Abstract
Abstract
Introduction:
Near-infrared autofluorescence for the intraoperative identification of parathyroid glands is increasingly used. In addition to identifying normal parathyroid tissue for preservation, autofluorescence may be helpful in identifying abnormal parathyroid tissue because some studies have suggested that normal parathyroid tissue may have more intrinsic autofluorescence than abnormal parathyroid. 1 Small studies have suggested that patients with multiple endocrine neoplasia type 1 (MEN1) may have decreased parathyroid autofluorescence, potentially limiting the utility of this technology in these patients.2,3 We present two cases wherein autofluorescence effectively identified parathyroid tissue in patients with MEN1.
Methods:
Case 1: A 26-year-old woman was found to have primary hyperparathyroidism (calcium 10.3 mg/dL, parathyroid hormone [PTH] 98 ng/L) in the setting of MEN1. She underwent a nonlocalizing Sestamibi scan followed by ultrasonography that showed an abnormal right upper parathyroid gland. Case 2: A 51-year-old woman with MEN1 developed recurrent primary hyperparathyroidism 21 years after total parathyroidectomy and parathyroid autotransplantation into her left brachioradialis. The PTH from her left arm was 3745 ng/L compared with 145 ng/L from her right arm. Her calcium was 11.3 mg/dL. Ultrasonography showed a 1 cm cluster of hypoechoic nodules in the left forearm that had Sestamibi uptake.
Results:
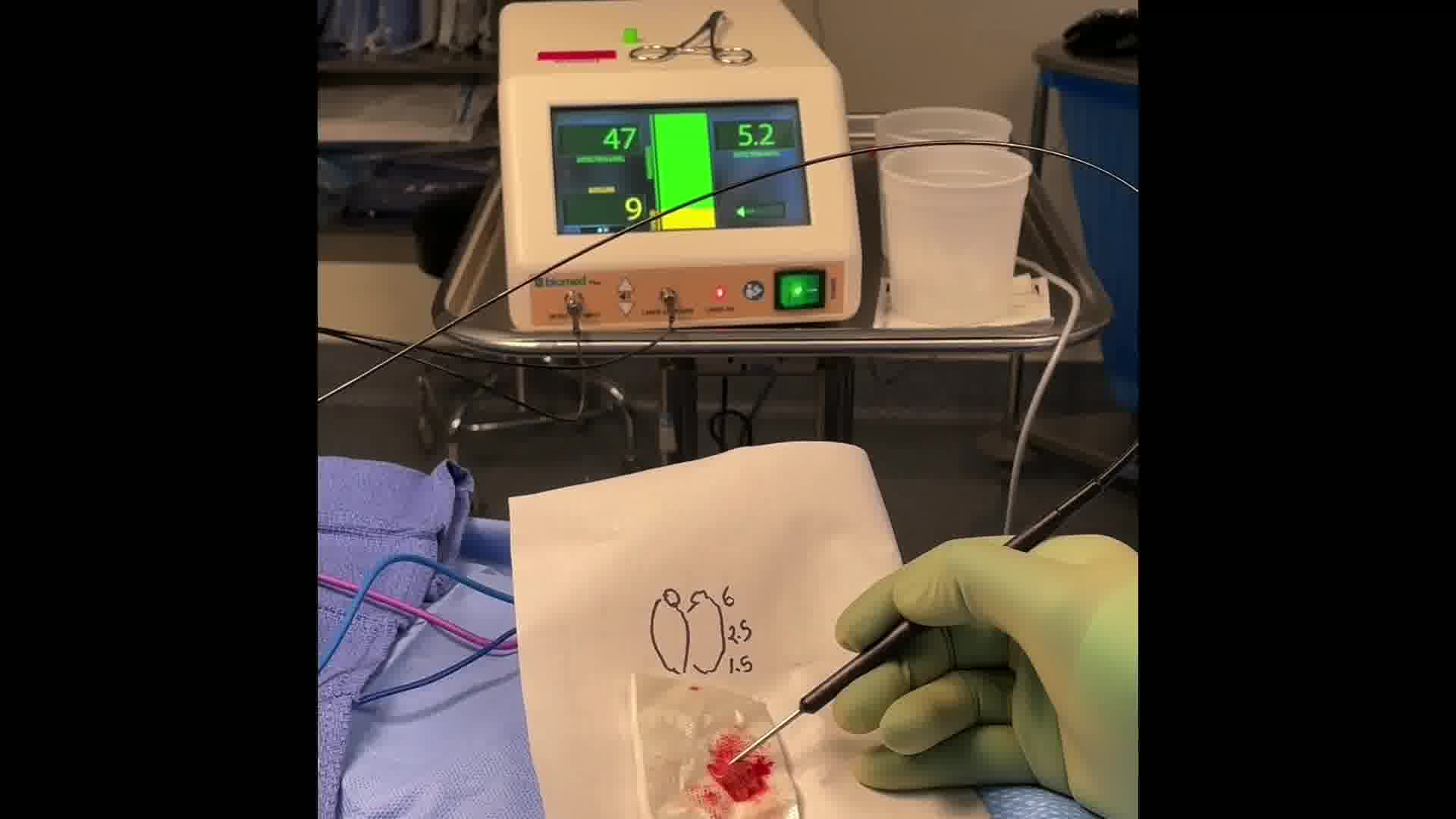
Case 1: After informed consent was obtained, we proceeded to the operating room for exploration. Using the PTeye and Fluobeam, we found heterogeneous autofluorescence of the right upper parathyroid nodule itself, with the highest signal in the normal-appearing cap, which was cryopreserved. We proceeded to bilateral exploration after insufficient PTH drop. We resected an abnormal left upper parathyroid gland and performed a left cervical thymectomy after failing to identify the left lower gland. The right lower gland was subtotally resected and also cryopreserved. Final pathology analysis confirmed hypercellular parathyroid tissue. Calcium was 10.1 mg/dL and PTH was 65 ng/L 1 month postoperatively. The patient will be followed closely by her endocrinologist given her risk of hyperparathyroidism recurrence. Case 2: After informed consent was obtained, we proceeded to the operating room for exploration of her left forearm. On exploration, palpation, ultrasonography, and the PTeye were used to identify three clusters of parathyroid tissue, one of which was cryopreserved. With PTeye, the autotransplanted parathyroid tissue had autofluorescence that was two to three times higher than the muscle background. Although Fluobeam did not detect any obvious parathyroid tissue
Conclusions:
These cases suggest that near-infrared autofluorescence can identify parathyroid tissue in MEN1 patients. Higher autofluorescence in the normal-appearing parathyroid tissue of MEN1 patients may guide cryopreservation. Autofluorescence can also aid excision of autotransplanted parathyroid tissue.
Consent: Authors have received and archived patient consent for video recording/publication in advance of video recording of procedure.
Funding: P.C.C. was supported by the National Center for Advancing Translational Sciences, National Institutes of Health, UCSF-CTSI [Grant No. TL1 TR001871] and the National Cancer Institute, National Institutes of Health [Grant No. T32CA25107001]. These contents are solely the responsibility of the authors and do not necessarily represent the official views of the NIH.
Runtime of video: 5 mins 37 secs
Presentation: This study was presented at the 4th Symposium on Parathyroid Fluorescence, held in San Francisco, CA, from February 25 to 26, 2022.


Keywords
Get full access to this article
View all access options for this article.
