Abstract
BACKGROUND:
Adolescent idiopathic scoliosis (AIS), which is the most common type of scoliosis, is a progressive disease that occurs in children aged 10–16 years. Abnormal curvature in AIS provokes spinal asymmetry of the upper body alignment and might deteriorate postural balancing and control ability.
OBJECTIVE:
To evaluate the effect of exercise interventions on balance and postural stability in patients with adolescent idiopathic scoliosis.
METHODS:
Embase, Scopus, Pubmed (Medline) and Web of Science databases were searched using the terms idiopathic scoliosis, physiotherapy, and balance. The articles selected were published in English in peer-reviewed journals from 2012 to July 2022.
RESULTS:
Ten studies met the inclusion criteria. The PEDro scale values ranged from 2 to 6 (mean, 3.6), indicating a low level of scientific rigor. In the sample studies, spinal stabilization exercises were most often trialed (
CONCLUSIONS:
Physical therapists will be able to apply hippotherapy, Schroth exercise, physiotherapy scoliosis-specific exercise, trunk stabilization, proprioceptive neuromuscular facilitation exercise, spinal stabilization exercise, core stabilization exercise, and body awareness therapy to manage balance impairments in patients with adolescent idiopathic scoliosis, and further studies are needed to provide stronger evidence.
Introduction
Scoliosis is a type of structural three-dimensional spinal deformity accompanied by lateral deviation and abnormal sagittal curvature of the spine with a Cobb angle
However, the etiology of AIS remains unclear [3]. Genetic issues such as heredity, as well as endocrine, body mass, practice of high risk sports, and postural problems have been considered possible causes of AIS [3, 6, 7, 8]. Nutrients such as vitamin D, calcium, and melatonin had also been reported to occur and progress the symptom of AIS [9]. Furthermore, according to the neuro-osseous timing of maturation concept of Burwell et al., AIS patients have several abnormal growth factors [10]. AIS is usually regarded as pain-free; however, previous studies have revealed that AIS can produce negative effects on muscle imbalance, back pain, breathing dysfunction, and morphological problems [11, 12, 13, 14, 15]. In addition, the development of spinal deformities may lead to functional impairments and balance disorders [16, 17].
Abnormal curvature in AIS provokes spinal asymmetry of the upper body alignment and might deteriorate postural balancing and control ability [3]. Morphological deformity is closely related to the central nervous system, causing impairment of the sensory integrator process and a balance disorder of static stability [16]. However, some studies have shown that AIS patients do not have impaired postural balance when compared to healthy controls [18, 19], while several others have found an effect of AIS on postural balance [20, 21, 22]. Nault et al. reported that AIS patients showed increased sway area measured by enhanced anteroposterior center of pressure (COP) and center of mass compared with controls [23].
Scoliosis treatment options can be divided into surgical or conservative treatments, with the choice depending on the patient’s age, risk of disease progression, type of deformity, and quality of life [11, 24]. Among, conservative therapies, interventions such as brace, casting, specific scoliosis exercise, and core stabilization exercises have been used to alleviate pain, prevent curvature progression in AIS, and improve quality of life [2, 11]. In particular, therapeutic and specific exercises for scoliosis, such as Schroth exercise, pilates, and tai chi, could assist in the stabilization of curves, correct spinal alignment, and increase muscle strength and endurance [2, 25, 26, 27]. Exercises are commonly used alone or incorporated with a brace that facilitates self-correction of posture and improves self-awareness of general body alignment [1, 28, 29].
Exercise approaches have also been used to improve postural balance and stability in AIS patients. A previous study by Radwan et al. demonstrated that scoliosis exercise improved postural stability and Cobb angle in the AIS group compared with the control group [2]. AIS patients who are known to have a posteriorly shifted COP position on the sagittal plane, also have a greater postural instability than typically developed adolescents [30]. However, the currently available studies that investigated the effects of exercise on balance in AIS are inconsistent, and there is limited evidence on whether exercise treatments are effective in improving postural balance and stability [31, 32]. This scoping review aimed to evaluate the effects of exercise interventions on balance and postural stability in patients with AIS.
Methods
Search strategy
Flowchart of the study selection process based on PRISMA guidelines.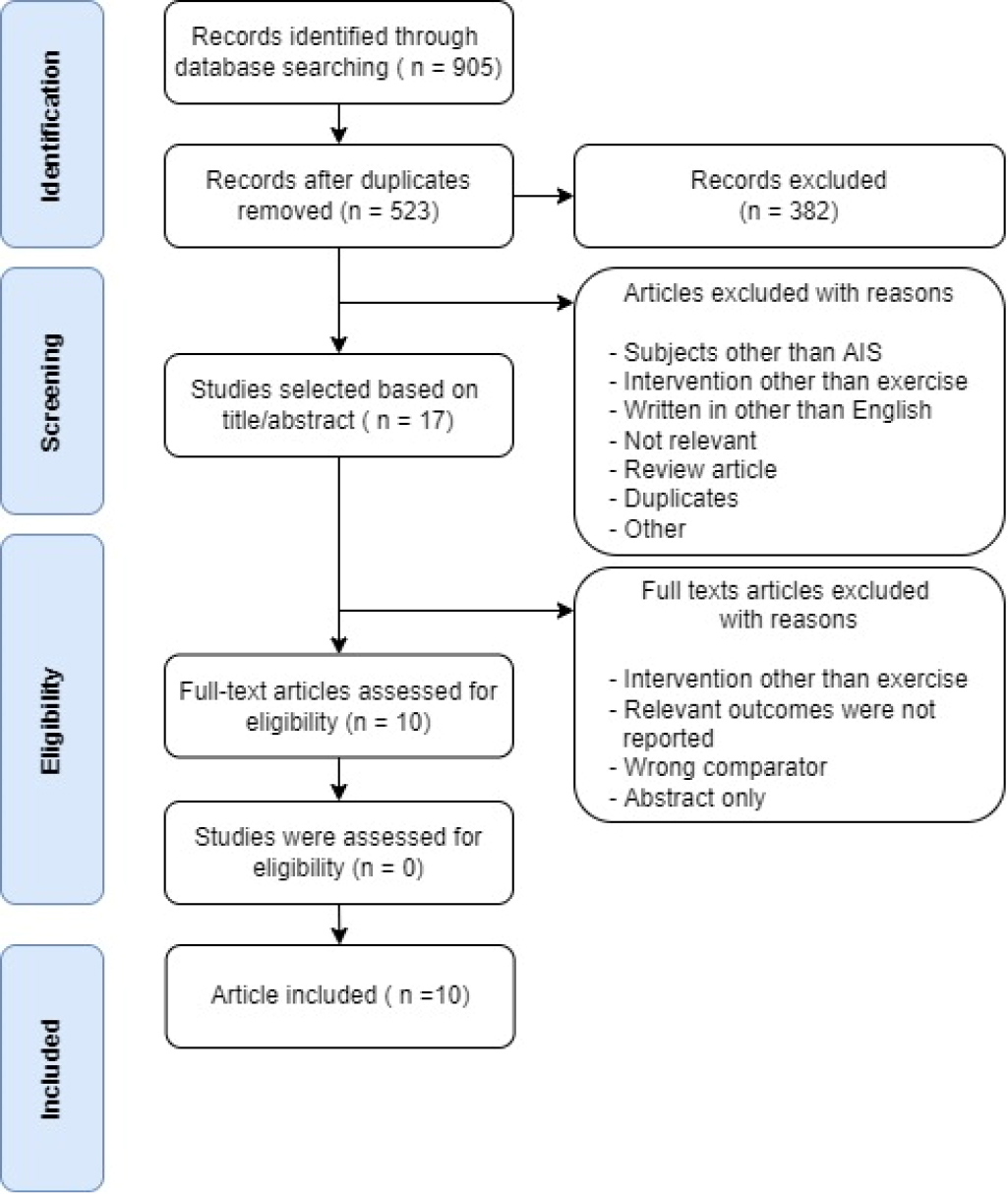
In this review, we utilized the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) guidelines to describe the study selection procedure in the following four databases: Embase, Scopus, PubMed (Medline), and Web of Science. The keywords used were idiopathic scoliosis; AND one of the following: exercise, physiotherapy, physical therapy, rehabilitation, exercise therapy, therapeutic exercise, yoga, Pilates, or tai chi; AND one of the following: kinetic, kinematic, balance, stability, or postural control. The selected studies from each database were cross-checked by two researchers (SMB and SHK). Potentially relevant studies that included the above keywords in the title were screened according to inclusion criteria, and the final selection was validated by investigating relevant abstracts based on the inclusion criteria. Full-text articles from the selected studies were obtained and assessed for eligibility. The risk of bias was minimized by reviewing the titles, abstracts, and full-text articles independently by the two authors. If there was any disagreement on the selection of studies, the two researchers reached a consensus through discussion and third researcher (JHL) also participated in final decision (Fig. 1).
Inclusion criteria
The PICOS principle was used to establish inclu-sion criteria as follows: P (population), subjects with adolescent idiopathic scoliosis; I (intervention), exercise in either experimental or control group; C (comparison), compared with non-scoliosis-specific exercise, conventional exercise or treatment, or no treatment (observation only); O (outcome), balance parameters such as center of pressure variance in antero-posterior and medio-lateral directions, COP sway area and velocity, body alignment and maximal tilt angle, foot pressure, and subjective postural perception; and S (study design); due to the limited number of available randomized controlled trial (RCT) studies, clinical, cross-sectional study, multi-group pre-test-posttest design, one-group pretest-posttest design, and single subject design were also included. Only studies written and published in English have been included.
Exclusion criteria
(1) animal studies; (2) improper statistical methods or descriptions; (3) duplicate publications or incomplete data; (4) systematic reviews; (5) reviews; and (6) meta-analysis.
Data extraction and evaluation of methodological quality
The titles and abstracts of the potentially relevant studies were screened. Two researchers extracted specific data, such as author and date of publication, characteristics of participants, study design, types of interventions, primary and secondary outcome measures, and key results from each selected study. All studies were assessed based on the inclusion criteria, and methodological quality was evaluated. The methodological quality of the selected studies was measured using the PEDro scale. The PEDro scale has verified the validity and reliability of assessing the methodological quality of clinical trials. The PEDro scale consists of 10 items: 1) random allocation of subjects; 2) concealed allocation; 3) similar prognosis at baseline; 4) blind subjects; 5) blind therapists; 6) blind assessors; 7) more than 85% follow-up; 8) intention-to-treat analysis; 9) between-group statistical analysis; and 10) point of variability. PEDro scores of 0–3 are regarded as poor, 4–5 as fair, 6–8 – regarded as good and 9–10 are regarded as excellent [33]. Studies with the above information in the title or abstract were eligible for inclusion. Only studies written and published in English were included (Table 1).
The investigation was reviewed by the Institutional Review Board of Baekseok University, Republic of Korea (BUIRB-202210HR-027) and deemed exempt from ethical approval.
Level and methodological quality of the evidence at PEDro scale
Level and methodological quality of the evidence at PEDro scale
Studies that investigating the effects of exercise on balance parameter
Abbreviation: RCT, randomized controlled trial; OSI, overall stability index; APSI, anteroposterior stability index; MLSI, mediolateral stability index; COP, center of pressure; COP-AP, anteriorposterior center of pressure; COP-ML, mediolateral center of pressure; COP-OS, center of pressure oscillation; PSSE, physiotherapy scoliosis-specific exercise; AP, anteroposterior; ML, mediolateral; EO, eyes opened; EC, eyes closed; PNF, proprioceptive neuromuscular facilitation; COP-TL, center of pressure trace length; C90A, center of pressure 90%-confidence-level ellipse area; BBAT, basic body awareness therapy; CSE, core stabilization exercise; TE, traditional exercise; SPP, subjective postural perception.
The results of the final 10 articles are summarized in Table 2.
Hippotherapy and Schroth’s exercise
Abdel-aziem et al. reported that the overall stability index (OSI), anteroposterior stability index (APSI), and mediolateral stability index (MLSI) significantly decreased after Schroth’s exercise alone or with hippotherapy in patients with AIS [31]. Post-intervention, the Schroth’s exercise with hippotherapy group showed significantly lower OSI, APSI, and MLSI than the group with Schroth’s exercise alone.
Radwan, Ibrahim, and Mahmoud also demonstrated the effects of Schroth’s exercise for three months on OSI, APSI, and MLSI in patients with AIS [2]. The OSI decreased significantly with each measurement (baseline, one-month and three-months post-intervention). The APSI score significantly decreased from baseline to one-month or three-month post-intervention. One month post-intervention, MLSI was significantly decreased compared to baseline, and three-month post-intervention was significantly decreased compared to one-month post-intervention.
Stretching exercise
Radwan et al. measured the head, upper trunk, lower trunk, and pelvic angles during postural exercise to quantify the ability to maintain postural body alignment in patients with AIS [34]. The head and pelvic angles during postural exercise showed no significant differences before and after the stretching exercises. However, the upper and lower trunk angles were significantly increased after stretching exercise.
Self-elongation exercise
Marin et al. measured the displacement of the COP during self-elongation (SE) exercises in patients with AIS [35]. However, the maximum display of the COP along the medio-lateral or anteroposterior direction, the total sway area, and the speed of the COP displacement showed no significant difference between the standing position and the performance of SE.
Exercise protocol of Blount and Moe
Bidari et al. demonstrated the effect of exercise based on the Blount and Moe protocol [36] on static balance in patients with AIS [32]. Patients were allocated into three groups (good, ordinary, and weak) according to the quality and amount of exercise performed, and there were no significant differences in all balance parameters (anterior-posterior or medio-lateral COP displacement on firm or foam surface, with or without brace) among the three groups.
Physiotherapeutic scoliosis-specific exercise
Selthafner et al. demonstrated the effects of physiotherapy scoliosis-specific exercise (PSSE) on postural sway in AIS [37]. Although not statistically analyzed, COP displacement in the anterior-posterior direction increased by 15% and COP displacement in the mediolateral direction decreased by 25%. The COP oscillation effectively moved away from the midline by approximately 16% on the left. The oscillation of the entire body from the midline became more symmetrical after PSSE. For the maximum pressure of the foot, improvements were observed in the forefoot at the left fifth metatarsal (
Lumbar stabilization exercise
Shin, Lee, and Song reported that lumbar stabilization exercise (LSE) effectively improved sitting balance of AIS [4]. With the eyes open, there were significant decreases in the anteroposterior sway angle, sway area, and sway path after LSE. However, sitting balance parameters such as mean balance, right-left sway angle, and maximum velocity were not significantly different. With the eyes closed, the anterior-posterior sway angle, right-left sway angle, sway area, and sway path significantly decreased after LSE. There were no significant differences in the mean balance and maximum velocity.
Proprioceptive neuromuscular facilitation exercise
A single case study by Lee revealed the effects of proprioceptive neuromuscular facilitation (PNF) exercise programs on balancing abilities in female patients with AIS [38]. For the static balance test, sway of the posture on the COP measured by the trace length and COP confidence ellipse area decreased after the 6-week PNF exercise program. Furthermore, the weight distribution between the two feet was even. For the dynamic balance test, dynamic balancing ability symmetry expressed by the maximum leaning angle showed a maintained balance after the PNF exercise programs.
Spinal stabilization exercise
Spinal stabilization exercises (SSE) also affected the dynamic foot pressure of AIS in a study by Lee and Shim [39]. Although plantar pressure measurements of the bag load of 0% of the subjects’ body weight before and after the SSE showed no significant difference, the two areas of the fifth metatarsal and lateral heel had significantly lower plantar pressure with a bag load of 15% of the subjects’ body weight after the SSE.
Core stabilization exercise and basic body awareness therapy
Yagci, Yakut and Simsek investigated the effects of core stabilization exercise (CSE) and basic body awareness therapy (BBAT) on perception of verticality in AIS [40]. Subjective postural vertical perception and total subjective postural perception (SPP) score significantly increased after CSE and BBAT, but there was no significant difference after traditional exercise (TE). However, no significant difference was observed between the CSE and BBAT groups. For SPP parameters at 60
Discussion
The purpose of this scoping review was to evaluate the effects of exercise interventions on balance and postural stability in patients with AIS. According to the results from 10 articles that investigated the effects of exercise programs, several exercises improved the balance parameters such as OSI, APSI, and MLSI.
During hippotherapy, precise, rhythmic, and repetitive patterns of movement that mimic human gait are given to riders, and riders activate stabilizing muscles as a reaction [31, 41, 42]. This riding intervention provides vestibular stimulation, and riders who adapt to the movements of horses change muscle utilization by developing neuromuscular coordination [31, 43, 44]. Therefore, it seems that the activation of the trunk core muscles caused by horse riding contributes to improving OSI, APSI, and MLSI in patients with AIS.
Similarly, the Schroth exercise is also core muscle training and consists of three-dimensional self-correction and stabilization of the corrected posture, as well as patient education [45, 46]. This individualized, corrective breathing exercise causes the contraction of convex areas of the trunk; thus, lengthening and mobilization of soft tissues are provoked in concave areas by directing the inspired air [2, 47]. Thus, improvements in trunk symmetry, weight distribution, and neuromuscular control following corrective exercise can trigger improvements in stability indices, such as OSI, APSI, and MLSI [2].
However, stretching exercises appear to have a negative effect on balance in AIS [34]. Nelson, Kokkonen, and Arnall reported that the stretching technique converts motor units into a fatigue-like state, which decreases the pool of motor units available for activation [48]. This loss of motor units eventually leads to a decrease in performance [48]. Furthermore, static stretching also decreases the viscosity of tendon structures, which results in a reduction in the ability to produce force [34, 49]. For these reasons, stretching prior to tasks negatively affects motor learning [34]. In addition, despite of characteristics of scoliosis as an asymmetric and three-dimensional deformity, it seems there is a lack of studies applied stretching exercises to every muscle involved. Nevertheless, the application of stretching exercise should be considered carefully, since a recent study reported the asymmetry of erector spinae tone in the thoracic or lumbar region in children aged 7–8 with scoliosis [50].
The SE and Blount and Moe exercise protocols had no effect on the dynamic or static balance in AIS [32, 35]. SE involves a variation of the spine that depends on a linear combination of the positions in the pelvis, thoracic spine, lumbar spine, and sacral spine [35]. The Blount and Moe exercise protocol also focuses on the orientation of body segments and curve correction [32]. However, balance impairments in patients with AIS are under the control of the central processing of balance, and it seems that SE or Blount and Moe exercise protocols may have no direct effect on the central nervous system that processes balance control [32].
PSSE decreased COP sway in the coronal plane and pressure of the forefoot and medial hind foot, indicating a procedure for creating proper equilibrium, leading to improved symmetry [37]. When comparing PSSE with the Schroth method, which incorporates sensorimotor, postural, and breathing exercises, and spine stabilization exercises, PSSE has both characteristics. PSSE has been utilized to improve postural static and dynamic balance and correct postural alignment during functional activities [51, 52]. In a study by Selthafner et al., PSSE altered postural control patterns and weight distribution in subjects with AIS [37].
Webber et al. demonstrated that trunk stabilization decreased peak lumbar acceleration during the motion of the upper and lower extremities [53]. Shin, Lee, and Song demonstrated that LSE provided trunk stability for static postural control, and thus reduced sway angle, area, and path, suggesting improved postural balance [4]. In addition, LSE with the eyes closed changed mediolateral sway compared to open eyes because individuals with AIS depend more on proprioception than visual input to maintain balance [22].
Lee demonstrated that a 6-week PNF exercise program increased static and dynamic balance compared to baseline by reducing trace length and sway area and increasing the leaning angle in balance test [38]. The PNF program has been proven effective in correcting spine alignment and enhancing static and dynamic balance [54]. Lee utilized the PNF technique to stabilize the lumbopelvic system during bridge exercises by manual resistance, which progressively narrowed the supporting plane [38]. This PNF technique and instruction decreased spinal deformity and increased the strength of the abdominal muscles, which are associated with balancing ability [38].
Lee and Shim found that spinal stabilization exercises improved balancing ability by effectively spreading the distribution of plantar pressure when a load was applied [39]. In the standing position, the foot is the first body region that contacts the external surface, and plantar pressure is used to diagnose foot problems [56]. To maintain body balance, sensory input is critical for generating normal spinal and pelvic alignment, physical balance, and stability during walking [57, 58, 59]. Park et al. demonstrated that the movement patterns of plantar pressure in both feet were correlated with the magnitude of scoliosis, which affects foot balance [60]. Spinal stabilization exercise may be an effective exercise to prevent morphological changes and improve neuromotor control and physical balance stability.
Yagci, Yakut and Simsek showed that SPP was improved in BBAT and CSE [40]. These results may be associated with improved motor coordination and an upright body orientation. In particular, BBAT educates deep spinal muscles, thereby facilitating postural awareness, dynamic balancing ability, and coordination [61]. CSE stimulates the proprioceptive facilitation effect for correcting contraction of the stabilizer by providing feedback about trunk position, as well as enhanced endurance of core muscles that are essential for maintaining dynamic stability of the spine [62]. Both BBAT and CSE restored the capacity for body awareness and remained upright; thus, they may have a better SPP [63].
AIS patients have fear and dissatisfaction with the abnormal growth and appearance of their bodies [64]. Applying exercise to AIS patients with incorrect perceptions of their spine would help overcome physical and psychological discomfort [65]. In addition, the postural control ability obtained through exercise would help improve self-proprioception through the promotion of spin alignment, resulting in an improvement in response to the rehabilitation process [66]. Thus, the results of the present study can be useful in prescribing exercise therapy for patients with AIS.
This study has several limitations. First, the 10 studies included in this review had a poor to good level of evidence derived from the PEDro scale. Furthermore, only three studies had a control group design. Second, patient characteristics such as Cobb angle, curve type, and type of intervention were heterogeneous. Third, several studies omitted the statistical analysis or failed to demonstrate a significant difference between the groups. Therefore, further studies including high-quality RCT or applying a blinding design, with the qualification of heterogeneity of patients, are needed.
Conclusion
Our results revealed that the effects of different types of exercise on balance in AIS remain controversial. Emerging evidence has shown that interventions stimulating the postural system such as hippotherapy, Schroth exercise, PSSE, trunk stabilization, PNF exercise, spinal stabilization exercise, BBAT, and CSE improve postural balance, but geometric and mechanical detorsion such as stretching and self-elongation exercises do not affect postural balance in patients with AIS. Therefore, physical therapists will need to apply exercise therapy carefully to manage balance impairments in patients with AIS, and further studies are needed to provide stronger evidence.
Ethical approval
The investigation was reviewed by the Institutional Review Board of Baekseok University, Republic of Korea (BUIRB-202210HR-027) and deemed exempt from ethical approval.
Funding
This research was funded by the Ministry of Education (NRF-2021R1G1A1093552).
Informed consent
Not applicable.
Author contributions
All authors contributed to the concept, design, data collection, and analysis of this study.
Footnotes
Acknowledgments
This research was supported by the Basic Science Research Program through the National Research Foundation of Korea (NRF).
Conflict of interest
The authors declare that they have no conflict of interest.
