Abstract
Significance
This review demonstrates a trend toward improvement in the rate of surgical success of endoscopic dacryocystorhinostomy (endoDCR) when routine endonasal debridement was instituted 2 weeks following surgery. We believe that removal of nasal debris at the osteotomy site improves tear outflow and reduces cicatricial healing enhancing patency of the surgically derived lacrimal-nasal fistula. We advocate for postoperative debridement in the perioperative management of endoDCR patients to optimize successful outcomes.
Introduction
Endoscopic dacryocystorhinostomy (endoDCR) has proven to be an effective minimally invasive surgical procedure for treatment of nasolacrimal duct obstruction. 1 Surgical failure is commonly attributed to inadequate osteotomy, ostium granuloma, mucosal stenosis and scarring, turbinate hypertrophy, previous trauma, and incomplete opening of the nasolacrimal sac.2-4 Factors suggested to optimize patient outcomes following dacryocystorhinostomy (DCR) surgery include prolonged nasolacrimal intubation, use of post-operative ophthalmic and intranasal steroids, and intraoperative anti-fibrotic agent application.1-4
Post-operative sinonasal debridement has been shown to yield superior anatomic outcomes and fewer intranasal adhesions following functional endoscopic sinus surgery (FESS). 5 Early post-operative nasal vault debridement has been anecdotally advocated following endoDCR surgery in the otolaryngology and oculoplastic literature though without formal assessment.6,7 The authors herein postulate that post-operative inflammatory debris in the nasal vault may contribute to osteotomy obstruction and that surgical debridement may yield superior long-term outcomes. This study aims to evaluate the independent effect of post-surgical debridement on functional endoDCR success.
Materials and Methods
A retrospective review was performed of all patients who underwent endoDCR by an experienced oculofacial plastic surgeon over 7 years (2012-2019). Institutional Review Board approval was obtained and research was performed in accordance to the Declaration of Helsinki. Surgical indications included prior history of dacryocystitis and/or evidence of nasolacrimal duct obstruction upon in-office probe and irrigation. Patients with complete canalicular obstruction, nasolacrimal obstruction from a mass, and those undergoing simultaneous septoplasty were excluded. Surgery was performed by a single American Society of Ophthalmic Plastic and Reconstructive Surgery (ASOPRS)-trained surgeon (T.N.) with 5 years of endoDCR experience prior to the procedures under study. All patients underwent standard endoDCR with lacrimal sac flap preservation, followed by bicanalicular stent tube insertion and triamcinolone acetonide-soaked absorbable gelatin sponge placement at the osteotomy site. Bicanalicular nasolacrimal intubation was maintained for 4-6 weeks post-operatively. All patients were treated with topical intranasal and intraoperative steroid medication for 2 weeks immediately post-surgery, and for 1 additional week post-stent removal. The employment of nasal vault debridement was the only variable modified in surgical technique and post-operative management among the 2 cohort groups.
Post-operative intranasal debridement was not routinely performed from March 2012 to February 2016. From March 2016 to June 2019, all patients underwent routine ipsilateral intranasal debridement at post-operative week 2. Surgical debridement was performed in-office with use of a lighted headlamp, handheld rigid endoscope, or penlight. A combination anesthetic spray comprised of benzocaine, aminobenzoate, and tetracaine was applied intranasally. Debridement involved removal of all visible nasal crusts and blunt lysis of circum-osteotomy adhesions, performed using bayonet forceps, until clear patency of the osteotomy was visualized.
Patient demographics, surgical details, and post-operative management were reviewed. Surgical success was assessed via subjective assessment of epiphora resolution at the patient’s final post-operative visit. Stent tubes were routinely removed 4-6 weeks post-operatively. Success rates were analyzed using Fisher Exact Test with P-value of less than .05 considered significant.
Results
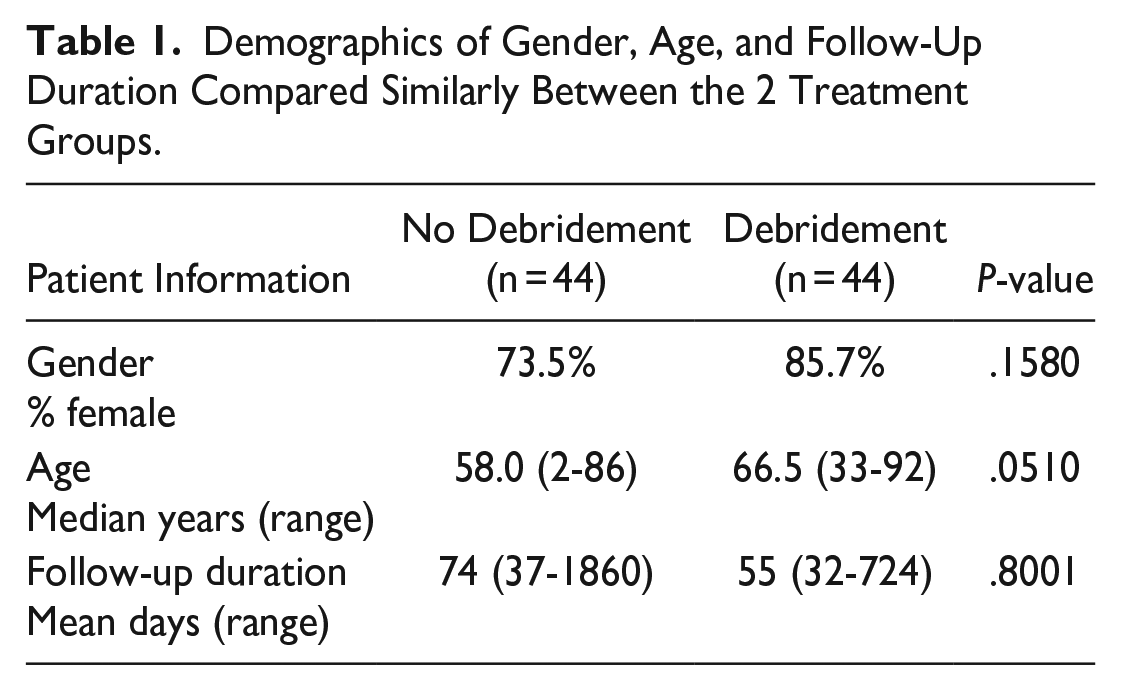
A total of 69 patients (88 surgeries) were included (Table 1). Fifty patients underwent unilateral surgery and 19 patients underwent bilateral simultaneous endoDCR. A total of 35 patients had standard post-operative follow-up without debridement, whereas 34 underwent endonasal debridement at post-operative week 2 (Figure 1). The median age was 57 years (range 2-86 years) in the non-debridement group, and 66 years (range 33-92 years) in the debridement group. Both groups were comprised of a majority of female patients (73.5% and 85.7%, respectively). The median time to final follow-up time was 61 days (range 32-1860 days).
Demographics of Gender, Age, and Follow-Up Duration Compared Similarly Between the 2 Treatment Groups.
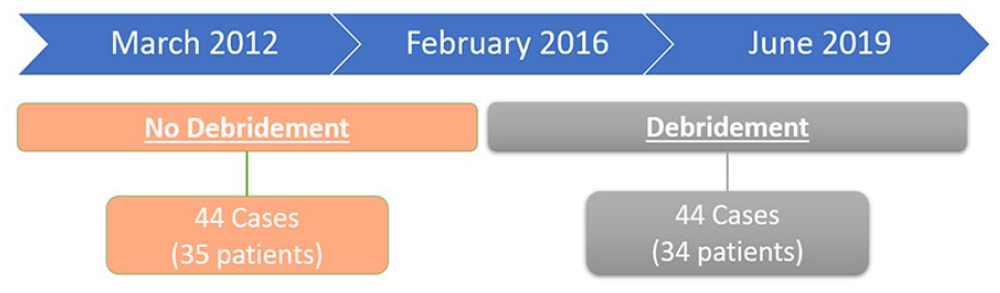
From March 2012 to February 2016, no post-dacryocystorhinostomy endonasal debridement was routinely performed. From March 2016 to June 2019, routine post-operative debridement was performed 2 weeks following surgery.
In the non-debridement cohort, 84.1% of patients had successful resolution of their epiphora and objective patency of their lacrimal system upon long-term follow-up, whereas 97.7% of patients in the debridement group had a successful surgery (P = .058) (Table 2). One patient who was not initially debrided presented with recurrent tearing at post-operative month 2, underwent delayed debridement, and achieved complete resolution of their epiphora upon final follow-up.
Surgical Success, as Determined by Resolution of Symptomatic Epiphora, for the 2 Intervention Groups.

The failures identified in the non-debridement group were attributed to canalicular stenosis (n = 4, 57.1%), lacrimal sump syndrome (n = 1, 14.3%), small osteotomy (n = 1, 14.3%), and soft tissue fibrosis (n = 1, 14.3%). In the debridement group, there was 1 failure, secondary to canalicular stenosis. This patient was successfully managed with canalicular trephination and bicanalicular stenting in a revision procedure.
Discussion
Post-nasal debridement following FESS has been thoroughly assessed in the otolaryngology literature. A 2018 Cochrane review summarized results of randomized controlled trials comparing surgical outcomes with and without post-operative debridement, finding similar revision rates between the 2 groups, but better anatomic success and fewer endonasal adhesions in those debrided. 5 Similar analysis of this practice has not previously been performed in the DCR literature.
The study herein found a trend toward improvement in functional endoDCR outcomes when post-operative endonasal debridement is performed. These authors find the procedure to be a straightforward, quick and well-tolerated at the 2-week time point following surgery. Earlier debridement may be complicated by patient sensitivity and risk of hemostasis disruption.
Proposed mechanisms by which post-operative endonasal debridement improves endoDCR outcomes includes improved patient comfort and respiration, with ensuing decreased bicanalicular tube manipulation, removed nidus for scar scaffold and inflammation, and normalization of nasal flora. Perhaps the most critical benefit of debridement is the early facilitation of neo-nasolacrimal fistula tear flow and ultimate patency. Similar debridement may be less essential following external DCR surgery given presumably more limited nasal mucosal trauma.
While this study was limited to a single surgeon, the results are uncomplicated by surgeon skill and technique variability that would be present in a multi-provider study. The results from this study showed a sizeable difference in surgical success when debridement was employed that we hypothesize would reach the threshold of statistical significance in a larger study. While a prospective randomized controlled trial would be the optimal for assessing the impact of debridement on surgical outcomes, the applicability of these results are supported by a single surgeon’s consistent technique and similar demographics between our treatment groups. Surgeon skill improvements during the sequential study period is a potential bias; however, this is unlikely given the surgeon’s multi-year experience prior to the study’s initiation. Finally, surgical debridement cannot be readily performed in the pediatric population, thus limiting this post-surgical intervention to cooperative adult patients.
This review suggests an improvement in the rate of surgical success of endoDCR when routine endonasal debridement was instituted 2 weeks following surgery. The removal of nasal crusts, residual absorbable nasal packing, and fibrotic tissue at the osteotomy site appears to improve tear outflow and maintenance of patency of the surgically derived lacrimal-nasal fistula. We advocate for postoperative debridement in the perioperative management of endoDCR patients to optimize successful outcomes.
Footnotes
Consent Statement
There are no patient photos or other identifying information included in this manuscript.
Data Availability
Datasheet available.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Ethical Statement
The authors have the following disclosures, none relevant to the content of this manuscript. T.N.: Shareholder, AVYA Skincare.
Grant Number
N/A.
Meeting Presentation
This was shared as an oral presentation at the 2021 Spring ASOPRS Symposium.
