Abstract
This study aimed to investigate the impact of the Nordic hamstring exercises (NHE) on acute fatigue-induced alterations in the mechanical and morphological properties of hamstring muscles. The second aim was to define the blood flow and perfusion after NHE in recreational active volunteers. Twenty-two individuals volunteered to participate in the study. This study investigated fatigue outcomes: rate of perceived exertion (RPE) scale and average force generated during NHE; mechanical properties (stiffness); morphological properties (thickness, pennation angle, and fascicle length), and vascularity index (VI) of the semitendinosus (ST) and biceps femoris long head (BFLH) at baseline, immediately post-exercise and 1-h post-exercise. The NHE fatigue procedure consisted of six bouts of five repetitions. The results showed an increase in thickness and pennation angle of BFLH and ST immediately post-exercise and a decrease in thickness and pennation angle of BFLH and ST 1-h post-exercise. While the fascicle length of BFLH and ST decreased immediately post-exercise and increased 1-h post-exercise. The VI for two muscles increased immediately post-exercise and after 1-h post-exercise. Moreover, we found a relationship between RPE and average force, that is, as RPE increased during NHE, average force decreased. In conclusion, eccentric NHE exercises significantly and acutely affect BFLH and ST. The NHE fatigue protocol significantly affected the mechanical and morphological properties of BFLH and ST muscles, changing their thickness, fascicle length, pennation angle, and VI.
Introduction
Acute hamstring fatigue affects muscle strength, thereby making them unable to maintain a certain intensity or power output. 1 Many authors have studied the effect of acute fatigue on hamstring properties.2–4 Schwiete et al. 2 used a fatigue training session consisting of 1 × 50 concentric leg curls with maximum effort assessing the impact on the morphological properties of muscles. Marshall et al. 3 assessed hamstring fatigue during six bouts of five repetitions of Nordic hamstring exercises (NHE). Whereas, Lovell et al. 4 evaluated an acute fatigue NHE routine before or after soccer training. Hamstring fatigue may indicate a greater chance of stretching the musculotendinous units of the hamstring group, predisposing to a hamstring injury, especially the biceps femoris.5–8 This is due to the reduction in the amount of energy that is absorbed by the elongating muscle, leading to a significant deficit in the strength and endurance of the tendons, and hence the injury rate of the hamstrings may increase.9,10
Various measurements were used to determine both morphological and mechanical properties after fatigue-induced exercises of hamstring muscles.11–13 Compared to other imaging methods (e.g. magnetic resonance imaging/computed tomography), ultrasound imaging seems to be more advantageous due to safety, noninvasiveness, and the possibility of real-time assessment.14–16 Ultrasonography using B-mode gives the ability to measure thickness, pennation angle, and fascicle length in real time, while Power-Doppler provides analysis of vascularization in real time. Currently, vital microscopy17,18 and Laser Doppler Flowmeter19,20 are the most commonly used methods to assess blood flow. It seems that the simultaneous use of both B-mode (thickness, pennation angle, and fascicle length) and Power Doppler (vascularity) may become the new standard muscle physiological measurements. Muscle stiffness was assessed using a hand-held myotonometer, which is quick and reliable for diagnosis. 21 The myotonometer assesses dynamic muscle stiffness with good validity and reliability. 22 Myotonometry was taken at specific points to generate a topography of muscle morphological properties.23,24 In previous studies the eccentric strength of the hamstring after NHE was assessed by isokinetic dynamometry. 4 Alternatively, the Nord Bord® platform was proposed to measure the average eccentric force of the hamstring. Nordbord® allows to assessment of the eccentric strength of the knee flexors in real time during NHE exercises.25,26
Eccentric exercise triggers oxidative distress and inflammation, inducing a decrease in vascular endothelial and vascular smooth muscle function. 27 Nevertheless, a series of time points observations of blood flow after eccentric muscle fatigue has not been made. Increased blood flow using the color Doppler in the elbow flexor was found after the eccentric exercise. 28 However, this finding may be related to the metabolic demands of contracting muscle, causing vasodilation, and is not necessarily related to the muscle damage from eccentric exercise. Depending on the amount of blood present, the power Doppler is better than the color Doppler in depicting increased flow in dilated vessels because of an inflammatory response. 29 The power Doppler permits monitoring of serial blood flow changes after exercise and allows the investigators to distinguish flow changes related to the inflammatory response to eccentric exercise. 29 A power Doppler-derived parameter, vascularity index (VI), denotes the ratio of color-coded voxels to all voxels within the volume and is expressed as a percentage. 30 VI may be preferred because, in clinical practice, oncologists already use the vessel density (i.e. the number of vessels as a measure of tumor vascularization); however, VI has not been used to investigate the blood flow after eccentric exercise.
A better understanding of changes in the mechanical and morphological properties of the hamstring after acute NHE fatigue may be useful both in proposing specific training strategies and in the prevention and rehabilitation of the hamstring. Previously, no one paid attention to the vascularity of the muscles immediately after acute training. Other studies assessed blood flow after eccentric exercise when the muscle was already inflamed.18,31,32 Therefore, the first objective of this study was to investigate the effect of the Nordic hamstring on acute fatigue-induced changes in the mechanical and morphological properties of the hamstring muscles. The second goal was to define the blood flow and perfusion after the fatigue procedure after NHE in recreational active volunteers.
Material and methods
Study design
This study investigated a repeated measure study of Nordic hamstring's session on functional (average force of knee flexors muscles and rate of perceived exertion (RPE)), mechanical (stiffness), and morphological (thickness, pennation angle, fascicle length, and vascularity index) alterations of the hamstring muscles (semitendinosus (ST) and biceps femoris long head (BFLH)). The functional outcomes were assessed using the Nord Bord® platform, while the morphological measurements were by ultrasonography imagining and mechanical using myotonometry at baseline, immediately post-exercise (IP), and 1-hour post-exercise protocol (1-h). Measurements were made in the same order starting with (1) myotonometry, ST,(2) ultrasonography, and (3) Power-Doppler mode to assess the degree of vascularization for ST and BFLH.
The participants read and signed the informed consent form approved by the Bioethics Committee at the Regional Medical Chamber in Gdańsk (project identification code: 66/22, approval date: 27 December 2022).
Participants
Twenty-two recreational active individuals (males (n = 2) and females (n = 20); 20.3 ± 1.5 years, 173.1 ± 3.4 cm, 65.2 ± 1.5 kg) volunteered in this study. All participants were physical therapy students at the college level practicing in individual and team sports (i.e. kickboxing, handball, volleyball, and judo). Their weekly sports activity was 6 ± 1 hours. Inclusion criteria included a recreational lifestyle activity in individual and team sports of at least 5 hours per week and previous experience in the technical implementation of an NHE exercise and technique. Exclusion criteria included previous amateur training experience, participation in indoor or outdoor events in the past month, and knee, hip, or lower back pain, muscle fatigue, overtraining, injury, or surgery within 6 months before the intervention.
The G*Power software (version 3.1.9.2; Kiel University, Kiel, Germany) was used to estimate the required sample size. A sample size estimated with a repeated measure analysis of variance (ANOVA) within and between factors, an α of 0.05, set a minimum expected effect size (Cohen's f) of 0.4, β of 0.95, and correlation among repeated measures of 0.5. The procedure included a minimum number of 18 participants, but four extra participants were recruited to account for potential drop-out.
Procedure
Measurements were taken three times: at baseline, IP, and 1-h post-NHE procedure. The experimental procedure included two phases.

The Nordic hamstring exercise on the NordBord platform (a) and an example of force [N] courve (b).
Measurements outcomes
Functional properties
Functional outcome measurements were analyzed by the Nord Bord® platfrm's software. To analyze the data we used average force [N]. The volunteers were placed in a kneeling position on the platform. Their ankles were secured with hooks placed above the side ankle. The ankle hooks were perpendicular to the ground at all times. All patients were instructed to gradually lean forward as slowly as possible during the test. The force curve was recorded in the NordBord application (Vald Performance NordBord software).26,33
Rate of perceived exertion scale
The RPE is a tool that has been used to monitor and quantify individual effort perception during fatigue training. 34 The Borg scale (0–10), in which 0 means no perceived effort, and 10 means the maximum perceived effort, was assessed before fatigue training and after each set of repetitions in the subjects. 35
Mechanical properties
The stiffness of the ST and BFLH was measured using a hand-held myotonometer. Optometry is a reliable method of measurement and can detect differences in physical properties compared to stretched muscle fibers. 36 The measurement method consists of registering the damped natural vibrations of soft biological tissue in the form of an acceleration signal, and then simultaneously calculating the parameters of the state of stress and biomechanical properties: muscle tension (T), dynamic stiffness (S), and elasticity (E). 37 Myotometric measurements were performed on the posterior surface of the thigh, three times at each reference point (8 points) including the ST (4 points) and BFLH (4 points). 38 Participants were lying in a prone position with their feet on the massage table. The measurement for one point lasted about 5 seconds, while the total test time did not exceed 2 minutes.
Morphological properties
Morphological properties, including thickness, pennation angle, fascicle length, and vascularity index of ST and BFLH were investigated by ultrasonographic imaging using B-mode and Power-Doppler mode (SonoScape E2, SonoScape Medical Corp, Shenzhen, China) with a 4–16.0 MHz and 40 mm linear probe (L741). Power Doppler mode was set at 370 Hz for pulse repetition frequency and filtered at 1 for detection of vessels with low blood flow. Moreover, the color gain was also set from the highest signal level and decreased until the noise disappeared. 39 A single examiner (7 years of experience in musculoskeletal imaging) obtained ultrasound images of ST and BFLH along their long axis. Participants were lying in a prone position with their feet on the massage table. To identify the region of interest for ST and BFLH, the examiner had to define the proximal and distal landmarks for muscle–tendon junctions. Thus, the linear probe was placed on the transverse axis to the long axis of the muscle. Next, the probe was placed in the longitudinal axis when the most hyperechogenic area was defined. The proximal landmark was marked in a similar procedure, however, the probe moved in the proximal direction. The region of interest for ST and BFLH was searched in the mid-region in the longitudinal axis to define a proper image. 40 Each measurement was taken twice and averaged for data analysis.
Ultrasound images we stored in DICOM files and measured using MicroDicom viewer software (MicroDicom DICOM Viewer, Bulgaria). The ST and BFLH thicknesses were measured as the average distance between the superficial and mid-muscle aponeuroses at 5 points on the image separated by 10 mm from one another (Figure 2(a)). The pennation angle was measured by determining the angle between a fascicle and the deep aponeurosis. The fascicle length
41
was calculated from the following equation (1) (Figure 2(b)):

An example of morphological properties measurements of the biceps femoris long head, including (a) thickness, (b) pennation angle (α), and fascicle length. To calculate fascicle length: h is the perpendicular distance between the superficial aponeurosis and distal point of the fascicle, and β the angle between the fascicle and the superficial aponeurosis.
Vascularity index
Power-Doppler mode was used to assess the blood flow and perfusion by vascularity index. The vascularity index was calculated using ImageJ version 1.47 software (National Institutes of Health, Bethesda, MD). This software allowed us to count the total number of pixels and the color pixels in the region of interest. The region of interest was defined as the 5 × 2 cm box (width × length). The vascularity index
39
might be calculated as in equation (2):

Calculation of the vascularity index.
Statistical analysis
The SPSS statistical software (version 18., SPSS Inc., Chicago, Illinois, USA) was used for data analysis. Mean values ± standard deviation (SD) or confidence interval (95% CI) are reported. The normality of the data distribution was tested using Shapiro-Wilk tests, while homogeneity of variance was analyzed by Levene's test. The analyzed data were normally distributed for all parameters, while the variances were equal for all parameters. A one-way repeated measure analysis of variance (RM-ANOVA) with Time (baseline, IP, and 1-h post-exercise) was conducted for RPE and average force, while a two-way RM-ANOVA with Time (baseline, IP, and 1-h post-exercise), and Muscle (ST and BFLH) was conducted for morphological (thickness, Lf, θp, and VI) and mechanical (stiffness) properties. If a significant interaction between factors was found, the Bonferroni adjustment for multiple comparisons was used for post hoc tests (p = 0.0083). The effect size was estimated using partial eta square (η2), classified as small (0.2<η2<.049), medium (0.5<η2 < 0.79), or large (η2 ≤ 0.8). 42 Pearson's correlation test was applied to determine the relationships between pre-immediately after, and immediately after 1-hour post-exercise differences of stiffness, thickness, pennation angle, fascicle length, and vascularity index of semitendinosus and BFLH. The correlation coefficients were classified as trivial (0.0), small (0.1), moderate (0.3), strong (0.5), very strong (0.7), nearly perfect (0.9), and perfect (1.0). 42 For all statistical tests besides post hoc tests, a p value ≤0.05 was considered significant.
Results
Functional alterations
The one-way RM-ANOVA revealed a statistically significant main effect of Time (F5,115 = 109.0, p ≤ 0.001, η2 = 0.83) for average force. Average force decreased significantly during all bouts of NHE except after the second bout (p ≤ 0.001 for all). For RPE, the one-way RM-ANOVA revealed a statistically significant main effect of Time (F6,126 = 293.5, p ≤ 0.001, η2 = 0.93). The RPE increased significantly during all bouts of NHE except after fifth bout (p ≤ 0.001 for all) (Figure 4).

Mean ± SD of the average force (N) and RPE scale during six bouts of NHE protocol. An asterisk (*) indicates significant changes compared with baseline (p < 0.05). NHE: Nordic hamstring exercises; RPE: rate of perceived exertion.
Mechanical properties
Figure 5 shows the mean ± SD of the hamstring muscles mechanical and morphological properties, as well as vascularity between both muscles (BFLH and ST) at baseline, IP, and 1-h post-exercise. The two-way RM-ANOVA revealed a statistically significant main effect of Time (F2,100 = 4.8, p = 0.01, η2 = 0.09) and Muscle (F1,50 = 70.0, p ≤ 0.001, η2 = 0.38). Overall, muscle stiffness was greater IP compared to baseline (p = 0.005). Moreover, we observed greter stiffness in the BFLH compared to ST (p ≤ 0.0001).
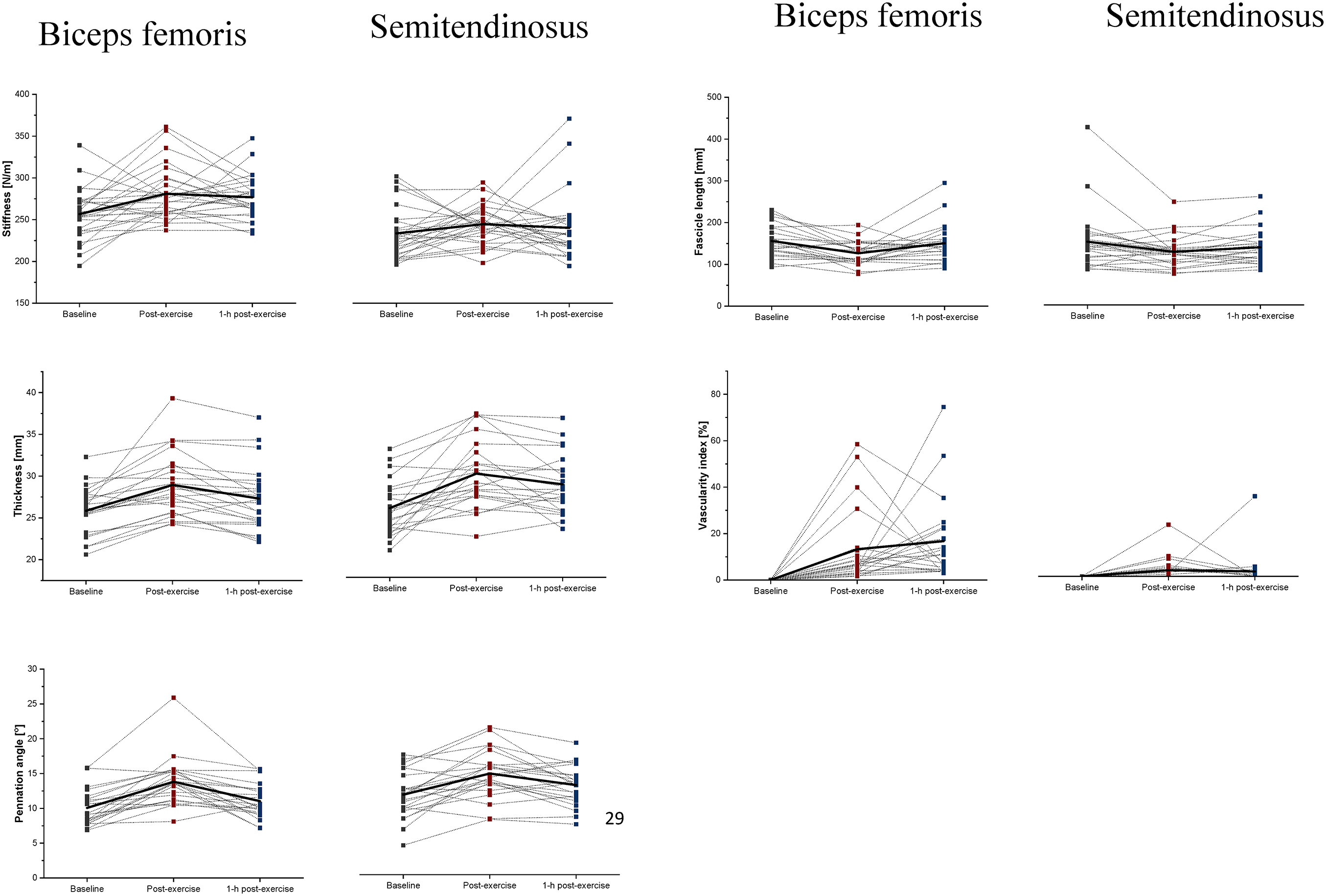
Mean ± SD of the mechanical (stiffness [N/m]) and morphological (thickness [mm], pennation angle [o], and fascicle length [mm]) and vascularity index [%] of the ST and BFLH, immediately post-exercise, and 1-h post-exercise NHE protocol. BFLH: biceps femoris long head; NHE: Nordic hamstring exercises; ST: semitendinosus.
Morphological properties
The two-way RM-ANOVA revealed a statistically significant main effect of Time (F2,84 = 31.0, p = 0.001, η2 = 0.42) for thickness; pennation angle (F2.84 = 30.1, p = 0.001, η2 = 0.42), and fascicle length (F2.84 = 8.4, p = 0.001, η2 = 0.17). Muscle thickness increased immediately after the fatigue protocol (p ≤ 0.001) and decreased after 1-h post-exercise (p = 0.001). The pennation angle of hamstring muscles increased significantly immediately after the fatigue protocol (p ≤ 0.001) and decreased 1-h post-exercise (p ≤ 0.001), while the fascicle length decreased significantly immediately after the fatigue protocol (p ≤ 0.001) and increased 1-h post-exercise (p ≤ 0.001) (Figure 5).
Vascularity index
The two-way RM-ANOVA revealed a statistically significant main effect of Time (F2.42 = 9.8, p ≤ 0.001, η2 = 0.2) and Muscle (F1,42 = 22.2, p ≤ 0.001, η2 = 0.35) for the VI. Moreover, the analysis revealed a statistically significant interaction effect between Time and Muscle (F2,84 = 5.5, p ≤ 0.011, η2 = 0.11). The post hoc analysis showed that the VI of BFLH and ST increased significantly immediately after exercises compared to baseline (p ≤ 0.001). Moreover, greater VI was observed in BFLH 1-h post-exercise compared to ST (p = 0.001) (Figure 5).
Correlation
Pearson's correlation test showed very strong positive correlations between pennation angle and fascicle length (r = 1.0; p < 0.01), VI (r = 1.0; p < 0.01) for BFLH between immediately post and baseline. Pearson's correlation analysis also revealed correlations between VI and thickness (r = 0.47; p < 0.05) for ST between immediately post and baseline. However, about the value between immediate post and 1-h post-exercise, very strong correlations were found in the case of BFLH for pennation angle and fascicle length (r = 0.90; p < 0.01) and VI (r = 0.82; p < 0.01) and between fascicle length and VI(r = 0.98; p < 0.01). (Figure 6).

Pearson's correlation between morphological properties (pennation angle [o], fascicle length [mm], and thickness [mm]) and vascularity index [%] of the ST and BFLH, immediately post-exercise, and 1-h post-exercise. BFLH: biceps femoris long head; IP: immediate post-exercise; ST: semitendinosus.
Discussion
In this study, we have investigated acute post-exercise alterations in the morphological and mechanical properties of the BFLH and ST muscles after the NHE protocol. The current study showed that acute fatigue developed over time (increased RPE and decreased average force) during eccentric exercises resulting in simultaneous changes in muscle morphology and mechanical properties of both BFLH and ST muscles in recreational volunteers. The findings of this study supported the hypotheses and may provide new explanations regarding acute fatigue-induced changes in hamstring muscles. These changes can be explained by various factors, for example, changes in muscle architecture, fiber type, and changes induced by acute fatigue. 21
The present study showed the average force decreased by 16.5 N after each bout (except second) after NHE and a significantly higher RPE (except fifth) with each subsequent attempt confirming that our protocol consisted of six bouts of five repetitions interspaced by 2 minutes resulting in fatigue development. Allen 43 proposed that the reduction in force results from the uncontrolled elongation of the sarcomeres during eccentric contractions and thus shifts the peak of the force-length curve. This confirms that our protocol of six bouts of five repetitions caused the development of fatigue. Earlier studies showed similar results of 697.95 N and a decrease in the average force per series −54.48 N. 44 However, it should be emphasized that different designs and experimental procedures were performed in these studies. Burrows et al. 45 analyzed RPE using NHE to support various loads and determined knee flexor strength under various NHE bouts. Park et al. 46 showed that the RPE score increased with increasing Nordic exercise angle and base slope angle. In conclusion, the protocol used makes it possible to assess the acute changes caused by the development of fatigue during NHE exercises.
In the current study, we examined the mechanical changes in BFLH and ST, expressed in stiffness immediately after NHE and 1-h post after exercise. The results showed an increase in muscle stiffness immediately post-NHE compared to baseline. Evangelidis et al. 47 reported a significant impact of fatigue on the mechanical properties of hamstring muscles, measured as shear wave velocity. Their study demonstrated that hamstring eccentric exercises using an isokinetic dynamometer may lead to an increase in stiffness post-exercise. On the other hand, our results also showed a significantly greater stiffness in the BFLH compared to the ST. Our findings are in line with Evangelidis et al., 47 who found the BFLH to be a more fatigable muscle compared to the ST or semimembranosus. Andonian et al. 48 found that greater stiffness after strenuous exercise may be related to altered extracellular water volume. Acute changes in hamstring stiffness may be also related to changes in muscle tissue density (extracellular matrix) resulting in an increased rate of collagen turnover. 49 Moreover, greater mechanical alterations in BFLH compared with ST might be related to the fact that BFLH experiences the greatest strain compared to other muscles in the posterior thigh. 47 A research study performed by Seymore et al. 21 showed that NHE training did not significantly affect muscle fascicle length, stiffness, or eccentric hamstring strength. Noticeable changes in muscles may be related to increased vascularity resulting from greater muscle activity during acute fatigue. Future studies are therefore warranted to determine the effect of NHE training-induced muscle hypertrophy on muscle mechanical changes.
We observed changes in muscle morphological properties: thickness, pennation angle, and fascicle length as a result of acute muscle fatigue. Our results showed increase in BFLH and ST thickness immediately after acute fatigue, with a decrease in BFLH after 1-h post-exercise. The pennation angle increased IP in BFLG and ST, followed by a decreased after 1-h post-exercise. Finally, the fascicle length decreased significantly after IP with an increase 1-h post-exercise. The potential explanation for post-exercise changes in muscle morphology and architecture could be related to geometrical alterations due to increased water and fluid content. 50 Therefore, greater muscle thickness may induce a pennation angle and simultaneously result in a decrease in fascicle length, as reported in this study. Previous study by Alonso-Fernandez et al. 50 showed results after NHE training, where the BFLH thickness increased significantly (p ≤ 0.001), while the pennation angle showed a significant decrease (p ≤ 0.001). Maxwell et al. 51 in their theoretical model described the interaction of variables determining muscle architecture. They proposed that for a given muscle length and fiber length, an increase in the cross-sectional area of the fiber must be accompanied by an increase in pennation angle. Abe et al. 41 experimentally demonstrated the relationship between muscle thickness, fascicle length, and pennation angle in leg muscles. A larger pennation angle can be explained by a shorter fascicle length or an increase in muscle volume induced by acute fatigue. These results provide evidence that NHE can cause changes in the architectural conditions of the hamstring and may have practical implications for injury prevention and rehabilitation programs. Timmins et al. 52 showed that athletes with shorter fascicle length BFLH were 4.1 times more likely to maintain hamstring strain injury (HSI) than those with longer fascicle lengths. Such changes in morphological structure seem to underline the risk of hamstring injury with intense efforts. Fatigue after eccentric exercise training that drastically alters muscle architecture may also increase the risk of hamstring injuries.
We observed a significant increase in VI in BFLH and ST immediately after NHE and 1 hour after exercise in BFLH and ST. Furthermore, a greater VI was observed in BFLH immediately after exercise and 1 hour after exercise compared with ST. These findings suggest that oxidative stress and inflammation trigger acute vasodilation and increased microvascular perfusion from eccentric exercise utilizing anaerobic glycogenolysis and lactic acid accumulation, concomitant microvascular dilation, and impairment of capillary function for transporting and distributing oxygen in muscles. 32 Heap et al. 17 demonstrated that eccentric exercise increases the diameter of terminal arterioles and the diameters of larger and smaller veins that cause hyperemia. Hanson et al. 53 also found that microcirculatory function can modulate the hyperemic response to high-intensity exercise but not low-intensity exercise. In muscles stretched by eccentric exercise, blood flow, and oxygen distribution are disturbed, and a neovascular response dependent on vasodilation may occur. 18 Our study first demonstrated an acute increase in microvessel perfusion and hyperemia after NHE. And also found that the VI in BFLH indicates a preferential muscle activation or a location of muscle damage in the BFLH. This assumption corresponds to the literature that supports that most hamstring injuries occur in the BFLH.52,54 Our findings have collectively indicated that the VI potentially can be used to monitor the inflammatory responses in the hamstring after NHE, and recovery with intervention to reduce the occurrence or recurrence of the injuries.
Practical implications
This study suggests that an effective warm-up for NHE is relatively simple and fits easily into a typical training and muscle strength monitoring program. NordBord allows warm-up and monitoring of muscle strength at the same time. An additional advantage of introducing a constant warm-up or a bout of NHE exercises during training for amateur or professional athletes is, consequently, morphological, and mechanical properties changes in the hamstring on the long muscles of the posterior thigh group. This in turn reduces the risk of HSI and HSI rehabilitation. Eccentric training with long muscles can be of practical value in sports and rehabilitation.
Limitation
Some limitations of the present study should be acknowledged. Firstly, the study should be repeated on athletes or create two study groups: amateur athletes and professional athletes. Secondly, past injuries in the subjects were not taken into account. This information can be used to isolate an even more homogeneous study group and obtain detailed results for hamstring strengthening in both injured and uninjured players. Additionally, future research should include a division into men and women to assess whether the results differ by gender. Future research should include additional measurements 12 or 24 hours after the first measurement.
Conclusion
In conclusion, this study showed that eccentric NHE significantly affected acute BFLH and ST muscle fatigue, resulting in a decrease in average muscle strength during the procedure. The NHE fatigue protocol significantly affected the mechanical and morphological properties of BFLH and ST muscles, changing their thickness, fascicle length, pennation angle, and VI.
Footnotes
Author's contribution
MP-G, BB, H-KW, and SK contributed to the study desing. MP-G, BB, and SK conducted the study and drafted the paper and were involved in the field work. MS, RT, and H-KW revised the paper.
Data availability statement
The data generated during the current study are available from the corresponding author upon reasonable request.
Declaration of conflicting interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethics approval
The study was conducted following the Declaration of Helsinki and was approved by the Bioethical Committee of the Regional Medical Society (project identification code: 66/22, approval date: 27.12.2022).
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.


