Abstract
Background:
Medical students are at an increased risk of developing substance use and related problems (SURP) because of the inherent stress associated with the professional medical course apart from the developmental risk factors. However, this is under-researched. Moreover, a comprehensive review on the prevalence of SURP among the medical undergraduates (UGs) and associated factors is lacking from India. To fill this gap, the current research work is aimed to review the existing literature on the magnitude of the SURP among UGs of India and its determinants.
Methods:
PubMed, Medline, and Google Scholar databases were searched for the original articles studying the prevalence of SURP among medical UGs of India, published from inception till date. Non-original articles, studies on behavioral addictions, and those not directly assessing the prevalence of SURP among the medical UGs were excluded.
Results:
A total of 39 studies were found eligible for the review. Alcohol (current use: 3.2%–43.8%), followed by tobacco (3.7%–28.8%) and cannabis (1.6%–15%), were the common substances used by the medical students. Among the females, an increasing trend of substance use, particularly of nonprescription sedatives (even higher than males), alcohol, and smoking, was seen. Family history, peer pressure, transition from school to college life, and progression in the medical course were important associated factors.
Conclusion:
Sensitizing medical students and college authorities, increasing the duration of training on SURP in medical curricula, and providing psychological support for the students with SURP could address this issue.
Substance use and related problems (SURP) are one of the most important public health concerns with wide ranging implications. A national survey from India reported that the prevalence of the current use of alcohol (even a single use in the past 12 months) in the general population was 14.6% (making it the most common psychoactive substance used by adults, excluding tobacco). Lower rates were found for cannabis, opioids (2.8% each), sedatives (1.08%), and inhalants (0.7%). 1 The Global Adult Tobacco Survey found that in India, the prevalence of tobacco smoking and use of smokeless tobacco (SMT) was 10.7% and 21.4%, respectively. 2
Youths (adolescents and young adults) are particularly prone to experiment with substances. This is mediated by the developmental traits of sensation seeking and impulsivity, way of socializing, and peer pressure.3,4 Data from the United States (US) found that as high as 33.8% of medical students consumed >5 drinks in one sitting in the last two weeks It assess prevalence of risk drinking (heavy episodic drinking) in the last two weeks. 5 A review from India reported the prevalence of substance use among medical students, interns, and house physicians to range from 32.5% to 81.2%. 6 Literature suggests that the transition from school to college predisposes the students to indulge in substance-using behaviors regarding initiation and maintenance of substance use.7–9 Longitudinal research reported that smoking; regular use of alcohol; history of alcohol-related difficulties, anxiety, or anger; and frequent use of alcohol in nonsocial settings in medical students during the undergraduate (UG) course serve as the risk factors for future alcohol abuse in them. 10
Training and teaching in psychiatry, including in substance-use disorders, in the medical-UG curriculum in India is grossly inadequate. Mental health training is often considered elective/optional, which deprives medical UGs of acquiring necessary skills in psychiatry. Medical educationists have proposed for an increase in the hours of teaching and skill-based training in psychiatry and substance use in the UG medical curriculum.11–13
Despite such a high prevalence of the SURP among the medical students and its academic and social implications, there is a dearth of robust studies that systematically reviewed the magnitude of SURP and their risk factors. The availability of such data would help sensitize the medical students, college administration, and the authorities involved in the medical curriculum to take up necessary precautionary and therapeutic interventions.
The current review attempts to determine the magnitude of SURPs among the medical UGs of India and its determinants. The objectives of this review are threefold: (a) to identify the prevalence of various SURPs among the medical UGs of India, (b) to identify the risk and protective factors for the initiation and maintenance of the substance use among them, and (c) to propose recommendations for substance-use-related training in the medical curriculum and mental health support system for the students in medical teaching institutions.
Material and Methods
Search Strategy
The literature was searched in the PubMed, Medline, and Google Scholar databases using the search terms like “Smoking” [Mesh] OR “Alcohol Drinking” [Mesh] OR “Alcoholism” [Mesh]) OR “Substance-Related Disorders” [Mesh] OR Drug Abuse OR Drug Addiction OR Drug Dependence AND “Students, Medical” [Mesh] OR “Undergraduate Medical Education” OR “Education, Undergraduate Medical” AND “Republic of India” OR “India.” Bibliographic search was also performed to obtain additional records.
The inclusion criterion for the review were (a) peer-reviewed original articles that studied the prevalence of substance use disorders (tobacco, alcohol, smoking, cannabis, opioids, inhalants, sedative/hypnotics, or stimulants) among medical students (medical UGs from 1st to 4th years and interns), (b) studies conducted between January 1, 1980, and April 30, 2020, and (c) studies conducted in a medical college of India or has at least one center from India in case of a multicountry study. The exclusion criteria were (a) studies focusing on behavioral addictions (BAs, such as internet gaming disorders, pathological gambling, etc.), (b) research papers whose full text could not be retrieved (despite contacting the corresponding author or journal), and (c) studies assessing only knowledge, attitude, and beliefs regarding substance use among medical students.
Data Collection Process
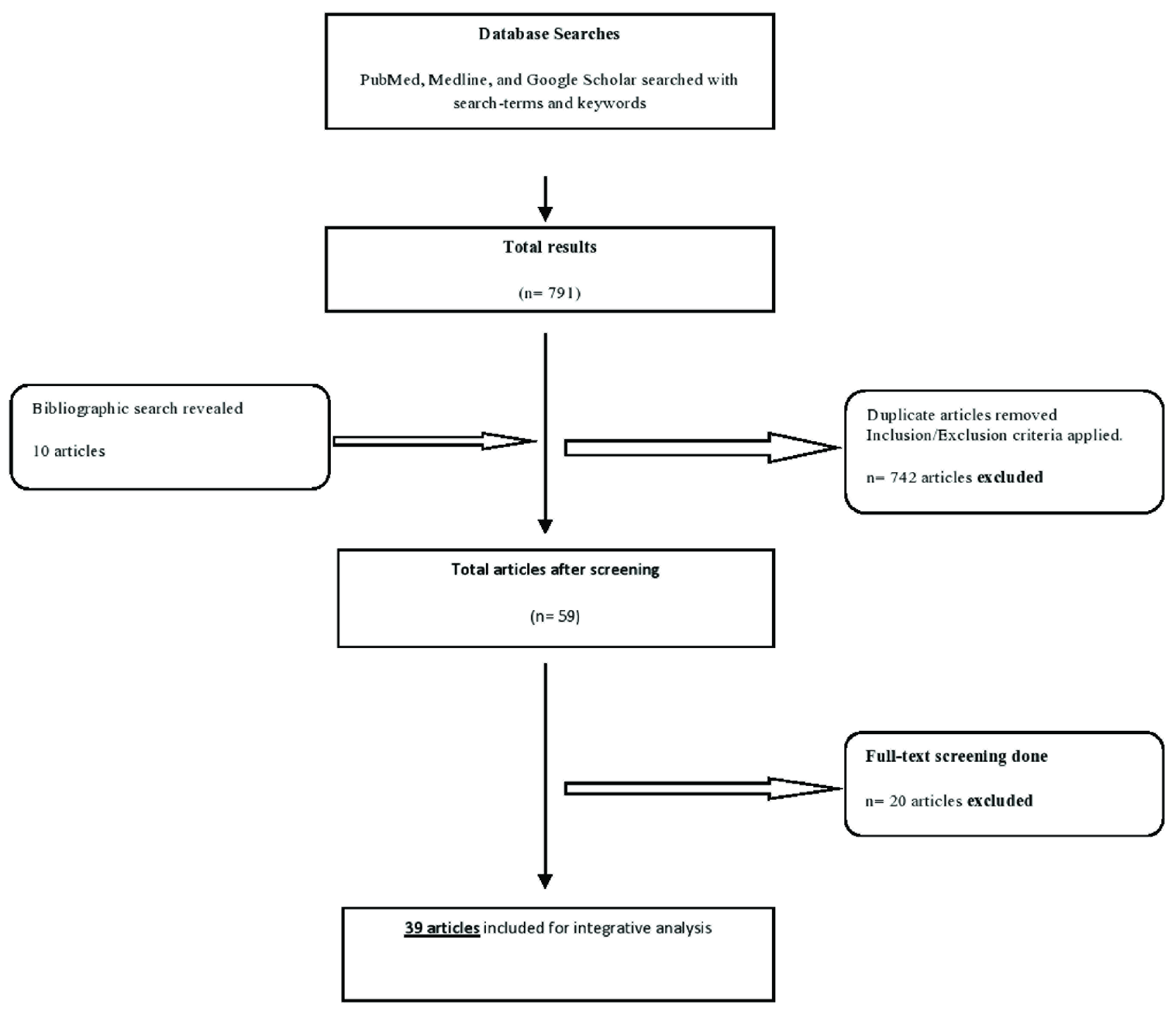
The initial search was conducted by one of the authors (HG). Subsequently, two authors (HG and SG) performed the title and abstract screening and removed duplicate and nonoriginal research papers. The differences in the opinions and doubts were cleared by mutual discussion. Following this, the first round of the full-text screening of the selected articles was performed (HG and SG) to ascertain the eligibility of short-listed articles. Doubts or differences between the authors were resolved through mutual discussions or by seeking the opinion of the third author (ARR). The process of data screening has been depicted in a flowchart (see Figure 1).
Flowchart Depicting the Process of Data Screening
Results
Initially, a total of 721 results were obtained. Upon applying the inclusion and exclusion criteria, a total of 49 studies were found suitable to be considered for the review. The bibliographic search yielded another ten records. Thus, a total of 59 studies were considered for the full-text review.
After the full-text screening (by HG; 10% of the records were screened in detail by another author, SG), a total of 20 articles were further excluded, out of which ten were excluded as they only assessed the knowledge, belief, and attitude about substance use or were reviews or commentaries, while ten articles were excluded as their full-text could not be retrieved despite making efforts to contact the authors. Finally, 39 articles were included in the review (see Table S1).
Study Design
All the studies were cross-sectional and questionnaire based. Most of the available studies were on tobacco use (n = 25, 64.1%), one study specifically assessed the prevalence of alcohol use, 14 and 13 (33%) dealt with more than one substances.
Sample Size
The sample size of the study varied according to the setting of the study, whether it is multicentric or unicentric, and the number of batches of medical students considered. The sample sizes of the studies varied from 64 to 3288, with four studies having a sample size of more than 2000.15–18 These were multicentric studies with more than one college and collected data on separate time periods.
Measuring Instruments
Regarding the assessment tools, 14 studies (35.8%) used a pretested self-designed questionnaire, 11 (28.2%) used a standardized WHO questionnaire for tobacco/drug use (with modifications), seven studies (17.9%) used either Global Health Professions Survey or Global Health Professions Student Survey to assess the prevalence of tobacco use, one study used CAGE Alcohol Questionnaire to assess alcohol dependence, while rest of the seven studies (17.9%) used different types of questionnaires. One study also looked for the prevalence of burnout and mental health problems, by utilizing the Oldenburg Burnout Inventory and General Health Questionnaire-12 (GHQ-12), respectively (see Table 1).
Potential Preventive Strategies at Different Levels for Reducing Prevalence of Substance Use Among Medical Students
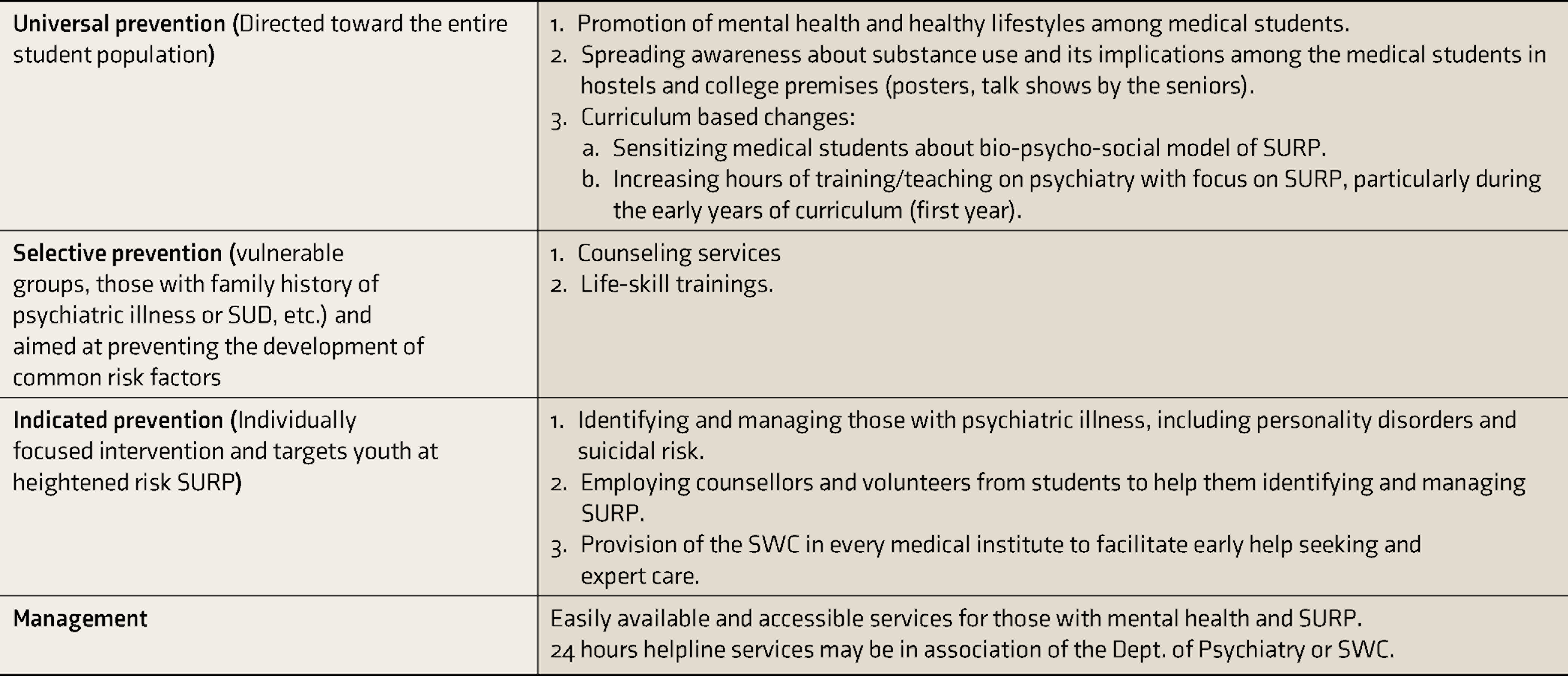
SUD: substance use disorder, SURP: substance use and related problems, SWC: student wellness clinic.
Setting of the Study
16 studies (41%) were multicentric in nature and conducted on students in more than one medical institute, while 23(59%) studies were unicentric. Most studies were from medical colleges located in big cities, and very few studies were from small cities.
Regional Distribution of the Studies
Most of the studies were from the Southern part of India (with maximum studies coming from Karnataka (nine), followed by the Western part of the country (Maharashtra, Gujarat). There were fewer studies from the Northern and Eastern parts of the country (with the exception of West Bengal). There were very few studies from the North-eastern part of the country.
Prevalence of Substance Use
Tobacco Use
The range of current (past one month) tobacco use was 1.0%–50.7%. Most of the studies gave prevalence in the range of 3.7%–28.8%. One study, which was limited to males, reported a prevalence as high as 50.7%, 19 and another multicentric study (conducted on 479 medical students from four colleges) reported the prevalence of SMT use to be as low as 1%. 20 The prevalence of current smoking varied from 2.1% to 26.1%. The prevalence of daily smoking ranged from 3.2% to 31.5%. The majority of studies gave prevalence between 3.2% and 10.4%. Two multicentric studies reported the prevalence of 27% and 31.5%, respectively. Both these studies had majorly male participants.21,22
Alcohol Use
The prevalence of current use of alcohol ranged from 3.2% to 43.8%. One study conducted on the fourth year medical UGs found the prevalence of the current alcohol use (alcohol use even once since the joining of the UG course) to be 43.8%, 23 while another study involving polysubstance use found the prevalence of the current use (last month use) to be a low 3.2%. 24
Cannabis Use
The prevalence of the current use of cannabis ranged 1.6%–15%.
Other Substances of Use
The prevalence of any substance use was found to be 25.9%–57.4%. We also found that medical students were also involved in the consumption of other licit (sedatives) and illicit substances (heroin, cocaine, and amphetamines).18,25–27
Factors Associated with Substance Initiation or Continuation
We found that the common factors associated with tobacco use/smoking were being male, family history (use in parents or siblings) of tobacco use/smoking, year of UG course, living in a hostel, peer pressure, and use of other substances like alcohol. A few studies also found that entry into medical college, being in supplementary batch, and perceiving one’s own substance use as not harmful were associated with tobacco use. When it comes to illicit drugs, it was found that the past 12-months use of licit drugs such as tobacco and alcohol, joint family living arrangement, substance use in family, and nonsatisfactory intrafamilial relationship were the associated factors.18,27,28 Importantly, students suffering from mental health conditions had a higher proportion of cannabis use. 29
Discussion
The present review was conducted to assess the magnitude and extent of the SURP among the medical students in India and to determine the factors associated with the same. This study focused primarily on the current use (past one month) of various substances among medical students. We found that a significant proportion of medical students were currently using substances, licit or illicit.
The prevalence of any substance use among medical students was 25.9%–57.4%. The most common substance of use was alcohol, followed by tobacco (smoking>smokeless) and cannabis. Further, the use of illicit drugs (excluding cannabis) was also observed. However, there was a lack of uniformity in the definitions for the “current use” of substance, with some studies considering single use in the last one month, to others considering use as infrequent as even single use in the past 12 months to single use in the past four years. Because of such discrepancies in the definition of the substance use frequency, the exact prevalence of the current substance use is difficult to ascertain. It would be prudent to keep last one month’s substance use as the current use as it correlates better with the present state of SURP. 30 Future studies, especially multicentric ones, with a uniform definition of current substance use, are warranted to get a clearer picture of the magnitude of the substance use.
We found that alcohol was the most commonly used substance, with the prevalence of current use ranging from 3.2% to 43.8%. This finding is consistent with the previous literature. 31 Further, the prevalence of alcohol use among medical students is similar to the general population. The national survey reported the current prevalence of alcohol use among the general population to be 14.6%, the prevalence in males being 27.3%. 1 However, more studies need to be conducted using a standardized tool; 32 studies are also required that compare the prevalence of alcohol use in medical students and the general population in the same location.
We found tobacco to be the next most common substance of use. A systematic review of the prevalence of tobacco use among medical students had reported the prevalence to be 17.2%. 31 Further, contrary to the nationwide epidemiological survey, which reported a higher prevalence of SMT use than smoking, 1 studies on the medical UGs found smoking as the most common mode of tobacco consumption. On a positive note, there has been a declining trend in tobacco use among medical students. 33 This could be attributed to the national prohibitory measures, including the anti-tobacco campaigns running across the country in which medical professionals are actively involved,34,35 and institutional level policy of smoking-free campus. Contrary to alcohol, the prevalence of tobacco use among the medical students was lower than that of the general population (9% and 21% for tobacco smoking and SMT, respectively) in India. 36 One article comparing the prevalence of substance use in medical and nonmedical students found that medical students, in general, had better awareness about the ill effects and harm of smoking. 37 However, more comparative studies are required in this regard to draw any firm conclusion.
Despite such a high prevalence of tobacco use among medical students, a world-wide survey among final year medical students revealed that medical students are not properly and systematically educated about the hazardous effects of tobacco use, including nicotine dependence and its treatment. 38 Hence, it would be imperative that the medical curriculum should allot more time in teaching and training in psychiatry, including the preventive and therapeutic strategies for nicotine dependence.11,13 This would result in the reduction in smoking habits among the students and also promote better clinical care for their patients with tobacco-related problems.
When it comes to the use of illicit drugs, we found cannabis to be the most common drug of use among medical students, with a prevalence of 1.6%–15.1%. This prevalence is in agreement with a previous systematic review that reported the prevalence to be 11.8%. 31 However, it is higher than the national average for the general population (ganja/marijuana use—1.2%). 1 The higher prevalence of cannabis use among medical students can be understood in the light that medical UGs often consider it to be an innocuous drug and that cannabis, having the anxiolytic, hypnotic, mood-altering, and appetite-promoting properties, becomes a source for the same.39–42 Literature suggests that stress, anxiety, depression (62% students satisfied the criteria of “caseness” by General Health Questionnaire-9 [GHQ-9]), and insomnia are common mental health issues among medical students; 29 cannabis use might represent a form of self-medication for the ongoing psychological distress. Further, the latest trend of legalization of cannabis in some of the western countries could also portray it as a safer drug. 43 Further, cannabis being a gateway drug, its use often precedes other licit and illicit drugs use or becomes a concomitant drug with the use of other substances.44–47 Hence, medical students should be taught about the psychotomimetic effect of cannabis and its adverse psychological consequences and also about its tendency to predispose an individual to use of other substances.
Other illicit substances, apart from cannabis, that have been found to be used by medical students include heroin, cocaine, and amphetamines. A study from India reported the prevalence of illicit drug use among medical students to be 1.5%. 18 However, there is a dearth of studies that assess the magnitude of the use of illicit substances, including the newer psychoactive substances among medical students; therefore, their exact prevalence cannot be ascertained.
Literature suggests that medical students have the highest proportion of current cigarette smokers among various health-related courses (dental, pharmacy, and nursing students). 48 Similar finding has been reported concerning current use of alcohol. 14 Although prevalence of substance use has been lower among medical students compared to students of other courses such as engineering, commerce, arts, etc., 49 it is still sizeable and warrants preventive and health-promotive measures.
We also found considerable regional variations with regards to the availability of the studies from the country, with maximum studies coming from southern, followed by the western part of the country. The latter can be attributed to the significantly higher number of medical colleges located in this part of the country.1,25,36,49 Hence, the findings of the current review cannot be generalized to the whole of India. On the other hand, SURP, both licit and illicit, are common in the other regions of India as well, particularly the northern and north-eastern parts. 1 These findings warrant the need for more nationwide studies that would assess the prevalence of substance use among medical students and compare its region-wise distribution.
Most of the studies were conducted on male medical students. We found that the overall prevalence of substance use for all substances except nonprescription benzodiazepines was higher among males than females. 18 These findings are consistent with western literature.31,50,51 Further, there has been an increasing trend of smoking among females in India. 52 The latter can be attributed to an increasing social acceptance of smoking among females in the country and the country’s changing sociodemographic characteristics, especially in the tier-1 cities. 52 Experimental use of alcohol among female medical students (4.2%) has also been reported in the literature. 53 Although this figure is lower than the rates available from the western literature (reported to be as high as 21.4%), 54 the Indian picture still warrants attention, especially in the context that females are at a higher risk of alcohol-related intoxication (telescoping) and related complications.55,56 Hence, the medical curriculum should teach students about safe drinking practices, including refraining from drunk driving.
The current review found that the common associated factors for SURP among the medical students are male gender, peer pressure, progression in medical education, family history of substance use (particularly for tobacco), living in a hostel, and previous history of use of other substances. However, it should be emphasized that the studies included in the current review are cross-sectional; hence, a causal relationship cannot be established. Furthermore, studies have not used a multivariate analysis (regression analysis) to provide the exactness and strength of association.
Male gender was found to be a major associated factor for substance use. Several studies have found a positive correlation between male gender and the use of tobacco,16,37,38,48,57–60 alcohol, 14 and other substances, including polysubstance use.24,28,34,49 One study showed that there is an increase in tobacco products among female students. 15 In contrast, the female gender has been shown to have a negative association with illicit drug use. 18 This gender difference for substance use is in agreement with previous research on medical students.31,33 However, these differential findings in Indian epidemiological studies should also be seen in the light of a lesser number of available studies assessing the prevalence of use of different substances among females, lack of longitudinal data, and its correlates such as peer-influence (social factor), psychological stress related to academics or otherwise (psychological factor), family history (biological factor), etc. Hence, more research is required particularly involving female medical UGs to enhance our understanding about the female substance use and associated factors.
Peer pressure was found to be the most common important factor associated with the initiation of substance use.31,61–63 A positive correlation was found between tobacco use and peer pressure,21,22,64,65 a finding consistent with the western literature. 31 This association can be explained by the peer cluster theory, which highlights that socialization is important for adolescent developmental characteristics and that their interactions with their peers produce peer clusters that can encourage their involvement in drug use. 66 Since first-year students are the first to encounter the effects of peer pressure, it is important to regularly conduct sessions on ill-effects of substance use for these students as a part of curriculum and induction program. Furthermore, modifiable risk factors such as mental stress related to academics and life challenges and adverse peer influence may be addressed through workshops on time management and stress management skills (including promoting traditional relaxation activities such as yoga, meditation, etc.) and by psycho-educating them about the social-cognitive model of substance use and assertiveness training, respectively.
A correlation was noticed between the prevalence of substance use and one’s progression in medical education, with a higher prevalence of substance use in the final year medical students than in freshers.16,17,24,27,53,59,64,67 This finding is in sync with the available reviews.31,50,68 However, some studies in our review gave a different result as well. One study gave a negative correlation between tobacco use and year of medical education 37 , and one gave no correlation between them. 60 The majority of studies showed a positive association. Literature suggests that the medical education program is intrinsically stressful and, especially with the maladaptive form of coping to the academic stressors, predisposes medical students for substance use either as a form of avoidant coping or self-medication for the underlying psychological problems.69,70 Therefore, it becomes imperative that medical students and college administrations are sensitized about the interaction of stress, mental health problems, and substance use. Although some steps have been taken in this regard by posting the medical students in the substance use treatment facilities during their posting of psychiatry and by establishing student wellness centers for the preventive and therapeutic measures, they are restricted to some premier institutes of the country. 71 Other possible interventions are increasing the awareness about SURP among students by using posters (with catchy themes) in college or hostel premises, senior/peer support system, promotion of healthy lifestyles (sports, arts, music, literature, etc.), and rewarding those excelling in these extracurricular activities. Improving the availability and accessibility of the psychologist/psychiatrist, in a nonstigmatizing and anonymous manner, along with a 24/7 helpline or time-bound volunteer support (peer or senior) system in the institution (like other existing mental health-related helpline services in the country) would give the students an easy access to professional help.
Family history of substance use (in parents and siblings) was consistently found to be an associated factor for substance use,14,21,22,27,34,53,58–60,64,65,67,72–74 a finding in concordance with studies on adolescents and nonmedical college students.75–79 This association can be explained by the shared bio-psycho-social vulnerabilities among the family members; It also underscores the potential benefits of preventive measures for the medical students with psychological problems and those found to be involved in problematic substance use.
Living away from the family and staying at hostels (as compared to staying with their families) was associated with an increase in substance use,19,25,27,28,72–74,80 a finding consistent with the previous research. 50 Staying away from the family has also been associated with heavy episodic drinking and increased severity of alcohol-related adverse consequences. 81 These findings can perhaps be understood in light of the loss of parental supervision in those staying at the hostels, perceived sense of freedom, and subsequent experimentation with the substances, compounded by need of socialization, peer pressure, and also a form of coping to deal with the stress of transiting from school to medical-college life. However, some studies found no correlation for the current place of residence.14,24,67,82
We also noted that use of alcohol was an associated factor for the initiation of other drugs (licit and illicit).18,21,22 This finding is in sync with available research on the “gateway drug” hypothesis. 83 Alcohol, because of its social acceptance, particularly in medical school, and easy availability, acts as a gateway drug for the substances that fall later in the substance use trajectories of an individual. Hence, it is prudent to identify students with problem (hazardous or harmful) alcohol use, so that these young medical students can be prevented from indulging in more harmful substance use.
Implications
The current review highlights that magnitude of SURP among Indian medical students is significant. Indeed, it has a profound impact on the academic performance and academic and professional career of this bright class of students.84–86 Moreover, the attitude of the medical students towards SURP does have a bearing on their approach to the patients with substance use or medical problems with comorbid substance use. Inadequate orientation of the medical students in their UG course about the bio-psycho-social model of mental illness and SUD, including the adverse effects of the psychoactive substances, can cause lack of understanding among them about SURP. This also results in an increased indulgence in substance use and low psychiatric help seeking when actually required. Therefore, they need to be sensitized about it early in their medical curricula; the medical curriculum emphasizing the bio-psycho-social model of SURP would be an important step in this direction (see Table 1). Further, the continuum of occasional substance use to harmful/hazardous use to dependence pattern, and its neurobiological underpinning, including the interaction of the substance use and mental health, should be part of their training in psychiatry. Such an approach would serve as an important health promotion and prevention strategy, especially for those who are early in their substance use trajectory. 87 Young health professionals need to play a vital role in curbing the menace of substance use (licit and illicit) in the society; hence, the mindset with which they take up the issue of substance use is important. These findings underscore an urgent need to establish student wellness centers/student support systems in medical schools across the country to promote a healthy lifestyle and address the issue of substance use and mental health. Lastly, more epidemiological studies on SURP among medical students need to be conducted with robust methodology, including longitudinal design, involving medical students from different geographical regions, of both genders, and from different stages of medical curriculum (freshers, students facing year backs, final year students, interns, etc.), and studying their relevant bio-psycho-social determinants. This could provide a clearer picture of the SURP among medical students, a finding that would be generalizable and guide the appropriate interventions.
The present review has some important limitations. First, we did not include BA (such as internet addiction, gambling disorder, etc.), despite it being an emerging problem among Indian students (nonmedical or medical). However, as the concept is still evolving and there is limited prevalence data on BA in medical UGs, the scope of the current review was restricted to substance-related addictive disorders; this also ensured homogeneity across the available literature on substance use in medical UGs. Second, we did not explore the magnitude of the psychiatric comorbidities in students involved in substance use, though these two conditions often co-exist and complicate the course of each other. Third, we explored only the prevalence of and associated factors for SURP, while the aspects of knowledge and attitude of the medical students towards substance use were not assessed. Lastly, our review was restricted to the medical UGs, while the magnitude of the SURP in the medical postgraduate and other allied health professionals and students was not assessed.
Conclusion
The magnitude of the SURP is worth a concern among the medical students. Alcohol is the most common substance of use in this population. However, a sizeable proportion of them is also involved in the use of tobacco and illicit drugs such as cannabis, opioids, stimulants, and nonprescription sedatives. Notably, there has been an increasing trend in substance use among female medical students, particularly of nonprescription sedatives. Family history of substance use, peer pressure, the transition from the school to college life and from home environment to hostel life, intrinsic stress of medical course, progression in the medical course, and use of other substances are the common factors associated with the initiation or maintenance of substance use. Sensitizing medical students and college authorities about the impact of substance use on the health and quality of life of students, increasing the hours of teaching and training in psychiatry (including on the identification and management of SURP), and establishing student wellness center in the college premises are the potential strategies to curtail these problems. There is a need for nationwide epidemiological studies and longitudinal studies to assess the magnitude of SURP and the associated factors among medical students.
Supplemental Material
Supplemental material for this article is available online.
Footnotes
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
