Abstract
Background:
Patients’ satisfaction with healthcare services contributes to their compliance with the treatment and thus impacts their health. Therefore, patient satisfaction is increasingly being used as an indicator of health system performance in a country. Though several studies have been reported from different parts of India, most did not include psychiatric patients. This study assessed the level of satisfaction of psychiatric outpatients and its association with socio-demographic, hospital-related, and treatment-related variables.
Methods:
This cross-sectional study assessed 152 patients attending psychiatry outpatient department (OPD) of a tertiary care hospital. Treatment-related satisfaction was measured using the Short Assessment of Patient Satisfaction (SAPS) scale, and variables not related to treatment were assessed using Likert scales.
Results:
Most participants were satisfied with the overall cleanliness of the hospital (82.9%), the useable condition of toilets (73%), and waiting time in the OPD ticket counter, doctor’s room, and pharmacy. More than 80% were pleased with the OPD staff’s behavior and working efficiency. In the seven dimensions of the SAPS scale, satisfaction level was variable. Overall satisfaction with the care received in the hospital was 60.5%.
Conclusions:
The level of patient satisfaction is good in psychiatry OPD services of our hospital, and it depends on treatment-independent variables also. So, liaison between the medical- and non-medical-management teams is crucial to augment patient satisfaction.
Keywords
About 60% of patients with psychiatric disorders, who were stable and attending the hospital regularly, were satisfied with the OPD services. Both factors related and unrelated to treatment contributed to overall patient satisfaction.Key Message:
Patient satisfaction can be defined as a feeling of pleasure or disappointment that shows the perceived differences between patient expectations and what is actually received during the care process. 1 The level of patient satisfaction varies from country to country and even within a country or state from region to region. Assessment of patients’ satisfaction towards the service is easier than evaluating the quality of medical services they receive. 2 Patient satisfaction with the healthcare services has been seen to determine their compliance with the treatment to a great extent, contributing to the positive impact on health. 3 Thus, patient satisfaction is increasingly being used as an indicator of health system performance in a country. Patients’ expectations from healthcare facilities are increasing, and to cope with this demand, our healthcare sector needs to grow and improve at a rapid pace. The outpatient department (OPD) is the first point of contact for patients with the health care system; globally, 80% of patients need only OPD-based treatment. 4 Thus, the level of satisfaction of patients availing OPD services can be a good indicator of the effective healthcare delivery of an institution. Studies have estimated the level of satisfaction in different parts of India.1, 3, 5–17 But surprisingly, most of them excluded psychiatric patients.
This study was conducted to assess the overall level of satisfaction of the often- overlooked persons suffering from psychiatric disorders and to evaluate the association between the level of satisfaction and their socio-demographic, hospital-related, treatment-related, and non-treatment-related variables.
Materials and Methods
This cross-sectional, observational study was conducted in a psychiatry OPD of Calcutta National Medical College, a tertiary care teaching institute in Kolkata. The Institutional Ethics Committee approved the study. It was conducted over 6 months (October 2020 and April 2021). All the consecutive adult patients with an established diagnosis of a psychiatric disorder (as per ICD-10 criteria) who had been undergoing treatment in the OPD of the hospital for at least 6 months and had at least a primary level of education were enrolled in this study. Data were collected from patients not treated by the investigators (on non-OPD days) so that the subjective bias of the investigators and the implied pressure on the patients could be minimized.
For inclusion in the study, patients who gave written consent were screened using the Global Assessment of Functioning (GAF) Scale. Patients with a GAF score >50 (indicating mild to moderate symptoms or difficulty in social, occupational, or school functioning) were included. Patients who were admitted or discharged on the day of the interview, medical or paramedical students or staff of the hospital, or brought by police or Non-Government Organizations (NGOs) or any other organizations were excluded. Figure 1 depicts the flowchart of the recruitment of patients. Six patients didn't complete the interview and the statistical analysis was done on 152 patients (n=152).

GAF: Global Assessment of Functioning, NGO: Nongovernmental organization.
Assessments
Socio-demographic and related data, including age, gender, education, occupation, marital status, residence, distance from the hospital, travel time, and travel cost, were obtained using a semi-structured questionnaire. Information related to cleanliness (hospital and toilets) and waiting times (at the ticket counter, outside doctor’s room, and pharmacy) were gathered by 2-point and 3-point Likert scales, respectively. Behavior and work efficiency of non-medical OPD staff and the availability of required medicines in OPD pharmacy and investigations in central pathology laboratory were gathered by a 4-point Likert scale.
Global Assessment of Functioning (GAF) 18 scale was used to assess patients’ psychological, social, and occupational functioning on a continuous scale of 0 to 100 (a higher score indicates better functioning).
Information regarding the level of satisfaction of patients towards medical treatment and care was obtained using the Short Assessment of Patient Satisfaction (SAPS) scale. The SAPS is a reliable (Cronbach alpha = 0.86) scale that assesses patient satisfaction in seven dimensions, including treatment satisfaction, explanation of treatment results, clinician care, participation in medical decision-making, respect by the clinician, time with the clinician, and satisfaction with hospital/clinic care. Responses for each dimension are measured using a 5-point Likert scale (from 0 to 4, the maximum possible score being 28; highest satisfaction). Categorical responses for SAPS are interpreted as 0–10 very dissatisfied, 11–18 dissatisfied, 19–26 satisfied, and 27–28 very satisfied. The scale is concise and easy to use and score, and may be applicable in different settings. 19 The SAPS is a self-administered scale in English. Two bilingual persons translated it into the local language (Bengali) and then that version was retranslated into English by another two bilingual persons who did not know the original scale. Then, after finer modification, we applied the scale to the study population.
Data Analysis
Data were compiled in an Excel sheet. We used descriptive statistics (mean with standard deviation) for data enumeration and unpaired t-test, Spearman’s Rank Sum test, and Analysis of Variance (ANOVA). Post-hoc analysis of the significant ANOVA results was done using the Tukey test. Statistical analysis was done using SPSS version 22.
Results
Socio-Demographic and Clinical Profile
A total of 152 patients completed the study. They had a mean age of 42.67 (SD: 15.20) years. The majority were male (53.3%), Muslim (50.7%), married (55.9%), and from urban (52%) background, with median years of education of 12 (IQR: 6). About half of them (48.5 %) were employed (Table 1).
Socio-Demographic and Clinical Profile (N = 152).
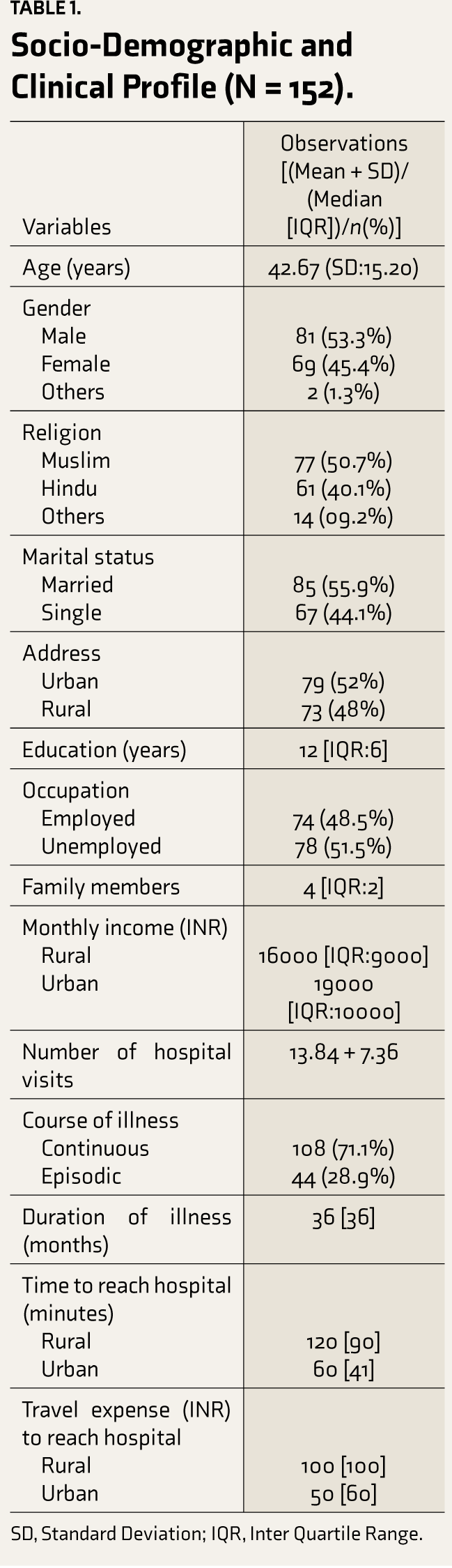
SD, Standard Deviation; IQR, Inter Quartile Range.
Their median duration of illness was 36(36) months, and the average number of hospital visits was 13.84 (SD: 7.36). The time and money spent to reach the hospital were more in those from rural than urban areas. They had a wide range of psychiatric disorders; the most prevalent were neurotic, anxiety, stress-related, and somatoform disorders category of ICD 10 (F40–F48, 32.2%), followed by mood disorders (F30–F39, 31.6%) and psychotic disorders (F20–F29, 21%).
Satisfaction and Sociodemographic and Clinical Variables
The mean SAPS score was 17.34 (SD: 5.87). Satisfaction levels and comparisons of SAPS scale scores among gender, residence, and different ICD10 diagnostic categories are summarized in (Table 2).
SAPS Score Comparison Among Age Group, Gender, Locality, and Diagnostic Category.
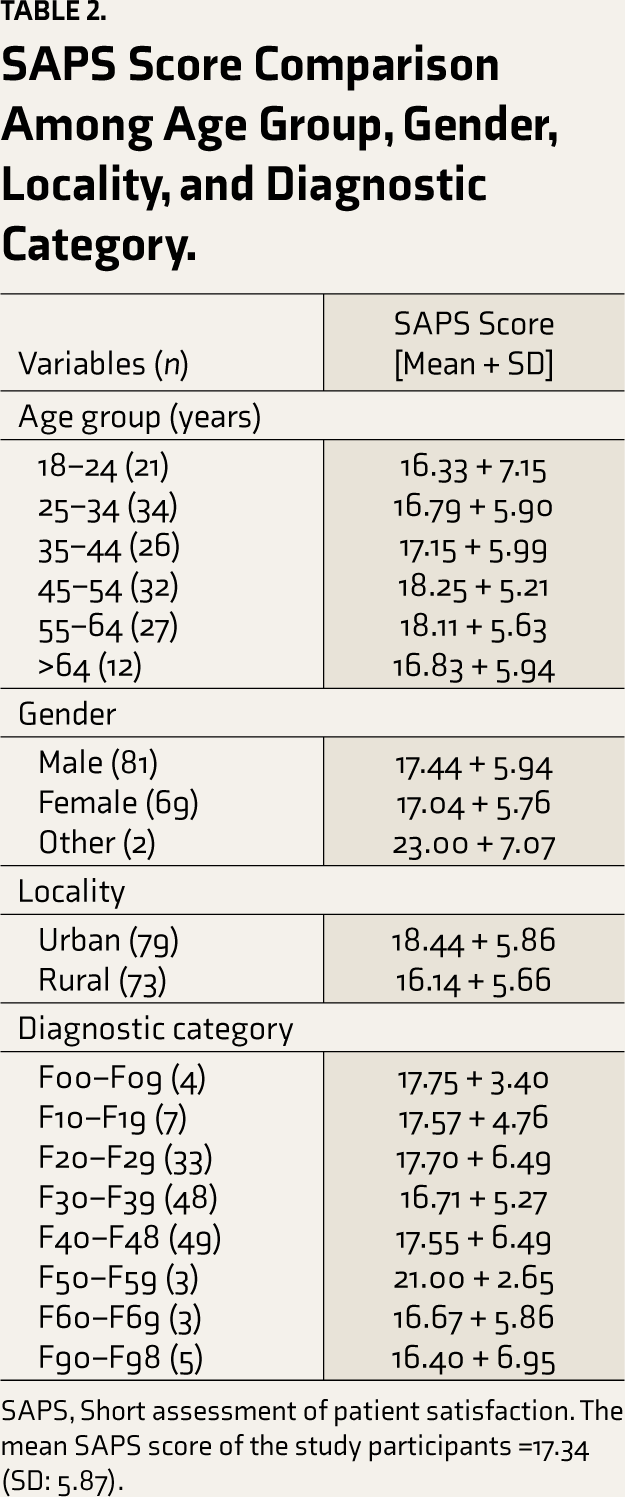
SAPS, Short assessment of patient satisfaction. The mean SAPS score of the study participants =17.34 (SD: 5.87).
Comparisons of mean SAPS scores among different age groups, gender, religion, marital status, education level, occupational statuses, number of family members, and different diagnostic categories were non-significant.
Satisfaction About Factors Not Related to Treatment
Most of the patients were satisfied about non-treatment-related ariables including cleanliness of the hospital, toilets, behavior, and work efficiency of the non-medical opd staff (Table 3).
Patients’ satisfaction regarding the overall cleanliness of the hospital and the usable condition of toilets were statistically significant.
Profile of Satisfaction About Factors Not Related to Treatment.

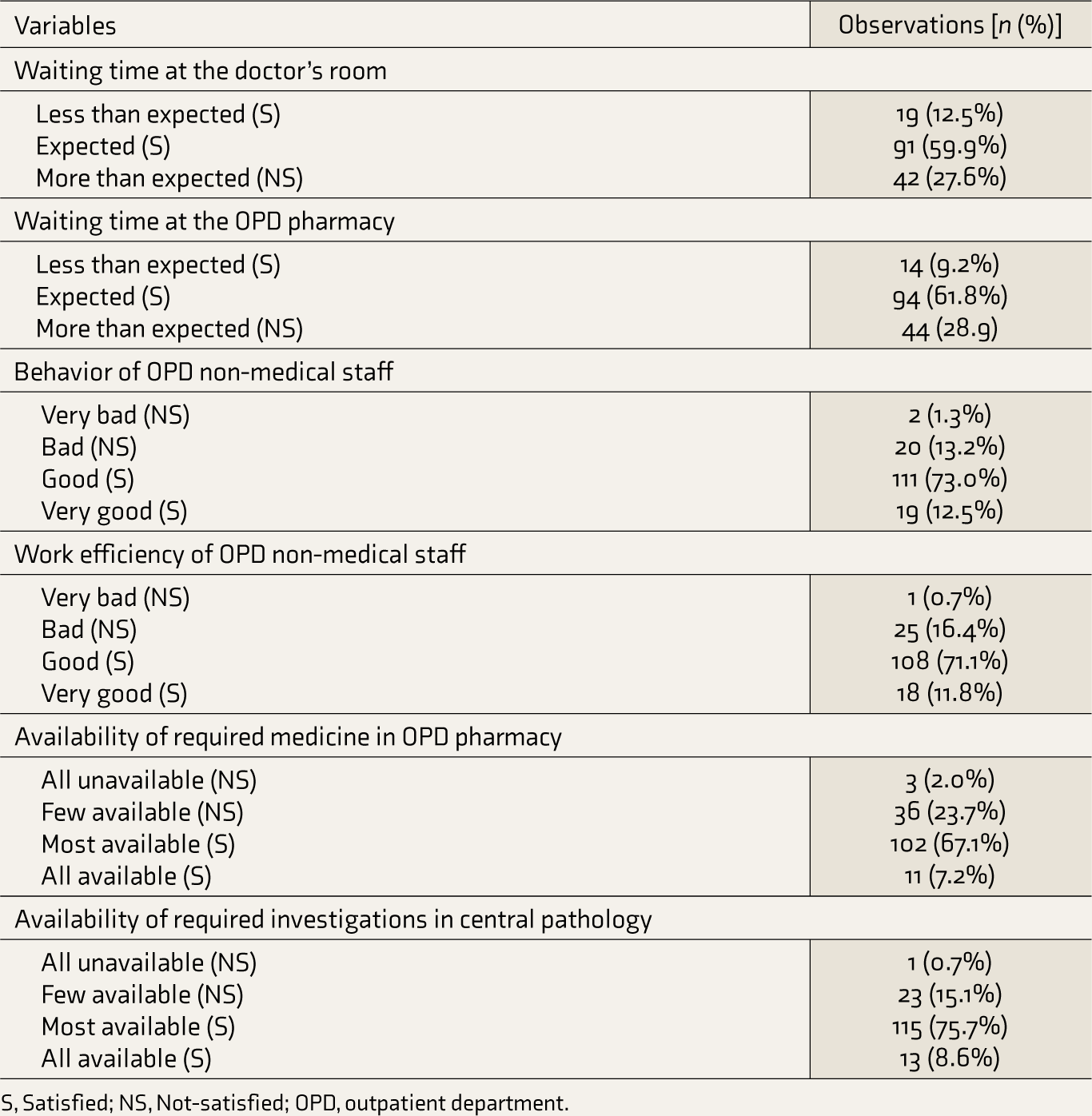
S, Satisfied; NS, Not-satisfied; OPD, outpatient department.
Satisfaction was also significantly associated with waiting time at the ticket counter, outside the doctor’s room, at the OPD pharmacy and behavior, and work efficiency of OPD staff (one-way ANOVA and post-hoc analysis of the significant ANOVA result). SAPS score was not significantly affected by the availability of medicine at the OPD pharmacy or the availability of investigations at the central pathology laboratory (Table 5).
Satisfaction About Treatment-related Factors
The treatment-related satisfaction and subscale score of seven items of the SAPS are given in Figure 2 and Table 4. The overall satisfaction (satisfaction and high satisfaction) was 60.4%. The effect of treatment (65%), explanation by doctors (56.%), and careful examination (63.8%) had higher satisfaction rates than other items.
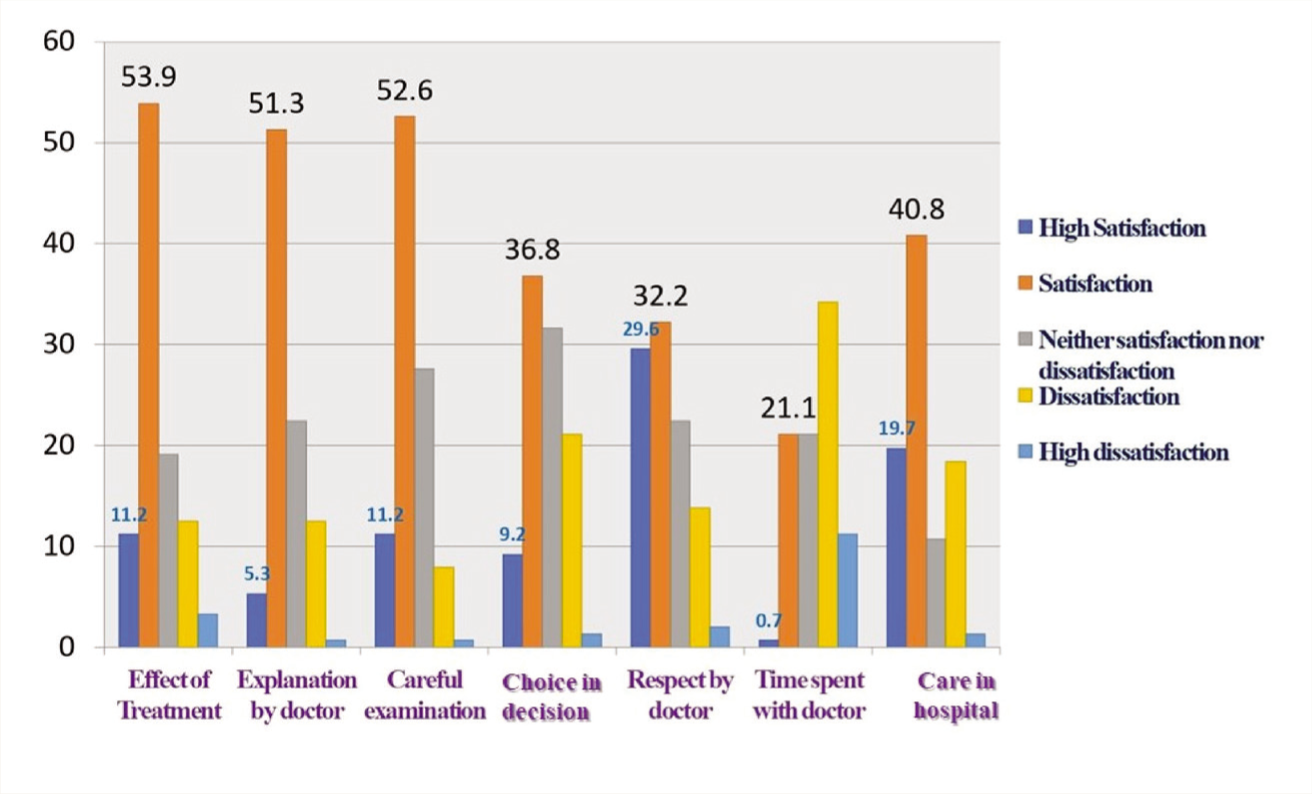
SAPS: Short Assessment of Patient Satisfaction.
Scoring of Different Dimensions of SAPS Scale.
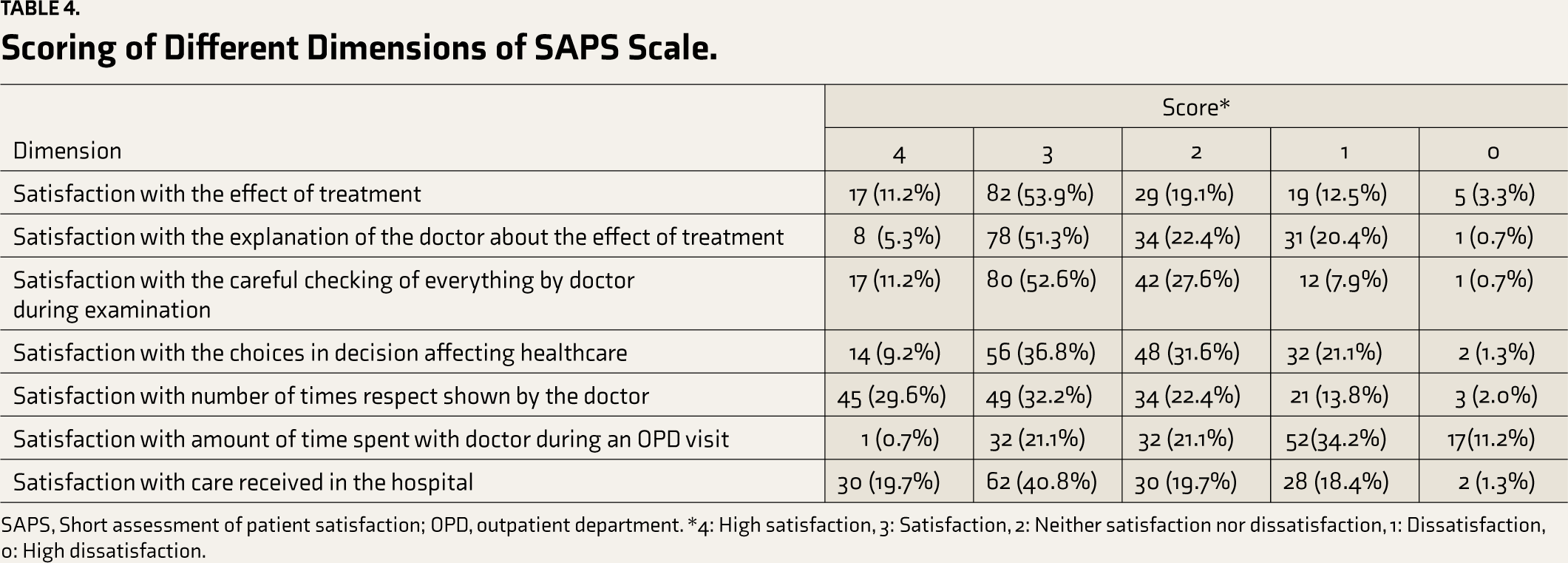
SAPS, Short assessment of patient satisfaction; OPD, outpatient department. *4: High satisfaction, 3: Satisfaction, 2: Neither satisfaction nor dissatisfaction, 1: Dissatisfaction, 0: High dissatisfaction.
No significant correlations were found between the SAPS score and monthly income, the number of hospital visits, total duration of illness, time to reach the hospital, or travel expenses to reach the hospital.
To assess the correlation between SAPS score and different factors non-related to treatment, unpaired t-test and one-way ANOVA were used. A strong positive correlation was observed between the SAPS score and the overall cleanliness in the hospital, condition of the hospital toilet, behavior of the OPD clerical staff, work efficiency of the OPD clerical staff, and availability of medicines in OPD pharmacy. In contrast, waiting time at the ticket counter, doctor’s room, and OPD pharmacy were negatively correlated with the SAPS score. We found no correlation between the SAPS score and the availability of required investigations in the central pathology laboratory (Table 5).
Association of SAPS Score with Non-treatment-related Variables.
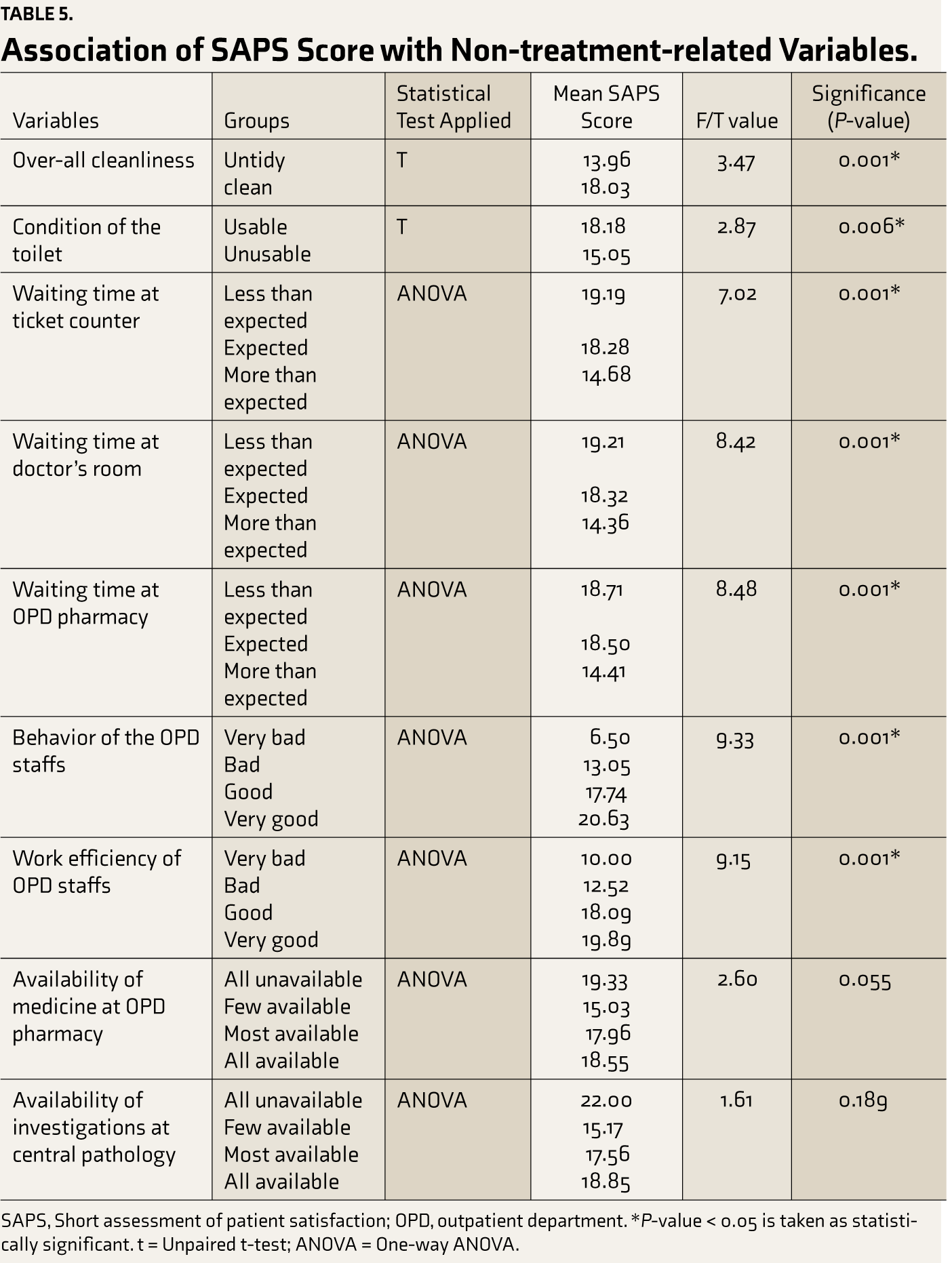
SAPS, Short assessment of patient satisfaction; OPD, outpatient department. *P-value < 0.05 is taken as statistically significant. t = Unpaired t-test; ANOVA = One-way ANOVA.
Post-hoc analysis of the significant ANOVA results showed that patient satisfaction level has been increased proportionally with decreasing waiting time at the ticket counter, doctor’s room, and OPD pharmacy, with better behavior and work efficiency of the OPD staff, and all these associations were found to be statistically significant (Table 6).
Post-hoc Analysis of the Significant ANOVA Results.
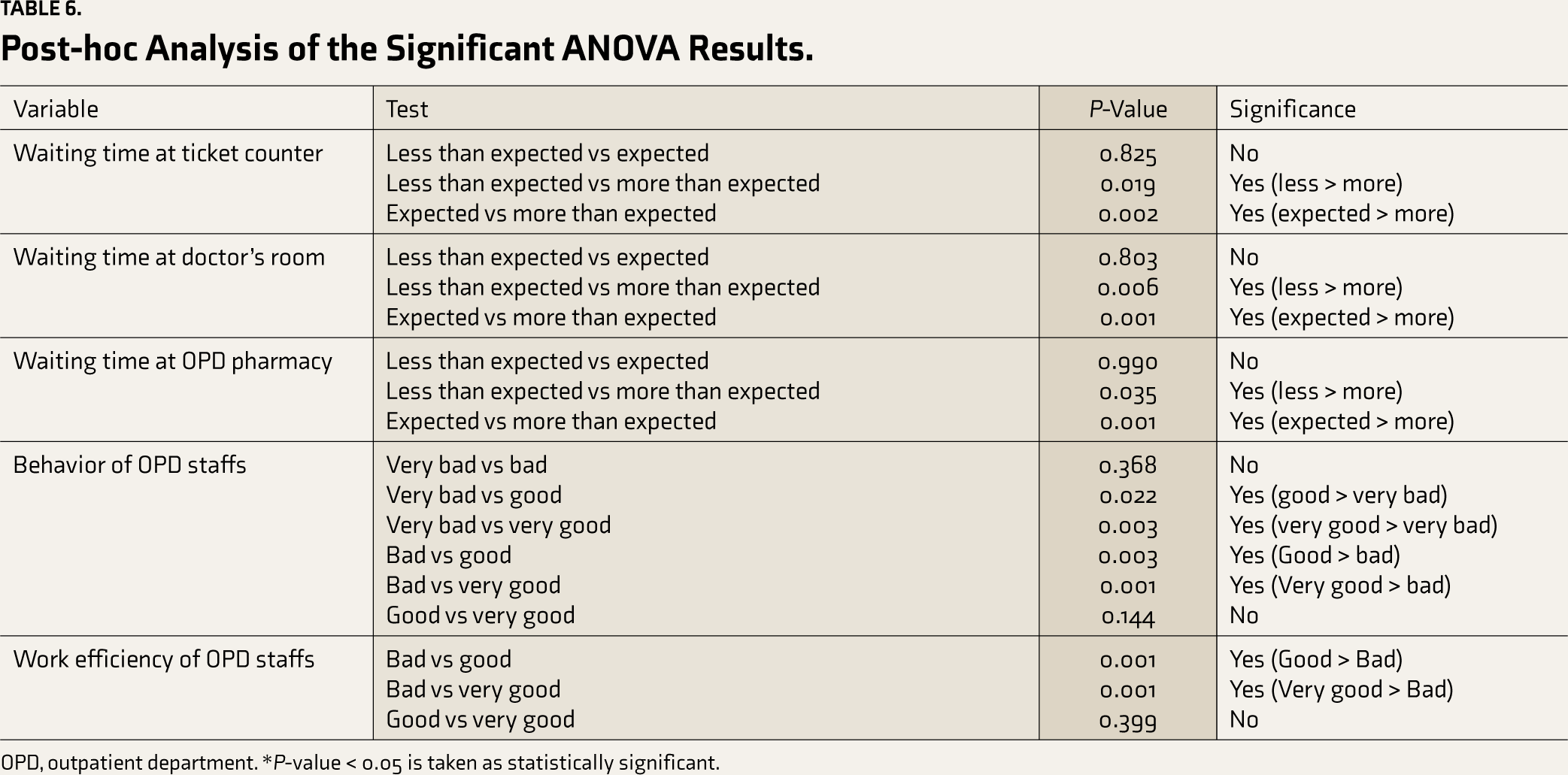
OPD, outpatient department. *P-value < 0.05 is taken as statistically significant.
Discussion
Patient satisfaction surveys are valuable for understanding patients’ needs and perceptions of the service they received. Satisfaction is influenced by a myriad of factors, including expectations from the health care system, state of a person’s emotion at that particular moment, and many more.
We evaluated the level of satisfaction among psychiatric patients attending psychiatric OPD: in treatment-related domains by the SAPS scale and non-treatment-related domains by a Likert scale questionnaire. The overall treatment-related satisfaction (satisfaction and high satisfaction) was 60.4%. Most participants were satisfied with the OPD staff’s behavior (85.5%) and work efficiency (82.9%) and overall cleanliness of the hospital (82.9%). The satisfaction was significantly correlated with patients’ locality of residence, overall cleanliness of the hospital, usable conditions of the OPD toilets, behavior and work efficiency of the OPD staff, and waiting time at the ticket counter, doctor’s room, and OPD pharmacy.
Holikatti et al. (n = 60) reported a general satisfaction level of 57%, with a higher level of satisfaction noted in interpersonal aspects (71.4%) and time spent with doctors (62.4%). They also found variations in satisfaction levels associated with different categories of psychiatric diagnoses, with the highest satisfaction reported by patients with depression. 17 We found that patients with ICD-10 diagnosis of F50–F59 had the highest satisfaction score, though the result was not statistically significant.
Another study with 104 participants (45 patients and 59 family members) reported that >90% of patients and family members were satisfied with the OPD services and that 75%–80% were satisfied with the supply of drugs, clinical care, and cleanliness of the hospital. 20 Jena et al. reported 87.28% satisfaction with OPD services; the study was conducted with a large sample size (n = 519) but did not include psychotic patients. 21
Studies from various countries on the satisfaction about psychiatric outpatient services also had reported a high level (70%–90%) of satisfaction.22–25
In our study, 126 participants (82.9%) were satisfied with the overall cleanliness of the hospital, which is lower than the rate Prasanna et al. observed in a private hospital. 10 About three-fourth of our participants (73%) were satisfied with the usable condition of the toilets, which is much higher than the finding by Kumari et al. (31.3% and 2.9% were satisfied with the usable condition of toilets of tertiary care government hospitals and primary care hospitals, respectively). 3 Qureshi et al. also reported very poor satisfaction: only 13% (inpatients of a maternity government hospital) were satisfied with toilet condition, 26 whereas Kulkarni et al. found a rate of 43.9% (inpatients of a private hospital). 27 The study set-up (indoor/ outdoor), nature of the participants, and difference between government and private settings might explain the differences between our findings and that of the other authors.
The present study’s participants were satisfied (expected + less than expected) with the waiting time at the ticket counter (71%), doctor’s room (72.4%) and OPD pharmacy (71%), and the rates are higher than what was reported by Goyal et al. 9 and Jawahar et al. 28 Most of our participants were satisfied (“good” and “very good”) with the OPD staff’s behavior (85.5%) and their work efficiency (82.9%): a higher proportion than what Kulkarni et al. found (59.5%). A higher proportion of participants (74.3%) were satisfied with the availability of required medicines in OPD pharmacy than in the study of Kaushal et al. 12 and Goyal et al. 9 However, our rate was comparable to that of Qadri et al. 29
Regarding the level of satisfaction about the different dimensions of the SAPS scale, we found that 65.1%, 63.8%, and 61.8% of the participants were pleased with the effect of their treatment, affirmed that the doctors were very careful to check everything during the examination, and felt respected by the doctors, respectively. These findings are comparable to the findings of an OPD-based study by Jawahar et al., involving multiple disciplines. 28 However, higher rates of satisfaction were reported by Kulkarni et al. (87.8% of the participants were satisfied with the behavior of doctors) 27 and Kaur et al. (80% of OPD patients were satisfied with the care the doctors provided). 30 We found a slightly lower level of satisfaction (56.6%) in the “explanation of the doctor about the result of treatment” than in the studies of Kaur et al. 30 and Prasanna et al. 10 ‘Patient’s choice in decisions affecting his/her healthcare’ dimension (46%) and “time spent with doctor” dimension (21.8%) too had lower satisfaction rates. Both Jawahar et al. 28 and Kaur et al. 30 reported a very high satisfaction rate with regard to the time spent with the doctor. This may be attributed to our huge patient load and the fact that comparatively a smaller number of psychiatrists are posted in this hospital. However, this area needs to be explored further and necessary corrections to be made.
Patients’ overall satisfaction with healthcare services varies widely in India. In studies conducted in different parts of this country, it has been reported to be >90%,12, 28 between 80% and 90%,3, 9, 29 between 70% and 80%,14, 26, 27, 31 and <70%,32–34. One study reported very poor satisfaction (23%). 34
Limitations
The level of satisfaction is a dynamic construct that can vary over time, depending on patients’ disease severity. This was a cross-sectional study, and such changes can be picked up in a longitudinal study only.
This was an observational study and somewhat exploratory too, where we found an association between patient satisfaction and non-treatment-related areas of the healthcare system. The correlation might be due to a Type I error (false positive). So, interpretations should be drawn carefully.
The non-treatment-related variables were assessed by a Likert scale that was not validated. Validation of the scale is needed for wider use in future. We used SAPS scale after translating it into its Bengali version, which was not validated.
Lastly, we included patients who attended the OPD regularly for at least six months. If the defaulted subgroup had been included, we may have found a lower level of satisfaction.
Conclusion
Patient satisfaction is an important parameter to assess the quality of the overall services provided by a hospital. This OPD-based study found that apart from treatment-related factors, non-treatment-related variables too play an important role in satisfying patients. Thus, liaison between the medical and non-medical management teams is crucial to improving health services and patient satisfaction.
Footnotes
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
