Abstract
Crocodile attack injuries plague communities near bodies of water and continue to be an infrequent but significant form of trauma encountered in our medical facility. Regional anesthesia techniques are a novel adjunct to treatment and may facilitate simplified definitive management and better utilization of constrained operating room resources. We report a case of an adult male who presented with a large lower extremity wound after a crocodile bite. The patient was managed with initial debridement and irrigation and serial wound care entirely under regional anesthesia at the bedside. The patient did not develop wound infection, eventually receiving a skin graft with good functional outcomes. Regional anesthesia techniques are increasingly being used in the trauma setting, and their versatility allows for their use in multiple settings, by practitioners with limited experience and in resource-limited environments. No specific guidelines exist for performance of neuraxial techniques in the setting of animal bite injuries, but concerns about infectious complications have been raised. Regional anesthesia techniques may be useful in the management of extremity trauma due to crocodile attacks without infectious complications. They may reduce utilization of theatre resources and reduce opioid requirements.
Introduction
This case has been reported in accordance with the surgical case report guidelines criteria. 1 Crocodiles (family Crocodylidae) are one of 3 families of surviving ancient Archosaurian, predatory, semiaquatic reptiles. Other than medically important venomous snakes, crocodilians are responsible for more human injuries globally than any other reptile. 2 The Nile crocodile (Crocodylus niloticus) in particular has been responsible for more human fatalities than all of the other species of crocodilians combined.2,3
The risk of human–crocodile conflict is higher in some global regions where riparian communities are dependent on local water bodies that are inhabited by crocodiles (eg, the Shire River in Malawi, 4 Lake Victoria in Uganda 5 and Lake Tanganyika in Tanzania). 6 C niloticus has extensive distribution in Africa, from Southern Africa 7 to the Sahara 8 and from Eastern Africa extending to the Albertine rift. 9 However, relict populations persist in Chad and Mauritania 8 as well as in Madagascar. 10 Its range is now considered to be much smaller than was previously thought after populations to the west of the Albertine rift were recently designated as a new species, the West African crocodile (Crocodylus suchus). 7 –10
The Nile crocodile is distributed throughout Zimbabwe. 11 The largest populations tend to be found in warmer waters, especially in the north part of the country, including Lake Kariba, Lake Manyame, and Lake Chivero. 12 Lake Chivero is a reservoir on the Manyame River in Zimbabwe, located southwest of Harare, and provides the main water supply for the city. These water bodies are home to substantial biodiversity, including 26 species of fish. 13 These not only provide sustenance for the crocodile population but are also one of the principal reasons for human–crocodile conflict because they attract human fishermen and crocodiles alike. 14
It is frequently said in the lay press that more people are killed by crocodiles each year in Africa than by all other animals combined. However, the true incidence of crocodile attacks on humans is difficult to obtain. 3 Attacks frequently occur in remote, inaccessible areas, and the majority of attacks are thought to go unreported. Available data show that attacks are seasonal, with a peak in incidence during the rainy season.3,9
We report a case report of a bite from C niloticus in an adult male managed with regional anesthesia techniques. This provided effective analgesia that facilitated initial debridement, serial daily dressings, and physiotherapy. This is a useful technique in management of these wounds.
Case presentation
A previously well 31-y-old male patient presented to our accident and emergency department after having been attacked by a crocodile 19 h earlier while fishing on the shores of Lake Chivero in Zimbabwe. He had been in the water up to his knees on the south shore of the lake at 2300 the night before in the company of 1 other person. The crocodile had approached him from behind and lunged forward, biting his right thigh. He was submerged in the water when the crocodile rolled over in the water once. He held the snout of the crocodile and attempted to open its jaws while his companion made noises in an attempt to distract the animal. He was eventually released by the retreating crocodile after a 3- to 5-min struggle. His companion called for help, and he was taken by boat to the National Parks office and from there to a district hospital, after which he was transferred to our institution. Five hours elapsed from the incident to arrival at our hospital.
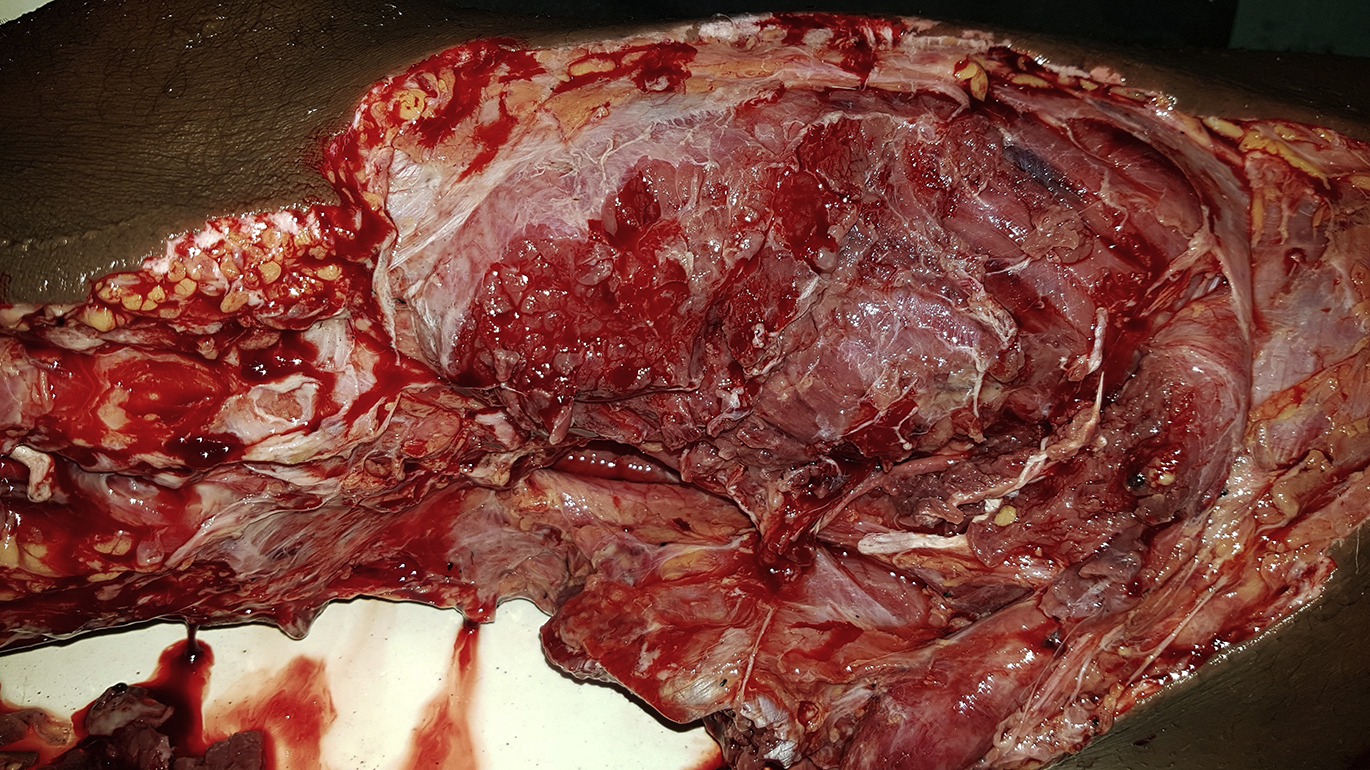
On arrival he was tachycardic (103 beats·min-1) and blood pressure was 145/62 mm Hg. He was mildly pale and in significant pain but was fully alert. He had a large anteromedial thigh and leg laceration with ragged edges (Figure 1). The major vessels were exposed due to transection of the sartorius muscle in the midthigh but were uninjured. There was no major active bleeding. There was no neurologic deficit of the sciatic or femoral nerves and distal pulses were present. He also had defensive injuries to the fingers of both hands with avulsion of the tip of the distal phalanx of the right middle finger (Figure 2).

Appearance of the bite wound in the emergency department, which shows ragged, irregular wound edges with significant tissue loss.
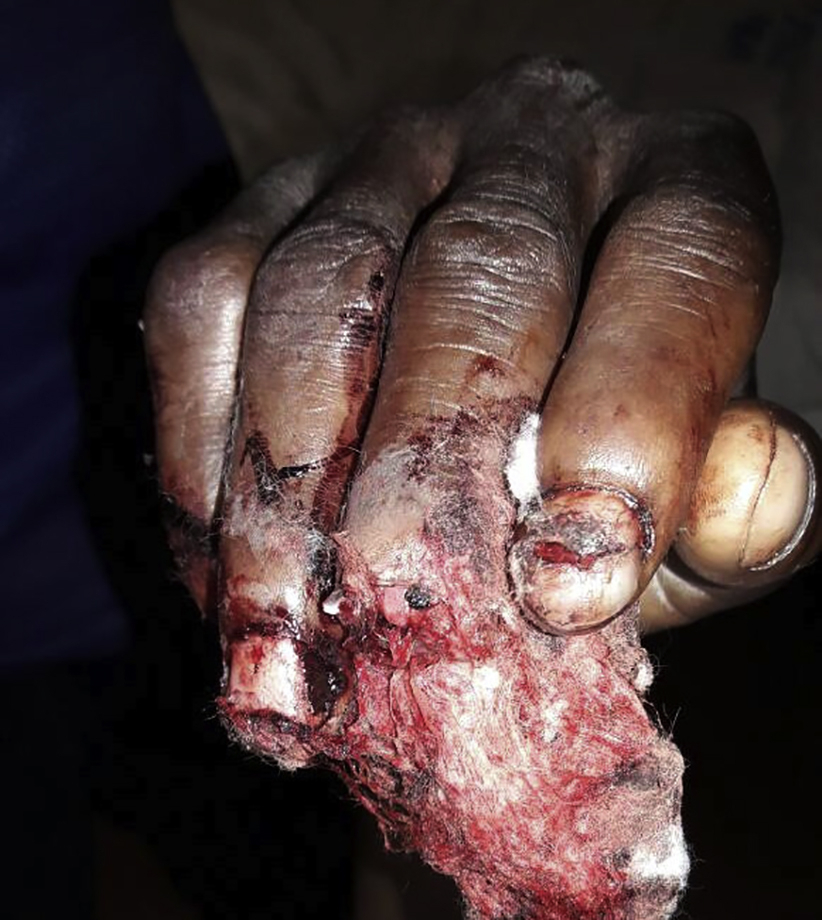
Appearance of the fingers of the right side, which shows defensive injuries including amputation of the terminal end of the middle finger.
The patient was admitted immediately for fluid resuscitation and intravenous empirical antibiotic therapy that consisted of 1 g of ceftriaxone twice daily and 500 mg of intravenous metronidazole 3 times a day as well as 80 mg of gentamycin twice a day for 5 d pending microbiologic sensitivity results. Because of significant pain, rated as 8 out of 10 on a verbal rating scale, analgesia with 100 mg of intramuscular pethidine and 75 mg of intramuscular diclofenac was administered and continued 3 times a day thereafter. There was an improvement of the pain score to 4 out of 10 after administration of analgesia. He was subsequently prepared for emergency debridement. Initial blood tests revealed a leukocytosis of 14.3 cells·μL-1 and normal hemoglobin of 13.4 g·dL-1.
Because of an inability to get access to the operating room that night, a decision was made to debride the wound under regional anesthesia. The required field was determined to be the anteromedial thigh: L2, 3, and 4, and posteromedial thigh: S1 and S2. A sciatic nerve block was performed with the posterior transgluteal (Labat) approach using 10 mL of 10% lignocaine with 1:100,000 adrenaline. A femoral nerve block was performed without ultrasound guidance. Block success was determined by absence of pain on stimulation with a needle in the required area because no nerve stimulator was available. Both blocks had their duration of action prolonged with simultaneous administration of 8 mg intravenous dexamethasone. Ultimately the duration of blockade was 18 h.
Both blocks resulted in extremely effective anesthesia of nearly the entire lower limb. Sharp debridement was done with lavage of the wound with 5 L of saline and betadine (Figure 3). The blockade provided effective analgesia for the wound after debridement and allowed for early mobilization of the patient. Adequate pain relief was achieved with a combination of nerve blocks and diclofenac, facilitating subsequent serial wound irrigation and dressing by the surgeon (Figure 4) every day for 2 wk after the incident and intensive physiotherapy. Pethidine was reduced to 50 mg on the first postoperative day, and this was stopped altogether the next day. Microbiology from the initial debridement sample eventually revealed profuse growth of Klebsiella pneumoniae, and antibiotics were switched to intravenous meropenem: 500 mg given 3 times a day, according to the sensitivity of the isolate shown on the antibiogram. During admission the patient maintained a normal white cell count (below 10.0 cells·μL-1) and a consistently normal temperature. The wound bed never showed signs of infection. The wound eventually was considered ready for skin graft, and postoperatively the function of the limb was maintained (Figure 5). The patient was doing well after discharge on review.
Appearance of the bite wound immediately after debridement. Clean, healthy bleeding wound edges are shown.
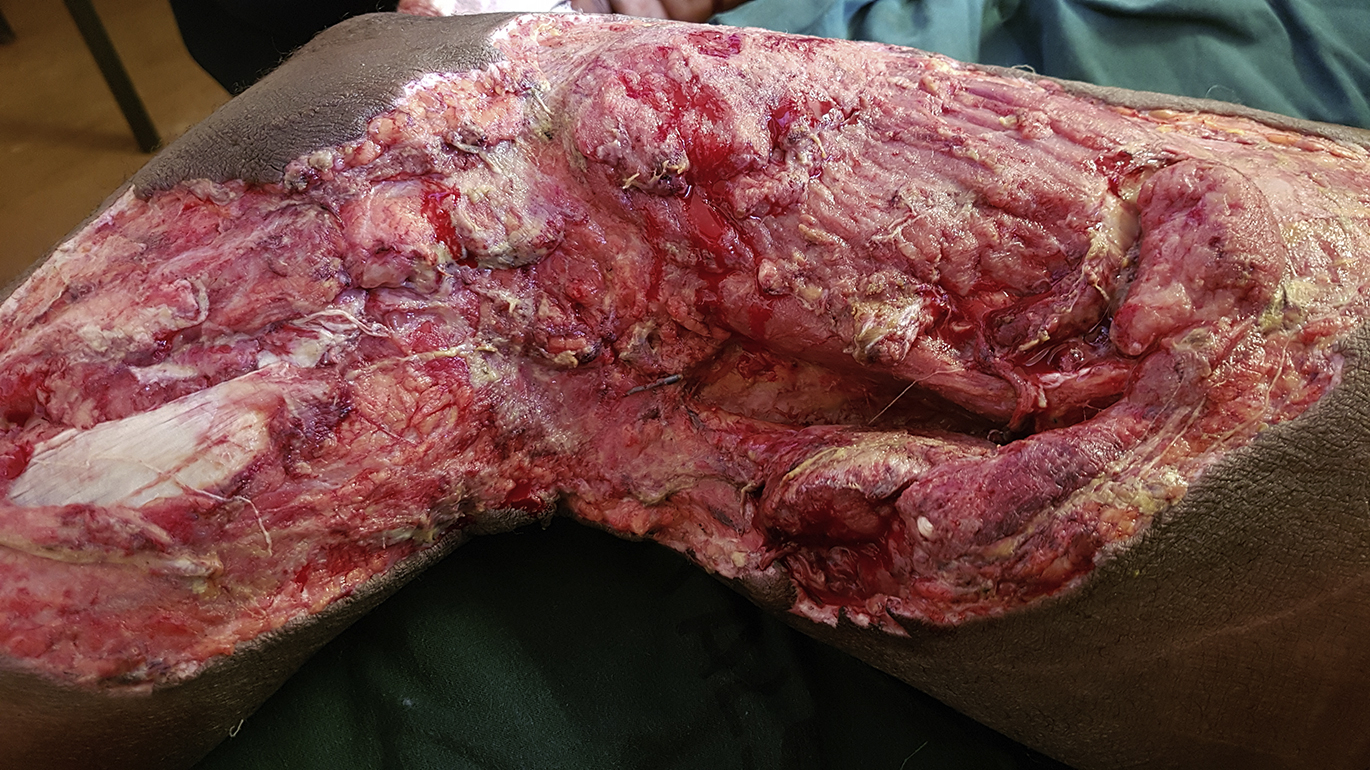
Appearance of the wound on the third day of admission. The wound remains clean after serial debridements and cleaning facilitated by regional anesthesia.
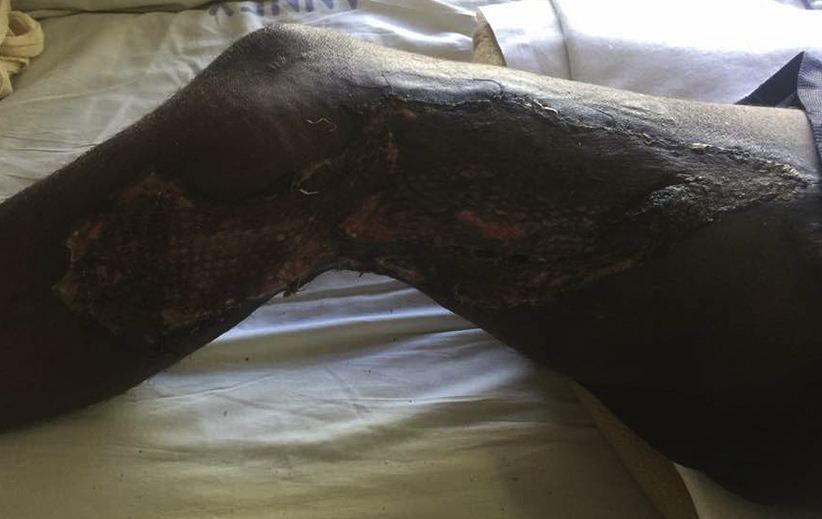
Appearance of the wound after skin graft. The aesthetic and functional outcome is good after successful management of the bite wound.
Discussion
Common in popular culture, crocodiles are admired for their predatory prowess. Attacks frequently involve stealth with a lunge and bite from under the water, 15 followed by the death roll, a maneuver intended to dismember the victim. 15 The ferocity of this initial phase means that people who survive attacks may sustain major injuries with tissue loss, fractures, and exsanguination. Injury mechanisms include penetrating injury from long, sharp teeth and blunt injury from powerful pterygoid muscles. 3 The anatomic distribution of wounds favors the extremities, which is consistent with an attack behavior that involves striking from below or the side. In a large series from Australia, 88% of injuries were sustained on limbs (upper and lower). 3 Additionally, the clinical condition may frequently be complicated by drowning. 16
Because attacks occur in remote areas, the importance of the first responders and their prehospital care cannot be overemphasized. This initial management phase can have a significant impact on whether victims arrive safely at the hospital. Early, adequate debridement and copious irrigation is the most important aspect of definitive treatment to avert infection by the unusual organisms that may be present in crocodile bite wounds.4,17 Good debridement is facilitated by robust analgesia, which is usually achieved under general anesthetic in the operating room. However, regional anesthesia is a quick, safe method to achieve analgesia. In our case the patient presented after an almost 24 h delay, and therefore prompt debridement was of the essence. There are limited reports of the use of regional anesthesia techniques in the management of animal bite injuries, particularly crocodile bites. In Australia, researchers found that continuous infraclavicular block of the forearm reduced opioid requirements after a Crocodylus porosus bite and was a useful technique even with limited experience with the techniques. 18 In our case regional blocks facilitated serial redebridement and irrigation, which contributed to averting the overwhelming soft tissue infection that is so common in these bite wounds. 4 This also reduced usage of operating room resources and may have helped decrease duration of stay and admission costs.
The use of peripheral nerve blockade in trauma patients is a relatively new but rapidly expanding application that has been spurred by the experience in military trauma situations. 19 Advantages of peripheral nerve blocks include hemodynamic neutrality, versatility in the emergency department and ward, and more rapid, complete analgesia. A 2003 randomized control trial demonstrated that femoral block provided more rapid reduction in pain scores than systemic opioids in patients with femur fracture. 20 There is also a risk of undertreatment of pain in trauma patients using systemic agents because of fear of adverse events, particularly from opioids. 21 The early concerns of the dangers of masking acute compartment syndrome and exacerbating neural injury (double crush syndrome) have been assuaged with newer data. 22 A consideration that has not been investigated in the setting of animal bite injuries is the risk of infection at the injection site. Selection of a site distant from the wound is an obvious remedy, but there is presumably an increased risk of infection on that site in a trauma patient, particularly when there is a breach in the integument. A reluctance to perform regional anesthesia because of the risk of infection has been noted, 23 but those fears appear to be unfounded with the meticulous use of appropriate periprocedural precautions.23,24 The American Society of Anesthesiologists recently offered updated guidance on these precautions for prevention of infection. 25 There are no specific recommendations for animal bites per se, but universal precautions are applied that reduce the risk of infectious complications of neuraxial techniques. 25 We did not experience any injection site infections in our case.
Infections from aquatic animal bite wounds run the gamut from subclinical colonization of bacteria to life-threatening necrotizing fasciitis due to often fastidious organisms. 26 Crocodile bite wounds are also characterized by large amounts of tissue loss and crushing. Comminuted fractures and dismemberment may be anticipated, as well as neurovascular injury. There is currently no structured way to describe and grade crocodile bite injuries that predicts outcome. The Lentz shark-induced trauma scale 27 and the Durban classification system developed for shark bite injuries predict mortality and are intriguing approaches. 28 Vascular injury is a crucial determining factor. A useful system should predict mortality and permanent functional disability while being appropriate for practical use by practitioners in the field. Additional research needs to be done in this regard. Future prospective studies are also required to determine whether regional anesthesia has benefits in terms of functional outcomes and reduction of opioid needs.
Conclusions
Regional anesthesia techniques are useful adjuncts to management of patients with extremity injuries from crocodile attacks. They allow for prompt initial management even when theatre resources are constrained and facilitate early mobilization and continued care as well as reducing the need for opioid analgesia.
Footnotes
Acknowledgments
The authors thank Tanya Salome.
Author Contributions
Study concept and design (DM, CM, GIM, STC); acquisition and analysis of the data; (DM, CM, GIM, STC); drafting of the manuscript (DM, CM); critical revision and approval of final manuscript (DM, CM).
Financial/Material Support: None.
Disclosures
None.
