Abstract
Background
The aim of this study was to estimate the diagnostic accuracy of serum carcinoembryonic antigen (CEA) levels in conjunction with Ca125 in the triage of adnexal masses.
Methods
This retrospective cohort study was carried out in 495 patients referred to the Gynecology Department at Carmel Medical Center due to adnexal mass, between 2005 and 2012. All patients underwent surgery with histopathologically confirmed diagnosis and preoperative measurements of serum Ca125 and CEA. For each marker, sensitivity, specificity, positive predictive value, negative predictive value and risk ratio were calculated.
Results
Combination of CEA with Ca125, compared with Ca125 levels alone, yielded a nonsignificant effect on sensitivity (87.4% vs. 88.9%, respectively, p = 0.64) and specificity (79.3% vs. 74.3%, p = 0.18) in differentiating malignant from benign adnexal masses. CEA levels were higher in mucinous histological types, but were not helpful in detection of borderline tumors. Significantly higher CEA (21.4 ± 53.6 vs. 3.2 ± 11.9 ng/mL, p = 0.0002) and lower Ca125 values (103.9 ± 84.9 vs. 796 ± 1,331.5 U/mL, p = 0.0338) were demonstrated in the 17 metastatic cases compared with 181 primary ovarian malignancies.
Conclusions
The combination of the tumor markers CEA and Ca125 did not contribute significantly to the detection of malignant adnexal masses compared with Ca125 alone. As our results suggest that higher CEA levels could be useful in differentiating metastatic tumors from primary ovarian malignancy and in diagnosis of mucinous histology, this issue should be investigated in large, well-designed, prospective cohort trials.
Introduction
Adnexal mass is a common gynecological finding, demonstrated in up to 7.8% of premenopausal and 2.5% of postmenopausal women (1, 2). The main concern of the managing physician is to exclude malignancy, and several parameters are currently used to assess the preoperative risk of cancer, including patient's age, menopausal state, gynecological examination, ultrasonography and tumor markers.
Tumor marker Ca125, a monoclonal antibody that detects ovarian cancer antigen OC125, is used most extensively in evaluation of patients with adnexal masses, alone and in combination with other assays. According to a recent meta-analysis of 51 studies, Ca125 assay has an overall sensitivity of 78.7% and a specificity of 77.9% in ovarian cancer diagnosis (3). The suboptimal specificity is explained by elevated serum Ca125 levels in a variety of common benign conditions, including leiomyomas, pelvic inflammatory disease, endometriosis, pregnancy and even menstruation (4).
Given the imperfect performance of Ca125 in evaluation of adnexal mass, other serum markers have been evaluated alone and in combination with Ca125 by several investigators (5). Combining Ca125 with other markers has been shown to increase sensitivity by 5%-10%; however, specificity is decreased (5).
Carcinoembryonic antigen (CEA) is one of the longest known tumor antigens (6), and at present is still the most widely used tumor marker in the management of colorectal cancer (7, 8). Since elevated serum levels of this assay were demonstrated in patients with ovarian adenocarcinomas (9, 10), up to 87%-88% in mucinous histotypes (11, 12), several papers have suggested that concomitant measurement of Ca125 and CEA could aid in ovarian cancer diagnosis (13-15). Consequently, in some institutions, CEA has been incorporated as a tumor marker for evaluation of patients with adnexal masses. However, other studies have shown that CEA measurement has no clinical utility in the differentiation between benign and malignant adnexal masses (16-18). Moreover, its levels were shown to be elevated in several benign ovarian conditions (19), and even in nongynecological disorders such as rheumatoid arthritis (20).
None of the national guidelines, including those of the American College of Obstetricians and Gynecologists (ACOG), the Society of Gynecologic Oncologists (SGO) and the National Institute for Health and Care Excellence (NICE), have included CEA measurement as an adjunct in evaluation of patients with adnexal masses (21, 22). Nevertheless, in many institutions, this assay is still sparingly used as a preoperative tumor marker in the triage of a patient with an ovarian mass.
Thus, the objective of this study was to examine the value of CEA measurement as a preoperative tumor marker in the evaluation of a patient with an ovarian mass.
Methods
Data from all cases referred to the Gynecology Department at Carmel Medical Center because of adnexal mass between January 2005 and December 2012 were retrospectively obtained from a computerized database of hospital charts and the pathological registry. All patients underwent a tertiary transvaginal or transabdominal sonography, and only cases with preoperative measurement of serum Ca125 and CEA levels (drawn as part of regular clinical practice) were included in the study. Oophorectomy, cystectomy or hysterectomy with unilateral or bilateral salpingo-oophorectomy were performed as treatment modality according to age and menopausal status, fertility considerations, physical examination and sonographic findings. Patients with concomitant gastrointestinal pathology were excluded. Also, cases were excluded from the study if the final histological type of the adnexal finding was not documented. The reports were reviewed, and the retrieved parameters included patient's age and histological type of adnexal mass. The latter was then divided into 6 categories: benign, borderline, primary ovarian malignancy, tumor metastatic to the ovary, granulosa or germ cell tumor.
All serum marker measurements were performed in the Clinical Chemistry department of Carmel Medical Center, by electrochemiluminescence immunoassay on a Roche Cobas e analyzer (Roche Diagnostics, Mannheim, Germany). Serum Ca125 of < 35 U/mL and CEA of < 5 ng/mL were taken as within the normal range. Sensitivity, specificity, positive predictive value (PPV), negative predictive value (NPV) and relative risks (RRs) with 95% confidence interval (95% CI) were calculated for each tumor marker and for their combination in evaluation of benign vs. malignant adnexal masses. A separate examination of CEA and Ca125 values was made in borderline tumors, mature cystic teratomas (MCTs) with or without malignant transformation, and mucinous findings.
The study was approved by the local Institutional Review Board Committee for Human Subjects.
Statistical Analysis
Data were analyzed using SPSS software (SPSS Inc., Chicago, IL, USA). Continuous variables were presented as means ± SD and were tested by Student's t-test. Categorical data were expressed as numbers and compared using the Fisher's exact test and
Results
Four hundred ninety-five women aged 18-88 years, referred to our institution due to adnexal masses, were identified and included in the study. Benign pathology was diagnosed in 261 of the cases (52.7%), 181 of the histology reports (36.6%) were malignant and 17 metastatic (3.4%), including 13 cases of gastrointestinal origin, 3 cases of metastatic breast carcinoma and 1 case of sarcoma of unknown origin. The remaining cases included 28 borderline tumors (5.7%), 7 granulosa cell tumors (1.4%) and 1 case of germ cell tumor.
Mean preoperative serum Ca125 levels were 319.7 ± 890.6 U/mL. Preoperative serum CEA was elevated above 5 ng/mL in 34 cases (6.87%) and averaged 3.2 ± 12.9 ng/mL. Using the Spearman rank correlation test, no correlation was found between the 2 markers (data not shown). Table I presents tumor markers levels by each pathology outcome.
Ca125 and CEA levels according to pathology outcome
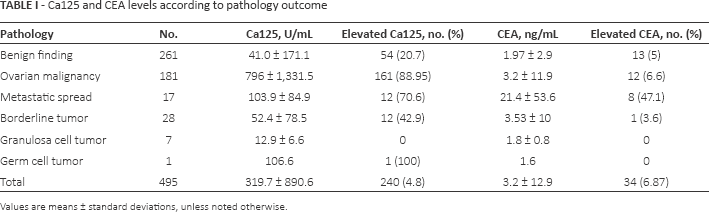
Values are means ± standard deviations, unless noted otherwise.
Since only 7 cases of granulose cell tumor and 1 case of germ cell tumor were reported, these cases were omitted from the primary calculation. In addition, the borderline tumor group was analyzed separately because of its unique nature. In the remaining 459 cases, 261 benign and 198 malignant (primary ovarian and metastatic) cases were demonstrated (Tab. II).
Analysis of Ca125 and CEA levels in malignant vs. benign cases
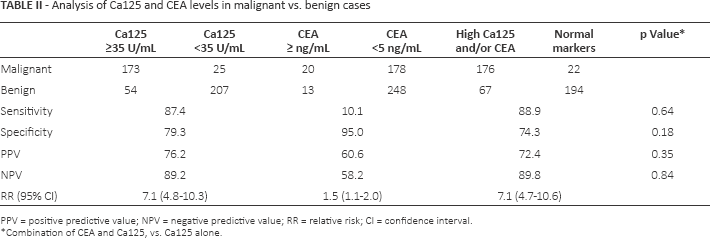
PPV = positive predictive value; NPV = negative predictive value; RR = relative risk; CI = confidence interval.
Combination of CEA and Ca125, vs. Ca125 alone.
Mean Ca125 levels in the malignancy group were 736.6 ± 1287.7 U/mL, and mean CEA values 4.7 ± 19.7 ng/mL, both significantly higher than in the benign group (p<0.0001 and p = 0.0266, respectively). However, the combination of CEA with Ca125, compared with Ca125 levels alone, yielded a nonsignificant effect on sensitivity (87.4% vs. 88.9%, respectively, p = 0.64) and specificity (79.3% vs. 74.3%, p = 0.18) in differentiating malignant from benign adnexal masses. Of note, for CEA levels of >16 ng/mL (and up to a maximal value of 224 ng/mL), 9 of the 11 cases were malignant, excluding 1 case of mucinous cystadenoma and 1 borderline tumor (with levels of 40.2 ng/mL and 54.5 ng/mL, respectively).
In the 232 cases with normal Ca125 level, which included 25 malignancies, elevated CEA was found in 16 cases. Of these, 13 cases were benign and 3 malignant, with varying pathology (Tab. III). Mean CEA levels did not differ between the 25 malignant (3.7 ± 9.1 ng/mL) and 207 benign (2.1 ± 3.3 ng/mL) cases with normal Ca125 levels (p = 0.0794).
Pathology of malignant cases with abnormal CEA and normal Ca125 levels

Out of 198 malignant cases, 181 primary ovarian malignant tumors were found and 17 cases of metastatic spread to the ovary (Tab. IV). Significantly higher mean Ca125 levels were observed in primary ovarian malignant tumors compared with metastatic group (see Tab. I; p = 0.0338); however, the RR did not yield a statistical significance (RR = 1.3, 95% CI, 0.9-1.7). On the contrary, significantly higher mean CEA levels were observed in the metastatic group (see Tab. I; p = 0.0002), with RR = 7.1 (95% CI, 3.4-14.9) for metastasis differentiation by levels above 5 ng/mL. Ca125/CEA ratio above 25 also yielded a significant RR for primary ovarian tumor differentiation (RR = 2.4, 95% CI, 1.3-4.6).
Analysis of elevated Ca125, CEA and Ca125/CEA ratio incidence in primary ovarian vs. metastatic tumors
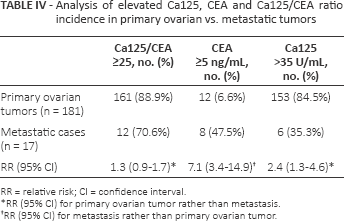
RR = relative risk; CI = confidence interval.
RR (95% CI) for primary ovarian tumor rather than metastasis.
RR (95% CI) for metastasis rather than primary ovarian tumor.
Of the 28 borderline tumors, Ca125 was elevated in 12 cases (42.9%). When combined with benign cases (Tab. V), borderline tumors were found in 18.2% of cases with elevated Ca125 compared with 7.2% of cases with normal Ca125, a statistically significant difference (p = 0.0155). High CEA was observed in 1 of 28 borderline tumors (3.6%), with PPV of 7.1% compared with 10.9% in normal CEA levels, which was not statistically significant. No significant differences were found between mean Ca125 or CEA levels in borderline vs. benign groups.
Analysis of elevated Ca125 and CEA incidence in borderline tumors vs. benign cases
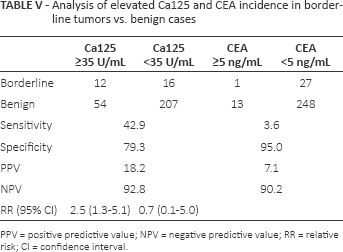
PPV = positive predictive value; NPV = negative predictive value; RR = relative risk; CI = confidence interval.
Excluding 2 cases of borderline tumors in which the exact histotype was not recorded, 15 serous and 11 mucinous tumors were observed. CEA was elevated in 1 mucinous and in none of the serous borderline tumors, a difference not statistically significant (p = 0.423). Also, no significant differences were found between mean CEA levels in serous vs. mucinous borderline tumors (Tab. VI).
Comparison between mucinous adnexal masses and nonmucinous histotypes
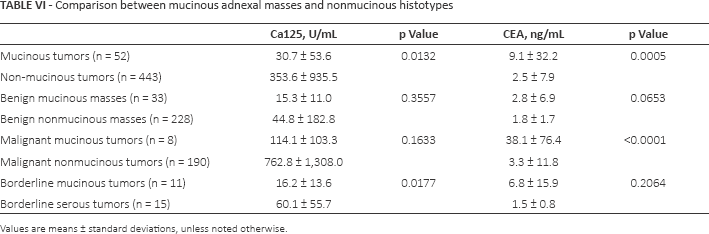
Values are means ± standard deviations, unless noted otherwise.
Regarding mucinous histological types, 52 cases were found overall, including 30 benign mucinous cystadenomas/cystadenofibromas, 11 borderline tumors, 5 cases of primary ovarian mucinous adenocarcinomas and 3 adenocarcinomas of colon (Tab. VI). CEA was elevated in 8 of these cases (15.4%): 3 benign, 1 borderline tumor, 2 ovarian and 2 metastatic tumors. This proportion was significantly higher compared with the nonmucinous cases (26/443 or 5.9%, p = 0.0181). A comparison of mean Ca125 and CEA serum levels in mucinous masses and the rest of the cases is presented in Table VI. Of note, CEA levels in the 8 mucinous malignant histotypes were higher than in benign mucinous masses (38.1 ± 76.4 ng/mL vs. 2.8 ± 6.9 ng/mL, p = 0.0098).
Thirty-two cases of MCTs were noted, 1 of which (3.1%) demonstrated elevated CEA levels. Mean MCT CEA levels (1.6 ± 1.5 ng/mL) did not differ from the rest of the cases (p = 0.4839). Three cases of malignant transformation of MCT were noted, with mean CEA level of 2.8 ± 2.4 U/mL, not different from benign MCT CEA levels (p = 0.2038).
In addition, CEA levels were high in 1 of 26 endometrioma cases (3.8%) – not a statistically significant proportion compared with the rest of the cases (p = 0.1558). Also, mean CEA levels in this group (1.6 ± 1.7 U/mL) did not differ from the rest of the cases (p = 0.5280).
Discussion and Review of the Literature
CEA and Malignancy
CEA is one of the longest known tumor antigens. It was initially described in 1965 by Freedman and Gold, who performed serological studies using extracts of colon adenocarcinoma tissues (6). This component was also demonstrated in embryonic digestive system, and since at first it could not be detected in any other adult human tissues, it was termed carcinoembryonic antigen. The initial serological studies revealed that 70% of patients with primary nonmetastatic tumors of the digestive system had circulating anti-CEA antibodies in their sera (23). In 1969, a new radioimmunoassay for determining CEA serum levels in patients with cancer of the colon and rectum was introduced, with a high degree of reproducibility and specificity (24). At present, CEA is still the most widely used tumor marker for the management of colorectal cancer (7, 8). However, the initial claim that serum CEA assay might serve as an exclusive immunodiagnostic test for colon cancer was dismissed by subsequent studies, as abnormal CEA levels were found in many other kinds of cancer, as well as in nonmalignant diseases such as pancreatitis, liver cirrhosis and ulcerative colitis (25-27), and even in sera from heavy smokers (28). In particular, elevated serum CEA levels were demonstrated in about 50% of patients with ovarian adenocarcinomas (9, 10) and up to 87%-88% in mucinous histotypes (11, 12).
In 1981 a new murine monoclonal antibody, Ca125, reacting almost exclusively with ovarian cancer cells, was discovered by Bast et al (29). An immunoassay using Ca125 antibody demonstrated a significant correlation between the test measurements and the course of epithelial ovarian carcinomas (30), and soon it became the preferred tumor marker in the diagnosis and management of ovarian cancer (5). Several articles have suggested that concomitant measurement of Ca125 and CEA serum levels can improve ovarian cancer diagnosis, despite the lowered specificity (13-15). In addition, Kikkawa et al noted that CEA may serve as a screening marker for squamous cell carcinoma arising from MCTs (31). However, other works claimed that CEA measurement has no clinical utility in evaluation of masses suspicious for ovarian cancer (16-18), and none of the consensus groups has included CEA evaluation in the guidelines regarding evaluation of suspicious adnexal masses.
Our results have shown that CEA levels above 5 ng/mL have sensitivity of 10.1% and specificity of 95% in differentiating malignant from benign cases, approximating the findings reported by other studies (16, 32). Combination of both markers did not exhibit a significant effect on the performance of Ca125 alone. Of note, no differences in CEA levels were found between MCTs and the cases of malignant transformation of MCT. Therefore, in our opinion and consistent with several previous studies, preoperative CEA levels have no substantial value in predicting whether a suspected adnexal finding is benign or malignant.
CEA and Metastases
Metastatic carcinomas account for approximately 15% of malignant tumors involving the ovary. The most common primary sites are stomach, large bowel, appendix, breast, uterus, lung and skin. Eighty percent of ovarian metastases from extragenital sites are derived from gastrointestinal tract carcinomas, which commonly mimic primary neoplasms (33). Factors suggestive of metastasis include history of malignancy, younger age, bilaterality, absence of ascites, reduced multilocularity and an increased resistance index (34, 35). Still, the preoperative differentiation of primary and metastatic ovarian tumors, though of paramount importance for subsequent management, can be very difficult.
Several immunohistochemical studies have reported the ability of anti-CEA monoclonal antibodies to differentiate gastrointestinal metastasis to the ovary from ovarian adenocarcinomas, as the former show significantly higher immunoreactivity in tumor tissues (36-38). Serum CEA levels were also shown to be elevated in nongynecological ovarian carcinoma compared with primary ovarian tumors (35, 39). In addition, some of the studies have recommended using the Ca125/CEA ratio, since values exceeding 25 showed a high sensitivity (73%-100%) and specificity (62%-100%) for ovarian malignancy diagnosis (13, 40, 41).
Our analysis has also noted higher CEA levels in metastatic tumors compared with primary ovarian cancer, accompanied by lower Ca125 measurements. Thus, our findings suggest that in debatable cases, the combination of these 2 markers can aid the managing physician in determination of tumor origin. As previously reported, cases with Ca125/CEA ratio above 25 may indicate to primary ovarian tumor diagnosis (RR = 2.4, 95% CI, 1.3-4.6, according to our study). As CEA elevation alone imparts a meaningful magnitude of effect for metastatic tumor (RR = 7.1, 95% CI, 3.4-14.9), it seems that its serum levels are able to differentiate between primary and metastatic ovarian carcinomas at least as well as the Ca125/CEA ratio. It should be noted, though, that only 17 metastatic cases were found in our study, encompassing 8.6% of malignant cases and 3.4% of overall ovarian masses. Thus, no solid conclusions can be drawn without future large, well-designed, prospective cohort trials.
CEA and Mucinous Histotypes
Ovarian mucinous tumors constitute a spectrum subdivided into benign mucinous cystadenomas (about 80% of cases), borderline mucinous tumors and invasive mucinous carcinomas (42). Diagnosis of these lesions is complicated by lower sensitivity of the Ca125 assay (43, 44) and by higher underdiagnosis rates on frozen section examination as compared with serous tumors (45).
Many studies have demonstrated the relationship between CEA tumor marker and mucinous ovarian tumors, whether by increased serum measurements, cyst fluid levels or by immunohistochemical examination (11, 46). Abnormal CEA levels were noted in 87%-88% of mucinous cancer cases (11, 12), and high CEA content in immunohistochemical studies was found to parallel the increased malignant potential of the tumor (47).
Our analysis has shown that mucinous masses exhibit higher CEA and lower Ca125 levels compared with the nonmucinous cases. In addition, while Ca125 levels do not differ between malignant mucinous and malignant nonmucinous tumors, higher CEA levels are associated with the former group. Thus, our results suggest that the addition of CEA to Ca125 measurement in evaluation of patients with adnexal masses not only raises the suspicion of metastatic cases, but also may potentially lead to a specific histological characterization. However, the small number of malignant mucinous tumors (n = 8) and the high standard deviation compared with the mean CEA level (38.1 ± 76.4) in these cases interfere with drawing any solid conclusions, and large-cohort prospective studies are necessary to further explore this subject.
CEA and Borderline Ovarian Tumors
Borderline ovarian tumors (BOTs) account for 10%-20% of ovarian epithelial tumors and have a favorable prognosis (48). Their main histological criteria are cellular proliferation and slight nuclear atypia without stromal invasion (49). Many studies examining tumor marker measurements in BOTs have reported low rates of abnormal CEA levels (8%-20%) (50-53) and concluded that CEA did not have any association with tumor presence (50). However, Nomelini et al, in their retrospective analysis of 21 patients, have noted that abnormal CEA levels were found more frequently in stages IB-IIIC, and suggested that this marker might have prognostic value in BOTs (54). Zhang et al evaluated 70 BOT patients, 60% of whom had abnormal CEA levels, and concluded that CEA can be effective in monitoring of BOT (55). In addition, a case report of a postmenopausal woman with extremely high tumor markers including CEA (398 ng/mL) was described, with imaging studies suspicious of ovarian cancer. Postoperative examination of the specimen revealed torsion of the left ovarian mucinous cystadenoma with borderline malignancy (56).
Our study has noted a low rate of abnormal CEA levels in the 30 BOT cases (3.5%), and found no difference in CEA levels between BOT and benign cases. Thus, according to our analysis, and in agreement with several previous studies, CEA measurement has no value in detecting BOTs.
CEA and Benign Conditions
Abnormal CEA levels may mislead the diagnosis, as several benign disorders involving increased CEA were described in the literature, including rheumatoid arthritis (20), appendiceal mucocele (57), true splenic cyst (58) and a case report of a patient with bronchial asthma and mucoid impaction (59). Sasaki et al have suggested that CEA assessment could serve as a prognostic factor in predicting the future regression of simple ovarian cysts (60), and Pinto et al have shown that combination of CEA and Ca125 measurements could be helpful in the distinction of functional from epithelial ovarian cysts (61).
One study demonstrated a relationship between higher CEA levels and increasing size of ovarian dermoid cysts (19), and normal CEA values have been reported in patients with endometriosis (62, 63).
Our study found abnormal CEA values (up to 40.2 ng/mL) in 5% of the benign cases. This tumor marker was elevated in only about 3% of dermoid cases and endometriomas. Thus, although lower CEA values can imply the diagnosis of a benign condition, high levels can be found in nonmalignant cases as well.
The value of our manuscript is in its review of prior studies and in the analysis of data from a relatively large cohort of women who all underwent CEA levels as part of a routine preoperative workup of an adnexal mass. However, several limitations are worth mentioning, including lack of distinction between age groups, menopause vs. premenopause and smoking vs. nonsmoking status; and the retrospective collecting date approach. In addition, the high prevalence of ovarian cancer in this specific group of patients who all underwent surgery might be related to possible selection bias, which may interfere with the generalization of these results.
In summary, the combination of CEA with Ca125 did not exhibit clinical significance in distinguishing between benign and malignant adnexal masses compared with Ca125 alone. As our results imply that abnormal CEA levels can aid in distinguishing metastatic disease from primary ovarian tumors and in detection of mucinous histological subtypes, this subject should be further investigated in large, well-designed, prospective cohort trials.
Footnotes
Financial support: This research received no specific grant from any funding agency in the public, commercial or not-for-profit sectors.
Conflict of interest: None of the authors have any conflict of interests to declare.
