Abstract
Background:
The mechanism of sudden sensorineural hearing loss (SSNHL) remains incompletely understood, but immune cell infiltration has been identified as a crucial component in the sickness. The patients with SSNHL may benefit from investigating markers related to inflammation.
Methods:
From April 2022 to 2023, 80 patients who were diagnosed with SSNHL in the Department of Otolaryngology at Yangzhou University’s Clinical Medical College were enrolled in the SSNHL group. And patients were separated into effective and ineffective groups based on the degree to which their hearing had recovered prior to discharge. As the control group, 80 healthy volunteers were chosen from hospital’s physical examination center. Neutrophils, lymphocytes, platelets, and white blood cells were counted. Additionally, quantified and statistically examined were the neutrophil-to-lymphocyte ratio (NLR), platelet-to-lymphocyte ratio (PLR), and systemic immune inflammation index (SII). The risk variables for prognosis were identified using logistic regression models, and the prediction accuracy of the model was calculated using the receiver operating characteristic (ROC) curves.
Results:
The SSNHL group had higher levels of white blood cells, neutrophils, platelets, NLR, PLR, and SII than the control group. While the PLR lacked statistical significance, the NLR and SII of the patients in the ineffective group were noticeably higher than those in the effective group.
Conclusion:
Patients with SSNHL exhibit inflammatory immune responses. Patients with SSNHL can have their prognosis determined by the simple peripheral blood indicators NLR and SII, particularly SII, which is significant for predicting prognosis and directing treatment.
Keywords
Introduction
A sudden, unexplained sensorineural hearing loss (SSNHL), commonly referred to as sudden deafness (SD), is defined as one that happens within 72 hours and is accompanied by a drop in at least 3 adjacent frequencies and a hearing loss of 30 dB or more. 1 The annual incidence rate of SSNHL has been continuously growing over the past decades in countries, including China, United States, Japan, and Germany.2 -5 The incidence is rising mainly due to the aging society, increasing chronic disease prevalence, advanced industrialization and urbanization, increased disease awareness, and increased environmental noise. 6 The high disability rate and large growth in incidence rate result in a significant challenge to global health.
Although the etiology and pathophysiology of SSNHL are less clear, it is generally accepted that viral infections, vascular conditions, and autoimmune illnesses are connected to the condition. 7 The significance of chronic inflammation in the pathophysiology of SSNHL has come to light recently with the idea of abnormal activation of cellular stress pathways being put forth. 8 Autoimmune sensorineural hearing loss was first described by McCabe in 1979 as spontaneous bilateral hearing loss that progresses over weeks or months and is responsive to therapy with glucocorticoids and immunosuppressive drugs. 9 Because immunosuppressive medication is beneficial, it is assumed that an immunological mechanism may mediate the condition, but since a biopsy of the human inner ear cannot be done, there is no direct evidence to support this theory. Nevertheless, immune-mediated or inflammatory-mediated hearing loss is starting to get a lot of attention.
Neutrophil-to-lymphocyte ratio (NLR) and platelet-to-lymphocyte ratio (PLR) have both been utilized as indicators of inflammation in the previous studies. 10 Additionally, a new indication for forecasting patient inflammation as well as immunological and thrombotic state is the systemic immune inflammation index (SII). 11 In routine blood testing, the predictive value of this index has been confirmed. For cardiovascular disorders such as heart failure, myocarditis, coronary artery disease, acute coronary syndrome, and acute anterior myocardial infarction, it is a potent and independent predictive factor.12 -15 Neutrophils (N), platelets (P), and lymphocytes (L) are the components of the SII calculation formula. 11 Increased neutrophils are a reflection of inflammation increased platelets are a reflection of thrombosis; and increased lymphocytes are a reflection of stress response in SII. 16 Through this study, we investigated the relationship between NLR, PLR, or SII levels and SSNHL, and explored the function of the 3 markers in the prognosis of SSNHL.
Materials and Methods
Study Populations
This retrospective analysis comprised 80 SSNHL patients in SSNHL group who received care at Yangzhou University’s Clinical Medical College between April 2022 and 2023. Eighty healthy volunteers were chosen from hospital’s physical examination center to serve as the control group. According to the Chinese medical association’s guidelines for diagnosis and treatment of SD, 17 a set of inclusion and exclusion criteria was established for our analysis. No prior use of steroid medication, unilateral SSNHL, and the exclusion of hearing loss brought on by organic lesions that were verified by magnetic resonance imaging were the inclusion criteria. Acute or chronic renal failure, diabetes, hypertension, hyperlipidemia, coronary heart disease, chronic liver disease, lung disease, infectious disease, immune disease, and any ear disease (such as chronic otitis media, otosclerosis, history of ear trauma, and Meniere’s disease), vestibular schwannoma, or traumatic lymphatic fistula were exclusion criteria. The Yangzhou University Clinical Medical College’s Ethics Review Committee granted approval for this study, which was carried out in accordance with the Helsinki Declaration (approval number: 2023ky052).
Gathering Samples for the Index Test
Prior to therapy, peripheral blood samples from each participant were taken. After 7 to 10 days of treatment, a standard blood cell assay was carried out. The samples were collected after the individuals’ 8-hour fast, which was about 7 a.m. Neutrophils (N), lymphocytes (L), platelets (P), and peripheral white blood cells (absolute counts) were collected, and the NLR, PLR, and SII values were computed for each case. The formula N × P/L was used to get the baseline SII level. 11
Analytical Hearing Test
All 80 SSNHL patients underwent pure-tone audiometry (PTA) both before and after therapy. Bone and air conduction thresholds were measured at frequencies of 250, 500, 1000, 2000, 4000, and 8000 Hz. The therapeutic outcomes were classified into cure, significantly effective, effective, and ineffective according to the efficacy evaluation criteria of the Chinese medical association’s guidelines for diagnosis and treatment of SD. 16 In the event of a cure, the average hearing threshold of the damaged frequency is totally recovered. A significantly effective treatment raises the average hearing threshold of the damaged frequency by 30 dB on average. An average increase of more than 15 to 30 dB in impaired frequency hearing is considered effective treatment. Impaired frequency of hearing with an average improvement of less than 15 dB is considered ineffective treatment. 17 The “effective group” consisted of patients who were cured, significantly effective, or effective. The “ineffective group” consisted of patients with an “ineffective” outcome. 17
Interventions and Dosage
The following protocol was used to treat the 80 SSNHL patients, 5 mg of dexamethasone was injected every other day for 3 times into the tympanic cavity of the afflicted ear. Methylprednisolone and neurotrophic medications (Ginaton) were given intravenously at doses of 40 or 70 mg for 7 to 10 days, respectively.
Statistical Procedures
Statistical Package for the Social Sciences (SPSS) 22.0 was utilized for the statistical evaluation. The Chi-square test was used to analyze count data, which were presented as n (%). Using the Kolmogorov–Smirnov test, the normality of measurement data was evaluated. If the data were regularly distributed, the means and standard deviations were expressed and the student’s t-test was used to analyze them. To determine the variables influencing therapy efficacy, multivariate logistic regression analysis was utilized. To examine the predictive value of factors for treatment effectiveness, receiver operating characteristic (ROC) curves were created, and the area under the ROC curves (AUC) was determined. The 2-tailed significance level was set at .05.
Results
Comparison of Clinical Data Between SSNHL Group and Control Group
Although age, gender, and lymphocyte counts did not differ substantially (P > .05) between the 2 groups, statistically significant differences (P < .05) were found between the SSNHL group and the control group in the levels of white blood cells (8.31 ± 1.76 vs 5.66 ± 1.54), neutrophils (5.69 ± 2.31 vs 3.67 ± 1.05), platelets (247.41 ± 53.39 vs 215.42 ± 53.21), NLR (3.97 ± 2.38 vs 2.21 ± 0.94), PLR (140.96 ± 61.11 vs 117.30 ± 42.68), and SII (823.03 ± 348.40 vs 423.74 ± 186.48) (Table 1).
Comparison of Clinical Data Between the 2 Groups.
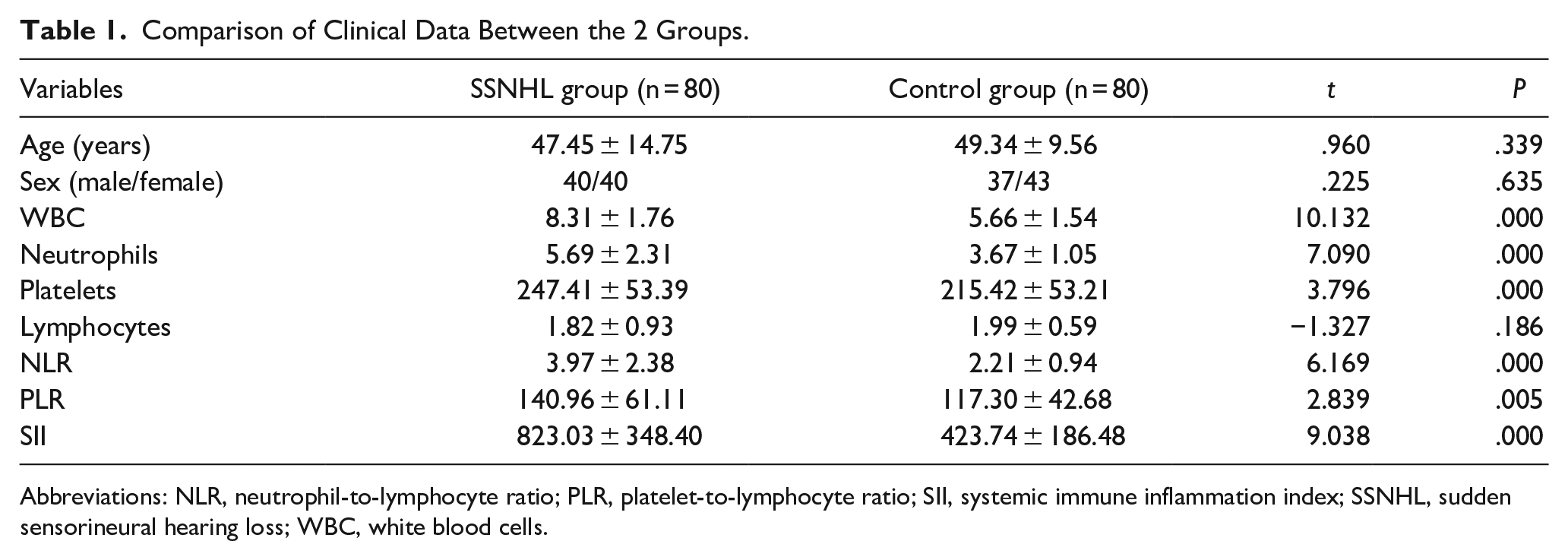
Abbreviations: NLR, neutrophil-to-lymphocyte ratio; PLR, platelet-to-lymphocyte ratio; SII, systemic immune inflammation index; SSNHL, sudden sensorineural hearing loss; WBC, white blood cells.
Comparison of Clinical Data From Patients With Different Efficacy
No significant difference was found in age, gender, white blood cells, neutrophils, platelets, or PLR between effective group and ineffective group (P > .05). While the NLR (3.39 ± 1.71 vs 4.85 ± 2.95) and SII (693.13 ± 217.29 vs 1017.87 ± 415.24) levels were lower in the effective group than in the ineffective group, the lymphocyte levels (1.99 ± 1.08 vs 1.57 ± 0.56) were higher in the effective group than in the ineffective group (P < .05) (Table 2).
Comparison of Clinical Data of the Patients With Different Therapeutic Effects in the Sudden Deafness Group.
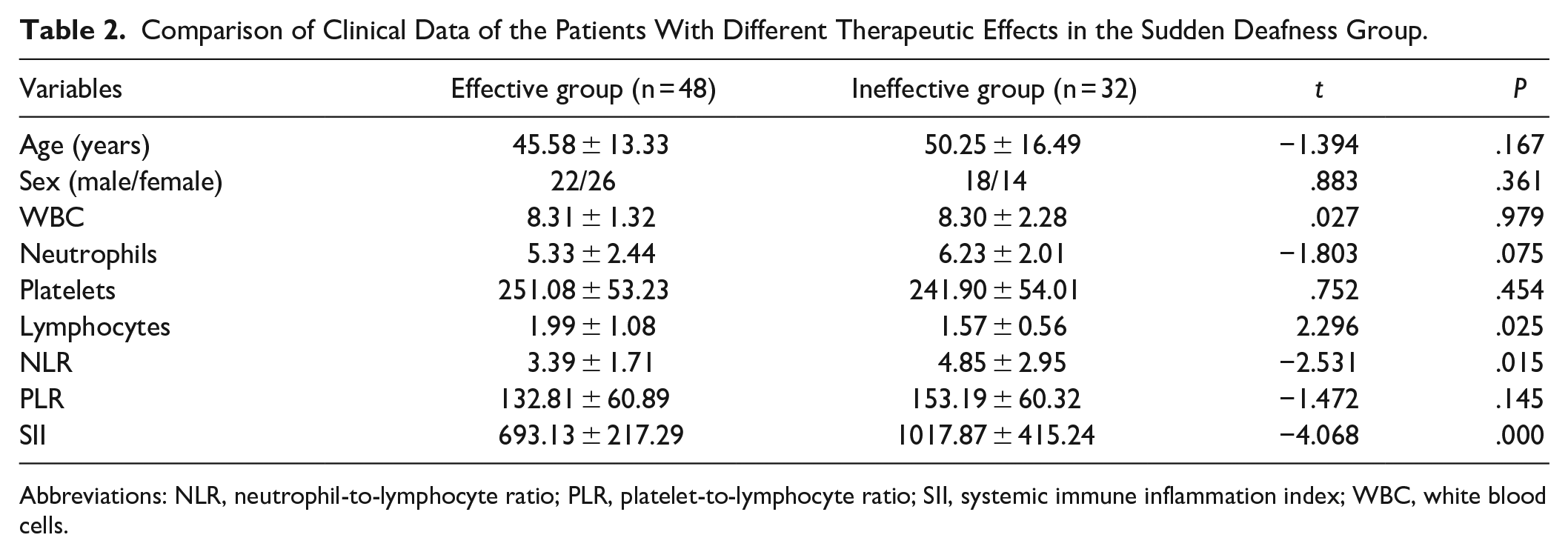
Abbreviations: NLR, neutrophil-to-lymphocyte ratio; PLR, platelet-to-lymphocyte ratio; SII, systemic immune inflammation index; WBC, white blood cells.
Investigation of the Factors Affecting Treatment Efficiency
A logistic regression analysis was performed with factors, including lymphocytes, NLR, and SII, found to be statistically significant based on the above univariate analysis results (P < .05). The results of logistic regression analysis have revealed that elevated NLR and SII were risk factors affecting the curative effect for patients with SSNHL (Table 3).
Multivariate Logistic Regression Analysis of Factors Affecting Treatment Effectiveness.
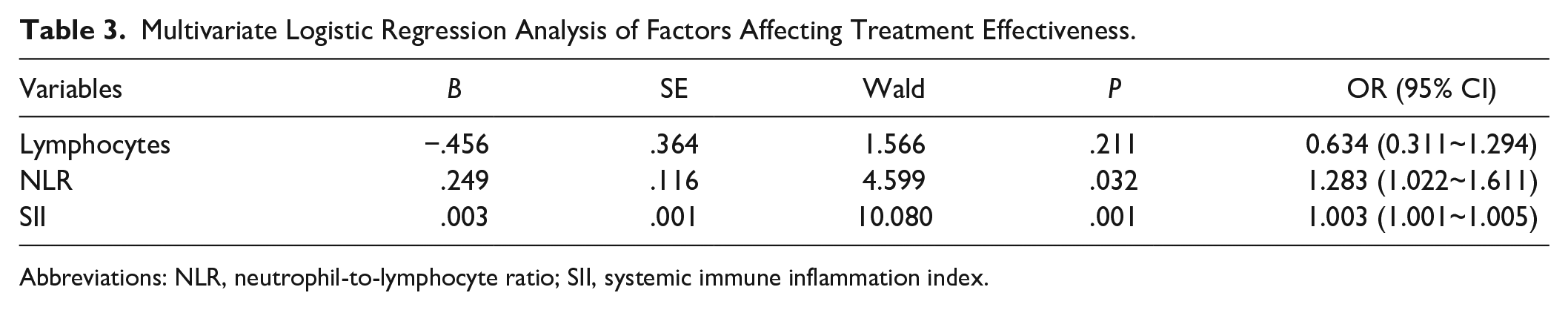
Abbreviations: NLR, neutrophil-to-lymphocyte ratio; SII, systemic immune inflammation index.
ROC Curve Analysis for Prediction of NLR and SII
To assess the prediction value of NLR and SII for treatment effectiveness, the ROC curve was developed. The NLR and SII curves’ AUCs were .630 and .781, respectively, showing that they have satisfied predictive value for treatment outcome. When the ideal cutoff values were used, also evaluated were the sensitivity and specificity of NLR (sensitivity = .406, specificity = .688) and SII (sensitivity = 1.000, specificity = 0.812) (Table 4 and Figure 1).
Analysis of the Predictive Value of NLR and PLR for Treatment Effectiveness.
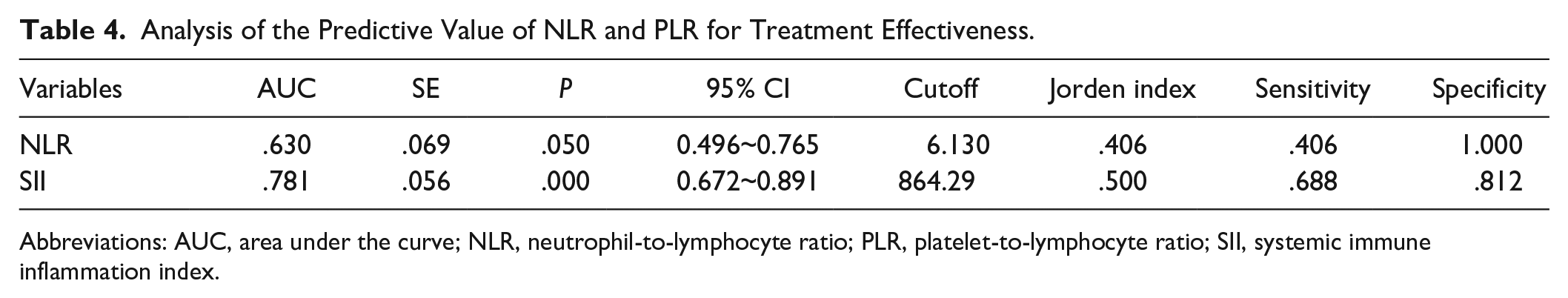
Abbreviations: AUC, area under the curve; NLR, neutrophil-to-lymphocyte ratio; PLR, platelet-to-lymphocyte ratio; SII, systemic immune inflammation index.
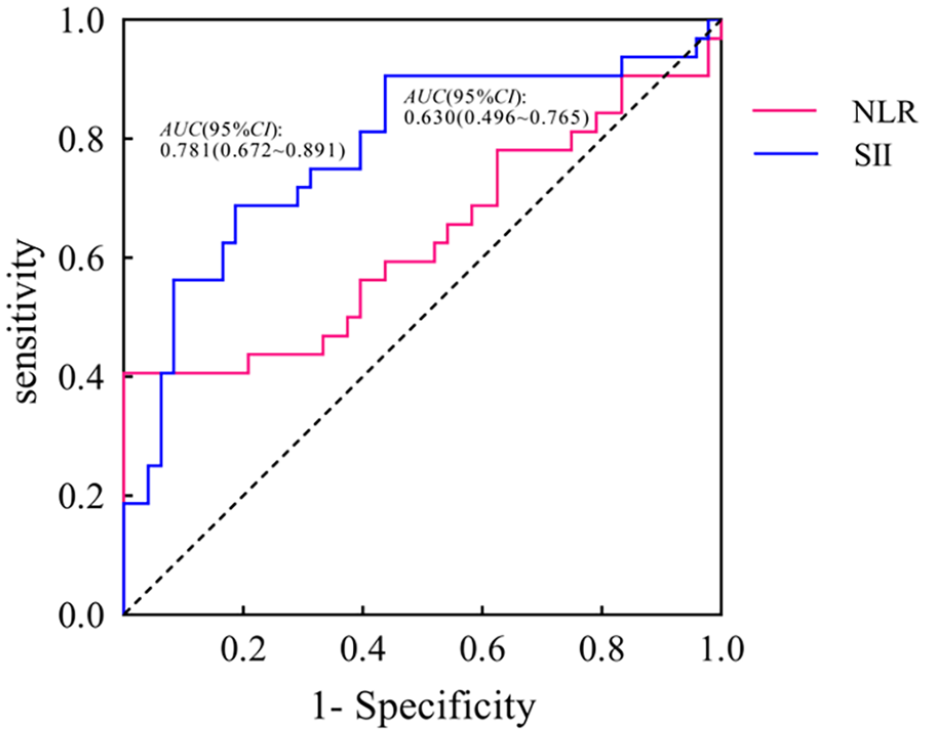
ROC curves of the predictive value of NLR and PLR for treatment effectiveness.
Discussion
In 3 days or less, PTA must detect a SSNHL of 30 dB or more at 3 consecutive frequencies. 1 It usually manifests unilaterally and has a quick onset. 1 SSNHL may result from both local and systemic sources, although the exact pathogenic mechanism is yet unknown. Numerous researchers have proposed viral infection as the underlying cause, although antiviral therapy has not yielded positive outcomes. 18 The temporal bone tissue of individuals with SSNHL was subjected to a pathological analysis in a previous study, and researchers discovered no signs of virus infection. 19 As a result, there was no concrete proof that the inner ear had a viral infection. At the same time, the theory of thrombus formation should be questioned because there is no discernible difference between males and females in the incidence of SSNHL. 20 Chronic inflammation is the main topic of current studies on the etiology of SSNHL. The cochlea’s labyrinthine artery lacks collateral arteries, making cochlear hair cells extremely vulnerable to ischemia injury. SSNHL may result from endothelial failure or vascular spasm brought on by bacterial or viral infections. The development of thrombus or increased blood viscosity in the cochlea, along with certain cardiovascular risk factors, can result in SSNHL. 21
Neutrophils and lymphocytes, 2 kinds of white blood cells, are regarded as inflammatory indicators of cardiovascular disease. 22 In atherosclerosis, platelets are crucial. 23 As a possible indicator of inflammation in both cardiac and noncardiac disorders, NLR has been described. 22 PLR and peripheral artery occlusive conditions such atherosclerosis and thrombosis are intimately connected. 23 A predictive predictor for inflammatory illnesses and malignant tumors, SII is a novel inflammatory index. 15
In our study, the white blood cell count, neutrophil count, and platelet count were all substantially higher in the SSNHL group than in the control group, and similar findings have been reported in prior research. 24 Additionally, it has been noted that high neutrophil counts are a useful predictor of a bad prognosis in SSNHL. 25 Indicating that there is inflammation in SSNHL patients, NLR, PLR, and SII levels were statistically substantially higher in the SSNHL group than in the control group.
We identified a strong correlation between a higher NLR value and a bad prognosis for SSNHL. Similar findings from earlier studies support the notion that a higher NLR value predicts a worse outcome for SSNHL, which denotes the presence of local microvascular inflammation, including that of the labyrinthine artery. 26 Prior to therapy, the NLR value of the ineffective group was greater than that of the effective group, indicating that the microvascular inflammation of the cochlea was more severe. Therefore, using glucocorticoids locally or systemically to lessen microvascular local inflammatory reactions involving the labyrinthine artery is beneficial in treating SSNHL patients. 27 Elevated PLR value as an inflammatory marker is linked to a bad prognosis, especially in cardiovascular illness. 23 However, the degree of PLR is not significant for patient prognosis in any of the recent research on SSNHL, which is in line with the findings of our investigation. 28
SII has been shown to be preferable to other systemic immune-inflammatory markers, such as PLR and NLR, in terms of inflammation.29,30 The AUC value of SII in our study ranged from 0.7 to 0.8, showing that SII can also be a reliable indicator of the prognosis of SSNHL. As a result, we think glucocorticoids are necessary for the treatment of SSNHL patients. However, because glucocorticoids have some undesirable side effects, alternative therapeutic modalities, such as intravenous steroid injection (200 mg daily for 3 days) and associated anti-inflammatory therapy, may be preferable for individuals with extremely high NLR or SII values. Patients with higher NLR or SII value can have other biomarkers such NLRP3, Caspase-1, IL-6, and TNF-α evaluated. These biomarkers have all been shown to be negatively connected with SSNHL patients’ prognoses and to have a better predictive value.25,31,32 Additionally, under the influence of inflammatory cytokines, monocytes can develop into macrophages, 33 and macrophages found in the cochlea may drive local inflammation that results in SSNHL by activating inflammasomes and secreting IL-1β. 34 To help clinical physicians assess the risk stratification of SSNHL patients, clarify the prognostic value and pathological and physiological functions of additional inflammatory markers in SSNHL patients, encourage early intervention and reduce the disability rate, and use patient assessment for individualized treatment, more research is required in the future.
Meantime, the study included a number of restrictions. For instance, we studied the peripheral blood inflammatory markers of 80 SSNHL patients in few existing clinical data. These SSNHL patients only had data available at the time of admission, and the follow-up time was brief. Secondly, the study has only remained at the level of cells, and no in-depth studies have been performed. Future prospective studies with larger sample sizes and exploration at the level of gene are required. It is still worth noting the results of our study despite these limitations.
Conclusion
Corticosteroids are advised for the treatment of SSNHL patients since elevated NLR and SII may indicate the existence of immune-inflammatory reactions. Considering the hazards associated with steroid, it is important to carefully weigh the benefits and risks of steroid use, and alternative and anti-inflammatory treatments can be taken into consideration for this group of patients. Patients with high NLR and SII scores, nevertheless, might also not respond to therapy well. For patients with higher NLR or SII value, we advise examining additional inflammatory markers and providing patients with customized therapy based on the results.
Footnotes
Acknowledgements
Authors’ Contributions
The study’s concept and layout were proposed by Xu Zhang and Bing Guan. The data collection and analysis were carried out by Xu Zhang, Ying Wang, and Qi Yan. The literature search was completed by Xu Zhang, Wentao Zhang, and Li Chen. The core article was written by Xu Zhang, while editing and critical revision were carried out by Maohua Wang and Bing Guan. The study was managed by Maohua Wang and Bing Guan. The funding was obtained by Bing Guan. The final draft of the article has been approved by all authors once they have read it. The final article was read and approved by all writers.
Availability of Data
The datasets generated and analyzed during the current study are available from the corresponding author upon reasonable request.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This study was financially supported by the technical projects supported by the Institute (No. FCJS202316), Jiangsu Province Natural Science Foundation (BK20201220).
Ethical Approval
The study was approved by the Ethics Committee of the Ethics Review Committee of the Clinical Medical College, Yangzhou University (Approval number: 2023ky052) and conducted according to the Declaration of Helsinki.
Informed Approval
Before every procedure, patients gave their informed consent.
