Abstract
The most common method for SARS-CoV-2 testing is throat or nasal swabbing by real-time reverse transcription polymerase chain reaction (RT-PCR) assay. In South Korea, drive-through swab test is used for screening system and community treatment centers (CTCs), which admit and treat confirmed COVID-19 patients with mild symptoms, are being used. This retrospective study was conducted on patients admitted to a CTC on March 6, 2020. A total of 313 patients were admitted. The nasal and throat swabs were collected from the upper respiratory tract, and a sputum test was performed to obtain lower respiratory samples. The positive rate of the first set of test, sputum test was higher than that of the swab test (
Introduction
In December 2019, an outbreak of an unknown pneumonia began in Wuhan, China. A virus, now called severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2), was found to be the pathogen. 1 SARS-CoV-2 has been reported to cause a wide range of symptoms; some people remain asymptomatic or exhibit only mild symptoms, such as headache and fever, while others develop severe symptoms such as dyspnea, sepsis, and acute respiratory distress syndrome. The disease is called COVID-19.2,3 The most common method for SARS-CoV-2 testing is detection of the viral ribonucleic acid (RNA) sequence through throat or nasal swabbing by real-time reverse transcription polymerase chain reaction assay (RT-PCR). 4 However, problems with sample collection and diagnostic kits, among other issues, have occurred with use of RT-PCR. 5 In addition, other studies have reported that a sputum test is more sensitive than nasal or throat swabs, so debate remains regarding the optimal diagnostic method. 6 Without diagnostic tests, young and healthy people, who are often asymptomatic or only mildly symptomatic, are likely to silently spread the virus throughout the wider community. 7 Therefore, isolation and treatment of both severely ill and healthy, asymptomatic patients is important.
In South Korea, March 2021, a total of 104,194 COVID 19 has been confirmed, and the number of deaths has reached 1737. And while vaccination is actively progressing, COVID-19 patients and deaths continue to increase. The United States and European countries are also experiencing rapid increases in the number of cases of, and deaths from, COVID-19. In Korea, to prevent the increase and transmission of COVID-19, cohort quarantine was initiated for people entering from foreign countries, and the spread of the virus was effectively controlled by the wearing of masks and strict social distancing. To effectively distribute medical resources and prevent transmission of the virus, community treatment centers (CTCs), which admit and treat only confirmed COVID-19 patients with mild symptoms, are being used. The patients were admitted to a CTC of the Cheonan Postal Service Institute. The CTC is a novel quarantine treatment facility used in Korea to improve accessibility to medical services, and isolate asymptomatic and mildly symptomatic COVID-19 patients. In addition, it helps to ensure that medical resources for severely ill patients are appropriately allocated by distinguishing them from mildly symptomatic patients. CTCs are cost-effective, save resources, and prevent disease transmission; moreover, they can effectively cope with an outbreak of COVID-19 or other infectious diseases. 8
In addition, diagnostic testing in Korea using drive-through and walk-through methods has attracted attention worldwide because it allows a large number of tests to be carried out with minimal contact among people. This method is very useful for screening test to minimize the transmission from patient to medical staff. However, this method may has limitations because it uses the swab test. Therefore, we analyze the swab test and sputum test at the CTC to confirm the limitations that can occur when only the swab test is performed.
Methods
Participants and data collection
This retrospective study was conducted on asymptomatic and mildly symptomatic patients admitted to a CTC located at the Cheonan Postal Service Training Center, Korea, on March 6, 2020. The patients were confirmed as having COVID-19 by other medical institutions prior to admission, with intervals of up to 3–23 days before admission. During the admission period, medical personnel, who were equipped with level D protection to prevent infection, attended to and monitored patients twice daily. The nasal and throat swabs were collected from the upper respiratory tract, and a sputum test was performed to obtain lower respiratory samples. There was a possibility of aerosol generation during sputum collection, so the sputum was collected in a negative pressure chamber. Discharge decisions were based on the swab and sputum tests for SARS-CoV-2; when all RT-PCR test results within a 24-h period were negative, discharge was permitted. If the swab was negative twice but sputum results were inconclusive, patients were released from quarantine according to the Korea Centers for Disease Control and Prevention guideline (Figure 1).

Study population and test algorithm.
Also, if the initial test after admission was negative, but in serial test continued show positive results defined as a possible false negative case. A possible false positive case was defined if the patient had a positive result again despite the three or more consecutive negative results. Patients were classified as children and adolescents (<20 years of age; junior group), adults (20–40 years of age; “transition” group), or middle-aged and older (>40 years of age; senior group). The disease duration was defined as the period from the time of diagnosis to the end of quarantine.
RT-PCR assay for SARS-CoV-2
The RT-PCR test for SARS-CoV-2 was performed using the Allplex™ 2019-n-CoV-assay (Seegene®, Seoul, ROK), and aimed to detect the envelope gene, RNA-dependent RNA polymerase gene, and nucleocapsid protein gene. The cycle threshold (Ct) value means the cycle in which virus is detected through virus amplification, and the lower the Ct value, the higher the amount of viral load. The Ct value of all genes was detected less than 40 cycles was defined as positive. 9
Statistical analysis
The normality of continuous variables was confirmed using the Shapiro–Wilk test; these data were analyzed using Student’s
Ethics approval
The study protocol was approved by our Institutional Review Board (IRB No. 2021-03-031) and conducted in accordance with the provisions of the Declaration of Helsinki.
Results
A total of 313 patients were admitted to the CTC on March 6, 2020. Seven patients in whom initial samples had been collected inappropriately were excluded from the analysis. Finally, 306 patients were enrolled (Figure 1).
General characteristics
The mean age of the 306 patients was 30.7 years. The mean duration of disease was 25.74 ± 7.8 days. In total, 145 (47.4%) patients were asymptomatic and 161 (52.6%) were symptomatic. The most common symptoms were cough (
General characteristics.
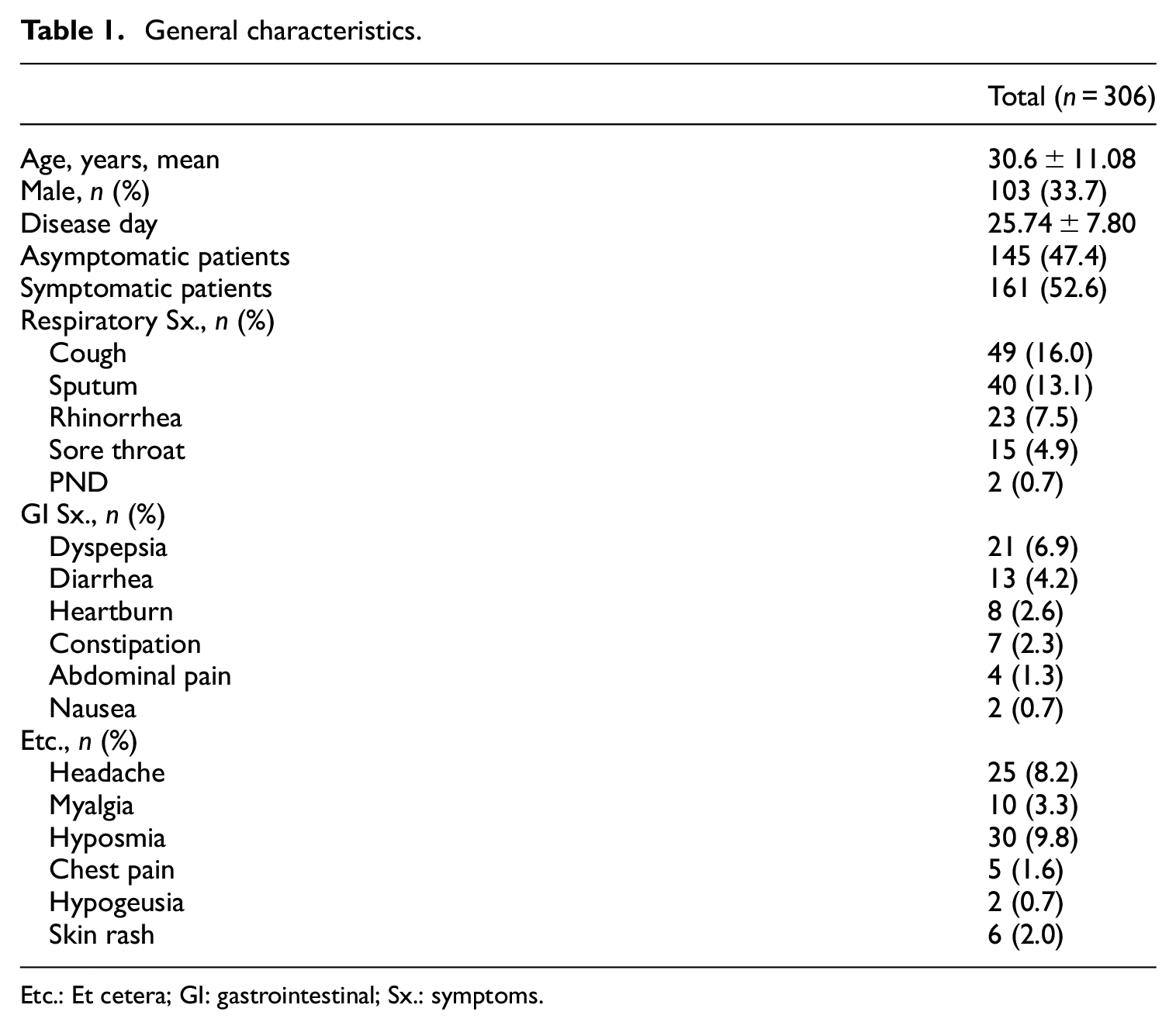
Etc.: Et cetera; GI: gastrointestinal; Sx.: symptoms.
Comparison by groups
There were 103 males and 203 females, with a mean age of 28.62 ± 10.11 and 31.70 ± 11.42 years, respectively (
Comparison by gender.
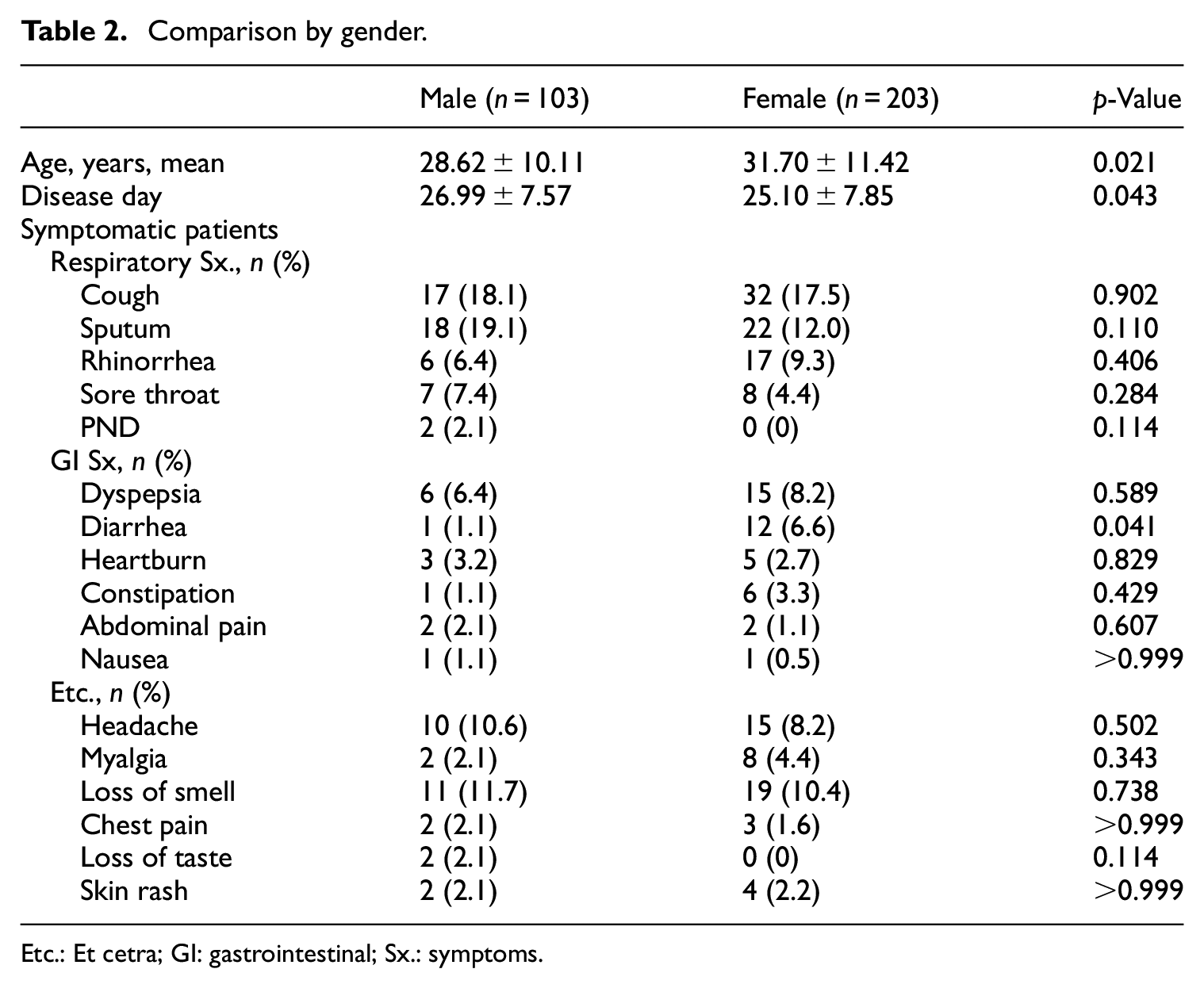
Etc.: Et cetra; GI: gastrointestinal; Sx.: symptoms.
There were 15 (4.9%) patients in the junior group, 218 (71.2%) in the transition group, and 73 (23.9%) in the senior group. There was a significant difference in disease duration between the junior and senior groups (30.53 ± 5.37 vs 23.71 ± 7.78 days;
Comparison by age group.

GI: gastrointestinal; Sx.: symptoms.
Two groups showed statistically significance in post-hoc analysis.
Difference between swab and sputum tests
The first set of RT-PCR test
The first RT-PCR tests after admission to the CTC, using swab and sputum samples, were performed in 306 patients: the results were inconclusive for 84 (27.5%) and 87 (28.2%), negative for 140 (45.8%) and 107 (35.1%), and positive for 82 (26.8%) and 112 (36.7 %), respectively (
Comparison of swab test versus sputum test (first initial test and consecutive results at 24-h interval).

The second set of RT-PCR test
For the 222 patients who did not meet the discharge criteria, a second examination was performed 1 week later. The results of the swab and sputum tests were inconclusive for 77 (34.7%) and 64 (28.8%) patients, negative for 87 (39.2%) and 115 (51.8%), and positive for 58 (26.1%) and 43 (19.4%), respectively (
Comparison of swab test versus sputum test (second initial test and consecutive results at 24-h interval).
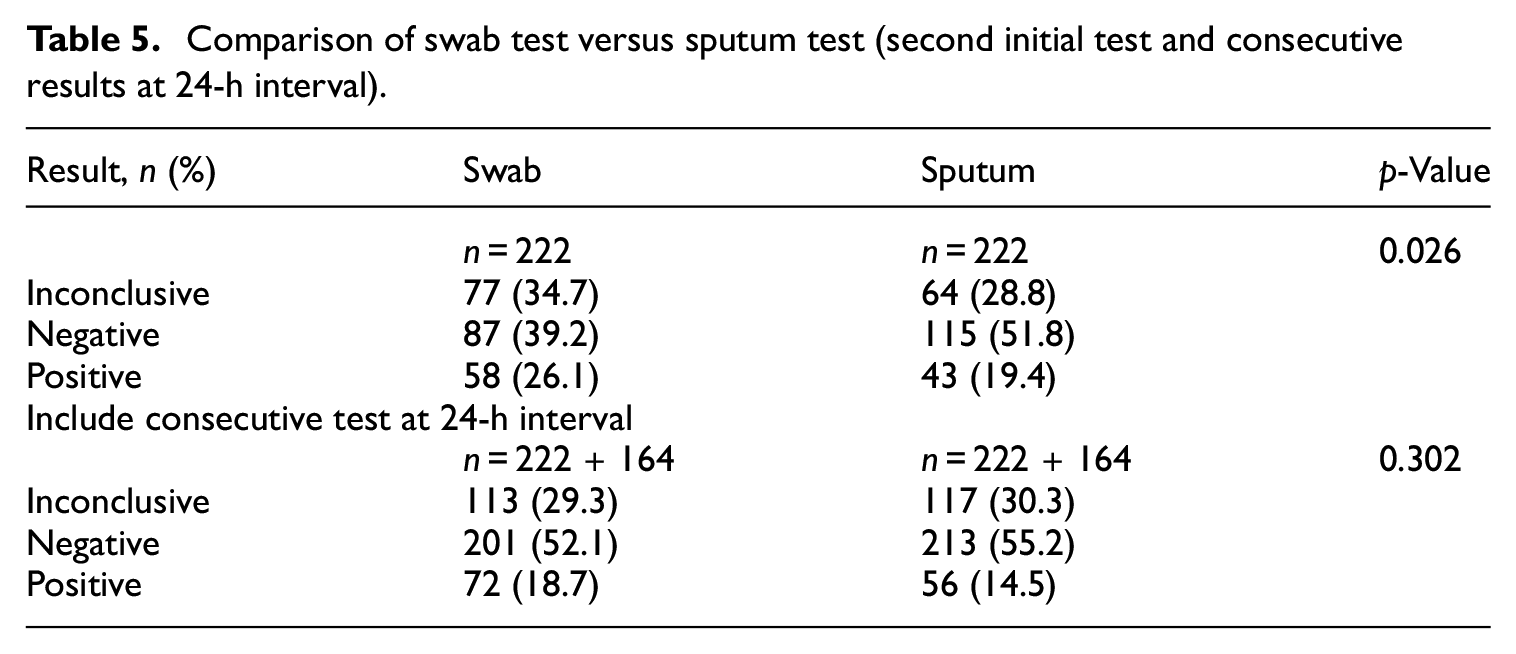
Possible false negative and false positive
The RT-PCR tests show possible false negative cases were 9 (2.94%) in swab test and 7 (2.28%) in sputum test. Possible false positive cases were 3 (0.98%) in both specimens respectively.
Consecutive negative results
In the first set of test, 66 of 152 (43.4%) patients showed consecutive negative swab test results, thereby satisfying the indication for discharge. However, when the sputum test results were considered together, that number fell to 29 patients (19.1%) (

Comparison of consecutive negative results between swab only and swab plus sputum.
Discussion
Appropriate sampling and testing is very important to detect respiratory system viruses. 10 To diagnose SARS-CoV-2 infection in suspicious cases, viral nucleic acid detection using a sample from the upper respiratory tract (obtained with a nasal or throat swab) has commonly been used. 11
However, there have been reports that the results of these RT-PCR tests differ depending on whether swab or sputum samples are used.5,6,12 In this study, we analyzed the general characteristics of asymptomatic and mildly symptomatic patients, and compared nasal and throat swab RT-PCR test results with those obtained using sputum samples. We found that the sputum test was more sensitive for detecting patient with virus shedding and it is more helpful to determining whether to release patients from quarantine, and for initial diagnosis, compared to the swab test alone. In addition, in other studies of the same population group, it is confirmed that the Ct value of the swab test is generally higher than that of the sputum. 9 It can be recognized as dead viral particles until now, but it is very important to recognize these characteristics in a pandemic situation because the infectivity of virus cannot be completely excluded.
Patients between the ages of 20 and 39 years accounted for 71.2% of the cohort. Relatively young and healthy people with COVID-19 usually have no, or only mild, symptoms. The typical recovery time of COVID-19 patients is known to be approximately 2–6 weeks. 13 In this study, the mean duration of disease was in line with this, at 25.74 ± 7.80 days. Respiratory system symptoms, such as cough and sputum, were the most frequent symptoms among our cohort; also, some patients had digestive system symptoms, such as indigestion and diarrhea, while others experienced a loss of smell or taste. Therefore, it is important to check not only for respiratory symptoms, but also for digestive and other non-specific symptoms. However, all of the patients admitted to the CTC were hemodynamically stable, in terms of blood pressure, heart rate, and respiratory rate, regardless of symptoms.
The ratio of women to men was relatively high in this CTC (103 males and 203 females). Disease duration differed by gender, being 26.99 ± 7.57 days for males and 25.10 ± 7.85 for females (
Previous studies have shown that children suffer less severe symptoms of SARS-CoV-2 than adults.14,15 Our junior group consisted of 15 people, thus accounting for a relatively small proportion of the patients. However, the CTC discharge time was longer than that for the senior group (30.53 ± 5.37 vs 23.71 ± 7.78 days;
In this study, the positive rate of the first sputum test after entering the CTC was higher than that of the first swab test. This is because SARS-CoV-2 mainly affects lung and lower respiratory tract cells, 12 and it has been shown that the viral load is higher in sputum than throat or nasal swabs. 16 Thus, the sputum test is more sensitive for early stage SARS-CoV-2. In drive-through facilities and screening tests, where only swab tests are performed, COVID-19 patients may be missed. Thus, in the early stages of the disease, it is important that sputum tests be performed as well as swab tests.
In the second set of tests conducted in this study, 1 week after the first ones, the rate of positive swab tests was relatively high. As patients recover from COVID-19, the virus remains in the upper rather than lower respiratory tract. Nevertheless, the rate of positive sputum tests was high, at 19.4%. There was no significant difference in the positivity rate between the two samples, even after hours. Over time, the rate of positive swab tests may be higher than that of sputum tests, but not necessarily significantly. Difficulty in making a diagnosis of SARS-CoV-2 based on only one test has been known; this was supported by the results of our study.
About the RT-PCR test for confirming COVID-19, a false negative rate of initial test is reported 0.018–0.58, 17 and false positive rate is reported 0.008–0.04. 18 This results may differ from commercial RT-PCR diagnostic kits. The Allplex™ used in this study reported high specificity and sensitivity.19,20 In this study, possible false negative cases were found 9 (2.94%) in swab test and 7 (2.28%) in sputum test. Possible false positive cases were 3 (0.98%) in both specimens respectively. However, it is cautious to generalize because this result is from the COVID-19 confirmed patients. Also, in Korea, pulmonary tuberculosis is prevalent, all nation people had BCG vaccination during childhood. There have been reported about Bacillus Calmette–Guérin vaccination could affect COVID-19 infection.21–24 Therefore, it may be need to reconsider the criteria for discharge and quarantine criteria for COVID-19 patients and the validity of the post-recovery PCR test. 25
Finally, we compared the results of swab-alone and swab-plus-sputum tests. When swab and sputum test results were considered together in both the first and second set of testing, the rate of negative result was reduced by half compared to the swab test alone. Thus, using the swab test alone may increase the risk of social transmission, because patients who may have tested positive in the sputum test can be missed. Therefore, it is concerned that only swab test is performed as screening test.
The limitations of this study were as follows. Because data from a single treatment center was analyzed, the generalizability to other regions, in Korea and worldwide, may be limited. Although there have been reports on severe cases of COVID-19 worldwide, further studies are needed to understand the characteristics of the virus in asymptomatic and mildly symptomatic cases. Moreover, the RNA profiles of viruses evolve differently among countries. Nevertheless, understanding the characteristics of Asian viruses could be highly instructive regarding the response of the international community to pandemics. Our results could also be used as background data for future studies of mutations.
Conclusion
Although swab tests using the drive-through method are widely employed to test for SARS-CoV-2, there is a concern that some cases may be missed. Therefore, a sputum test should also be conducted together for screening test.
Footnotes
Author’s Note
Hyo Jeong Choi is currently affiliated with Department of Emergency Medical trainee, Sunmoon University, Asan, Republic of Korea.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by the Soonchunhyang University Research Fund.
