Abstract
Objective:
To evaluate the effects of alcohol consumption and cigarette smoking on sperm quality using transmission electron microscopy and light microscopy.
Methods:
Semen samples were collected from 62 healthy men. The subjects were classified according to alcohol consumption and smoking status. Semen analysis was performed according to World Health Organization criteria. Transmission electron microscopy was used to examine sperm ultrastructure.
Results:
Heavy smoking (> 20 cigarettes/day) was associated with a decreased sperm count. Moderate/high alcohol consumption (≥15.4 g/day) was associated with an increase in morphologically abnormal sperm. Transmission electron microscopy revealed no effect of smoking on sperm ultrastructure. Alcohol consumption resulted in significant increases in morphologically abnormal nuclei and plasma membranes.
Conclusions:
Heavy smoking was associated with decreased sperm counts and alcohol consumption was associated with increased numbers of morphologically abnormal sperm.
Introduction
Cigarette smoking is a widely recognised health hazard and a major cause of mortality, yet ∼20% of the worldwide adult population are smokers. 1 Alcohol abuse is also a major health issue and is responsible for 2.5 million deaths worldwide each year. 2 Smoking and alcohol consumption are frequently associated with impaired male reproductive function.3,4
Studies have examined the effects of tobacco smoking and alcohol consumption on human seminal quality.3–5 It is likely that smoking adversely affects male reproductive health.3,5,6 Although chronic heavy alcohol consumption has been associated with abnormal sperm morphology,4,7 studies regarding the relationship between moderate alcohol consumption and sperm morphology have yielded conflicting results.3,6
The objective of the present study was to evaluate the effects of alcohol consumption and cigarette smoking on the sperm quality of healthy, randomly selected men, using transmission electron microscopy and light microscopy.
Patients and methods
Study Population
Men aged ≥ 20 years, who were attending Chung-Ang University College of Medicine, Seoul, Republic of Korea for routine medical screening in January 2005, were randomly recruited to the study via a computer generated random number scheme. Exclusion criteria were: (i) previous disease or surgery associated with reproductive function (including varicocele, cryptorchidism, epididymitis, mumps, azoospermia); vasectomy and vasectomy reversal; (ii) occupational chemical exposure; (iii) chronic renal failure, diabetes mellitus, hypertension or tuberculosis; (iv) history of excessive testicular heat injury. Participants were questioned regarding their careers, alcohol consumption, smoking habits, and medical and family histories.
The study was approved by the Ethics Committee and Institutional Review Boards of Chung-Ang University. Written informed consent was obtained from all subjects prior to enrolment.
Study Groups
Subjects were initially stratified into four groups according to smoking status and alcohol consumption quartiles, with low alcohol intake classified as < 15.4 g/day and high intake as ≥ 15.4 g/day: nonsmokers with low alcohol intake (NL); nonsmokers with high alcohol intake (NH); smokers with low alcohol intake (SL); smokers with high alcohol intake (SH).
Subjects were further stratified according to the number of cigarettes smoked per day: 0, nonsmokers; 1 – 20, smokers; > 20, heavy smokers. In addition, the study population was divided into quartile groups according to alcohol consumption: very low (< 6.4 g/day); low (≥ 6.4 – < 15.4 g/day); moderate (≥ 15.4 – < 33.3 g/day); high (≥ 33.3 g/day).
Semen Analysis
Semen samples were collected into a sterile cup by masturbation in a comfortable room with audiovisual sexual stimuli, after 3 – 5 days abstinence. Samples were allowed to liquefy for 30 min, after which semen appearance, liquefaction, viscosity, volume and pH were assessed according to World Health Organization (WHO) procedures. 8 Samples were examined via light microscopy and sperm count was determined using a haemocytometer. Motility was assessed using the sperm progression rating: A, rapid forward progressive motility; B, slow or sluggish progressive motility; C, nonprogressive motility; D, immotility. Motility was defined as normal when ≥ 50% of sperm were classified as grade A + B, or ≥ 25% were grade A. 8 Sperm morphology was assessed using WHO criteria, 9 and expressed as (morphologically normal sperm cells/total sperm cells) × 100%. All examinations were performed by a single specialist investigator (Y.W.K.) who was blinded to smoking/alcohol consumption status.
Transmission Electron Microscopy
Semen samples were transferred to a 15-ml polyethylene centrifuge tube and combined with 2.5% gluteraldehyde (0.1 M phosphate buffered saline, pH 7.4, 4 °C). The tube was capped and repeatedly inverted until thoroughly mixed. After fixation overnight at 4 °C, the specimen was centrifuged at 500
Statistical Analyses
Data were presented as mean ± SD. Sperm count data were highly skewed and were therefore log-transformed before statistical analysis. Between-group comparisons were performed using one-way analysis of variance and Scheffé's post hoc test. Statistical analyses were carried out with STATA® software, version 10.0 (StataCorp LP, College Station, TX, USA). A P-value < 0.05 was considered statistically significant.
Results
The study included 62 participants (mean age 37.9 ± 2.0 years, range 34 – 44 years). Demographic and basic semen characteristics stratified according to smoking status and alcohol consumption are shown in Table 1. There were no statistically significant between-group differences in age or proportion of morphologically normal sperm. Semen volume, sperm count and sperm motility were lower in smokers than in nonsmokers, but these differences were not statistically significant. Representative transmission electron photomicrographs of normal sperm (from a nonsmoker with a low alcohol intake) and abnormal sperm (from a smoker with a high alcohol intake) are shown in Figs 1 and 2, respectively.
Representative transmission electron photomicrographs of sperm from a 36-year-old nonsmoker with a low alcohol consumption (< 15.4 g/day). (A) Longitudinal section of the head region (acrosome and nucleus) showing no cytoplasmic residue. Scale bar, 3 μm. (B) Longitudinal section of the midpiece head region showing regular shape and helical mitochondrial assembly. Scale bar, 3 μm. (C) Cross section of tail, indicating the structure of the axoneme (nine pairs of filaments arranged radially around two central filaments [9 + 2 arrangement]). Scale bar, 0.1 μm. (D) The axonemal microtubule system is surrounded by nine accessory fibres. The outer fibrous sheath is a normal shape. Scale bar, 0.1 μm Representative transmission electron photomicrographs of sperm from a 39-year-old smoker with a high alcohol consumption (≥ 15.4 g/day). (A) The head region shows acrosomal hypoplasia, uncondensed chromatin and an irregularly shaped nucleus. Scale bar, 3 μm. (B) Cytoplasmic residue in the midpiece. Scale bar, 3 μm. (C) The shape and helical mitochondrial assembly are irregular and swollen. Scale bar, 3 μm (D) The axoneme is composed of nine pairs of filaments, with the central pair of filaments absent (9 + 0 arrangement). Scale bar, 0.1 μm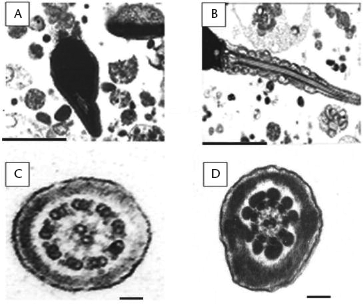

Demographic and semen characteristics of healthy men, stratified according to smoking status and alcohol consumption (n = 62)

Data presented as mean ± SD.
Alcohol intake < 15.4 g/day.
Alcohol intake ≥ 15.4 g/day.
Grade A or B. 8
(Morphologically normal sperm cells/total sperm cells) × 100%. 9
No statistically significant between-group differences (P ≥ 0.05; one way analysis of variance).
Table 2 shows data regarding semen volume and sperm count, motility and morphology stratified according to the number of cigarettes smoked or the quantity of alcohol consumed. The mean sperm count was significantly lower in heavy smokers than in smokers, and the proportion of morphologically normal sperm cells was significantly lower in those with high alcohol consumption compared with those with moderate alcohol consumption (P < 0.05 for both comparisons; Table 2).
Semen quality parameters assessed by light microscopy in semen from healthy men, stratified according to the number of cigarettes smoked or the quantity of alcohol consumed (n = 62)

Data presented as mean ± SD.
Nonsmoker, 0 cigarettes/day; smoker, 1 - 20 cigarettes/day; heavy smoker > 20 cigarettes/day.
Very low, < 6.4 g/day; low, ≥ 6.4 - < 15.4 g/day; moderate, ≥ 15.4 - < 33 g/day; high, ≥ 33 g/day.
P < 0.05 vs smokers; one way analysis of variance and Scheffé's post hoc test.
P < 0.05 vs moderate; one way analysis of variance and Scheffé's post hoc test.
Data regarding ultrastructural characteristics of sperm stratified according to smoking or alcohol consumption are shown in Table 3. Smoking was not associated with any differences in ultrastructural characteristics. Moderate and high alcohol consumption were associated with significantly fewer normally shaped nuclei than very low alcohol consumption (P < 0.05 for both comparisons; Table 3). In addition, significantly fewer sperm cells in the low alcohol consumption group were found to have normal plasma membranes than in the very low alcohol group (P < 0.05; Table 3).
Ultrastructural characteristics assessed by transmission electron microscopy in sperm from healthy men, stratified according to the number of cigarettes smoked or the quantity of alcohol consumed (n = 62)

Data presented as mean ± SD.
Nonsmoker, 0 cigarettes/day; smoker, 1 - 20 cigarettes/day; heavy smoker > 20 cigarettes/day.
Very low, < 6.4 g/day; low, ≥ 6.4 - < 15.4 g/day; moderate, ≥ 15.4 - < 33 g/day; high, ≥ 33 g/day.
P < 0.05 vs very low; one way analysis of variance and Scheffé's post hoc test.
Discussion
Tobacco smoking is known to have a detrimental effect on sperm quality, in particular concentration, motility and morphology.11 – 14 Smoking has also been associated with increased levels of aneuploidy in human sperm,15,16 lower seminal plasma antioxidant levels16,17 and increased oxidative damage to sperm DNA.18,19 In addition, chronic alcohol intake may affect male fertility by decreasing sperm volume, count and motility, and by affecting morphology.4,20,21
Several studies have reported the effects of cigarette smoking or alcohol intake on sperm characteristics determined by light microscopy,4,11– 14,20,21 but few transmission electron microscopy studies have been conducted. The effects of cigarette smoking on sperm quality have also been studied by DNA analysis.15– 19,22,23 Reports concerning malformation of sperm related to infertility have demonstrated that transmission electron microscopy can be a valuable tool in determining the presence and nature of morphological defects.24 – 27 Some studies have used transmission electron microscopy to demonstrate smoking- or alcohol-associated morphological changes in sperm ultrastructure.28,29 The present study used the sensitive transmission electron microscopy method to maximize detection of the effects of smoking and alcohol on sperm. A systematic classification of the ultrastructural pathology of human sperm is difficult to compile because of its organisational complexity. The current study therefore followed recognized protocols to investigate all ultrastructures comprehensively. 10
A meta-analysis found that smoking was associated with a 13 – 17% decrease in sperm concentration. 30 In addition, cigarette smoking has been shown to be associated with reductions in several parameters including sperm numbers, motility and normal morphology. 5 Data from the present study indicate an association between smoking and sperm count, but not semen volume, motility or morphology.
Alcohol consumption was associated with an increase in morphologically abnormal sperm in the present study, which is consistent with the findings of others. 20 The sperm head is considered normal when the plasma membrane, nuclear envelope, acrosome and chromatin are all of normal appearance; in addition, normal axonemal components, mitochondria and plasma membrane are required for the tail to be considered normal. 27 Axonemal or periaxonemal anomalies and axonemal deficiencies are presented in infertile men, and are thought to interfere with sperm motility.31,32 Regional nuclear shape malformation has been associated with DNA damage in spermatozoa. 33 There were significant differences in the numbers of sperm with morphologically abnormal nuclei and plasma membranes associated with alcohol consumption in the present study.
In conclusion, the present study revealed an association between heavy smoking (> 20 cigarettes/day) and decreased sperm count. In addition, alcohol consumption was associated with increased numbers of morphologically abnormal sperm.
Footnotes
Acknowledgements
This work was supported by Hanmi Pharmaceutical Co., Ltd. and Chung-Ang University Research Institute for Biomedical and Pharmaceutical Sciences.
Conflicts of interest: The authors had no conflicts of interest to declare in relation to this article.
