Abstract
BACKGROUND:
Despite progress in the treatment of oral squamous cell carcinoma (OSCC) over past years, the prognosis for OSCC patients remains dismal. MicroRNA-99a (miR-99a) has been found to involve in the development of many cancer types, but its clinical role in OSCC is unclear.
OBJECTIVE:
The aim of this study was to explore the clinical implications of serum miR-99a in OSCC.
METHODS:
This study detected serum miR-99a levels in 121 OSCC cases and 55 healthy controls by using quantitative reverse transcription polymerase chain reaction (qRT-PCR) analysis.
RESULTS:
The data showed that serum miR-99a expression was significantly decreased in OSCC patients compared with normal controls. OSCC patients with low miR-99a expression experienced more frequent poor differentiation and advanced clinical stage. Furthermore, in screening OSCC cases from normal controls, miR-99a could yield a receiver-operating characteristic (ROC) area under the curve (AUC) of 0.911 with 83.6% specificity and 80.2% sensitivity. Notably, patients with high miR-99a expression had longer overall survival and recurrence free survival. Finally, serum miR-99a was identified to be an independent prognostic indicator for OSCC.
CONCLUSIONS:
These results suggested that miR-99a might be a valuable marker for the prediction of early detection and prognosis in OSCC.
Introduction
Oral squamous cell carcinoma (OSCC) represents 90% of oral cancer is the sixth most prevalent human cancer around the world [1, 2]. In China, more than 11,900 cases are diagnosed with oral cancers and about 5,000 cases die of the malignancy every year [3]. Despite progress achieved in OSCC treatment, the overall survival rate has changed only marginally over the past decades, mainly because most of OSCC cases were detected at advanced stage [4, 5]. Screening and early recognition of OSCC are effective methods to improve patient survival and reduce the mortality rate of the disease. Thus, it is imperative to explore sensitive biomarkers to improve diagnostic efficiency in cases of OSCC.
Expression of serum miR-99a in subgroups divided by clinical characteristics in PTC patients
Expression of serum miR-99a in subgroups divided by clinical characteristics in PTC patients
MicroRNAs (miRNAs) are small, 18–25 nucleotides long, non-coding RNAs that regulate gene expression by targeting messenger RNA for translational repression or degradation. Dysregulated miRNAs were involved in cancer progression and multiple cellular process, such as proliferation, differentiation, apoptosis, migration and invasion [6, 7]. miRNAs have been demonstrated to be highly stable in clinical samples of plasma and serum [8]. The plasma/serum miRNAs were stable refrigerated or frozen for up to 72 h and were stable at room temperature for 24 h [9]. The stability of serum miRNAs enables them to become promising biomarkers for cancer diagnosis and prognosis prediction. Thus far, many circulating miRNAs acted as tumor growth promoters or suppressors in OSCC have been reported. For instance, miR-9, miR-375 and miR-214-3p were frequently decreased in OSCC, while miR-200b-3p was overexpressed in OSCC [10, 11, 12].
Recently, increasing evidences indicated that miR-99a, which is located at chromosome 21 (21q21.1), plays a critical role in various tumor types. MiR-99a was found to be downregulated in various cancers, including bladder cancer [18, 19, 20], breast cancer [21, 22, 23], anaplastic thyroid cancer [24], malignant pleural mesothelioma [25], renal cell carcinoma [26], glioma [27], osteosarcoma [28, 29], non-small cell lung cancer [30], hepatocellular carcinoma [31], whereas in other cancers such as gastric cancer [32], pediatric myeloid leukemia [33], miR-99a was upregulated. To better understand the role of miR-99a in OSCC, we evaluated the serum miR-99a expression in OSSC patients and further investigated its association with clinical variables and prognosis. To the best of our knowledge, our report for the first time explore the clinical significance of serum miR-99a in OSCC.
Serum samples
Our study enrolled 121 patients diagnosed with OSCC and 55 healthy individuals as controls. Patients who received any treatment before serum collection were excluded. Tumor stage was classified following the criteria of the American Joint Committee on Cancer (AJCC), seventh edition. Of all 121 cases, 73 males and 48 females; 75 subjects in stage I/II group, 46 subjects in stage III/IV group; 92 cases in G1/G2 grade group, 29 cases in G3 grade group. Histological grading was based on keratinization, nuclear pleomorphism, mitoses, pattern of invasion, stage of invasion, and lymphoplasmacytic infiltration. Overall survival (OS) was defined as the time from cancer onset until death or the last follow-up. Recurrence-free survival (RFS) was defined as the time from cancer onset until death or the first sign of progression or the last follow-up [13, 14]. The duration of follow-up was 5 years and all OSCC subjects were followed up completely. This study protocol was approved by Jinan Stomatological Hospital Ethics Committee and written informed consent was obtained from all participants. The clinical data of OSCC cases were summarized in Table 1.
RNA isolation and quantitative reverse transcription polymerase chain reaction (qRT-PCR)
Up to 5-ml blood was withdrawn from each participant. All blood samples were centrifuged at 3500 g for 5 min within 1 hour after collection, and then the serum was stored at
Total cellular RNA was extracted from serum samples with TRIzol LS reagent (Invitrogen, San Diego, CA, USA). RNA purity and concentration were determined on a NanoDrop ND-1000 spectrophotometer (Thermo Fisher Scientific, San Jose, CA, USA). A total of 100 ng RNA was reverse transcribed using the TaqMan MicroRNA Reverse Transcription Kit (Applied Biosystems, Foster City, CA, USA), followed by real-time PCR on a MyiQ Real-Time PCR Detection System (Bio-Rad, Richmond, CA, USA). The relative miR-99a expression was normalized with respect to cer-miR-39 using the 2
Statistical analyses
Statistical analyses were conducted with MedCalc 9.0 (MedCalc, Mariakerke, Belgium) and GraphPad Prism 5.0 (GraphPad Software, Inc., San Diego, CA, USA). As the data of the serum miR-99a levels was not subjected to normal distribution, Mann-Whitney U-test was used to compare the serum miR-99a levels between cancer patients and healthy controls Association of miR-99a expression with clinical features was analyzed by the Chi-square test. The diagnostic accuracy of serum miR-99a was generated using the receiver operating characteristic (ROC) curve. Survival curves were constructed using the Kaplan-Meier curves and the log-rank tests. The Cox hazard regression model was used to determine the prognostic factors for OSCC. For all tests,
(A) Reduced levels of serum miR-99a in OSCC compared to healthy control (HC). (B) Serum miR-99a expression in OSCC patients with G3 tumor grade was lower than those with G1/G2 tumor grade. (C) Serum miR-99a expression in OSCC patients with advanced TNM stage was decreased compared to those with early TNM stage.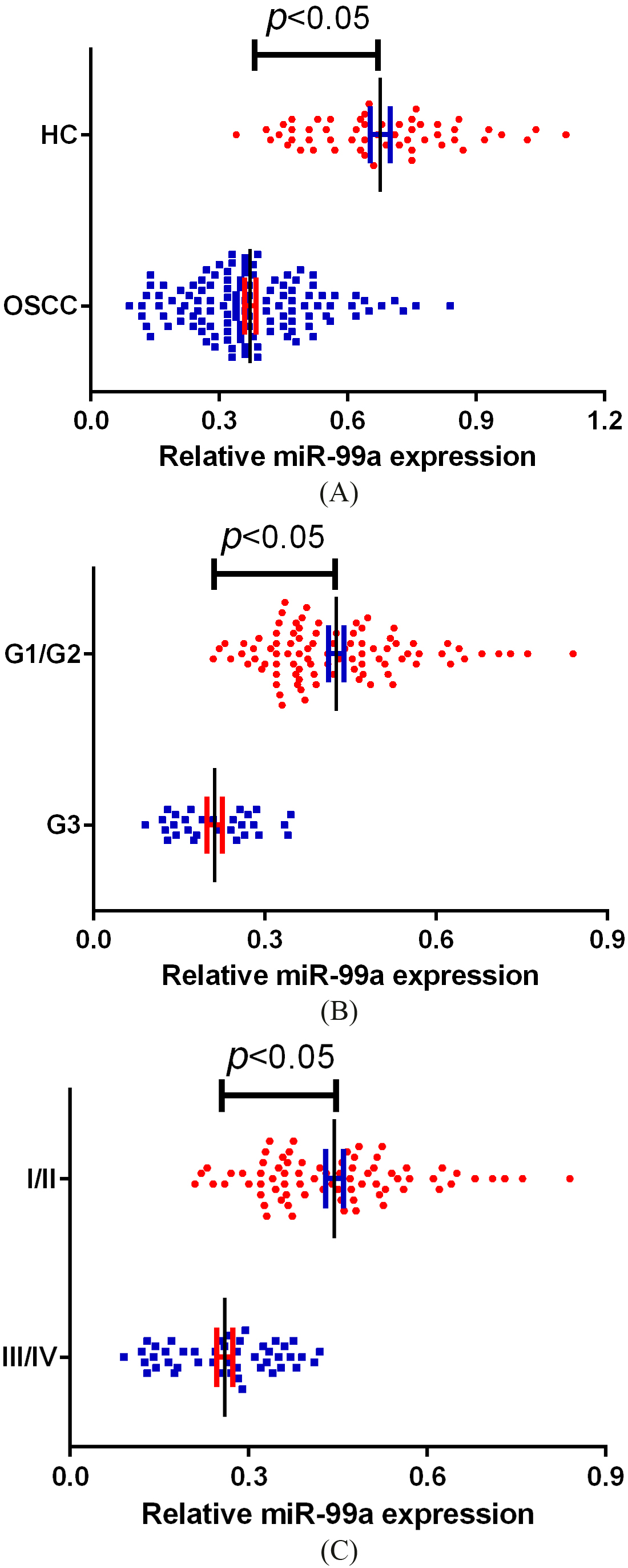
Serum miR-99a was significantly decreased in OSCC patients
Serum miR-99a levels in all participants were examined by using qRT-PCR, and the results revealed that miR-99a was dramatically reduced in OSCC patients compared to healthy controls (
Serum miR-99a as diagnosis signature for OSCC
Next, ROC curve analysis demonstrated that serum miR-99a had a specificity of 83.6% and a sensitivity of 80.2%, and with an area under the curve (AUC) of 0.911. The results indicating miR-99a could well screen OSCC patients from normal controls (
ROC curve analysis of serum miR-99a levels in OSCC detection.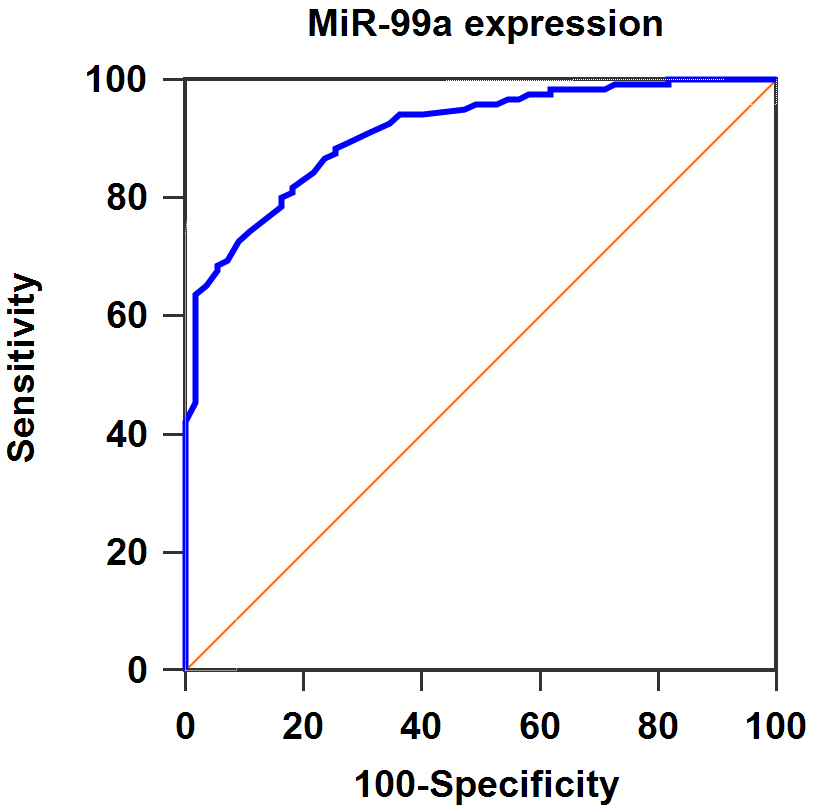
For 75 OSCC patients with I/II stage, serum miR-99a levels were greatly elevated after surgery.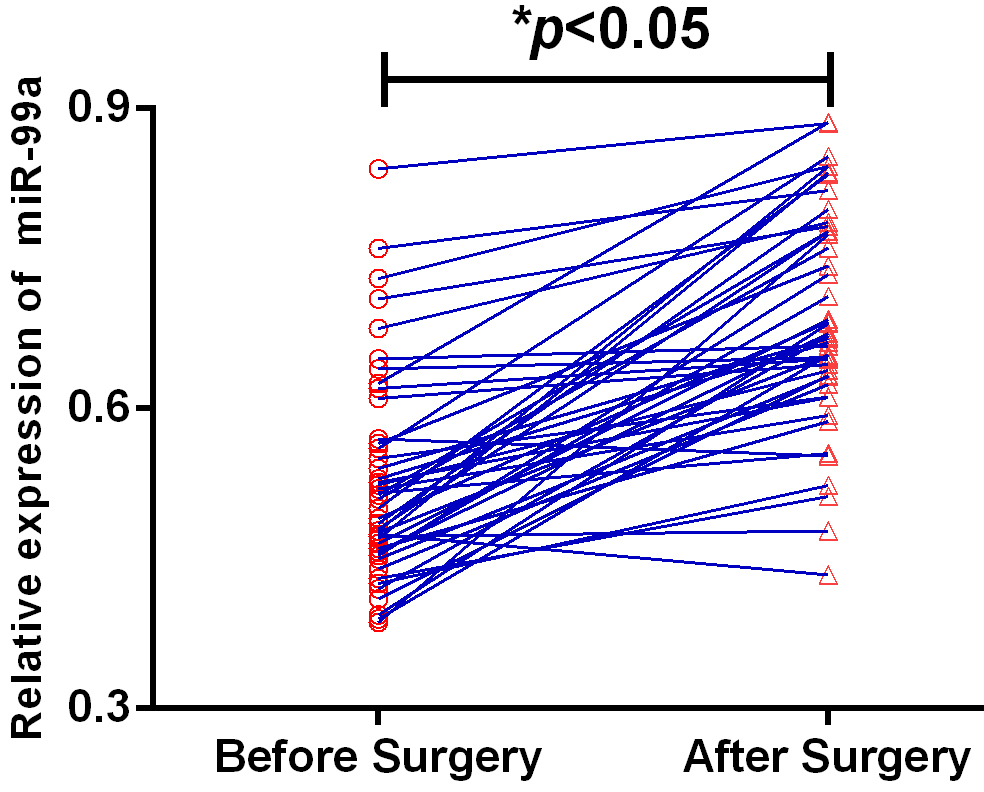
The median miR-99a expression level of all OSCC was utilized to divide the patients into two groups. Fifty eight cases belonged to the low expression group and the remaining 63 subjects were assigned to the high expression group. As illustrated in Table 1, miR-99a expression levels were strongly and negatively associated with tumor-node-metastasis (TNM) stage (
Dynamic changes in serum miR-99a of early stage patients with OSCC
Out of 121 OSCC cases, 75 patients were of stage I/II and their post-operative blood samples were obtained for qRT-PCR validation 40 days after surgery. Compared to pre-operative samples, the increase of the miR-99a in post-operative samples was significant with a
(A) Overall survival in 121 OSCC patients in relation to the miR-99a level. (B) Recurrence free survival in 121 OSCC patients in relation to the miR-99a level.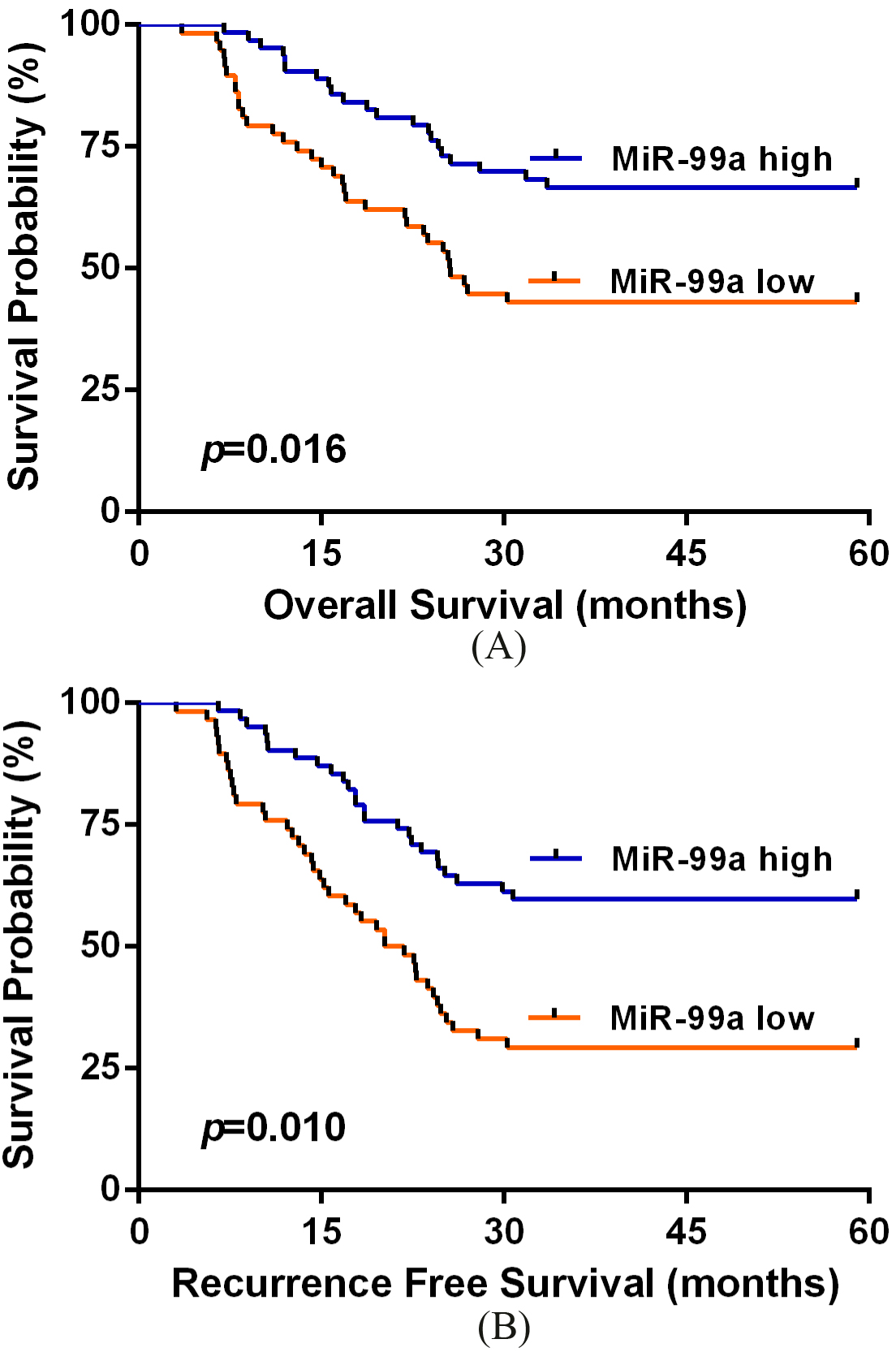
Univariate and multivariate analysis of 5-year overall survival in 121 OSCC patients
Abbreviations: CI, confidence interval; NS, not significant.
Univariate and multivariate analysis of 5-year recurrence free survival in 121 OSCC patients
Abbreviations: CI, confidence interval; NS, not significant.
Survival analysis was carried out to reveal whether miR-99a expression could predict OSCC prognosis. Patients in the high serum miR-99a expression group exhibited highly longer OS than those in low expression group (
Table 2 elucidated the findings of univariate and multivariate Cox hazard regression analysis for overall survival in OSCC patients. TNM stage (
Discussion
In the present study, serum miR-99a level was downregulated in the sera from OSCC patients, and its downregulation was closely associated with poor differentiation and advanced clinical stage. For T stage, although the
Importantly, miR-99a has also been found to be frequently decreased in various tumors. In bladder cancer, a reduction in miR-99a expression was observed in cancer tissues and negatively correlated with tumor aggressive phenotypes. Meanwhile, increased miR-99a expression significantly repressed cancer cell proliferation and invasion, and fibroblast growth factor receptor 3 (FGFR3) was identified as its downstream target [18, 19, 20]. In breast cancer, Wang et al showed miR-99a expression was downregulated in cancer tissues, and loss of miR-99a was strongly correlated with poorer prognosis [21]. Also, repression of miR-99a targets, including homeobox A1 (HOXA1) [21], mTOR [22] and IGF1R [23], markedly increased cell viability, motility and invasiveness. In anaplastic thyroid cancer, miR-99a inhibition promoted cell proliferation, while overexpression of miR-99a suppressed carcinogenesis in vivo [24]. Similarly, malignant pleural mesothelioma (MPM) patients with high miR-99a expression had significantly longer median overall survival than those with low expression, suggesting miR-99a exerted a tumor suppressive role in MPM [25]. In renal cell carcinoma (RCC), Cui and colleagues reported that miR-99a expression was remarkably downregulated in tumors and cell lines and provided in vitro and in vivo evidence to show miR-99a overexpression strongly inhibited the biological behaviors of RCC [26]. Moreover, decreased miR-99a expression was positively correlated with advanced tumor grade of glioma patients, and miR-99a underexpression resulted in the promotion of cancer cell migration and invasion [27]. Additionally, low miR-99a expression in osteosarcoma clinical samples was closely linked to worse prognosis, and upregulated miR-99a expression significantly attenuated the tumorigenic properties of osteosarcoma cells both in vitro and in vivo. TNF-α-inducible protein 8 (TNFAIP8) and mTOR were its regulatory targets [28, 29]. Moreover, reduced miR-99a levels were observed in non-small cell lung cancer tissues, and its downregulation greatly enhanced cancer cell migration and invasion via the IGF1R pathway [30]. In hepatocellular carcinoma, deregulated miR-99a was associated with reduced survival of patients, and miR-99a inhibition led to cell growth by inversely regulating IGF1R and mTOR [31].
More interestingly, several studies have demonstrated that miR-99a might function as an oncogene. For instance, miR-99a expression was increased in cisplatin resistant gastric cancer cells. Furthermore, overexpression of miR-99a significantly promoted cisplatin sensitivity of the resistant cells, indicating miR-99a acted as an oncogene in GC [32]. In pediatric myeloid leukemia, miR-99a was highly expressed in patients while dramatically decreased when they achieved complete remission. Moreover, reduced miR-99a expression significantly decreased cell proliferation and induced cell apoptosis [33]. Also, Si and colleagues verified that miR-99a overexpression was closely associated with dismal survival of acute myeloid leukemia patients. Enforced expression of miR-99a promoted the oncogenic activities of myeloid leukemia cells [34]. Therefore, the role of miR-99a in tumorigenesis might be dependent on the differences in tumor types and microenvironment.
Conclusion
Taken together, our study first demonstrated that serum miR-99a levels were significantly decreased in OSCC patients, and its downregulation was strongly associated with unfavorable prognosis. Therefore, serum miR-99a might serve as a promising biomarker for the diagnosis and prognostic prediction of OSCC, which might help assessment of disease activity and individualized therapy.
Footnotes
Conflict of interest
None.
