Abstract
Objective
Secondary hyperparathyroidism (sHPT) is one of the most serious complications in patients on long-term hemodialysis. These patients may suffer from metabolic bone diseases, severe atherosclerosis, and undesirable cardiovascular events. Endoscopic parathyroidectomy with autotransplantation is a treatment option for those who do not respond to clinical management. This study aimed to investigate practical use of a self-made device in parathyroid autotransplantation for patients with sHPT, and to compare this device with ordinary surgical scissors.
Methods
A total of 15 patients with sHPT were treated with endoscopic parathyroidectomy and autotransplantation. Pieces of parathyroid tissue were squeezed in our self-made device and injected into the brachioradialis muscle. Sixteen patients with sHPT who were treated with traditional parathyroid transplantation served as controls. Serum levels of parathyroid hormone, alkaline phosphatase, calcium, phosphorus and intact parathyroid hormone were measured before and after surgery.
Results
Preoperative symptoms were alleviated, and serum parathyroid hormone and alkaline phosphatase levels, hyperphosphatemia, and hypercalcemia were improved or normalized in all of the patients in both groups. Pathological examinations showed that parathyroid cells remained active.
Conclusion
Application of our squeezing device is an economic, effective, and safe method in endoscopic parathyroidectomy and autotransplantation for patients with sHPT.
Keywords
Introduction
Secondary hyperparathyroidism (sHPT) is a frequent complication of end-stage renal failure, involving metabolic bone diseases, severe atherosclerosis, and undesirable cardiovascular events. 1 Advances in medical treatment of sHPT have reduced the need for surgery, but 5% to 10% of patients still require parathyroidectomy. 2 Parathyroidectomy is required for approximately 10% to 30% of these patients with more than 10 years of hemodialysis. 3 The best surgical approach for sHPT is still debatable and controversy remains. Either subtotal parathyroidectomy or total parathyroidectomy can be performed with or without autotransplantation. 4 Autotransplantation of parathyroid grafts into the sternocleidomastoid muscle have been widely used, but Wells et al. 5 showed that the forearm muscle can be more advantageous. Subcutaneous injection or transplantation into the forearm is also effective in patients with chronic renal failure. 6 This study’s aim was to investigate the practical application of a self-made device in parathyroid autotransplantation for patients with sHPT, and to compare it with ordinary surgical scissors.
Patients and methods
A total of 15 patients in the experimental group and 16 patients in the control group had suffered from chronic renal failure for longer than 5 years. Patients in both groups had similar clinical status, and no significant differences in age, sex, ASA classification, or surgical procedure were found between the groups. Hemodialysis was performed two or three times a week in these patients. All of these patients had endoscopic parathyroidectomy and autotransplantation performed by the same team under general anesthesia. Total parathyroidectomy was performed in 25 patients and subtotal parathyroidectomy was performed in six patients (Table 1). This study was approved by the ethics committee of Shuguang Hospital, Shanghai University of Traditional Chinese Medicine. Written informed consent was obtained from each patient or their parent/carer.
The clinical information of all patients.

NOTE: IQR, interquartile range; ASA, American Society of Anesthesiologists; PTX, parathyroidectomy.
After the patient was placed in the supine position, a pillow was placed beneath the shoulder to extend the head and neck. A 10-mm incision was made in the intersection point of the median thoracic line and bilateral nipples. A metal rod with a blunt, round end was used to create a straight line tunnel towards the sternal notch. Two 5-mm incisions were made in the intersection point of the bilateral midclavicular line and the second rib. Additionally, two 5-mm metal rods were used to create straight line tunnels (Figure 1a).
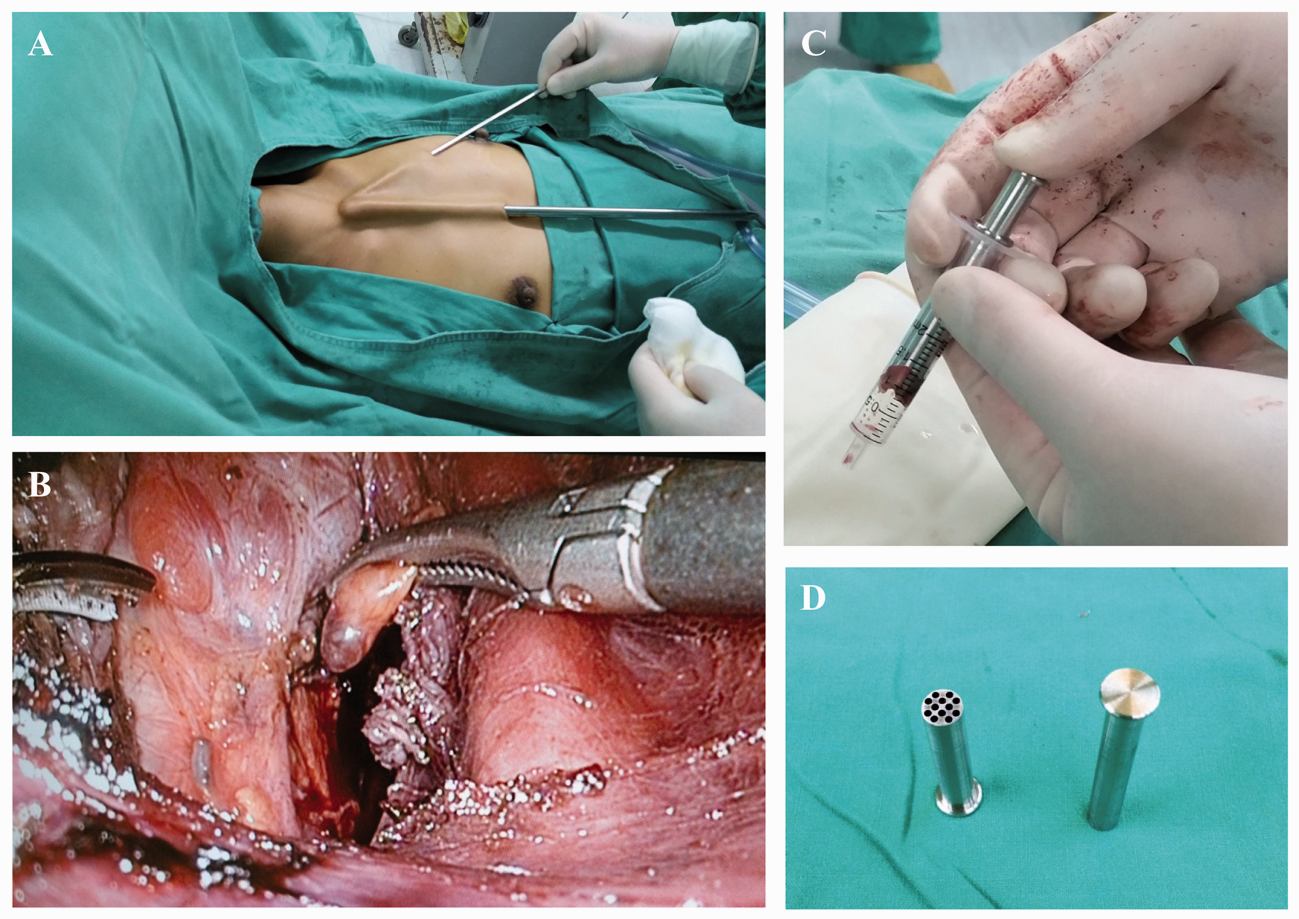
(a) Creating straight line tunnels. (b) Dissecting the parathyroid gland. (c) The metal squeezing device and (d) Squeezing parathyroid fragments
After the blunt dissection, three trocars were inserted through each tunnel. Carbon dioxide gas was injected with a pressure of 8 mmHg. A 30-degree 10-mm endoscope was inserted through the middle 10-mm trocar, and an ultrasonic scalpel and a grasping forceps were inserted through the two 5-mm trocars. A subplatysmal space was dissected to create a working space from the suprasternal fossa to the thyroid cartilage level and laterally to the medial edge of the sternocleidomastoid muscles.
A longitudinal incision of the cervical linea alba was made and the bilateral infrahyoid muscle groups were transected to expose the thyroid gland. The posterior surface of the thyroid was examined to identify the parathyroid glands according to the surgical anatomy (Figure 1b).
The removed parathyroid glands were carefully examined to select a non-nodular area that was rich in stromal fat cells for immediate graft implantation. The selected parathyroid fragment was gently diced into small pieces that measured approximately 2.0 mm³. The device for dicing the parathyroid was a metal sleeve, which could easily be put into a syringe. The metal sleeve was composed of two parts; the outer part was a hollow tube with multiple holes and the inner part was a solid core (Figure 1c). This squeezing device has a Chinese utility model patent (ZL 2016 20280921.2).
Parathyroid fragments were roughly diced and put into the metal sleeve, and squeezed in a syringe. After squeezing, the parathyroid tissue was mixed with normal saline and injected into the brachioradialis muscle in the forearm without formation of an arteriovenous fistula for hemodialysis (Figure 1d).
Levels of parathyroid hormone (PTH) and alkaline phosphatase (ALP) in serum were determined using an immunology analyzer (cobas E602; Roche, Basel, Switzerland). Serum calcium, phosphorus, and ALP levels were measured using an automatic biochemical analyzer (Olympus AU5400; Olympus Corporation, Tokyo, Japan). Detailed methods can be found in the protocols of the manufacturers of these analyzers.
Statistical analysis
All data are expressed as mean ± standard deviation. The independent-sample t-test was used to analyze the differences between the experimental and control groups. Multivariate analysis of variance was performed to analyze differences before and after the surgery. A value of p < 0.05 was considered statistically significant. Data were analyzed using SPSS Statistics software (version 22.0; IBM Corporation, Armonk, NY, USA).
Results
Clinical information of the patients is shown in Table 1. All of the patients had endoscopic parathyroidectomy successfully performed without any complications. No laryngeal nerves (e.g., recurrent laryngeal nerve) were apparently injured during the operation (Figure 2), although vocal hoarseness was observed after the operation. These symptoms were relieved after conservative treatment.

Photograph showing an uninjured laryngeal nerve in endoscopic surgery. RLN: recurrent laryngeal nerve
Thirty days after parathyroidectomy, the patients’ clinical symptoms had improved and serum PTH levels were significantly decreased compared with before parathyroidectomy (p < 0.001, Figure 3a). Serum PTH levels in the forearm that was injected with parathyroid cells showed a similar tendency to be increased compared with PTH levels in the uninjected forearm after surgery (Figure 3b). During 30 days after injection with parathyroid cells, serum calcium levels did not decline within or below the normal range in all of the patients (Figure 3c). In the experimental group, serum phosphorus levels appeared to decline after surgery, but this was not significantly different from the control group (Figure 3d). ALP levels did not significantly change after surgery and were similar between the experimental and control groups (Figure 3e). Pruritus and bone pain was relieved or disappeared within 6 months. Recurrence of graft-dependent hyperparathyroidism was not observed in any of the patients during a 6-month follow-up. Although the results of these biochemical indices were not as we expected, non-significant differences between the experimental and control groups indicated that using our self-made device in parathyroidectomy was as effective as traditional methods.

Serum PTH, Ca, P, and ALP levels before and after surgery. ***p < 0.001, compared with 1 day before the operation. PTH: parathyroid hormone; Ca: calcium; P: phosphorus; ALP: alkaline phosphatase
We were able to save a considerable amount of time by using this practical device compared with implantation in forearm muscles. A pathological examination showed that at least 80% of the parathyroid cells remain active (Figure 4).

Parathyroid cells after squeezing. Hematoxylin and eosin stain, × 100
Discussion
Despite improvements in medical management, severe sHPT remains a common complication of chronic renal failure. A longer survival of patients with chronic renal disease has increased the incidence of symptomatic hyperparathyroidism. 7 The prevalence of parathyroidectomy in end-stage renal disease ranges from 9.2% after 10 to 15 years of dialysis to 20.8% after 16 to 20 years of dialysis.8,9 In patients who are eligible for surgery, parathyroidectomy is generally considered when hyperparathyroidism is severe and refractory to medical management. Hyperparathyroidism usually occurs after a therapeutic trial of calcitriol and a vitamin D analog. Hyperparathyroidism can also occur when medical management to reduce intact PTH levels results in an unacceptable rise in serum calcium and/or phosphorus levels, or when medical management is not tolerated because of adverse effects. 10
The best surgical approach for sHPT remains controversial. Wells et al. 11 reported their experience in total parathyroidectomy with parathyroid autotransplantation in forearm musculature in 1975. Total parathyroidectomy with a forearm autograft has been considered the standard procedure since this time. However, this technique has some restrictions. In 1979, Wells reported three (7.5%) patients with graft-dependent hyperparathyroidism, of whom one presented with persistent hyperparathyroidism, even after the parathyroid graft was excised. 12 To avoid these undesirable recurrences, other researchers have found alternative areas for transplantation of parathyroid tissue as follows: Jansson and Tisell used subcutaneous abdominal adipose tissue, 13 Kinnaert et al. used the presternal subcutaneous region, 14 Monchik et al. used subcutaneous forearm tissue, 15 and Lieu et al. used sternocleidomastoid muscle. 16 In our study, we used fresh parathyroid tissue that was buffered in 2 mL balanced saline in the form of a suspension for intramuscular injection. 17 Use of pre-transplantation frozen sections is sometimes performed if there is doubt regarding whether the tissue is actually the parathyroid, or to determine whether the tissue is active. However, this technique is not routinely recommended because of maintaining maximum parathyroid tissue and avoiding loss of time and cost.
Hyperparathyroidism recurrence and graft-dependent recurrence cannot be neglected after parathyroid autotransplantation. Endoscopic bilateral exploration was performed in all of the patients in our study to identify the parathyroid glands. We did not miss any parathyroid glands with improved visualization and amplification of the endoscope. Santos reported a graft-dependent recurrence rate of 9.09% in 66 patients, and all recurrences occurred in patients under dialysis treatment, with no recurrence observed among kidney-grafted patients throughout an extensive follow-up. 7 In our study, there was no recurrence of hyperplastic parathyroid tissue in the forearm muscles, possibly due to the short follow-up period. However, using B-ultrasonic localization, we can easily excise hyperplastic parathyroid tissue under local anesthesia or inject anhydrous alcohol.
Transplanted parathyroid tissue spontaneously revascularizes and becomes innervated. This transplanted tissue usually begins functioning in 2 to 4 weeks and regains full function in 2 months. 18 Autograft function may also be indirectly assessed by measuring serum PTH levels from the antecubital veins of grafted and nongrafted arms, with a PTH ratio of 1.5 or greater indicating functional parathyroid tissue. 19 According to this criterion, all of the patients in our study had satisfactory results.
Several limitations were inevitable because our study was intended as a pilot study. First, the number of samples was small. A lack of decrease in serum calcium levels in the experimental and control groups might have been due to a lack of statistical power. Therefore, more statistical data are required to confirm the function of transplanted parathyroid tissue. Second, our follow-up period of only 6 months may not have been long enough to show all complications after surgery. We also need more experience in dealing with complications, as well as prognosis. Third, there are no other studies with the same surgical approach to compare surgical results with.
In conclusion, application of the practical squeezing device is an economic, effective, and safe method in endoscopic parathyroidectomy and autotransplantation for patients with secondary hyperparathyroidism. This device enables ideal outcomes, while saving a considerable amount of time.
Footnotes
Declaration of conflicting interest
The authors declare that there is no conflict of interest.
Funding
This study was supported by the Shanghai Health and Family Planning Commission Research Fund (Grant No.: 201540308).
