Abstract
Mucoepidermoid carcinoma is the most common malignant tumor of the salivary gland. The oncocytic variant of mucoepidermoid carcinoma (OMEC) is rare and a small subset shows exclusive oncocytic morphology. Here we report an OMEC case of the parotid gland in a 74-year-old woman with exclusive oncocytes and rare mucocytes. The oncocytes showed diffuse nuclear positivity with p63 immunostaining. The MAML2 translocation was present, supporting the diagnosis of OMEC. Distinguishing OMEC with exclusive oncocytes from oncocytoma and oncocytic carcinoma can be very challenging for pathologists and is critical for proper clinical management. Our experience suggests that appropriate ancillary studies, especially the MAML2 translocation, may provide the essential evidence in difficult cases. Our literature review shows that the presence of mucocytes in an oncocytic neoplasm might be an important morphologic clue of OMEC.
Introduction
Mucoepidermoid carcinoma (MEC) is the most common malignant tumor of the salivary gland.1,2 Arising from salivary gland ducts, MEC is typically characterized by various combination of squamoid (epidermoid), intermediate, and mucus-producing cells. 3 Oncocytic metaplasia in MEC is not uncommon; however, the oncocytic variant of MEC (OMEC), composed of 50% or more oncocytic cells, is very rare.4,5
Given its rarity and atypical morphology, differentiating OMEC from other oncocytic neoplasms (Warthin tumor, oncocytoma, oncocytic carcinoma, etc.) could be very challenging and certain ancillary studies have great values in assisting the diagnosis. For example, a diffuse nuclear staining from p63 immunostaining has been used to diagnose OMEC. 5 Importantly, the MAML2 gene rearrangement is detected in both typical MEC 6 and OMEC, 7 which is of great value in the distinction of OMEC from other oncocytic neoplasms. We report an OMEC case of the left parotid gland in a 74-year-old woman. The neoplasm was composed exclusively of oncocytic cells and rare mucocytes. Fluorescence in situ hybridization (FISH) detected the MAML2 rearrangement in 44.5% of the tumor cells. Our case highlights the diagnostic challenge in OMEC with exclusive oncocytic morphology and the importance of utilizing appropriate ancillary studies in difficult cases. A literature review of previously reported OMEC cases with exclusive oncocytic morphology is also provided.
Case Report
The patient was a 74-year-old African American female with a past medical history of hypertension, smoking, sarcoidosis, and fibromyalgia. She presented with a painful swelling in her left neck and the symptoms did not improve with antibiotics and oral steroids for 4 months. She was referred for head and neck surgical evaluation. Physical examination demonstrated a 2-cm mobile tender mass inferior to the left earlobe. The overlying skin was unremarkable. Facial movement was intact and no cervical lymphadenopathy was identified. Contrasted CT of the neck revealed a 2.5×1.6 cm oval-shaped, cystic mass with irregular borders within the left parotid gland. The mass demonstrated peripheral enhancement and central hypo-attenuation. The top differential diagnoses by imaging included malignancy and infection. A fine needle aspiration was performed at the outside hospital and inconclusive.
The patient was transferred to the Veterans Affairs San Diego Healthcare System for surgery, due to the suspicion of a salivary neoplasm with malignant potential. Left parotidectomy was performed, during which a relatively well-demarcated cystic tumor was encountered within the superficial lobe of the parotid gland. There was no clinical evidence of extra-parenchymal extension, and no difficulty was encountered in dissecting the tumor from the facial nerve branches. The tumor and surrounding superficial parotid lobe were removed en bloc. Several slightly enlarged lymph nodes from Level II were also biopsied for histologic examination. No frozen section examination was requested intraoperatively.
Pathological Findings
Macroscopically, the tumor measured 2.8×1.5×1.2 cm in size with an ill-defined boundary. There were cystic and hemorrhagic changes within the tumor. The vast majority of the tumor were sampled and submitted in six tissue blocks, in addition to one block of the uninvolved parotid gland. Microscopically, the tumor had an infiltrative growth pattern with centrally cystic areas and focal necrosis (Figure 1A). The neoplastic cells were exclusively oncocytic, characterized by abundant eosinophilic granular cytoplasm, uniformly round nuclei, and variably-sized nucleoli (Figure 1B,C). There were rare mucocytes, comprising less than 1% of the neoplasm (Figure 1C). No discernible populations of squamoid (epidermoid), or intermediate cells were noted. A focus of perineural invasion was present as shown in Figure 1D. No mitotic figures or significant lymphoid infiltrates were identified within the neoplasm. The uninvolved salivary parenchyma showed scattered small foci of chronic inflammation and otherwise unremarkable morphology. There were two lymph nodes identified with no involvement by the tumor cells.

Morphologic features of the oncocytic mucoepidermoid carcinoma. A) Hematoxylin and eosin stained slide demonstrates the infiltrative border and exclusively oncocytic tumor cells with central cystic changes (asterisk, magnification 20×). B) There are variably sized nests of neoplastic cells (Magnification 100×). C) The neoplastic cells are characterized by abundant eosinophilic cytoplasm, centrally located round nuclei, delicate nuclear membrane, and a small nucleolus. A single mucocyte is present (arrow, magnification 400×). D) A focus of perineural invasion is present (Arrow, magnification 200×).
The infiltrative pattern suggested a malignant neoplasm and the differential diagnoses included oncocytic carcinoma and oncocytic variants of other salivary malignancies, including OMEC. Mucicarmine stain confirmed the presence of rare mucocytes (Figure 2A). p63 immunostaining (Clone: BC4A4, monoclonal, BioCare Medical, Concord, CA, USA) revealed moderate-to-strong nuclear positivity in the oncocytes with a diffuse staining pattern (Figure 2B). p63 were negative in mucocytes (not shown). FISH was performed to detect the MAML2 translocation using a break-apart probe flanking the MAML2 gene at 11q21 locus (Leica DM 6000B, Mayo Clinic, Rochester, MN, USA). 6 The result was nuc ish (MAML2x2)(5MAML2 sep 3MAML2x1) [89/200], i.e. 44.5% of the cells were positive for the MAML2 translocation (Figure 2C). Thus, the overall findings supported the diagnosis of OMEC with exclusive oncocytic morphology. Because of necrosis and perineural invasion, this case was graded as intermediate grade according to Armed Forces Institute of Pathology (AFIP) method.

Ancillary studies performed on the oncocytic mucoepidermoid carcinoma. A) Mucicarmine histochemical staining highlights a single mucocyte (the black arrow). B) The neoplastic cells show moderate-to-strong nuclear immunoreactivity for p63 antibody with a diffuse pattern. C) Fluorescence in situ Hybridization with a break-apart probe detects the MAML2 rearrangement. The 5’ end of the FISH probe is labeled with Spectrum Orange and the 3’ end with Spectrum Green. White arrows indicate representative nuclei harboring the MAML2 rearrangement.
Post-Operative Management
Based on the pathologic diagnosis of an intermediate grade MEC and the presence of perineural invasion, the patient received adjuvant radiation therapy postoperatively with a total of 6600 centiGray (cGy) to the parotid bed and 5040 cGy to the ipsilateral neck via volumetric-modulated arc therapy. She remained disease-free 16 months after the surgery.
Discussion
Clinical presentation is of limited use in the diagnostic evaluation of parotid neoplasms. Although malignant parotid neoplasms have certain clinical features (affecting older population, facial nerve palsy, deep fixation, lymphadenopathy, and rapid enlargement), the distinction is difficult due to the much higher incidences of benign neoplasms and non-neoplastic conditions.
In addition to the typical composition of squamoid, intermediate and mucus-producing cells, MEC has other morphologic variants, including OMEC, clear cell, sclerosing with or without eosinophilia, sebaceous, spindle cell, goblet cell, etc.8,9 OMEC is rare and comprises about 2% of all MEC cases according to one study. 10 Even though there is no consensus on the minimal amount of oncocytic cells needed, most reports use 50% or more oncocytic cells as the cutoff to diagnose OMEC.5,11 There are more than 30 OMEC cases found in the PubMed database. Specifically, 3 cases7,12,13 of OMEC with exclusive oncocytic morphology have been reported (Table 1). Including our case, the median age is 56.5 years old. All four cases are in major salivary glands (3 in parotid and 1 in submandibular gland). The median tumor size is 2.7 cm. Two cases tested for p63 immunostaining reported nuclear staining patterns. MAML2 translocation is detected in 2 of 2 cases tested. The popular grading systems of MEC include the AFIP method and the Brandwein method, which are also used empirically on OMEC. All four cases are either low or intermediate grade. The median follow-up time is 1.7 years, during which the patients remained disease free.
Reported cases of mucoepidermoid carcinoma with exclusive oncocytic morphology in salivary glands.
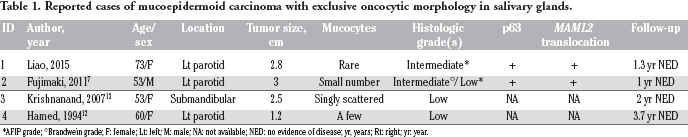
AFIP grade;
Brandwein grade; F: female; Lt: left; M: male; NA: not available; NED: no evidence of disease; yr, years; Rt: right; yr: year.
The top differential diagnoses of the exclusive oncocytic neoplasms in salivary glands include oncocytoma, and oncocytic carcinoma. The distinction is clinically important due to the different prognosis. Oncocytoma is a benign neoplasm and possesses well-defined capsule, a feature distinct from the other two malignant entities. Oncocytic carcinoma is considered a high-grade malignancy and often shows infiltrative growth pattern, cytologic atypia and pleomorphism. OMEC usually shows low-to-intermediate grade of malignancy. Interestingly, all four cases of OMEC with exclusive oncocytes consistently show small numbers of mucocytes,7,12,13 suggesting that it is an important morphologic clue in diagnosing OMEC. The distinction could be very challenging and ancillary studies are needed for difficult cases. p63 immunostaining typically shows diffuse nuclear positivity throughout tumor nests in OMEC, distinct from the peripheral staining pattern of oncocytoma and oncocytic carcinoma.5,14 The MAML2 gene is a component of the Notch signaling pathway. MAML2 translocation by FISH is detected in approximately 66% typical MEC cases. 6 The most common partner gene is CRTC1 (CREB-regulated transcription coactivator), resulting in t(11:19)(q21;p12-13). MAML2 translocation is also detected in OMEC.7,11 In comparison, no MAML2 translocation was detected in most of MEC mimics, including oncocytoma, oncocytic carcinoma, pleomorphic adenoma, acinic cell carcinoma.6,15,16 Therefore, MAML2 translocation is a useful tool for diagnosing OMEC. However, MAML2 translocation is not specific to MEC and has been reported in Warthin's tumor, clear cell hidradenoma and odontogenic cyst.15,17
Conclusions
In summary, we present a rare morphologic variant of MEC composed of exclusive oncocytes and rare mucocytes. The presence of mucocytes in oncocytic neoplasms should raise the suspicion of OMEC and warrants further workup. In addition to p63 immunostaining and mucicarmine histochemical staining, analysis of MAML2 rearrangement could provide the critical evidence for the correct diagnosis.
Footnotes
Acknowledgements
The authors thank Drs. Suzanne E. Peterson and Robert Fitzgerald for their comments.
