Abstract
The present study examined the hypothesis that spinal cord ischemic tolerance induced by hyperbaric oxygen (HBO) preconditioning is triggered by an initial oxidative stress and is associated with an increase of antioxidant enzyme activities as one effector of the neuroprotection. New Zealand White rabbits were subjected to HBO preconditioning, hyperbaric air (HBA) preconditioning, or sham pretreatment once daily for five consecutive days before spinal cord ischemia. Activities of catalase (CAT) and superoxide dismutase were increased in spinal cord tissue in the HBO group 24 h after the last pretreatment and reached a higher level after spinal cord ischemia for 20 mins followed by reperfusion for 24 or 48 h, in comparison with those in control and HBA groups. The spinal cord ischemic tolerance induced by HBO preconditioning was attenuated when a CAT inhibitor, 3-amino-1,2,4-triazole,1 g/kg, was administered intraperitoneally 1 h before ischemia. In addition, administration of a free radical scavenger, dimethylthiourea, 500 mg/kg, intravenous, 1 h before each day's preconditioning, reversed the increase of the activities of both enzymes in spinal cord tissue. The results indicate that an initial oxidative stress, as a trigger to upregulate the antioxidant enzyme activities, plays an important role in the formation of the tolerance against spinal cord ischemia by HBO preconditioning.
Introduction
In our previous studies, we showed that repeated hyperbaric oxygen (HBO) preconditioning, but not hyperbaricity, induced an ischemic tolerance both in the brain and spinal cord (Dong et al, 2002; Xiong et al, 2000), which was consistent with the results reported by Wada in gerbil hippocampus (Wada et al, 1996). We further proved that administration of dimethylthiourea (DMTU), a scavenger of oxygen-free radicals, abolished the ischemic tolerance induced by HBO (Xiong et al, 2001). It has been proposed that a nonlethal level of reactive oxygen species (ROS) generation is an initiator or mediator for ischemic tolerance induction (Ohtsuki et al, 1992). On the other hand, the molecular mechanism underlying HBO preconditioning remains poorly understood.
Several studies have shown that endogenous antioxidant enzymes could be induced in parallel to the development of the neuroprotection by different other preconditioning methods such as lipopolysaccharide (LPS), brief ischemia and peroxisome proliferator-activated receptor-alpha (PPAR-α) activation, etc. (Bordet et al, 2000; Deplanque et al, 2003; Duan et al, 1999; Garnier et al, 2001; Kato et al, 1995; Toyoda et al, 1997). Therefore, we postulate that during HBO preconditioning ROS activates endogenous antioxidant enzymes, which then scavenge the ROS produced during ischemia–reperfusion and protects the spinal cord from ROS-mediated injury. The current study is undertaken to investigate that (1) whether the antioxidant enzymes are activated after HBO preconditioning; (2) if so, whether an inhibitor on antioxidant enzyme administered before spinal cord ischemia can abolish the ischemic tolerance; (3) whether the antioxidant enzyme activities are changed after repeated HBO preconditioning when an ROS scavenger is administered before each session of HBO treatment.
Materials and methods
The experimental protocol used in this study was approved by the Ethics Committee for the Animal Experimentation and was conducted according to the Guidelines for the Animal Experimentation of our institutes. The animals were studied at Xijing Hospital, Fourth Military Medical University (Xi'an, China).
Animals and Surgical Preparation
All experiments were performed on male New Zealand White rabbits weighing 2.2 to 2.5 kg. After an overnight fast with unrestricted access to water, the rabbits were anesthetized with pentobarbital sodium (30 mg/kg, intravenous). The lactated Ringer solution (4 mL/kgh) was infused intravenously. A 22-gauge catheter was inserted into the ear artery to measure the proximal blood pressure. Another catheter was inserted to the left femoral artery to measure the distal blood pressure. Blood pressure was monitored continuously by using a calibrated pressure transducer connected to an invasive pressure monitor (Spacelabs Med. Inc., Redmond, WA, USA). Rectal temperature was maintained between 38°C and 39°C by an overhead lamp during the experiments. Arterial blood was sampled at preischemic state, 10 mins after ischemia as well as 10 mins after reperfusion, respectively, for the determination of arterial oxygen tension (PaO2), arterial carbon dioxide tension (PaCO2), pH, and plasma glucose. Arterial blood gases were measured by means of the OMNI Modular System (AVL List GmbH Medizintechnik, Kleiststraße, Graz, Austria).
Spinal Cord Ischemia
Animals were placed in supine position. The abdominal aorta was exposed at the level of the left renal artery through a 3 to 4 cm long medial incision. Spinal cord ischemia was induced with the aorta clamping with a bull-dog clamp just below the renal artery and 400 units of heparin was administered 5 mins before the aortic occlusion. Obstruction of the blood flow lasted for 20 mins. Then the bull-dog clamp was removed and the abdominal wall was closed with wound clips. The local infiltration around the wound with 0.25% of bupivacaine hydrochloride was applied for postoperative analgesia. An antibiotic (40,000 IU gentamicin) was administered intramuscularly immediately after the operation. The animals were then returned to their home cage and survived for 2 days. Bladder content was compressed manually as required.
Neurologic and Histopathologic Evaluations
In experiment 1, the animal's behavior was neurologically assessed at 6, 24, and 48 h after reperfusion by an observer who was unaware of the grouping. A modified Tarlov criteria (Jacobs et al, 1987) was used: score (0) no voluntary hind-limb function; (1) only perceptible joint movement; (2) active movement but unable to stand; (3) to be able to stand but unable to walk; (4) complete normal hind-limb motor function.
A histopathologic evaluation was performed in the spinal cord at 48 h after reperfusion in experiment 2. Transcardiac perfusion and fixation were performed with 1,000 mL heparinized saline followed by 500 mL 10% buffered formalin. The lumbar spinal cord was removed and refrigerated in 10% phosphate-buffered formalin for 48 h. After dehydration in the graded ethanol and butanol, the spinal cord was embedded in the paraffin. Coronal sections of the spinal cord (L5 segment) were cut at a thickness of 6 μm and stained with hematoxylin and eosin. Neuronal injury was evaluated at a magnification of × 400 by an observer who was unaware of the grouping. Injured neurons were identified by intensely eosinophilic cytoplasm with loss of Nissl substance and by the presence of pyknotic homogenous nuclei. The remaining normal neurons in the ischemic ventral spinal cord in each animal, judged by their morphological appearance, were counted in three sections selected randomly from the rostral, middle, and caudal levels of the L5 segment and then averaged. The numbers of normal neurons per section were compared among four groups.
Measurement of Antioxidant Enzyme Activity and Malondialdehyde Content
Spinal cord tissues of L5–7 level were homogenized in cold saline with a weight-to-volume ratio of 1:10. The homogenate was centrifuged at 3,000 r/min for 15 mins at 4°C and the supernatant was removed to a cuvette for the next assay. Both the measurements of antioxidant enzyme activities and malondialdehyde (MDA) content in tissue homogenate were performed according to the technical manual of the detection kits (Jianchen Biological Institue, China)(Dong et al, 2000; Liu et al, 2004). Malondialdehyde content was measured with a visible light spectrophotometer in mmol/mg prot for spinal cord tissue by using the thiobarbituric acid reactive substances assay. Superoxide dismutase (SOD) activity was measured following the reduction of nitrite by a xanthine-xanthine oxidase system, which is a superoxide generator. One unit of SOD is defined as the amount that shows 50% inhibition. The activity was expressed as U/mg prot. Catalase (CAT) activity in the spinal cord tissue was assayed by measuring absorbance at 240 nm using an ultraviolet light spectrophotometer (Beckman, USA) and was expressed as U/g prot. The definition of its activity was based on the hydrogen peroxide decomposition rate at 240 nm in the reactive mixture, of which the absorbance was between 0.5 and 0.55. Glutathione peroxidase (GSH-px) activity was measured by measuring the absorbance at 412 nm. The GSH-px in 1 g protein that led to the decrease of 1 μmol/L GSH in the reactive system per minute was defined as one vital unit.
Experimental Designs
Experiment 1: effect of repeated hyperbaric oxygen preconditioning on spinal cord antioxidant enzyme activities: A total of 57 male New Zealand White rabbits were randomly divided into three groups (n = 19 for each): the HBO, hyperbaric air (HBA), and control groups. Animals in the HBO group were exposed to HBO at 2.5 atmosphere absolute (ATA) in 100% oxygen 1 h each day for five consecutive days. Animals in the HBA group underwent 1 h treatment in 21% O2 at 2.5 ATA 1 h each day for 5 days. Animals in the control group were placed in a chamber (21% O2), in which the air was not pressurized for sham pretreatment, on the same schedule as for the HBO and HBA groups. Four rabbits from each group were killed at 24 h after the last pretreatment as preischemic controls, the others (n = 15 for each group) were subjected to a spinal cord ischemia for 20 mins. During the reperfusion period, animals were reanesthetized and killed at 6, 24, and 48 h after reperfusion (n = 5 for each time point in each group). Spinal cord tissue of L5–7 level were sampled and frozen at −70°C in freezer for the determination of antioxidant enzyme activities and MDA content.
Experiment 2: effect of catalase inhibitor 3-amino-1,2,4-triazole on the induction of ischemic tolerance by hyperbaric oxygen: Part I: The purpose of this part of the experiment was to determine the adequate dose of the inhibitor to be administered. Twenty male New Zealand White rabbits were randomly assigned into four groups averagely. All the animals were exposed to HBO (2.5 ATA, 100% O2) 1 h a day for five consecutive days. Animals in the HBO group received an injection of saline, while animals in HBO + AT1, HBO + AT2, and HBO + AT3 groups received a CAT inhibitor 3-amino-1,2,4-triazole (AT, Sigma-Aldrich Co., USA) intraperitoneally at doses of 0.5, 1, and 1.5 g/kg, respectively, at 23 h after the last pretreatment of HBO. Spinal cord tissue was sampled 1 h after AT administration for the determination of CAT activity.
Part II: Thirty-two rabbits were randomly assigned into four groups: control, AT, HBO, and HBO + AT groups (n = 8 for each). Animals in HBO and HBO + AT groups underwent HBO pretreatment, and those in control and AT groups received sham pretreatment as described in experiment 1. Twenty-four hours after the last pretreatment, all animals were subjected to a spinal cord ischemia for 20 mins. One hour before ischemia, AT was administered intraperitoneally in AT and HBO + AT groups according to the dose screened from Part I, while rabbits in the control and HBO groups received a saline administration. Forty-eight hours after reperfusion, the hind-limb motor function was evaluated by using Tarlov criteria and the histopathologic analysis in H&E-stained sections from lumbar spinal cord (L5 segment) were performed. The numbers of normal neurons per section were compared among four groups.
Experiment 3: the effect of dimethylthiourea on antioxidant enzyme activities after repeated hyperbaric oxygen preconditioning: Twenty-four rabbits were assigned into four groups (n = 6 for each): control, HBO, HBO + DMTU, and DMTU groups. In control and HBO groups, the 5 mL/kg of saline was administered to the rabbits 1 h before each session of pretreatment. In DMTU and HBO + DMTU groups, 10% DMTU (Sigma-Aldrich Co., USA) dissolved in saline (5 mL/kg) was administered at the same time point. The method for sham pretreatment and HBO preconditioning was the same as experiment 1. Spinal cord SOD activity, CAT activity, and the content of MDA were measured 24 h after the last session of pretreatment.
Statistical Analysis
Blood pressure, blood gases, plasma glucose, antioxidant enzyme activities, and MDA content were expressed as mean ± s.d. and compared by using a one-way analysis of variance (ANOVA), followed by a Student–Newman–Keuls (SNK) test for multiple comparisons. The scores of hind-limb motor function and the numbers of normal neurons in the anterior spinal cord were analyzed by using a non-parametric method (Kruskal–Wallis test) followed by the Mann-Whitney U-test with Bonferronic correction. A P-value of less than 0.05 was considered to be statistically significant.
Results
Experiment 1
Physiologic variables: Physiologic variables are shown in Table 1. The hemodynamics, rectal temperature, arterial pH, PaCO2, PaO2, and blood glucose concentrations were similar in all groups, regardless of the treatment patterns (Table 1). The distal blood pressure was approximately 12 to 13 kPa before blocking the abdominal aorta and decreased to 1.0 to 1.1 kPa during the artery was clamped. Ten minutes after the beginning of reperfusion, the value of the distal blood pressure was recovered to nearly preischemic level.
Physiologic variables during pre- and post-ischemic state (n = 15 in each group)
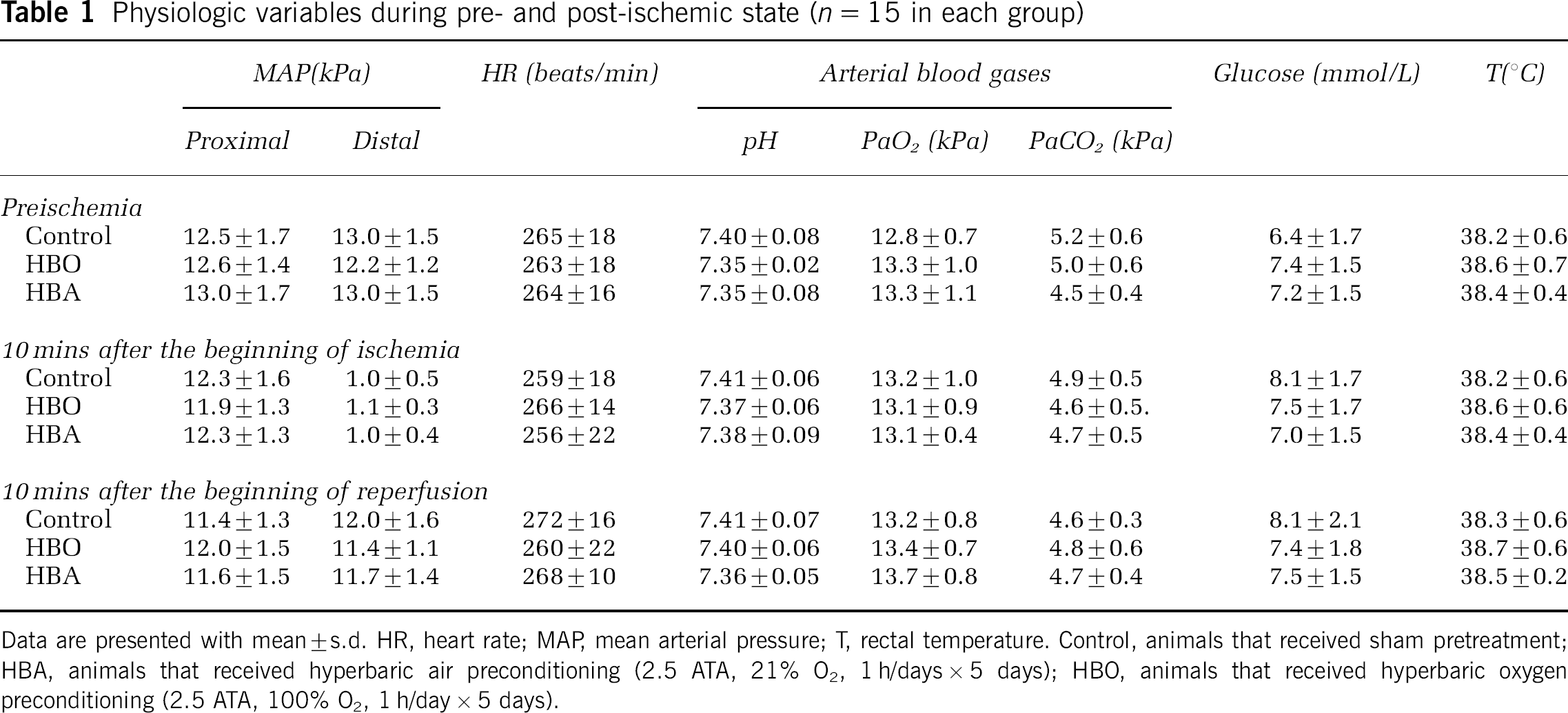
Data are presented with mean ± s.d. HR, heart rate; MAP, mean arterial pressure; T, rectal temperature. Control, animals that received sham pretreatment; HBA, animals that received hyperbaric air preconditioning (2.5 ATA, 21% O2, 1 h/days × 5 days); HBO, animals that received hyperbaric oxygen preconditioning (2.5 ATA, 100% O2, 1 h/day × 5 days).
Neurologic outcome: All animals survived until the final neurologic behavior assessment at 6, 24, and 48 h after reperfusion. The neurologic outcome in the HBO group was better than that of the control and HBA groups, respectively (P < 0.05). Four animals showed complete normal motor function (Tarlov score = 4) in the HBO group at 48 h after reperfusion. No animals in either the control or the HBA group showed normal motor function at 48 h after reperfusion. The hind-limb motor function scores of three groups at different time points after reperfusion are shown in Table 2.
Hind-limb motor function scores in each group at different time after reperfusion
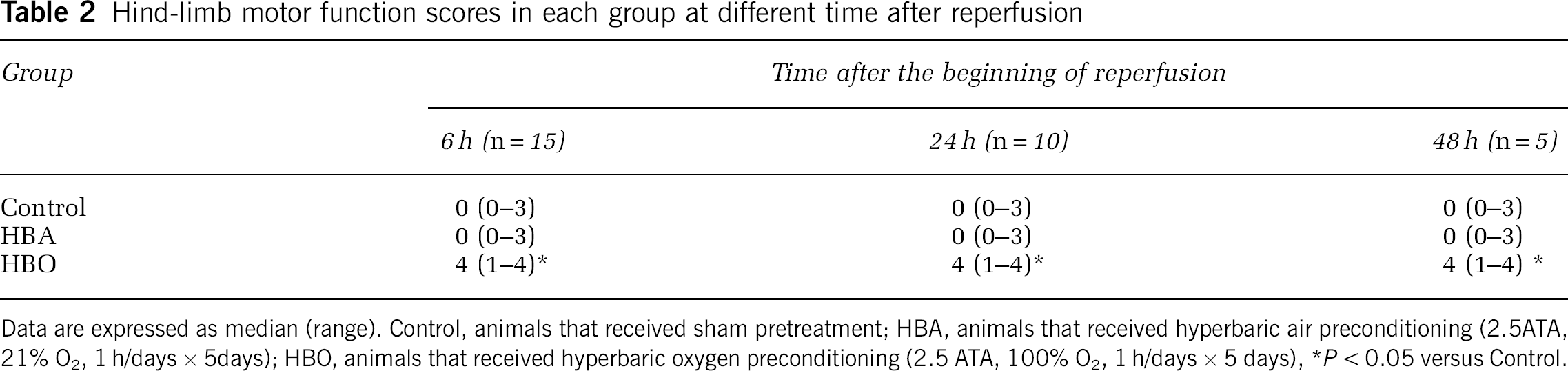

Data are expressed as median (range). Control, animals that received sham pretreatment; HBA, animals that received hyperbaric air preconditioning (2.5ATA, 21% O2, 1 h/days × 5days); HBO, animals that received hyperbaric oxygen preconditioning (2.5 ATA, 100% O2, 1 h/days × 5 days)
P < 0.05 versus Control.
Antioxidant enzyme activities in spinal cord: At 24 h after the last pretreatment, activities of CAT and SOD in spinal cord tissue in HBO group were higher than that of the control and HBA groups (P < 0.001 for both). A higher activity of CAT was found in the HBO group when compared with that in the other two groups at 6 h (P = 0.032 versus control; P = 0.023 versus HBA), 24 h (P = 0.004 versus control; P = 0.006 versus HBA), and 48 h (P < 0.001 versus both control and HBA) after reperfusion. The comparison of SOD activity among three groups revealed similar results as that of CAT at 24 h after reperfusion (for HBO, P = 0.021 versus control; P = 0.017 versus HBA) and 48 h (for HBO, P = 0.003 versus control; P < 0.001 versus HBA). No significant difference was observed between the control and HBA groups at corresponding time points. In addition, CAT and SOD activities in all three groups decreased at 24 and 48 h after reperfusion, compared with preischemic state (P < 0.05) (Figures 1A and 1B).
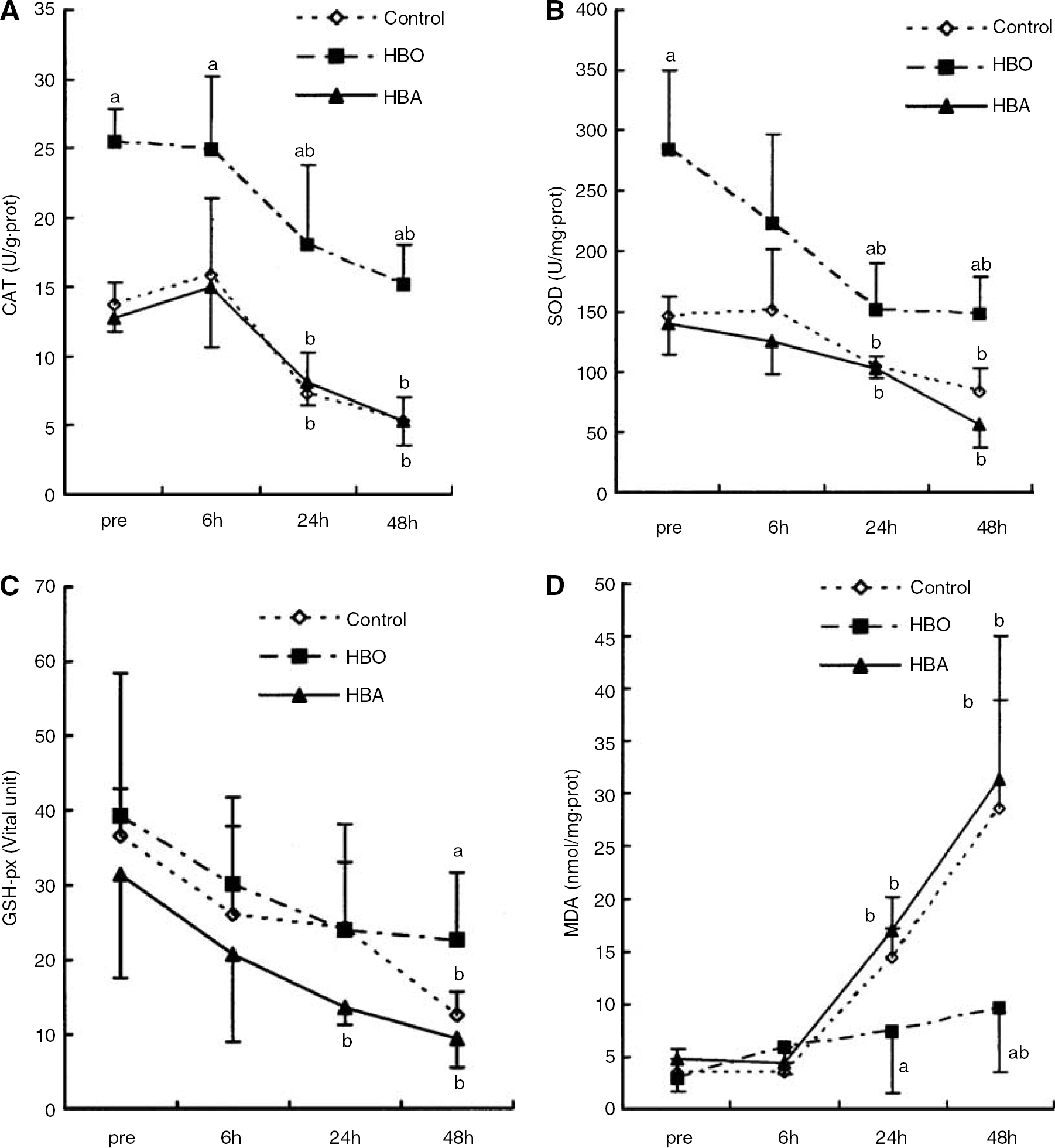
Experiment 1: Activities of catalase (CAT) (
As for GSH-px activity, no difference was found among three groups at 24 h after last pretreatment, although its activity in the HBO group was higher than that in the other two groups at 48 h after reperfusion (P = 0.042 versus control; P= 0.012 versus HBA). In control and HBA groups, GSH-px activity decreased at 48 h after reperfusion in comparison with preischemic state (P = 0.002 for control; P = 0.003 for HBA). While in the HBO group, no significant difference was observed among different time points (Figure 1C).
Malondialdehyde content in spinal cord tissue: Malondialdehyde content in the spinal cord tissue in the HBO group was significantly lower at 24 and 48 h after reperfusion compared with that in the control (P = 0.041 for 24 h; P = 0.033 for 48 h) and HBA (P = 0.009 for 24h; P = 0.018 for 48 h) groups. It is noticed that within HBO group, MDA content increased at 48 h after reperfusion, compared with preischemic state (P = 0.038). While in the control and HBA groups, MDA content increased significantly compared with preischemic state at both 24 and 48 h after reperfusion (Figure 1D).
Experiment 2
Determination of 3-amino-1,2,4-triazole dose: Increased CAT activity in the spinal cord induced by HBO preconditioning was obviously attenuated by an administration of AT at doses of 1 or 1.5 g/kg intraperitoneally at 23 h after the last treatment (Figure 2). While at the dose of 1 g/kg, the level of CAT activity after HBO preconditioning was inhibited to the level near the control. Therefore, in the following experiment a dose of 1 g/kg for AT was used 1 h before ischemia in the AT and HBO + AT groups.

Experiment 2: the inhibitory effect of 3-amino-1,2,4-triazole (AT) on the activity of catalase (CAT) in the spinal cord tissue. The dashed line represents CAT activity in the control group at 24 h after the last sham pretreatment (13.82 U/g · prot).
Effect of 3-amino-1,2,4-triazole on ischemic tolerance induced by hyperbaric oxygen preconditioning: Forty-eight hours after reperfusion, animals in the HBO group showed higher hind-limb motor function scores than those in the control (P = 0.006) and AT groups (P = 0.0012). There were no significant differences in hind-limb motor function scores of animals in the HBO + AT group in comparison with the HBO, AT, or control groups (P > 0.05 for each comparison). Also, no difference was observed between the control and AT groups (P = 0.878) (Figure 3).
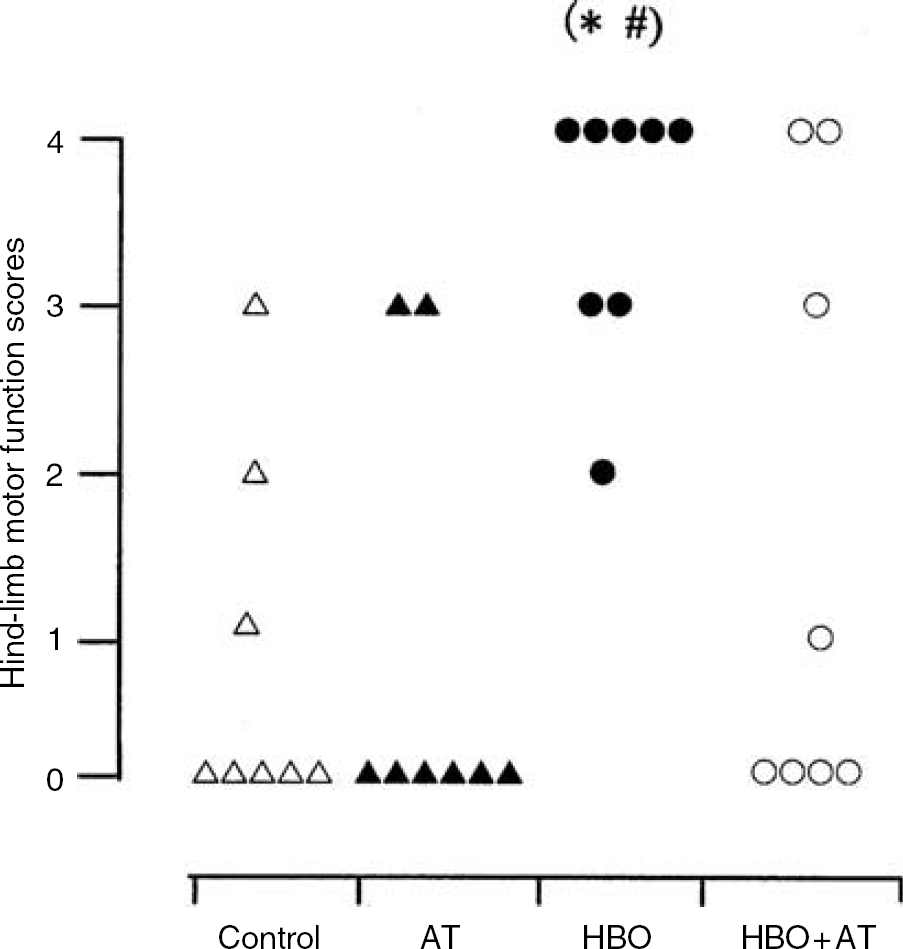
Experiment 2: hind-limb motor function scores in each animal of four groups at 48 h after reperfusion (*P < 0.05 versus control, #P < 0.05 versus 3-amino-1,2,4-triazole (AT)). △, ▴, •, and ◯ represents animals in control, AT, hyperbaric oxygen (HBO), and HBO + AT groups, respectively. Control, animals that received sham pretreatment; HBO, animals that received hyperbaric oxygen preconditioning (2.5 ATA, 100% O2, 1 h/day × 5 days); AT, animals that received sham pretreatment and AT administration 1 h before ischemia began; HBO + AT, animals that received HBO preconditioning and AT administration 1 h before ischemia began.
Forty-eight hours after reperfusion, more normal motor neurons in the anterior spinal cord were seen in HBO group compared with the other three groups (P = 0.012 versus control; P = 0.012 versus AT; P = 0.012 versus HBO + AT). The numbers of normal motor neurons in the HBO + AT group revealed no significant difference compared with the control (P = 0.328) and AT (P = 0.065) groups. No difference was observed between the control and AT groups (P = 0.505) (Table 3).
Numbers of normal neurons in the anterior spinal cord 48 h after reperfusion
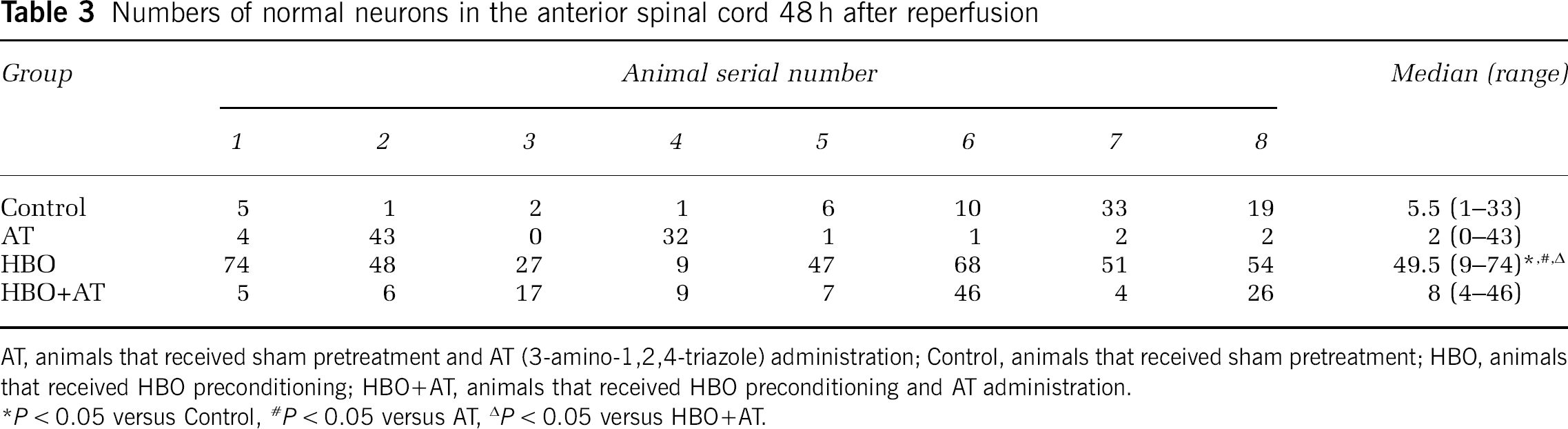
AT, animals that received sham pretreatment and AT (3-amino-1,2,4-triazole) administration; Control, animals that received sham pretreatment; HBO, animals that received HBO preconditioning; HBO+AT, animals that received HBO preconditioning and AT administration.
P < 0.05 versus Control
P < 0.05 versus AT
P < 0.05 versus HBO+AT.
Experiment 3
Twenty-four hours after the last pretreatment, the activities of CAT and SOD in spinal cord tissue of HBO group were higher than those in the control, DMTU, and HBO + DMTU groups (P < 0.01). No difference was observed among the control, DMTU, and HBO + DMTU groups. Malondialdehyde contents in the spinal cord were lower in DMTU and HBO + DMTU groups than that in the control (P = 0.025) and HBO (P = 0.008) groups, respectively. No difference in MDA content was observed between DMTU and HBO + DMTU groups (P = 0.943) (Figure 4).
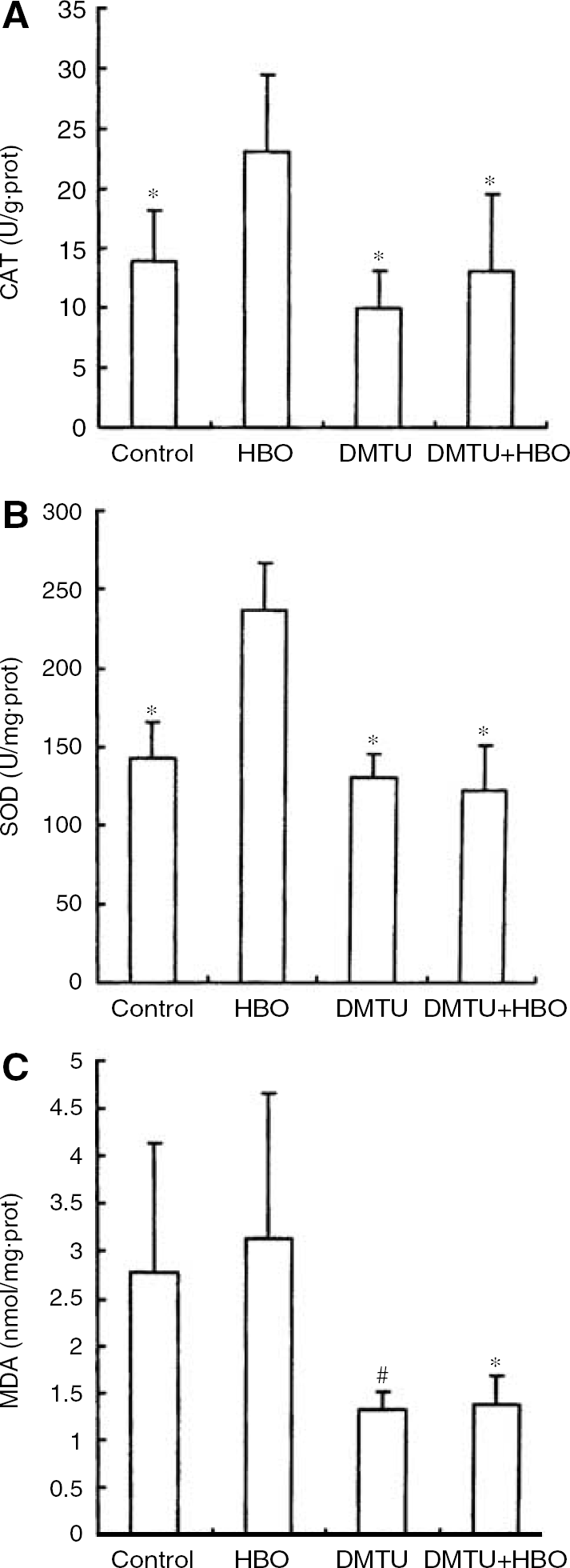
Experiment 3: (
Discussion
In the present study, we showed that repeated HBO preconditioning induced an increase in activities of major antioxidant enzymes, especially CAT and SOD, in the spinal cord tissue without affecting the activity of GSH-px. Although antioxidant enzyme activities decreased after transient spinal cord ischemia, significantly higher activities of CAT and SOD were seen in the HBO group than that in the control and HBA groups at several time points. The results in experiment 2 showed that tolerance against spinal cord ischemia after HBO pretreatment was attenuated by an administration of CAT inhibitor, AT. Furthermore, DMTU (a potent free radical scavenger) administration before each day's HBO treatment completely abolished the increase of CAT and SOD activities after HBO preconditioning, indicating a close relationship between the ROS generation and the increase of antioxidant enzyme activities. Our results strongly suggest the involvement of enhanced endogenous antioxidant enzyme activities, especially CAT, in the induction of tolerance against spinal cord ischemia by HBO preconditioning is via a ROS -mediated way.
Our results are in accordance with those studies that suggest the role of antioxidant enzymes in the formation of the ischemic tolerance induced by various ischemic and nonischemic preconditioning means. It has been reported that occlusion of the middle cerebral artery for 20 mins, 24 h in advance, significantly increased the activity of the antioxidant enzyme SOD and reduced the cerebral infarction volume caused by test ischemia (Toyoda et al, 1997). Ischemic tolerance is induced in part by enhanced synthesis of Mn-SOD in the tolerance-acquired hippocampus (Kato et al, 1995). LPS-induced ischemic tolerance in the brain parallels the LPS-induced increase of SOD synthesis in the organ (Bordet et al, 2000). The LPS is responsible for the induction of SOD in cultured neuronal and glial cells (Kifle et al, 1996; Yu et al, 1999). Chronic treatment with peroxisome proliferator-activated receptor-alpha (PPAR-α) activator induces an increase in activities of copper/zinc SOD and enzymes involved in glutathione metabolism, which protect against the subsequent brain injuries (Deplanque et al, 2003). Oxygen radicals and their specific scavenging enzymes seem to be involved in the development of tolerance to hypoxia (Duan et al, 1999). Transient hypoxia enhances the antioxidative enzymatic defenses of the brain, which are susceptible to increased tolerance against a subsequent damaging insult (Garnier et al, 2001).
Hyperbaric oxygen preconditioning is capable of inducing ischemic tolerance not only in the brain (Prass et al, 2000; Wada et al, 1996; Xiong et al, 2000) but also in other organs, such as the liver, heart, and spinal cord. Hyperbaric oxygen preconditioning attenuated the ischemia-reperfusion injury in the liver in rat model (Chen et al, 1998). Ischemic tolerance was also found in the myocardium in HBO-pretreated rats (Kim et al, 2001). Earlier in a model of spinal cord ischemia, we showed that repeated HBO preconditioning induced tolerance against spinal cord ischemia in rabbits (Dong et al, 2002). We postulate that something common might account for the mechanism underlying the induction of tolerance in different tissues. Kim et al (2001) found that catalase gene was induced in the hearts of HBO-pretreated rats, which was responsible for the myocardial tolerance against ischemia–reperfusion. Our data on histopathologic examination of the experiment 2 indicate that administration of CAT inhibitor, AT, attenuated the ischemic tolerance induced by HBO, but the result of neurologic behavioral outcome of same group was inconsistent. By using the latter method, no difference was found between HBO and HBO + AT groups, indicating that the neurologic behavioral scoring is less sensitive in evaluation of the protective tolerated effect of preconditioning. The results of Kim et al (2001) and ours suggest that CAT plays an important role in the induction of ischemic tolerance by HBO preconditioning both in hearts and spinal cords. In a study of immunocytochemical localization of CAT in the central nervous system of the rat, the researchers found that intensely stained CAT-immunoreactive cells corresponded to neurons known to be resistant to ischemia-reperfusion injury, whereas weakly stained cells corresponded to neurons that are more susceptible to ischemic damage (Moreno et al, 1995). Thus, the activity of CAT may be critical for a protective effect against oxidative stress under pathological conditions, such as ischemia–reperfusion injury.
How HBO preconditioning upregulates the activities of antioxidant enzymes is an interesting question. Reactive oxygen species seems to play a role of activator. Reactive oxygen species has proven to be the second messenger for the induction of antioxidant enzymes in both prokaryotes and eukaryotes. It has also been reported that in prokaryotes H2O2 modifies protein structure of a transcription factor oxyR to an activated form that induces the expression of the catalase gene (Storz et al, 1990; Storz and Tartalia, 1992). Since HBO stimulates ROS production, it is reasonable to imagine that the increased level of ROS stimulates the induction of the catalase gene in HBO-pretreated spinal cord. In our experiment, DMTU administration abolished the increase of antioxidant enzyme activities by HBO preconditioning, indicating ROS is a crucial activator of the activities of antioxidant enzymes.
We also noticed an increase of SOD activity in the spinal cord tissue in HBO-pretreated rabbits. A similar result was found in the experiment carried on the brain of gerbil, in which Wada et al (2001) have showed an increased immunoreactivity of Mn-SOD in CA1 in HBO-pretreated gerbils. Therefore, SOD probably plays a role in the ischemic tolerance formation. It has been proved that the 5′ flank region of the Mn-SOD gene contains a putative binding site for NF-κB, which is activated by ROS (Lenardo and Baltimore, 1989). To understand its real role in the process of ischemic tolerance formation demands further study. As for GSH-px activity, no significant difference was observed among three groups at 24 h after the last pretreatment in the present study. Although higher activity of GSH-px was seen in the HBO group compared with that in the control and HBA groups at 48 h after reperfusion, its relationship with the ischemic tolerance is unclear.
The content of MDA, an indicator of lipid peroxidation, was measured in our experiments. The present results did not show an obvious change on MDA level in the spinal cord tissue 24 h after the last pretreatment of HBO. There are two possible explanations: firstly, HBO preconditioning increased the activities of CAT and SOD, thus scavenged excessive ROS and attenuated the lipid peroxidation; secondly, the ROS was not obviously increased at the time points examined. In the reperfusion period, MDA content in the spinal cord tissue in the HBO group was lower than that in control and HBA groups, indicating that ROS-mediated damage was limited owing to the enhanced activity of antioxidant enzymes to scavenge excessive free radicals.
It is needed to point out that there exist some other mechanisms, in addition to free radicals, responsible for ischemic damage, such as neurotoxic excitatory amino-acid accumulation, inflammation, overloaded calcium, apoptosis, and so on (Kuzelova and Svec, 2001; Schaller and Graf, 2004; Zhang et al, 2004). Thus, the induction of ROS and the subsequent enhancement of the capability of tissue to sustain another oxidative cascade may possibly be one of potential mechanisms for HBO preconditioning-induced ischemic tolerance. To explore other related mechanisms demands further studies.
In conclusion, the present study shows that repeated HBO preconditioning (2.5 ATA, 100% O2, 1 h/day × 5 days) upregulated the activities of CAT and SOD in ischemic spinal cord tissue thereby protected spinal cord against ischemia-reperfusion damage. The DMTU, a potent free radical scavenger, abolished the increase of CAT and SOD activities in the spinal cord after serial HBO preconditioning. The CAT inhibitor AT attenuated the ischemic tolerance induced by HBO. The results suggest that ROS generated in HBO process triggers the cascade in cellular events leading to increased antioxidant enzyme activities, which scavenge the ROS and protect spinal cord from ischemia–reperfusion injury.
Footnotes
Acknowledgements
This work was conducted in the laboratory of Department of Anesthesiology, Xijing Hospital, Fourth Military Medical University, Xi'an, Shaanxi, China.
