Abstract
Background
The Dutch guideline algorithm for the analysis of anaemia in patients of general practitioners (GPs) was programmed in a Clinical Decision Support system (CDS-anaemia) to support the process of diagnosing the cause of anaemia in the laboratory. This research aims to assess the supplementary benefit provided by the automated algorithm in various demographic categories, including different sexes, age groups and severities of anaemia, in comparison to the manual diagnostic approach employed by GPs.
Methods
This was a retrospective cohort study of 5399 primary care patients where the cause of anaemia was diagnosed by GPs with or without the aid of CDS-anaemia within the age groups 18–44, 45–64, 65–79 and 80 and older. Anaemia was defined according to the Dutch College of General Practitioners (DCGP) guideline. Causes of anaemia were based on the DCGP guidelines with the corresponding blood tests. By calculation of rate ratios and percentage differences of the determined cause of anaemia we evaluated the effect of the diagnostic algorithm.
Results and conclusion
The percentage patients in which an underlying cause of anaemia was found increased 34 and 46 percentage points in females and males, respectively, when GPs were supported by CDS-anaemia compared to GPs who were not supported by CDS-anaemia. The highest increase in percentage points when CDS-anaemia was used, was found in younger- and middle-aged males and mild or moderate anaemia.
Introduction
Anaemia guidelines are instrumental in the work up of anaemia. When used consequently, anaemia algorithms guide the general practitioners (GP) to find the underlying cause of anaemia. However, several studies showed that the underlying cause of anaemia is not always revealed, particularly in younger males.1,2 We therefore developed an automated algorithm that supports GPs in finding the cause of anaemia according to the Dutch College of General Practitioners (DCGP) guidelines. This automated algorithm (CDS-anaemia) adds extra tests in a stepwise manner after anaemia is detected. We previously reported the marked effectiveness of CDS-anaemia by cause finding in patients from GPs supported by CDS-anaemia compared to patients from GPs who did the work-up manually. 3 Especially deficiencies and inflammatory diseases were shown to cause anaemia and by using CDS-anaemia the percentage of undetermined causes dropped from 64.7% to 24.9%. 3 It is, however, not known how effective an automated anaemia algorithm is in different age and sex groups and different severities of anaemia. This study investigates the added value in those subgroups.
Methods
Study design and data collection
The study design was identical to our previously published work. 3 In short, laboratory results showing the underlying cause of anaemia were compared between GPs aided by CDS-anaemia (CDS-group) and GPs that did the cause finding manually. The latter group was divided in three groups, that is, the same GPs before using CDS-anaemia (pre-CDS group) and a group of GPs not receiving CDS-anaemia assistance during the same time periods (control and pre-control). The anaemia algorithm was defined according to the DCGP criteria. 4 CDS-anaemia became activated when Hb and indices were requested for patients from selected GPs. Subsequently, CDS-anaemia added ferritin tests in all patients with anaemia. Depending on the results of ferritin and red cell indices tests might be added, that is, vitamin B12, folate, reticulocyte and LDH and/or CRP, iron, transferrin, eGFR, thrombocytes and leukocytes. After all tests were completed an interpretative comment was generated.
The data used for this analysis was requested between 11 November 2017 and 15 March 2020 (pre-control and pre-CDS group), and 11 November 2020 and 15 March 2023 (control and CDS-group).
Statistical analysis
To investigate differences between the study groups rate ratios (RR) and percentage point differences of the determined causes of anaemia were calculated for each specific patient group to determine the effectiveness of the CDS-anaemia in the different subgroups. The data were analysed with IBM SPSS Statistics version 29.
Results
This database yielded a retrospective cohort study of 5399 primary care patients where the cause of anaemia was diagnosed with (CDS-group) or without (pre-control, control and pre-CDS group) CDS-anaemia within the age groups 18–44, 45–64, 65–79 and 80 and older. Patient characteristics of the study groups are shown in addendum 1. Apart from a marginal lower haemoglobin (7.9 mmol/l) in the CDS-group as compared to 8.0–8.1 mmol/l in the other groups, there were no statistically significant differences in patient characteristics between the study groups. Since the pre-CDS group, pre-control and control groups were found not to be different, these groups were combined.
Rate Ratio and Difference of Determined Causes of Anaemia for Sex and Age Groups and Severities of Anaemia (CDS-Group Versus Control).
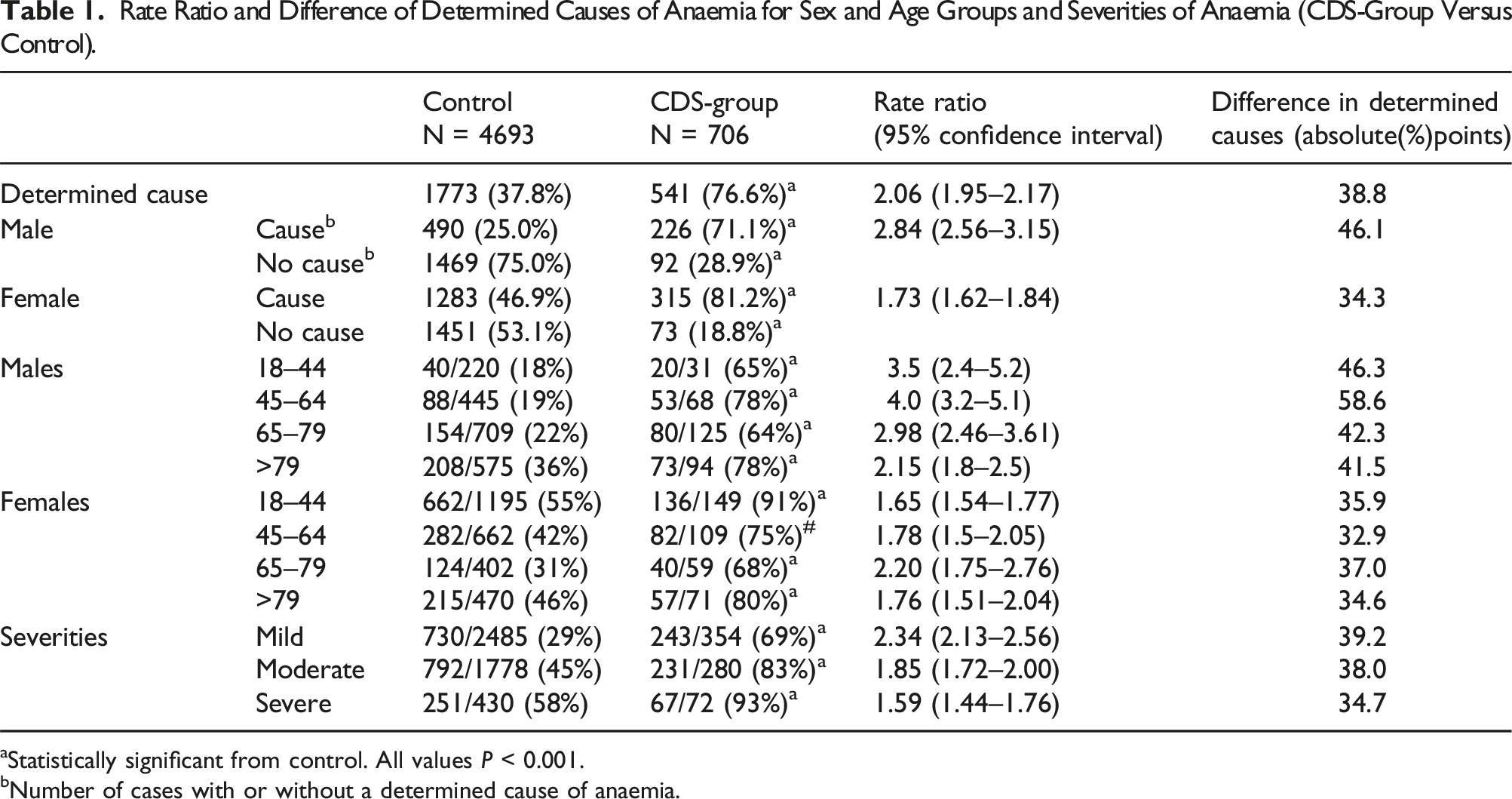
aStatistically significant from control. All values P < 0.001.
bNumber of cases with or without a determined cause of anaemia.
Males aged 18–44 and 45–64 years benefitted most of the CDS-anaemia support: the rate ratio and risk difference was increased the most (RR 3.5; increase 46.3% and RR 4.0; increase 58.6% resp.). The lowest impact was found to be for women aged 18–44 and 45–65 years (RR 1.65; increase 35.9% and RR 1.78 and increase 32.9% resp.). Furthermore, CDS-anaemia was more beneficial in mild and moderate anaemia (RR 2.34; increase 39.2% and RR 1.85; increase 38% resp.) then in severe anaemia (RR 1.59; increase 34.7%).
In all subgroups (age, sex and severity of anaemia), CDS-group GPs found more causes of anaemia. Interestingly in younger females and in patients with more severe anaemia 46% and 58% of underlying causes were already found by the GPs manually. These percentages increased to 81% and 93% when CDS-anaemia was used. In contrast, in younger- and middle-aged males and patients with mild anaemia an underlying cause of anaemia was found in 18, 19 and 29% of the cases by the GPs manually. These percentages increased dramatically when CDS-anaemia was used, resulting in rate ratios of 3.5, 4.0 and 2.3 and an absolute increase of 46%, 58% and 39%, respectively.
Discussion
This study investigates the efficacy of automated Clinical Decision Support for anaemia in identifying the causes of anaemia across various demographic groups, comparing its performance with GPs who do the work-up manually. This research reveals that: (1) GPs aided by CDS-anaemia consistently exhibit a superior ability to identify the aetiology of anaemia in both males and females across all age groups and (2) in patients with all severities of anaemia and (3) the results also suggest that CDS-anaemia is the most beneficial in assisting GPs when finding a cause of anaemia in males of all ages, (4) whereas added value of CDS-anaemia is the least when diagnosing females between the age of 18 and 44.
The discrepancy between men and women does not imply ineffectiveness of CDS-anaemia for women, but the data shows that GPs simply diagnose the underlying causes of anaemia more often in women than in men without the aid of CDS-anaemia. Notably, GPs are aware that anaemia within younger females is frequently attributed to iron deficiency resulting from menstrual bleeding.
Furthermore, this study also suggests that CDS-anaemia is most beneficial in assisting GPs in finding the cause of mild and moderate anaemia as compared to severe anaemia. Most likely, when examining patients with severe anaemia, GPs are more likely to proceed to further testing to find the underlying cause. In contrast, the subtle symptoms of mild anaemia may not trigger immediate concern among GPs. However, identifying the root cause of mild anaemia is crucial, as it allows for effective treatment, such as the provision of iron or vitamin B12 supplements.
In a study conducted by Schop et al., the effectiveness of an extensive work-up of laboratory testing in general practice for anaemia was assessed. 5 The results of that study align with the present study, indicating that automated programs, including CDS-anaemia, dramatically increase identification of underlying causes of anaemia.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethical approval
Not applicable.
Guarantor
BdB.
Contributorship
Conceptualization, study design and data collection: BADB and AMDJ; data preparation: TTVL; methodology: BADB, TTVL, KVS, AMDJ; investigation: TTVL, BADB and AMDJ; statistical analysis: TTVL, KVS; writing - original draft preparation: TTVL; writing - review and editing: BADB, FC, AMDJ. All authors have read and agreed to the published version of the manuscript.
Correction (October 2024):
Article updated to correct the values of male and female patients percentage in the results and conclusion section of the abstract.
