Abstract
Papillomas of the conjunctival surface in people can be of viral or nonviral origin and are found in high association with human papillomavirus. Canine conjunctival papillomas are seldom described, and published accounts have mostly been associated with canine oral papillomavirus infection. Here, we describe conjunctival squamous papillomas that do not express papillomavirus proteins and compare them with papillomavirus-associated conjunctival papillomas. Conjunctival squamous papillomas presented a distinct histopathologic profile and lacked the cytopathic effects seen in viral papillomas. They appeared as exophytic, papilliferous, pedunculated lesions with delicate fronds and angular terminal margins. Squamous papillomas presented with a delicate fibrovascular core and were associated both clinically and grossly with a feeder vessel. Pigmentation was variable within the epithelium and stroma of these lesions, and inflammatory infiltrates were characteristically minimal. Conjunctival squamous papillomas resembled squamous papillomas of the skin; however, they lacked significant hyperkeratosis. Compared with conjunctival viral papillomas, these masses occurred in older dogs and were smaller and solitary. Furthermore, polymerase chain reaction and immunohistochemistry failed to demonstrate papillomavirus genetic material and antigens in conjunctival squamous papillomas. Both viral and nonviral conjunctival papillomas were considered benign.
Canine papillomas have been described both on skin and mucosal surfaces and are commonly associated with a viral etiology. Although some papilliferous growths are malignant or may undergo malignant transformation, most of these masses are benign. 8 Viral papillomas can be diagnosed by histopathology, polymerase chain reaction (PCR), immunohistochemistry, and in situ hybridization. By convention, viral papillomas are morphologically identified based on the presence of cytopathic effects within superficial epithelial cells, including hyperplasia of the stratum granulosum and formation of giant keratohyaline granules, keratinocytes with clear or amphophilic cytoplasm, and small, smudged, or vesiculate nuclei (koilocytes) or occasional basophilic intranuclear viral inclusions. Nonviral papillomas of the skin are also termed squamous papillomas; these lesions are poorly described in the literature and typically exhibit delicate keratinized fronds with minimal inflammatory infiltrates and no cytopathic effect. 3 Papillomas of the canine conjunctiva are seldom described, and published accounts have been mostly associated with papillomavirus infection. 1,2,4 In people, papillomas of the conjunctiva are often, but not invariably, associated with human papillomavirus. 5 At the Comparative Ocular Pathology Laboratory of Wisconsin (COPLOW), we recognize 2 categories of primary benign papillomas of the conjunctival surface: those with characteristic features of papillomavirus infection and those with features resembling those seen in cutaneous squamous papillomas. Here, we describe the features of squamous papillomas of the conjunctival surface in dogs that do not present features associated with papillomavirus infection and differentiate them from their viral counterpart. Five papillomas resembling the conjunctival squamous papillomas described herein were described in a published account; however, etiology was not investigated. 4
Materials and Methods
Sample Population
The COPLOW archives approximately 30 000 formalin-fixed, paraffin-embedded canine ocular tissues of various animals. A search of the database for the terms conjunctiva and papilloma revealed 145 samples classified as conjunctival squamous papillomas and 31 as conjunctival viral papillomas. Submission sheets, including signalment and chief complaint, were available for all specimens. Histologic sections were routinely prepared and stained with hematoxylin and eosin and at times with alcian blue/periodic acid–Schiff. Two board-certified veterinary pathologists (L.B.C.T. and R.R.D.) examined the histologic specimens and recorded histologic features for each specimen.
Immunohistochemistry
Ten tissues classified as conjunctival squamous papillomas and 4 tissues classified as conjunctival viral papillomas were selected for immunohistochemical staining. The 4-µm-thick unstained histologic sections were used for immunohistochemical staining performed with an automated staining system (intelliPATH, BiocareMedical, Concord, CA). A cocktail of 2 monoclonal antibodies raised against bovine papillomavirus (BPV)–1 major capsid protein and the major capsid protein L1 of human papillomavirus type 16 were used as the primary antibody in a 1:400 dilution (ab2417; Abcam, Cambridge, MA) and incubated for 45 minutes at room temperature. A canine cutaneous papilloma with microscopic lesions typical of infection with papillomavirus was used as a positive tissue control, and a normal canine eye with associated conjunctival tissue was used as a negative control. Heat-induced epitope retrieval was performed in a decloaker chamber using citrate buffer (DIVA; BiocareMedical), and an immunoperoxidase detection kit (ProMark; BiocareMedical) was used to demonstrate the reaction by using 3,3′-diaminobenzidine as chromogen and Mayer’s hematoxylin as counterstain.
PCR
The same 10 tissues classified as conjunctival squamous papillomas and 4 tissues classified as viral papillomas were selected for papillomavirus PCR testing. Of these tissues, 5-µm-thick paraffin-curls were sterilely prepared and used for PCR. Laboratory technicians were blinded to the histologic diagnosis of the examined tissues.
Four primer pairs were used for the examination of canine papillomavirus using previously described methods. Three canine oral papillomavirus (COPV) primer pairs were used as previously described and validated in the literature: 2,7 L1+ sense and L1– antisense primers, providing a 261-bp amplicon of the late gene open reading frame of COPV; E6+ sense and E6– antisense, providing a 350-bp amplicon of the conserved transformation-associated E6 reading frame of COPV; and E7+ sense and E7– antisense primer, providing a 204-bp amplicon of the conserved transformation-associated E7 reading frame of COPV. One primer pair was used for BPV as previously described and validated in the literature: 6 E5+ sense and E5– antisense, providing a 244-bp amplicon of the conserved transformation-associated E5 reading frame of BPV-1 or a 248-bp amplicon from BPV-2. Tissues with BPV and an equine sarcoid were used as positive controls for the BPV primer set E5+ and E5–.
Results
Conjunctival squamous papillomas presented clinically as small, pigmented, or tan raised lesions (Fig. 1). These masses were often smaller than conjunctival masses later diagnosed as viral papillomas (Fig. 2). Dogs that presented with a conjunctival squamous papilloma had a mean ± SD age of 9.4 ± 2.6 years. Breed and sex predilections were not observed; 45 breeds were represented in 145 cases, of which 68 were female, 70 were male, and 7 were of unknown sex. Dogs that presented with conjunctival viral papillomas had a mean ± SD age of 3.7 ± 3.4 years. Breed predilection was not observed, and 19 breeds were represented in 31 cases. There was a slight male predilection with 11 females, 19 males, and 1 dog of unknown sex.
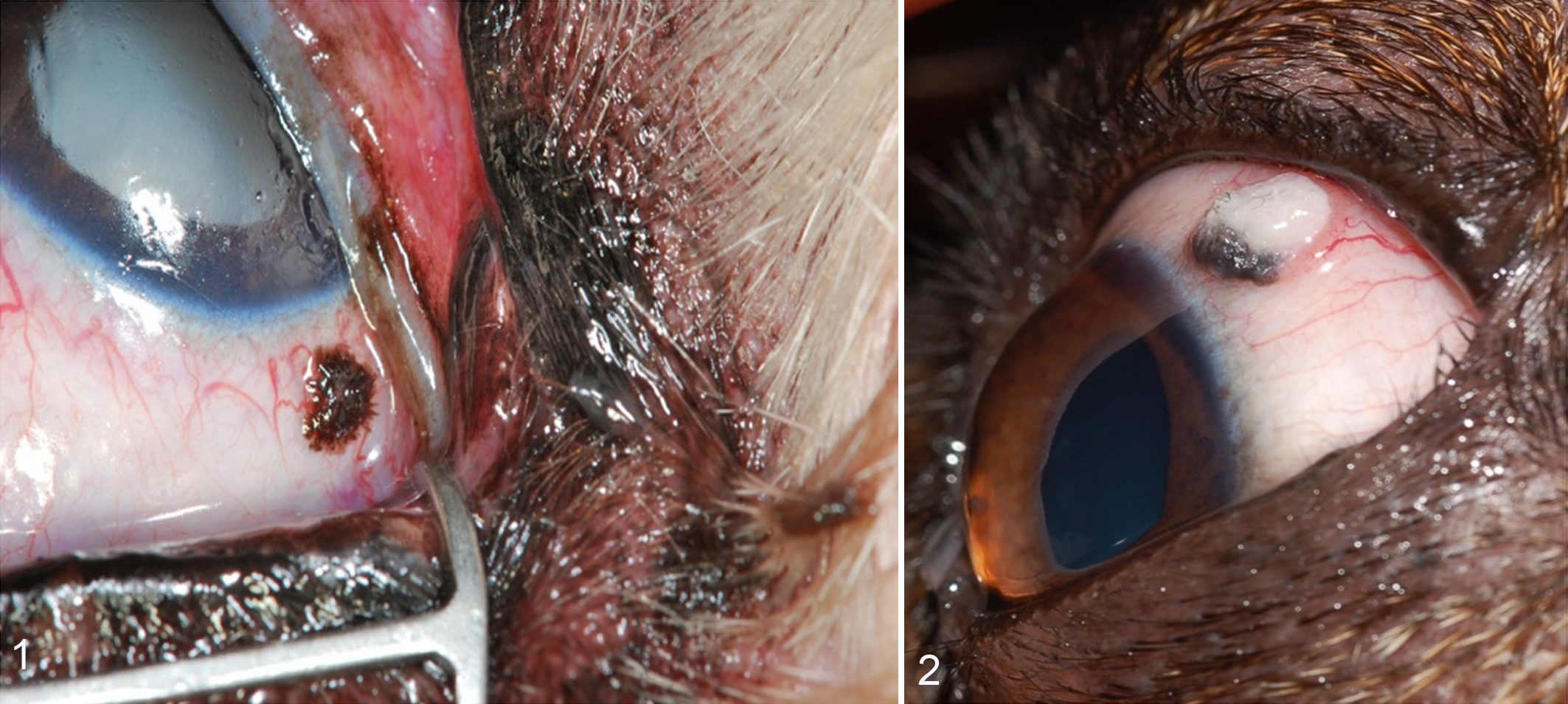
Bulbar conjunctiva, dog.
Pathologic Features
Clinically, conjunctival squamous papillomas were only occasionally recognized for what they were. Occasionally, the papillary nature of these lesions was obvious, and feeder vessels were macroscopically evident (Figs. 1, 3).
Conjunctival squamous papilloma, dog, conjunctiva.
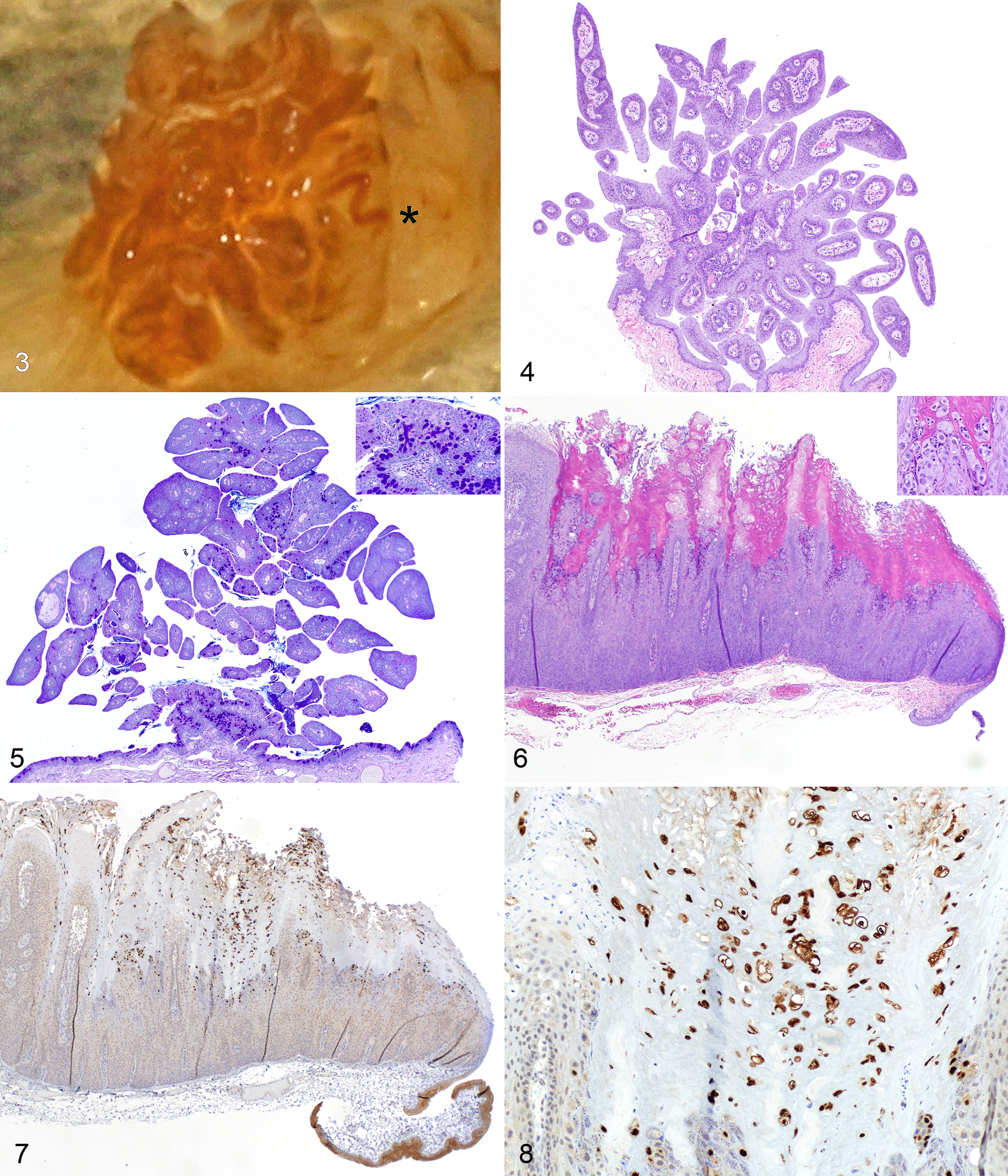
Histologically, conjunctival squamous papillomas contained numerous delicate fronds, often with sharp edges (Fig. 4). The fronds were connected with a fine fibrovascular core, which often attached to the conjunctiva by a stalk (Fig. 5). The degree of lesion pigmentation varied, and melanin granules appeared either in the epithelium or within the superficial substantia propria. The epithelial surface of the fronds was hyperplastic but did not exhibit hyperkeratosis, and the presence of goblet cells was minimal to marked (Fig. 5). Within the fibrovascular core, lymphoplasmacytic infiltrates were minimal to absent.
Conjunctival viral papillomas presented histologic features similar to those described in previous literature. 2 Briefly, viral papillomas were most often papilliferous exophytic lesions that presented hyperkeratosis and cytopathic effects such as a thickened stratum granulosum and large epithelial cells interpreted as koilocytes as well as occasional intranuclear inclusions (Fig. 6).
Immunohistochemistry
Immunohistochemistry against the papillomavirus antibody did not label any (10/10) conjunctival squamous papillomas; positive labeling was observed in all (4/4) viral papillomas (Figs. 7, 8). Diffuse positive staining interpreted to be inconsequential background staining was observed in epithelial cells of conjunctival squamous papillomas. The same background staining pattern was also seen in the unaffected epithelium at the margins of viral papillomas (Fig. 7) and in negative control tissue. Positive immunolabeling in viral papillomas was seen as strong nuclear staining and, less commonly, as intense cytoplasmic staining (Fig. 8) within keratinocytes that showed a cytopathic effect on hematoxylin and eosin staining. Labeling was located in the upper layers of the stratum spinosum and granulosum and was less defined in the stratum corneum.
PCR
The 4 primer pairs L1+ and L1–, E6+ and E6–, E7+ and E7–, and E5+ and E5– were positive in 4 of 4 samples diagnosed as canine conjunctival viral papillomas and were negative in 10 of 10 samples diagnosed as canine conjunctival squamous papillomas.
Discussion
Squamous papillomas occur on both skin and mucosal surfaces. The literature regarding papillomas occurring on the conjunctival surface of dogs has focused on those with a viral cause. We present conjunctival squamous papillomas that occur without evidence of papillomavirus infection. Histologically, conjunctival squamous papillomas resembled the appearance of squamous papillomas of the skin with delicate sharp-edged fronds; however, they lacked hyperkeratosis. Moreover, they occasionally presented goblet cells, which are particularly frequent in the conjunctiva of the third eyelid. It is possible that the papillary nature of these lesions is often not clinically apparent because the tear film molds the lesion, therefore obscuring the papillary fronds (Fig. 1). A similar molding effect was seen when removing biopsied tissues from the liquid fixative (Fig. 3).
Conjunctival squamous papillomas were surgically removed later in life than most viral-associated papillomas and were often smaller and pigmented. We suspect that clinicians may not submit typical viral papillomas from younger dogs for histopathologic assessment because the diagnosis would be apparent from the clinical presentation. Likewise, conjunctival squamous papillomas are usually innocuous, and affected dogs may have carried the lesion for an extended period.
Our results demonstrate a strong relationship between the histologic appearance of these lesions and the results of both immunohistochemistry and PCR testing for papillomavirus. Although negative PCR and immunohistochemistry results for conjunctival squamous papillomas do not rule out the possibility of historic involvement of a papillomavirus, such involvement was neither demonstrated by molecular methods in 10 cases nor was it suspected by histologic appearance in any of the 145 cases.
In previous accounts, immunohistochemistry failed to consistently demonstrate the presence of papillomavirus antigens, otherwise demonstrated by PCR and in situ hybridization. 2,7 In this study, immunohistochemistry showed strong positivity in all tissues suspected to be associated with papillomavirus infection. The monoclonal antibodies against papillomavirus antigens used in this study differed from the polyclonal antibody used in both prior accounts, possibly affecting the difference observed between the results seen in our study compared with previous studies.
A previous publication describing 3 papillomavirus-associated conjunctival papillomas referred to one as a conjunctival squamous papilloma, 2 but it presented with cytopathic effects and marked hyperkeratosis. We contend that careful attention should be made to use terminology that accurately differentiates conjunctival papillomas associated with papillomavirus infection (viral papilloma) from those papillary lesions not associated with papillomavirus (conjunctival squamous papilloma).
Footnotes
Author Contribution
B. Beckwith-Cohen contributed to conception and design; contributed to acquisition, analysis, and interpretation; drafted manuscript; gave final approval; and agrees to be accountable for all aspects of work ensuring integrity and accuracy. L. B. C. Teixeira contributed to acquisition, analysis, and interpretation; critically revised manuscript; gave final approval; and agrees to be accountable for all aspects of work ensuring integrity and accuracy. J. A. Ramos-Vara contributed to analysis and interpretation; critically revised manuscript; gave final approval; and agrees to be accountable for all aspects of work ensuring integrity and accuracy. R. R. Dubielzig contributed to conception and design; contributed to acquisition, analysis, and interpretation; critically revised manuscript; gave final approval; and agrees to be accountable for all aspects of work ensuring integrity and accuracy.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
