Abstract
Recently, contamination of pharmaceuticals with diethylene glycol (DEG) and food with melamine and cyanuric acid has demonstrated the impact of globalization on drug and food safety. By examining the details of these outbreaks, some important lessons can be learned. Toxicoses from contaminated food and drugs are often identified only when large numbers of people or animals are affected and numerous deaths result. Populations most at risk are those repeatedly exposed to a single product. Toxicoses may be complex, involving synergism among relatively nontoxic co-contaminants. Although some contamination may occur inadvertently, practices of deliberate contamination of food and drug ingredients may be widespread but escape detection in poorly regulated markets. If this deliberate contamination is motivated by personal financial gain, it is likely to recur and be concealed. The contaminated raw material produced in a poorly regulated market may cross national boundaries and be used in manufacturing processes for numerous products, sometimes in more well-regulated markets. Once in the production chain, contaminated raw materials may be widely disseminated. It is not clear that regulatory organizations have the capacity to identify significant contaminations despite their best efforts. The veterinary and medical communities, in cooperation with regulatory agencies, should develop cooperative programs designed to detect and limit these global outbreaks. Although addressing regional or national outbreaks remains an important role for regulatory agencies, the veterinary and medical communities must develop proactive global approaches to this global problem.
Do not look where you fell, but where you slipped. —African proverb
Within the last 10 years, there has been increased globalization of drug manufacturing as well as outsourcing of production of constituent drug and food ingredients. 1 Although final product manufacturing may be performed under highly regulated guidelines, the raw materials entering the regulated production process may have originated in countries under poorly regulated conditions. Recent incidents of toxicity associated with contaminated raw materials offer lessons about the effects of globalization of drug and food manufacturing on consumer safety. 1,6,18
Real-World Examples: Nephrotoxicity Caused by Diethylene Glycol and Melamine/Cyanuric Acid
The addition of diethylene glycol (DEG) to liquid medicines and melamine/cyanuric acid to food ingredients produced in China has raised international health concerns and is illustrative of the potentially disastrous effects of outsourcing of food and pharmaceutical production on public and animal health.
Intoxication with DEG is not a new phenomenon. In 1937, more than 100 people died in the USA from acute renal failure after ingesting DEG-contaminated sulfanilamide elixir. 18,21 In this episode of DEG poisoning, DEG was added as a liquid sweetener without knowledge of its highly toxic nature. This accidental toxicosis, in part, led to the enactment of the 1938 Federal Food, Drug, and Cosmetic Act requiring proof of safety before drugs were introduced into the marketplace. Although subsequent mass poisonings from DEG have not been recognized in the USA, repeated episodes of DEG toxicosis continue to occur in the developing world. In late 1995 and early 1996, more than 100 children were admitted to hospitals in Haiti with acute renal failure due to ingestion of DEG-contaminated acetaminophen syrup manufactured in Haiti; 99 of 109 affected children died. 14,16 Between 1990 and 1998, similar outbreaks of DEG poisoning caused the deaths of hundreds of children in Argentina, Bangladesh, India, and Nigeria. 26,30 In 2006, a Panamanian physician reported an unusual number of cases of acute renal failure in adults. 21 Twelve of 21 affected patients died. With assistance from the Centers for Disease Control and Prevention (CDC) in the USA, DEG was identified in samples of prescription cough syrup. In these outbreaks, DEG was present in a single constituent ingredient, glycerin, a sweetener used worldwide in liquid medicaments. Most recently, 84 children died in Nigeria after being exposed to a teething mixture contaminated with DEG. 6
In early 2007, large numbers of dogs and cats in North America developed acute renal failure associated with ingestion of certain brands of pet food. 2-4 Shortly thereafter, a pet food company observed acute renal failure in cats engaged in a routine palatability study, prompting the March 2007 voluntary recall of food produced by Canadian-based Menu Foods at plants in the USA. Primarily through the Internet, clinical and pathologic features of this apparently unique toxicosis were rapidly disseminated throughout the US veterinary community. By the end of March, melamine was identified in wheat gluten, a thickening agent primarily used in wet pet foods, supplied by Chinese manufacturers to Menu Foods and in tissues and urine from an affected cat. 4 Melamine was subsequently found in rice protein from a different source in China and, following an outbreak of renal failure in South Africa, in corn gluten in that country. Although it is impossible to determine how many animals died and how many will have chronic kidney disease associated with melamine/cyanuric acid toxicosis, the number of affected animals likely is in the thousands. A clinically similar outbreak of pet food–associated renal failure, affecting an estimated 6,000 dogs and involving a different pet food manufacturer, occurred in Asia in 2004. 11 Reexamination of tissues from these Asian dogs following the 2007 outbreak confirmed that they were also victims of melamine/cyanuric acid toxicosis. 2,24,33 More than 100 class action law suits were brought against Menu Foods, Inc., resulting in a $24 million settlement agreement to cover economic damages incurred by owners of affected pets. 22 Chinese authorities closed 2 companies linked to the contaminated vegetable proteins.
In 2008, an estimated 294,000 infants and children in China ingested milk-based formula tainted by melamine. Almost 53,000 children required hospitalization, and acute renal failure was reported in 2.5%. 1,9,32 The clinical disease in these children was described as nephrolithiasis. Complete clinical data in these cases are limited. In one report, affected children had been exposed to the tainted milk for 3–6 months before the onset of stones. 9 Another group of 34 children drinking contaminated formula for 15 days to 13 months developed uroliths, and all 34 children had acute renal failure requiring hospitalization. 31 Subsequent testing by the Chinese Administration of Quality Supervision, Inspection, and Quarantine revealed 22 brands of milk powder with detectable levels of melamine. 31 The Chinese government has arrested 60 people and 21 have been tried for actions related to the milk powder contamination. The chairwoman of the largest national distributor and exporter of milk powder, the San Lu Company, was sentenced to life in prison and 2 other individuals were executed. 6
Magnitude of the Problem
Question 1: Are We Fully Aware of the Magnitude of the Problem?
The outbreaks of DEG and melamine cyanurate poisoning share some characteristics. In particular, they both affected large populations of people or animals and caused clinically obvious disease and/or death.
During the DEG mass poisoning in Panama, a Panamanian citizen made the observation that the label on his 59¢ tube of toothpaste listed as an ingredient the same toxin responsible for the recent deaths in his country, DEG. 12 He reported his discovery, which resulted in a worldwide recall of toothpaste made in China and containing DEG. The Food and Drug Administration (FDA) warned US consumers to avoid using toothpaste labeled as made in China and issued an import alert to prevent DEG-containing toothpaste from entering the USA. 28 Although the FDA is not aware of any US reports of poisoning from toothpaste containing DEG, toothpaste from China has previously entered the US market. As the health impact of prolonged exposure to DEG in toothpaste is unknown, it is also unknown whether exposure has occurred.
Beginning in the latter part of 2002, the Minnesota Urolith Center began receiving canine stones with a unique appearance and an infrared spectrum that did not match any of the minerals in their database. 17 Some of these uroliths were sent for further evaluation to colleagues in Germany, and the uroliths were identified as uric acid monohydrate. Coincident with the outbreaks of melamine/cyanuric acid nephrotoxicity in dogs and cats, the center identified peaks of urolith submissions identified as uric acid monohydrate in 2003–2004 from dogs in Asia and in 2007 from dogs and cats in North America. These uroliths are now presumed to be melamine cyanurate crystals, suggesting that dogs were being poisoned in Asia as early as 2002. Similarly, a report from a human urolith laboratory in Germany identified 15 unusual uroliths submitted between 1990 and 1999; these stones were also identified via crystallographic techniques as uric acid monohydrate. 17,23 These human patients were between 45 and 83 years of age, 3 had passed multiple similar appearing stones, 11 of 15 stones were present in the kidney only, and azotemia was present in at least 5 of the patients. Given these findings, chronic exposure to melamine and cyanuric acid in these people is possible.
Lesson 1
Toxicoses from contaminated food and drugs are often identified only when large numbers of people or animals are affected, numerous deaths result, an unusual circumstance reveals the outbreak, or an astute individual recognizes the outbreak. Thus it is plausible that smaller outbreaks and contamination resulting in clinically mild disease have occurred and gone unrecognized.
Prevention of Outbreaks
Question 2: Do Regulatory Organizations Have the Capacity to Prevent Future Outbreaks?
Although outsourcing leads to lower prices for the consumer and increased profits for the producer, this practice introduces risks associated with the inability of regulators to closely monitor the raw materials, manufacturing processes, and distribution of less-well-regulated foreign products before they arrive at the port of entry. The increasingly complex responsibility for the oversight of these foreign drug firms and inspection and testing of imports in the USA is under the auspices of the US FDA. FDA officials are faced with large numbers of imports from countries with less stringent regulatory protection. Particularly problematic are deliberate attempts by foreign producers to adulterate or mislabel products to optimize monetary gain, putting human and animal health at risk. 32
Following the 2009 outbreak of acute renal failure in Panama associated with DEG-contaminated cough syrup, the FDA identified a series of problems common to the handling of contaminated materials in all of these recent outbreaks of DEG toxicosis. In all cases, the pharmaceutical manufacturers did not test for DEG, relying instead on the certificate of analysis (COA) provided by the supplier. In addition, the origin of the product was not easily apparent from the COA. 26 The FDA subsequently released an alert to pharmaceutical manufacturers, pharmacy compounders, repackers, and suppliers related to the potential health hazard of glycerin along with a series of 4 nonbinding recommendations designed to avoid future DEG poisoning. These recommendations were for drug product manufacturers to test all lots of glycerin for DEG, for manufacturers to “know their supply chain for glycerin” (the manufacturer and any subsequent distributors), for manufacturers and all their personnel to be aware of the importance of proper testing of glycerin, and for repackers or others who distribute and prepare glycerin for use in drug products to similarly test for DEG. Although absolute adherence to these guidelines will stop the introduction of contaminated glycerin into pharmaceutical products, the guidelines do not address means to prevent the deliberate contamination of glycerin with DEG in other products.
Subsequent to the 2007 melamine cyanurate contamination of pet food and animal feed, the FDA developed a risk assessment for melamine on human health. 25 This assessment evaluated the potential effects of consumption of meat, fish, or eggs from animals eating melamine-contaminated food. Although federal scientists correctly concluded that melamine contained in animal products poses “a very low risk to humans,” it is not clear whether regulatory agencies considered at that time whether the common practice of adding these nitrogen-rich compounds to falsely elevate protein content was also used in products intended for human consumption. It was not until after the widespread consumption of tainted powdered milk by infants in China that the potential for direct poisoning of the human food supply and the uncertainty associated with synergistic toxicity were recognized. In recognition of gaps in current knowledge and increased risk of toxicity in infants, the tolerable daily intake (TDI) for melamine or cyanuric acid ingested alone has been decreased. 29,31 The TDI for the combination of melamine and cyanuric acid has not yet been determined. In response to the infant poisonings in China, the FDA has announced the establishment of an office in Beijing that will examine food exports destined for the United States. 10,29
Lesson 2
Globalization has led to market forces and practices that might exceed regulatory capacities; regulatory responses are characteristically more reactive than proactive.
Product Testing
Question 3: How Readily Can Product Testing for Contaminants Be Used to Ensure Food Safety?
Melamine is an organic base commercially synthesized from urea. Melamine is 66% nitrogen by weight and is further processed to produce melamine resin, a very durable plastic, and melamine foam, a cleansing agent. Melamine has also been used in fertilizers and was tried, but proved to be ineffective, as a nonprotein nitrogen source in cattle feed. 9 The synthesis of melamine also results in the formation of other by-products (analogs), including cyanuric acid, ammeline, and ammelide. Depending on the purity of the melamine, these by-products may be present in different lots of melamine in widely varying amounts.
Melamine is not metabolized by animals and is rapidly eliminated in the urine, with greater than 90% eliminated within 24 hrs. 1 The acute median lethal dose (LD50) in rats has been reported as 3,400 mg/kg of body weight. 25 Subchronic and chronic melamine toxicity has been evaluated extensively in multiple species, including dogs, mice, and rats. 5 Diuresis but not renal toxicity was observed in dogs fed 3% (30,000 ppm or mg/kg) melamine in their diet for 1 year. 13 Although some dogs developed uroliths, intratubular crystals and renal failure were not described. Similarly, urolith formation was induced in rats, with the incidence of formation increasing with increased amounts of melamine from 750 ppm per day to greater than 15,000 ppm per day. 31 Although urethral obstruction occurred in some rats, intrarenal crystals were not detected and intrinsic renal failure did not occur. An increased incidence of transitional cell carcinoma associated with urolithiasis was also observed in male rats, but not female rats or mice, chronically given high doses (4500 ppm) of melamine. 15 Renal tissues from studies conducted by the National Toxicology Program in 1976–1983 were recently reevaluated. 8 In these studies, rats had been given up to 12,000 ppm of melamine daily for 13 weeks and up to 9,000 ppm melamine daily for 2 years. Rats given 6,000 ppm melamine for 13 weeks did not develop renal lesions, and rats given the highest concentration of melamine (12,000–18,000 ppm) had mild renal lesions of tubular dilation and increased tubular epithelial basophilia without renal failure. Rats fed 6,000 ppm melamine for 2 years had only mild renal scarring; these subchronic and chronic lesions were attributed to vesicoureteral reflux secondary to the urolithiasis.
Following the discovery of melamine in pet food, veterinary scientists were not convinced, given published toxicology studies, that melamine was responsible for the observed nephrotoxicity. Continued investigation revealed the presence of a critical second contaminant, cyanuric acid, both in contaminated pet foods and in renal tissues of fatally poisoned animals. 4 Cyanuric acid is practically nontoxic when administered as a single oral dose; the LD50 is greater than 10,000 mg/kg.
As recently as 2006, the FDA permitted cyanuric acid in nonprotein nitrogen additives used in animal feed. 27 Cyanuric acid is structurally related to melamine, and its chlorinated derivatives are used as disinfectants and algicides in outdoor swimming pools. 7 Like melamine, cyanuric acid is not metabolized and is excreted unchanged in the urine. When given in high concentrations in subacute and chronic toxicity studies, cyanuric acid causes diuresis and bladder calculi but no direct renal morphologic effects. 7 Suspecting synergistic toxicity, veterinary scientists tested the acute toxicity of melamine, cyanuric acid, and a combination of these chemicals in cats, fish, and pigs and quickly verified the nontoxic nature of these compounds alone and the highly nephrotoxic nature of the 2 chemicals together. 5,18,19 Cats given a single oral dose as low as 32 mg/kg of the combination of melamine and cyanuric acid required humane euthanasia 48 hours after dosing because of severe acute renal failure, 18 representing more than a 300-fold increase in toxicity compared with the LD50 for cyanuric acid (>10,000 mg/kg in rats) alone. The resultant intrinsic (ie, intrarenal) acute renal failure is attributed to the formation of histologically unique melamine cyanurate crystals within the renal distal tubules (Fig. 1), causing tubular obstruction and tubular epithelial cell injury. Ironically, this co-crystallization is the basis of a common turbidometric test to assess cyanuric acid content in swimming pool water using melamine as a coprecipitate.
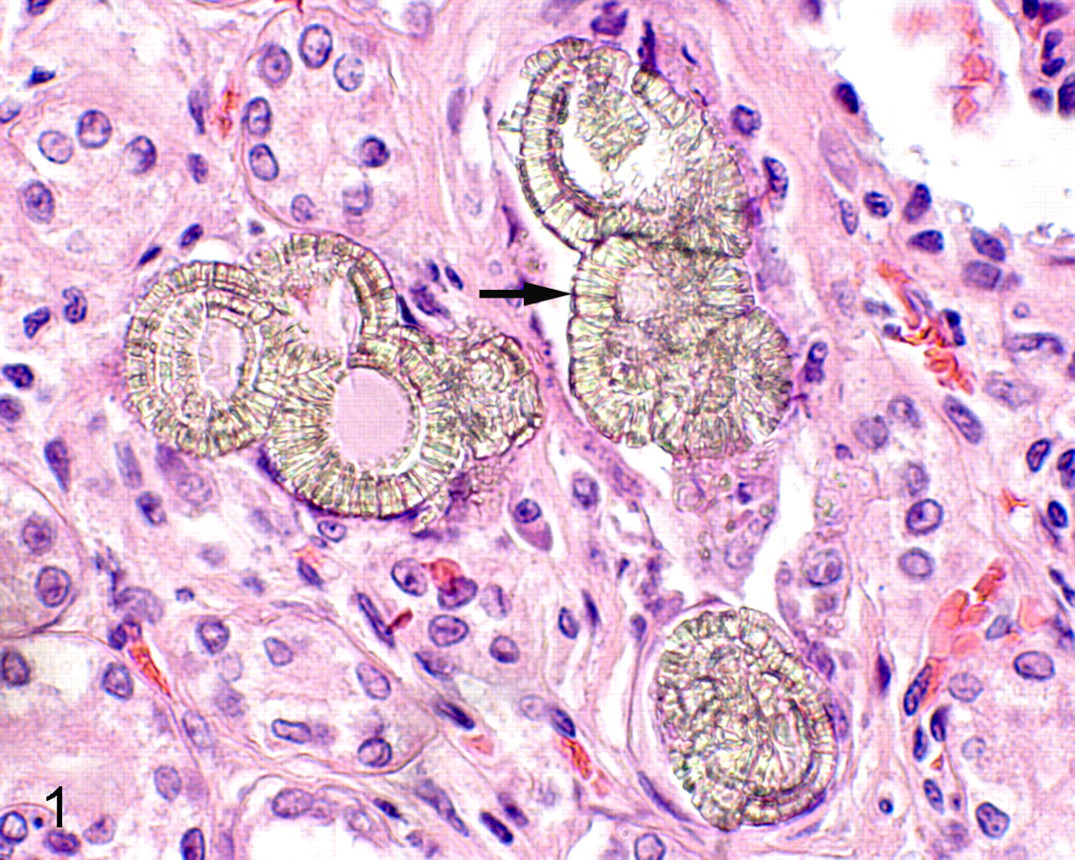
Kidney, dog. Characteristic intratubular melamine cyanurate crystals following the ingestion of melamine/cyanuric acid–contaminated pet food. Tubules are obstructed by these crystals, and there is associated epithelial cell necrosis (arrow). HE.
It is clear that wheat gluten in those pet foods causing nephrotoxicity in 2007 was contaminated with melamine and varying amounts of cyanuric acid and other melamine analogs. Measured concentrations of melamine and cyanuric acid in contaminated pet food scraps destined for swine or poultry feed ranged from 10.6 to 1,952 ppm and from 6.6 to 2180 ppm, respectively. 24 Similarly, analysis of raw material used to make infant formula revealed median levels of 188,000 ppm melamine and 3.2 ppm cyanuric acid. 30 In the case of melamine/cyanuric acid, it was not known until the 2007 investigation of the outbreak of toxic renal disease in pets that this synergistic toxicity even existed.
Lesson 3
Some toxicoses are complex, involving synergism among co-contaminants, each of which may be known to be present at “nontoxic” levels. Given the wide array of possible contaminants and myriad of potential interactions, testing is only part of the solution.
Contaminants in the Production Cycle
Question 4: How Do Contaminants Enter the Production Cycle?
DEG is a colorless, odorless sweet liquid found in commercial products such as resins, antifreeze, inks, and glues. 25 It is composed of 2 ethylene glycol moieties joined by an ester bond. Despite its long history as a human nephrotoxin, little is known about the pathophysiology of DEG toxicity. The toxicology of DEG is presumed to be similar to that of ethylene glycol toxicosis, a common cause of acute renal failure in dogs and cats. However, DEG is not metabolized into ethylene glycol, and it causes acute tubular necrosis without deposition of intratubular oxalates, which are plentiful in ethylene glycol intoxication. 6 The motivation for deliberate adulterations with DEG appears to be financial, given that DEG is an inexpensive vehicle that is more profitable to use than the more expensive propylene glycol or glycerin. 14 It is possible that this substitution occurs repeatedly, and clinical toxicity occurs only when DEG is present in high concentrations in the final product. As noted above, the renal effects of single or repeated exposure to lower doses of DEG remain to be determined.
It has become apparent that melamine was intentionally added for financial gains to vegetable proteins and infant milk powder produced in plants in China. Melamine is a cheap, readily available industrial nitrogen-containing product that falsely elevates apparent protein content as measured by current techniques, thereby increasing the monetary value of protein-based food ingredients to which it is added. There is compelling evidence that this practice of adding melamine to boost measured protein content is not new. The outbreak of renal failure in dogs that occurred 3 years prior to the 2007 outbreak was also the result of adulteration of pet food ingredients with melamine and cyanuric acid. It is unknown whether cyanuric acid was also deliberately added to boost protein content of vegetable proteins or whether it was a contaminant present in cruder preparations of melamine. It is likely that the adulteration of food with either of these compounds alone in pet foods would have gone undetected because of the relatively nontoxic nature of melamine. Financial gain coupled with the lack of sufficient regulation during the production of wheat gluten apparently led to the widespread practice of adding melamine to pet food to falsely boost protein content.
Lesson 4
Although some contamination may occur inadvertently, practices of deliberate contamination of food and drug ingredients may occur but escape detection in poorly regulated markets. If deliberate contamination is motivated by personal financial gain, it is likely to recur and be concealed.
Global Outbreaks
Question 5: Why Do Contaminants Lead to Global Outbreaks?
Trace-back investigations following the 2006 outbreak of DEG-induced renal failure in Panama found that imported raw material labeled as glycerin and used by the Panamanian pharmaceutical manufacturer in the formulation of the cough syrup contained 22.2% DEG. 20 Similarly, imported glycerin containing 24% DEG caused the 1995 outbreak of renal failure in Haiti. 16 In both cases, DEG-containing glycerin was imported from China via a European broker. In Panama, the contaminated glycerin was used in at least 1 other prescription liquid medication and in 2 topical creams, leading to the recall of more than 60,000 medications presumed to be contaminated by DEG and widespread screening for renal dysfunction in potentially exposed people. 21
Menu Foods, Inc., the primary pet food manufacturer linked to the 2007 melamine/cyanuric acid toxicosis, is a central producer of many brands of pet food, resulting in widespread contamination of the US pet food supply and the ultimate recall of more than 100 brands responsible for more than 1,000 potentially contaminated pet food products. Some of these recalled pet foods were sent as salvage feed to hog and chicken producers in several states in the USA, and melamine was detected in fish feed, prompting concern about the public health risk of eating contaminated meat, eggs, or fish. 25 Although this health risk was believed to be low, affected groups of animals were quarantined to prevent entrance of potentially contaminated products into the human food supply. Following the outbreak of melamine poisoning in children, the Chinese Administration of Quality Supervision, Inspection, and Quarantine revealed 22 brands of milk powder with detectable levels of melamine. Children outside of mainland China, in Taiwan, Hong Kong, and Macau, were also affected. 31 There were reports of melamine in foodstuffs from around the globe, and imports of Chinese-made infant formula and milk-based products such as cookies and chocolates were banned and/or recalled in 42 countries including the USA.
Lesson 5
Contaminated raw material produced in a poorly regulated market may cross national boundaries and be used in manufacturing processes for numerous products, sometimes in more well-regulated markets. Once in the production chain, contaminated raw materials may be widely disseminated.
Identification of Contaminants
Question 6: Why Were Melamine/Cyanuric Acid Nephrotoxicities Observed in Pets and Children and Not in the General Population?
It is possible that these 2 chemicals were present in the food chain as co-contaminants on only a few occasions. However, it is more likely that infants and pets were sentinel populations for a much more widespread occurrence. Although it is possible that higher uric acid excretion in infants compared with adults may increase their sensitivity to melamine toxicosis through the development of uric acid-melamine uroliths, this is not the case for pets. Milk-based formula intoxication in infants and children in China and melamine/cyanuric acid toxicity in dogs and cats are both examples of intoxications occurring in populations consuming diets composed primarily of a single food. Pet animals often ingest the same pet food as their complete diet. Likewise, formula often constitutes the majority of an infant’s diet. Chronic dietary exposure to contaminated food products places these unique groups at risk for cumulative intoxication and, unfortunately, makes them sentinel populations.
Lesson 6
Contaminations pose more risk in populations repeatedly exposed to a single product. As a corollary and reinforcing Lesson 1, it is possible that subclinical toxicity from contamination of food and drugs would be unappreciated in populations with heterogeneous exposure.
Interspecies Differences and Similarities
Question 7: Toxicoses Occurring in Animals and People From Melamine Ingestion Resulted in Somewhat Different Syndromes: Are These Examples of Interspecies Differences or Are There Similarities?
Superficially, the primary clinical manifestations of the syndrome caused by ingestion of melamine-contaminated milk in infants appear somewhat different from the clinical disease observed in poisoned dogs and cats in 2007. The primary effect reported in the infant formula incident was urolithiasis with acute renal failure reported in only 2.5% of infants. Surprisingly, although this toxicosis was severe enough to require tens of thousands of children to be hospitalized, only 6 deaths were reported. 6 In contrast, although melamine cyanurate stone formation occurred in some dogs, 17 this urolithiasis was overshadowed by severe, often fatal, renal failure observed in all clinically identified cases. This difference between the animal and human outbreaks has been explained by the participation of both melamine and cyanuric acid in the pet food toxicosis versus melamine alone in the infant formula poisoning. The ability of melamine alone to cause disease in human infants has also been explained as being due to increased urinary excretion of uric acid in humans compared with other species of animals. These melamine-related stones in affected children consist primarily of melamine and uric acid and are typically multiple, present in both kidneys, and usually less than 1 cm in diameter. These stones are fragile and soft and fortunately will often break up and pass if the patient is well hydrated. 6,9 The analyzed samples of infant formula were primarily contaminated with melamine. Although the infant powder appears to contain less cyanuric acid and more melamine compared with the pet food, the marked synergistic toxicity of melamine/cyanuric acid makes any co-contamination a significant health risk. The high melamine/cyanuric acid ratio in the infant formula may have led to a preponderance of melamine uroliths with a lower prevalence of melamine cyanurate crystals and acute renal failure. Unfortunately, given that renal histopathology has not been reported in any of these human cases, complete assessment of the role of melamine cyanurate in the infant formula outbreak is not possible.
Safety limits of chemicals for people have long been derived from results of toxicity studies in animals. Rather than showing differences, these outbreaks associated with melamine/cyanuric acid exposure emphasize the similarities across species. Physiologic similarities among different mammalian species outweigh the differences and allow extrapolation of data from animals to people and vice versa. In fact, a physician traveling to China to treat affected infants contacted veterinary pathologists and nephrologists familiar with melamine/cyanuric acid toxicosis in pets to develop potential treatment strategies for these children (personal observation, C. Brown and S. Brown).
Lesson 7
Human health and animal health are interrelated; to rapidly address global incidents, experts in animal and human health must be able to work effectively together.
Summary
Obtaining food and pharmaceutical ingredients from less-regulated countries provides economic benefits to both the exporting and importing countries and helps to foster positive international relationships. Unfortunately, along with these benefits is the cost associated with using raw materials that may not be safe. Preventing future subclinical or clinical mass poisoning requires cooperation between different regulatory agencies and with the scientific communities with improved regulation at the point-of-origin of raw materials being an important goal.
In Pursuit of Safety
Pharmaceutical contamination with DEG and food contamination with melamine/cyanuric acid have taught us important lessons about the effects of globalization on human and animal health. Critically, globalization has permitted contaminated materials to cross national boundaries with wide dissemination. The problem is important because it is possible that contaminations, inadvertent or deliberate, have gone unnoticed.
How should we proceed? It seems unlikely that limiting access to local markets will be viable in an increasingly global economy. Market forces have achieved some success in enhancing safety in poorly regulated markets but often only after loss of life. Where toxicants or dangerous practices are known, product testing has a vital role. For known contaminants, such as DEG and melamine, regulatory agencies should strive to eliminate the motivation for adulteration and to adopt testing methods that represent effective deterrents. In the case of melamine and cyanuric acid, true protein rather than total nitrogen determinations should be required. In at least a portion of the food industry (ie, the dairy industries in the USA, Australia, France, and Hungary), true protein measurements have replaced crude protein assays as the standard for determination of protein content. We must educate manufacturers on the importance of providing pure and safe product and the potential dire health consequences caused by any product adulteration.
Given the complexity of contaminant interactions, as seen with melamine/cyanuric acid, testing will at times rely on knowledge gained through incidents causing loss of life. An important step for regulatory agencies will be to develop more effective proactive approaches. Suppose someone posed the following question in 2007 after the pet food contamination with melamine/cyanuric acid had been fully characterized by veterinary scientists: “Since the quality of infant formula is dependent on protein content measured with the same assay as pet food wheat gluten protein content, I wonder whether there is melamine in infant formula?” That question should have been asked by Chinese regulatory authorities in 2007, resulting in proactive product testing the year before 53,000 children were hospitalized as a result of this deliberate and widespread practice.
The complex regulatory burden, national focus of regulatory agencies, rules of conduct, interference by financial motivations and market protectionism, and limited resources available to regulatory agencies are problematic. Some regulatory organizations do not have the capacity to identify all, or even most, contaminations despite their best efforts. Ironically, markets are global but regulation is primarily local. Provision of additional resources to national and international efforts with a renewed focus on coordinated international regulation must be pursued. Effective improvement in oversight of local production and education of producers is also critical.
Populations potentially at risk, such as infants and pets, should be identified and studied more thoroughly. The primary target organs for many toxicoses are the kidney, as in the examples here, and the liver. Clinicians and pathologists in the veterinary and medical community, in concert with regulatory agencies, could use shared registries of renal and hepatic disease of unknown cause to more effectively identify otherwise unappreciated toxicoses.
Footnotes
The authors declared that they had no conflicts of interests with respect to their authorship or the publication of this article.
The authors declared that they received no financial support for their research and/or authorship of this article.
