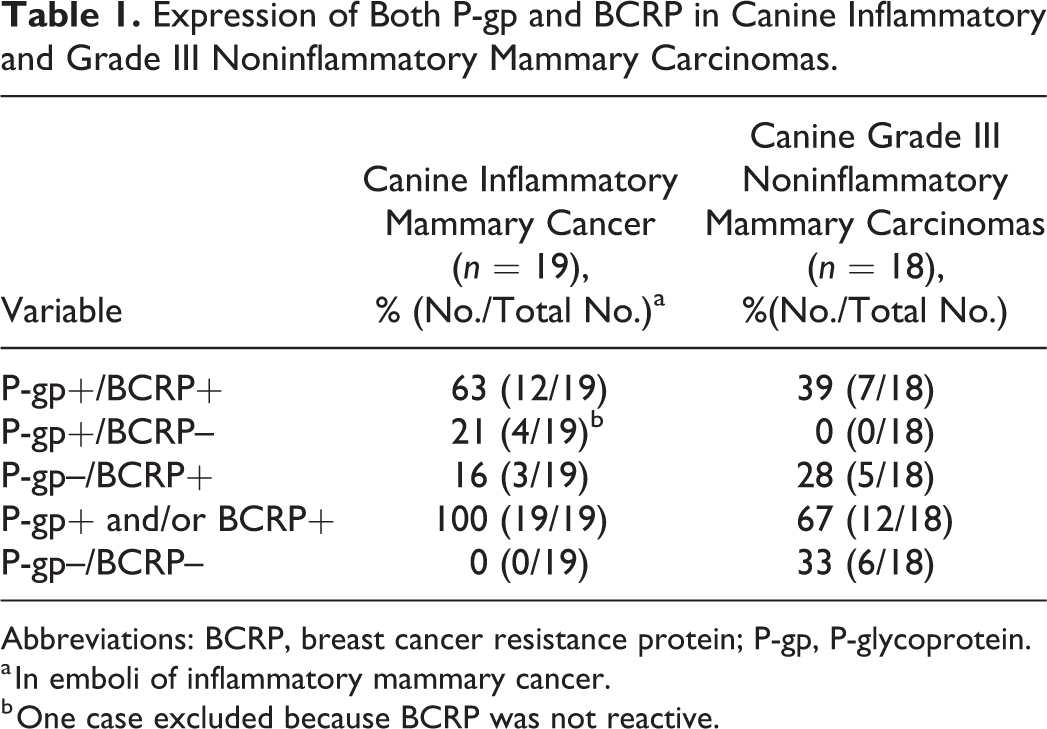
Abbreviations: BCRP, breast cancer resistance protein; P-gp, P-glycoprotein.
a In emboli of inflammatory mammary cancer.
b One case excluded because BCRP was not reactive.
Considering IMCs, 12 of 19 (63%) emboli expressed both P-gp and BCRP, and all IMCs expressed at least one of the transporters (Fig. 7a,b). Considering non-IMCs, 7 of 18 (39%) expressed both P-gp and BCRP, and 12 of 18 (67%) expressed at least one of the transporters.
Non-IMC lacking both P-gp and BCRP expression included 2 solid carcinomas, 2 micropapillary invasive carcinomas, 1 adenosquamous carcinoma, and 1 tubulopapillary carcinomas.
Considering the subgrouping of the positive carcinomas, IMCs showed mostly a high number of positive cells for both transporters (>50% P-gp–positive cells in 11 of 17 positive cases; >50% of BCRP-positive cells in 9 of 15 positive cases). Of the 7 P-gp–positive primary non-IMCs, 3 contained between 20% and 50% of P-gp–positive cells and 4 cases had >50% P-gp–positive cells. Of the 12 BCRP-positive primary non-IMC cases, 3 had between 10% and 50% BCRP-positive cells and 9 had >50% BCRP-positive cells.
Discussion
This is the first study to compare the expression of chemoresistance-associated markers P-gp and BCRP in canine grade III IMCs and comparable grade III non-IMCs. These 2 uncommon tumor groups are biologically aggressive, especially IMC, and hence are potentially suitable for chemotherapy.
This study presents a valuable caseload as it comprises rare neoplasms. The histological malignancy of the cases selected is represented not only by the high grade (grade III) but also by numerous highly malignant histotypes: micropapillary invasive carcinomas (6/20 cases) and comedocarcinomas (3/20 cases) in the IMC group, as well as micropapillary invasive carcinomas (5/18) and solid carcinomas (7/18) among the non-IMCs. Comedocarcinoma and solid carcinoma have been recently defined as histotypes bearing a poor prognosis. 55
P-gp and BCRP both seem to significantly contribute to multidrug resistance in human oncology. 14,15,24,34 According to human breast cancer literature, chemoresistance associated with P-gp and BCRP expression in tumors not subjected to chemotherapy at the time of biopsy is presumably an intrinsic phenomenon, and ABC transporters’ expression by neoplastic cells may lead to the failure of induction chemotherapy from the start. 10
P-gp expression is the most widely studied mechanism of chemoresistance in breast cancer. 11,12,36,42,44,63 About 40% of breast cancers express P-gp, and its expression after exposure to chemotherapeutic drugs known to be P-gp substrates is correlated with a worse response to treatment in both the adjuvant and neoadjuvant settings. 11,31,58,63
Studies on P-gp expression in canine mammary tumors have reported P-gp protein, or MDR-1 messenger RNA (mRNA), and its correlation with general clinical parameters. 5,16,30,32,35,53 P-gp expression varied from 76% to 50%. 4,53 Increased P-gp expression has been found in canine mammary carcinomas compared with adenomas, and most authors agree that this finding is linked to the degree of tumor malignancy. 4,32,35,53
The present study found that IMCs expressed P-gp in 85% of emboli and in 80% of primary carcinomas, whereas this transporter was expressed in 38% of non-IMCs. Therefore, immunohistochemistry (IHC) can detect P-gp expression in both non-IMCs and IMC. The higher percentage of P-gp–positive cases (63%) in the present study compared to that of Petterino et al 53 could be explained by the fact that we included IMCs and grade III non-IMCs that are very aggressive, a feature related to a higher expression of chemoresistance markers. 32
The chemoresistance marker BCRP has been reported to be expressed in breast cancer and has been correlated with resistance to 5-fluorouracil. 8,13,38,39,45,67 Few studies are available on BCRP expression in canine mammary tumors. 25,35,48,49 Interestingly, BCRP was reportedly expressed in all canine tumor cell lines examined, and thus it was suggested that since BCRP induces resistance to doxorubicin, treating canine mammary tumors with doxorubicin should be considered with caution. 25 Other IHC studies found a high percentage of neoplastic cells expressing BCRP and a positive correlation with the degree of canine mammary tumor malignancy. 35,48 The present study found BCRP expressed in 79% of IMC emboli, 80% of primary IMCs, and 67% of non-IMCs. These findings are in accordance with the literature reporting that aggressive canine mammary tumors often display resistance to chemotherapeutic drugs and that the administration of BCRP substrates should be carefully considered.
Another interesting finding in the present study is that all IMCs expressed at least 1 of the 2 pumps, while 63% of IMCs and 39% of non-IMCs coexpressed both BCRP and P-gp. This suggests these tumors are likely capable of developing resistance toward substrates of both P-gp and BCRP, bearing a more complex multidrug resistance phenotype. Expression of more than 1 ABC transporter mRNA by the same tumor has been described in 56% of 103 canine mammary tumors where 7 ABC transporters, including P-gp and BCRP, were coexpressed. P-gp and BCRP were expressed in 92% and 100% of the tumors, respectively. 25 These findings suggest caution when substrates of P-gp and BCRP (ie, doxorubicin, vincristine, mitoxantrone) are prescribed in the treatment of IMCs, non-IMCs, and canine mammary gland tumors. The routine evaluation of P-gp and BCRP expression may be potentially useful to select patients for chemotherapy as some human patients appear to have a naturally more aggressive phenotype associated with high levels of baseline P-gp expression. 11,20,68
Conclusions
The expression of P-gp and BCRP seems to be common in dogs with highly malignant non-IMC and IMC. Caution is therefore required when administering substrates of P-gp and BCRP, because these tumors may bear chemoresistance toward these drugs. Routine evaluation of MDR marker expression may serve to select patients for chemotherapy.
Future prospective studies are needed to demonstrate the association between chemoresistance and the expression of MDR markers in canine mammary cancer, as well as to shed more light on the complexity of its pathogenic mechanisms. This will serve to devise adequate patient-tailored chemotherapy protocols. Spontaneous canine IMC could represent a model to help understand its human counterpart, IBC, an understudied entity to date.
Supplemental Material
Supplemental Material, DS1_VET_10.1177_0300985819868647 - P-Glycoprotein and Breast Cancer Resistance Protein in Canine Inflammatory and Noninflammatory Grade III Mammary Carcinomas
Supplemental Material, DS1_VET_10.1177_0300985819868647 for P-Glycoprotein and Breast Cancer Resistance Protein in Canine Inflammatory and Noninflammatory Grade III Mammary Carcinomas by Michela Levi, Laura Peña, Angela Alonso-Díez, Barbara Brunetti, Luisa Vera Muscatello, Cinzia Benazzi, Maria Dolores Pérez-Alenza and Giuseppe Sarli in Veterinary Pathology
Footnotes
Acknowledgements
We thank Pedro Aranda for histological technical assistance. Anne Collins edited the English text.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This study was supported by the travel bursary assigned to junior scientists (M. Levi) in 2017 by the Journal of Comparative Pathology Educational Trust.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
