Abstract
The Severe Acute Respiratory Syndrome Coronavirus-2 (SARS-CoV-2) pandemic had a significant impact on the Italian healthcare system, although geographical differences were present; regions in northern Italy have been the most severely affected while regions in the south of the country were relatively spared. Otolaryngologists were actively involved in the management of the pandemic. In this work, we analyzed and compared the otolaryngology surgical activity performed during the pandemic in two large public hospitals located in different Italian regions. In northern Italy, otolaryngologists were mainly involved in performing surgical tracheotomies in COVID-19 positive patients and contributed to the management of these patients in intensive care units. In central Italy, where the burden of the infection was significantly lower, otolaryngologists focused on diagnosis and treatment of emergency and oncology patients. This analysis confirms the important role of the otolaryngology specialists during the pandemic, but also highlights specific differences between two large hospitals in different Italian regions.
Introduction
The first wave of the Severe Acute Respiratory Syndrome Coronavirus-2 (SARS-CoV-2) pandemic had a significant impact on Italy although geographical differences were present; regions in northern Italy, such as Lombardy, Emilia-Romagna, and Piedmont have been severely affected while regions in the south of the country were relatively spared.1,2
Healthcare activity was profoundly affected and changed according to the restrictions adopted and to new forms of management of patients with Coronavirus Disease 19 (COVID-19). 2
In this work, we compared the otolaryngology surgical activity performed during a critical period of the first wave of the pandemic (March 10—April 28, 2020) in two large public hospitals located in regions differently affected: the Policlinico Umberto I University Hospital in Rome, central Italy, and the Niguarda Hospital in Milan, northern Italy. Ethic committee approval was not required by the institutions as per national regulations.
Geographic differences in COVID-19 cases in Italy
The spread of the SARS-CoV-2 pandemic showed different data between northern and central Italy. As of April 28, 2020, the number of COVID-19 positive patients in the general population was 74.348 in Lombardy (northern Italy) and 7.772 in Lazio (central Italy), respectively. The number of hospitalized positive patients was 7.280 in Lombardy and 1.468 in Lazio. At the time of the epidemic peak, in Lombardy there were 922 patients in intensive care units (ICU), compared to 185 patients in the Lazio region. The number of COVID-19 related deaths in Italy was 27.359; 13.575 (49.6%) of them in Lombardy and 414 (1.5%) in Lazio. 3
Otolaryngology activity during COVID-19 pandemic
The otolaryngology activity in Italy underwent major changes during the pandemic; outpatient visits and elective surgical activities were suspended, while the only allowed procedures were related to emergency and oncology patients.4,5
Between March 10 and April 28, 2020, the otolaryngology unit of the Policlinico Umberto I performed 96 surgical procedures; 74 (77%) for the diagnosis and treatment of malignant tumors of the neck and head, 14 (14.7%) for the management of upper airway obstructions, 6 (6.2%) abscess drainage and two (2.1%) for the treatment of nasal bone fractures. No tracheotomies were performed for airway management in COVID-19 patients. All patients undergoing surgery were COVID-19 negative. 6
During the same period, the otolaryngology unit of the Niguarda Hospital performed 73 surgical procedures; 57 (78%) for the management of upper airway obstructions, 14 (19.2%) for the diagnosis and treatment of malignant tumors in the head and neck, one (1.4%) abscess drainage, one (1.4%) tympanoplasty for chronic otitis media. Of the 57 tracheotomies, 56 were in COVID-19 positive patients admitted to ICU (Figure 1).
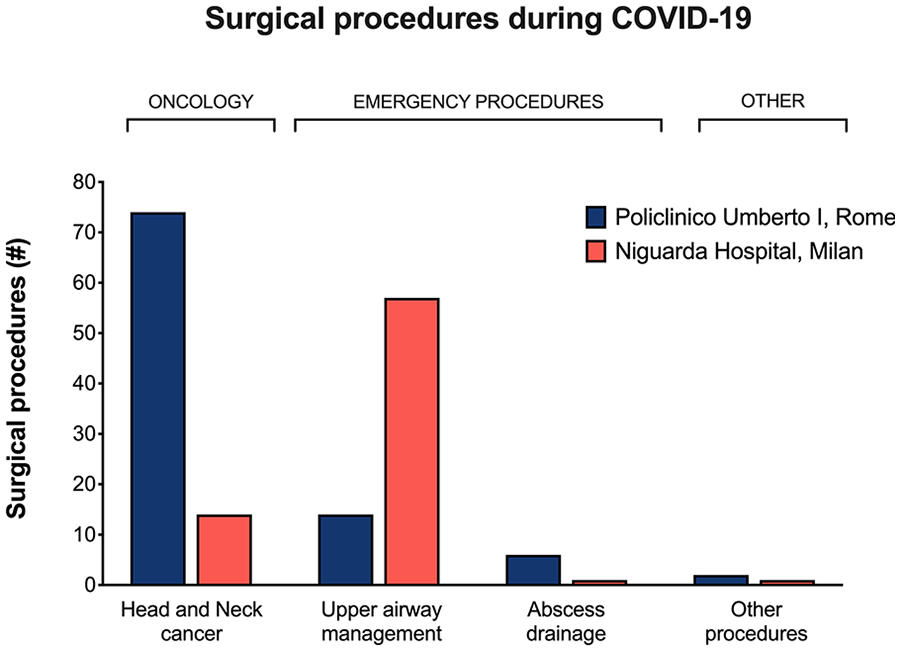
Surgical procedures performed in the Policlinico Umberto I, central Italy, and in the Niguarda Hospital, northern Italy, during the pandemic (reference period: March 10 to April 28, 2020).
Oncological activity
Surgical procedures in head and neck cancer patients were significantly different between the two hospitals included in the study. In the Policlinico Umberto I, otolaryngologists ensured continuative oncological surgical activity with 74 oncology procedures out of a total of 96 (77%). 6 At the Niguarda Hospital, the otolaryngology unit performed only 14 procedures for the diagnosis and treatment of malignant tumors in the head and neck (19.2%), due to the substantial number of tracheostomies performed in COVID-19 patients undergoing prolonged intubation.
Focus on tracheotomy in COVID-19 patients
Upper airway management through surgical tracheotomy was the far most common surgical procedure involving otolaryngologists during the pandemic 7 ; however, significant differences were observed between the two hospitals included in the study.
In the Policlinico Umberto I, the presence of COVID-19 positive patients with prolonged intubation was limited and the workload allowed to manage these patients with percutaneous tracheotomy, which was performed in 39 patients by the anesthesiologists. Differently, in the Niguarda Hospital surgical tracheostomy was preferred to percutaneous tracheotomy and was performed by otolaryngologists in ICU in 56 positive patients.
Guidelines from the Italian Otolaryngology Society were followed regarding procedures to limit the production of aerosols. 7 Tracheostomy, as well as all other medical procedures, should be performed with a careful use of personal protective equipment (PPE); as a general rule, all patients should be treated as being COVID-19 positive, with health care workers using the highest level of PPE. 8
Positive COVID-19 intubated patients who underwent tracheostomy ranged from 27 to 83 years with an average of 58 years. Of these patients, two were under 30 years of age (3.6%) and one over 80 years (1.8%). Mortality in the short term was 40%. Among surviving patients, after weaning, the tracheotomy tube was removed and the tracheostomy was closed through surgical procedure. The main recorded complication, found in nearly 15% of the patients, was local infection due to Staphylococcus aureus, Acinetobacter baumannii complex, Pseudomonas aeruginosa, Serratia marcescens, Klebsiella pneumoniae and Proteus mirabilis.
Focus on otolaryngology training
The severe impact of COVID-19 pandemic on surgical activity has also affected training of young otolaryngology surgeons and residents. In fact, the overall reduction of surgical procedures and the abolishment of elective surgery have drastically reduced the learning opportunities for otolaryngology residents. In a recent article published by the Italian Polyspecialistic Young Surgeons Society (SPIGC), the authors evaluated through a questionnaire the effects of the pandemic on residents, showing that the COVID-19 pandemic has severely impacted the educational program of Italian surgical residents and, despite regional differences, this survey highlighted the overall shortage of planning in the re-allocation of resources. 9
Conclusions
In the Niguarda hospital in northern Italy, otolaryngologists played a significant role in the team that has faced the health emergency working in synergy with anesthesiologists and contributing to lighten the workload of colleagues in the ICU. In the Policlinico Umberto I in central Italy, the otolaryngology surgical activity has been reduced to adapt to the restrictions and to the limited number of available anesthesiologists; however, a significant number of oncology procedures was performed.
The main limit of this study is that it only included two large hospitals and, therefore, results cannot be generalized on a national level. However, the comparison of two similar otolaryngology units in hospitals in northern and central Italy suggests that the healthcare system may have been affected differently across the country.
Even in the difficult scenario of the COVID-19 pandemic, otolaryngology proved to be an essential discipline. In the most affected regions, otolaryngologists contributed to optimize the workforce at the ICU, collaborating with anesthesiologists and resuscitators. In the less affected areas, otolaryngology focused more on the treatment and diagnosis of malignant diseases, ensuring adequate assistance in terms of early diagnosis and appropriate treatment. The different number of diagnostic and therapeutic procedures in oncology patients may have a significant impact in the near future, as it may cause delayed diagnosis and treatment of oncology patients.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Availability of data and materials
The datasets used and/or analysed during the current study are available from the corresponding author on reasonable request.
