Abstract
The case of a 35-year-old man presenting microscopic hematuria allows the following topics to be examined in depth:
How is hematuria defined and classified? What are the causes of hematuria? Hematuria is an important sign for the diagnosis of cancer of the urinary system. What are the risk factors for bladder carcinoma? What is the role of the urinary dipstick test in the diagnosis of hematuria? What is the role of the examination of urine sediment in the diagnosis of hematuria? Once microscopic hematuria is confirmed, how can we proceed to reach a final diagnosis?
Study case
A 35-year-old man presented to the nephrology clinic for evaluation of microhematuria. After a positive dipstick test for blood in the urine, his family physician required an automated urine test, confirming the presence of 30 red blood cells (RBCs) per microscopic field.
Family history was remarkable for the presence of kidney disease, including dialysis, on the maternal side. The physical examination was normal, with the exception of moderate high-tone sensorineural hearing loss. A microscopic evaluation of the urinary sediment demonstrated the presence of dysmorphic RBCs.
How should the finding of hematuria be addressed in this patient?
How is Hematuria Defined and Classified?
Hematuria is the presence of RBCs (erythrocytes) in the urine. Hematuria can be broadly divided in two categories:
Macroscopic hematuria (i.e., grossly visible). This is considered as little as 1 mL of blood per liter of urine, which can induce a visible color change (1). It can be accompanied by the passage of blood clots, which usually indicate an origin from the lower urinary tract or from renal tumors in which massive blood loss accumulates in the bladder.
Microscopic hematuria (i.e., detectable only on urine examination). Clinically significant microscopic hematuria is defined as 3 or more RBCs per high power field (400×), corresponding to 10-12 erythrocytes per microliter to automated analyzers (2), confirmed in 2 urinalysis test performed when there is no benign etiology, such as menstruation, recent exercise, recent sexual activity, or recent instrumentation of the urinary tract (3).
The incidence of hematuria is about 10%, representing a clinical finding commonly encountered by primary care physicians (3). As a general principle, hematuria itself does not cause direct harm, with the exception of bleeding with clots blocking the ureter and causing obstructive acute kidney injury, or bleeding with clots blocking the urethra and causing acute urinary retention. Transient hematuria is common and almost always benign in young patients, and a cause is often not identified. An important exception to the typically benign nature of transient hematuria occurs in patients over the age of 40 in whom even transient hematuria carries an increased risk of malignancy (assuming there is no evidence of glomerular bleeding) (1).
Based on other characteristics, hematuria can also be classified as:
transient or persistent (confirmed in 3 consecutive samples of urine for more than 3 months);
isolated or associated (e.g. with proteinuria and/or loss of renal function)
Asymptomatic or symptomatic (hypertension, impairment of diuresis, signs of systemic disease)
We can find transient hematuria (micro or macro) in athletes and people who practice intense physical activity, after physical exercise. It is an isolated hematuria, but it also can be associated with proteinuria; although it probably reflects renal damage, it cannot be considered a sign of disease.
What are the Causes of Hematuria?
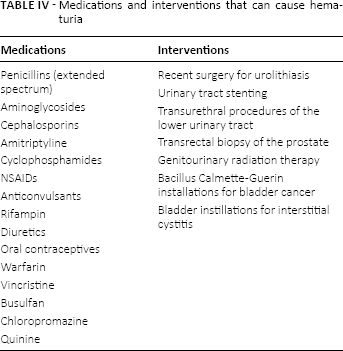
Microhematuria can be of nonglomerular (Tab. I), glomerular (Tab. II), or uncertain origin (Tab. III) (4). The etiologies of microscopic hematuria are numerous and range from clinically insignificant causes to potentially life-threatening neoplastic lesions. A consistent number of medications and medical interventions have also been associated with microhematuria (Tab. IV) (3, 5).
Non-glomerular causes of microscopic hematuria

Glomerular causes of microscopic hematuria

Causes of uncertain origin

Medications and interventions that can cause hematuria
The identification of the glomeruli as the source of bleeding is important both prognostically and to optimize the subsequent evaluation for reaching the correct diagnosis. Findings in support of glomerular etiology include red cell casts, protein excretion exceeding 500 mg/day at a time when there is no gross bleeding, a dysmorphic appearance of some red cells (particularly acanthocytes), and brown, cola-colored urine (with gross hematuria). Thus, proteinuria (2+ or greater on the dipstick) is an important indicator of glomerular disease (6).
An additional important abnormality is the presence of blood clots, which virtually never occur in glomerular disease (1), perhaps due to the presence of urokinase and tissue-type plasminogen activators in the glomeruli and the renal tubules.
The most common nonglomerular causes of significant hematuria (Tab. I) are:
Urinary tract infections (e.g. cystitis or prostatitis): These usually appear with voiding symptoms, especially dysuria and acute urinary frequency.
Urolithiasis: These smaller stones in the kidney are usually asymptomatic and microhematuria may be the only finding. Larger stones, including Staghorn calculi (that may be associated with urinary tract infection caused by urease-producing pathogens), may present with gross hematuria. Stones moving into the ureters are typically associated with hematuria and lateralizing, colic flank pain.
Malignancies: These micro-hematuria are more common with renal cell carcinomas, whereas gross hematuria tends to be the most common symptom with urothelial carcinomas. Typically, prostate cancer causes hematuria only in the more advanced stages (along with hesitancy, a weak stream of urine, straining to urinate, chronic urinary retention, overflow, or paradoxical incontinence).
Benign prostatic hyperplasia (BPH): This may be the most common cause of micro-hematuria in men (3).
Patients with glomerular causes (Tab. II) may be asymptomatic or may present with nephritic syndrome, which is characterized by hypertension, edema, and renal insufficiency (3).
In patients with glomerular diseases, the presence and the kind of casts at urinary microscopy is very helpful in the differential diagnosis, as outlined below.
When persistent hematuria is essentially the only manifestation of glomerular disease, one of four disorders is most likely:
Thin basement membrane nephropathy: This inherited glomerular disorder is defined histologically by diffuse thinning of the glomerular basement membranes. Immunoglobulin A (IgA) nephropathy (Berger's disease): This is defined histologically by glomerular IgA deposits, and may be associated with both micro- and macrohematuria. Non-IgA mesangioproliferative glomerulonephritis: In a cohort of 57 patients, hematuria was present in about 40% (macroscopic 16%, microscopic 23%). Patients with macroscopic hematuria also had nephrotic range proteinuria (7). Alport syndrome: This is an inherited disease (often X-linked) that results in renal failure, deafness, and ocular abnormalities. Mutations affect the gene encoding chains of type IV collagen, the major protein found in the glomerular basement membrane (8).
Rare causes of hematuria include:
Arteriovenous malformations and fistulas (AVM). These can be either congenital or acquired. The primary presenting sign is gross hematuria, but high-output heart failure and hypertension also may be seen (presumably due to activation of the renin–angiotensin–aldosterone system resulting from ischemia distal to the AVM). Nutcracker syndrome. This refers to compression of the left renal vein between the aorta and proximal superior mesenteric artery, and can cause both microscopic and gross hematuria. The hematuria is usually asymptomatic but may be associated with left flank pain. Loin pain hematuria syndrome. This is a disorder characterized by loin or flank pain (often severe) and hematuria with dysmorphic erythrocytes, suggesting a glomerular origin (1).
There are often clues from the patient's history pointing toward a specific diagnosis, such as concurrent pyuria and dysuria (urinary tract infections or bladder malignancy), recent upper respiratory infection (post-infectious glomerulonephritis or IgA nephropathy), positive family history of renal disease (polycystic kidneys), or cyclic hematuria in women during menstruation (endometriosis of the urinary tract) (1).
If gross hematuria appears throughout the urinary stream, then it probably originates above the level of the bladder outlet, including the upper urinary tract and kidneys. If blood is detected only at the initiation of urination, then it is likely from the urethra. Gross hematuria at the end of urination may be from the prostate or bladder neck (3).
The frequency of presentation of the disorders causing hematuria modifies with age, especially after the fourth decade; in these patients, microhematuria from neoplastic cause is much more likely. Renal cell carcinoma is second, and renal pelvis or ureteral transitional-cell carcinoma is fifth, among the most frequent causes of hematuria originating from the upper urinary tract.
With regard to hematuria from the lower urinary tract, bladder carcinoma is the second cause, and prostate carcinoma the third cause; whereas the frequency of benign lesions (e.g., benign bladder and ureteral polyps and tumors) is relatively reduced.
Hematuria is an Important Sign for the Diagnosis of Cancer of the Urinary System. What are the Risk Factors for Bladder Carcinoma?
Most cases of urologic microhematuria are due to benign prostatic hypertrophy, urinary calculi, and infections. Although rarer, microhematuria signals urinary tract malignancy in a clinically relevant number of patients (9). Hematuria may be present years before bladder cancer is diagnosed. Therefore, once discovered, microhematuria should be promptly investigated by the physician (10).
As previously outlined, it should be kept in mind that isolated hematuria is rather common, being present in about 10%-13% of the population (11).
Hematuria associated with significant urologic diseases can be intermittent (12); therefore, the first appearance of asymptomatic microhematuria should be investigated through urinary sediment analysis. However, the cytological analysis of urine may produce false negative results and is affected by many factors, including the number of urine samples examined and the stage of the cancer.
Cystoscopy is another crucial tool to investigate microhematuria, since it explores the bladder mucosa entirely, as well as the urethra and ureteral orifices. The cystoscopy exam should be performed on all adults over 35 years affected by microhematuria, and on all patients who present risk factors for the development of bladder cancer (Tab. V). A 2-tiered screening, in which a repetitive hematuria test is followed by cystoscopy, may help to discover lesions in the early stages when they are not invasive yet. The patient should repeat the urine analysis at least once every 12 months for 2 years. If the analysis is found negative at each control, the patient may be released from care, but if changes in the clinical scenario appear (e.g., an increase in the microhematuria, the appearance of proteinuria or dysmorphic RBCs, the development of gross hematuria, pain, hypertension) there should be a re-evaluation of the case (9).
Common risk factors for urinary tract malignancy in patients with microhematuria

Many urine markers have also been proposed for bladder cancer diagnosis and surveillance; however, none of them have proved sensitive and specific enough to replace cystoscopy. The combination of multiple urinary biomarkers with cytology has shown interesting results (13), but, overall, the available evidence is insufficient to warrant the substitution of the cystoscopic follow-up scheme with any of the currently available urine marker tests (14).
What is the Role of the Urinary Dipstick Test in the Diagnosis of Hematuria?
The simplest, most common and less expensive way to detect hematuria is the urinary dipstick test (UDT). This test is based on the detection of hemoglobin, either free in the urine or bonded to urinary RBCs, through a chemical reaction between hydrogen peroxide and a chromogen (15).
How to Perform the Test
To do a UDT, the patient is required to provide a fresh, midstream urine sample. To avoid flawed results, the urine sample should not be stored at room temperature for more than 2 hours. Furthermore, the dipsticks should be stored at the correct temperature and not have expired. When performing the test, the dipstick should be quickly and completely immerged into the urine sample, then it should be tapped on its edge with the purpose of eliminating excess urine and the reduction of the mixture of reagents from different test pads. After that, if hematuria is detected, the dipstick will show a positive color reaction, with the degree of color change reflecting the amount of hemoglobin in the specimen (3).
Efficiency for Diagnosis
The UDT is very useful to establish the presence of hematuria in the primary care setting. In fact, its sensitivity is 91%-100%, but there are many false positive results because of its lower specificity, ranging from 65%-99% for 2 and for 5 RBCs per higher power microscopic field (HPF), respectively (15). Moreover, UDT is considered an unreliable method, acceptable in the sole contest of level-one diagnostics, because of its inadequate standardization and the low expertise of operators that can perform it. In fact, UDT can be made directly by patients at home (auto-diagnosis) or by health operators without specific competence in the laboratory field (2).
We have to consider the large number of false positive results, which are caused by (1):
For this reason, the most recent American Urological Association Guidelines for the evaluation of asymptomatic microscopic hematuria in adults suggest that, after a positive UDT, microscopic examination of the specimen is needed to confirm the diagnosis of hematuria (9).
A positive dipstick test with a negative microscopic urinalysis can be identified as “dipstick pseudohematuria,” which is considered an insignificant clinical finding (19). Symptom-free patients with “dipstick hematuria” without microscopic hematuria do not need further nephrologic or urologic evaluation.
False negative results may be due to a high concentration of ascorbic acid (20), a urinary pH of <5.1, or prolonged exposure of the dipstick to air (16). However, false negatives are very rare, and a negative dipstick can rule out abnormal hematuria (17).
To allow proper use of the UDT when it is performed, there are some recommendations that must be taken into account:
The automatized interpretation of UDT is strongly recommended to eliminate the subjectivity linked to the evaluation of chromatic change. UDT is not recommended in hospitals in which a 24-hour laboratory is available. The analytical valence of UDT must be only used as a support of clinical suspicion, requiring further investigation when results are discordant. The presence of tables including all the interferences that could lead to flawed results is recommended to eliminate analytical uncertainty in data evaluation. The storage of results is recommended to permit revaluation in the light of any change in the patient's clinical status and the longitudinal evaluation of data (2).
For urinary tract cancer, there is controversy on the evaluation of asymptomatic microscopic hematuria as a marker of occult cancer (21).
Early studies (22, 23), in which a cohort of asymptomatic men was screened for microhematuria using UDT at home for long periods, concluded that a hematuria home-screening regimen, followed by a complete urologic evaluation, was feasible and economical, promoting the early detection of urinary tract cancers and other diseases in men more than 50 years old. However, further evaluation of this approach raised concerns on the low positive predictive value (PPV) of hematuria screening, due to the large variety of benign urologic conditions associated with microhematuria, making the costs of screening unaffordable. Indeed, in an asymptomatic population screened for microhematuria the incidence of bladder cancer was similar between patients with positive and negative UDT, confirming the low PPV, and, therefore, the lack of recommendation to screen asymptomatic adults (24). To overcome this problem, hematuria screening using UDT in combination with an available molecular marker test could reduce the number of false positive tests and increase the cost effectiveness and public acceptance (25).
Currently, routine testing for hematuria to screen for bladder cancer in asymptomatic patients is discouraged (19, 21).
The American College of Physicians (21), after reviewing the available guidelines and best practice policy recommendations, also suggested additional “high value care advice” regarding hematuria:
Include gross hematuria in the routine review of systems and specifically ask all patients with microscopic hematuria about any history of gross hematuria. Confirm positive results of dipstick testing with microscopic urinalysis that demonstrates 3 or more erythrocytes per high-powered field before initiating further evaluation in all asymptomatic adults. Refer for further urologic evaluation in all adults with gross hematuria, even if self-limited. Consider urology referral for cystoscopy and imaging in adults with microscopically confirmed hematuria in the absence of some demonstrable benign cause. Pursue evaluation of hematuria even if the patient is receiving antiplatelet or anticoagulant therapy. Avoid obtaining urinary cytology or other urine-based molecular markers for bladder cancer detection in the initial evaluation of hematuria.
Concerning the role of UDT in the evaluation of patients with suspected renal colic at the emergency department, it is useful to detect hematuria because of its high level of accuracy (sensitivity 92.5% in patients with ureteral stones and 60% in those with renal stones) (26).
In conclusion, the UDT is a useful first-line test for detecting hematuria that can be easily performed at point of care, but it needs further diagnostic studies. It should be used in symptomatic patients, because screening in asymptomatic patients has not been proved to be cost effective. Possible harm of the evaluation of hematuria as a marker of occult urinary tract cancer include complications related to cystoscopy (pain or infection), radiation exposure (for computed tomography [CT]), hypersensitivity reactions and contrast nephropathy (for iodinated contrast with CT), and potential association with subsequent unnecessary, invasive, and expensive procedures (21).
What is the Role of the Examination of Urine Sediment in the Diagnosis of Hematuria?
The exam of urine sediment is considered the gold standard for the diagnosis of microscopic hematuria (27-28-29). In addition to manual urinary microscopy, automated instruments, based on either flow cytometry or digitized microscopy, are currently in use in clinical laboratories. Automated urinary microscopy allows the examination of large numbers of samples over a limited time, and is considered reproducible, accurate, and more economic than manual microscopy because of labor cost savings.
How to Perform Manual Urinary Microscopy
The analysis should be done on a first-morning midstream urine specimen, obtained with a clean-catch technique (30). Although prior cleansing of the external genitalia often is recommended in women, it has no proven benefit. The urine sample should be analyzed shortly after collection (1 hour maximum), otherwise the specimen must be refrigerated to prevent pH alteration, osmotic lysis of RBCs, and overgrowth of bacteria. The specimen should be prepared with a standard technique: 10 mL from the specimen has to be centrifuged in 15 mL tubes at 2,000 rpm for 10 minutes (or, alternatively [16], 5 mL from the specimen at 3,000 rpm for 5 minutes). Then, the supernatant should be discarded and the sediment should be suspended again in 0.3 mL of supernatant or saline. The specimen then should be placed on a microscopic slide and covered with a cover slip.
Positivity for microhematuria is defined by the finding of 3 or more RBCs/HPF, according to American Urologic Association Guidelines (9). For an accurate evaluation with manual microscopy, a phase-contrast microscope is recommended to make it possible to discriminate between the glomerular or nonglomerular origin of the bleeding through the morphology of the RBCs (16). As alternatives to manual urinary microscopy, there are 2 types of machines for counting urine particles, using either flow cytometry with fluorescent dyes or software analysis for digitized microscopic images (29). Laser-based flow cytometry has been shown to be useful in screening for pyuria, bacteriuria, and hematuria, reducing the need for microscopy or culture (31). However, this produces scattergrams rather than images, and microscopy is still required to differentiate similar particles, such as dysmorphic and isomorphic RBCs. Interestingly, with digitized instruments, the actual images of the urinary sediment can be reviewed by the pathologist or nephrologist, if needed, for a closer evaluation of the individual patient sample (32). In addition, images are digitally stored and they can be sent to other sites for review (29). Regardless of the employed method, microscopy sediment evaluation remains the gold standard analysis to confirm the dipstick's diagnosis of microhematuria.
False positive cases may occur in menstruating and postpartum women, patients who performed physical exercise (it is recommended to wait at least 48 hours to collect the urine specimen), and patients with urinary catheterization. False negative cases are uncommon, but they can occur if the analysis starts more than 1 hour after urine collection, or if an osmotic lysis of RBCs occurs in much diluted urine.
Efficiency for Diagnosis
In order to confirm the diagnosis of suspected microscopic hematuria from a positive dipstick, not only the presence or absence of RBCs has to be investigated, but also the association of hematuria and other patterns of the urinary sediment (1). Observing the morphology of RBCs, analysis of the urine sediment is useful to distinguish glomerular or nonglomerular bleeding (Fig. 1). A glomerular source of the bleeding is suggested by the presence of RBC casts, the dysmorphic aspect of some RBCs, and brown, cola-colored urine. Often, glomerular bleeding is also suggested by the onset of temporally related proteinuria exceeding 500 mg/day (1). In nonglomerular bleeding, RBCs are isomorphic (uniform, biconcave disk shape) and casts are absent. According to the American Urologic Association Best Practice Guidelines, the cut-off identified for glomerular bleeding is associated with at least 80% dysmorphic RBCs, and lower urinary tract bleeding is associated with at least 80% RBCs of normal morphology. Percentages falling between these values are indeterminate and could represent bleeding from either source (12). However, Fogazzi et al (33) suggested a cut-off of 40% dysmorphic erythrocytes for the diagnosis of hematuria of glomerular origin. Acanthocytes, ring-formed erythrocytes of variable size and shape characterized by several membrane protrusions, represent a characteristic form of dysmorphic erythrocytes, indicating hematuria of glomerular origin. They correlate strictly with glomerular disease if they represent >5% of excreted RBCs, showing a sensitivity of 52% and a specificity of 98% (34).
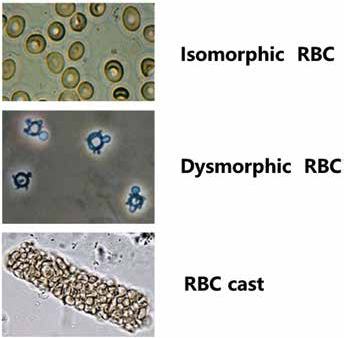
Representative images of isomorphic and dysmorphic red blood cells (RBC). An erythrocytes cast is also presented.
When a nonglomerular bleeding is confirmed, a urology referral is suggested; whereas a bleeding of glomerular origin requires a nephrologic consult. The optimal recognition of RBC morphology requires an inverted phase-contrast microscope, and this fact makes it difficult to utilize the cell's shape to identify the source of the bleeding in clinical practice at point of care. The subjective nature of identifying “dysmorphism” is another potential limitation. However, the development of digitized urine microscopy with remote access to the central laboratory could enable nephrologists to personally examine their patients’ urine in everyday office practice, and rekindle their interest in the urinary sediment (29). An alternative point of care development could be the availability of miniaturizing digital analyzers for personal use.
Considering the available techniques used to perform urine sediment analysis (conventional microscopy, contrast phase microscopy, and automated analyzer), sensitivity and specificity have wide ranges in detecting the glomerular causes of microhematuria: from 31.9% to 100% for sensitivity, and from 33.3% to 100% for specificity (9).
Microscopic urinalysis is also recommended to evaluate a flank pain or urinary symptoms, such as frequency, urgency, retention, and dysuria. In patients with renal colic, the UDT has a high sensitivity for the diagnosis of hematuria associated with nephrolithiasis, so it is not necessary to perform the urine sediment analysis if the UDT is positive. However, when the UDT is negative or doubtful, microscopic analysis is required (26).
Once Microscopic Hematuria is Confirmed, how we can Proceed to Reach a Final Diagnosis?
Figure 2 describes an algorithm for identifying the cause of microscopic hematuria. To evaluate the origins of the hematuria, the first investigation is the analysis of the urinary sediment, where it is possible to distinguish two main forms of RBC: isomorphic and dysmorphic. The former is normally present in urinary tract or extra-glomerular bleeding; the latter is typically found in glomerular disease (1, 4, 9). Another characteristic marker of glomerular bleeding is acanthocyturia. In addition, the examination of urinary sediment with the analysis of different casts, if present, is a crucial point in the diagnostic approach of patients with microhematuria, especially when it is associated with proteinuria. A thorough dissertation on urinary cast is out of the scope of this manuscript.
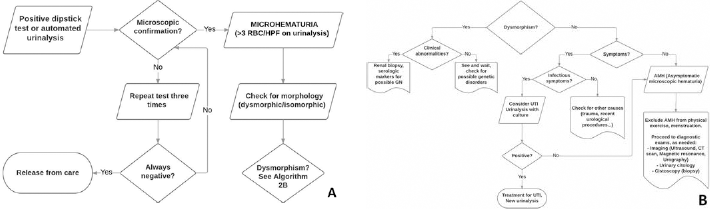
Diagnostic algorithm for microscopic hematuria. (
Diagnostic path for Probable Glomerular Disease
Once the glomerular origin of hematuria has been ascertained, it is necessary to consider the presence of symptoms or other abnormalities, such as proteinuria, oliguria, edema, hypertension, and a decrease in the glomerular filtration rate. If these elements are present, with a clincal picture ranging from oligo-symptomatic manifestations to the classic nephrotic or nephritic syndrome, further possible investigations are serological analyses and renal biopsy (3, 21, 35). In the case of isolated hematuria, the common practice instead is wait and see, especially in young patients, because benign causes of isolated and intermittent hematuria are particularly common.
As dysmorphic RBCs also may occur with nonglomerular causes of hematuria, a urological work-up can be considered (3).
Diagnostic path for Probable Urinary Tract or Extra-Glomerular Disease
If isomorphic RBCs are found, the diagnosis is generally linked to extra-glomerular causes. If the patient has symptoms of infection (e.g., fever, flank pain, or dysuria) with signs of inflammation (e.g., elevated C-reactive protein), then a urinalysis with culture should be undertaken to identify the pathogenic source. In the case of positive results, antibiotic therapy is suggested. After treatment, urinalysis should be repeated in order to evaluate the patient's health status. (3, 9). If the patient has abdominal pain suggesting a renal colic, it should be investigated for the presence of stones. To confirm the diagnosis, ultrasonography or a non-contrast-enhanced CT scan (sensibility 94%~98%) should be prescribed (12). If risk factors for malignancy are present, a screening cystoscopy and cytologic exam are suggested (21). In selected cases, the diagnostic hypothesis of malignancy could be further examined with a CT scan. Alternative examinations with lower sensibility and/or specificity are ultrasound and magnetic resonance imaging (3, 9, 12).
Conclusion
Based on the approach revealed in this article, microhematuria in this patient was considered of glomerular origin. Microhematuria associated with a positive family history and hearing loss led to the clinical diagnosis of Alport's syndrome. A renal biopsy and genetic tests were performed, which confirmed the clinical diagnosis.
Footnotes
Financial support: No grants or funding have been received for this study.
Conflicts of interest: None of the authors has financial interest related to this study to disclose.
