Abstract
Background
Knee osteoarthritis presents with posterior knee pain, stiffness, and restricted mobility, potentially affecting periarticular muscle biomechanics. We ultrasonographically assessed the gastrocnemius medialis properties in patients with knee osteoarthritis compared with those in healthy controls.
Methods
This study comprised 76 participants divided into symptomatic patients with knee osteoarthritis and gastrocnemius medialis involvement and healthy controls. Gastrocnemius medialis morphology (thickness and pennation angle) was evaluated using conventional ultrasound, whereas shear touch elastography was applied to assess tissue stiffness via elasticity (Gmean).
Results
Gastrocnemius medialis thickness was similar between the groups (p = 0.343); however, patients with knee osteoarthritis exhibited significantly smaller pennation angles (p < 0.001) and lower Gmean values (p = 0.009). Sex-stratified analysis revealed a reduced pennation angle in females (p = 0.003) and a smaller pennation angle (p = 0.036) and lower Gmean value (p = 0.013) in males with knee osteoarthritis.
Conclusion
Patients with knee osteoarthritis demonstrated significantly decreased gastrocnemius medialis pennation angles and Gmean values compared with those in controls, with sex-specific differences: males exhibited lower Gmean values, whereas females showed no difference. Gastrocnemius medialis ultrasonography may serve as an effective tool for detecting knee osteoarthritis-related biomechanical changes, supporting clinical assessment and rehabilitation planning.
Keywords
Introduction
Knee osteoarthritis (KOA) is a chronic degenerative joint disease characterized by articular cartilage deterioration, subchondral bone remodeling, and synovial inflammation. Clinically, it manifests as progressive joint pain, stiffness, swelling, reduced mobility, and eventual deformity, resulting in significant functional impairment and diminished quality of life.1–3 Although the precise etiology of KOA remains elusive, established risk factors include advanced age, female sex, genetic predisposition, prior joint injury, aberrant biomechanical loading, and obesity. 1 The disease pathogenesis involves a complex interplay between mechanical stress and low-grade inflammation, leading to structural alterations in the joint and periarticular musculature. 4
The gastrocnemius and quadriceps femoris (QF) muscles play essential roles in maintaining knee joint stability and absorbing mechanical load.5,6 Coactivation of gastrocnemius with other periarticular muscles increases tibiofemoral compressive forces, joint stiffness, and proprioception, thereby enhancing dynamic knee stability. 7 During gait, synergistic gastrocnemius–QF activation reduces medial knee joint laxity. 8 As a knee flexor, abnormal gastrocnemius activation may modulate knee adduction moments, altering periarticular soft tissue mechanics, a key factor in KOA pathogenesis. Notably, patients with KOA exhibit interlimb muscle asymmetry, which may further compromise biomechanical muscle properties. 9 Quantitative evaluation of the gastrocnemius medialis (GM) structural and functional alterations in KOA is thus crucial for improving diagnostic precision and guiding personalized therapeutic strategies.
Current clinical assessment of musculoskeletal (MSK) changes in osteoarthritis combines direct and indirect methods, including pain scales, functional evaluations, dynamometry, goniometry, and advanced imaging. 10 Although radiography and magnetic resonance imaging (MRI) remain the most widely used imaging modalities, each has significant limitations. Radiography offers limited soft tissue resolution and involves ionizing radiation, whereas MRI, despite its excellent soft tissue contrast, is costly, time-intensive, and subject to contraindications.
MSK ultrasound (MSK-US) offers distinct advantages by enabling real-time, high-resolution visualization of muscle architecture (thickness and pennation angle), tendon integrity, synovial pathology, and cartilage morphology in patients with KOA. Crucially, these structural parameters, particularly muscle thickness, pennation angle, and elasticity, correlate strongly with muscle function and serve as reliable quantitative indicators of muscle biomechanical properties. 11
Conventional B-mode US accurately quantifies morphometric parameters, such as thickness and pennation angle, whereas shear wave elastography (SWE) provides a complementary functional assessment through quantitative stiffness measurements.12,13 Notably, shear touch elastography (STE) represents a relatively new SWE technique. Shear modulus (G), a measurement index of STE, is considered a reliable biomechanical index that reflects soft tissue stiffness.14,15
Patients with KOA demonstrate significant alterations in periarticular muscle architecture, including reduced thickness of the rectus femoris (RF), vastus lateralis (VL), vastus medialis (VM), and peroneus longus (PL) muscles,16–18 along with modified elastic properties of the hamstrings, 19 QF, and patellar tendon. 20 However, the impact of KOA on gastrocnemius muscle morphology (thickness and pennation angle) and biomechanical properties (elasticity) remains poorly characterized.
This study employed conventional ultrasonography combined with STE to quantitatively assess GM thickness, pennation angle, and G in patients with KOA and healthy controls. By systematically comparing these ultrasonographic parameters, we aimed to elucidate GM-specific degenerative changes in KOA and inform clinical decision-making and early therapeutic interventions.
Data and methods
Participants
We conducted a prospective cross-sectional study with consecutive enrollment of 46 patients diagnosed with KOA from our orthopedic department, including 18 unilateral and 28 bilateral cases. The medial gastrocnemius muscles of the symptomatic limbs were designated as Group 1. Thirty age- and sex-matched healthy volunteers served as the control group (Group 2).
The diagnostic criteria for KOA in this study were based on the “2023 Guidelines for Integrated Traditional Chinese and Western Medicine in the Diagnosis and Treatment of Knee Osteoarthritis,”
21
with specific criteria outlined as follows:
Recurrent pain in the knee joint within the past month; Age ≥ 50 years; Morning stiffness lasting ≤30 min; Presence of crepitus during knee movement; X-ray findings (in standing or weight-bearing positions) characterized by joint space narrowing, subchondral bone sclerosis, cystic changes, and osteophyte formation at the joint margins; MRI results indicative of cartilage injury, osteophyte formation, subchondral bone marrow edema, cystic changes, degenerative tears of the meniscus, and partial or full-thickness cartilage loss.
Patients meeting criteria (a), (b), (c), and (d); (a) and (e); or (a) and (f) can be diagnosed with KOA.
The exclusion criteria for patients with KOA were as follows:
Accompanying neurological disorders, such as stroke,
22
spinal-related diseases, vertigo, or Parkinson disease; History of significant trauma, surgery, or deformities in the lower limbs; Use of any medications that may affect muscle and tendon tension, stiffness, and other characteristics (statins, sulfonylureas, glucose‐lowering drugs, antineoplastic drugs, and immune checkpoint inhibitors); Participation in vigorous exercise within 48 h prior to the trial; Presence of other types of inflammatory arthritis.
The control group consisted of healthy participants without knee osteoarthritis. These participants were selected based on medical history review and physical examination. The exclusion criteria for the control group were as follows: (a) presence of other osteoarthritis diseases and (b) a history of significant lower limb surgery, other arthritic conditions, leg pain, or neurological disorders affecting lower limb activity.
This study was a case–control study, and prior to the commencement of the research, thorough explanations of the experimental procedures were provided to each participant. Written informed consent was obtained from all participants, and all research procedures were conducted in accordance with the principles outlined in the Declaration of Helsinki.
All participant identifiers were removed from the dataset to ensure complete anonymity. The analyzed data contained no information that could potentially identify individual participants.
The reporting of this study conforms to the Strengthening the Reporting of Observational studies in Epidemiology (STROBE) guidelines. 23
Data acquisition with B-mode US and STE
Ultrasound assessments were performed using a Mindray Resona 7 s diagnostic system (Mindray, China) equipped with STE and an L3-9U high-frequency linear transducer. To minimize potential exercise-related confounders, participants were instructed to abstain from strenuous physical activity for at least 24 h prior to scanning.
During the examination, participants were positioned in the prone position with their legs fully extended and slightly overhanging the edge of the examination table. The standardization of the joint range of motion was crucial, as it has been shown to influence measurement results. 22 To ensure consistent limb alignment, the knees were maintained in full extension, the ankles were stabilized in a neutral position with a brace, and the ankle joints were held at approximately 90°. For ultrasonographic imaging of the gastrocnemius muscle, the transducer was aligned parallel to the muscle fascicles and perpendicular to the skin surface to enhance reproducibility and minimize the risk of oblique sampling of the muscle fibers. 16 Two types of US measurements were performed. First, B-mode imaging was performed to assess the morphology of the GM at 30% of the proximal distance from the popliteal crease. The imaging depth was set to 3–4 cm, and scans were acquired in the longitudinal plane. Muscle thickness was defined as the distance between the superficial and deep aponeuroses, 16 whereas the pennation angle was measured as the angle of insertion of the muscle fibers into the deep aponeurosis. Second, muscle elasticity was assessed using STE. A region of interest (ROI), measuring 3.5 × 2.5 cm (system default), was positioned within the muscle, and the diameter of the Q-box was adjusted to correspond with the muscle thickness. The Gmean value was automatically calculated by the system within the Q-box. As illustrated in Figure 1(a), the median of three measurements from each site was used for the analysis. Data from bilateral gastrocnemii were averaged to represent each participant. Schematic diagrams illustrating GM thickness, pennation angle, and Gmean values in patients with KOA and healthy adults are presented in Figure 1(b) to (g). Given the established excellent intra and interevaluator reliability of US elastography for measuring calf muscle G in KOA, all scans were performed by a single primary operator (HZ). 24 This operator had 5 years of experience in MSK-US and was supervised by a senior examiner (QW) with 10 years of experience.
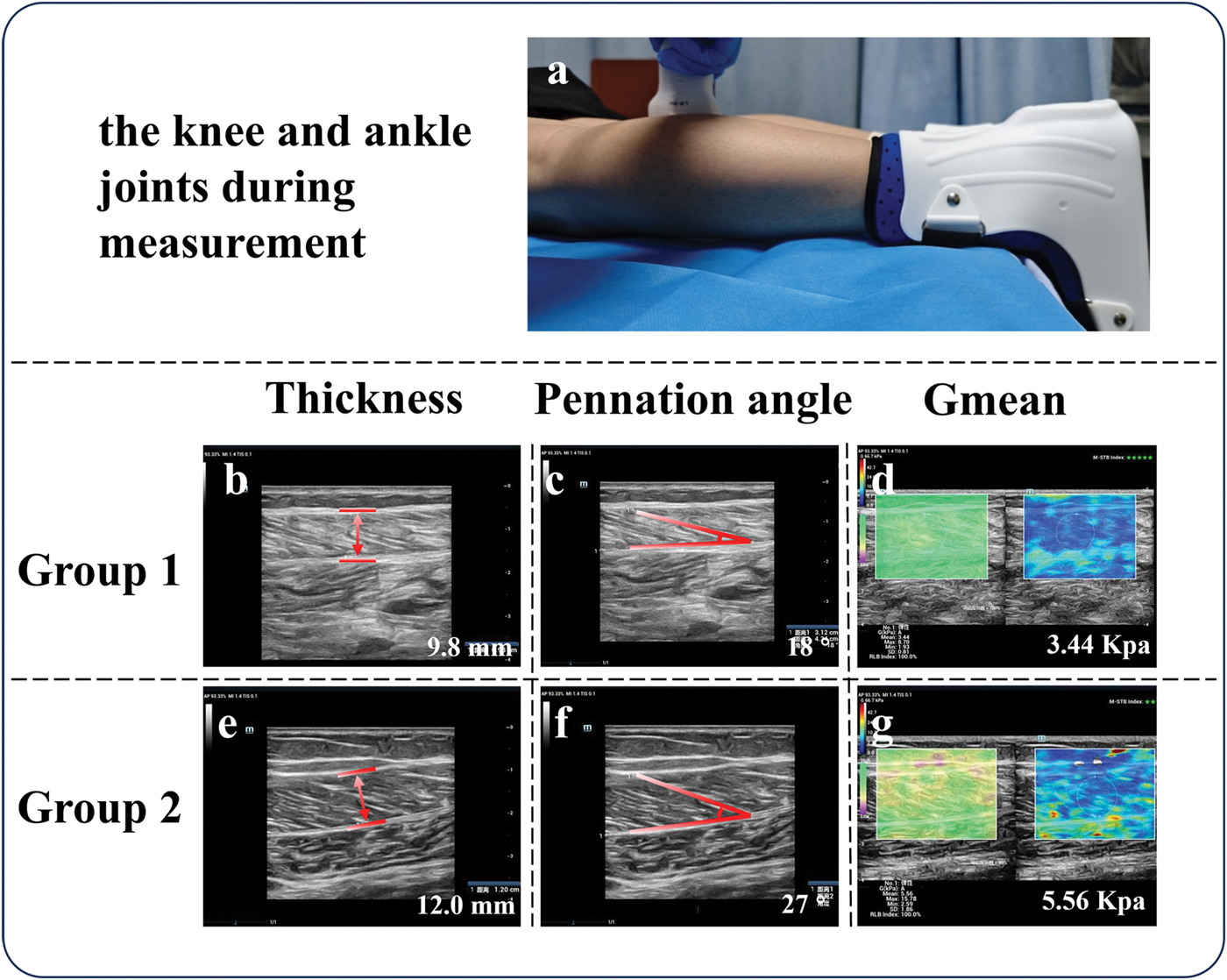
(a) Schematic diagram of the knee and ankle joints angles during measurement. (b–d) Schematic representations of GM thickness, pennation angle, and Gmean in the symptomatic side and (e–g) healthy adult participants. GM: gastrocnemius medialis.
Statistical analysis
All statistical analyses were conducted using IBM Statistical Package for Social Sciences (SPSS) Statistics for Windows, version 22.0 (released 2013, IBM Corp.; Armonk, NY, USA). Continuous variables, including age, body mass index (BMI), disease duration, GM thickness, pennation angle, and G, were assessed for normality using the Shapiro–Wilk test. Normally distributed data were presented as mean ±SD, whereas non-normally distributed data were expressed as median with interquartile range (IQR). Between-group comparisons were performed using parametric tests (independent t-tests) for normally distributed data and nonparametric tests (Mann–Whitney U test) for data that did not meet normality assumptions. Pearson correlation analysis was used to assess the correlations between US parameters of the symptomatic KOA side and Kellgren–Lawrence (K–L, class 0–4) classification system. The statistical threshold levels of correlation used for interpretation were defined as follows: ≤0.29, no correlation; 0.30–0.49, weak correlation; 0.50–0.79, moderate correlation; and >0.8, strong correlation. A p value of <0.05 was considered statistically significant.
Results
Participant characteristics
As presented in Table 1, participants in the KOA group demonstrated significantly higher BMI values than those in the control group (p = 0.012). No other baseline characteristics demonstrated statistically significant intergroup differences (all p > 0.05), indicating comparable demographic profiles apart from BMI.
Characteristics of participants [
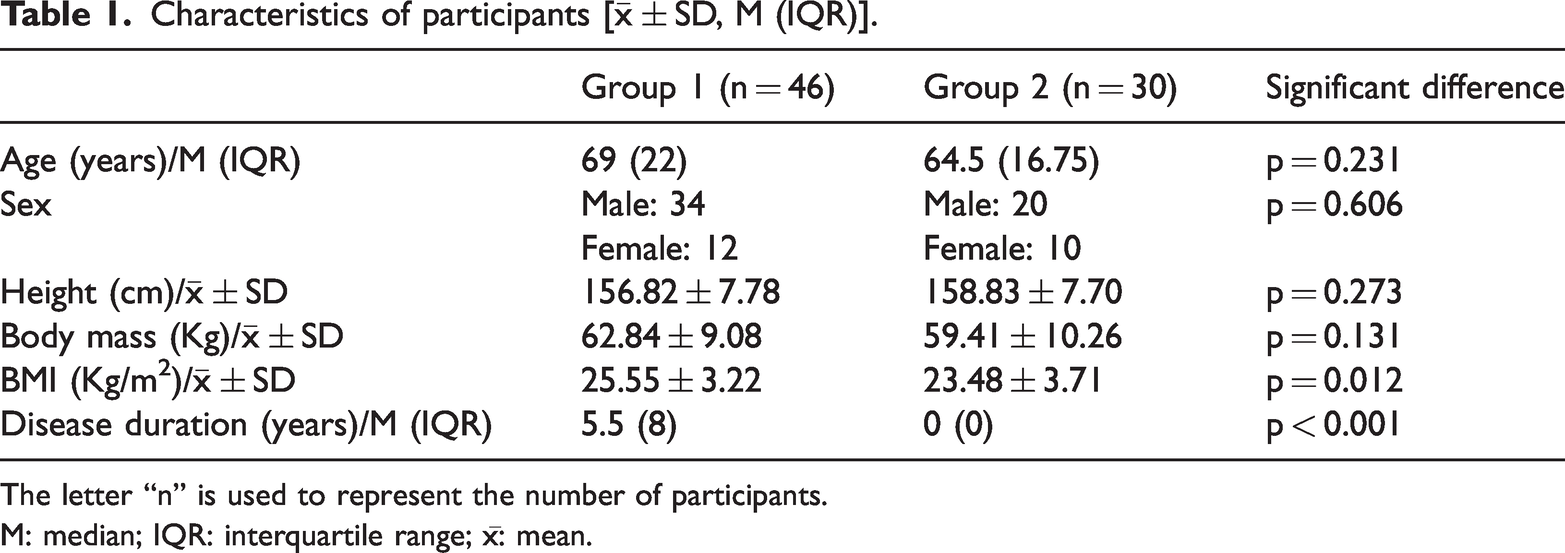
The letter “n” is used to represent the number of participants.
M: median; IQR: interquartile range; x̄: mean.
Comparative analysis of GM ultrasonographic parameters
Although GM muscle thickness did not differ significantly between the KOA group and control group (p = 0.343), two key parameters exhibited statistically significant reductions in the KOA group, as presented in Table 2 and Figure 2.
Data on the thickness, pennation angle, and Gmean of GM [
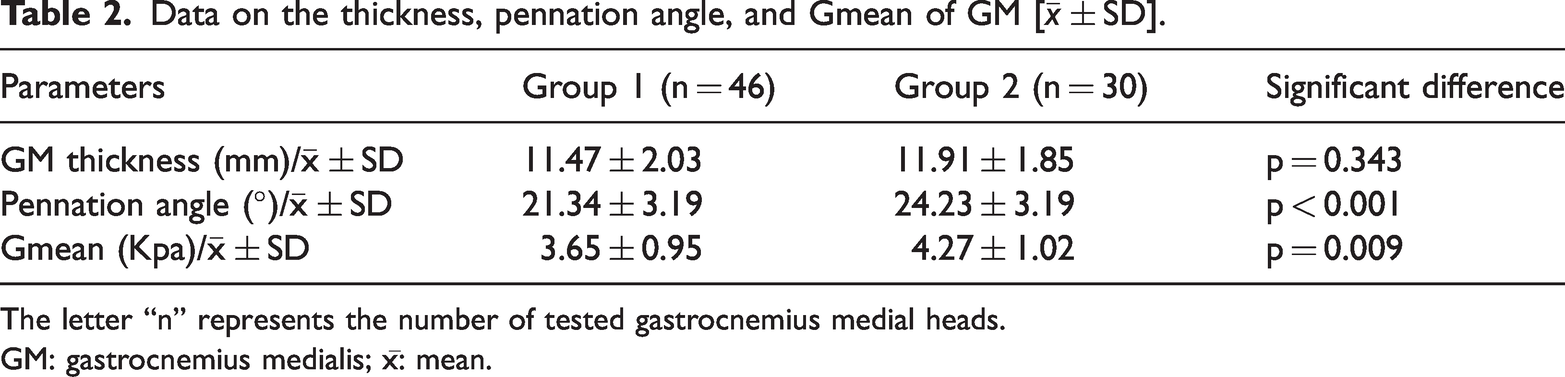
The letter “n” represents the number of tested gastrocnemius medial heads.
GM: gastrocnemius medialis; x̄: mean.
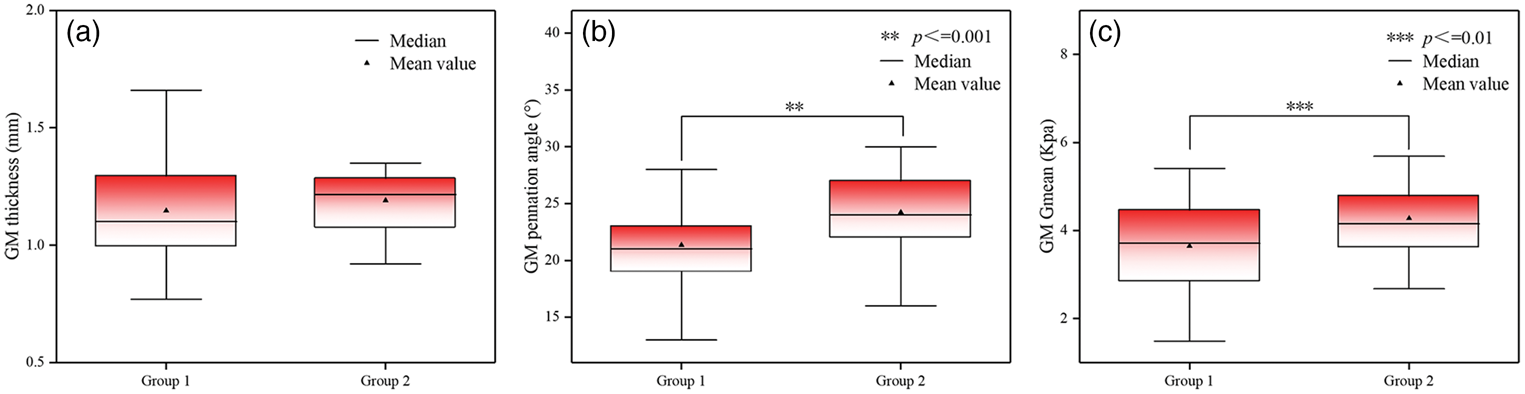
(a) Thickness, (b) pennation angle, and (c) Gmean of GM. GM: gastrocnemius medialis.
First, the pennation angle was significantly lower in participants with KOA than in healthy controls, representing an 11.9% decrease (p < 0.001). Second, the Gmean value was also lower in the KOA group than in the control group, corresponding to a 14.5% reduction (p = 0.009). These findings indicate measurable structural and mechanical impairments in GM of patients with KOA, potentially contributing to altered functional capacity.
Sex-specific differences in GM ultrasonographic parameters
Sex-stratified analyses further revealed distinct patterns of muscle alterations in male and female participants with KOA. As detailed in Table 3, among female participants, no significant difference in GM thickness was observed between the KOA and control groups (p = 0.872). However, a significant reduction in pennation angle was noted in the KOA group (p = 0.003), whereas the Gmean values did not differ significantly between the groups (p = 0.356).
The differences in ultrasound parameters between different genders within each of the two groups [

The term “ni” represents the number of tested gastrocnemius medial heads.
GM: gastrocnemius medialis; M: median; IQR: interquartile range; x̄: mean.
In male participants, GM thickness remained comparable between the KOA and control groups (p = 0.489). Nevertheless, a significantly lower pennation angle was observed in the KOA group (p = 0.036), along with a marked reduction in Gmean values (p = 0.013).
Sex differences in ultrasonographic parameters
Within the KOA group, no significant sex-related differences were observed in any of the assessed US parameters, including GM thickness, pennation angle, and Gmean values (all p > 0.05). In contrast, as detailed in Table 4, among healthy controls, males exhibited significantly higher Gmean values (p = 0.005) than females. No significant sex-related difference in pennation angle and GM thickness was detected in the control group (p > 0.05).
Differences in ultrasound parameters among sex by groups [

GM: gastrocnemius medialis; M: median; IQR: interquartile range; x̄: mean.
Differences in US parameters of gastrocnemius muscle between patients with unilateral and bilateral KOA
No significant differences were observed in GM thickness, pennation angle, or Gmean values between the affected sides of unilateral and bilateral KOA patients (all p > 0.05; Table 5).
Comparison of ultrasound parameters in the gastrocnemius muscle between affected sides of unilateral and bilateral knee osteoarthritis patients [

GM: gastrocnemius medialis; x̄: mean.
Correlation of GM thickness, pinnation angle, and Gmean values on the symptomatic side of KOA with the K–L classification of patients
A total of 74 GMs were evaluated on the symptomatic side, including 3 GMs at K–L Grade 2, 7 GMs at K–L Grade 3, and 64 GMs at K–L Grade 4. Pearson correlation analysis revealed no significant linear correlation between GM thickness, pinnation angle, and Gmean values on the symptomatic side of KOA (rthickness = −0.153, p = 0.193; rPennation angle = 0.065, p = 0.582; rGmean = −0.017, p = 0.884).
Discussion
To the best of our knowledge, this is the first study to comparatively assess the gastrocnemius muscle between patients with KOA and healthy volunteers utilizing Mindray STE technology. According to Jain et al., 25 knee joint US and hamstring SWE are not only valuable screening modalities for KOA but also aid in developing personalized rehabilitation and management plans. This study builds upon established evidence supporting US17,18 and SWE16,20,24 for assessing lower limb musculature in KOA by demonstrating significant alterations in GM architecture and biomechanical properties. Although GM thickness remained comparable between KOA patients and healthy controls, we observed substantial reductions in pennation angles and G, suggesting that these parameters may enhance the detection of KOA-related muscle deterioration (loss of strength and stiffness) when incorporated into routine US assessments. Notably, the sex-stratified analysis revealed distinct biomechanical changes: male patients with KOA exhibited significant reductions in pennation angle and elasticity, whereas female patients exhibited only angular changes with preserved tissue stiffness, potentially reflecting sex-specific biomechanical adaptations or hormonal influences. These findings provide the first comprehensive characterization of GM alterations in KOA using combined conventional US and STE, offering valuable insights for developing targeted rehabilitation strategies and underscoring the importance of sex-specific approaches in KOA management. Future longitudinal studies are warranted to explore the temporal relationship between these US parameters and functional decline.
Extensive research has documented reduced thickness of periarticular muscles (VM, VL, and PL) in patients with KOA compared with those in healthy controls.16–18 Although these studies consistently report muscle atrophy in quadriceps components (VL, VM, and VI) and PL among KOA populations,16–18 our findings demonstrate a distinct preservation pattern in the GM, with no statistically significant reduction in thickness. However, this observation may be attributable to the limited sample size. Importantly, our study is the first to demonstrate the absence of significant sex-related differences in GM thickness among patients with KOA. These findings carry significant clinical implications. Reliance solely on muscle thickness may be insufficient for a comprehensive biomechanical assessment of KOA and may underestimate the extent of muscle involvement. Although past studies have correlated muscle atrophy with disease severity 17 and age, 18 our inclusion of patients across the disease spectrum may have influenced these observations, a limitation warranting future stratified investigations. Nevertheless, these results emphasize the need for muscle-specific, multidimensional assessment approaches in the management and rehabilitation planning of KOA.
Our study identified a clinically significant 12% reduction in GM pennation angle among patients with KOA compared with that in healthy controls. This finding has important functional implications, as the pennation angle directly correlates with muscle force-generation capacity. 26 Larger angles permit greater packing of contractile elements within a given muscle volume, thereby enhancing force production potential. 27 The observed architectural changes align with established patterns of muscle degeneration, wherein atrophy typically results in decreased pennation angles. 28 This finding suggests that muscle strength is significantly reduced in patients with KOA compared with that in healthy volunteers. Notably, our sex-stratified analysis revealed consistent reductions across both genders, aligning with findings from studies on other periarticular muscles in KOA populations.16,29 These results demonstrate the following. (1) GM architectural changes follow pathological patterns similar to quadriceps alterations in KOA.16,27 (2) The observed angular reductions represent functionally detrimental modifications likely impairing force-generation capacity. (3) These changes occur independently of the individual’s sex. The robust consistency of these findings across multiple muscle groups and studies16,26–29 strongly supports incorporating pennation angle measurements into clinical assessments and underscores the therapeutic importance of targeted lower limb strengthening regimens in KOA management.
Our study revealed a 14% reduction in Gmean values of GM in patients with KOA compared with that in healthy controls, as illustrated in Figure 2. These findings align with established patterns of skeletal muscle pathology, where decreased tissue stiffness and reduced shear wave velocity are recognized as characteristic features.30,31 The observed elasticity changes may reflect multiple pathological mechanisms. (1) Chronic low-grade inflammation in KOA alters tissue composition and increases water content, potentially reducing muscle stiffness. (2) Disease-related biomechanical adaptations result in differential changes in periarticular musculature. Notably, previous studies have reported seemingly contradictory findings, with increased stiffness in distal muscles such as the hamstrings 19 and decreased elasticity in proximal structures (QF and patellar tendon). 20 This spatial variation suggests a compensatory mechanism whereby muscles located closer to the affected joint (e.g. QF and patellar tendon) undergo atrophy and stiffness reduction, whereas more distal muscles (e.g. hamstrings) demonstrate increased stiffness due to altered movement patterns. These results highlight the complex, location-dependent nature of muscular adaptations in KOA and emphasize the importance of muscle-specific evaluation in clinical assessment and rehabilitation planning.
Our study identified distinct sex-specific patterns in GM elasticity among patients with KOA, showing notable differences from previous literature. Although we found no significant difference in GM Gmean values between healthy women and female patients with KOA, this finding contrasts with that reported by Wang et al., 32 who reported significantly lower Gmean values in healthy women than symptomatic and asymptomatic sides in patients with KOA. This discrepancy may stem from variations in sample characteristics (age and BMI distributions), disease severity, or measurement protocols. In this study, female patients with KOA demonstrated significantly higher age and BMI values than those reported by Wang et al. 32 In clinical practice, relying solely on tissue stiffness to assess muscle pathology in older patients with KOA with elevated BMI may result in misjudgment. Importantly, our male cohort demonstrated a marked 20% reduction in Gmean values on the symptomatic side compared with those in healthy controls, consistent with established patterns of muscle degeneration in osteoarthritis and indicative of greater mechanical alterations in male patients. These findings collectively underscore the importance of sex-stratified analysis in KOA research, reveal potential biological differences in disease progression between genders, and highlight the need for standardized elastography protocols and larger-scale studies to clarify these relationships, ultimately providing new insights into the complex, sex-dependent muscular changes characteristic of osteoarthritis pathophysiology.
Limitations
This study has several limitations that should be acknowledged. First, the relatively small sample size may limit the generalizability of our findings. Future investigations should include larger cohorts. Second, the single-center design and lack of interobserver reliability testing may affect the external validity of our results. Although all measurements were performed by an experienced sonographer (5 years of MSK-US experience) under senior supervision (10 years of experience), future multicenter studies should include interrater reliability assessments to confirm the reproducibility of these US protocols across different operators and clinical settings. Such methodological refinements would enhance the clinical applicability of our findings and facilitate their translation into standardized assessment protocols for KOA management.
Conclusion
This study demonstrates that KOA is associated with significant alterations in GM architecture and biomechanical properties, characterized by reduced pennation angles and lower G values compared with those in healthy controls. The sex-stratified analysis revealed important differences: male patients with KOA exhibited significant reductions in both parameters, whereas female patients exhibited only angular changes with preserved tissue elasticity. Although preliminary, these results support the incorporation of ultrasonographic muscle assessment in the evaluation and management of KOA, particularly for guiding personalized rehabilitation strategies.
Footnotes
Acknowledgments
The authors have no acknowledgments to disclose.
Contribution statement
Hui Zuo: Writing–original draft. Ting Xu: Investigation. Qianwen Wang: Formal analysis. Wei Tan: Data curation. Xu Liu: Writing–review & editing.
Data availability statement
Not applicable.
Declaration of competing interest
The authors declare that they have no known competing financial interests or personal relationships that could have appeared to influence the work reported in this paper.
Ethical statement
Approval of this study was obtained from the Ethics Committee of Sichuan Provincial Orthopedic Hospital (Approval No. KY2024-043-01).
Funding
The author(s) received no financial support for the research.
