Abstract
Background:
Competency-based medical education (CBME) offers avenues for effective psychiatry teaching to medical students. However, data concerning the feasibility, effectiveness, and students’ perspectives on CBME-based clinical rotation, including psychiatry, needs to be explored in India. Therefore, this research aims to evaluate the student’s learning effectiveness and feedback on the CBME-informed psychiatry posting.
Methods:
This cross-sectional retrospective research evaluated the 7th-semester MBBS students (n = 101, 39 [38.6%] females and 62 [71.4%] males), from a tertiary-care teaching hospital in central India, perceived change in Knowledge, Attitude, and Skill and feedback on the CBME-based clinical rotation (July-December 2023) using a mixed-method approach through an online feedback form.
Results:
A “considerable or marked perceived change,” ranging from 70% to 97%, in the knowledge, attitude, ethical aspects, psychomotor skills, and soft skills were noted. 84%–91% of students were “satisfied/quite satisfied (or rated it good to very good)” with the pattern and content of the program, including the assessment. 37% expressed their desire to take psychiatry as an elective. Descriptive responses showed that participants felt improvement in their communication skills, knowledge about non-pharmacological interventions, opportunity to observe and present cases in the Outpatient Department, and satisfaction with the teaching and assessment methods. The need for minor changes regarding case-based formative assessment and the opportunity for more case workups were also cited.
Conclusion:
The CBME-informed psychiatry clinical rotation can be instrumental in improving psychiatry training and promoting mental health among students. Research involving a comparison arm, longitudinal design, and validated assessment tools can bring greater insights into the subject.
Keywords
It is feasible to deliver the CBME-based psychiatry clinical rotation to medical students; such rotations enhance their learning effectively. Such clinical posting must involve considerable patient exposure and case workup opportunities for medical students to meet their expectations and learning requirements. A team-based approach, including actively involving senior residents in enriching psychiatry training for medical students, is of paramount importance. The comparative longitudinal research using validated instruments should inform the outcome assessments of such teaching programs.Key Messages:
Acompetency-based medical education curriculum (CBME) was implemented in India in 2019. CBME emphasizes the attainment of competencies among the Indian Medical Graduates (IMGs) for performing their expected role of first contact with the patients. Unlike the traditional curriculum, which focuses on acquiring knowledge and a “know-how” approach, the CBME prioritizes a skill-based and learner-centric teaching approach and an “expertise and performance independently” approach. The latter also involves robust formative and summative assessment methods and adequate feedback mechanisms to enhance pupils’ learning.1,2
Including CBME in medical education, including in psychiatry, is crucial for developing the competencies of medical students. 1 However, this framework is relatively new for developing nations like India versus developed nations. 2 While positive outcomes have been reported in developed countries,2–4 CBME has also received criticism in these countries due to limited effectiveness evidence and some adverse outcomes.5,6 Data from developing countries is still sparse,7,8 highlighting the need for evidence generation and periodic assessment of CBME’s effectiveness and feasibility.
There has been a long-felt need to increase psychiatry exposure for undergraduates, especially given the role it can play in developing attitude, ethics, and communication (AETCOM) skills, ensuring holistic patient care, adopting biopsychosocial approaches to treatment, and developing appropriate legal and ethical mindsets while dealing with patients.9,10 Under CBME, psychiatry comprise 19 topics and 117 competencies, with an increase from 20 to 40 hours of lectures and 2–6 weeks of clinical rotations, reflecting the perceived usefulness of the psychiatry exposure in undergraduate training. 3 However, implementing CMBE in India (like other developing nations), that too in psychiatry, which is not a major subject, can be anticipated with inherent challenges, including a lack of educational infrastructure and trained psychiatry educators, negative attitudes toward psychiatry and mental health among students and administrators, low acceptance of psychiatry among medical teachers and students, and a lack of evidence-based assessment in psychiatry like EPA (The Entrustable Professional Activities) and Workplace-based assessment (WPBA).2,9
Traditionally, psychiatry exposure involves clinical rotation, didactic lectures, and assessments that primarily evaluate knowledge domain. Medical educators emphasize the importance of participatory and self-directed learning (SDL) to enhance professionalism, ethical considerations, attitude, and skill domains. Likewise, the formative assessment includes tapping all the domains of learning and simultaneously promoting their learning. Despite the adoption of CBME by many institutions, there needs to be more evidence from India on the effectiveness of the National Medical Commission’s (NMC) CBME in undergraduate medical education.
The Department of Psychiatry, All India Institute of Medical Sciences (AIIMS), Bhopal, has adopted a newer, CBME-based method of training medical students during their clinical rotations. It is prudent to explore how the newly adopted teaching-learning methods (T-L Methods) for training medical undergraduates in psychiatry during their clinical rotation, and competency-based objective assessment methods influence their learning. Additionally, we wanted to evaluate the strengths and limitations of such a clinical posting.
The overarching aim of this retrospective research is “To study the change in the knowledge, attitude, and skills (KAS) among the medical students, and analyze (both quantitatively and qualitatively) their feedback on newly adopted T-L Methods during the clinical orientation of medical undergraduates in psychiatry.” The objectives are to (a) highlight the CBME curriculum and T-L Methods used during students’ psychiatry rotation, (b) assess the perceived change in the KAS among the students following clinical rotations, and (c) evaluate feedback on newly implemented CBME-based clinical posting, including the formative assessment methods as a part of their ward leaving test (WLT).
Materials and Methods
For the current retrospective review article, we followed the REporting of studies Conducted using the Observationally Routinely Collected Health Data (RECORD) Statement. 4
Study Design and Setting
The present study involved a retrospective analysis of students’ feedback at the end of their 5-week clinical rotation in Psychiatry in a tertiary-care teaching hospital in central India, after institutional ethical committee clearance. The data was collected over one academic year (2023). The feedback was obtained on Google form after their formative assessment, that is, WLT.
Participants
All the 7th-semester students (MBBS batch 2020) who attended the psychiatry rotation and the WLT (July-December 2023) were invited to fill out a feedback form as part of the department’s routine academic exercise. Students who didn’t fill out the feedback form were naturally excluded from the study.
Students were free to provide (or not provide) their feedback after finishing their clinical posting in psychiatry, with the provision of anonymity, confidentiality, and their participation (or non-participation) having any bearing on their assessment. Importantly, an exemption of consent was obtained from the institute’s human ethics committee (Project ID IM23004) as this research was envisaged after the completion of data collection.
Data Collection Process
A Google form was developed by the investigators (faculty members: SG & AP; and senior residenrs (AK & JJ)) involved in undergraduate psychiatry teaching (attached below).
The students were posted in the Department of Psychiatry in batches of 20–25, and the total strength of students was 124; however, 115 students appeared for the WLT (93%). Their perspectives on the posting were analyzed both quantitatively and qualitatively. The form also explored perceived change in their KAS and ethical considerations while dealing with patients or their caregivers.
The feedback questionnaire involved 11 items with a Likert scoring (e.g., How would you rate change in your knowledge in psychiatry/mental health following this posting? With options marked/considerable/slightly/no change). Additionally, it contained five items that solicited descriptive responses from the participants (e.g., What more can be done to improve the quality and content of clinical training?).
It must be underscored here that the feedback proforma was filled out before the results of the WLT were declared to prevent biased responses or socially desirable responses from the students.
Description of the Psychiatry Posting
The clinical posting involves different phases, incorporating various critical components to enhance student’s learning. Typically, it begins with an orientation session by the undergraduate course coordinator (SG) (details in Table 1) followed by classes on clinical psychiatry, such as history taking and demonstration, psychological assessment, and interventions. The subsequent classes are interspersed with routine Outpatient Department (OPD) and ward postings.
Description of the Psychiatry Clinical Rotation for the Undergraduates.
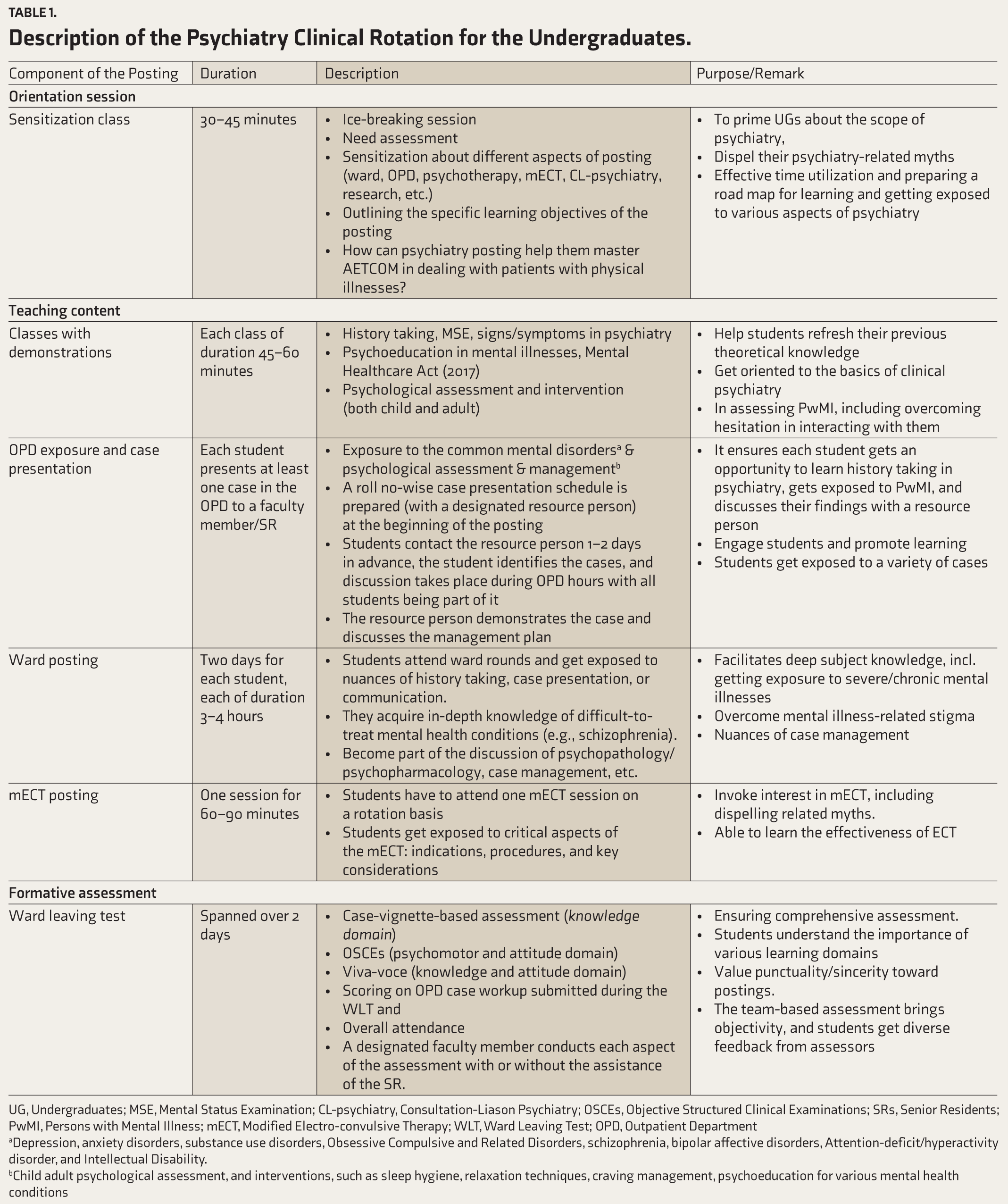
UG, Undergraduates; MSE, Mental Status Examination; CL-psychiatry, Consultation-Liason Psychiatry; OSCEs, Objective Structured Clinical Examinations; SRs, Senior Residents; PwMI, Persons with Mental Illness; mECT, Modified Electro-convulsive Therapy; WLT, Ward Leaving Test; OPD, Outpatient Department
aDepression, anxiety disorders, substance use disorders, Obsessive Compulsive and Related Disorders, schizophrenia, bipolar affective disorders, Attention-deficit/hyperactivity disorder, and Intellectual Disability.
bChild adult psychological assessment, and interventions, such as sleep hygiene, relaxation techniques, craving management, psychoeducation for various mental health conditions
In the OPD, students get exposed to common mental health conditions (depression, anxiety disorders, substance use disorders, etc.) and their management (including basics of psychopharmacology, psychoeducation for Lithium/clozapine, behavioral interventions, etc.). They also attend psychotherapy sessions/psychological assessments with clinical psychologists and have to present OPD cases to the faculty members/SRs, with case discussion and demonstrations, which also carry marks during the WLT.
Students are also mandated to attend the ward rounds and modified Electroconvulsive Therapy (mECT) sessions. They are encouraged to attend departmental academics, particularly case conferences, sessions like movie clubs, or book reviews.
Attendance is a key tenet of their psychiatry posting. It also carries marks in the WLT, which contribute to their internal marks in the summative assessment under the general medicine subject.
To elaborate, the formative assessment in the form of the WLT targets all learning domains: knowledge, attitude, and psychomotor. Additionally, it assesses punctuality through attendance, and AETCOM (Objective Structured Clinical Exam [OSCE] involves demonstrating these skills). The case vignettes and viva-voce assess knowledge, while OSCEs (also viva-voce) assess psychomotor and attitude domains (details in Table 1). The assessment is conducted over 2 days involving a team of four faculty members and two SRs. Each part of the assessment is performed by a designated faculty with or without the assistance of the SRs to maintain homogeneity in assessment and to ensure feedback is provided to the students. The latter also ensured objectivity in the assessment and provided students with opportunities to obtain diverse input from the assessors.
The posting concludes with student feedback on their clinical rotation experience, learnings, and the characteristics (format and content) of the posting (details of the psychiatry rotations provided in Supplementary File 1).
Statistical Analysis
The responses were extracted in a spreadsheet embedded with the Google form. AK performed the data cleaning in consultation with the SG. The data was represented using descriptive statistics; the mean (Standard Deviation) or median (Interquartile Range) was used for continuous variables. Categorical data was represented in terms of frequency (%). The statistical analysis was performed using Microsoft Excel.
Descriptive responses were presented in terms of common themes that had emerged. Two independent co-investigators (DB and AK) manually conducted the qualitative analysis. Themes and sub-themes were generated and categorized for interpretation. Since all the items in the feedback were mandatory to fill by the students; therefore, we did not face challenges with missing data and its management.
Results
Out of 115 students who appeared for the WLT, 101 (87.8%) students filled out the feedback form, comprising 39 (38.6%) females and 62 males. The findings are outlined below.
Perceived Change in the Knowledge, AETCOM, and Skills Among the Students
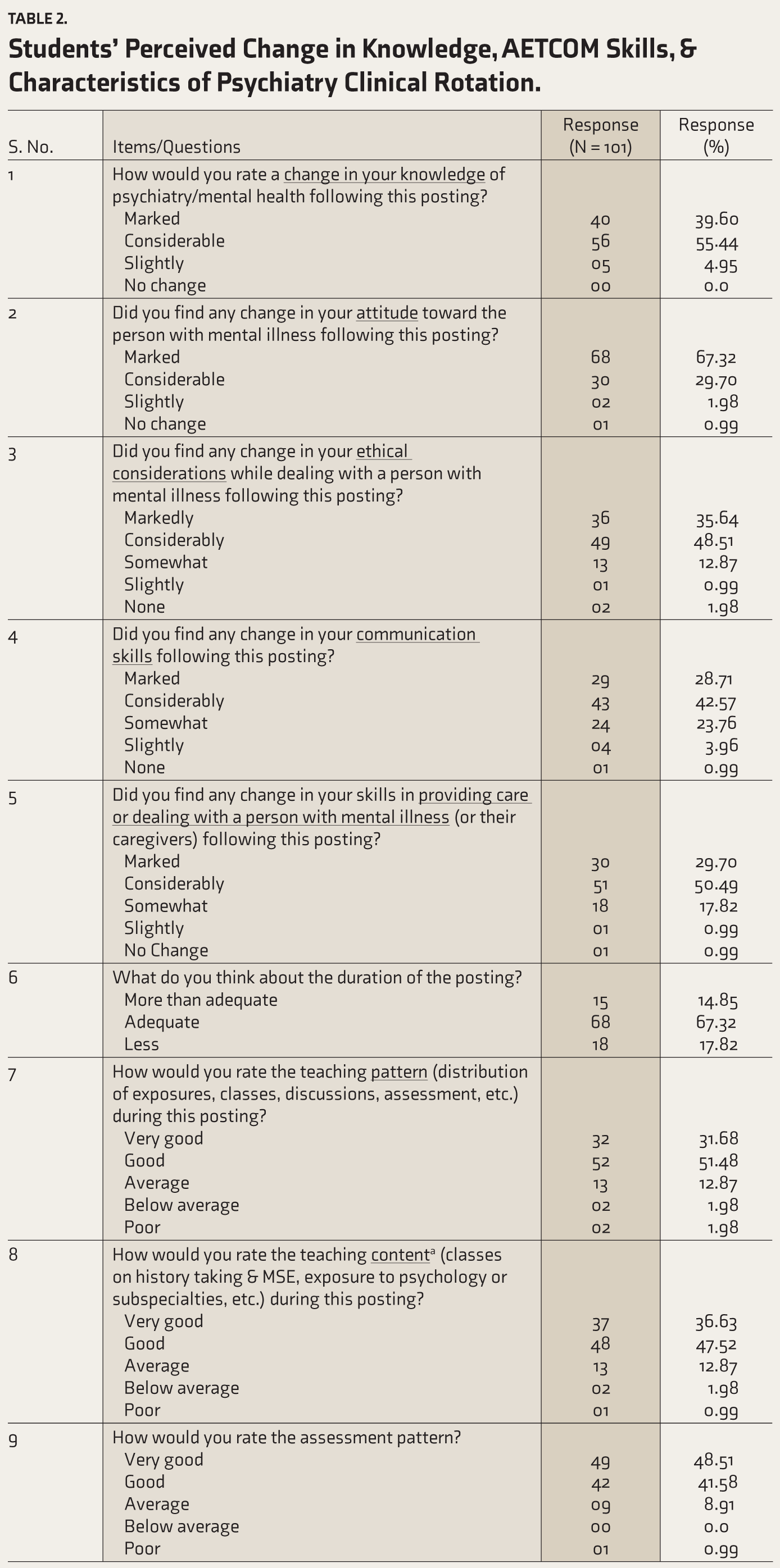
Ninety-six (95%) of students perceived a ‘marked or considerable’ change in their knowledge of psychiatry following the posting (Table 2). A vast majority of the students (n = 81, 80%) experienced a (significant) change in their skillset in delivering psychiatric treatment (or providing care) to patients and their caregivers.
Almost all felt a considerable change in their attitude toward Persons with Mental Illness (PwMI) (n = 100, 99%), including around two-thirds (n = 68) who perceived a ‘marked change’. Similarly, a vast majority of them (n = 99, 98%) felt a change in ethical considerations (e.g., respecting patients’ rights and ensuring confidentiality) while dealing with PwMI, with about one-third and half finding a ‘marked and considerable’ change, respectively. It was also found that almost all perceived a change in the way they would interact and communicate with patients or their caregivers, with 70% of students reporting a ‘marked (n = 29, 29%) or considerable change’ (n = 43, 43%).
Students’ Perceived Change in Knowledge, AETCOM Skills, & Characteristics of Psychiatry Clinical Rotation.
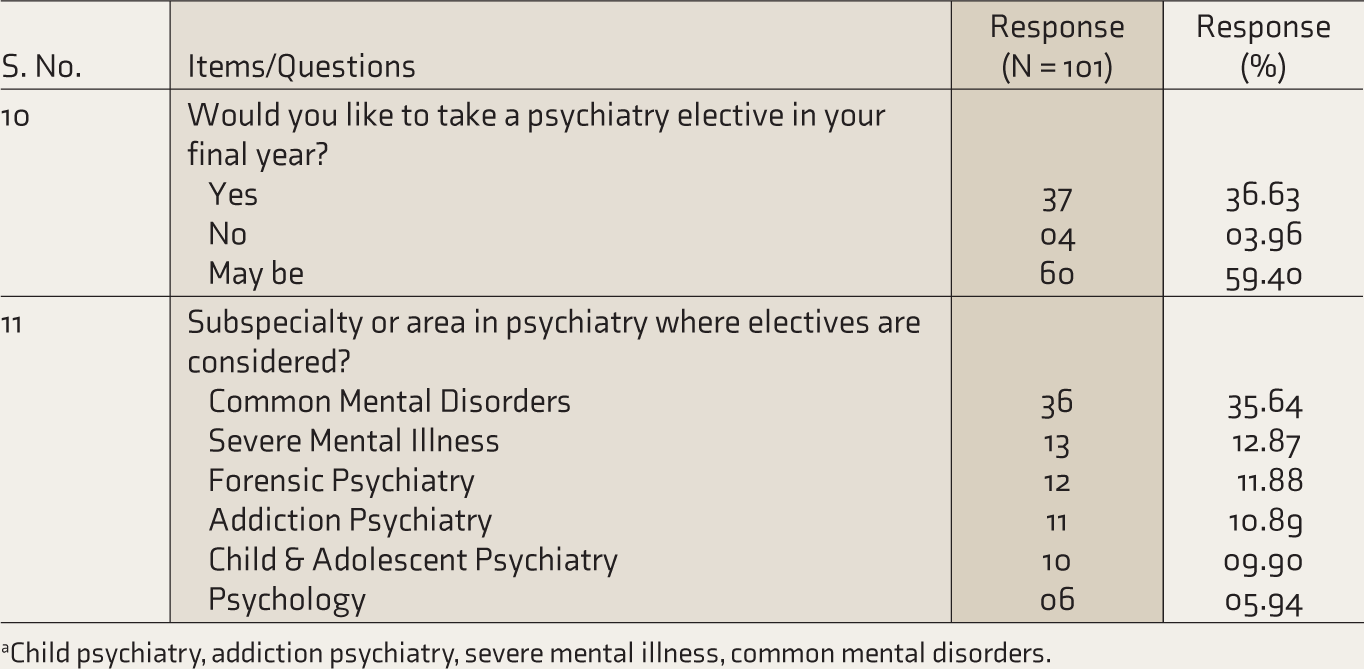
aChild psychiatry, addiction psychiatry, severe mental illness, common mental disorders.
Responses of the Participants on the Characteristics of Clinical Rotation in Psychiatry
Eighty-two (82%) and Eighteen (18%) of students, respectively, expressed that the duration of posting was adequate (more than adequate) and less than what is required.
Concerning the pattern of the T-L approach (rotation, case distribution in the OPD, timing, and pattern of classes), a total of around 83% (n = 84) of students were quite satisfied and rated them as very good (n = 32, 32%), or good (n = 52, 52%). A similar pattern was observed in terms of the content of the T-L framework (like classes on history taking, Mental Status Examination [MSE], exposure to specialty clinics, and psychology), with 84% (n = 85) rating it as very good/good. Notably, 90% (n = 91) rated the pattern and content of the assessment (i.e., WLT) as good/very good.
Preference for Psychiatry Elective in the Future
In the end, more than one-third of students (n = 37, 37%) expressed a “clear desire” to opt for a psychiatry elective in their final year, while around 59% (n = 60) reported that they “may consider” it as an elective. In students’ responses to which psychiatry subspecialty or area they would consider as an elective in the final year, the majority expressed interest in common mental disorders (n = 36), followed by forensic psychiatry (n = 12) and addiction medicine (n = 11. Few students expressed their interest in severe mental illness and child psychiatry (n = 10 each) and psychology (n = 6).
Thematic Analysis of Students’ Responses to Descriptive Questions
Based on students‘ responses to the descriptive items, common themes were generated (through manual coding). The themes of various inquiries made are provided below.
Learning(s) beyond changes in KAS:
Students mentioned perceived improvements in their “clinical, communication, and history-taking skills.” They appreciated that the latter skills would help them improve their clinical skills not only in psychiatry but also in other specialties (e.g., internal medicine and surgery). Another common theme that emerged was “learning how to establish rapport with PwMI,” which will help them become better clinicians.
Another recurrent theme was “learning psychoeducation and non-pharmacological management strategies” for various mental health conditions, which are usually ignored during training in other specialties (e.g., internal medicine, maybe because of time constraints). Few students also felt an “improvement in their soft skills/professional attributes”, such as being more confident, patient, and disciplined. One student each reported a “reduction in stigma related to psychiatry” and learning “the importance of psychiatry” as a specialty.
Most liked part of the teaching pattern:
Students consistently reported that they “liked the OPD posting the most,” including how to evaluate psychiatry cases and the myriad presentations of psychiatric conditions presented to the OPD. Most students responded that SRs and faculty members in the OPD taught them the nuances and brief about establishing the diagnosis and management of the cases. All students felt that “this exposure instilled confidence in them.”
Some students also reported enjoying OPD posting as they could learn in a limited/short time how to approach a patient with a psychiatric disorder. One student interestingly replied, “We got to learn about such varied aspects of human nature and behavior, at the same time trying to understand how even slight variations might lead to multiple problems, some bigger ones that require an in-depth analysis to correct or improve issues.”
Notably, a few students also liked the ward rounds, where the ward cases were discussed in detail and interviewed in front of them. Few students reported liking the pattern of assessment and classes by SRs.
Part of the teaching requiring improvement:
Most students iterated that it would have been good if they had had opportunities to “present more cases to the faculty and senior residents” in the OPD or ward. Few also reported that more theory/clinical classes, especially separate classes for MSE by SRs, can be included. Notably, most students mentioned being “satisfied with the teaching and training”; not many changes/modifications are required.
Steps to improve the quality and content of clinical training:
Overall, students expressed a desire to “interact more with PwMI.” They also reported the need for “more case presentations, active involvement in the discussion” about the case with SR/Faculty, and case-based teaching (phenomenology, diagnosis, and management, including psychopharmacology). Most of the students recommended that there should have been “more days for OPD postings,” where they tend to see a variety of cases. In contrast, few students endorsed the need for more ward postings, where in-depth discussions of difficult-to-treat cases are usually discussed.
Furthermore, another key theme was the need for “more exposure to psychotherapy” sessions so that they could learn the practical aspects of such therapies. A few students also reported that the timing of posting should be increased as there was so much more to learn and more skills to acquire, as well as more research-oriented OPD exposure of cases (rare cases). As they often felt there was less time to discuss cases in OPD due to the increasing patient load on SR/faculty, the number of available doctors should be more. Importantly, one of the students highlighted that “instead of a single-time assessment, there should be a weekly formative assessment so that they feel motivated to study each day.” Notably, a significant number of students reported that the content of teaching was adequate to excellent and suggested no points to be improved.
Steps to improve the quality and content of clinical assessment:
Most students were satisfied with the “methods and quality of clinical assessment” and replied that “no change” was required. However, some students suggested some scope for improvement; the common themes that emerged were “more number real patients/simulatory cases” for history taking, “examination and presentation during the assessment” to demonstrate their communication and interaction with them. Similarly, a few students also replied that the assessment should be a more practical and skill-based approach that is less of a theory-based question/Multiple-Choice Questions (MCQ) and more of real patients/simulator-based or OSCE/Objective Structural Practical Examination (OSPE)-based assessments and fewer theory-based questions. One student replied that there should be MCQ exams every week during the posting. Few other students reported that there should be “more numbers of case-based OCSEs and more time” to assess cases in OSCEs.
Discussion
This retrospective research assessed the feasibility and effectiveness of CBME-based clinical posting on knowledge, AETCOM skills, and clinical skills among medical students. Additionally, it delved into the students’ feedback on the pattern, content, and delivery of these teaching modules so that timely course correction can be done; we followed an iterative approach to improve the content and quality of psychiatry training based on (batch-wise) students’ continual feedback.
This is pioneering work in undergraduate psychiatry training in India. The strength of the research lies in consistency in its execution across the 7th-semester medical students. The survey comprised a change in KAS in psychiatry coupled with bi-directional feedback, a crucial tenet of the CBME. A response rate of >85% adds to the validity and reliability of the findings.
We found that there was a “considerable or marked perceived change” in the KAS and ethical aspects among the students, ranging from 70% to 97%, following the CBME-based clinical rotation in psychiatry. Furthermore, there was positive feedback on the rotational program, with 84%–91% of students being “satisfied/quite satisfied (or rated it good to very good)” with the pattern and content of the program, including the assessment.
Ninety-five (95%) of the students perceived a “considerable or marked change” in their knowledge of psychiatry and mental health. These findings align with previous literature, which has also reported improvement in psychiatry-related knowledge among undergraduates after clinical posting in psychiatry.12–15 Our quantitative finding in this regard was supported by the qualitative data, wherein one of the common themes was that “students learned not only the basic aspects of mental disorders and their pharmacological management but also the various non-pharmacological interventions (e.g., psychoeducation, cognitive-behavioral therapy) and the significance of involving caregivers in the treatment process.” However, we did not explicitly enquire about which areas students’ knowledge changed substantially and which areas they still lack. Future research must delve into the nuances of students’ knowledge changes that follow psychiatry rotations.
We found that >95% of the students felt “considerable or marked (positive) attitudinal change” toward the PwMI after the posting. Again, this finding is consistent with the available literature.13,15,16 Our qualitative data substantiated these quantitative findings, wherein students reported that following the posting, they “learned about key professional attributes, the significance of psychiatry as a discipline and a reduction in stigma toward PwMI or psychiatry as a discipline.” These findings suggest that students following the clinical posting found psychiatry a relatable and relevant subject. The latter findings also concur with the literature on psychiatry-related stigma among medical students and health professionals; exposure to PwMI has the greatest effect on people’s attitudes toward psychiatric patients or psychiatric disorders. 17 The same applies to medical undergraduates who become more empathetic or sensitive in their careers toward the needs of the patients/caregivers. 18 This finding is critical as research also shows that a knowledge change may not translate into attitudinal change. 14
Desai et al., based on their observations from Western India, pointed out that a well-established psychiatry department and exposure to community mental health bring about a positive attitudinal change among the students toward psychiatry. 14 Our program and active involvement of department resource persons in imparting psychiatry training might have significantly influenced the above positive results. Again, more granular evaluation, including robust qualitative research and behavioral manifestations of the perceived attitudinal changes among the students following the psychiatry rotation, is warranted in this regard.
We noticed that 85% and 70% of students felt that their ethical considerations while dealing with PwMI and communication skills have “changed markedly or considerably” after the posting. These findings are noteworthy considering NMC’s huge emphasis on AETCOM as a key tenet of medical education and the requisite qualities of the IMGs (communicator and professional). Communication is vital in psychiatry, as well as in history elicitation, rapport building with the patients, psychoeducation about the illness, engaging patients/caregivers in treatment, and working in a team. Our finding is important given that the literature indicates that the training for communication skills in psychiatry is often relaxed during undergraduate training. This may affect patients’ quality of care, esp. if encountered by a general physician (GP) with no formal psychiatry training. 19 For instance, Stensrud et al., 5 in their study among GPs, found that GPs need communication skills in consultations with PwMI. Changes in the ethical consideration post-clinical rotation reflect students’ perception of psychiatry posting, making them aware of such ethical issues. Psychiatry posting can be a useful tool to orient students in ethics in the medical profession (autonomy, beneficence, non-maleficence, justice, and confidentiality), and it can be effectively practiced. However, ethical consideration, including instances around it, did not come as a prominent theme during qualitative analysis. It must be underscored that we also could not find any previous literature on medical undergraduates that has assessed the effect of psychiatry posting on their ethical considerations, highlighting the need for more research in this area.
About 80% of students felt that their skills in dealing with PwMI or their caregivers “changed considerably or markedly” after the posting in this study. This finding is critical given the huge burden of mental illness in the community, including on college campuses, and mental illness is common in persons with physical illness. Literature suggests that lack of psychiatry-related knowledge and skills among medical students results in poor identification of mental health issues among patients, improper management of common psychological issues (such as insomnia, anxiety, stress, alcohol, or tobacco-related problems), including among those with physical illnesses, and psychiatry-related stigma.18,21,22 Skills learned during psychiatry posting can help students better manage/timely refer clients with physical illness and mental health problems.
More than two-thirds of students felt that the duration of the psychiatry posting was adequate. This finding is critical given that existing research has yet to delve into students’ perspectives on the elevated duration of psychiatry exposure as per the NMC’s new CBME curriculum. However, they have reported that at least 4 weeks are required to bring about a significant attitudinal change among students.23,24 Interestingly, one in five students perceived that the 5-week duration may further be increased to have enough exposure to psychiatry. The latter finding can be attributed to our institutes’ provision of only a single clinical rotation in psychiatry during the entire MBBS; moreover, it may be possible that few students were positively biased or inclined toward psychiatry, hence wishing for greater posting duration.
In contrast, about 15% of students felt that the duration of psychiatry posting was more than adequate and could be reduced. The probable reasons could be to have minimal exposure to psychiatry and focus on other major subjects with more weightage in summative exams or entrance exams.25–28 Additionally, a single 5 weeks clinical rotation in psychiatry might have been overwhelming for a few students; the latter finding informs us that maybe the 5-week posting can be divided into two or three briefer postings scattered along the entire MBBS course.
In our study, we found that more than 80% of students rated the pattern and content of the posting as “good or very good.” This indicates that NMC’s CBME curriculum, which focuses on early clinical exposure, student-centric, and skill-based training coupled with greater engagement of students, provision of robust assessment methods, and feedback, is welcomed by students. Qualitative analysis of our research data informed us that students liked the clinical exposure, especially during the OPDs, and appreciated the opportunity given to them to actively interact with the patients, take case histories, and discuss them with the faculty/SRs. This may be because the cases of OPD predominantly are less severe; therefore, students could engage with and talk to them easily. Every day, one to two cases would be allotted to students, and they would independently evaluate the patients and present them to faculty/SRs in the OPD. Moreover, the students preferred practical-based assessment methods. Previous studies on students’ satisfaction with psychiatry teaching have revealed that they are usually unsatisfied with theoretical psychiatry teaching.22,29 In contrast, more practical teaching, greater interaction with the PwMI, the opportunity to see a variety of cases, and exposure to various psychiatric subspecialties, including learning psychotherapy, improve students’ attitudes and interest in psychiatry.18,25,30–32
Our program could bridge the gap between the student’s learning needs and what is typically or traditionally being offered to them in medical schools, thereby getting students positive feedback. However, these subjective reports should be considered considering the students’ tendency to provide socially desirable answers, especially when they fear that they might be judged by the teachers based on their feedback. Notably, to overcome the latter issues, we obtained the online feedback anonymously once their assessments were over.
The present study reveals that 91% of students found the assessment method to be “very good or good.” This can be attributed to the structure of the assessment involving OSCEs, case-based assessment, viva-voce, case presentation, and attendance, which was communicated to the students at the very beginning of their postings; moreover, marking on attendance and case presentation might have encouraged those students who were punctual toward clinical posting. Literature shows that traditional ways of assessment, such as MCQs-based, short-notes, or focused viva, have shown poor responses from the students and an overall negative attitude toward psychiatry or other subjects’ clinical rotations.25,33 The positive regard for our way of assessment also emerged as a major theme during the qualitative data analysis; the chance of students giving socially appropriate answers cannot be denied.
Interestingly, 37% expressed their desire to take psychiatry as an elective, whereas about 60% of them were unsure about it, and an abysmal proportion of students (4%) replied in negation. This finding is crucial given that most of the students liked the pattern and content of teaching and assessment and reported a significant change in their KAS following this posting, despite that they were still deciding about opting for psychiatry electives. This may be because many students do not consider psychiatry as a career option and want to focus on other subjects of their choice, or they consider the 5-weeks posting is enough and want to focus on other subjects.31,34,35 The associated factors may be inherent interest in other subjects, perceived better career opportunities in those disciplines, low quality of teaching in psychiatry, inadequate exposure, or stigma toward psychiatry.35,36 This again indicates that the students could give their responses unbiasedly and were not actually giving a socially desirable response.
Literature shows that knowledge and skill change following psychiatry rotation does not correlate linearly with an attitudinal change toward psychiatry among medical students. For instance, Anna et al. 14 reported that despite holding a positive attitude toward psychiatry, only 1/4th of students are ready to consider psychiatry as a career option. Our study found that about 1/3rd of students desired to choose psychiatry as an elective, which may lower down considering it as a career branch. This means that poor career choice in psychiatry persists despite their perceived changes in knowledge, attitude, etc. This informs us that to address the shortage of psychiatrists, the students’ feedback must be taken with due diligence, and appropriate course corrections must be made to motivate students to consider psychiatry as a career. However, we should have actively encouraged students to take psychiatry as an elective or a career. Clinical rotation could be a vital vantage point to orient them about the scope of psychiatry and how it can be professionally rewarding. More research, particularly of a qualitative and longitudinal nature, is needed to explore this phenomenon.
The review had some key limitations. First, as this was a cross-sectional and retrospective study, we cannot comment on the long-term effectiveness of our CBME-based clinical posting program. The students’ positive perceptions of psychiatry may be transient. Second, the study involved data collection based on self-report; moreover, the survey questionnaire needed to be validated; hence, there is an inherent risk of bias on the part of students, and the reliability and accuracy of some of the responses can be doubted. Third, there is a risk of social desirability in students’ responses; we tried to circumvent this potential bias by making feedback responses optional and anonymous and only collecting them following the formative assessments. Fourth, we did not obtain the participants’ baseline data to compare the actual change in KAS following our clinical rotation module; also, there needed to be a control group with which to compare the results. A comparison group may be chosen from a different institute with different curricula in future studies. In this way, the effect of change in the perception of students can be more strongly attributed to different aspects of the curriculum. Fifth, the current module of the program, which comprises different CBME modules, was designed by our department’s faculties based on our resources and teachers’ motivation; it needed to be externally validated, which may limit its generalizability. Lastly, the enthusiasm of the educators or their extra efforts might have indirectly influenced the findings of the study and may not be replicated in other institutes.
Conclusion
The current study highlights the substantial perceived change in the KAS of the students following the CBME-based clinical rotation coupled with positive feedback toward the formative assessment method. Moreover, students were inclined toward taking psychiatry electives. Qualitative analyses revealed that students endorsed greater interactions with patients and case presentations to the resource persons. Similarly, a need to learn some basic psychological interventions came prominently. The current research findings should be considered considering single-arm, cross-sectional study design and subjective change in the KAS in psychiatry. More research with sound methodology will help overcome some of the present study’s limitations and bring greater insights into the psychiatry teaching-learning under CBME.
Supplemental Material
Supplemental material for this article is available online.
Footnotes
Acknowledgements
We would like to extend our thanks to other faculty members (Professor Dr Vijender Singh, Dr Abhijit R. Rozatkar, and Dr Roshan F. Sutar) and senior residents (Dr Komal Kohat and Dr Bhavika Rai) of the Department of Psychiatry for supporting us in the effective implementation of the CBME-based clinical rotation in Psychiatry.
Data Availability Statement
The data of the current research can be obtained from the corresponding author upon making a reasonable request.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest regarding the research, authorship, and/or publication of this article.
Declaration Regarding the Use of Generative AI
No AI tools were used for data analysis and manuscript preparation. Authors assume full responsibility for the entire content of the manuscript.
Ethical Approval
An ethical approval and exemption of participants’ consent was provided by the Institute Human Ethics Committee of All India Institute of Medical Sciences, Bhopal (Project ID IM23004) as this this was a retrospective study.
Funding
The authors received no financial support for this article’s research, authorship, and/or publication.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
