Abstract
Objective:
Worldwide, little information is available about the extent to which children with mental disorders in the general population receive treatment from health professionals that meets minimal clinical practice guidelines. This study identifies the percentage of 6–17 year olds with mental disorders in the 2013–2014 Australian national survey of mental health who had sufficient contact with health professionals during the 18 months after the survey to have received treatment meeting criteria for minimally adequate treatment (MAT). It also identifies factors associated with children having this level of contact with health professionals.
Method:
Mental disorders were identified using the Diagnostic Interview Schedule for Children Version IV completed by parents. Health professional attendances and psychotropic medications dispensed were identified from linked national Medicare Benefits Schedule and Pharmaceutical Benefits Scheme records.
Results:
Only 11.6% (95% confidence interval [CI] [9.1, 14.8]) of children with disorders (
Conclusion:
During the 18 months after being identified with a mental disorder, only a small percentage of children have enough contact with health professionals to allow provision of MAT. This may be contributing to the unchanging high prevalence of childhood mental disorders.
Introduction
Over the last 20 years, there has been little change in the high prevalence of child and adolescent mental disorders reported in many countries (Sawyer et al., 2018a). One hypothesis that may help explain this is that treatment provided to children with mental disorders in the general population often fails to meet minimal standards required by clinical practice guidelines (for brevity, the term ‘children’ will be used to describe children and adolescents in this manuscript; Jorm et al., 2017). To date, however, there is little information about the extent to which the timeliness and amount of contact children with disorders have with health professionals are adequate to meet minimal standards recommended by clinical practice guidelines. There is also little information about the proportion of children with mental disorders in the general population who have a level of impairment that would benefit from treatment and who receive the treatment that is appropriate to their condition (De Silva et al., 2014). Information in both these areas is essential for effective service planning (De Silva et al., 2014; Jorm et al., 2017).
Most studies investigating patterns of service use by children with mental disorders have two important limitations. First, they typically employ a dichotomous indicator of service use that solely records contact versus no contact (Costello et al., 2014; Morris et al., 2011; Wolport and Ford, 2015). When this is done, it is not possible to know whether contact comprised a single visit or included a sufficient number of timely attendances to allow delivery of treatment meeting minimal clinical practice guidelines. This is an important issue because interventions recommended in treatment guidelines for the management of childhood mental disorders such as major depressive disorder (MDD), anxiety disorders (ADs), attention-deficit/hyperactivity disorder (ADHD) and conduct disorder (CD) uniformly require multiple contacts with service providers (National Institute for Health and Care Excellence, 2016, 2017a, 2017b). Reflecting this, Saloner et al. (2014) suggested that a minimum of four visits plus medication or eight visits without medication are required to achieve ‘minimally adequate treatment’ (MAT) for children with depression or ADHD. These recommendations are consistent with results from an earlier study reporting that eight or more sessions of outpatient psychiatric treatment were required to achieve ‘real improvement’ in the psychiatric symptoms experienced by a representative community sample of 997 children with mental disorders or psychiatric symptoms in the United States (Angold et al., 2000: 158). They are also consistent with standards utilised for this purpose in studies of adults (Harris et al., 2015).
Second, all previous studies of service use by children with mental disorders in the general population have relied on informant reports, typically parents, of service use that took place prior to the assessment of child, parent and family problems. This creates two problems for interpretation of results. First, the assessment of children’s disorders and key predictor variables after treatment has occurred makes it possible that the level of problems identified may not reflect those that were present before services were accessed. For example, family problems which may have encouraged help seeking before treatment commenced may have resolved following treatment by a health professional. Second, it is possible that parents may not accurately recall contact with health professionals, particularly if this took place months or even years earlier (Rhodes and Fung, 2004; Sawyer et al., 2018b).
This study had three aims: (1) to assess the level of contact 6–17 year olds in Australia had with health professionals during the 18 months after they were identified as having MDD, AD, ADHD and/or CD in the Australian Child and Adolescent Survey of Mental Health and Wellbeing (Lawrence et al., 2015), (2) to identify the percentage of children with these disorders having sufficient contact to allow delivery of MAT and (3) to identify factors associated with children having received sufficient contact to allow delivery of MAT.
Methods
Study design and participants
The participants were 6–11 and 14–17 year olds who were identified as having a mental disorder in the second Australian Child and Adolescent Survey of Mental Health and Wellbeing, and for whom consent was provided to access children’s Medicare Benefit Schedule (MBS) and Pharmaceutical Benefit Scheme (PBS) health records (Australian Government Department of Health, 2018a, 2018b; Lawrence et al., 2015). Australian Government regulations for access to MBS and PBS data require consent from parents if children are <14 years and consent from parents and children aged ⩾14 years. For children aged 12–13 years, consent for children’s participation in the survey was obtained from parents. However, this was insufficient for permission to access MBS and PBS prospective data because children would have been aged 14 years by the end of the follow-up period. As such, we were not able to obtain these data for children with disorders who were aged 12–13 years (
The design of the survey has been described in detail elsewhere (Hafekost et al., 2016; Lawrence et al., 2015). In brief, the survey used a multi-stage area-based sample selection procedure to ensure proportional representation of geographic areas across Australia (Hafekost et al., 2016; Lawrence et al., 2015). It identified a random probability-based sample of 6310 parents/carers of 4–17 year olds (response rate = 55%) who completed interviews with trained fieldworkers. Survey weights were developed accounting for the original probability of selection for each child, variations in response rates and in consent rates by age of children in the family and to benchmark them to the age–sex distribution of the population of children aged 6–17 years in Australia as determined by the Australian Bureau of Statistics (2016).
Written informed consent was obtained from parents, and from 14–17 year olds for MBS and PBS access. The study protocol was approved by the Australian Government Department of Health Ethics Committee (number 17/2012) and The University of Western Australia Human Research Ethics Committee (number RA/4/1/5538).
Measures
Sociodemographic information included family structure (single versus two parent households), household income and household location (metropolitan versus rural), and was collected using Australian Bureau of Statistics (2014) standard formats. Parent-perceived need for help was based on a report that children identified with mental disorders in the survey had used services for help with emotional and behavioural problems during the previous 12 months (and their parent considered that they needed this help) or that the parent considered that children needed help but it had not been accessed.
Information about attendances with general practitioners, paediatricians, psychologists, psychiatrists, social workers and occupational therapists was obtained from linked administrative data in the MBS (Australian Government Department of Health, 2018a). The MBS provides fees for medical practitioners’ services in Australia, including specialists, and for specific services provided by psychologists, social workers and occupational therapists. The MBS items used in this study to identify attendances with each of these health professionals relevant to children’s mental health problems are shown in Supplementary Table 2. Linked data from the administrative records of medicines dispensed through the PBS in Australia were used to identify children who had been treated with psychotropic medication (Australian Government Department of Health, 2018b). The PBS provides government-subsidised medicines for most medical conditions, including mental disorders. The linked PBS data contained details of all dispensed medications under the scheme, excluding medications supplied by hospitals and a very small number of non-approved pharmacies (Page et al., 2015). The psychotropic medications dispensed for children in the study are shown in Supplementary Table 3.
Statistical analyses
Using linked data from MBS and PBS records, all children were assigned to one of the three groups based on their level of contact with health professionals and their treatment with psychotropic medication during the 18 months after they were identified as having a mental disorder: (1) contact that met study criteria for MAT (i.e. 4–7 visits with a health professional plus concurrent medication or ⩾8 visits with or without medication, within a 12-month period after a child’s first contact with the health professional), (2) contact that did not meet criteria for MAT (i.e. 1–3 visits or 4–7 visits without medication, within a 12-month period) and (3) no contact with a health professional.
All statistical analyses were conducted using the Stata software version 15.1 ‘svy’ procedure to account for the clustered nature of the sample design and the use of survey weights (StataCorp, 2017). For ease of presentation, the initial results tables show prevalence estimates and 95% confidence intervals (CIs). Logistic regression was used to examine the strength of the relationship between level of treatment contact during the 18-month study period, and child and family characteristics, child diagnosis, child level of functioning, parent perceptions of need for help and children’s history of previous service contact. In these analyses, two sets of logistic regression models were fitted. Initially, bivariable logistic models were used to assess the strength of the relationship between level of treatment contact and each predictor variable. Subsequently, a single multivariable model was produced, in which all the predictor variables were included in the model to identify the strength of the relationship between level of treatment contact and each predictor variable, after adjusting for the effect of the other predictor variables. All results report sample numbers and weighted percentages unless otherwise indicated.
Data sharing
The 2013–2014 National Survey data set is available to research professionals through the Australian Data Archive (Zubrick et al., 2014). The linked MBS/PBS data will be available in the same location shortly.
Results
Participant characteristics
The demographic and psychosocial characteristics of children in this study (
Contact with health professionals
During the 18-month follow-up period, 47.4% (
Only 11.6% (
Percentage [95% CI] of children meeting criteria for minimally adequate treatment.
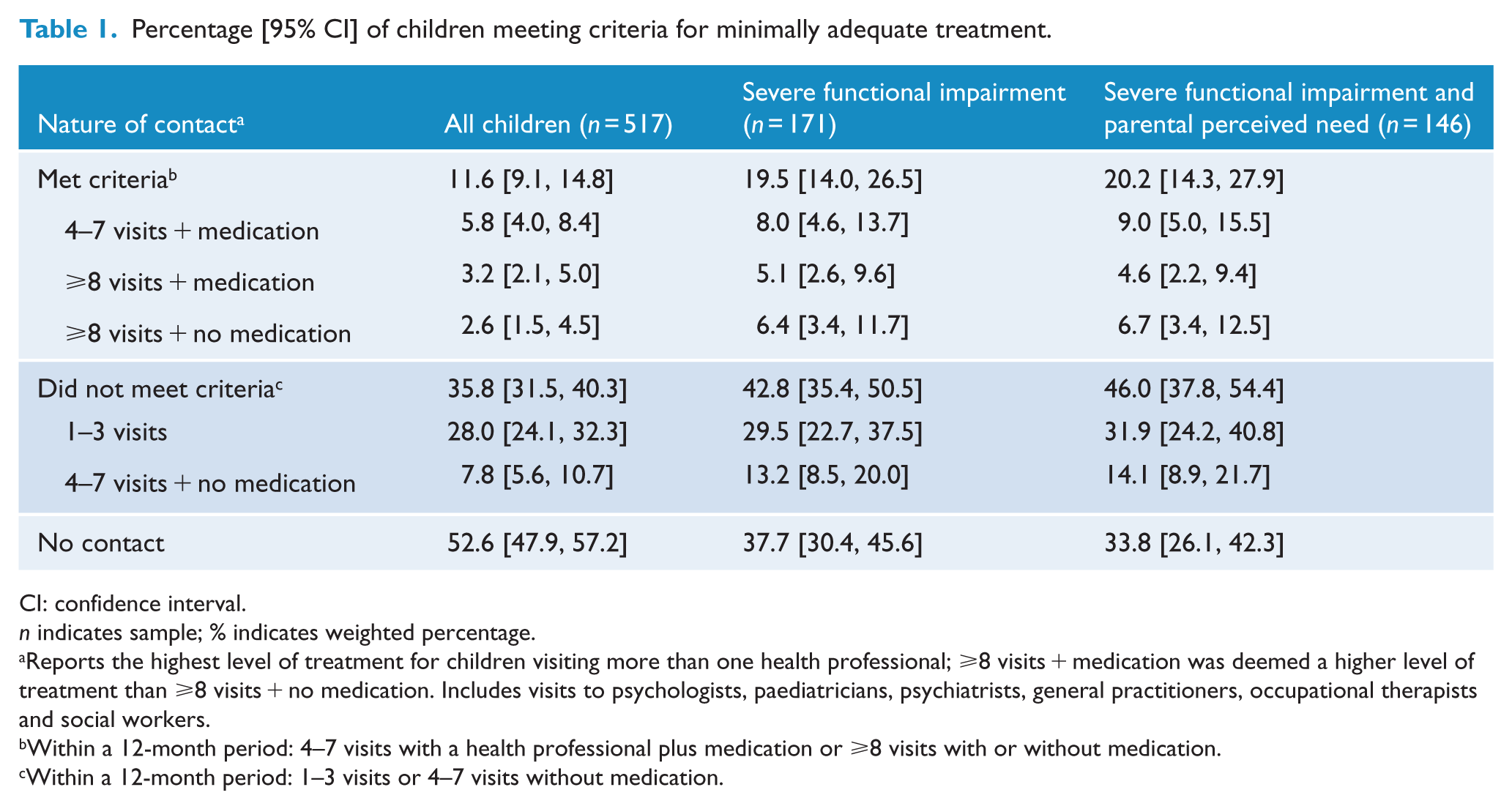
CI: confidence interval.
Reports the highest level of treatment for children visiting more than one health professional; ⩾8 visits + medication was deemed a higher level of treatment than ⩾8 visits + no medication. Includes visits to psychologists, paediatricians, psychiatrists, general practitioners, occupational therapists and social workers.
Within a 12-month period: 4–7 visits with a health professional plus medication or ⩾8 visits with or without medication.
Within a 12-month period: 1–3 visits or 4–7 visits without medication.
Factors associated with health professional contact
As compared to children who had no contact with health professionals, a higher percentage of children whose contact with health professionals met MAT criteria had depressive disorders, a more severe level of functional impairment, ⩾2 comorbid disorders, parents who perceived their child needed help and/or ⩾4 visits with health professionals during the 2 years prior to the National Survey (Table 2). A similar pattern of differences was evident between children who had contact that met MAT criteria and those whose contact did not meet these criteria (Table 2). However, the size of the differences between these latter groups was smaller.
Demographic and psychosocial characteristics (% [95% CI]) of children meeting minimally adequate treatment criteria in the 18-month follow-up period (
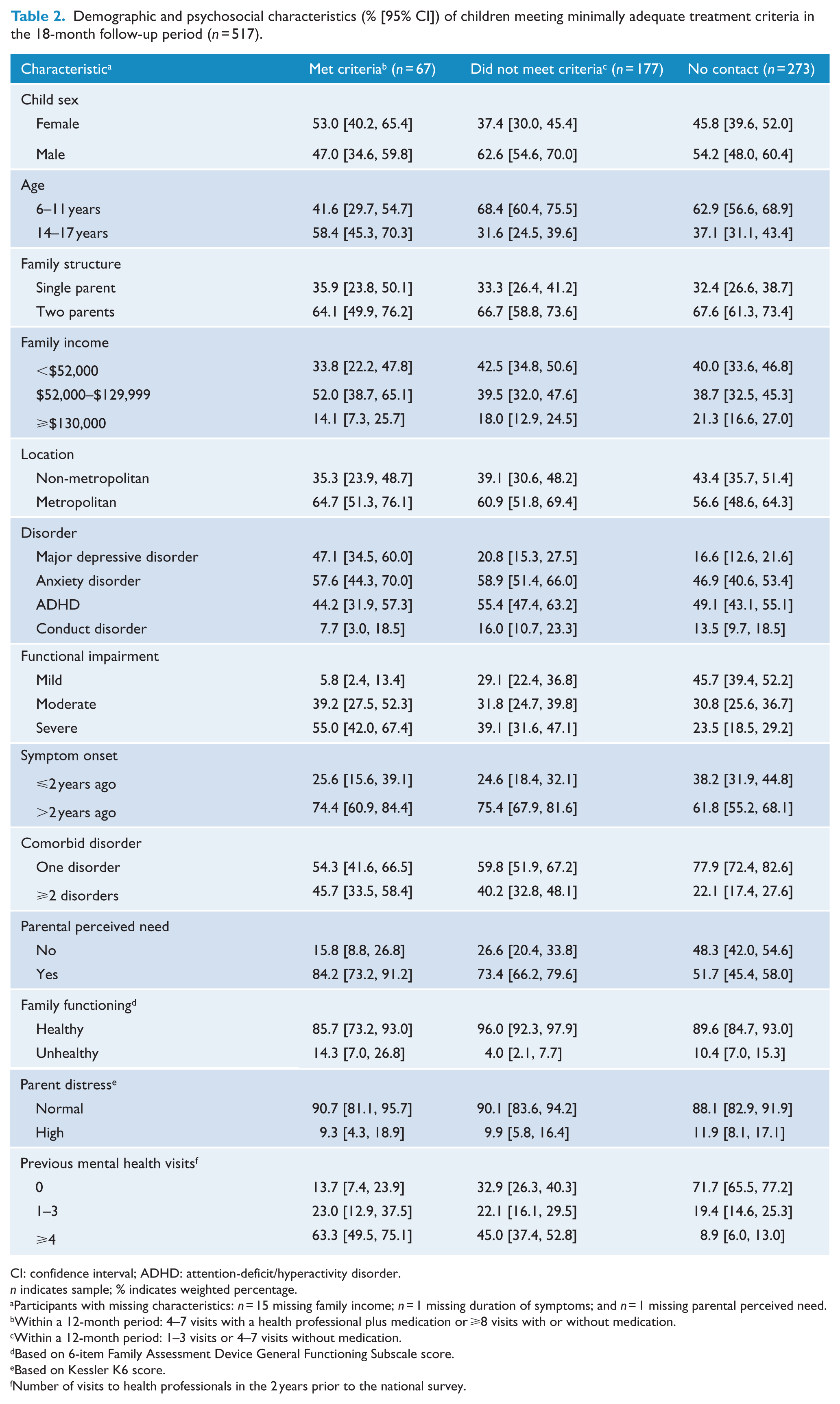
CI: confidence interval; ADHD: attention-deficit/hyperactivity disorder.
Participants with missing characteristics:
Within a 12-month period: 4–7 visits with a health professional plus medication or ⩾8 visits with or without medication.
Within a 12-month period: 1–3 visits or 4–7 visits without medication.
Based on 6-item Family Assessment Device General Functioning Subscale score.
Based on Kessler K6 score.
Number of visits to health professionals in the 2 years prior to the national survey.
In the multivariable logistic regression models (Table 3), children whose level of care met criteria for MAT were 11 times more likely to have severe functional impairment and 10 times more likely to have moderate functional impairment than children who had no contact with health professionals. They were also more likely to have had the onset of their symptoms >2 years before the survey and to have attended health professionals during the previous 2 years. A similar pattern was evident between children who had sufficient contact to meet MAT criteria and those whose contact did not meet these criteria (Supplementary Table 4). However, the size of the odds ratios was consistently smaller in these latter comparisons.
Odds ratios [95% CI] for receiving minimally adequate treatment
a
versus no contact (reference category) with mental health professionals in the 18 months after diagnosis (
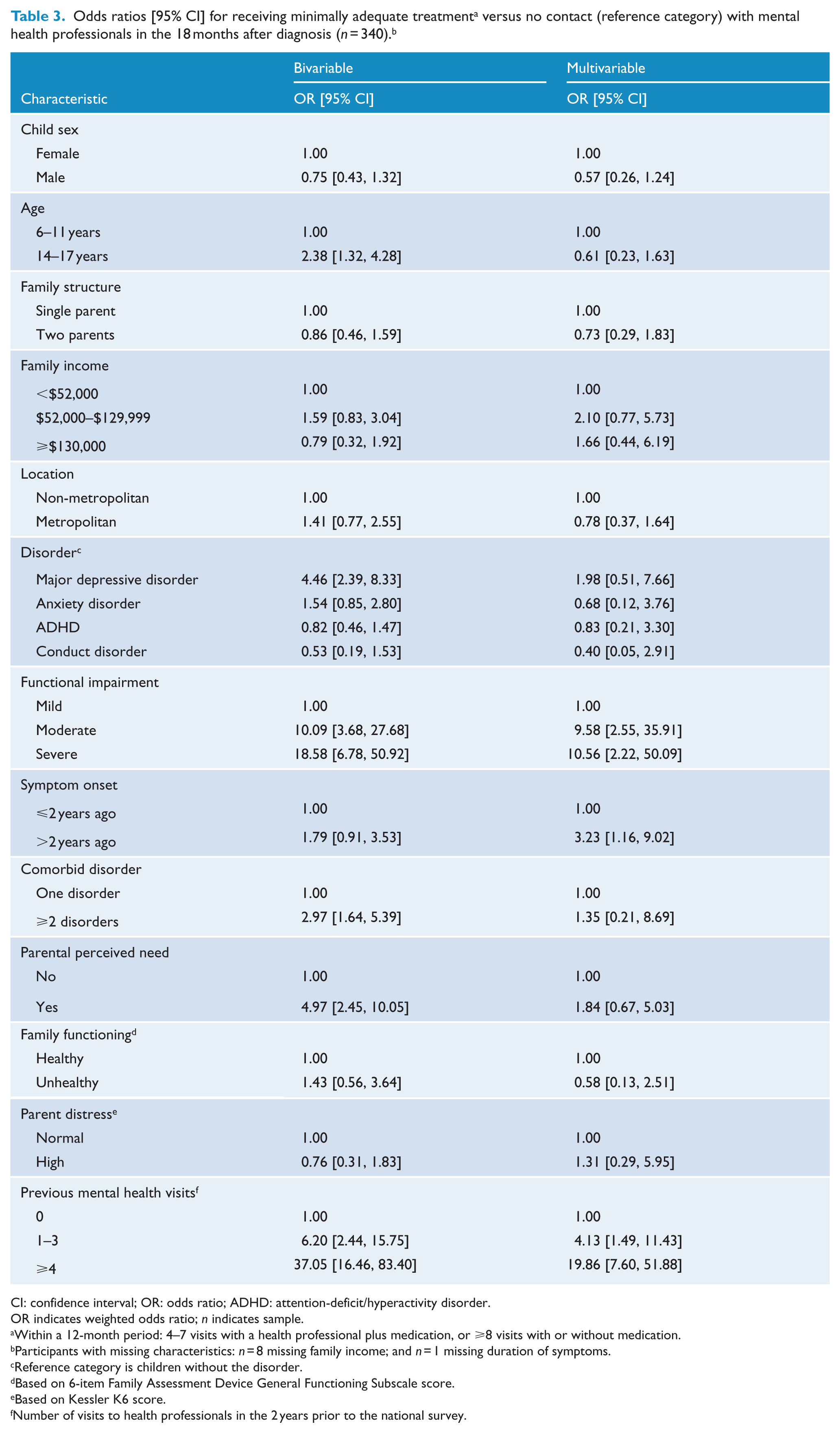
CI: confidence interval; OR: odds ratio; ADHD: attention-deficit/hyperactivity disorder.
OR indicates weighted odds ratio;
Within a 12-month period: 4–7 visits with a health professional plus medication, or ⩾8 visits with or without medication.
Participants with missing characteristics:
Reference category is children without the disorder.
Based on 6-item Family Assessment Device General Functioning Subscale score.
Based on Kessler K6 score.
Number of visits to health professionals in the 2 years prior to the national survey.
Sensitivity analyses
We undertook two sets of sensitivity analyses. First, children in Australia who attend psychiatrists, paediatricians or psychologists in government-funded hospitals or community child and adolescent mental health services may not have their attendances recorded in MBS. We investigated the potential impact of this on the results of the study by identifying children for whom there were parent-reported attendances in these settings but no MBS record during the year prior to the national survey (i.e. children who were receiving their care through a non-MBS-based service). In total, 42 children were reported by parents as having one or more such attendances. Extrapolating this to the 18-month follow-up period in this study suggests that 63 additional children (42 × 18/12 = 63) may have had contact with health professionals in a non-MBS-based setting during this period. Assuming that the same proportion of these 63 children had sufficient contact for them to receive MAT as the children in the MBS-identified group (i.e. 11.6%,
Second, the study follow-up period was limited to 18 months due to availability of post-survey MBS and PBS data. As such, it is possible that a longer period of follow-up would have identified additional health visits resulting in more children achieving the criteria for MAT. We investigated this in two ways. First, we investigated the percentage of children whose treatment achieved MAT criteria from 12 months prior to the survey to 18 months post-survey (i.e. a period of 2.5 years). The general pattern of results was similar to that reported for the 18-month period (Supplementary Table 5). As well, although a somewhat larger percentage of children had contact that met the criteria for MAT during this longer period (19.1%,
Discussion
The results from this study suggest that few children with MDD, AD, ADHD and CD in Australia have sufficient contact with health professionals to allow delivery of treatment meeting minimal clinical practice guidelines. For example, during the 18 months after they were identified as having one of these disorders, although 47.4% (
The relatively small number of children who had sufficient contact with health professionals to meet study criteria for MAT is consistent with results from previous studies. For example, in Great Britain, Meltzer et al. (2003) reported that over a 12-month period, only 25% of 5–15 year olds with a mental disorder had attended their general practitioner more than two times. In the United States, in a 1-year prospective study of 1007 children aged 9, 11 or 13 years at baseline, less than 10% used services during multiple 3-month periods across the year of the study (Farmer et al., 1999).
Jorm et al. (2017) have suggested that a potential reason for lack of change in prevalence of mental disorders among adults in the general population is that much of the treatment provided may fail to meet minimal standards of clinical practice guidelines. Support for this hypothesis was provided in results from a recent national study of adults with affective disorder and/or ADs in Australia, which found that only 16% of participants were receiving MAT, defined in a similar way to this study (Harris et al., 2015; Saloner et al., 2014). Results from this study suggest that a similar problem exists with the provision of treatment for children with mental disorders. It is plausible that failure to ensure that treatment provided to children with mental disorders in the general population meets minimal practice guidelines is contributing to the unchanging prevalence of child and adolescent disorders in Australia and other countries (Sawyer et al., 2018a).
There was little difference in the demographic characteristics of children who had contact with health professionals meeting the criteria for MAT and those who had no contact or contact not meeting these criteria. However, as compared to those who had no contact with a health professional, children with moderate or severe levels of functional impairment or children who had attended health professionals during the previous 2 years were more likely to have a level of contact that met criteria for MAT. Similar differences were evident between children whose contact met MAT criteria and those who had contact that did not meet these criteria. The results suggest that the level of children’s functional impairment rather than their demographic characteristics plays a key role in parent and clinician decisions about the provision of ongoing care and support. These findings are similar to that reported in one of the few previous studies to examine this issue which found that higher symptom levels among children were associated with persisting service use over a 12-month period (Farmer et al., 1999). They are also comparable to those reported in a prospective study of 4-year-old children which found that family burden and parent-perceived need for help when children were aged 4 years predicted service use when children were aged 7 years (Wichstrøm et al., 2014).
Strengths of this study include its national scope, the quality of its sampling methods, its use of well-established diagnostic criteria and methods, and its use of service information collected contemporaneously at the time of attendances. However, the study also has some limitations. First, the response rate in the national survey was 55%. Extensive checking showed that the participants in the survey were highly representative of the national population of 4–17 year olds (Hafekost et al., 2016; Lawrence et al., 2015). However, it is possible that inclusion of children who did not participate may have changed population estimates. Second, diagnostic information was limited to parent-report, and it is possible that additional information from other informants such as children or teachers may have altered the proportion of children who met the criteria for having a mental disorder. Third, information about the extent to which attendances to general practitioners and paediatricians are for mental health services is limited. For example, Britt et al. (2016) reported that general practitioners may be providing help for mental health problems in some attendances billed as generic MBS item numbers rather than mental health MBS item numbers. As such, it is possible that some attendances to general practitioners and paediatricians in this study represent false positives or false negatives. Finally, it was beyond the scope of this study to investigate use of school-based services, but previous work has shown that these are also an important source of support for children with mental disorders (Lawrence et al., 2015). It was also beyond the scope of the study to determine the extent to which treatment was offered but not accepted or offered but not attended.
In conclusion, previous studies have highlighted a treatment gap between the prevalence of childhood mental disorders and the prevalence of health service contact by children with disorders in the general population. However, less attention has been paid to the quantity and quality of treatment received by those who do attend services. The results from this study suggest that successfully reducing the prevalence of childhood mental disorders will require greater efforts to ensure that children’s level of contact with health professionals is sufficient to allow delivery of treatment that meets minimal standards of clinical practice guidelines for the provision of evidence-based treatments.
Supplemental Material
Supplementary_tables – Supplemental material for Adequacy of treatment for child and adolescent mental disorders in Australia: A national study
Supplemental material, Supplementary_tables for Adequacy of treatment for child and adolescent mental disorders in Australia: A national study by Michael G Sawyer, Christy E Reece, Alyssa CP Sawyer, Harriet Hiscock and David Lawrence in Australian & New Zealand Journal of Psychiatry
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Funding
The
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
