Abstract
Injuries caused by wild boar attacks are rare. A 34-year-old male shepherd sustained injuries caused by a wild boar attack, and was brought to our emergency department. The patient had 2 skin and deep tissue lacerations on the posterior aspect of his thigh. Herein, we discuss the clinical management of a wild boar bite wound with a review of the literature.
Introduction
Wild boar is a common name for various species of the pig of the genus Sus, part of the biological family Suidae. It is one of the most numerous and widespread large mammals in the world. They are native across Europe, Northern Africa, the Middle East, and Asia. 1 There are several subspecies in different geographical regions. Sus scrofa lybica inhabits Turkey. Although the wild boar is not native to North America, the size and range of the feral swine population has expanded over the centuries after its artificial introduction to the continent in the 14th century. Now, over 4 million feral pigs in the United States pose a growing problem for agriculture and stock-raising. 2
Typical wild boar habitat is generally dense forests, brushwood, and wild grassland. 3 The physical appearance of a wild boar is similar to a domestic pig. Average weight and length of a wild boar is 50 to 90 kg and 120 to 180 cm, respectively. After 2 years of age, male wild boars grow tusks from both the upper and lower canines that curve upwards (Figure 1). The lower tusks are extremely sharp and usually measure 6 cm in length. These tusks serve as weapons during fighting. Domestic male pigs also have tusks; however, tusks are regularly trimmed when the pigs are kept as livestock.
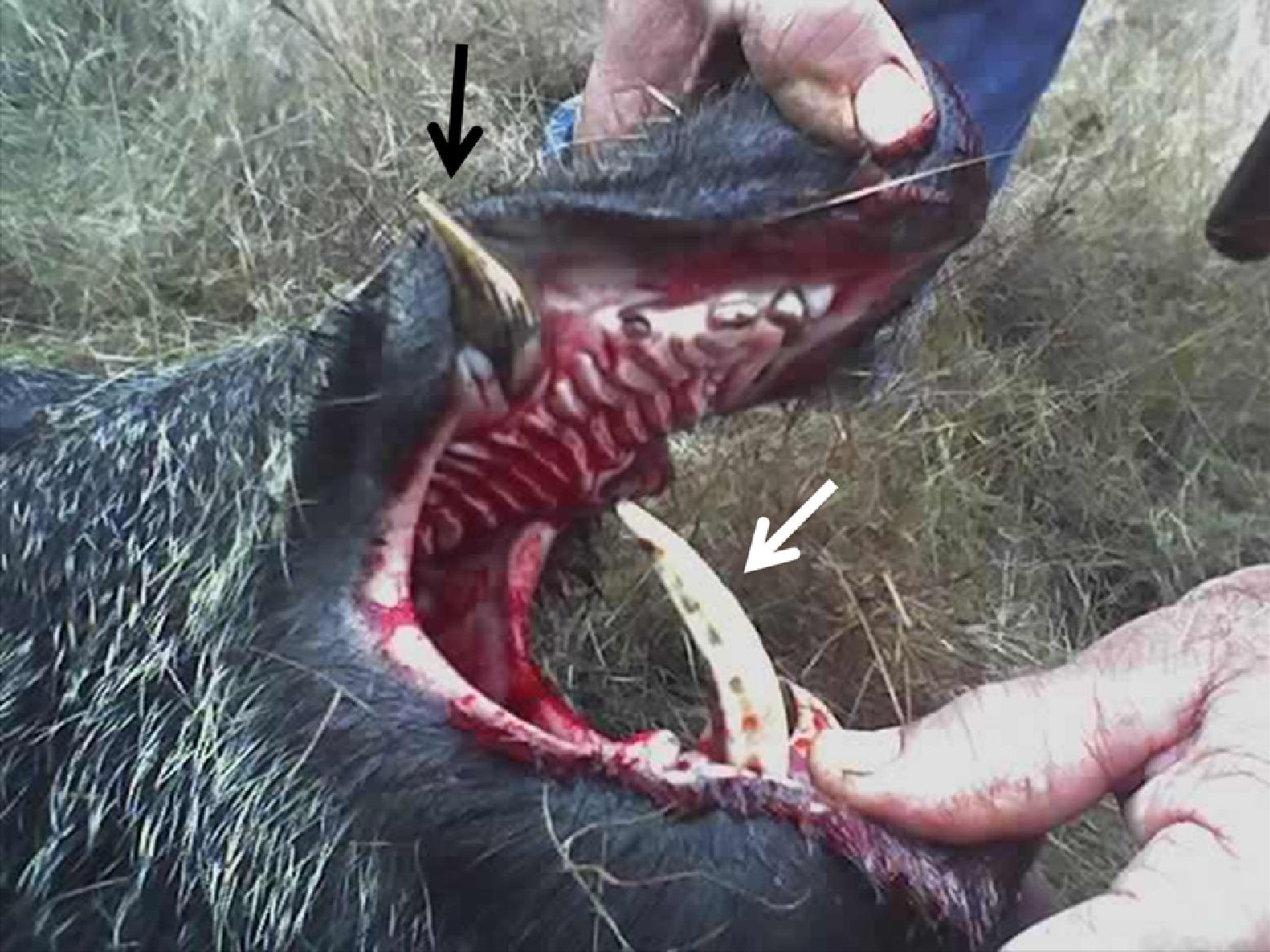
Tusks of a wild boar. The upper tusks (black arrow) act as a permanent whetstone against which the lower tusks (white arrow) produce sharp edges.
Wild boars are primarily nocturnal animals and are naturally shy; therefore, confrontation between wild boars and humans is very rare. In general, wild boars flee when they see human beings. 3 However, spread of human habitation into suburban areas, increased use of lands for agricultural purposes, deforestation, and rising hunting activities have increased the interactions between wild boars and humans. Furthermore, extinction of their natural enemies, the boars' high multiplication ability, and their adaptability to the environment have led to an increase in the wild boar population. 4 It is extremely rare for a boar to be aggressive towards humans, 3 but they are potentially dangerous animals due to their razor-sharp tusks and may cause serious injuries if aggression does occur. Wild boars are known to be more aggressive during mating season and when cornered. 5
Wild boar attacks are underreported in medical literature. To the best of our knowledge, there are only 3 case reports about wild boar attacks against humans in relevant medical literature. 5 –7 Herein, we present a case of a wild boar attack that resulted in bite injuries, and we discuss its medical management.
Case Report
A 34-year-old man was brought to our emergency department following a wild boar attack. A goat shepherd, he lived in a village surrounded by woodlands and shrublands, at an approximate altitude of 1000 m. He sustained the attack on February 5, 2011 at 10:30
On physical examination, the patient had 2 skin and subcutaneous tissue lacerations on the posterior aspect of the left thigh. One lesion was a simple skin and subcutaneous laceration that was 3 cm long, and the other was a deep penetration which was 8 cm long and 2 cm wide, extending down to the muscular fascia with resulting rupture of the biceps femoris muscle (Figure 2). Neurovascular examination was normal. The wound was irrigated with 1000 cc saline and iodine solution, and 5 nonabsorbable sutures were used to close the wound. As the patient was fully immunized in the past but had not received a booster for over 5 years, 0.5 ml of tetanus toxoid was administered. Rabies vaccine (HDVC, 4 mL) was also administered intramuscularly to the deltoid area, and a 4-vaccine regimen (0, 3, 7, and 14th days) was scheduled. Human rabies immune globulin (HRIG) (20 IU/kg body weight) was infiltrated into and around the wound using approximately four-fifths of the dose, and the remaining one-fifth dose was injected intramuscularly to the contralateral gluteal area. The patient was hospitalized and given 1 g amoxicillin plus 200 mg clavulanic acid (Augmentin 1.2 IU) IV, 3 times daily for 5 days. There were no complications and the wound healed without infection. Sutures were removed on the 10th day. At the final follow-up, 2 months after the attack, the patient had returned to his previous level of activity without any complication.
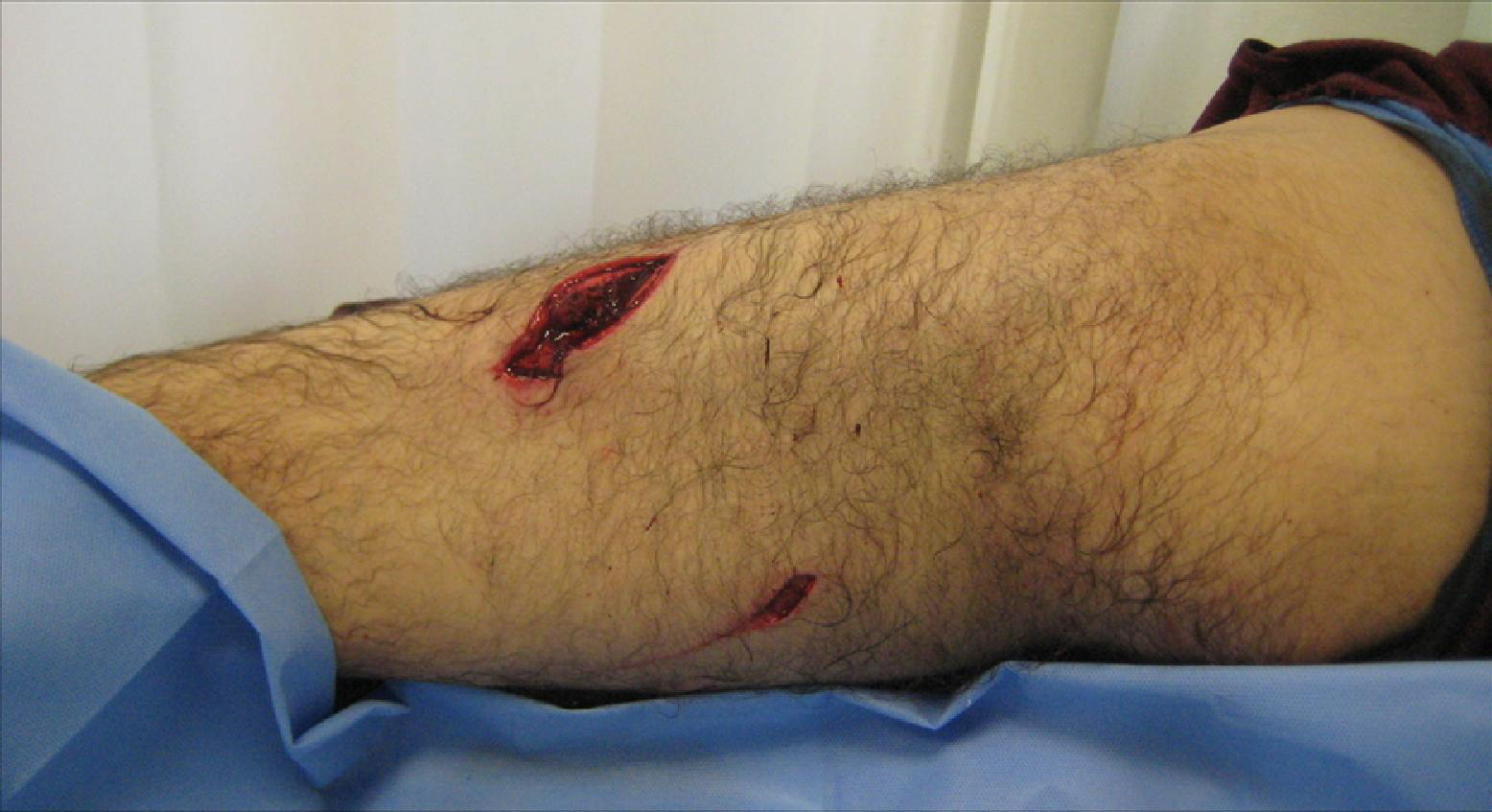
The photograph of the victim's thigh showing the lesions.
Discussion
Management of an animal bite wound should start with proper local care of the wound. The wounds should be washed vigorously and irrigated with saline solution to reduce the high inocula of the oral flora of the biting animal. Devitalized tissues should be debrided and, in cases presenting with deep injuries, the wound should be explored for possible nerve, tendon, joint, and blood vessel damage. 8
Surgical closure of animal-bite wounds is controversial and an evidence-based approach is currently lacking. Only one prospective controlled study has been performed to directly investigate infection rates in dog-bite wounds treated by primary closure compared with nonclosure. It was concluded that dog-bite wounds can be safely sutured at presentation. 9 However, this study excluded puncture wounds, wounds infected at presentation, wounds with other structures involved, and those with tissue defects requiring plastic surgery. In another cohort study concerning mammalian bites, the rate of wound infection for sutured bite wounds was 6% compared to 3.4% in sutured nonbite wounds. They concluded that mammalian bite wounds can be sutured with an approximately 6% rate of wound infection, which is acceptable for lacerations where cosmesis is the primary concern. 10 However, suturing is not recommended in wounds at high risk of infection.11,12 Some factors, related to wound properties and patient characteristics, place wounds at a high risk of infection (Table 1). The margins of certain wounds should be excised and left open after irrigation, and delayed primary closure or edge approximation should be performed. 8 Therefore, a decision to close the wound should be made on a case-by-case basis. In our patient, we closed the wound because there were no risk factors for infection, and the wound had involved muscle, which has adequate blood supply.
Factors that increase the risk of infection
A tetanus toxoid booster should be administered if the patient has previously been adequately immunized and has not received the most recent dose within the past 5 years. Tetanus immune globulin is required if tetanus immunization has not taken place or is inadequate. 8 Though there is no documentation that the wild boar population carries rabies infections, there is a theoretical risk of rabies in wild boar bites; therefore, we administered both human rabies immune globulin and active immunization (4-dose regimen) to our patient. Previously, the Advisory Committee on Immunization Practices recommended a 5-dose rabies vaccination regimen with HDCV; recently, however, the number of vaccine doses has been reduced to 4 for post-exposure prophylaxis to prevent human rabies. 13
The use of routine prophylactic antimicrobial therapy after mammalian bite wounds is controversial 14 ; prophylaxis is advised, however, when primary closure is performed. 12 The organisms that can be isolated from bite wounds generally represent the oral cavity of the biting animal and the victim's skin flora. Animal bite infections should be considered to be polymicrobial, but certain pathogens can be characteristic of particular animal species. 11 There is lack of knowledge about oral flora of wild boars in the current literature. However, the organisms recovered from domestic pig bite infections are Staphylococcus species pluralis (spp), Streptococcus spp (including Streptococcus sanguis, Streptococcus suis, and Streptococcus milleri), diphtheroids, Pasteurella multocida, other Pasteurella spp, Mycoplasma, Haemophilus influenzae, Actinobacillus suis, Flavobacterium IIb-like organisms, Bacteroides fragilis, and other anaerobic gram-negative bacilli. 15 –18 Amoxicillin plus clavulanate is the recommended antibiotic which covers most pathogens delivered by domestic pig bites. 16 One study recommends additional ciprofloxacin to cover newly isolated microorganisms that are resistant to amoxicillin plus clavulanate such as flavobacterium species group IIb and mycoplasmas. 17 We administered amoxicillin plus clavulanate to our patient immediately on the day of admission and no subsequent infection occurred.
Furthermore, wild boars harbor many important zoonotic infectious agents that are transmissible to humans who may come in contact with the boars' discharges or who consume infected meat. The lists of zoonotic infectious agents are presented in Table 2. Hunters who handle infected tissues of wild boar, veterinarians, and farmers who work on hog farms are at increased risk for these infections. 4
List of infectious agents that wild boars may harbor
According to the literature, the most common site of injury among reported cases of wild boar and domestic pig bites was the posterior thigh (Table 3). However, wild boar wounds can be fatal. There are 2 reported cases of deaths due to wild boar attacks,6,7 with the cause of death being craniocerebral injury and multiple abdominal penetrating injuries. In these fatal cases, lesions were also found on the posterior thigh. Similarly in our case, there were 2 lesions on the posterior aspect of the thigh. The authors of previously reported cases proposed explanations for this specific location of wounds. Gunduz et al related this pattern to the physical characteristics of the wild boar. 5 This seems logical, as the shoulder height of an adult wild boar is 90 cm on average, which approximately corresponds to the height of the thigh. However, multiple lesions and lesions other than the posterior thigh are thought to occur after the victim falls to the ground with repeated attacks. 6 This pattern shows that a wild boar has a typical offensive tactic. Initially, it attacks from behind—perhaps while the victim is trying to escape from the assault—and the victim may fall to the ground during this initial attack. As the boar continues its assault while the victim is on the ground, secondary lesions can occur in any anatomic location depending on the relative position of the victim.
Site of injury in reported cases of wild boar and domestic pig bites
In conclusion, a wild boar bite is a rarely seen case in emergency departments. However, there seems to be a rise in the number of these kinds of injuries because of the increase in wild boar populations and because the wild boars' natural habitat is increasingly occupied by humans. 3 Proper wound care, tetanus immunization, rabies prevention, and appropriate antibiotics should be administered to the survivors of wild boar attacks.
