Abstract
The concept of wellness incorporates many domains, including mental, physical, social, and integrated well-being. However, it is not well understood in most lower middle-income countries (LMIC). The significance of practicing wellness during residency, focusing on the context of LMIC, is described here. Based on the authors’ experiences of working in LMIC, the challenges faced during residency and the importance of prioritizing self-care and well-being is highlighted. Physician burnout is a global concern having a negative impact on patient care quality, patient satisfaction, and professionalism. Interventions to address wellness can be individual and organization-based. Individual interventions include mindfulness training, behavioral interventions, self-care practices, and support networks. Organizational interventions involve the establishment of wellness committees, introduction of wellness curricula, optimization of workflows, and creation of shared social spaces. There is a need for implementing wellness practices within residency programs in LMIC. By focusing on wellness, physicians can mitigate burnout, enhance their well-being, and improve patient care outcomes.
Introduction
Wellness is not a new concept. An article titled “Health of Residents,” published in The Hospital in 1907, emphasized the importance of taking time for oneself during residency, good sleep and taking time to enjoy leisure activities [1]. The authors concluded that, “We have now outlined the house surgeon’s duty towards himself, and we would conclude by reminding him that without due attention to his own health, he will sooner or later be unable to perform his duty towards his patients” [1]. Fast forward to 2023, and residency programs in many parts of the world are still struggling to inculcate wellness during residency, resulting in increased prevalence of burnout in low and lower middle income countries (LIC/LMIC) [2].
In a survey conducted by Malik et al. among residents of public hospitals of Pakistan, 57.9% of the residents reported burnout [2]. It was alarming that only 5% of residents with burnout sought professional help to deal with this issue [2]. Moradi et al., in a systematic review, documented that 44% of residents of obstetrics and gynecology had burnout [3], and Ogboghodo et al. reported 41.7% of residents in Nigeria had burnout [4]. It is interesting to note that, while all these studies point out the prevalence of burnout, none commented on the practice of wellness to combat burnout [2–4].
MTK (the lead author), a third year resident in a Physical Medicine and Rehabilitation program in Pakistan, shared his experience of residency as follows:
“I joined the specialty of my choice three years back. I got the specialty that I love, the specialty in which I could see myself evolving and spending the rest of my life in. It was ‘Love at first sight’. I was a motivated person, with the belief that I could face all the troubles of residency with firmness and dedication towards my goal. I was soon to be proven wrong. Three years in, I have suffered through two nights where I was about to harm myself, had multiple episodes of panic attacks, several crying sessions in the hospital parking lot, lost my dream team with which I initially thought to keep forever in touch and work to advance our specialty. I was not this person before my residency.
Residency is challenging. I was well aware of the challenges that I might face during my residency, but I had not appropriately judged the value of practicing wellness while I was daily exposed to various types of physical, mental, emotional and social challenges. During residency training, we spend most of our time in hospital, struggle to get decent sleep of six hours and try to juggle time for our family and friends. It is easy to forget oneself in all this.”
While wellness is not a new concept, it is not widely implemented in residency programs in LMIC. The residency and fellowship programs in Pakistan are not bound to address wellness as part of program requirements in residency. However, in higher income countries like America, burnout is assessed and institutions are required to provide resources to address wellness as an employee benefit [5]. The Accreditation Council for Graduate Medical Education addresses wellness as part of program requirements for residency and fellowship training programs [5]. The aim of this manuscript is to define wellness, describe its domains and highlight some of the interventions that are available in the literature to implement wellness in residency programs in LMIC.
Definition
In a recent systematic review by Brady et al., only 11 out of a total of 78 included studies explicitly defined wellness [6]. This presents a challenge. How can a concept be practiced without clearly defining its domains? Brady et al. defined physician wellness as “a multifaceted construct that includes
Importance of wellness
Lack of physician wellness is a global phenomenon [6]. According to some estimates, 20-50% of physicians report ‘burnout,’ which is a negative wellness indicator in physicians [6]. Burnout is characterized as a triad of physician exhaustion, depersonalization, and low sense of personal accomplishment [8]. Physician burnout affects patients’ quality of care, increases the risk for patient-related safety incidents, reduces patient satisfaction, and leads to low professionalism among doctors [9]. From 2010 to 2019, suicide-related deaths were reported among 105 residents and 126 physicians [10]. Female residents had a higher risk of suicide-related deaths [10]. In the United states, approximately 119 physician suicides occur annually [11]. It is important to improve physician wellness to mitigate physician burnout [9].
Domains of wellness
Wellness has been divided into four domains (Fig. 1):
Domains of wellness.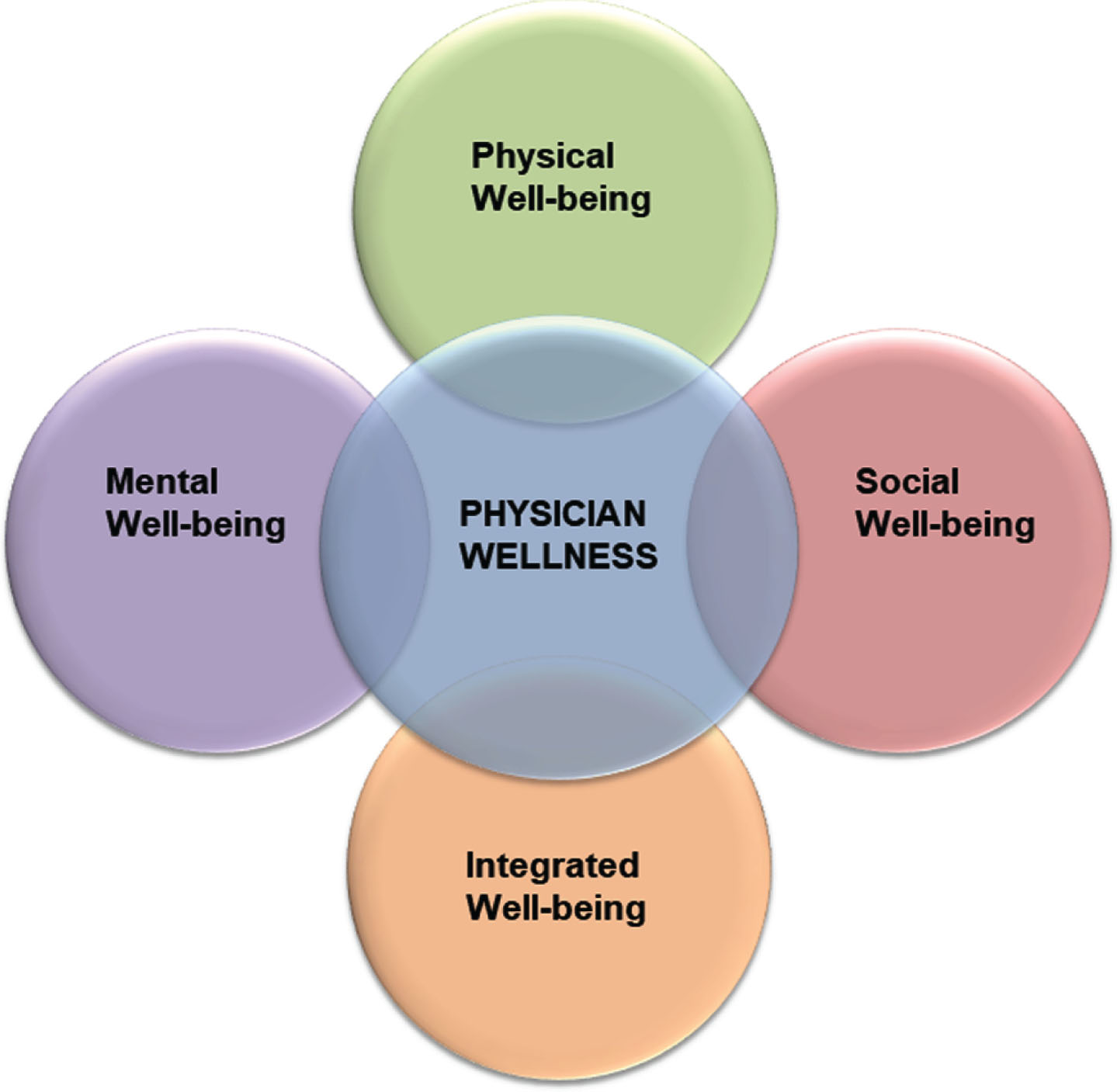
Interventions for wellness can be categorized into individual and organization based interventions that are directed towards incorporating the culture of wellness among residents. The following evidence-based interventions for wellness are being implemented in higher income countries, but these can be implemented in LMIC as well, owing to their universal nature.
Individual interventions
Having a strong
Organization-based interventions
For a residency program in LMIC trying to implement wellness initiatives, individual interventions like self-care and mindfulness should be prioritized. These interventions are financially resource-savvy, and residents can be taught to practice these interventions via workshops or group discussions. Out of the organizational interventions mentioned, optimization of workflows, residents’ schedules, and creation of wellness committees may be prioritized. The set of interventions mentioned above may be implemented as is, or may serve as a framework for residency programs in LMIC to implement wellness interventions as per their own requirements. These interventions can serve as a starting point for residency programs in LMIC.
Barriers for implementation of wellness programs
Addressing physician wellness in LMIC faces various challenges, and it is essential to recognize and overcome these barriers to promote a healthier work environment for residents.
Overcoming these barriers requires a collaborative effort from various stakeholders, including medical institutions, regulatory bodies, government authorities, and senior faculty members. Initiatives aimed at destigmatizing mental health, advocating for the inclusion of physician wellness in residency training, and allocating adequate resources for wellness programs are crucial steps to ensure the well-being and resilience of residents in LMIC. Moreover, fostering a cultural shift that emphasizes the importance of physician well-being and acknowledges the link between healthy physicians and improved patient care will create a more supportive and thriving environment for healthcare professionals. By addressing these barriers, LMIC can move towards fostering a culture of wellness in residency, ultimately benefiting the overall health system and the communities they serve.
Conclusion
The incorporation of wellness practices into residency programs within LMIC is of paramount importance. Implementing individual-centered interventions such as practicing self-care, mindfulness, and fostering a supportive network can significantly enhance wellness, even in resource-constrained settings. Prioritizing wellness not only helps physicians combat burnout but also uplifts their overall well-being, leading to improved patient care outcomes. Within advocacy for the advancement of medical education and training, it is imperative to underscore the integral role of wellness in nurturing resilient, compassionate, and effective healthcare professionals. By fostering a culture of wellness, LMIC can empower their resident physicians to thrive, thereby fortifying the foundation of their healthcare systems and ensuring the delivery of optimal care to their communities.
Footnotes
Acknowledgments
None.
Conflict of interest
The authors have no conflicts of interest to report.
Ethical considerations
This study, as a commentary, is exempt from Institutional Review board approval.
Funding
None.
