Abstract
Annual influenza vaccine is recommended for organ transplant recipients, but immunogenicity is known to be suboptimal. Islet transplant recipients receive immunosuppressive therapy, but there are no data on the immunogenicity of influenza vaccine in this population. In this prospective cohort study, adult islet transplant recipients at least 3 months posttransplant were enrolled. All patients received the 2010–2011 seasonal influenza vaccine. Serum was obtained pre- and postvaccination to determine humoral response to each of the three influenza strains included in the vaccine. Adverse effects of vaccine were also noted. A total of 61 islet transplant recipients were enrolled and completed the study protocol. The median time from last transplant was 1.9 years (range 0.26–11.4 years), and most patients had undergone multiple prior islet transplant procedures (90.2%). Overall immunogenicity of the vaccine was poor. Seroconversion rates to H1N1, H3N2, and B antigens were 34.4%, 29.5%, and 9.8%, respectively. In the subset not seroprotected at baseline, a protective antibody titer postvaccination was achieved in 58.6%, 41.9%, and 34.5% of patients, respectively. Patients within the first year of transplant were significantly less likely to seroconvert to at least one antigen (23.5% vs. 54.5%; p = 0.029). Alemtuzumab recipients trended toward lower seroconversion rates (25% vs. 51%; p = 0.11). No vaccine-related safety concerns were identified. Seasonal influenza vaccine had suboptimal immunogenicity in islet transplant recipients especially those who were less than 1 year posttransplant or had received alemtuzumab induction. Novel strategies for protection in this group of patients need further study.
Introduction
Seasonal influenza infections cause significant morbidity and mortality in transplant recipients (14). Influenza is an RNA virus that is classified into three subtypes: A, B, and C. Subtypes A and B cause the majority of human disease. Although most infections remain in the upper respiratory tract, up to one third of transplant patients can develop pneumonia requiring hospitalization (10,14). In addition, transplant recipients have high tissue viral loads and shed virus for prolonged periods (13). Current guidelines recommend annual influenza vaccination with a trivalent inactivated vaccine for all transplant recipients (4,15). The vaccine consists of two influenza A strains based on the surface glycoproteins, hemagglutinin (H) and neuraminidase (N), as well as a B strain. Seroresponses (i.e., seroprotection or seroconversion) to seasonal influenza vaccine in organ transplant recipients have been quite variable and range from 15% to 93% for at least one vaccine virus strain, but in the majority of studies is suboptimal (12). This variability is likely due to type of transplant studied, time from transplant, and various immunosuppressive regimens.
Allogeneic pancreatic islet transplantation has been used successfully as a therapy for patients with poorly controlled type 1 diabetes mellitus for over a decade. With current immunosuppressive protocols, insulin independence rates at 5 years posttransplant are more than 50% (20). Nevertheless, given the intense immunosuppression required to control both auto- and allo-immunity, patients remain at risk of complications of immunosuppression including viral infections such as influenza. There are no published data with regard to influenza vaccine immunogenicity in patients who have undergone islet transplantation. Islet transplant patients are a unique population to study the immune response to vaccination, since they receive a cellular rather than organ transplant, undergo induction using various immunosuppressive regimens, and can often undergo multiple transplant procedures. Commonly used immunosuppressant agents used for induction include antithymocyte globulin (ATG) or alemtuzumab or interleukin 2 (IL-2) receptor antagonist (daclizumab or basiliximab). In addition to one of these, patients may also receive an anti-tumor necrosis factor (TNF) agent such as etanercept or infliximab. Maintenance immunosuppressive strategies usually include tacrolimus and mycophenolate mofetil (MMF) or sirolimus. There are little comparative data in the literature evaluating vaccine responses in patients that receive these induction regimens or combinations of induction regimens.
The aim of the present prospective cohort study was to assess seasonal influenza vaccine immunogenicity and safety in a cohort of islet transplant recipients receiving tacrolimus and MMF.
Materials and Methods
Patient Population
This was an observational cohort study conducted at the University of Alberta Hospital. The study was approved by the Health Research Ethics Board, and all study participants gave written informed consent. Adult islet transplant recipients were identified and recruited from outpatient clinics in August 2010. Patients currently enrolled in NIH trials of islet transplantation were excluded. To be eligible, patients were at least 3 months from their most recent transplant and receiving at least one immunosuppressive medication. For transplant, all patients received induction immunosuppression that consisted of either an IL-2 receptor antagonist (daclizumab 2 mg/kg at days 0 and 5 or basiliximab 20 mg on days 0 and 4), antithymocyte globulin (ATG), or alemtuzumab. These were given with or without a TNF-α antagonist (etanercept 50 mg weekly or infliximab 10 mg/kg given at time of transplant). Patients also received maintenance immunosuppression with a combination of tacrolimus (to maintain a trough of 8–10 ng/ml) and MMF. Patients had to be willing to receive the influenza vaccine and have no contraindications to vaccination such as egg allergy or history of vaccine-related Guillain–Barre syndrome. The annual influenza vaccine Fluviral® (GlaxoSmithKline, Canada) was available to all transplant patients in October 2010, and study participants received vaccine at their local public health unit. The 2010–2011 influenza vaccine contained 15 μg each of the following virus strains: A/California/7/2009 (H1N1)-like strain, A/Perth/16/2009 (H3N2)-like strain, and B/Brisbane/60/2008. The vaccine dose was administered as a 0.5-ml intramuscular injection in the deltoid muscle. Patients were vaccinated between October 2010 and January 2011. Venous blood samples were collected prevaccination and at 4–6 weeks postvaccination.
Baseline demographic and transplant data were collected for each patient. For adverse event reporting, patients were contacted at 48 h postvaccination, and followed until 6 months postimmunization for the development of microbiologically documented influenza infection.
Laboratory Methods
Sera collected pre- and 4–6 weeks postvaccination were stored at −80°C until testing. All serum samples were tested for antibodies against the three influenza strains present in the vaccine using the hemagglutination inhibition assay (HAI). The test was performed at the Microbiology Services, Colindale, Health Protection Agency, UK, using methods previously described (6). Briefly, serum was incubated with a receptor-destroying enzyme to remove any nonspecific inhibitors of hemagglutination. Serially diluted sera were then incubated with influenza virus (containing 4 hemagglutination units of virus) followed by addition of 0.5% turkey red blood cells. Titers were determined by doubling dilutions of antibody. All sera were tested in duplicate. The lower limit of detection of the assay was a dilution of 1:10.
Definitions
The primary endpoints were based on criteria defined by the EMEA (European Agency for Evaluation of Medicinal Products) and the US Food and Drug Administration for use in trials assessing influenza vaccine immunogenicity (7,22). Primary endpoints included seroprotection defined as a HAI titer of ≥1:40 postvaccination and seroconversion, defined as a fourfold increase in HAI titers from pre- to postvaccination and achieving a titer of ≥1:40. For statistical analysis, a titer reported as less than 10 was assigned a value of 5.
Statistical Analysis
Geometric mean titers (GMTs) of strain-specific antibody and mean seroconversion factors were compared between baseline and postvaccination using a Wilcoxon rank-sum test for paired data. Seroconversion and seroprotection rates were compared between baseline and postvaccination using the McNemar test. The seroconversion factor or the fold increase in titer was calculated by dividing the postvaccination titer by the pre vaccination titer. A geometric mean of the seroconversion factor for each influenza strain was then calculated, termed the geometric mean fold rise (GMFR). Multivariate analysis using a forward conditional method was done for factors affecting seroconversion to at least one antigen. Variables were included that had a value of p < 0.2 on univariate analysis or factors previously shown to be clinically significant in affecting vaccine response. a was set equal to 0.05, and all tests of significance were two-tailed. The above analysis was done on the whole cohort and for patients in the following subgroups: IL-2 receptor antagonist group, ATG, and alemtuzumab. Statistical analyses were performed using PASW Statistics (version 19.0; Chicago, IL).
Results
Patient Population
A total of 92 patients were eligible, of which 71 patients agreed to participate in the study. Of these, three patients were excluded because they underwent retransplantation within 1 month after influenza vaccination. In addition, for seven patients, blood samples were not collected postvaccination, and they were excluded from analysis. Therefore, 61 patients were analyzed in the study, all of whom had undergone allogeneic islet alone transplantation, except for one patient who received an islet after kidney transplant. The clinical and demographic characteristics of the patients are listed in Table 1. The majority of patients (59%) had undergone two islet transplants, and a few (9.8%) had undergone up to four prior islet transplants. For induction immunosuppression at the time of most recent transplant, most patients (50.8%) received an IL-2 receptor antagonist, either daclizumab or basiliximab. Approximately half the patients also received a TNF-α antagonist, either etanercept or infliximab, in addition to the induction therapy. For long-term immunosuppression, most patients were prescribed a combination of tacrolimus and MMF. Only one patient received sirolimus. This patient was transplanted several years ago when the immunosuppression protocol for islet transplantation was sirolimus based. The sole kidney-islet recipient in the cohort was also receiving prednisone 5 mg daily. Immunosuppressant use remained stable from vaccination to postimmunization sample collection. Supplementary exogenous insulin was being used to ensure excellent glycemic control in 37 (60.7%) recipients. Almost all patients (60/61, 98.4%) had previously received influenza vaccine. No patient had developed microbiologically documented influenza infection by the 6 months of follow-up.
Baseline Demographics and Transplant Characteristics of Islet Cell Transplant Recipients Immunized With Influenza Vaccine

IL2RA, interleukin 2 receptor antagonist; TNF, tumor necrosis factor; MMF, mycophenolate mofetil; SD, standard deviation; IQR, interquartile range.
Vaccine Response
Seroprotection and seroconversion rates for each of three influenza strain contained in the vaccine are shown in Table 2. GMTs for all strains increased significantly after vaccination. Postvaccination seroprotection rates ranged from 67.2% to 78.7%. Seroconversion rates were lower and ranged from 9.8% to 34.4%. Seroconversion to at least one antigen was seen in 28/61 (45.9%) of patients. Of these, 14 (23%) patients seroconverted to one antigen only, 11 (18%) patients seroconverted to two antigens, and only 3 (4.9%) patients seroconverted to all three vaccine antigens. Older age defined as >60 years also negatively affected some vaccine responses; for example, patients of age >60 were less likely to be seroprotected with H1N1 strain (61.1% vs. 86.0%; p = 0.043) and B strain (44.4% vs. 76.7%; p = 0.014) and also less likely to seroconvert with H3N2 (11.1% vs. 37.2%; p = 0.042).
Geometric Mean Titers and Seroprotection/Seroconversion Rates to Vaccine Strains (N = 61)

For postimmunization GMTs, p < 0.001 for H1N1 and H3N2 and p = 0.004 for B.
Significant increase in seroprotection rates from baseline (McNemar test). GMT, geometric mean titer; GMFR, geometric mean fold rise.
Absolute pre- and postimmunization titers and seroprotection and seroconversion rates by induction immunosuppressive are shown in Figures 1 and 2. For statistical purposes, the induction agent assigned to a patient was the last one they received. The single patient who received belatacept was excluded from this analysis. There were no demographic differences in the three immunosuppressive groups. The patients classified as receiving IL-2 receptor antagonist had no previous exposure to alemtuzumab. Overall postimmunization seroprotection rates did not significantly differ between the three groups; however, the seroconversion rate to at least one antigen tended to be lower in those that received alemtuzumab versus other induction [3/12 (25%) with alemtuzumab vs. 25/49 (51%) with other induction; p = 0.11]. The geometric mean fold rise (GMFR or seroconversion factor) was significantly lower for H1N1 in those that had received alemtuzumab versus other induction therapy (1.33 vs. 3.10; p = 0.025) (Fig. 3). No significant differences in seroresponse were found in those who also received a TNF-α antagonist.

Pre- and postimmunization titers to influenza A/ H1N1 in individual patients grouped by most recent induction immunosuppression. Data shown exclude the one patient who received belatacept induction. Horizontal bars represent median values. Antibody titers are expressed as log2. IL2RA, interleukin 2 receptor antagonist; ATG, antithymocyte globulin; Alem, alemtuzumab.

(A) Seroprotection rates and (B) seroconversion rates postimmunization in a cohort of islet cell transplant recipients divided into three groups based on type of induction immunosuppression given at the most recent transplant. Data shown exclude the one patient who received belatacept induction. IL2RA, interleukin 2 receptor antagonist; ATG, antithymocyte globulin.
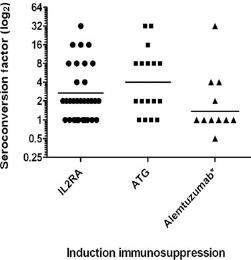
Seroconversion factors for influenza A/H1N1 in individual patients grouped by most recent induction immunosuppression. Horizontal lines represent geometric mean fold rise (GMFR) for each group. One patient was excluded from the alemtuzumab group to increase clarity. The GMFR for this patient was 0.06. IL2RA, interleukin 2 receptor antagonist; ATG, antithymocyte globulin. ∗GMFR for alemtuzumab, 1.33 versus 3.10 for other induction (p = 0.025)
Effect of Duration Posttransplant
There were 17 patients in the cohort that were less than 1 year posttransplant and 44 that had received their transplant greater than 1 year ago. Patients within the first year after their most recent induction were significantly less likely to seroconvert compared to those longer past their posttransplant [23.5% (4/17) vs. 54.5% (24/44), p = 0.029]. There was a trend to lower GMFR (geometric mean fold rise) for all strains for those within 1 year of transplant: H1N1 strain (1.7 vs. 3.1; p = 0.057), H3N2 (1.23 vs. 2.27; p = 0.079), and B (1.13 vs. 1.60; p = 0.11). For induction, 35.3% versus 56.8% received IL-2 receptor antagonist, 17.6% versus 31.8% received ATG, and 41.2% vs. 11.4% (p = 0.026) received alemtuzumab in the <1 year and >1 year groups, respectively. For maintenance immunosuppression, both groups were similar, with most patients receiving a combination of tacrolimus and MMF. In multivariate analysis of the following variables: within 1 year of transplant, alemtuzumab induction, TNF-α antagonist therapy, MMF >2 g daily, and age >60 years, time from transplant was the only independently significant variable (p = 0.035) (Table 3). There were only nine patients that were within 6 months from last transplant. Of these, only 2/9 (22.2%) seroconverted to at least one antigen.
Multivariate Analysis of Various Factors Affecting Vaccine Response (Defined as Seroconversion to at Least One Vaccine Antigen)

NS, not significant.
Univariate and multivariate analyses of factors that affect seroconversion to each vaccine antigen were done and included the above factors plus baseline seroprotection for each vaccine strain. In this subanalysis of each serotype, the following variables were significant on multivariate analysis: for H1N1, baseline seroprotection [odds ratio (OR) 1.20 (1.10–10.1); p = 0.03]; for H3N2, time from transplant [OR 1.66 (1.02–27); p = 0.048] and age >60 [OR 1.74 (1.12–29.2); p = 0.036]. No variable was predictive of seroconversion to influenza B.
Baseline Seroprotection
Baseline rates of seroprotection (i.e., a strain-specific titer of ≥1:40) ranged from 49.2% to 52.5%, depending on the influenza strain. For the subset of patients that were not seroprotected at baseline, GMTs to each strain increased significantly from baseline to postvaccination, although they remained low overall (Table 4). In this cohort, seroprotection rates after immunization ranged from 34.5% to 58.6%, whereas seroconversion rates ranged from 20.7% to 51.7%. The lowest responses were seen for the B strain. Patients who were not seroprotected at baseline had a greater GMFR in antibody titer. This was true for both influenza A strains, H1N1 (1.68 vs. 4.30; p = 0.004) and H3N2 (1.29 vs. 2.80; p = 0.02), as well as influenza B (1.14 vs. 1.91; p = 0.012).
Humoral Responses in Subgroup of Patients Who Were Not Seroprotected Prior to Immunization

p < 0.001 for all comparisons. GMT, geometric mean titer; GMFR, geometric mean fold rise.
Patients who were not protected at baseline were more likely to seroconvert to vaccine antigens. For H1N1, 7/32 (21.9%) with baseline seroprotection converted, whereas 14/29 (48.3%) without baseline seroprotection had a fourfold rise, p = 0.03. For H3N2, 6/30 (20%) with baseline protection seroconverted, whereas 12/31 (38.7%) naive at baseline seroconverted, p = 0.11.
We also analyzed whether any variables affected seroprotection and seroconversion rates to each strain for patients not previously seroprotected. These variables included age ≥60 years, time from transplant (<1 or ≥1 year), type of induction immunosuppression, and MMF daily dose (≥2 or <2 g). No patient within 1 year of transplant seroconverted with B strain (p = 0.55) and none aged ≥60 seroconverted with B strain (p = 0.10), although these were not statistically significant. The remaining variables did not significantly affect seroprotection or seroconversion.
Vaccine Safety
Safety data were available in 60/61 patients. Local adverse events occurred as follows: injection site tenderness in 17 (28.3%), induration in 13 (21.7%), erythema in 6 (10%) of 60 patients. Systemic reactions included fatigue in 12 (20%) and gastrointestinal effects in 2 (3.3%) of 60 patients. No patient had a febrile reaction. All the side effects related were of mild intensity. Two patients underwent repeat islet transplant within the follow-up period.
Discussion
Since influenza vaccination is recommended for all transplant recipients, it is important to have clear data on the efficacy and safety of such an intervention. Our study is the first to report on the immunogenicity of influenza vaccine in the allogeneic pancreatic islet transplant population. We evaluated the immunogenicity of trivalent seasonal vaccine in a cohort of islet transplant recipients and showed suboptimal responses in this population. This was especially true for the influenza B strain in the vaccine (seroconversion rate 9.8%) but also for the two other strains [seroconversion 29.5% and 34.4% for influenza H1N1 (2009) and H3N2 strains, respectively]. The main factor predictive of seroconversion to at least one vaccine antigen was time after transplant. Patients within 1 year of their most recent islet transplant responded poorly to vaccine. Older age was also a significant factor in strain-specific seroprotection and seroconversion. In addition, patients not already seroprotected prior to immunization had greater rises in antibody titer than those already seroprotected. We found that the vaccine was well tolerated in the cohort with minimal systemic adverse events.
Seroprotection and seroconversion are factors used to annually license influenza vaccines. In general, seroconversion is a more stringent criterion for licensure, since it takes baseline antibody titer into consideration. Although we used the standard definition of seroprotection (titer ≥1:40) in our study, the true titer that confers protection in transplant patients is unknown. The requirement for EMEA and FDA for yearly licensure of influenza vaccine in those 18–60 years of age is a seroprotection rate of >70%, seroconversion rate of >40%, and seroconversion factor >2.5 (7). Each antigen must meet at least one of these criteria. For Fluviral, pooled immunogenicity data in the healthy 18–60 years population over three seasons (2004–2007) show a seroprotection rate of 71–97% and a seroconversion rate of 64–79% (Fluviral product monograph) (9). In contrast, seroconversion rates in this study were 9.8%, 29.5%, and 34.4% for influenza B, H3N2, and H1N1, respectively. In studies on the healthy population, the geometric mean fold rise ranged from 6.8–13.8 compared to 1.46–2.63 in our study. In those with no prior seroprotection, the seroconversion rates ranged from only 13.8% to 48.3%, and seroprotection after vaccination ranged from 34.5% to 58.6%.
As noted above, there are no previously published data on vaccine immunogenicity in islet transplant recipients. Previous data in solid organ transplant recipients have indicated response rates of 15–93%, depending on several factors including the organ studied, time from transplant, and use of certain immunosuppressives (12). Previous studies have shown diminished responses in patients receiving mycophenolate mofetil (MMF) (11,18,21). One study found a 2.6- to 5-fold reduction in seroconversion in those receiving more than 2 g daily of MMF versus no MMF (19). Although most of our patients were receiving MMF, we did not find a difference in seroprotection or seroconversion rates for those receiving more than 1 g daily versus less than 2 g. There are little data on the role of different induction regimens and their effect on vaccine response. We previously conducted immunogenicity studies of influenza vaccine in two cohorts of lung transplant recipients (16,17). Responses to one dose of influenza vaccine in the 2007 cohort were significantly better than those in the 2011 cohort. This may have been partly due to the fact that only 30% of patients received any induction therapy in the 2007 cohort whereas 89% received induction in the 2011 cohort. However, maintenance immunosuppression was also different in the two studies (primarily calcineurin-inhibitor/azathioprine in the 2007 cohort and MMF/tacrolimus in the 2011 cohort), making a post hoc comparison difficult. The current study is novel in that provides a direct comparison of vaccine responses using three main induction strategies: IL-2 receptor antagonist, antithymocyte globulin, and alemtuzumab. Our study found significantly lower GMFR for H1N1 strain in those that received alemtuzumab and a trend to lower seroconversion for this strain.
We also addressed timing of influenza vaccine. Current guidelines by the American Society of Transplantation recommend that influenza vaccine be given starting at 3–6 months posttransplant; however, data on vaccine immunogenicity in the early posttransplant period are limited. Studies in organ transplant recipients have been conflicting with one study not demonstrating any difference in response based on time from transplant (3); however, more recently, Birdwell et al. showed diminished responses in kidney transplant recipients who received vaccine at less than 6 months posttransplant (2). Consistent with this observation, our study also showed a diminished seroconversion to at least one vaccine antigen when vaccine was administered within the first year post-transplant (23.5% vs. 54.5%, p = 0.029). We believe that the reason time from transplant is significant is in fact due to the degree of immunosuppression. Specifically, induction therapy likely has a prolonged immunological effect. For example, in a study of islet transplant patients, this effect was recently shown with CMV reactivation in patients receiving induction therapy (8).
Preimmunization vaccine titer was also an important predictor of the response to vaccination. Almost half the cohort had a strain-specific titer ≥1:40 prior to vaccination, and this group was less likely to have a significant response to vaccination. High baseline seroprotection rates lead to difficulty in analysis of vaccine response and have led to the use of the additional criteria of seroconversion rate and seroconversion factor (1,23). Therefore, we performed a separate analysis of the subgroup that was not protected prior to vaccination. Other studies of influenza vaccination in the organ transplant population have also found high baseline seroprotection rates, where up to 78% of subjects are already seroprotected prior to vaccination (19). Baseline seroprotection was also found to be a significant factor for vaccine response in another study of organ transplant recipients, where patients whose preimmunization titer was ≥1:40 had significantly less seroconversion (p < 0.001) (3).
Limitations of our study include the lack of a healthy control group; despite this, we are able to compare our responses to immunogenicity data gathered from healthy volunteers for this vaccine preparation over several seasons and to standards set by the EMEA and FDA for seroresponses to influenza vaccine in healthy individuals. Although we did not compare our responses to patients with type 1 diabetes, previously published studies have reported seroconversion responses up to 84% in this group comparable to that reported for healthy controls (9,24). It is also possible that differences in the effect of induction would have been better defined with larger number of patients in each group. However, the overall number of islet transplantation procedures remains relatively small worldwide, and we were able to enroll approximately half of the patients actively followed at our center. We did not determine the cellular immune response to influenza, which may differ from the humoral response; however, it has been proposed that neutralizing antibody is most important in prevention of infection (5).
In summary, this is the first study to evaluate influenza vaccine immunogenicity in islet transplant patients. We showed suboptimal responses to all three strains of virus contained in the 2010–2011 influenza vaccine. These responses were dependent on time posttransplant and baseline seroprotection. Vaccine was well tolerated and should continue to be recommended for these vulnerable patients. However, given the poor responses early post-transplant, additional measures to reduce influenza infection would include emphasis on hand hygiene as well as immunization of health care workers and close contacts.
Footnotes
Acknowledgments
M.S. was supported by Hospital Israelita Albert Einstein, Sao Paulo, Brazil. We are grateful to Lana Toth, Vali Toth, and Shauna McRae for their assistance in data collection. We also thank George Huang for technical assistance. The authors have the following conflicts of interest: D.K. has received research support from Sanofi-Pasteur and Hoffmann-LaRoche. A.H. has received research support paid to the institution from Hoffman-LaRoche. A.M.J.S. is supported through an Alberta Innovates Healthcare Solutions (AIHS) Senior Clinical Scholarship, through grant support from the National Institutes of Health (NIH) Clinical Islet Transplant Consortium (CIT), and from the Juvenile Diabetes Research Foundation (JDRF). K.H. has been investigator of clinical trials sponsored by Novartis, Baxter, Sanofi-Pasteur and CSL Australia Ltd. K.H. has been sponsored by Sanofi-Pasteur to take part and speak at one international meeting. The remaining authors have no relevant conflict of interest.
