Abstract
In a prospective controlled study, 172 polyurethane feet of different designs were fitted to 155 amputees with trans-tibial prostheses. These were followed in respect of their durability. The amputee compliance was in general good, and 87% were satisfied with their device. After 18 months the failure rate of 20% with the CIREC spring-blade foot was significantly better than the others, but poorer craftsmanship, higher complaint rate and lower compliance rate cast some doubt on the results. The results with the conventional SACH foot constructions with polyurethane as filling and covering materials were so poor after 18 months that their use cannot be recommended in tropical areas of the developing world.
Introduction
The Solid-Ankle-Cushion Heel (SACH) foot construction has been the basis for prosthetic feet in the Western world for more than half a century. It is not surprising that the non-governmental organizations preferred that model for local production, since it was fairly simple to manufacture from locally available or easily accessible materials. However, as is the problem with most prosthetic technology, scientific follow-up information does not exist either on SACH foot performance or on other designs evolved by the NGOs. A prospective controlled study was considered necessary to provide a rational basis for comparison and further development.
Materials and methods
Fifty trans-tibial amputees at University Don Bosco, San Salvador, El Salvador (UDB) were provided with a Kingsley Strider-08 foot (Kingsley Manufacturing Company, Costa Mesa, California, USA) and a laminated resin-wood shank attached by a bolt. The terminal device was a SACH foot consisting of a wooden keel with a textile belt drive forefoot reinforcement encapsulated by moulded polyurethane (PU) foam (Figure 1).

Kingsley Strider-08 Foot. Wooden keel, textile mid-foot blade encapsulated in polyurethane foam.
In three series of trans-tibial amputees the prosthesis provided was the modular polypropylene system (PP) developed and marketed by the International Committee of the Red Cross (ICRC), consisting of a drape wrapped polypropylene socket, two alignment discs and a tubular shank part.
In 32 cases at UDB the terminal device was a spring-blade foot developed by CIREC, Bogota, Colombia. It consists of a wedge formed solid PP keel moulded around two PP spring-blades. The core is placed in a metal mould, which is filled with PU foam that is cured to form the heel cushion and encapsulate the entire foot (Figure 2).

CIREC Foot. Polyethylene keel and polyethylene spring-blades encapsulated in polyurethane foam.
In 35 cases the Fujian foot from Endolite-Asia, Hanoi, Vietnam, was tested at VIETCOT, Hanoi, Vietnam. The internal construction of the foot is a tooth shaped wooden keel and textile belt forefoot reinforcement encapsulated by PU foam. A total of 55 SACH feet on 38 amputees from CR Instruments S.A., Geneva, Switzerland were tested at CSPO, Cambodia. The dog tailed, fenestrated PP keel was encapsulated in PU foam (Figure 3).

CR-SACH Foot. Fenestrated, dog-tailed keel of polypropylene surrounded by polyurethane foam.
The studies were conducted at the ISPO/WHO recognized Category-II schools for prosthetics and orthotics in El Salvador, Vietnam and Cambodia. The surveys were undertaken by teams of a Category-I prosthetist and an orthopaedic surgeon experienced with prosthetic performance studies. The amputees were recruited from cohorts of well-known users of prostheses, who all had availability of at least one more prosthesis at home. Consequently they did not seek repair of a failed prosthesis but awaited the call for follow-up. The plan was to see the amputees at 9 and 18 months after prosthesis provision, but an earth-quake in El Salvador and a different protocol for testing of sand-casting in Vietnam made it impossible to keep the proposed follow-up schedule. That eliminated the application of rigorous Kaplan-Meier survival statistics. Instead it was necessary to combine such analyses with crude comparisons at 12 and 18 months applying Student's t-test (unpaired, two-tailed, two sample, unequal variance). The follow-up rate was 77% (119/155), varying from 65% (53/82) in El Salvador, over 80% (28/35) in Vietnam, to 100% (38/38) in Cambodia. The study was completed either at failure or at the latest follow-up. Clinical field testing was conducted in accordance with the system developed by the International Society for Prosthetics and Orthotics (ISPO) (Jensen and Heim 1999; Jensen and Raab 2002).
Demographics and patient characteristics
The median follow-up was 11 (1 – 37) months (Tables I – II III), and there was no difference in follow-up between those who failed and those not failing (p = 0.09) in the overall group. The amputees had a median age of 24 (13 – 72) years at the time of amputation and 41 (20 – 73) years at the time of follow-up. Some 73% (87/119) lived in urban or dry rural areas; however, about half (20/38) of the Cambodians lived in sea-water areas. The majority was now employed in unskilled work, but 44% (52/119) were soldiers at the time of amputation, and in 59% (70/119) war ordnance was the cause of amputation.
Demographics, trans-tibial amputees with polypropylene prostheses.
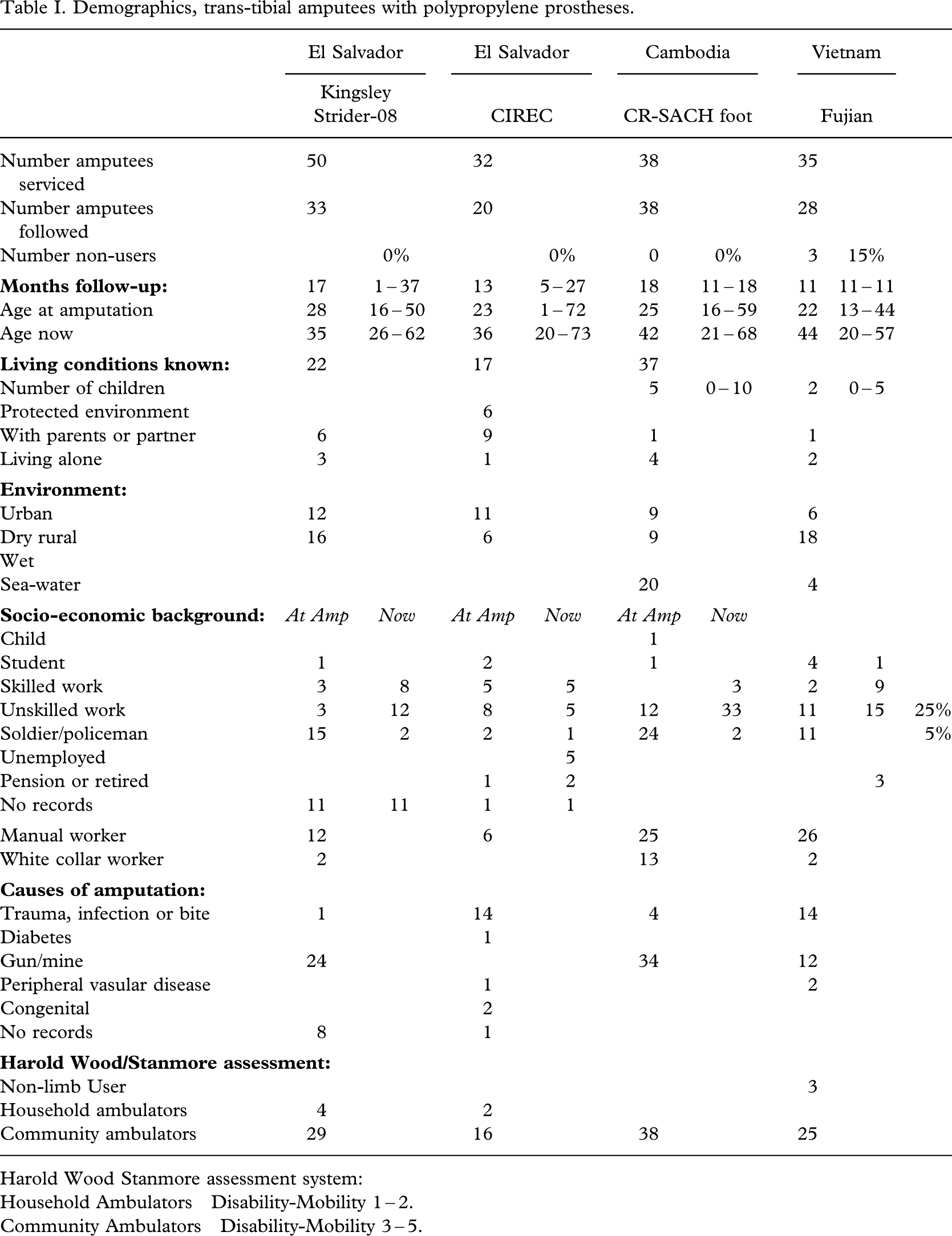
Harold Wood Stanmore assessment system:
Household Ambulators Disability-Mobility 1 – 2.
Community Ambulators Disability-Mobility 3 – 5.
Patient characteristics, trans-tibial amputees with polypropylene prostheses.
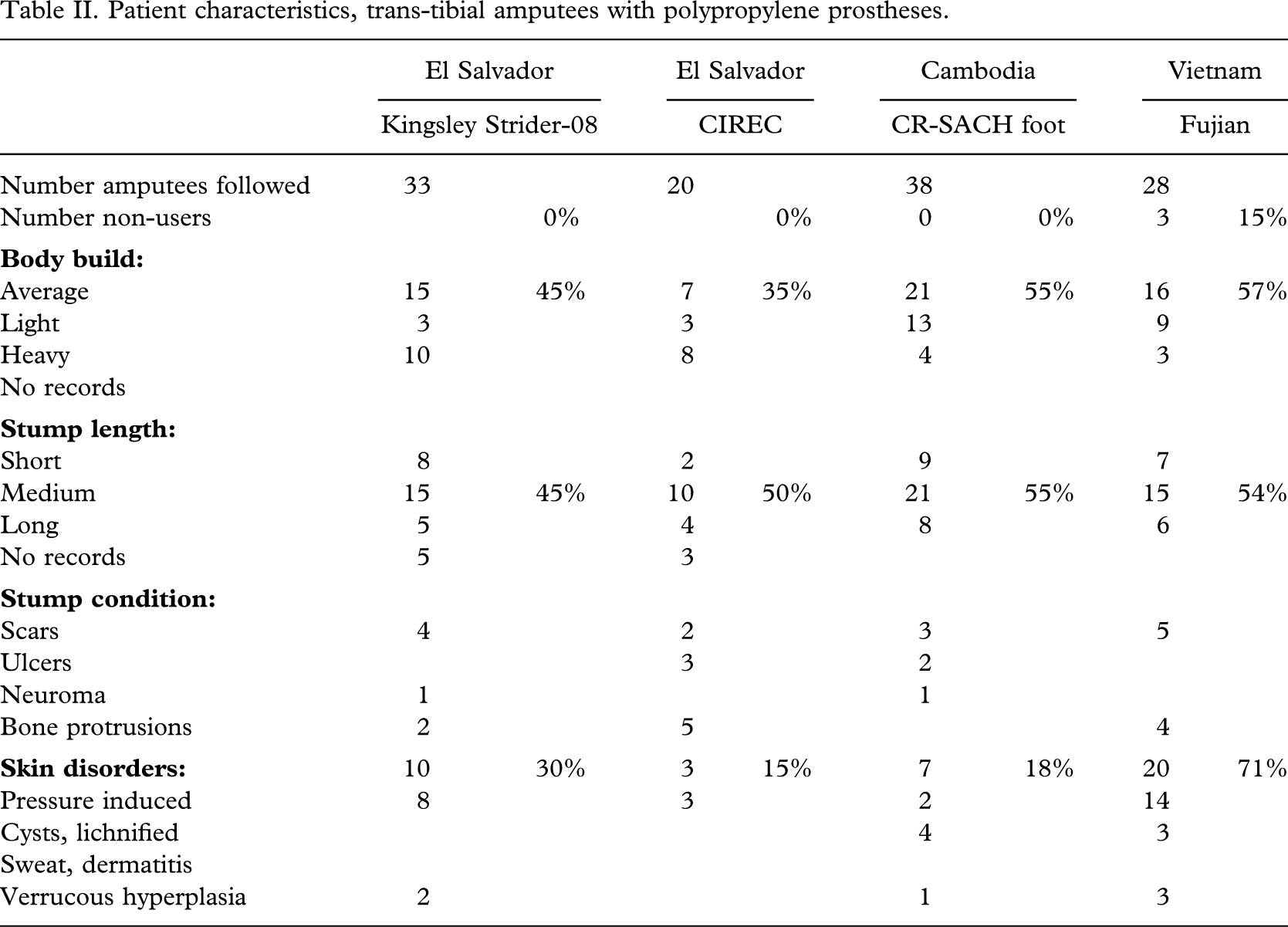
Demographics and patient characteristics, present and historical series.
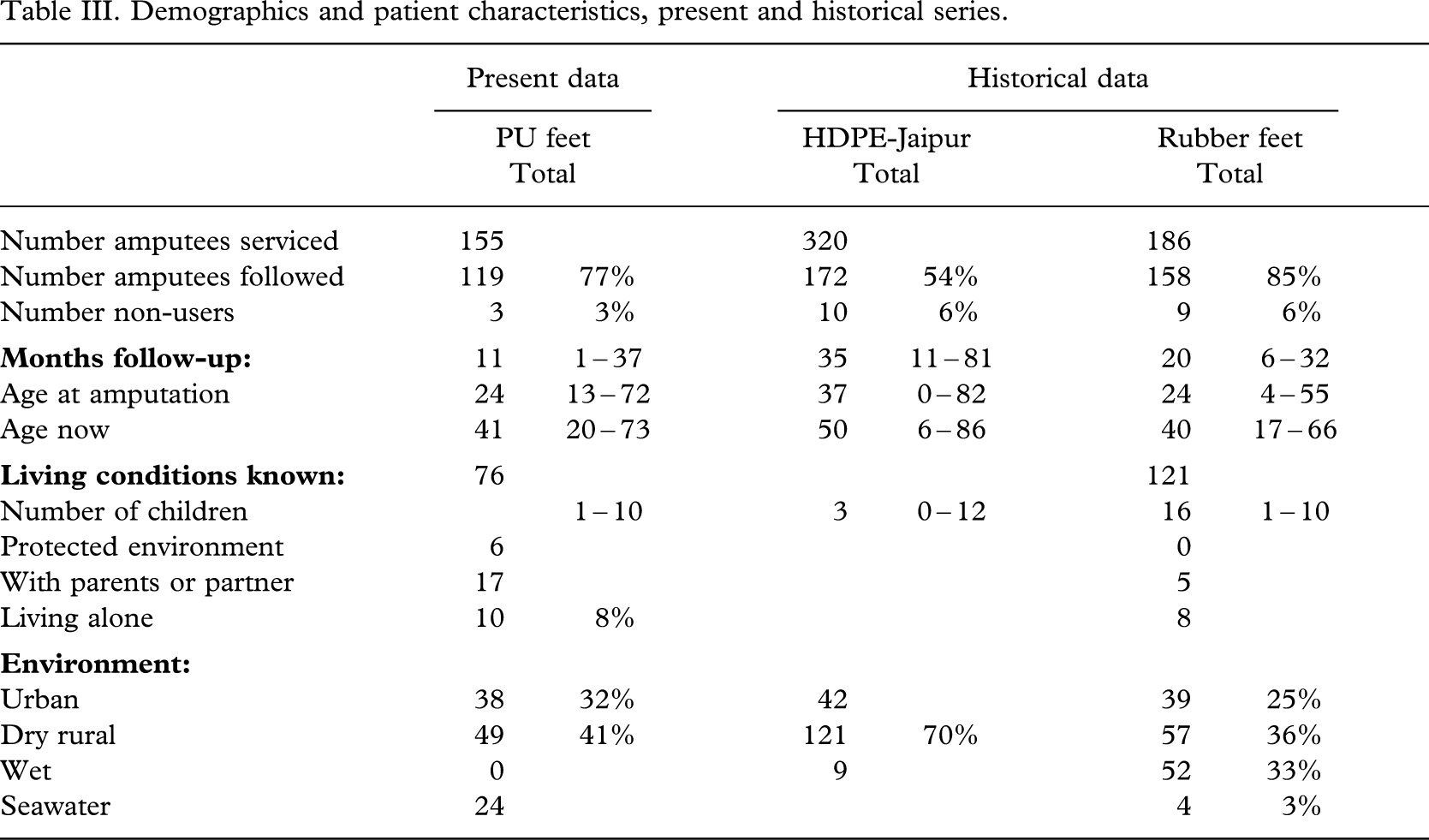
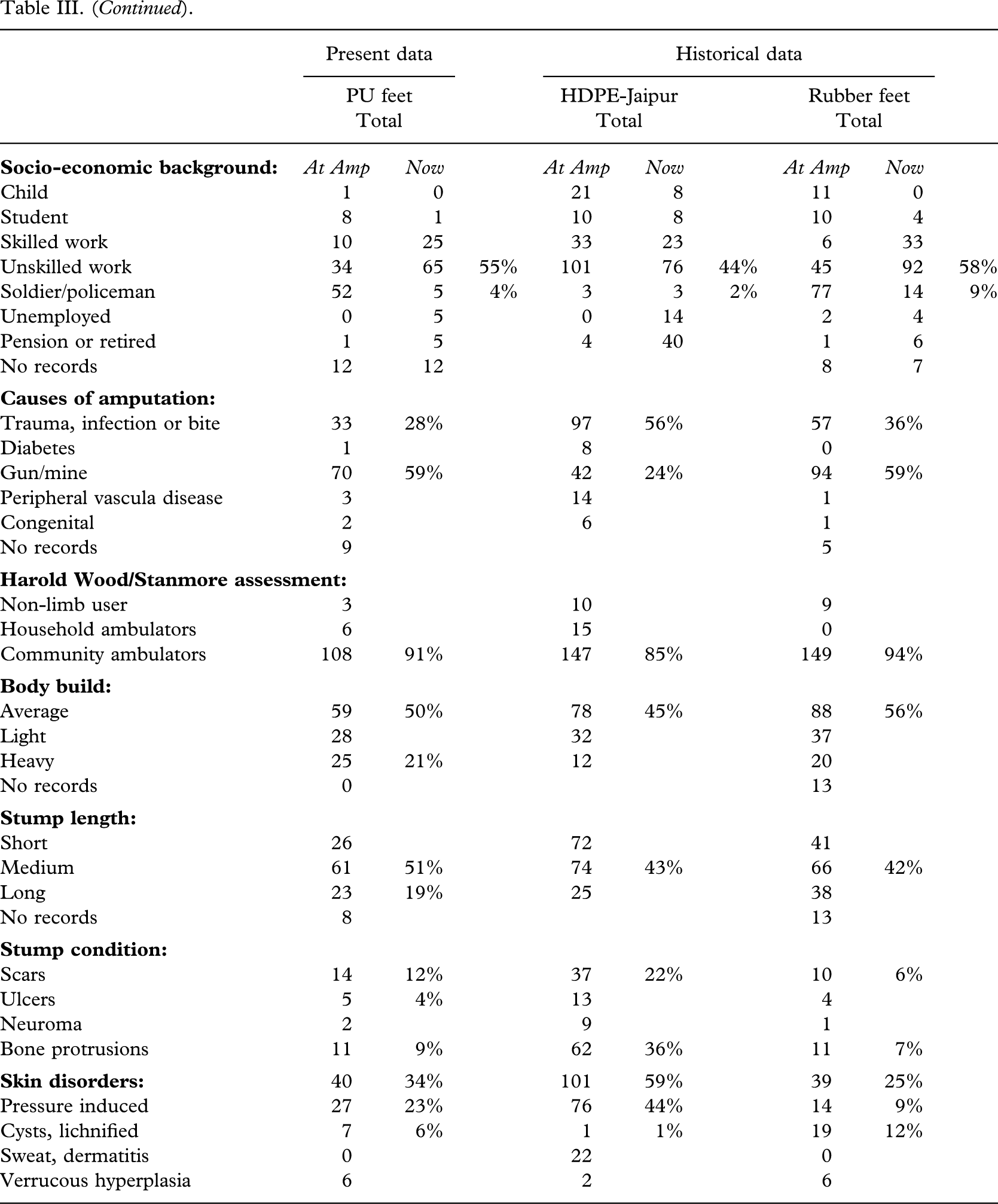
Three amputees did not use the prosthesis under investigation, but 94% (112/115) were community ambulators.
The stumps were straight forward for fitting; 70% (84/119) being of medium length or long; only 4% (5/119) having ulcers, and 9% (11/119) bone protrusions. Scars were encountered in 12% (14/119) and 29% (34/119) had pressure induced skin disorders, lichnified skin or cysts. There were no major deviations between the present and historical series (Table III).
Patient compliance and craftsmanship
The amputees were wearing their prosthesis for 14 (2 – 18) hours daily (Table IV), and 79% (94/119) walked more than 1 km. Only 9 amputees walked bare-footed. Intensive use of the prosthesis was recorded in 78% (93/119). Nearly one third of amputees complained about discomfort or pain, but 87% (103/119) were satisfied with the device.
Patient compliance and prosthetic fitting.
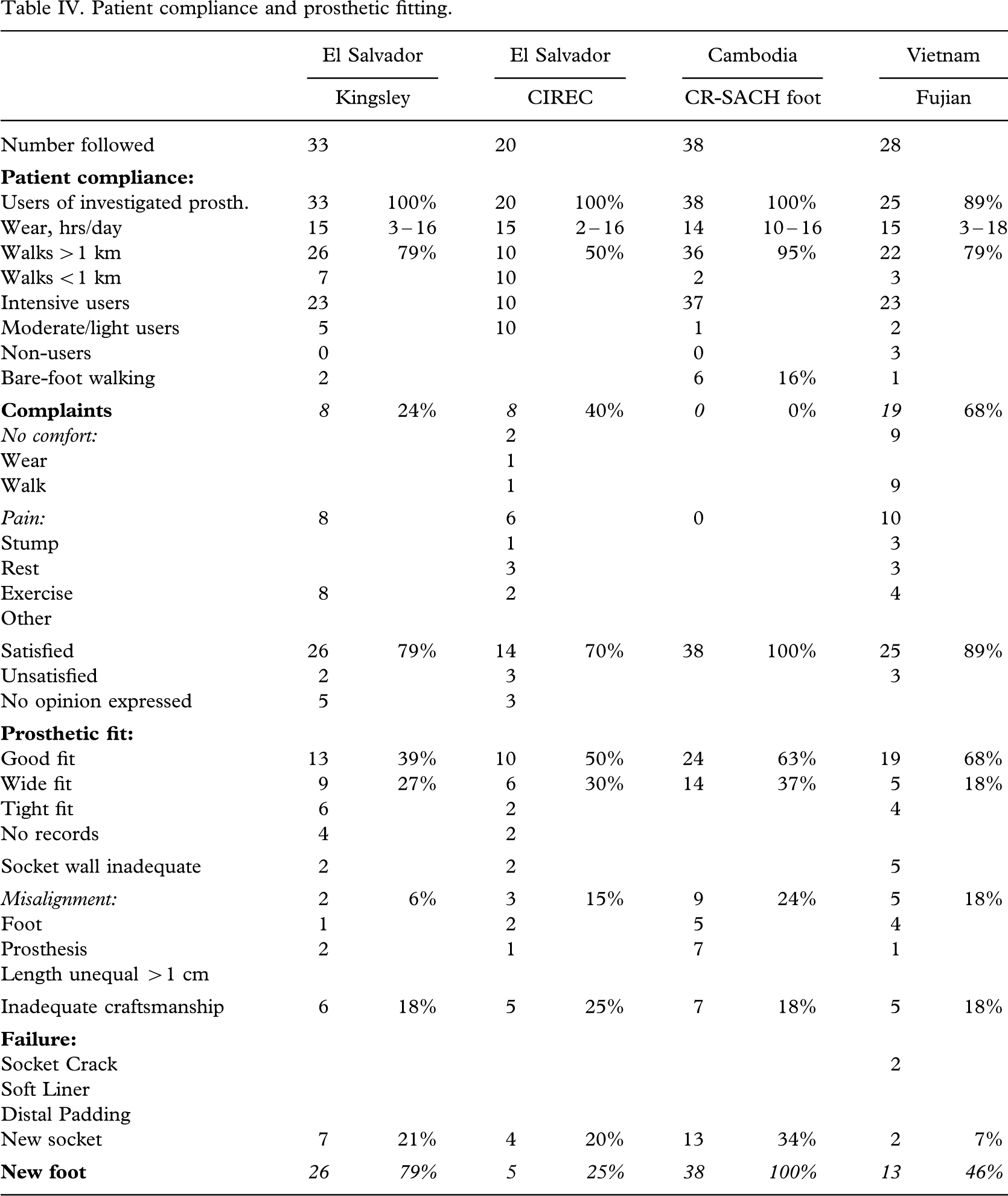
A tight socket fit was found in 10% (12/119), inadequate socket wall in 8% (9/119) and misalignment in 16% (19/119). In 19% (23/119) the craftsmanship was found to be inadequate.
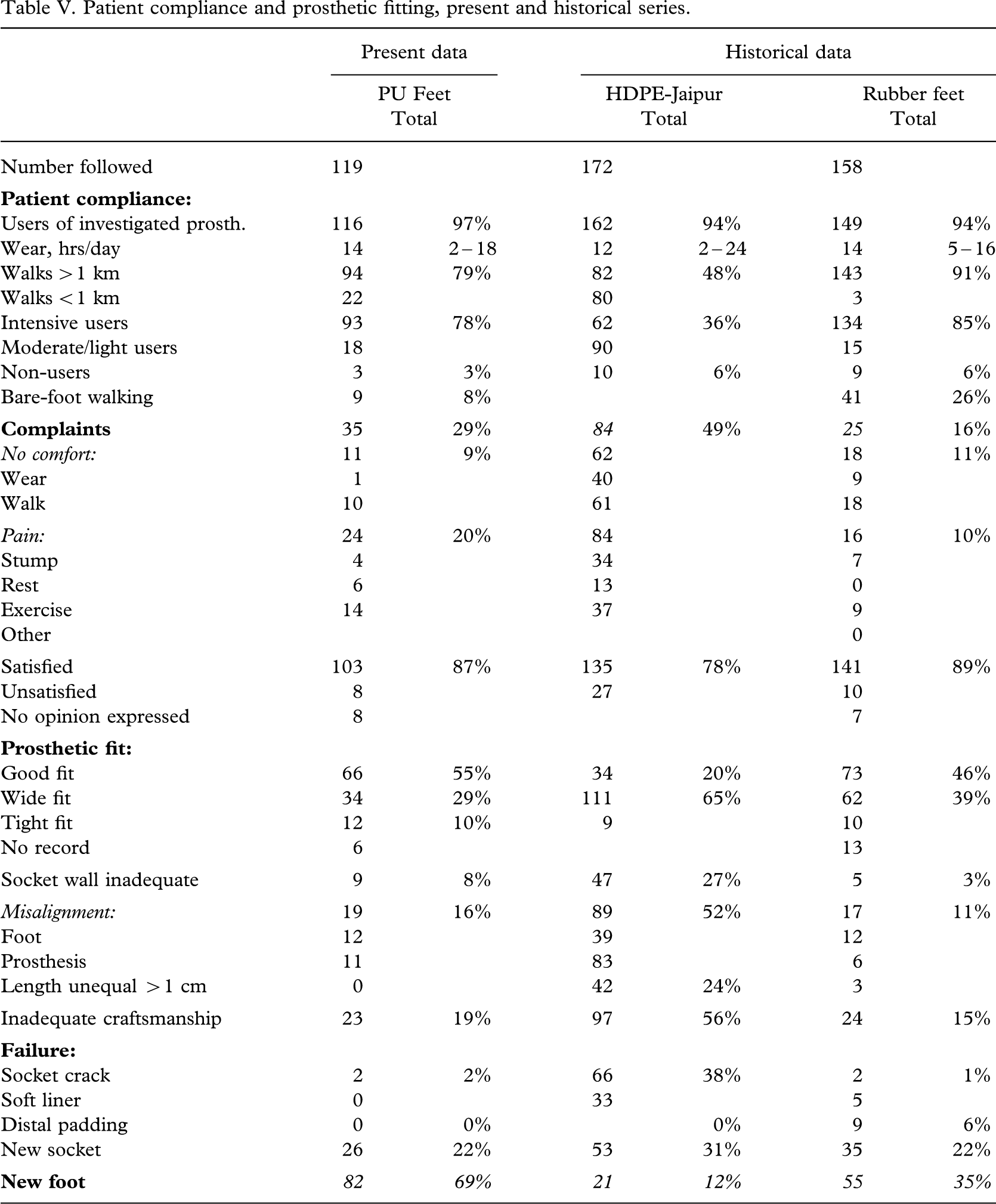
In comparison with five series of amputees supplied with rubber feet at the same institutions (Jensen et al. 2006) there were no differences of significance regarding patient compliance and craftsmanship (Table V). In comparison with high density polyethylene (HDPE) Jaipur prostheses (Jensen et al. 2004) the present results were better both with regard to patient compliance and not least in respect of adequate craftsmanship (p < 0.0007).
Patient compliance and prosthetic fitting, present and historical series.
Failures of the prosthetic foot
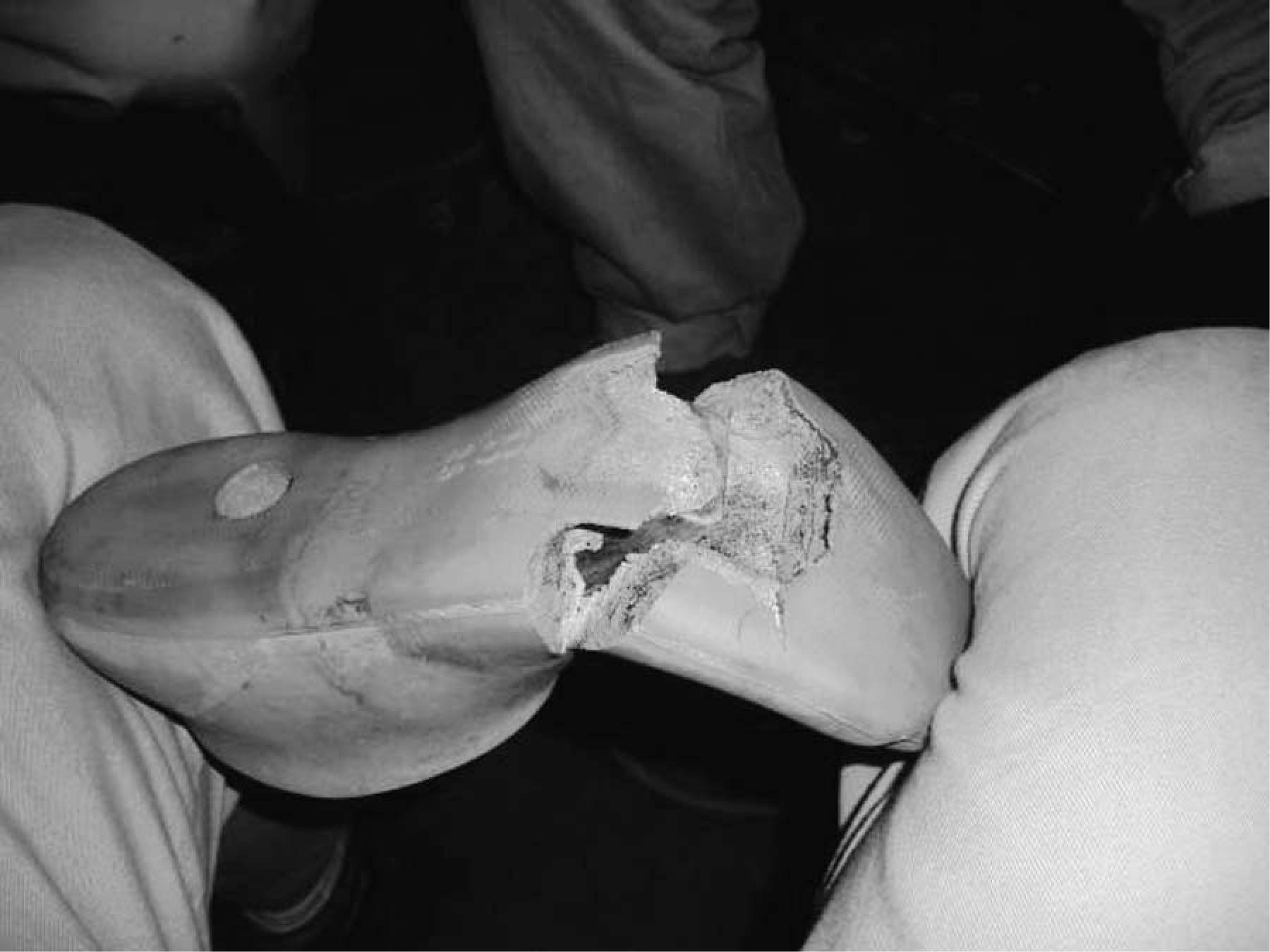
Failure of the foot cover (Table VI) was a particular feature with the CR-SACH foot in Cambodia (Figure 4).
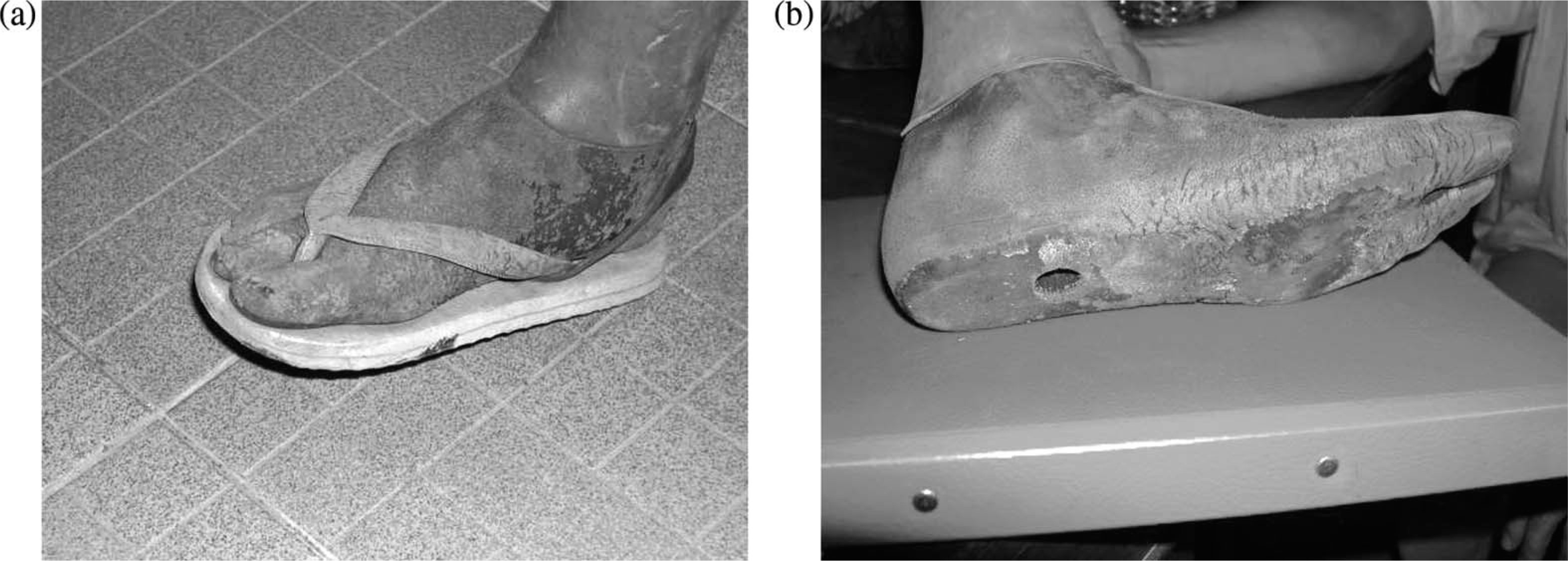
CR-SACH Foot. Severe deterioration of (a) foot cover and (b) sole.
Failure of prosthetic foot.
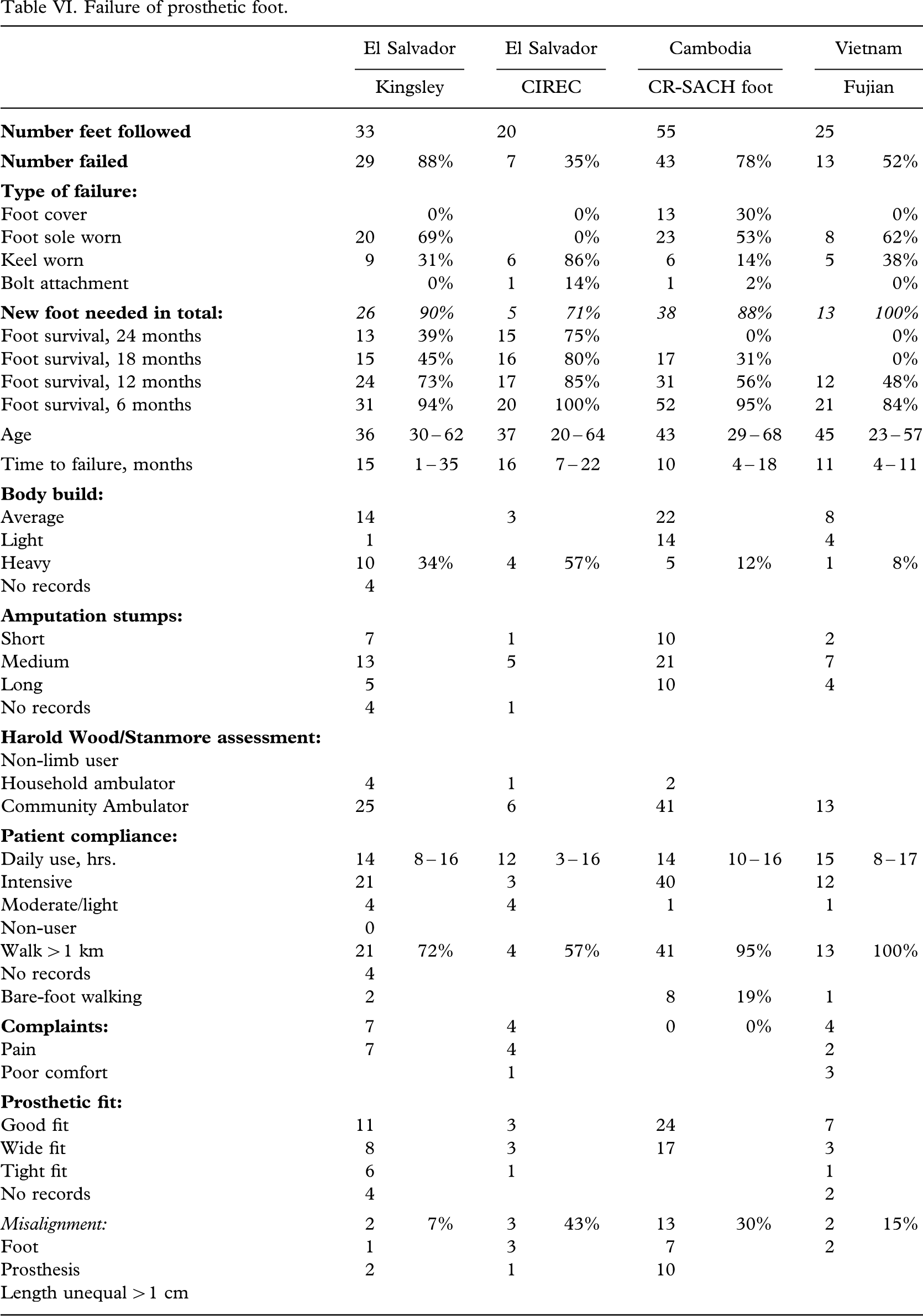
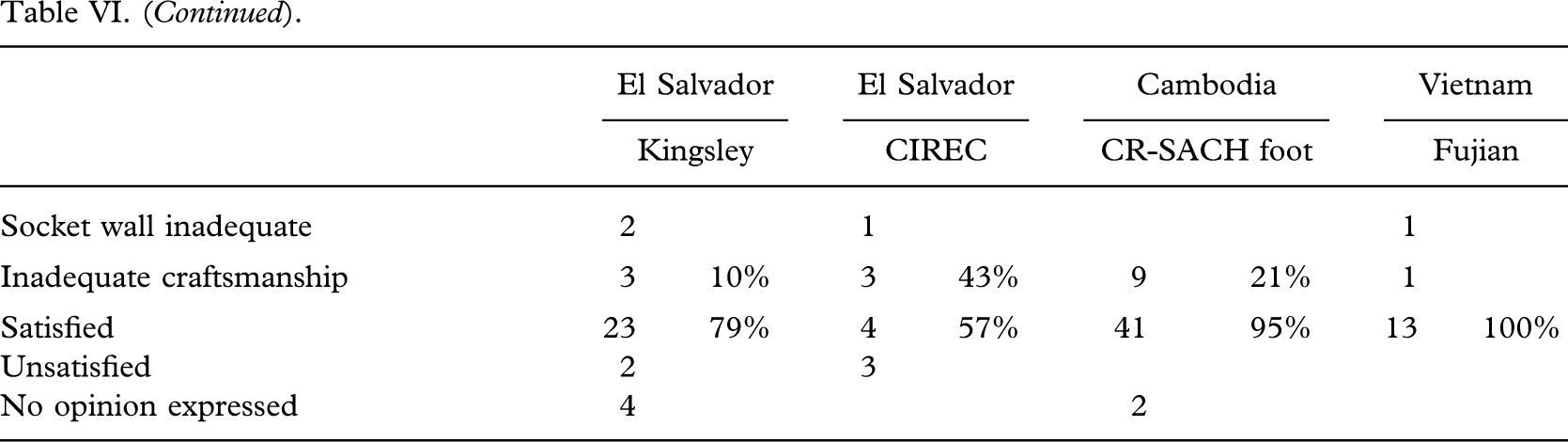
Fracture of the forefoot (Figure 5), worn foot sole with penetration of the keel (Figure 6), or wear of the keel (Figure 7) were the most frequent failures, which occurred in 65% (87/133) of feet provided and led to exchange of the foot in 89% (82/92) of cases.
Kingsley Strider-08 Foot. Fracture of fore-foot.
CR-SACH Foot. Deterioration of polyurethane foam and penetration of keel.
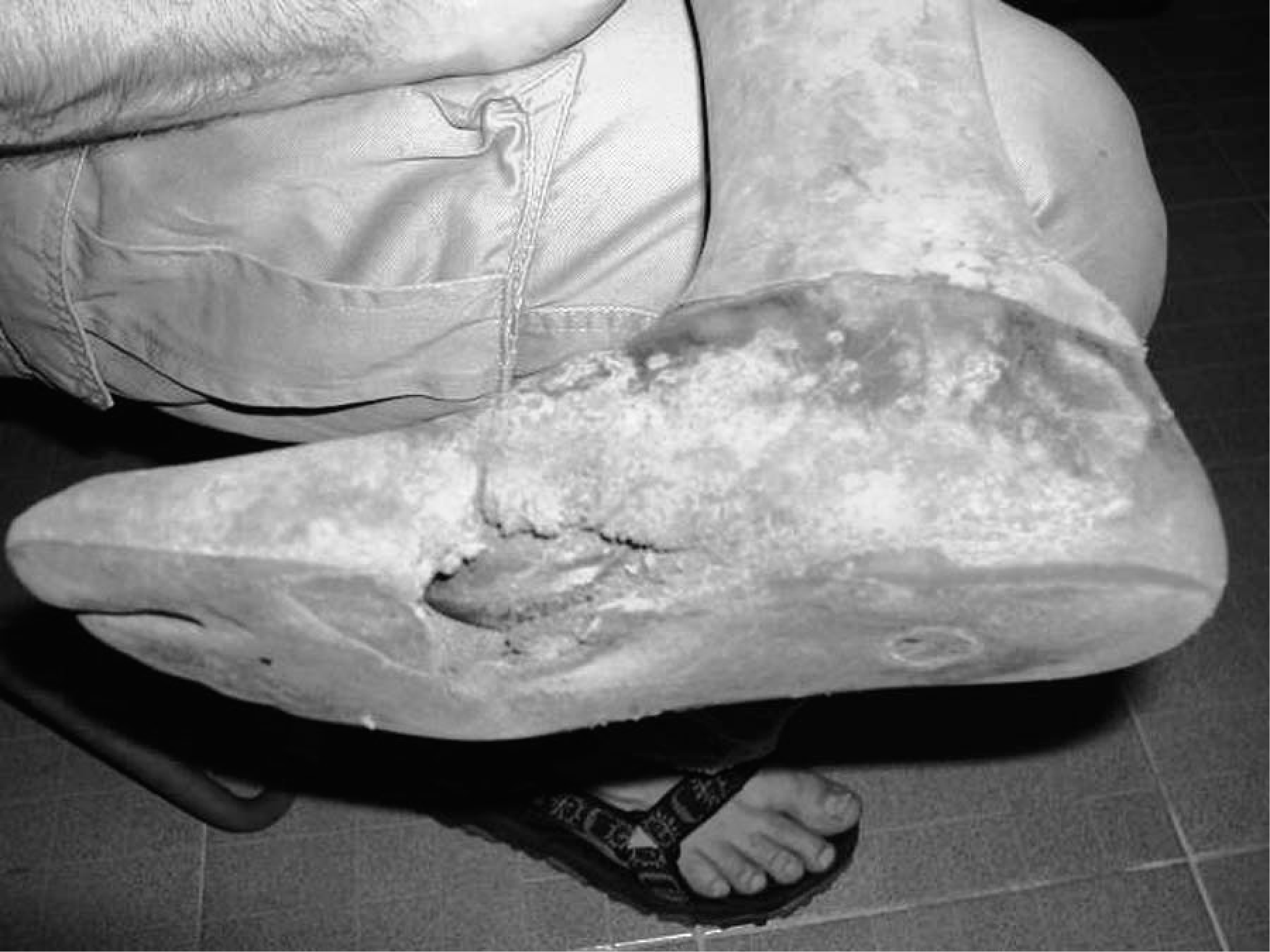
Fujian Foot. Rot of keel and deterioration of polyurethane foam.
The need for replacement of the foot at 12 months was 15% (3/20) for the CIREC foot, which was not significantly different from the 27% (9/33) for the Kingsley foot (p = 0.28), but significantly better than the 44% (24/55) for the CR-SACH foot (p < 0.0006), and the 52% (13/25) for the Fujian foot (p < 0.007). The Kingsley foot performed better than the Fujian foot (p < 0.06).
At 18 months, the need for replacement of the CIREC foot was 20% (4/20), which is better than the CR-SACH foot (p < 0.009) with 55% (18/33). The Kingsley foot needed replacement in 61% (20/33) of cases.
The influence of different factors on failure of the prosthetic foot was analysed. The amputees with Kingsley feet were younger than those with CR-SACH feet (p < 0.008) and Fujian feet (p < 0.00002). The amputees in Vietnam with Fujian feet were older than the other groups (p < 0.0003), but they were wearing the prosthesis longer during the day than the others (p < 0.04). There was no significant influence of body mass or walking more than 1 km. All 9 amputees walking bare-footed damaged the 11 feet provided. Analysis of Kaplan-Meier survival data showed that the CIREC foot performed better than the CRSACH (p < 0.01) and Fujian foot (p < 0.007) after 12 months.
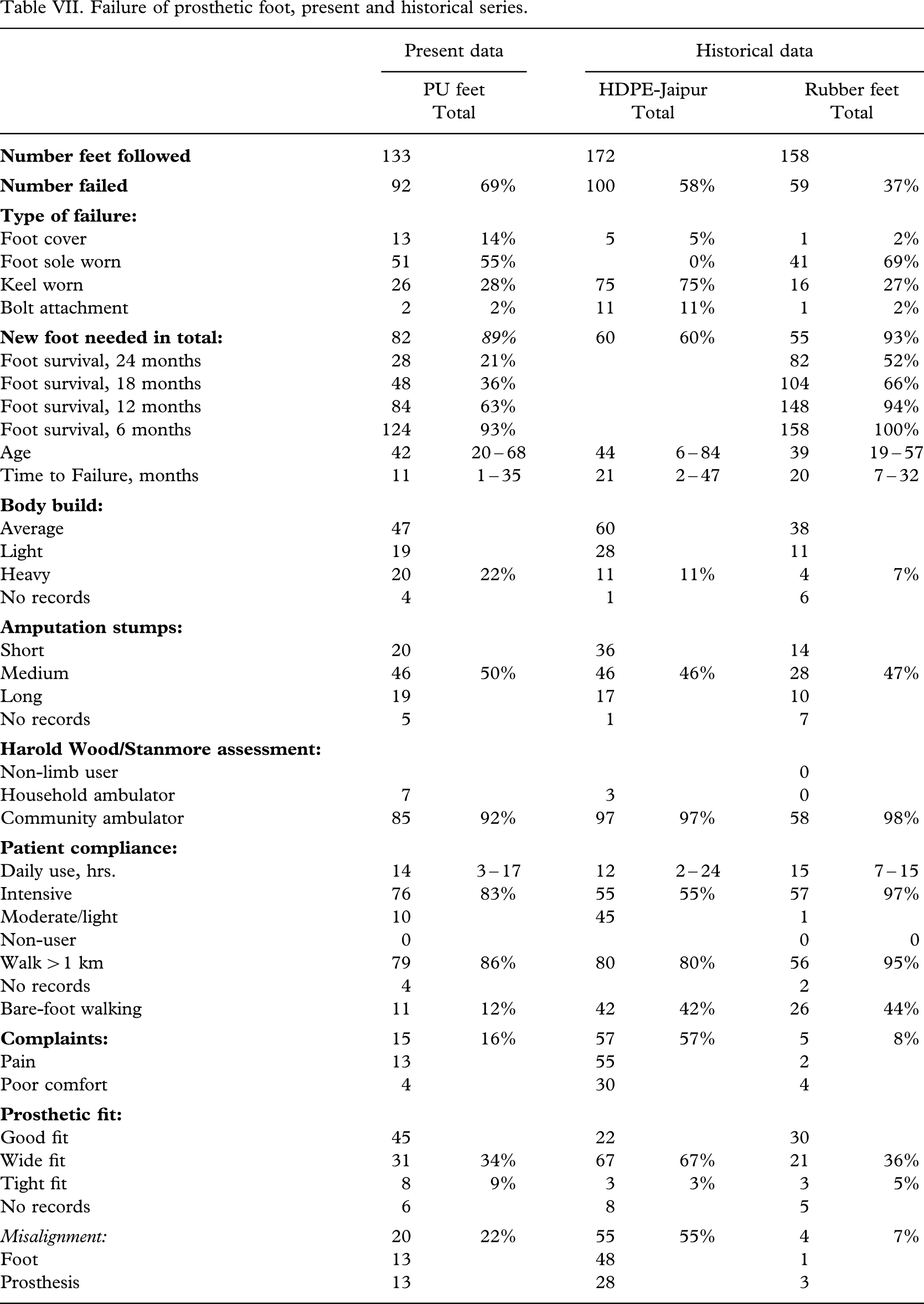
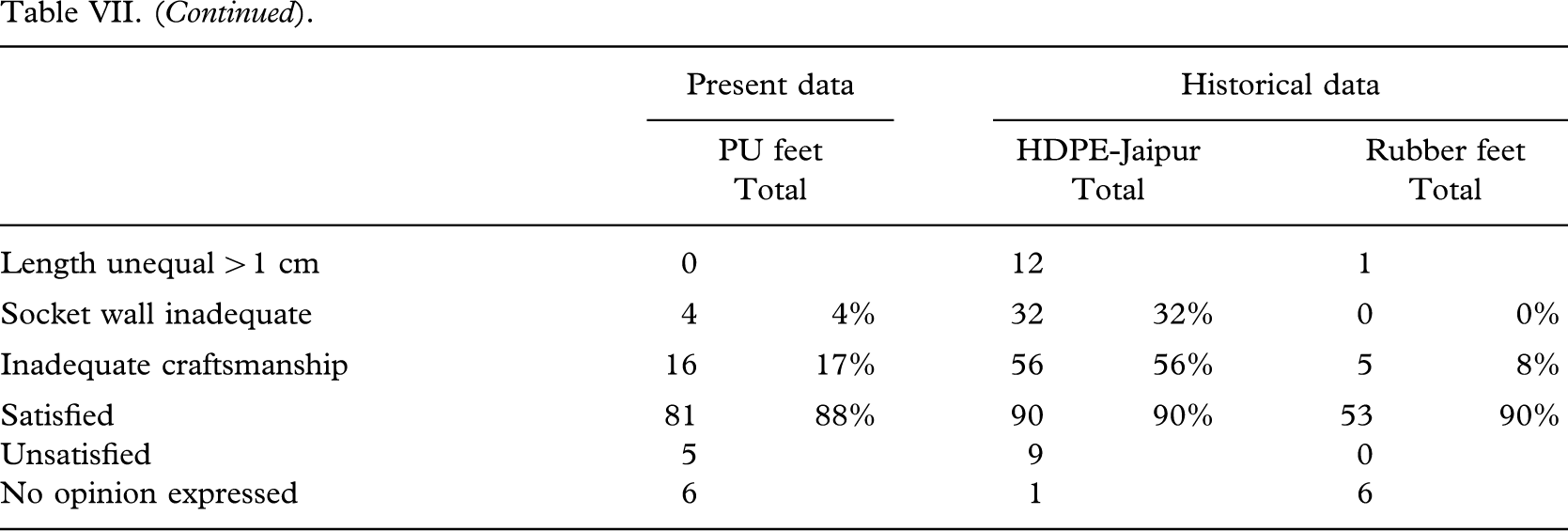
The results were compared (Table VII) with a previous clinical field testing series of vulcanized rubber feet (Jensen et al. 2006) and it was found that the CIREC foot matched the results with the tested rubber feet (p = 0.08 – 0.65) and that the Kingsley foot was at level with the HI-foot from Handicap International, Phnom Penh, Cambodia (p = 0.50), but inferior to the EB-1 foot from Prosthetic Outreach Foundation, Hanoi, Vietnam (p < 0.002), the PP-Rubber foot from the International Committee of the Red Cross, Phnom Penh, Cambodia (p < 0.03), and both rubber feet from VVAF, Kien Khleang, Cambodia (p < 0.006). The survival rate for the CR-SACH foot was significantly lower than any rubber foot tested (p < 0.02).
Failure of prosthetic foot, present and historical series.
Discussion
The best performing foot in this study was the CIREC foot from Bogota, Colombia. It was constructed with an attempt to provide energy storing and return during propulsion. Whether this was an advantage could not be disclosed by this study. All claimed to be intensive users, but the complaint rate was high, craftsmanship and user compliance low, and the drop-out from follow-up the highest. This means, that it is difficult to have confidence in the results.
The other feet were conventional SACH foot constructions with wooden or plastic keels and polyurethane foam as filling material around this and skin. All these feet had a very high failure rate, mostly because the polyurethane wore out in particular if walking was bare-footed. Further to that was added the problem of rapid deterioration of the skin of the CR-SACH foot when exposed to strong sunshine at the seaside in Cambodia, when walking bare-footed. It is difficult to understand the incentive for ICRC in centralizing production and distribution to workshops in areas where the locally manufactured foot performs better.
In conclusion, polyurethane based prosthetic feet cannot be recommended for tropical areas of the developing world.
Footnotes
Acknowledgements
The following feet were supplied at no cost by the manufacturers, Kingsley Strider-08 (Kingsley Manufacturing Company, Costa Mesa, USA); CIREC (CIREC, Bogota, Colombia); CR-SACH (CR Instruments, Geneva, Switzerland) The study was supported by the Leahy War Victims Fund, United States Agency for International Development (grant no. HRN-G-00-00-00015-00). The opinions expressed in this paper are those of the authors and ISPO, and do not necessarily reflect the views of USAID.
