Abstract
BACKGROUND:
Tissue flossing is a new method aiming to improving range of motion (ROM), pain, and enhancing injury prevention. Tissue flossing involves passive twisting and active movement with the muscle or joint tightly wrapped with a floss band. However, evidence is lacking regarding the effects of flossing.
OBJECTIVE:
To compare the effects of flossing and static stretching (SS) on gastrocnemius (GC) function.
METHODS:
Twenty healthy young men received three interventions (Flossing, SS, Rest). The experimental intervention involved flossing using a floss band (Sanctband COMPRE Floss
RESULTS:
The pre-post changes in RFD 0–50 and RFD 0–100 ms were significantly higher with Flossing compared to SS. The pre-post changes in dorsiflexion ROM was significantly higher with Flossing compared to Rest.
CONCLUSIONS:
Flossing on GC improved RFD 0–50 and RFD 0–100 ms with an increase in dorsiflexion ROM unlike SS. Research is warranted whether flossing before exercise may be more beneficial than SS for injury prevention and physical performance enhancement.
Introduction
Tissue flossing is a relatively simple bandage technique aiming to improve range of motion (ROM), relieve pain, and recover fatigue. Tissue flossing is performed by wrapping a floss band around a joint or muscle to partially obstruct the blood flow to the area while simultaneously performing ROM tasks for 1–3 min [1, 2]. This technique was popularized by the book written by Starrett and Cordoza [3], which proposed that the mechanisms behind flossing include fascial shearing and occlusion of blood to the muscle. However, few research articles support the mechanisms behind the effectiveness of flossing.
Tissue flossing is widely performed among athletes for rehabilitation purposes because of its empirically felt effects in alleviating muscle pain and improving muscle function [4], although current evidence is limited. A crossover trial suggested that flossing to either ankle joint might increase ankle ROM and single-leg jump height and velocity in 52 recreational athletes [1]. Subsequently, a parallel group-trial revealed the effects of flossing to both ankles on countermovement jump and sprint time which lasted for 45 min [2]. However, another crossover trial suggested limited support for the use of tissue flossing for improved ankle ROM, countermovement jump, and sprinting performance, up to 30 minutes post-application in elite rugby union athletes [5].
So far, no evidence of improvement in muscle function, including muscle exertion and flexibility, has been associated with flossing. Reduced ankle dorsiflexion ROM has been identified as risk factor for patellar tendinopathy, anterior cruciate ligament (ACL) injury, and other lower limb injuries in athletes [6]. Dorsiflexion ROM is known to be improved by static stretching (SS) [7, 8] which is therefore commonly performed prior to sports activity [9]. Meanwhile, conducting SS before exercise has a disadvantage of decreasing maximal isometric voluntary plantar flexion contraction (MVC), rate of force development (RFD), and physical performance [10]. Therefore, flossing, useful in improving ankle ROM and single-leg jump height and velocity, might overcome the disadvantage of SS [1]. In addition, to establish an effective new method of preventing injuries in athletes, it is crucial to examine the effects of flossing on the function of the gastrocnemius muscle (GC).
This study aimed to examine the effects of flossing on the GC exertion and flexibility in comparison with those of SS, which is generally performed for injury prevention before and after exercise.
Materials and methods
Participants
Twenty healthy young recreational male athletes (mean
Study procedure and measurements
This study was a non-randomized trial in a 2 (time)
Active dorsiflexion ROM
The participants laid supine with their knees in full extension and they were asked to actively dorsiflex their ankles to the point of limitation. Body markers were attached to the fibular head, lateral malleolus, fifth metatarsal bone head, and the bottom of the fifth metatarsal bone of the non-dominant leg. The lower leg and foot, with the ankle maximally dorsiflexed, was photographed from the same height and parallel with the lower leg of the participants. The obtained image was calculated using image analysis software (Image J ver 1.46r, NIH) to calculate the dorsiflexion ROM.
Passive moment
The “GC-relaxed position” was defined as a position of the ankle joint at an angle where the GC was relaxed. Participants were placed in a prone position while seating with an attached isokinetic machine (Cybex Norm, Medica Co., Ltd. Japan) with their knees extended. The non-dominant foot was fixed to the footplate and stabilized with inelastic straps to avoid compensatory movements. The footplate of the dynamometer of the isokinetic dynamometer was passively dorsiflexed at a constant velocity of 15
Fascicle length
The participants were laid in a prone position with the muscle in a relaxed state. Longitudinal images of the muscle belly of the medial head of the GC were obtained by B-mode ultrasonography (HI VISION Avius; Hitachi Aloka Medical Japan, Tokyo, Japan) using a high-resolution linear probe of 8.0 MHz (EUP-L65; Hitachi Aloka Medical Japan). A fascicle length of the medial head of the GC was estimated, using image J, through an analysis of each image, and an average of the two estimates was recorded. The fascicle length was determined as the length of the fascicular path between the superficial and deep aponeurosis. The outlined fascicle between the aponeuroses was reported in absolute terms (mm). As the entire fascicles were not visible in the probe’s field of view, lengths were estimated using the following equation [13]:
Fascicle length
where “visible fascicle length” represents the length of fascicle visible in the sonographic image. “h” represents the distance between the intersection point of the end of the visible fascicle and the edge of the image and the deep aponeurosis of the medial head of the GC. The “pennation angle” represents the angle between the fascicle and its superficial aponeurosis.
Muscle hardness
Muscle hardness is defined as the resistance offered by the muscle against a perpendicular pressure [14]. The participants were laid in a prone position with their muscles in a relaxed state. Axial B-mode and real-time tissue elastography (RTE) images of the medial head of the GC were obtained by manually applying light repetitive compression (rhythmic compression-relaxation cycle) using ultrasonography with a 14–16 MHz line array transducer. The elasticity of the acoustic coupler was 22.6 kPa according to the manufacturer’s specification. A reference material for elasticity was placed between the skin and the transducer by using a stabilizer (attachment of the acoustic coupler for L65; Hitachi Medical Corporation). The RTE enabled semi-quantitative evaluation of the hardness of the medial head of the GC by calculating the muscle/reference ratio. In response to the compression force, the strain value assessed by RTE is physically lower in harder tissue than in softer tissue. Therefore, as the muscle becomes harder, the strain ratio (the strain of the medial head of the GC divided by that of the reference material) decreases [15]. The RTE measurements were performed in triplicate, and the mean value of the strain ratio for each set of measurements was calculated.
MVC and RFD
Participants laid prone position on a seating with an attached the isokinetic machine with the non-dominant knee extended and with the foot firmly fixed to the footplate at the ankle neutral position. MVC maintained for 5 seconds with the instruction “as fast and strongly as possible,” was measured twice with a 1-minute rest between the 2 measurements. RFD reflects the ability to rapidly increase muscle force after the onset of an explosive voluntary contraction [16, 17]. RFD was determined as the slope of the moment-time curve over time intervals of 0–50 ms, 0–100 ms, 0–150 ms, and 0–200 ms relative to the onset of muscle contraction during the MVC test. The onset of muscle contraction was defined as the time point at which the moment curve exceeded the baseline moment by 2.5% of the MVC [18]. The average of the 2 values was used as the measurement value in MVC and RFD.
EMG
Muscle activity was measured during the measurement of passive moment and MVC using an EMG system (BioLog DL-4000, DKH, Co. Tokyo, Japan). Surface electrodes (DL-141, DKH, Co. Tokyo, Japan) were placed over the belly of the lateral head of the GC (20 mm inter-electrode distance) according to SENIAM guidelines [19]. The relaxation during passive moment, defined as the EMG activity of the GC, was
Intervention
Flossing was performed with the floss band in accordance with the following procedure on which the clinician was instructed by a qualified person on “Easy Flossing Instructor Course Levels 1–6”. The participants placed their non-dominant leg forward in the standing position. Then, a part just above the medial malleolus was wrapped around with the floss band not stretched tightly as an anchor. With maintained tension when the band was stretched to 1.5 times its natural length, the clinician wrapped the lower leg from above the medial malleolus to the patella with 50% overlapping of the previous part of the band (Fig. 1). Passive twisting of the wrapped part four times and active ankle plantar flexion and dorsiflexion movement twenty times were performed in the lower leg, and then the band was removed. This process was performed within 2 minutes and repeated once more with a break for 2 minutes. The interface pressure between the skin and the floss band was measured to assess the level of compression (mmHg) achieved by the wrapping technique. A probe of a contact pressure measuring device (AMI-3037–SB–SET AMI Techno Co., Ltd. Japan) was placed on the anterior aspect of the tibia on the midline between the lateral and medial malleolus [2]. The mean pressure (
Flossing on the GC using the floss band.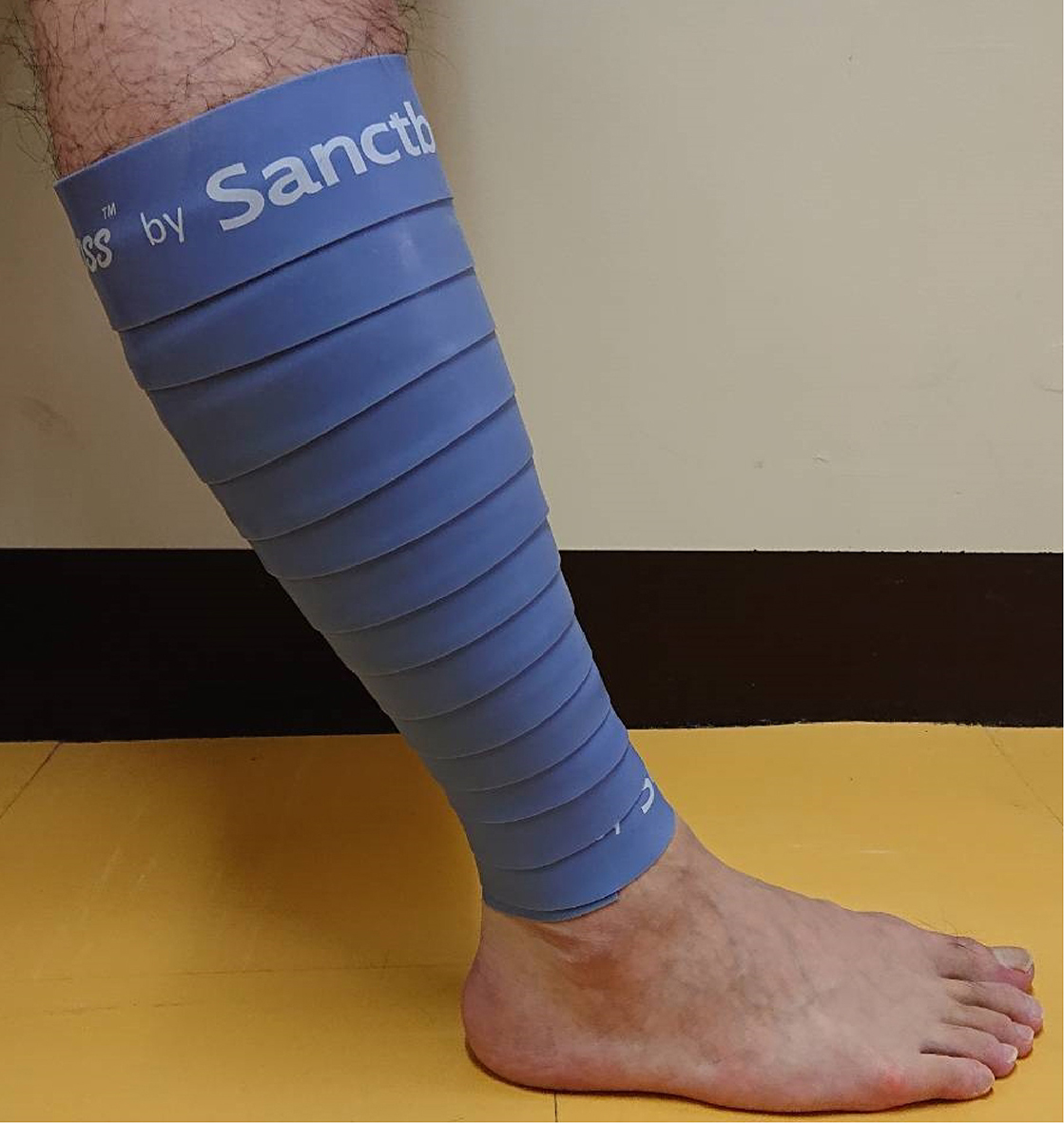
Static stretching was undertaken using the dynamometer of Cybex. Participants were positioned prone on the seating of an isokinetic machine, with the knee extended and the foot of the non-dominant leg attached securely to the footplate. The ankle which was fixed securely to the footplate was passively dorsiflexed by the clinician at a velocity of 5
The control intervention rest involved the participants assuming a relaxed supine position on the seating of an isokinetic machine for 6 minutes.
A pre-post change was obtained by subtracting the pre-value from the post-value. The within-intervention change in the outcome in three interventions was assessed using a paired
Results
Table 1 shows the demographic characteristics of the study participants. All participants were male and determined to be left leg non-dominant. No participants dropped out or were excluded from the study. No adverse or musculoskeletal events due to the flossing were reported. The EMG activity of the GC during passive moment was
Demographic characteristics of participants (
20, all male)
Demographic characteristics of participants (
SD, standard deviation; BMI, body mass index.
ICC
ICC, intraclass correlation coefficient; CI, confidence interval; ROM, range of motion.
ICC
ICC, intraclass correlation coefficient; CI, confidence interval; MVC, maximal isometric voluntary plantar flexion contractions; RFD, rate of force development.
Mean pre- and post-parameter values in Flossing, SS, and Rest
Table 4 shows the mean pre- and post-parameter values in Flossing, SS, and Rest. The dorsiflexion ROM, passive moment at end ROM, RFD 0–50 ms, and muscle activity were significantly higher after flossing than before flossing (
Differences between the pre-post changes among Flossing, SS, and Rest
Table 5 shows the differences between pre-post changes among Flossing, SS, and Rest. The ANCOVA revealed a significant main effect of the interventions on dorsiflexion ROM, RFD 0–50, RFD 0–100, RFD 0–150, and RFD 0–200 ms (
This is the first study to examine the effects of flossing on the GC exertion and flexibility in comparison with those of SS. The results showed that flossing was significantly associated with higher increases than SS in RFD 0–50 and RFD 0–100 ms. In addition, flossing showed significantly higher increases than Rest in dorsiflexion ROM and RFD 0–150 ms. Therefore, flossing on the GC before exercise could hypothetoically lead to better injury prevention and physical performance enhancement than SS.
A previous study reported that flossing on ankle joint increased dorsiflexion ROM, single-leg jump velocity [1]. The present study confirmed that flossing on the GC significantly enhanced dorsiflexion ROM when compared with Rest. Despite the differences in materials used for wrapping the floss band, the witnessed increase in dorsiflexion caused by flossing was consistent with the results of this study. Therefore, flossing may be useful both on the ankle joint and on the GC for improving the dorsiflexion ROM. Furthermore, flossing on GC significantly enhanced RFD 0–50 and RFD 0–100 ms when compared to SS. By contrast, SS on the GC enhanced the dorsiflexion ROM with a decrease in RFD 0–150 ms when compared with Rest, similarly to previous studies [12, 20, 22, 23]. Thus, we found that flossing and SS resulted in different outcomes in muscle exertion, although both improved dorsiflexion ROM. These results could provide useful information for establishing a new method that can potentially prevent injury before exercise and enhance physical performance.
The exact physiological mechanism of flossing has not been determined yet. However, with regard to the mechanisms of muscle exertion and flexibility by flossing, the mechanisms behind flossing, as proposed by Starrett and Cordoza [3], include fascial shearing and obstruction of blood to the muscle. The fascia comprises multiple fibrous layers and collagenous connective tissue that surround and interpenetrate the skeletal muscle, joints, organs, nerves, and vascular beds [24, 25, 26]. The smooth slide between the layers of fluid fascia allows muscles to contract or elongate [27, 28]. The fascia changes from a solid gel-like state to a fluid sol-like state in accordance with a decrease in fascial viscoelasticity when energy, in the form of heat or mechanical pressure (i.e., thixotropy), is applied to it [29]. A floss band provides intense mechanical pressure on the muscle, covering the limb from all directions in close contact with the skin. Twisting of the wrapped part affects deep fascia under tight compression to the upper tissues by the floss band. Muscle compression retains heat associated with the increase in intramuscular pressure and, therefore, muscle contraction under compression, which might produces heat that decrease fascial viscoelasticity [30]. Therefore, it is assumed that heat or mechanical pressure caused by flossing might allow muscles to easily elongate through decreasing fascial viscoelasticity. In addition, the factor of improved dorsiflexion ROM by flossing might include stretch tolerance, which is associated with pain threshold, was reported to increase with the auGCentation of the dorsiflexion ROM and passive moment at end ROM after SS [12, 31]. The present results of increased dorsiflexion ROM and passive moment at end ROM by flossing suggest that flossing might increase stretch tolerance. Transmission of the force caused by skin stretch may activate subcutaneous mechanoreceptors and modulate pain perception [32]. Thus, skin stretch caused by tension of flossing might activate subcutaneous mechanoreceptors and increase stretch tolerance. Furthermore, compression is likely to activate both cutaneous and muscle mechanoreceptors, which could modulate sensory feedback transmission and improve muscle power output [33, 34]. When muscle temperature rises due to an increase of blood circulation, the activation of metabolic activity and decreased fascial viscoelasticity render contraction smoother and increase muscle contraction rate, which might lead to an increase in RFD [35]. The key difference between Flossing and SS is the difference of Flossing involved in muscle compression or SS involved in muscle stretching. SS increase ROM by modifying muscle-tendon stiffness and stretch tolerance [10, 23, 36]. In addition, SS decreases acute MVC, RFD, and physical performance by stretch-induced strength deficit, mechanical factors such as changes in muscle stiffness, and neuromuscular factors such as altered reflex sensitivity [37]. The present result involving muscle exertion without decreasing passive moment by SS could suggest that SS involved neuromuscular factors. These findings could prove to be the key to elucidating the mechanism of the effects of flossing.
This study had several limitations. First, the participants of the present study were healthy young adult men. Meanwhile, flossing is typically used among athletes [1]. Athletes, especially professionals, might show changes in physical function with flossing that are different from the present results. Second, this study was a non-randomized trial. Thus, absent randomization might have caused systematic errors. Third, this study did not measure physiological parameters for the mechanisms of flossing. The physiological mechanisms of flossing are considered to include reducing the fascial viscoelasticity and activating the nerve receptors within fascia [3]. Finally, this study did not measure pain and fatigue indexes because we aimed to examine the effects of flossing on muscle exertion and flexibility of GC. Flossing is used not only for improvement of flexibility but also for pain relief and fatigue recovery [2]. Thus, further studies are required to measure pain, fatigue index, and the physio- logical mechanisms of flossing, such as fascial viscoelasticity and neural factors, in athletes.
Conclusions
We demonstrated that flossing on the GC significantly increased RFD 0–50 and RFD 0–100 ms than SS, and significantly caused a higher dorsiflexion ROM than Rest. Therefore, the results of this study revealed that flossing on the GC enhanced RFD 0–50 and RFD 0–100 ms with an increase in dorsiflexion ROM, unlike SS. These results might provide useful information for establishing a new method that can prevent injury before exercise and enhance physical performance. Therefore, these findings show that flossing before exercise may contribute to injury prevention and physical performance enhancement than SS. In addition, knowledge about whether flossing can affect ROM increases or muscle exertion could provide useful information to coaches, an athletes and the rehabilitation staff when prescribing flossing.
Footnotes
Conflict of interest
The authors declare no conflicts of interest.
